Introduction
In Japan 8,069 individuals (2,023 men and 6,046
women) were diagnosed with thyroid cancer in 2003, of whom 1,427
(447 men and 980 women) succumbed to their disease. Thus, the crude
death rate is estimated to be 0.84 and 1.61 per 100,000 in men and
women, respectively (1). Over 90%
of the patients have histologically well-differentiated cancer,
with a good prognosis regarding long-term survival. Noguchi et
al (2) reported that >74.4%
of male and >88.8% of female patients with thyroid papillary
cancer in the poor risk group survived for >10 years. However,
the terminal stage of the disease may be associated with airway
stenosis secondary to thyroid enlargement, which, according to the
English-language literature, may occur in 16–60% of the patients
(3).
Upper airway stenosis secondary to thyroid cancer
exhibits characteristics that distinguish it from that caused by
other malignant tumors. First, the slowly progressing nature of
well-differentiated thyroid cancer tends to mask the symptoms and
results in acute onset of severe airway obstruction. Second, this
type of tracheal stenosis is often associated with tracheal
compression caused by the solid thyroid cancer tissue surrounding
the trachea in the limited space of the thoracic inlet; this means
that sufficient enlargement of the airway cannot be achieved
immediately after stent placement, but time is required for the
stent to expand and open up the airway. Third, thyroid cancer
invasion may cause vocal cord paralysis, resulting in difficulties
with sputum expectoration and a deteriorating state of dyspnea.
Even when airway enlargement is achieved after stent placement,
dyspnea may not sufficiently improve in the presence of vocal cord
paralysis, particularly when this is bilateral.
Although severe obstruction of the airway secondary
to thyroid cancer may be considered as a symptom of terminal-stage
disease, it may be quite extensive. Airway stenting may relieve the
symptoms of respiratory impairment and play an important role in
palliative medicine. In this study, we aimed to evaluate the
efficacy of self-expandable metallic stents for relieving central
airway stenosis secondary to thyroid cancer and the complications
associated with long-term stent placement.
Patients and methods
Patients
A retrospective study was conducted of 5 patients
with thyroid cancer, who presented with central airway stenosis
caused by thyroid cancer invasion or lymph node metastases. The
characteristics of the patients, who were recruited in 2009 and
2010, are summarized in Table I.
The indications for interventional bronchoscopy were acute stridor
leading to respiratory insufficiency and surgical inoperability.
The 5 patients were divided into two groups, according to the
location of the stenosis (Table
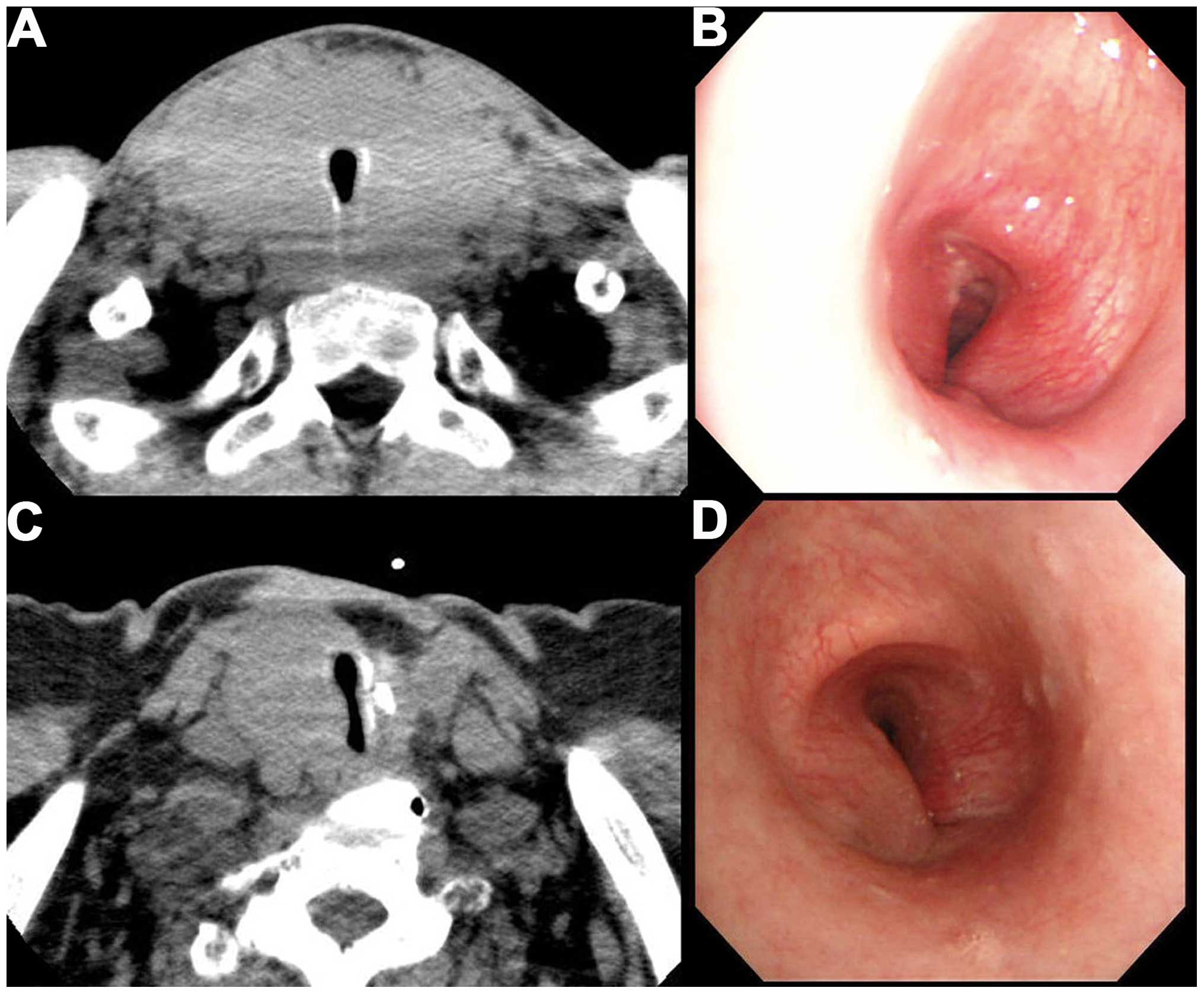
II). Group A had tracheal stenosis at the cervical level,
caused by thyroid cancer (Fig. 1)
and group B had stenosis at the mediastinum, caused by thyroid
cancer or metastatic lymph nodes. The minimal diameter of the
central airway was 2–3 mm and the length of the stenosis was 2–7 cm
(Table II). Four of the 5
patients also exhibited vocal cord paralysis.
 | Table IClinical characteristics of the 5
patients. |
Table I
Clinical characteristics of the 5
patients.
| Characteristics | Data |
|---|
| Gender, no. |
| Male/female | 4/1 |
| Age, years ± SD
(range) | 66±16 (50–82) |
| Histological type,
no. |
| Papillary
carcinoma | 3 |
| Medullary
carcinoma | 1 |
| Anaplastic
carcinoma | 1 |
| Initial
tumor/recurrence, no. | 2/3 |
| Vocal cord paralysis,
no. |
|
Absent/unilateral/bilateral | 1/2/2 |
 | Table IIType of airway stenosis and stent
size. |
Table II
Type of airway stenosis and stent
size.
| Group | Patient | Age (years), gender
histological type | Stenosis | Vocal cord
paralysis | Stent size (mm) |
|---|
|
|---|
| Diameter, mm (%) | Length, cm |
|---|
| A | 1 | 50, M
Medullary | 3 (60) | 2 | Bilateral | 16×60 |
| 2 | 70, F
Papillary | 2 (90) | 3 | Bilateral | 18×60 |
| B | 3 | 82, M
Papillary | 3 (70) | 4 | Absent | 18×60 |
| 4 | 50, M
Anaplastic | 3 (70) | 7 | Right | 18×80 |
| 5 | 76, M
Papillary | 3 (80) | 2 | Left | 18×60 |
Approval for this study was granted by the
Institutional Review Board of Toho University Omori Medical Center
(assurance no. 25–39).
Patient workup
Prior to stenting, computed tomography (CT),
three-dimensional (3D) CT and bronchoscopy were performed to
evaluate the diameter, length and location of the stenosis.
Spirometry with peak-flow analysis and interviewing were performed
to evaluate the objective and subjective symptoms, performance
status (PS), peak expiratory flow (PEF) and percent predicted
forced expiratory volume in 1.0 sec (%FEV1.0). After
stenting, the same procedures were performed periodically to assess
the condition of the stents and monitor complications. Written
informed consent for airway stenting was obtained from each
patient.
Stenting procedures
All the procedures were performed under general
anesthesia in an operating theater equipped with an X-ray
fluoroscope and with a rigid bronchoscope and an argon plasma
coagulator on standby. Following laryngeal mask airway placement,
covered self-expandable metallic stents (Ultraflex; Boston
Scientific, Marlborough, MA, USA) were inserted using a guide wire.
The diameter of the inserted stents ranged between 16 and 18 mm and
their length ranged from 60 to 80 mm (Table II).
Results
Symptom relief
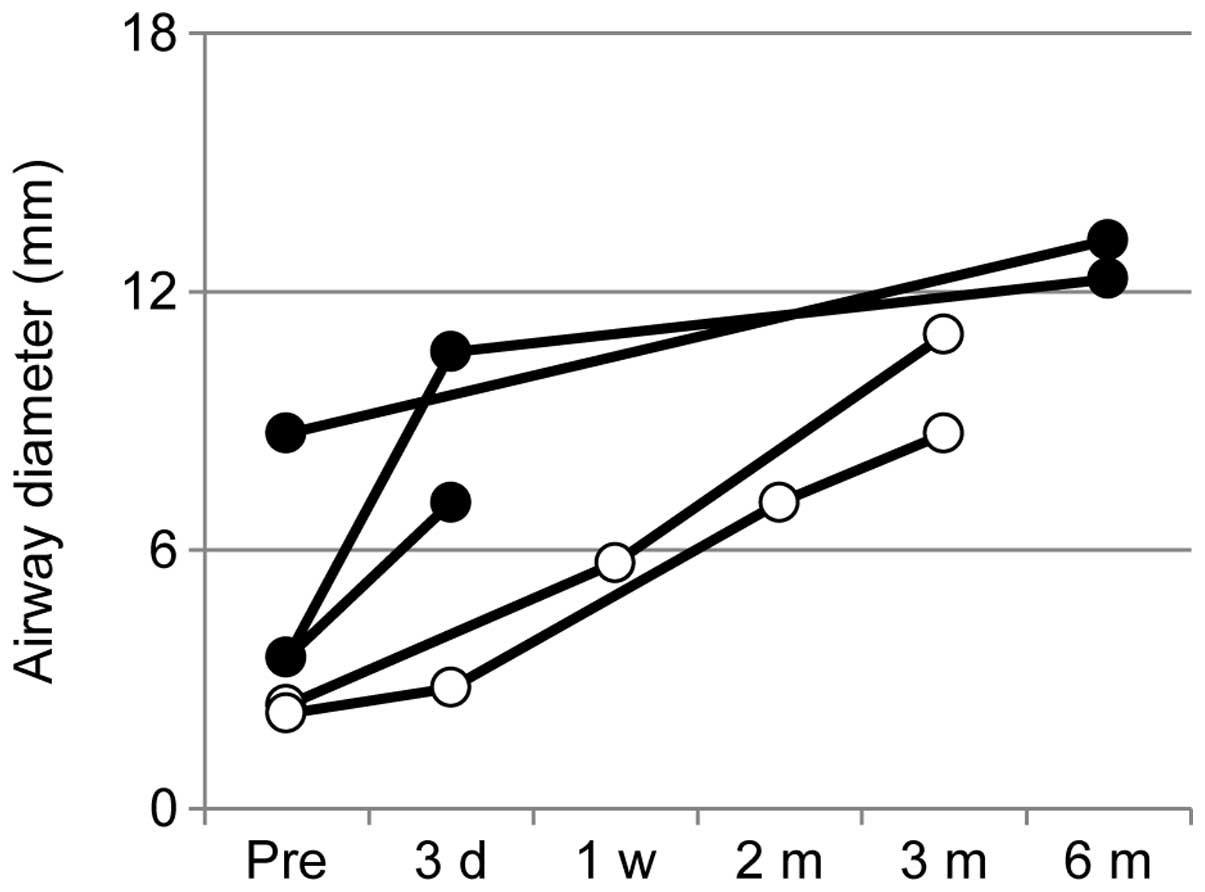
After stenting, immediate symptom relief and
sufficient airway enlargement was achieved in group B within a few
days; however, ~3 months were required in group A (tracheal
stenosis at the cervical level caused by surrounding thyroid
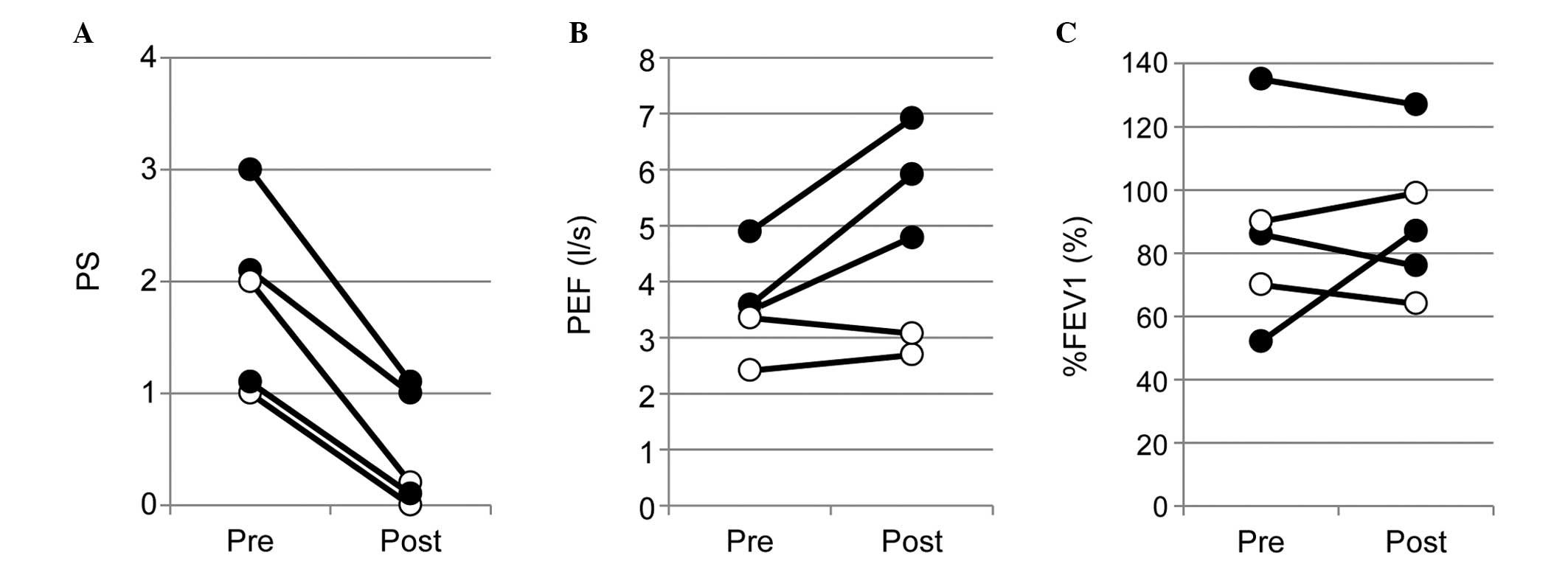
cancer, Fig. 2). Despite vocal
cord paralysis, improvement of PS was achieved in all cases after
stent placement (Fig. 3). Three
patients also exhibited an improvement of pulmonary function
reflected in improved PEF, whereas one patient exhibited an
improvement in %FEV1.0.
Course after stent placement
During the follow-up period, the patient with
anaplastic thyroid cancer (patient 4) succumbed due to rapid
progression of the disease 2 months after stent placement.
Including this case, 3 patients in total (patients 1, 3 and 4)
succumbed to the disease within 8 months, due to deterioration of
their general condition caused by the carcinoma (papillary and
medullary carcinoma). Patient 3 required tracheostomy 6 months
after stenting due to tumor growth. We have been following up the
remaining 2 patients with papillary carcinoma (cases 2 and 5) for
27 and 21 months, respectively, and the patients remain
dyspnea-free (Table II). However,
additional tracheostomy was required in patient 2 due to proximal
granulation tissue formation and progressive bilateral vocal cord
paralysis.
Granulation tissue formation
All the patients were administered tranilast to
prevent granulation tissue formation after stenting. However,
granulation tissue at both ends of the stent developed in 3
patients (Table III). Patient 2,
who suffered from papillary carcinoma and poorly-controlled
diabetes mellitus, experienced rapid and repeated granulation
tissue formation. An additional metallic stent was inserted to
cover the granulation tissue at the bare distal portion of the
initial stent 9 months later and tracheotomy was performed
immediately below the cricoid cartilage 1 month later, due to
granulation tissue formation at the bare proximal portion and
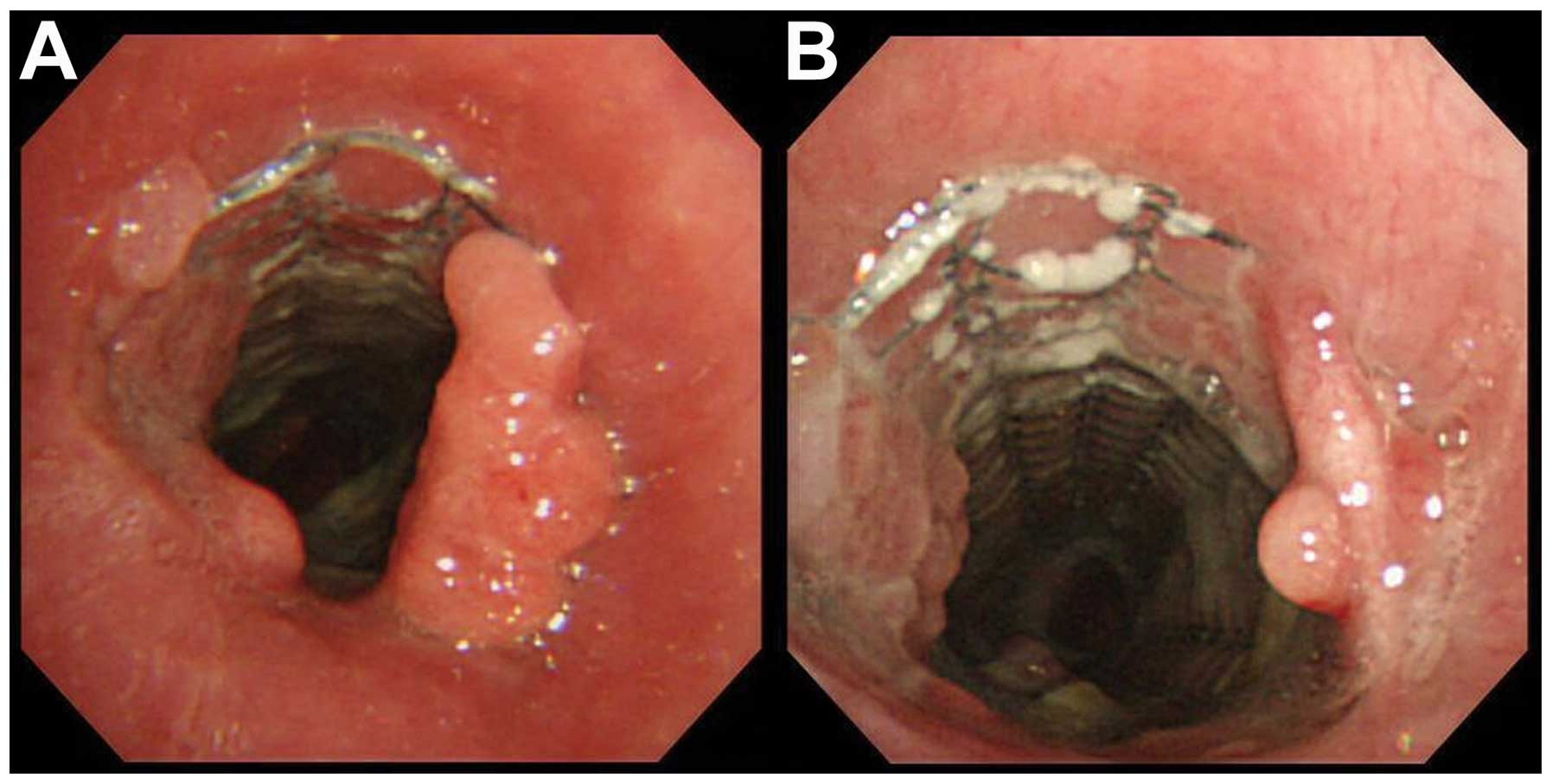
progressive bilateral vocal cord paralysis. In patient 5,
granulation tissue developed at the bare proximal portion 6 months
after stent placement (Fig. 4) and
local treatment with prednisolone (PSL) and mitomycin C (MMC) was
successful and resulted in regression.
 | Table IIIComplications and prognosis. |
Table III
Complications and prognosis.
| Patients | Granulation
tissue | Retained
secretions | Colonization | Prognosis |
|---|
| 1 | Both ends (3 mo) | No | P.
aeruginosa | 8 mo, D |
| 2 | Both ends (9 mo) | Yes | P.
aeruginosa
MRSA | 27 mo, A (10 mo,
tracheostomy) |
| 3 | Absent | No | P.
aeruginosa | 8 mo, D (6 mo,
tracheostomy) |
| 4 | Absent | Yes | P.
aeruginosa
K. oxytoca | 2 mo, D |
| 5 | Both ends (6 mo) | No | MSSA
St. pneumoniae | 21 mo, A |
Sputum retention
Retention of sputum and dried secretions inside the
stent required intervention in patients 2 and 4. As difficulties
with sputum expectoration aggravated the dyspnea, emergency
bronchoscopic lavage was performed in both cases. In patient 4, in
particular, the production of bloody sputum at the site of
anaplastic carcinoma invasion could not be adequately controlled
with the use of the covered metallic stent. Consequently,
solidified adhesive secretion-coagulation deposits developed and
obstructed the stent after 8 days. This coagulated adherent deposit
was removed with a metal brush under general anesthesia.
Bacterial colonization inside the
stent
Table III shows
the results of the sputum culture. Although clarithromycin was
administered to the patients to prevent infection immediately after
stenting, all the stents were colonized by bacteria. Pseudomonas
aeruginosa was detected in all patients, except patient 2.
Methicillin-resistant Staphylococcus aureus (MRSA) was
detected in patient 2 and Klebsiella oxytoca,
Streptococcus pneumoniae and methicillin-sensitive
Staphylococcus aureus were detected in patient 5.
Levofloxacin hydrate was added to the treatment regimen for patient
5 but it was not effective in controlling colonization.
Discussion
The type of stent most suitable for relieving upper
airway stenosis secondary to thyroid cancer remains controversial.
Noppen et al (3) reported
30 patients with airway stenting for tracheal obstruction secondary
to thyroid disease, consisting of 17 with benign disease and 13
with malignancies. The type of stent used in that study was mainly
silicone stents, Dumon or Tygon-Noppen stents for the 13 cancer
patients and an Ultraflex stent for replacement in 1 case where the
Dumon stent had migrated. The Tygon-Noppen stent is a screw-thread
silicone stent modified from an esophageal stent, designed not to
migrate (4). Ultraflex stenting
was also discussed in 3 patients with benign disease, due to
‘specific stenosis characteristics (stenoses of variable axis
diameter)’. Since thyroid cancer has a relatively indolent course,
Tsutsui et al (5)
hypothesized that the durable and replaceable nature of silicone
stents may provide good results and compared 45 stents (12
silicone, 20 metallic and 13 T-tubes) in 35 patients with thyroid
cancer. However, among 10 patients in whom the silicone stents had
been placed in close proximity to the cricoid cartilage, 5 suffered
from supraglottic stenosis and 4 from stent migration. The authors
concluded that use of the uncovered Ultraflex stent had fewer
critical complications compared to the silicone stents. Kim et
al (6) reported that the
placement of covered retrievable self-expandable nitinol stents was
safe and effective in patients with malignant (n=7) or benign (n=2)
thyroid disease. Although one of their three types of stents was
designed with barbs at the middle to prevent migration, the stent
migrated in 2 of 4 such patients and stent replacement was required
twice in each patient.
We selected covered Ultraflex self-expandable
nitinol stents for all the cases, since we consider this type to be
more appropriate compared to silicone stents in cases of extrinsic
tracheal compression (7). These
stents may also be more efficient in preventing tumor ingrowth
through the mesh and are expected to be less harmful compared to
other metallic stents with strong expansion. Therefore, potential
rigid bronchoscope-related supraglottic stenosis in advanced
thyroid cancer patients with edematous changes around their
epiglottis may be avoided. However, in patients with extrinsic
tracheal compression at the cervical level, surrounded by solid
thyroid cancer tissue, a relatively long time was required to
sufficiently enlarge the airway. Although the immediate enlargement
benefits may be marginal with this approach, the patients
benefitted psychologically from arresting the progress of dyspnea.
Effective enlargement was achieved gradually over the next 3
months, without the requirement for intervention using a rigid
bronchoscope.
Although the indications for stenting patients with
anaplastic carcinoma may be debatable, one of our cases achieved a
significant improvement of PS after stenting, despite the poor
prognosis. Stent placement was useful not only for patients with
well-differentiated thyroid cancer, but also for the acutely
deteriorating anaplastic thyroid carcinoma patient. Thus, even only
short-term placement of the stent may play an important role in
palliative medicine.
Granulation tissue formation, sputum retention and
bacterial colonization of the stents are the most common but
burdensome complications of long-term stent placement (5,8). It
has been reported that airway colonization tends to be associated
with sputum retention (3).
Formation of granulation tissue was observed in 3 of our patients.
Bacterial colonization was detected in all patients, 4 of whom had
Pseudomonas aeruginosa. One patient had both Pseudomonas
aeruginosa and MRSA and frequently suffered from dyspnea due to
sputum retention within the stent. That patient required urgent
bronchoscopic lavage. Granulation tissue was observed frequently at
the proximal or the distal bare part of the otherwise covered
stents. Saad et al (8)
described 3 risk factors for developing granulation tissue with
self-expandable metallic stents as follows: i) improperly sized
stents (undersized, with excessive friction; or oversized, with
excessive radial pressure); ii) exuberant bronchial mucosal
inflammation; and iii) placement of any type of stent in the
subglottic trachea. The mechanisms responsible for granulation
tissue formation at the bare parts of the metallic stents have not
been identified thus far; therefore, there are no known means of
prevention. We hypothesized that the mechanisms may be similar to
those occurring in chronic wounds (9). Prolonged periods of inflammation in
wound healing are considered to significantly affect
malgranulation. Factors which prolong inflammation include the
following: i) general conditions due to metabolic disorders,
nutritional problems and wasting syndromes; ii) hypoxia caused by
respiratory or circulatory disorders; iii) interruption of the
circulation due to ischemic disease, congestion, or lymphedema; iv)
continuous infection; and v) secondary injury caused by continuous
external pressure or friction (10). Although we considered the stents
placed in all our patients to be appropriately sized, as documented
by follow-up using 3DCT and/or bronchoscopy, granulation tissue
developed in 3 patients. The pressure and friction exerted by these
metallic stents and the persistent infection possibly participated
in triggering the formation of granulation tissue. According to the
abovementioned hypotheses, patients with thyroid cancer are
considered to be at high risk of granulation tissue formation. The
subglottic trachea is often involved in the stenotic lesion caused
by thyroid cancer, exuberant bronchial mucosal inflammation or
continuous infection occasionally accompanies these phenomena due
to vocal cord paralysis and congestion or lymphedema may be
associated with advanced thyroid cancer, which may lead to
supraglottic stenosis after rigid-bronchoscopic procedures
(5). Levofloxacin and tranilast
had been administered to the patients reported in this study, in
order to prevent granulation tissue formation (11,12),
but proved to be ineffective. In our patients, local injection of
PSL and topical use of MMC (14)
were successful in controlling granulation tissue. Therefore,
testing this regimen in more patients may be of value.
Tsushima et al (14) reported a patient with metallic
stents placed to relieve tracheobronchial stenosis secondary to
thyroid cancer; the patient suffocated at home 56 days after stent
placement, due to sputum retention associated with vocal cord
paralysis. In our study, patient 2 frequently suffered from
obstruction in the stents due to viscous secretions, which had to
be repeatedly removed by bronchoscopy. In patient 4, the anaplastic
thyroid tumor was hemorrhagic and a large number of clots and
viscous secretions obstructed the stent 8 days after placement. We
removed the clots by bronchoscopy under general anesthesia. Noppen
et al (15) recommended
inhalation of aerosolized saline solution twice daily to avoid the
accumulation of dried secretions inside the stents. All the
patients in this study had been instructed to follow similar
procedures; however, frequent observation of the stent interior
remained indispensable. Dried secretions or sputum retention should
be taken into consideration, particularly for patients with vocal
cord paralysis or hemosputum.
This study demonstrated that the placement of
self-expandable metallic stents to relieve central airway stenosis
secondary to advanced thyroid cancer is a beneficial treatment,
even in terminal-stage disease or in patients with anaplastic
thyroid carcinoma. In conclusion, particularly with reference to
differentiated thyroid tumors, as such patients have a relatively
good prognosis in general, periodic and long-term bronchosopic
follow-up is required to control for complications, including
bacterial colonization, sputum retention and granulation tissue
formation.
Acknowledgements
This study was supported in part by a Grant-in-aid
for Scientific Research (C) no. 26462140 from the Japanese Ministry
of Education, Culture, Sports, Science and Technology.
Abbreviations:
|
CT
|
computed tomography
|
|
3D
|
three-dimensional
|
|
PS
|
performance status
|
|
PEF
|
peak expiratory flow
|
|
%FEV1.0
|
percent predicted forced expiratory
volume in 1.0 sec
|
|
PSL
|
prednisolone
|
|
MMC
|
mitomycin C
|
|
P. aeruginosa
|
Pseudomonas aeruginosa
|
|
MRSA
|
methicillin-resistant
Staphylococcus aureus
|
|
K. oxytoca
|
Klebsiella oxytoca
|
|
St. pneumoniae
|
Streptococcus pneumoniae
|
References
|
1
|
Japanese Society of Thyroid
Surgery/Japanese Society of Endocrine Surgeons. Incidence,
morbidity and mortality of thyroid carcinoma in Japan. Guidelines
For Management of Thyroid Tumor. Japanese Society of Thyroid
Surgery/Japanese Society of Endocrine Surgeons, . Kanehara Press;
Tokyo: pp. 21–26. 2010, (In Japanese).
|
|
2
|
Noguchi S, Murakami N and Kawamoto H:
Classification of papillary cancer of the thyroid based on
prognosis. World J Surg. 18:552–557. 1994. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Noppen M, Pierard D, Meysman M, Claes I
and Vincken W: Bacterial colonization of central airways after
stenting. Am J Respir Crit Care Med. 160:672–677. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Noppen M, Meysman M, Claes I, D’Haese J
and Vincken W: Screw-thread vs. Dumon endoprosthesis in the
management of tracheal stenosis. Chest. 115:532–535. 1999.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Tsutsui H, Kubota M, Yamada M, et al:
Airway stenting for the treatment of laryngotracheal stenosis
secondary to thyroid cancer. Respirology. 13:632–638. 2008.
View Article : Google Scholar
|
|
6
|
Kim WK, Shin JH, Kim JH, Song JW and Song
HY: Management of tracheal obstruction caused by benign or
malignant thyroid disease using covered retrievable self-expandable
nitinol stents. Acta Radiol. 51:768–774. 2010. View Article : Google Scholar
|
|
7
|
Nomori H, Kobayashi R, Kodera K, Morinaga
S and Ogawa K: Indications for an expandable metallic stent for
tracheobronchial stenosis. Ann Thorac Surg. 56:1324–1328. 1993.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Saad CP, Murthy S, Krizmanich G and Mehta
AC: Self-expandable metallic airway stents and flexible
bronchoscopy: long-term outcomes analysis. Chest. 124:1993–1999.
2003. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Yuasa R, Takagi K, Takahashi S, et al:
Treatment of granulation after airway stent placement for thyroid
papillary carcinoma in a single case. J Jpn Soc Resp Endoscopy.
33:458–463. 2011.(In Japanese with English abstract).
|
|
10
|
Japanese Society of Pressure Ulcers.
Overview of pressure Ulcers. Guideline for Prevention and
Management of Pressure ulcers. Japanese Society of Pressure Ulcers,
. Kanehara Press; Tokyo: pp. 18–23. 2009, (In Japanese).
|
|
11
|
Terada Y, Sakaguchi Y, Kono T, Nohara J
and Noguchi T: Intrabronchial foreign body extracted with tranilast
and corticosteroid. Ann Thorac Surg. 86:1686–1688. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Suzawa H, Kikuchi S, Arai N and Koda A:
The mechanism involved in the inhibitory action of tranilast on
collagen biosynthesis of keloid fibroblasts. Jpn J Pharmacol.
60:91–96. 1992. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Penafiel A, Lee P, Hsu A and Eng P:
Topical mitomycin-C for obstructing endobronchial granuloma. Ann
Thorac Surg. 82:e22–e23. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Tsushima K, Wakamatsu T, Furihata K, et
al: A case of thyroid cancer treated with stent-in-stent placement
to relieve tracheobronchial stenosis. J Jpn Soc Resp Endoscopy.
24:86–90. 2002.(In Japanese with English abstract).
|
|
15
|
Noppen M, Poppe K, D’Haese J, Meysman M,
Velkeniers B and Vincken W: Interventional bronchoscopy for
treatment of tracheal obstruction secondary to benign or malignant
thyroid disease. Chest. 125:723–730. 2004. View Article : Google Scholar : PubMed/NCBI
|