Introduction
Hepatocellular carcinoma (HCC) is a common
malignancy worldwide and is now the third major cause of
cancer-related death in Japan (1).
Vascular invasion, particularly portal veinous tumor thrombus
(PVTT), is one of the indicators of patient prognosis and has been
well documented. The mortality rate is very high in patients with
unresectable tumors, and the quality of life (QOL) is poor due to
intractable ascites or esophageal bleeding. In such a situation,
conventional therapies generally have no clinical effect,
therefore, a new strategy is required for patients of advanced HCC
with PVTT in the major trunk.
Recently, sorafenib, an oral multikinase inhibitor
of the vascular endothelial growth factor receptor, the
platelet-derived growth factor receptor and Raf, has been
demonstrated to prolong median survival and the time to progression
by nearly 3 months in patients with advanced HCC as compared with
those administered a placebo (2).
However, no complete response and few partial responses (2%) were
found in the same study. Although this drug can be used for the
treatment of patients with advanced HCC, its clinical effectiveness
is still controversial in Japan. According to the consensus-based
clinical manual proposed by the Japan Society of Hepatology
(3), arterial infusion
chemotherapy using an implantable drug delivery system is
recommended as one of the treatments for advanced HCC with portal
venous invasion. Several recent studies have indicated the
beneficial effects of interferon (IFN)-α-based combination
chemotherapies for HCC (4–8). We also reported the clinical
efficiency of IFN-α and 5-fluorouracil (5-FU) combination therapy
for advanced HCC with portal venous tumor thrombi and intrahepatic
metastasis (9–11), including the mechanism of the
anti-tumor effect (12–19). In addition, we applied this
combined chemotherapy (IFN/5-FU) for resectable HCC as a
postoperative adjuvant (20) and a
multimodal treatment (21).
In the present study, we investigated the clinical
effect of IFN/5-FU therapy for resectable advanced HCC with PVTT as
a postoperative adjuvant therapy, as an extention of our previous
report (20).
Patients and methods
Patients
Of the patients with HCC who were admitted and
underwent curative hepatic resection at the Department of Surgery,
Osaka University Hospital, 50 were included in this study based on
the identification of a tumor thrombus either in the major or first
branch of the portal vein (Vp3 or 4) (22). Liver function tests and imaging
techniques, including computed tomography (CT) with hepatic
angiography and arterial portography, revealed that these cases
were resectable and subsequently they underwent hepatectomy. Of the
50 patients, 30 patients, from 1998 to 2008, had an intra-arterial
catheter inserted through the gastro-duodenal artery with an
implanted drug delivery system during the operation to facilitate
postoperative adjuvant IFN/5-FU combined chemotherapy (9–11).
They were treated with 3 cycles as a postoperative adjuvant. The
demographic data of these patients are shown in Table IA. The 15 patients, no. 1–15, are
the same patients as in our previous study (20), followed up for a longer period.
Another 20 patients, from 1987 to 2007, with the same tumor stage
of advanced HCC and Vp3 or 4, underwent surgery but did not receive
combined IFN/5-FU therapy. They were treated with appropriate local
HCC therapy except for 3 cases (no. 44, 45 and 48) who received
only 5-FU intra-arterial chemotherapy without IFN. The demographic
data of these patients are shown in Table IB. The 15 patients, no. 31–45, are
the same patients as in our previous study (28), followed up for a longer period. The
cases, no. 31–43 are the historical controls; no. 44–50 refused
IFN/5-FU combined chemotherapy. These 2 groups were compared in
terms of features of HCC, hepatic function, surgery, clinical
effects, disease-free and overall survival.
 | Table IDemographics of the IFN/5-FU and
non-IFN/5-FU adjuvant groups. A, IFN/5-FU adjuvant group (n=30) |
Table I
Demographics of the IFN/5-FU and
non-IFN/5-FU adjuvant groups. A, IFN/5-FU adjuvant group (n=30)
A, IFN/5-FU adjuvant
group (n=30)
|
|---|
| Case | Age | Gender | T | M | N | Vp | Stage | Surgery | Alb | PT/HPT | ICGR-15 | AFP | PIVKA-II | Virus |
|---|
| 1 | 47 | M | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 4.5 | 81/91 | 4 | 11,400 | 7,900 | B |
| 2 | 69 | M | 4 | 0 | 0 | 3 | 4A | Extended anterior
segmentectomy | 3.7 | 86/85 | 21 | 768 | 14,784 | C |
| 3 | 54 | M | 4 | 0 | 1 | 4 | 4A | Right
lobectomy | 3.5 | 64/105 | 16 | 28 | 1,847 | B+C |
| 4 | 47 | M | 4 | 0 | 0 | 4 | 4A | Extended right
lobectomy | 3.4 | 74/67 | 26 | 27 | 2,067 | B+C |
| 5 | 60 | M | 4 | 0 | 0 | 3 | 4A | Extended posterior
segmentectomy | 3.9 | 71/69 | 16 | <5 | <40 | B |
| 6 | 80 | M | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 4.0 | 74/66 | 26 | 19 | 1,568 | B+C |
| 7 | 34 | M | 4 | 0 | 0 | 4 | 4A | Extended left
lobectomy | 3.9 | 90/89 | 4 | 456 | 1,153 | B |
| 8 | 66 | M | 4 | 0 | 0 | 3 | 4A | Extended medial
segmentectomy | 3.3 | 75/87 | 15 | 5 | 298 | C |
| 9 | 54 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.5 | 77/62 | 14 | 8,700 | 353,617 | B |
| 10 | 54 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.7 | 65/85 | 21 | 32,930 | <40 | B+C |
| 11 | 69 | M | 4 | 0 | 0 | 4 | 4A | Right lobectomy and
pancreato-duodenectomy | 4.1 | 90/93 | 17 | 7,473 | 205 | B+C |
| 12 | 54 | M | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 3.8 | 82/78 | 17 | 680 | <40 | C |
| 13 | 56 | F | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 3.6 | 71/63 | 19 | 13,260 | 1,039 | C |
| 14 | 62 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.6 | 63/73 | 18 | 23,500 | 476 | B+C |
| 15 | 58 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.8 | 85/87 | 16 | 6,500 | 1,200 | C |
| 16 | 63 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.2 | 93/97 | 29 | 390,000 | 40,775 | C |
| 17 | 58 | M | 4 | 0 | 0 | 4 | 4A | Extended left
lobectomy | 4.2 | 93/95 | 6 | 6,840 | 51,265 | B |
| 18 | 67 | M | 4 | 0 | 0 | 3 | 4A | Extended left
lobectomy | 4.4 | 76/81 | 15 | 27 | 48 | C |
| 19 | 61 | M | 4 | 0 | 0 | 4 | 4A | Extended left
lobectomy | 4.0 | 74/76 | 21 | 34 | <40 | C |
| 20 | 67 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.1 | 63/72 | 8 | 2,461 | 32,742 | B |
| 21 | 63 | M | 4 | 0 | 0 | 4 | 4A | Right lobectomy and
partial resection of lung | 3.4 | 68/85 | 17 | 6,325 | <40 | B |
| 22 | 58 | M | 4 | 0 | 0 | 3 | 4A | Extended posterior
segmentectomy | 4.4 | 68/61 | 12 | 7 | 76 | B |
| 23 | 73 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.9 | 72/71 | 26 | 23 | <40 | B+C |
| 24 | 56 | M | 4 | 0 | 0 | 4 | 4A | Extended left
lobectomy | 3.5 | 64/54 | 24 | 5 | <40 | B |
| 25 | 66 | M | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 3.5 | 57/85 | 20 | 19,735 | 97 | B |
| 26 | 58 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.2 | 78/79 | 14 | 486 | 88 | C |
| 27 | 70 | M | 4 | 0 | 0 | 4 | 4A | Left lobectomy | 4.3 | 68/57 | 7 | 56,479 | 282 | C |
| 28 | 62 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.9 | 77/76 | 13 | 89 | 263 | C |
| 29 | 55 | M | 4 | 0 | 0 | 3 | 4A | Extended anterior
segmentectomy | 4.3 | 70/72 | 12 | 847 | 1,174 | B |
| 30 | 61 | M | 4 | 0 | 0 | 4 | 4A | Extended right
lobectomy | 3.5 | 79/83 | 13 | 376 | 2,453 | B+C |
B, The non-IFN/5FU
adjuvant group (n=20)
|
|---|
| Case | Age | Gender | T | M | N | Vp | Stage | Surgery | Alb | PT/HPT | ICGR-15 | AFP | PIVKA-II | Virus |
|---|
| 31 | 72 | M | 4 | 0 | 1 | 3 | 4A | Right
lobectomy | 4.3 | ND/89 | 15 | 10,876 | - | - |
| 32 | 56 | M | 4 | 0 | 0 | 3 | 4A | Right
lobectomy | 3.2 | ND/74 | 23 | 377 | - | - |
| 33 | 42 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.1 | ND/82 | 14 | 67 | - | B |
| 34 | 65 | M | 4 | 0 | 0 | 4 | 4A | Extended left
lobectomy | 4.0 | ND/133 | 6 | 5 | - | B |
| 35 | 58 | M | 4 | 0 | 0 | 3 | 4A | Right
lobectomy | 3.7 | ND/72 | 16 | 227 | - | - |
| 36 | 61 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.7 | ND/75 | 80 | 10,256 | - | - |
| 37 | 62 | M | 4 | 0 | 0 | 3 | 4A | Leteral
segmentectomy | 3.8 | ND/73 | 19 | 105,360 | - | - |
| 38 | 34 | M | 4 | 0 | 0 | 3 | 4A | Right
lobectomy | 2.9 | 61/59 | 6 | 10,332 | 10,240 | B |
| 39 | 56 | M | 4 | 0 | 0 | 3 | 4A | Left lobectomy | 3.1 | 76/52 | 11 | 75 | 1,450 | B |
| 40 | 48 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 2.8 | 58/57 | 14 | 9 | 62.5 | B |
| 41 | 54 | M | 4 | 0 | 1 | 4 | 4A | Extended right
lobectomy | 3.0 | 85/93 | - | 1,500 | 21,300 | - |
| 42 | 58 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.2 | 84/72 | 19 | 2,208 | 62.5 | B |
| 43 | 68 | M | 4 | 0 | 0 | 3 | 4A | Extended posterior
segmentectomy | 4.2 | 62/65 | 14 | 144 | 6,846 | C |
| 44 | 69 | F | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.7 | 97/97 | 7 | 2,900 | 571 | C |
| 45 | 67 | M | 4 | 0 | 0 | 3 | 4A | Extended posterior
segmentectomy | 2.9 | 67/60 | 35 | 4,733 | 18,625 | C |
| 46 | 41 | M | 4 | 0 | 0 | 3 | 4A | Extended left
lobectomy | 3.4 | ND/64 | 13 | 5 | - | B |
| 47 | 58 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 4.1 | ND/84 | 19 | 30,646 | - | - |
| 48 | 63 | M | 4 | 0 | 0 | 3 | 4A | Extended posterior
segmentectomy | 3.4 | 72/84 | 15 | 21 | 62.5 | C |
| 49 | 76 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.5 | 85/78 | 18 | 16 | 224 | C |
| 50 | 74 | M | 4 | 0 | 0 | 4 | 4A | Right
lobectomy | 3.1 | 58/57 | 14 | 11 | 2,098 | B+C |
The TNM stage and grade of portal vein thrombus were
classified according to the 5th edition of the General Rules for
the Clinical and Pathological Study of Primary Liver Cancer by the
Liver Cancer Study Group of Japan (22). The criteria for selection for
intra-arterial combination treatment included i) the absence of
extra-hepatic metastases, ii) AST and ALT levels <100 IU/l, iii)
a platelet count >80,000/mm3, iv) successful
implantation of an intra-arterial catheter and drug delivery system
and v) a performance status (Eastern Cooperative Oncology Group,
ECOG) (23) of level 0–1.
Treatment regimen of IFN/5-FU combination
chemotherapy and follow-up after surgery
After obtaining informed written consent, each
patient was treated with subcutaneous administration of IFN-α (OIF,
Otsuka Pharmaceutical Co., Tokyo) and an intra-arterial infusion of
5-FU (Kyowa Hakko Co., Tokyo). IFN-α [5×106 U (5 MU)]
was administered on Days 1, 3 and 5 of every week (9–11).
Continuous infusion chemotherapy (5-FU, 300 mg/mm3/day)
through the proper hepatic artery was applied 5 days/week for 2
weeks via a catheter connected to a subcutaneously implanted drug
delivery system. All anti-cancer therapies were discontinued when
adverse effects reached level 2 according to the ECOG
classification (23). In addition
to serum chemistry, tumor markers such as α-fetoprotein (AFP) and
protein induced by vitamin K antagonist or absence (PIVKA-II) were
measured at least once every one month. An abdominal CT scan or
dynamic magnetic resonance imaging (MRI) was also performed at
least once every 3 months following surgery.
Statistical analysis
Survival curves were constructed using the
Kaplan-Meier method (24).
Survival curves were compared using the log-rank test. The features
of HCC, biochemistry, ICGR-15, and virus status were compared using
the Mann-Whitney test. The level of tumor markers (AFP and
PIVKA-II) was compared by the Wilcoxon matched-pair test.
Statistical significance was interpreted as P<0.05.
Results
Features of the preoperative hepatic
function, hepatocellular carcinoma and surgery
The features of the preoperative hepatic function
are shown in Table I. There was no
significant difference between the IFN/5-FU adjuvant and
non-IFN/5-FU adjuvant groups in terms of the preoperative hepatic
function: serum albumin (g/dl), prothrombin time (PT, %),
hepaplastin test (HPT, %), indocyanine green retention rate at 15
min (ICGR-15, %). No difference was also demonstrated in terms of
tumor stage, surgical procedure, including AFP (ng/ml) and PIVKA-II
(mAU/ml) (Table I).
Clinical effects, disease-free and
overall survival
Concerning the enrolled 50 patients, none developed
any major complications. The 30 IFN/5-FU patients started the
postoperative adjuvant therapy 3–5 weeks after surgery and
completed 3 cycles of treatment. In addition, the QOL of patients
in this study was excellent, as this adjuvant therapy was performed
at outpatient clinics; no hospital admission was necessary. The
patients were able to maintain their social life while receiving
IFN/5-FU adjuvant therapy.
The follow-up period of the present study was from 3
to 109 months (mean 24 months). The difference in follow-up was
significant compared to the prior study (20). Results for the IFN/5-FU adjuvant
treatment group were as follows: disease-free survival (n=9)
(15–109 months), survival with recurrence (n=6) (30–92 months),
cancer death (n=9) (14–60 months), death from other causes but no
recurrence (n=5) (13–87 months) and death from other causes with
recurrence (n=1, 22 months). The summary of these results for each
case is shown in Table IIA.
 | Table IIPrognosis and pathological findings
of the IFN/5-FU and non-IFN/5-FU adjuvant groups. |
Table II
Prognosis and pathological findings
of the IFN/5-FU and non-IFN/5-FU adjuvant groups.
A, IFN/5-FU
adjuvant group (n=30)
|
|---|
| Case | Recurrence | Recurrent site | Disease-free
period | Survival
period | Prognosis | Cause of death | Histology of
cancer | Non-cancer |
|---|
| 1 | - | - | 68 | 68 | Died | HBV, Lz, Liver
failurea | EdIII(por) | B′− |
| 2 | + | Liver | 18 | 60 | Died | Cancer | EdII(mod) |
CAH+ |
| 3 | - | - | 109 | 109 | Alive | - | EdII(mod) | B− |
| 4 | - | - | 87 | 87 | Died | Brain
bleedinga | EdIII(por) |
CAH+ |
| 5 | + | Liver, lung | 40 | 48 | Died | Cancer | EdIII(por) | B′− |
| 6 | + | Liver, lung,
adrenal | 38 | 46 | Died | Cancer | EdIII(por) | B′− |
| 7 | + | Liver, lung | 7 | 18 | Died | Cancer | EdIII(por) | B′− |
| 8 | + | Liver | 8 | 22 | Died | Cardiac
failureb | EdII(mod) | B′− |
| 9 | - | Lung | 28 | 92 | Alive | - | EdIII(por) | B′− |
| 10 | + | Lymph node,
liver | 6 | 24 | Died | Cancer | EdIII(por) | B− |
| 11 | + | Liver | 43 | 75 | Alive | - | EdIII(por) | B′− |
| 12 | - | - | 44 | 44 | Died | Cardiac
failurea | EdIII(por) | B′− |
| 13 | + | Liver | 32 | 73 | Alive | - | EdII(mod) | B− |
| 14 | + | Lung, liver | 8 | 14 | Died | Cancer | EdIII(por) | B′− |
| 15 | - | - | 13 | 13 | Died | Brain
infarctiona | EdII(mod) |
CAH+ |
| 16 | - | - | 18 | 18 | Died | Esophageal
varixa | EdIV(por) | B+ |
| 17 | + | Liver | 9 | 18 | Died | Cancer | EdIII(por) |
chr.glissonitis |
| 18 | + | Liver | 24 | 51 | Alive | - | EdII(mod) | CIH |
| 19 | - | - | 46 | 46 | Alive | - | EdIII(por) |
CAH+ |
| 20 | + | Lung, liver | 8 | 14 | Died | - | EdIII(por) | Liver fibrosis |
| 21 | - | - | 38 | 41 | Alive | - | EdIV(por) | B′− |
| 22 | - | - | 38 | 38 | Alive | - | EdII(mod) | B′+ |
| 23 | - | - | 37 | 37 | Alive | - | EdIII(por) | B′− |
| 24 | - | - | 36 | 36 | Alive | - | EdIII(por) | B′− |
| 25 | - | - | 31 | 31 | Alive | - | EdII(mod) | CIH |
| 26 | - | - | 30 | 30 | Alive | - | EdIII(por) | B− |
| 27 | + | Lymph node | 22 | 30 | Alive | - | EdIII(por) | B′− |
| 28 | - | - | 24 | 24 | Alive | - | EdIII(por) | B− |
| 29 | + | Liver, lung | 10 | 16 | Died | Cancer | EdIII(por) | CIH |
| 30 | - | - | 15 | 15 | Alive | - | EdIII(por) |
CAH+ |
B, The non-IFN/5-FU
adjuvant group (n=20)
|
|---|
| Case | Recurrence | Recurrent site | Disease-free
period | Survival
period | Prognosis | Cause of death | Histology
cancer | Non-cancer |
|---|
| 31 | + | Liver | 50 | 58 | Died | Cancer | EdIII(por) | CAH |
| 32 | + | Liver, lung | 1 | 3 | Died | Cancer | EdIII(por) | B′− |
| 33 | + | Liver | 1 | 5 | Died | Cancer | EdIII(por) | B′− |
| 34 | + | Liver | 12 | 18 | Died | Cancer | EdIII(por) | Unknown |
| 35 | + | Liver | 5 | 5 | Died | Cancer | EdII(mod) |
BA′+ |
| 36 | + | Liver | 42 | 63 | Died | Cancer | EdIII(por) | B+ |
| 37 | + | Liver | 4 | 33 | Died | Cancer | EdIII(por) | B+ |
| 38 | + | Liver | 5 | 10 | Died | Cancer | EdIII(por) |
CIH− |
| 39 | + | Liver | 3 | 5 | Died | Cancer | EdIII(por) | Glissonitis,se |
| 40 | + | Liver | 2 | 4 | Died | Cancer |
EdIV(undifferentiated) | Glissonitis |
| 41 | + | Liver | 1 | 3 | Died | Cancer |
EdIV(undifferentiated) |
Chr.glissonitis |
| 42 | + | Liver | 31 | 58 | Died | Cancer | EdIII(por) | B− |
| 43 | + | Liver, lung, lumph
node | 6 | 6 | Died | Cancer | EdIII(por) |
Chr.glissonitis |
| 44 | + | Liver, lung | 3 | 8 | Died | Cancer | EdIII(por) | CIH |
| 45 | + | Liver | 4 | 7 | Died | Cancer | EdIII(por) | B− |
| 46 | + | Liver | 6 | 9 | Died | Cancer | EdII(mod) |
B′−∼A′++ |
| 47 | + | Liver, lung | 6 | 8 | Died | Cancer | EdIII(por) | CIH |
| 48 | + | Liver, lung | 14 | 25 | Died | Cancer | EdIII(por) | B+ |
| 49 | + | Liver | 6 | 10 | Died | Cancer | EdIII(por) | CIH |
| 50 | + | Liver | 7 | 11 | Died | Cancer | EdIII(por) | B′+ |
In the group that received no adjuvant IFN/5-FU
therapy, 14 of 20 patients died of recurrent cancer within 1 year;
almost all patients (17 of 20) within 3 years. All patients
developed recurrences in the residual liver, 4 also had lung
metastasis, and one had lung and lymph node metastases. Recurrence
was identified within 1 year after hepatic resection in 16 of the
20 patients. These clinical results are summarized in Table IIB.
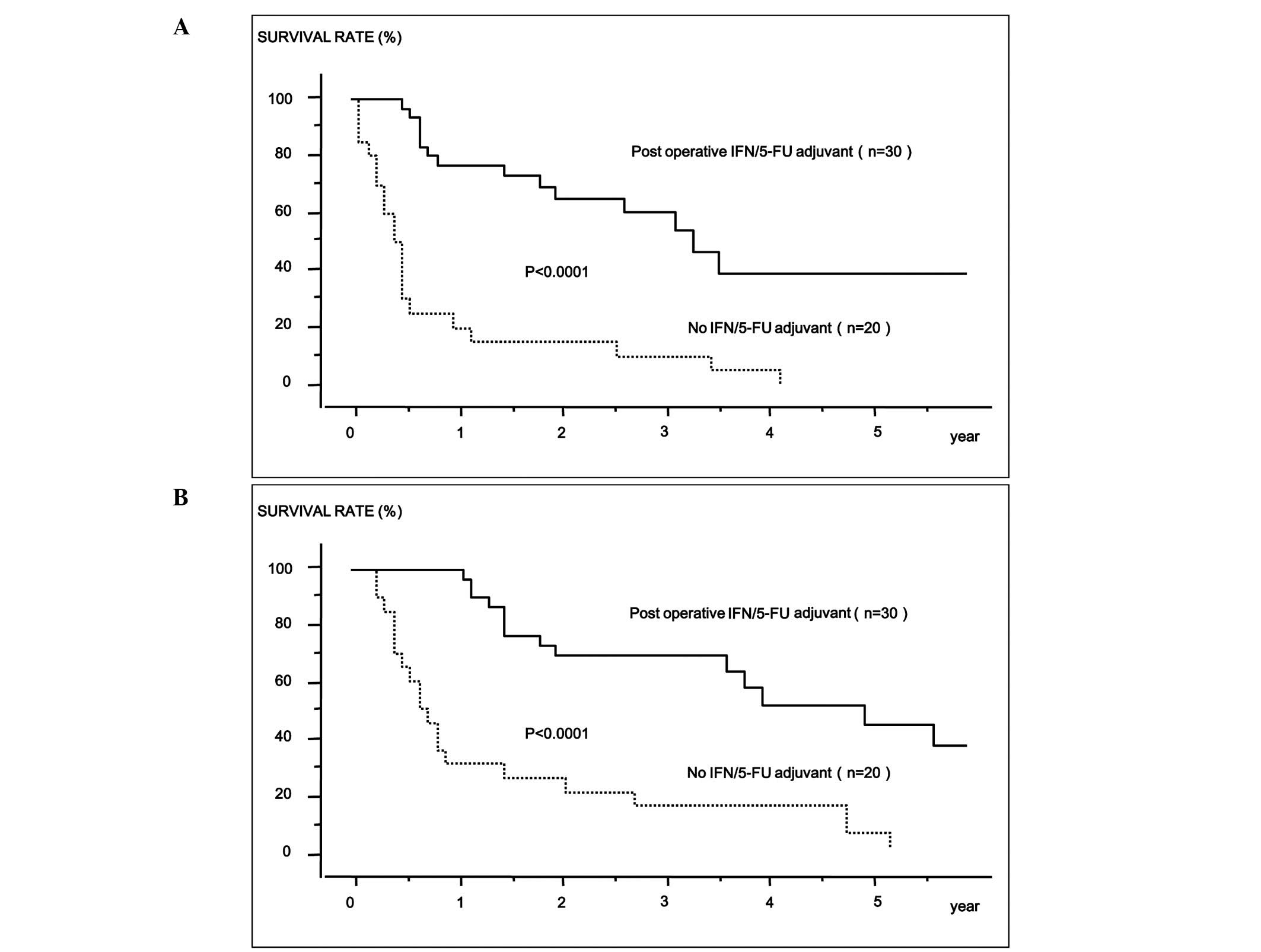
With respect to survival, the 1-, 3- and 5-year
disease-free survival rates were 77, 60 and 39% for patients who
received IFN/5-FU combination therapy (n=30); 20, 10 and 0%,
respectively, for the historical controls (n=20) (Fig. 1A). In addition, the 1-, 3- and
5-year overall survival rates were 100, 69 and 44% for patients who
received IFN/5-FU combination therapy (n=30); 30, 15 and 5% for the
historical controls (n=20) (Fig.
1B). There was a significant difference in disease-free and
overall survival rates between these two groups (disease-free,
P<0.0001; overall, P<0.0001) (Fig. 1).
Adverse effects
No leukopenia, thrombocytopenia, or
myelo-suppression was observed in the 30 patients of the IFN/5-FU
group. Other adverse effects were, in general, clinically
manageable. Fever was commonly observed but was easily controlled
by non-steroidal anti-inflammatory drugs prior to IFN injection. No
depression due to IFN administration was observed in any of the 30
patients.
Discussion
The present study is the extended examination of our
previous report (20) concerning
the clinical outcome of a combination therapy of IFN-α and 5-FU as
a postoperative adjuvant therapy for resectable HCC with PVTT. Our
results showed that this treatment regimen markedly decreased the
incidence of recurrence in the residual liver and significantly
prolonged the disease-free and overall survival periods compared
with historical controls. Amazingly, the 1-year overall survival
rate was 100% in the IFN/5-FU treatment group. This result
concerning the survival benefit for resectable far advanced HCC
with PVTT was much better than the Japan survey for HCC patients
(25).
Development of tumor thrombi in a major branch or
main trunk of the portal vein is a frequent terminal feature of
HCC, either with primary or recurrent tumors. The prognosis of such
patients is extremely poor, and survival is limited to a few months
after diagnosis (26–31). For these advanced HCCs,
conventional therapies like transcatheter arterial embolization
(TAE) and radiofrequency ablation (RFA) are not indicated due to
lack of efficacy and associated complications (30–32).
Liver transplantation is a contra-indication for such far advanced
HCC with PVTT cases (33). To
date, several reports have mentioned the feasibility of hepatic
resection for patients with PVTT, however the outcome is
unsatisfactory (28,29,34,35),
except for limited cases with PVTT located in the segmental or
sectoral branches (36). Based on
this finding, in the absence of effective preoperative and/or
postoperative adjuvant therapy, hepatic resection should not be
offered in cases with PVTT in the main trunk or first branch.
Several approaches have been attempted to improve the surgical
results, including radiotherapy and TAE (37–40).
Compared with these reports, our clinical outcome using IFN/5-FU
combined therapy as a postoperative adjuvant was excellent and
highly satisfactory, in terms of survival and long-term
outcome.
In regards to recurrence, extrahepatic metastases
often occurred following surgery even after IFN/5-FU adjuvant
treatment. The combination of IFN/5-FU is not effective against
extrahepatic metastases. This is understandable as 5-FU,
administered into the hepatic artery, does not reach extrahepatic
tissues at a high concentration. In such a situation, systemic
administration of 5-FU or related agents may be effective against
extrahepatic lesions in combination with IFN-α (41). This possibility is highly
interesting since the implantation of a dwelling catheter is one of
the demerits of the present combination therapy (9–11).
Recently, several molecular-targeting agents have been developed
and applied for HCC treatment (42–44).
Particularly, sorafenib is the first agent leading to improved
overall survival for patients with advanced HCC, as revealed in a
phase III clinical trial (10).
These molecular-targeting agents are a very effective therapeutic
modality, which exhibited a different mechanism of anti-tumor
effect compared to IFN/5-FU combination as an cytotoxic medicine.
Based on this evidence, mutual interaction and shared roles may be
extremely important for the progression of treatment for
intractable advanced HCC. We previously reported that PTK/ZK, a
type of molecular-targeting medicine, enhanced the anti-tumor
effect of IFN/5-FU in vitro(45).
Myelosuppressive adverse effects frequently occur in
patients with HCC. This is not only because thrombocytopenia and/or
leukopenia are often present prior to the initiation of anti-cancer
therapy, but because treatment often has to be discontinued due to
these side effects. Another advantage of our combination therapy
was the markedly low incidence of myelosuppressive side effects; no
patient developed leukopenia in the present study (data not shown).
In addition, the QOL of patients in the present study was
excellent, as IFN/5-FU adjuvant therapy was performed at outpatient
clinics. No hospital admission was necessary for the administration
of the IFN injection combined with the intra-arterial perfusion
chemotherapy. The patients were able to maintain their social life
while receiving IFN/5-FU adjuvant therapy. Moreover, they had no
symptoms related to liver dysfunction.
In conclusion, this study indicated that combination
chemotherapy with subcutaneous IFN-α and intra-arterial 5-FU is a
promising strategy for resectable advanced HCC with PVTT in the
main trunk or first branch, as a postoperative adjuvant therapy
following surgery.
Abbreviations:
|
HCC
|
hepatocellular carcinoma
|
|
IFN
|
interferon
|
|
AFP
|
α-fetoprotein
|
|
PIVKA-II
|
protein induced by vitamin K
antagonist or absence
|
|
PVTT
|
portal vein tumor thrombosis
|
|
5-FU
|
5-fluorouracil
|
|
TAE
|
transcatheter arterial
embolization
|
|
RFA
|
radiofrequency ablation
|
Acknowledgements
This study was supported by a grant in
aid for cancer research from the Ministry of Health and Walfare and
the Ministry of Culture and Science in Japan.
References
|
1
|
Arii S, Monden K, Niwano M, et al: Results
of surgical treatment for recurrent hepatocellular carcinoma;
comparison of outcome among patients with multicentric
carcinogenesis, intrahepatic metastasis, and extrahepatic
recurrence. J Hepatobiliary Pancreat Surg. 5:86–92. 1998.
View Article : Google Scholar
|
|
2
|
Llovet JM, Ricci S, Mazzaferro V, et al:
Sorafenib in advanced hepatocellular carcinoma. N Engl J Med.
359:378–390. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Kudo M and Okanoue T: Management of
hepatocellular carcinoma in Japan: consensus-based clinical
practice manual proposed by the Japan Society of Hepatology.
Oncology. 72(Suppl 1): S2–S15. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Chung YH, Song IH, Song BC, et al:
Combined therapy consisting of intraarterial cisplatin infusion and
systemic interferon-alpha for hepatocellular carcinoma patients
with major portal vein thrombosis or distant metastasis. Cancer.
88:1986–1991. 2000. View Article : Google Scholar
|
|
5
|
Kaneko S, Urabe T and Kobayashi S:
Combination chemotherapy for advanced hepatocellular carcinoma
complicated by major portal vein thrombosis. Oncology. 62(Suppl 1):
S69–S73. 2002. View Article : Google Scholar
|
|
6
|
Patt YZ, Hassan MM, Lozano RD, et al:
Phase II trial of systemic continuous fluorouracil and subcutaneous
recombinant interferon Alfa-2b for treatment of hepatocellular
carcinoma. J Clin Oncol. 21:421–427. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Obi S, Yoshida H, Toune R, et al:
Combination therapy of intra-arterial 5-fluorouracil and systemic
interferon-alpha for advanced hepatocellular carcinoma with portal
venous invasion. Cancer. 106:1990–1997. 2006. View Article : Google Scholar
|
|
8
|
Uka K, Aikata H, Takaki S, et al: Similar
effects of recombinant interferon-alpha-2b and natural
interferon-alpha when combined with intra-arterial 5-fluorouracil
for the treatment of advanced hepatocellular carcinoma. Liver Int.
27:1209–1216. 2007.
|
|
9
|
Sakon M, Nagano H, Dono K, et al: Combined
intraarterial 5-fluorouracil and subcutaneous interferon-α therapy
for advanced hepatocellular carcinoma with tumor thrombi in the
major portal branches. Cancer. 94:435–442. 2002.
|
|
10
|
Ota H, Nagano H, Sakon M, et al: Treatment
of hepatocellular carcinoma with major portal vein thrombosis by
combined therapy with subcutaneous interferon-alpha and
intra-arterial 5-fluorouracil; role of type 1 interferon receptor
expression. Br J Cancer. 93:57–64. 2005.
|
|
11
|
Nagano H, Wada H, Kobayashi S, et al:
Long-term outcome of combined subcutaneous interferon-α and
intra-arterial 5-fluorouracil treatment for advanced hepatocellular
carcinoma with major portal vein thrombosis. Oncology. (In
Press).
|
|
12
|
Eguchi H, Nagano H, Yamamoto H, et al:
Augmentation of antitumor activity of 5-fluorouracil by interferon
alpha is associated with up-regulation of p27Kip1 in human
hepatocellular carcinoma cells. Clin Cancer Res. 6:2881–2890.
2000.
|
|
13
|
Yamamoto T, Nagano H, Sakon M, et al:
Partial contribution of tumor necrosis factor-related
apoptosis-inducing ligand (TRAIL)/TRAIL receptor pathway to
anti-tumor effects of interferon-alpha/5-fluorouracil against
hepatocellular carcinoma. Clin Cancer Res. 10:7884–7895. 2004.
View Article : Google Scholar
|
|
14
|
Kondo M, Nagano H, Wada H, et al:
Combination of IFN-alpha and 5-fluorouracil induces apoptosis
through IFN-alpha/beta receptor in human hepatocellular carcinoma
cells. Clin Cancer Res. 11:1277–1286. 2005.PubMed/NCBI
|
|
15
|
Nakamura M, Nagano H, Sakon M, et al: Role
of the Fas/FasL pathway in combination therapy with
interferon-alpha and fluorouracil against hepatocellular carcinoma
in vitro. J Hepatol. 46:77–88. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Noda T, Nagano H, Takemasa I, et al:
Activation of Wnt/beta-catenin signalling pathway induces
chemoresistance to interferon-alpha/5-fluorouracil combination
therapy for hepatocellular carcinoma. Br J Cancer. 100:1647–1658.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Wada H, Nagano H, Yamamoto H, et al:
Combination of interferon-alpha and 5-fluorouracil inhibits
endothelial cell growth directly and by regulation of angiogenic
factors released by tumor cells. BMC Cancer. 9:361–372. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Tomimaru Y, Eguchi H, Wada H, et al:
Insulin-like growth factor-binding protein 7 alters the aensitivity
to interferon-based anticancer therapy in hepatocellular carcinoma
cells. Br J Cancer. 102:1483–1490. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Tomimaru Y, Eguchi H, Nagano H, et al:
MicroRNA-21 induces resistance to the anti-tumor effect of
interferon-α/5-fluorouracil in hepatocellular carcinoma cells. Br J
Cancer. 103:1617–1626. 2010.PubMed/NCBI
|
|
20
|
Nagano H, Sakon M, Eguchi H, et al:
Hepatic resection followed by IFN-alpha and 5-FU for advanced
hepatocellular carcinoma with tumor thrombus in the major portal
branch. Hepatogastroenterology. 54:172–179. 2007.PubMed/NCBI
|
|
21
|
Nagano H, Miyamoto A, Wada H, et al:
Interferon-α and 5-fluorouracil combination therapy following
palliative hepatic resection in patients with advanced
hepatocellular carcinoma, portal venous tumor thrombus in the major
trunk and multiple nodules. Cancer. 110:2493–2501. 2007.
|
|
22
|
The General Rules for the Clinical and
Pathological Study of Primary Liver Cancer. 5th edition. Liver
Cancer Study Group of Japan; 2008
|
|
23
|
Oken MM, Creech RH, Tormey DC, et al:
Toxicity and response criteria of the Eastern Cooperative Oncology
Group. Am J Clin Oncol. 5:649–655. 1982. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Kaplan EL and Meier P: Nonparametric
estimation from incomplete observations. J Am Stat Assoc.
53:457–481. 1958. View Article : Google Scholar
|
|
25
|
Ikai I, Arii S, Ichida T, et al: Report of
the 16th follow-up survey of primary liver cancer. The Liver Cancer
Study Group of Japan Hepatol Res. 32:163–172. 2005.PubMed/NCBI
|
|
26
|
Yamakado K, Tanaka N, Nakatsuka A, et al:
Clinical efficacy of portal vein stent placement in patients with
hepatocellular carcinoma invading the main portal vein. J Hepatol.
30:660–668. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Cancer of the Liver Italian Program (CLIP)
investigators: A new prognostic system for hepatocellular
carcinoma: a retrospective study of 435 patients. Hepatology.
28:751–755. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Asahara T, Itamoto T, Katayama K, et al:
Hepatic resection with tumor thrombectomy for hepatocellular
carcinoma with tumor thrombi in the major vasculature.
Hepatogastroenterology. 46:1862–1869. 1999.PubMed/NCBI
|
|
29
|
Ohkubo T, Yamamoto J, Sugawara Y, et al:
Surgical results for hepatocellular carcinoma with macroscopic
portal vein thrombosis. J Am Coll Surg. 191:657–660. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Furuse J, Iwasaki M, Yoshino M, et al:
Hepatocellular carcinoma with portal vein tumor thrombus:
embolization of arterioportal shunts. Radiology. 204:787–790. 1997.
View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Lee HS, Kim JS, Choi IJ, et al: The safety
and efficacy of trans-catheter arterial chemoembolization in the
treatment of patients with hepatocellular carcinoma and main portal
vein obstruction: a prospective controlled study. Cancer.
79:2087–2094. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Poon RT, Ng KK, Lam CM, et al: Learning
curve for radio-frequency ablation of liver tumors: prospective
analysis of initial 100 patients in a tertiary institution. Ann
Surg. 239:441–449. 2004.PubMed/NCBI
|
|
33
|
Mazzaferro V, Regalia E, Doci R, et al:
Liver transplantation for the treatment of small hepatocellular
carcinomas in patients with cirrhosis. N Engl J Med. 334:693–700.
1996. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Poon RT, Fan ST, Ng IO and Wong J:
Prognosis after hepatic resection for stage IVA hepatocellular
carcinoma: a need for reclassification. Ann Surg. 237:376–383.
2003. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Ikai I, Yamaoka Y, Yamamoto Y, et al:
Surgical intervention for patients with stage IV-A hepatocellular
carcinoma without lymph node metastasis proposal as a standard
therapy. Ann Surg. 227:433–439. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Shi J, Lai ECH, Li N, et al: Surgical
treatment for hepatocellular carcinoma with portal vein tumor
thrombus. Ann Surg Oncol. 17:2073–2080. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Tazawa J, Maeda M, Sakai Y, et al:
Radiation therapy in combination with transcatheter arterial
chemoembolization for hepatocellular carcinoma with extensive
portal vein involvement. J Gastroenterol Hepatol. 16:660–665. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Ishikura S, Ogino T, Furuse J, et al:
Radiotherapy after transcatheter arterial chemoembolization for
patients with hepatocellular carcinoma and portal vein tumor
thrombus. Am J Clin Oncol. 25:189–193. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Minagawa M, Makuuchi M, Takayama T and
Ohtomo K: Selection criteria for hepatectomy in patients with
hepatocellular carcinoma and portal vein tumor thrombus. Ann Surg.
233:379–384. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Peng BG, He Q, Li JP and Zhou F: Adjuvant
transcatheter arterial chemoembolization improves efficacy of
hepatectomy for patients with hepatocellular carcinoma and portal
vein tumor thrombus. Am J Surg. 198:313–318. 2009. View Article : Google Scholar
|
|
41
|
Nakamura M, Nagano H, Marubashi S, et al:
A pilot study of combination chemotherapy of S-1, a novel oral DPD
inhibitor, and interferon-alpha for advanced hepatocellular
carcinoma with extrahepatic metastasis. Cancer. 112:1765–1771.
2008. View Article : Google Scholar
|
|
42
|
Llovet JM and Bruix J: Molecular targeted
therapies in hepatocellular carcinoma. Hepatology. 48:1312–1327.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Yang ZF, Poon RT, Liu Y, et al: High doses
of tyrosine kinase inhibitor PTK787 enhance the efficacy of
ischemic hypoxia for the treatment of hepatocellular carcinoma:
dual effects on cancer cell and angiogenesis. Mol Cancer Ther.
5:2261–2270. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
44
|
Zhu AX, Sahani DV, Duda DG, et al:
Efficacy, safety, and potential biomarkers of sunitinib monotherapy
in advanced hepatocellular carcinoma: a phase II study. J Clin
Oncol. 27:3027–3035. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
45
|
Murakami M, Kobayashi S, Marubashi S, et
al: Tyrosine kinase inhibitor PTK/ZK enhances the anti-tumor
effects of interferon-α/5-fluorouracil therapy for hepatocellular
carcinoma cells. Ann Surg Oncol. 18:589–596. 2011.PubMed/NCBI
|