Introduction
The rate of non-small cell lung cancer (NSCLC)
patients presenting with brain metastases at the time of diagnosis
is 10-20 and 30-50% develop brain metastases during the course of
the disease (1-3). Brain
metastases may have a severe impact on morbidity thus affecting
quality of life due to a variety of symptoms such as nausea,
vomiting, dizziness, headaches, vision problems and neurological
difficulties and are a major cause of mortality. In previous
studies S100B has been suggested as a biomarker for detection of
early brain metastases before symptoms arise and may therefore be
of great clinical importance enabling early initiation of treatment
and possibly both improved quality of life and improved overall
survival (OS) (2,4).
S100B is a calcium binding protein. It is found as a
homo- or hetero-dimers of two different subunits, A and B. S100AB
and S100BB are described as S100B and both are specific for
astrocytes and Schwann cells. The protein is expressed mainly in
glial cells with the highest expression in astrocytes. Lower
expression is found in Schwann cells in the peripheral nervous
system, melanocytes, adipocytes and chondrocytes (2,5).
It is well known that S100B can downregulate the
tumor suppressor gene p53 in melanocytes and inhibit apoptosis
(6). It has been suggested that S100B
promotes brain metastases of lung adenocarcinoma by promoting cell
proliferation, preventing apoptosis and increasing cell migration
and invasion (3,7). Low concentrations of S100B stimulate
neurite outgrowth and survival of neurons whereas high
concentrations stimulate the expression of inflammatory cytokines
and induce apoptosis (5).
Elevated serum S100B is primarily found under
pathological conditions that also compromises the blood-brain
barrier as seen in traumatic brain injury, intracerebral vascular
disease, malignancy, epilepsy and schizophrenia (2). One exception is patients with malignant
melanoma (without brain metastases) where serum values increase
with the clinical stage due to the expression of S100B in
melanocytes (8).
The clinical utility of S100B has been evaluated in
several studies demonstrating that elevated levels are correlated
with a poorer outcome in patients with traumatic brain injury
(9-11).
Also, S100B has been shown to be a predictive biomarker of OS
before first line treatment of disseminated malignant melanoma with
high levels of S100B correlating with poorer outcome (12).
In a prospective study including 38 patients with
newly diagnosed NSCLC and no symptoms of brain metastases, it was
investigated if serum S100B level could be used as a biomarker to
detect subclinical brain metastases. Magnetic resonance imagining
showed brain metastases in seven patients, all presenting with
elevated S100B level (>0.10 µg/l). A total of nine patients also
presenting with elevated levels of S100B had vascular brain damage
with no evidence of brain metastases. However no patients without
brain metastases or vascular disease in the brain were found to
have elevated levels of S100B, thus suggesting that serum S100B may
be used as a screening tool to select patients in need of further
examination for brain metastases (10).
Also, subsequent studies suggested that serum S100B
might serve as biomarker to detect brain metastases in patients
with newly diagnosed NSCLC. Thus, a study by Choi et al
(2) including 128 patients with newly
diagnosed NSCLC found a sensitivity of 89% regarding the ability of
serum S100B to detect brain metastases, but a rather low
specificity which was found to be 43%. In addition, another study
by Pang et al (4) including 30
NSCLC patients showed significantly increased levels of S100B in 15
patients with brain metastases compared to 15 patients without
brain metastases with a very clear cut-off at 0.031 µg/l.
Surprisingly, Liu et al (7)
showed a correlation between S100B and longer OS in NSCLC patients
by analyzing 20 members of the S100 calcium binding protein
family.
Moreover, normal levels of S100B were found in
patients with glioma at the time of diagnosis and during treatment
with no influence on OS, whereas in patients with recurrent glioma
an elevated level of S100B at the time of recurrence was associated
with shorter median survival compared to patients without elevated
S100B (13).
In our previous study, including 101 breast cancer
patients, 46 of which had brain metastases, serum levels of S100B
were not able to identify those with brain metastases (14).
The clinical value of S100B to detect brain
metastases or predict outcome in patients with NSCLC remains
unclear. The aim of this study was to compare baseline level of
serum S100B in NSCLC patients with and without brain
metastases.
Materials and methods
Study population
The cohort of patients were obtained from a
prospective biomarker trial of advanced NSCLC (S-20070014)
conducted between March 2007 and February 2010 at the Department of
Oncology, Vejle Hospital, University Hospital of Southern Denmark
(Vejle, Denmark) (15). The
Declaration of Helsinki was observed and signed informed consent
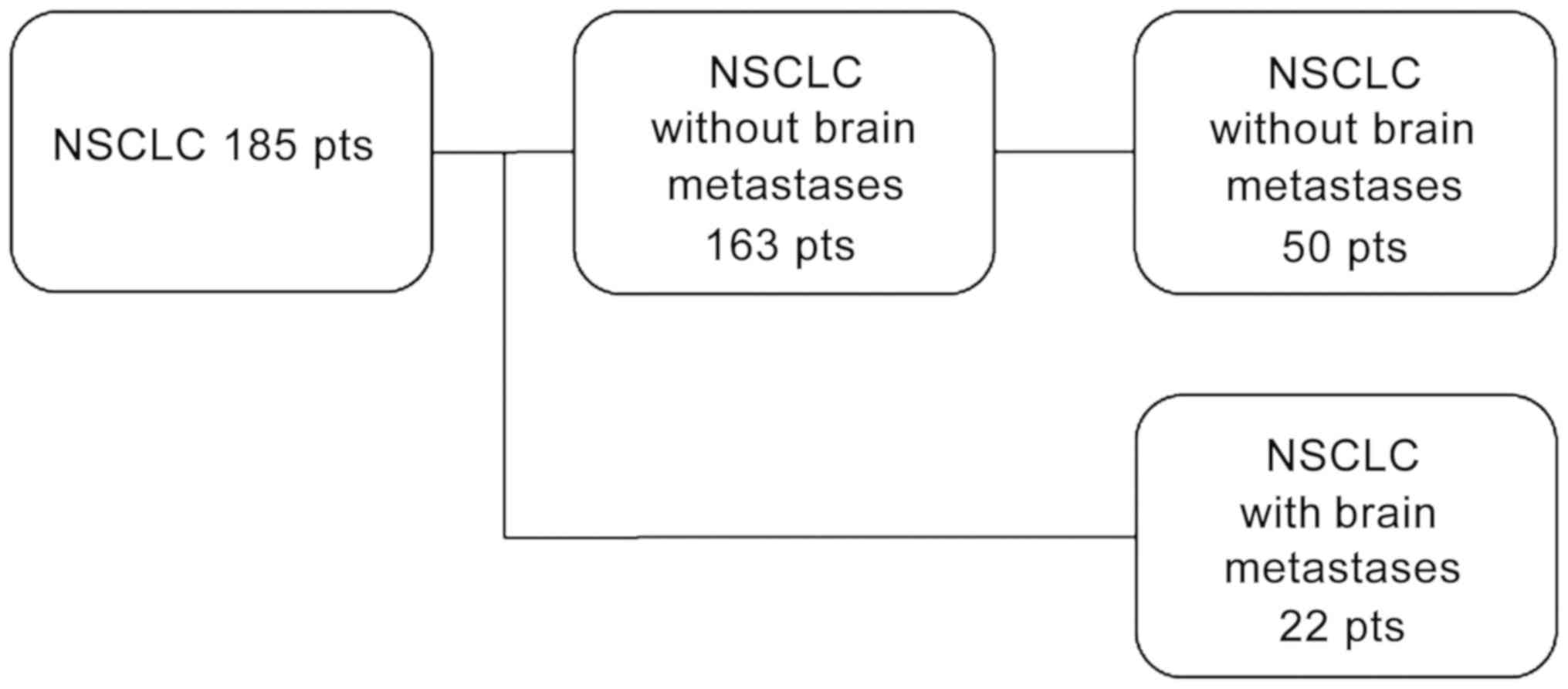
was obtained from all patients. A total of 185 patients with newly
diagnosed stage IV NSCLC were enrolled and pre-treatment blood
samples were drawn at the time of diagnosis. A total of 22 patients
had verified brain metastases at the time of enrollment. Patient
characteristics are shown in Table
I.
 | Table IPatient characteristics. |
Table I
Patient characteristics.
| Characteristics | n | % | n | % | P-value |
|---|
| Age | | | | | 0.016 |
|
≤65 | 16 | 72.7 | 21 | 42 | |
|
≥65 | 6 | 27.3 | 29 | 58 | |
| Sex | | | | | 0.332 |
|
Male | 15 | 68.2 | 28 | 56 | |
|
Female | 7 | 31.8 | 22 | 44 | |
| Performance
status | | | | | 0.206 |
|
0 | 9 | 40.9 | 13 | 26 | |
|
1-2 | 13 | 59.1 | 37 | 74 | |
| Smoking | | | | | 0.285 |
|
Non-smoker
+ | | | | | |
|
Former
smoker | 14 | 63.6 | 25 | 50 | |
| Smoking | 8 | 36.4 | 25 | 50 | |
| Histology | | | | | 0.054 |
|
Adenocarcinoma | 19 | 86.4 | 32 | 64 | |
|
Squamous
carcinoma/other | 3 | 13.6 | 18 | 36 | |
| Liver metastases | | | | | 0.647 |
|
Yes | 3 | 13.6 | 9 | 18 | |
|
No | 19 | 86.4 | 41 | 82 | |
| Bone metastases | | | | | 0.945 |
|
Yes | 5 | 22.7 | 11 | 22 | |
|
No | 17 | 77.3 | 39 | 78 | |
The present study was approved by The Regional
Committees on Health Research Ethics for Southern Denmark
(S-20110005). Serum S100B levels from the 22 patients with brain
metastases were compared with a control group of 50 patients
randomly selected from the remaining 163 patients without known
brain metastases as outlined in the flow chart (Fig. 1).
Clinical and histopathological
data
Histopathological data were obtained from the local
database at the Department of Pathology, Vejle Hospital. Clinical
data such as age, sex, Eastern Cooperative Oncology Group
performance status (PS), smoking history, histology and time of
death were collected from the patient record.
Sample storage and handling
Baseline venous blood (22 ml) was drawn in the
non-fasting state. Samples were collected with minimal stasis in
evacuated blood collection tubes. Blood was allowed to clot at room
temperature before the samples were centrifuged at 2,000 x g for 10
min at 20̊C and immediately after centrifugation the serum phase
was carefully transferred into cryo-tubes and stored at minus 80̊C
until use.
Biochemical analysis
Serum S-100B was analyzed using the CE marked
Elecsys S100 Immunoassay (Roche Diagnostics GmbH). The assay is an
automated sandwich immunoassay using two monoclonal antibodies
against S100B forming a complex to be measured by direct
chemiluminescent technology. Serum specimens were measured
according to the manufacturer's protocol, and each sample was
analyzed twice to ensure the results were valid. The lower
detection limit was 0.005 µg/l and the assay was controlled by
commercial controls at two levels: 0.176 and 2.280 µg/l with an
inter-assay coefficient of variation of 1.3 and 3.6%, respectively.
The reference interval in healthy individuals without NSCLC is
0.02-0.13 µg/l. A cut-off at 0.120 µg/l was used which is in
accordance with the results by Yoon et al (11).
Statistical analysis
Statistical analysis was performed using STATA 11
(StataCorp LP). Using qq-plots and a Shapiro-Wilk test it was found
that S100B was not normally distributed. Box-Cox analysis
determined the need for log transformation with -0.4. Kendall's tau
was used to determine associations between high levels of
correlated blood samples. A Wilcoxon rank sum test was used to test
for differences in S100B levels between the two groups. The levels
of S100B are presented as the range, mean and 95% confidence
intervals.
A univariate analysis was used to determine which
exposure variables might be associated with the outcome (Table II). Variables with P<0.2 were
included in a multivariate logistic regression analysis to further
explore their relation to the levels of S100B. A receiver operating
characteristics (ROC) curve analysis was used to set a cut-off
value for S100B in patients with and without brain metastases,
respectively. P<0.05 was considered to indicate a statistically
significant difference.
 | Table IIUnivariate analysis of prognostic
factors of brain metastases. |
Table II
Univariate analysis of prognostic
factors of brain metastases.
| Factors | P-value |
|---|
| Sex |
|
Male:
female | 0.088 |
| Age |
|
≤65;
>65 | 0.972 |
| Performance
status |
|
0; 1-2 | 0.691 |
| Smoking |
|
Never/former;
recent/unknown | 0.952 |
| Histology |
|
Adenocarcinoma;
squamous cell carcinoma/others | 0.028 |
| Brain
metastases |
|
No; yes | 0.852 |
| Distant
metastases |
|
No; yes | 0.244 |
Results
Patient characteristics
The final analysis included a total of 72 patients.
A total of 22 of the patients had brain metastases and 50 did not
have brain metastases. The two groups were comparable only
differing in age (P=0.016). In the group of patients with brain
metastases patients were younger and with a better PS compared to
the other group. The most common histological subtype was
adenocarcinoma (Table I).
S100B
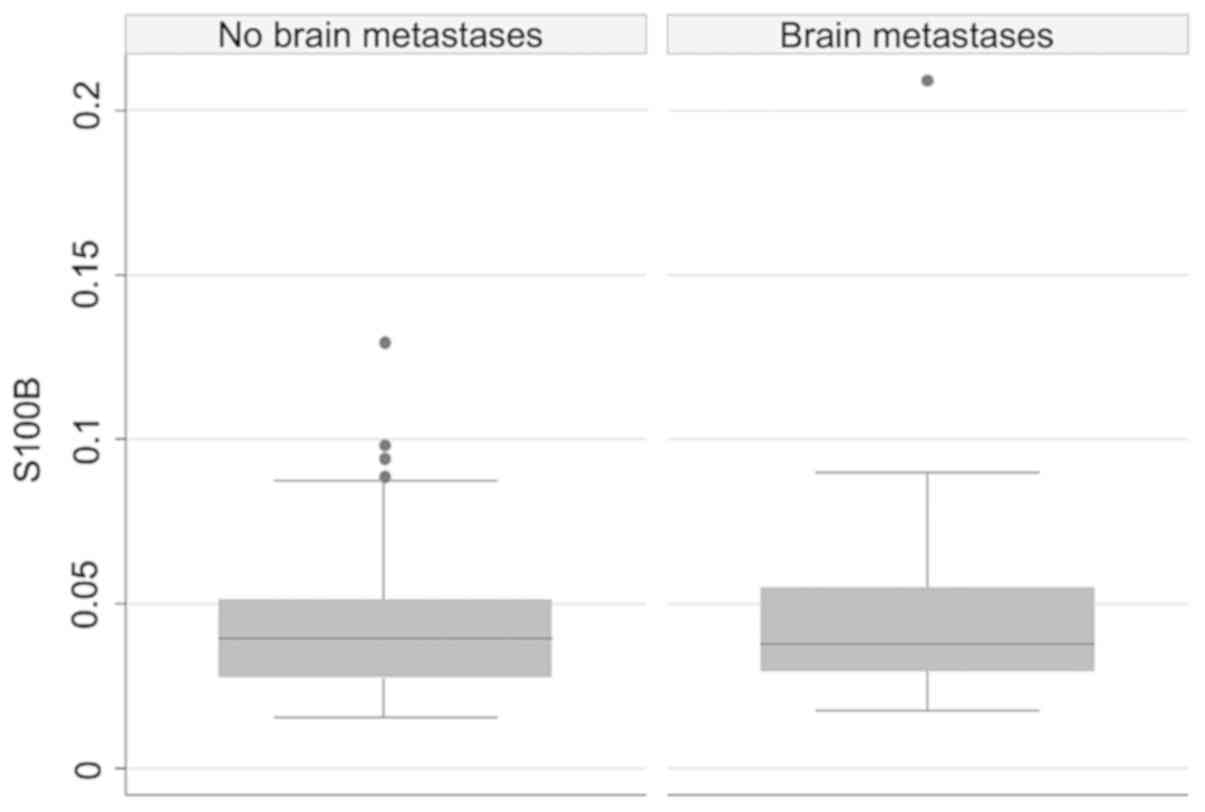
No statistically significant difference in the level
of S100B was found between the group with and without brain
metastases [range 0.018-0.209 µg/l, mean 0.049 µg/l, 95% confidence
interval (CI), 0.032-0.067 µg/l and range 0.016-0.130 µg/l, mean
0.044 µg/l, 95% CI, 0.037-0.051 µg/l], respectively (P=0.852). One
patient was considered an outlier and excluded due to S100B levels
>1.0 µg/l in both measurements, which is far higher than in any
of the other patients (Fig. 2).
Univariate and multivariate
analysis
A univariate analysis was performed for the
following variables: Sex (male; female), age (≤65;>65), PS
(0;1-2), smoking history (never/former; current/unknown), histology
(adenocarcinoma; squamous cell carcinoma/others), brain metastases
(no; yes), distant metastases other than in the brain (no; yes),
including metastases in the liver, bone, cutis and kidney. Only sex
(P=0.088) and histology (P=0.028) from the candidate variables for
multivariate modelling had a P<0.2. Table I presents the results of the
univariate analysis. In the multivariate analysis only histology
(P=0.029) remained statistically significant while sex (P=0.132)
was not statistically significant. Only three patients had S100B
levels exceeding the cut-off value of 0.120 µg/l. The ROC curve
analysis did not reveal a cut-off value for S100B in patients with
and without brain metastases (Fig.
S1).
Discussion
The current study found no difference in serum
levels of S100B between NSCLC patients with and without brain
metastases. Thus, the present study was not able to confirm the
results of previous studies which suggested that S100B may be used
as a diagnostic biomarker to detect early brain metastases in
patients with advanced NSCLC (2,4,16). The levels of S100B were surprisingly
equal in the two groups, suggesting that S100B cannot be used as a
biomarker to detect brain metastases. This correlates with the
results from our previous study showing no difference between
breast cancer patients with and without brain metastases (14).
Both Choi et al (2) and Pang et al (4) found significantly elevated levels of
S100B in patients with brain metastases compared to patients
without brain metastases, although the measured levels of S100B
still remained within the normal range. The clinical value of the
very clear cutoff of S100B in patients with and without brain
metastases demonstrated by Choi et al (2) could not be verified in the present
study. Chen et al (16) found
that S100B is a sensitive and specific biomarker of brain
metastasis in Chinese patients and can be used as a prognostic tool
in daily clinics.
Trauma to the brain caused by traumatic brain
injury, intracerebral vascular disease, malignancy, epilepsy and
schizophrenia is known to cause high levels of serum S100B. It is
obvious to conclude that the number, size and location of brain
metastases might be of importance to S100B serum levels (2). Large metastases are likely to cause more
damage and thereby release higher levels of S100B into the blood
stream, making this information relevant. Patients in the current
study had no imaging of the brain performed prior to entering the
study, which poses a risk of patients with subclinical metastases
falsely having been categorized as ‘without brain metastases’ and
furthermore the present study has no supplementary data on other
conditions potentially affecting the serum levels of S100B.
However, based on the very similar levels of S100B between the two
groups and among the patients in each group this is unlikely to
have influenced the results.
The univariate analysis was preplanned and to
investigate the subject further multivariate logistic regression
analysis was chosen too, knowing that the sample size was small,
and this might be a limitation in the present study.
Mu et al (17)
looked at the levels of serum S100B in 138 patients with small cell
lung cancer (SCLC) and compared with a healthy control group. The
results showed higher levels of S100B in the group with SCLC.
Furthermore, the subgroup with brain metastases had the highest
level of serum S100B and higher levels than the other subgroups.
They concluded that S100B can serve as a serological marker for
brain metastases from SCLC. Maybe these results are partly
explained by the high invasion ability seen in this type of lung
cancer and thereby more severe brain damage resulting in higher
levels of S100B.
In conclusion, the present results did not indicate
a significant correlation between the level of S100B and the
presence of brain metastases in patients with advanced NSCLC. The
current study could not verify a clear cut-off of S100B in patients
with and without brain metastases. Therefore, S100B was not found
to be useful as a biomarker in advanced NSCLC for detection of
brain metastases at the time of diagnosis. Since previous studies
have suggested otherwise, further investigation is warranted to
determine the clinical role of S100B as a biomarker for brain
metastases in NSCLC.
Supplementary Material
Receiver operating characteristic
curve showing that there was no cut-off value for S100B in patients
with and without brain metastases.
Acknowledgements
The authors would like to thank the medical
laboratory technologists Mrs Birgitte Knudsen and Mrs Lone
Frischknecht for their excellent laboratory work.
Funding
The present study was funded by the Research Council
at Vejle Hospital, University Hospital of Southern Denmark (Vejle,
Denmark).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
MK analyzed and interpreted the data regarding
s100B, and was a major contributor in writing the manuscript. TB
performed the statistical analysis, analyzed the data regarding
S100B, and was a major contributor in writing the manuscript. JSM
analyzed the blood samples and contributed to writing and
proofreading the manuscript. ADN collected the data and assisted in
proofreading the manuscript. All authors read and approved the
final manuscript.
Ethics approval and consent to
participate
The Declaration of Helsinki was observed and signed
informed consent was obtained from all patients. The present study
was approved by The Regional Committees on Health Research Ethics
for Southern Denmark (approval no. S-20110005).
Patient consent for publication
All patients provided signed informed consent for
publication in an international peer-reviewed journal with
authorship according to the Vancouver rules.
Competing interests
The authors declare that they have no conflict of
interest.
References
|
1
|
Preusser M, Winkler F, Valiente M,
Manegold C, Moyal E, Widhalm Tonn JC and Zielinski C: Recent
advances in the biology and treatment of brain metastases of
non-small cell lung cancer: Summary of a multidisciplinary
roundtable discussion. ESMO Open. 3(e000262)2018.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Choi H, Puvenna V, Brennan C, Mahmoud S,
Wang XF, Phillips M, Janigro D and Mazzone P: S100B and S100B
autoantibody as biomarkers for early detection of brain metastases
in lung cancer. Transl Lung Cancer Res. 5:413–419. 2016.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Jiang W, Jia Q, Liu L, Zhao X, Tan A, Ma N
and Zhang H: S100B promotes the proliferation, migration and
invasion of specific brain metastatic lung adenocarcinoma cell
line. Cell Biochem Funct. 29:582–588. 2011.PubMed/NCBI View
Article : Google Scholar
|
|
4
|
Pang X, Min J, Liu L, Liu Y, Ma N and
Zhang H: S100B protein as a possible participant in the brain
metastasis of NSCLC. Med Oncol. 29:2626–2632. 2012.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Korfias S, Stranjalis G, Papadimitriou A,
Psachoulia C, Daskalakis G, Antsaklis A and Sakas DE: Serum S-100B
protein as a biochemical marker of brain injury: A review of
current concepts. Curr Med Chem. 13:3719–3731. 2006.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Lin J, Yang Q, Wilder PT, Carrier F and
Weber DJ: The calcium-binding protein S100B down-regulates p53 and
apoptosis in malignant melanoma. J Biol Chem. 285:27487–27498.
2010.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Liu Y, Cui J, Tang YL, Huang L, Zhou CY
and Xu JX: Prognostic roles of mRNA expression of S100 in
non-small-cell lung cancer. Biomed Res Int.
2018(9815806)2018.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Sandru A Voinea SV, Bolovan M, Cinca S,
Bordea C and Blidaru A: The significance of serum S100, MIA and LDH
in cutaneus malignant melanoma. Rom J Biolchem. 48:75–88.
2011.PubMed/NCBI View
Article : Google Scholar
|
|
9
|
Vos PE, Jacobs B, Andriessen TM, Lamers
KJ, Borm GF, Beems T, Edwards M, Rosmalen CF and Vissers JL: GFAP
and S100B are biomarkers of traumatic brain injury: An
observational cohort study. Neurology. 75:1786–1793.
2010.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Vogelbaum MA, Masaryk T, Mazzone P,
Mekhail T, Fazio V, McCartney S, Marchi N, Kanner A and Janigro D:
S100beta as a predictor of brain metastases: Brain versus
cerebrovascular damage. Cancer. 104:817–824. 2005.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Yoon SM, Choi YJ, Kim HJ, Shim JJ, Bae HG
and Yun IG: Prognostic value of serum s100 protein by elecsys s100
immunoassay in patients with spontaneous subarachnoid and
intracerebral hemorrhages. J Korean Neurosurg Soc. 44:308–13.
2008.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Weide B, Richter S, Büttner P, Leiter U,
Forschner A, Bauer J, Held L, Eigentler TK, Meier F and Garbe C:
Serum S100B, lactate dehydrogenase and brain metastasis are
prognostic factors in patients with distant melanoma metastasis and
systemic therapy. PLoS One. 8(e81624)2013.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Holla FK, Postma TJ, Blankenstein MA, van
Mierlo TJM, Vos MJ, Sizoo EM, de Groot M, Uitdehaag BMJ, Buter J,
Klein M, et al: Prognostic value of the S100B protein in newly
diagnosed and recurrent glioma patients: A serial analysis. J
Neurooncol. 129:525–352. 2016.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Bechmann T, Madsen JS, Brandslund I, Lund
ED, Ormstrup T, Jakobsen EH, Jylling AM, Steffensen KD and Jakobsen
A: Predicting brain metastases of breast cancer based on serum
S100B and serum HER2. Oncol Lett. 6:1265–1270. 2013.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Nygaard AD, Garm Spindler KL, Pallisgaard
N, Andersen RF and Jakobsen A: The prognostic value of KRAS mutated
plasma DNA in advanced non-small cell lung cancer. Lung Cancer.
79:312–317. 2013.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Chen L, Hu X, Wu H, Jia Y, Liu J, Mu X, Wu
H and Zhao Y: Over-expression of S100B protein as a serum marker of
brain metastasis in non-small cell lung cancer and its prognostic
value. Pathol Res Pract. 215:427–432. 2019.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Mu S, Ma H, Shi J and Zhen D: The
expression of S100B protein in serum of patients with brain
metastases from small-cell lung cancer and its clinical
significance. Oncol Lett. 14:7107–7110. 2017.PubMed/NCBI View Article : Google Scholar
|