Introduction
Epilepsy is a chronic brain dysfunction syndrome
caused by highly synchronous abnormal discharge of neurons in the
brain (1). This common disorder in
clinical neurology has sudden onset. Patients with epilepsy, mainly
the elderly or children, are often accompanied by varying degrees
of transient disturbance of consciousness, and patients with more
severe epilepsy may have a general convulsion (2). It has been reported that (3) there are 50 patients diagnosed with
epilepsy in 100,000 people in North America each year. Another
study shows that (4) more than half
of the 50 million patients with epilepsy in the world are in Asia.
Childhood is a critical period for the development of human brain
function, and the long-term abnormal discharge in the brain has a
very adverse effect on the development of the brain function
(5). The treatment of epilepsy in
children needs to completely control the onset of the disease and
eliminate the cause, as well as ensure the learning and daily
living ability of children as much as possible. Therefore, how to
actively and effectively treat children with epilepsy has become
one of the problems that clinicians need to solve now.
New anti-epileptic drugs have emerged, bringing new
hope for the treatment of epilepsy. The main component of
levetiracetam (LEV) is a derivative of pyrrolidone. By binding to
SV2A in the brain, synaptic vesicle protein 2A, LEV effectively
inhibits the high-voltage-activated N-type Ca ion channel in the
vertebral neurons of the hippocampus CA1 region, and thereby plays
an anti-epileptic role (6). By
improving the activity of glutamic acid decarboxylase, sodium
valproate (SV) as a conventional therapeutic drug for epilepsy
promotes the synthesis of γ-aminobutyric acid in the brain,
inhibits γ-aminobutyrate transaminase and prevents the degradation
of γ-aminobutyric acid, thereby improving the epileptic symptoms in
patients (7).
MicroRNA (miR), a hot research topic in recent
years, is a small (19–22 nucleotides) non-coding single-stranded
RNA molecule. It causes the translational inhibition of target mRNA
or the cleavage of mRNA by regulating gene expression (8). Studies in recent years have shown that
miR is differentially expressed in tumor, cardiovascular and
nervous system diseases (9–11). In the study by Sun et al
(12), the expression of miR-106b is
significantly increased in the serum of adult patients with
epilepsy. However, there is no study showing the expression of
miR-106b in pediatric epilepsy. Whether it can be a potential
prognostic indicator has not been reported previously.
Therefore, the efficacy of LEV combined with SV in
the treatment of pediatric epilepsy was analyzed in this study, and
whether miR-106b could be used as a potential prognostic indicator
for the treatment of children with epilepsy was also analyzed, in
order to provide a reference for clinicians.
Patients and methods
A total of 120 children with epilepsy treated in
Xuzhou Children's Hospital (Xuzhou, China) from July 2015 to July
2017 were enrolled, and divided into the control group (n=60) and
the observation group (n=60) according to random sampling. The
control group consisted of 31 males and 29 females, and the
observation group consisted of 35 males and 25 females.
Additionally, 100 children undergoing normal physical examination
were collected as the normal group for this study.
This study was approved by the Ethics Committee of
Xuzhou Children's Hospital, Xuzhou Medical University. Patients who
participated in this research had complete clinical data. The
family members of the children were informed of this study and
signed an informed consent form.
Inclusion and exclusion criteria
Inclusion criteria: All children met the diagnostic
criteria for pediatric epilepsy developed by The Basic and Clinical
Aspects of Pediatric Neurological Diseases (13). Children had normal blood routine
indicators, coagulation function and liver and kidney function.
Exclusion criteria: Children with a history of
encephalitis, brain trauma and meningitis; children with
immunodeficiency; children complicated with other malignant tumors;
children treated with anti-epileptic drugs 1 month before
enrollment; children with abnormalities in CT and MRI detection and
children with an allergy to therapeutic drugs or a corresponding
contraindication.
Drugs and source of kits
SV (Hangzhou Sanofi Pharmaceutical Co., Ltd., SFDA
approval number: H20010595), LEV (UCB Pharma S.A., approval number:
H20160251), TransScript miRNA first-strand cDNA synthesis superMix
and easypure miRNA kit (TransGen Biotech, AT351-01, ER601-01), PCR
instrument (Applied Biosystems; Thermo Fisher Scientific, Inc.,
7500). The primers were designed and synthesized by Sangon Biotech
(Shanghai) Co., Ltd.
Treatment programs
Patients in the control group were treated with SV,
and the specific treatment was as follows: the initial dose was
5–10 mg/(kg × day). If epilepsy was not controlled 1 week after
medication, the dose would be added with 5–10 mg/(kg × day) per
week based on the initial dose, until the seizure did not occur
[the maximum dose was controlled at 30–40 mg/(kg × day)].
Patients in the observation group were treated with
LEV and SV, and the specific treatment was as follows: the initial
dose was 10 mg/(kg × day), which was added once a week. The target
dose was controlled at 20–60 mg/(kg × day) on the 3rd to 4th week,
the daily dose was divided into 2 doses.
RT-qPCR detection
Venous blood (5 ml) was collected from the child in
the morning, allowed to stand at room temperature for 15–30 min,
and centrifuged at 3,000 × g for 10 min at 4°C. Serum was collected
and centrifuged at 10,080 × g for 10 min using an ultra-speed
centrifuge at 4°C to remove the cell debris. A portion of the serum
was taken for subsequent experiments, and the rest was stored at
−80°C. The EasyPure miRNA kit was used for the extraction of total
RNA from the serum, UV spectrophotometer and agarose gel
electrophoresis for detecting the purity, concentration and
integrity of the total RNA extracted, TransScript® miRNA
RT Enzyme mix and 2X TS miRNA reaction mix (belonging to the PCR
kit) for the reverse transcription of cDNA. The reverse
transcription was carried out in strict accordance with the
instructions, and cDNA was taken for subsequent experiments. PCR
system was as follows: 1 µl of cDNA, each of 0.4 µl of upstream and
downstream primers, 10 µl of 2X TransStart® Top/Tip
green qPCR supermix, passive reference dye (50X) (optional), and
finally nuclease-free water supplemented to 20 µl. A two-step
method was used for detection. PCR reaction conditions were:
pre-denaturation at 94°C for 30 sec, denaturation at 94°C for 5
sec, annealing and extension at 60°C for 30 sec, for a total of 40
cycles. U6 was used as an internal reference gene in this
experiment, and 2−ΔCq was used to express the relative
expression of miR-106b. The primer sequences are shown in Table I (14).
 | Table I.Primer sequences. |
Table I.
Primer sequences.
| Genes | Upstream primer | Downstream
primer |
|---|
| miR-106b |
5′-TGCCTCCTCATTGTCTTCA-3′ |
5′-GCCATCTCAAATACCTCCC-3′ |
| U6 |
5′-CTCGCTTCGGCAGCACA-3′ |
5′-AACGCTTCACGAATTTGCGT-3′ |
Outcome measures
Main outcome measures: The clinical efficacy in the
children was evaluated according to The Diagnosis and Curing
Criteria of Clinical Diseases in 2002 (Table II). The difference in the expression
of serum miR-106b was observed in children in the control group and
the observation group before treatment and subjects in the normal
group. The relative expression of serum miR-106b in children was
observed before and 12 weeks after treatment, and that of serum
miR-106b in children with different efficacy was observed.
 | Table II.Clinical efficacy grading. |
Table II.
Clinical efficacy grading.
| Efficacy grade | Performance |
|---|
| Cured | No epileptic seizure
in children |
| Markedly
effective | No epileptic seizure
or seizure frequency reduced by >75% |
| Effective | Seizure frequency
reduced by 25–75% |
| Invalid | Seizure frequency
reduced by <25%, or no significant reduction, or increase in
seizure |
Secondary outcome measures: The clinical data of
children in the groups were observed. The ROC curve was plotted
according to the expression of serum miR-106b in control,
observation and normal group. The incidence of adverse drug
reaction (ADR) was compared between the two groups.
Statistical analysis
In this study, SPSS20.0 software package was used
for the statistical analysis of the data, GraphPad Prism 7 for
plotting the figures. Count data were expressed as rate (%), tested
by Chi-square and denoted by χ2. Measurement data were
expressed as mean ± standard deviation (means ± SD). Independent
sample t-test was used for comparison between the groups, paired
t-test for comparison in the group before and after treatment and
denoted by t. Grade data were tested by rank sum test and denoted
by Z. Analysis of variance was used for comparison between multiple
groups, LSD t-test for pairwise comparison in the group. The ROC
curve was plotted according to the expression of serum miR-106b in
the control, the observation and the normal group. The Spearman's
test was used to analyze the relationship between the expression of
miR-106b and the clinical efficacy. P<0.05 was considered to
indicate a statistically significant difference.
Results
Clinical data of children
The clinical data of children in the three groups
were analyzed. There were no statistically significant differences
in sex, age, BMI and place of residence between the three groups
(P>0.05). The children in the control group and the observation
group were compared. In the control group, the average course of
disease was 1.25 years and the seizure frequency was 2.48
times/year; there were 23 children with simple partial seizure, 11
children with complex partial seizure, 10 children with
tonic-clonic seizure, 7 children with tonic seizure and 9 children
with Lennox-Gastaut syndrome. In the observation group, the average
course of disease was 1.28 years and the seizure frequency was 2.52
times/year; there were 25 children with simple partial seizure, 9
children with complex partial seizure, 11 children with
tonic-clonic seizure, 9 children with tonic seizure and 6 children
with Lennox-Gastaut syndrome. There were no statistically
significant differences in other data between the two groups
(P>0.05) (Table III).
 | Table III.Clinical data of children. |
Table III.
Clinical data of children.
| Factor | Control group
(n=60) | Observation group
(n=60) | Normal group
(n=100) | t/χ2/F
value | P-value |
|---|
| Sex |
| Male | 31 (51.67) | 35 (58.33) | 58 (58.00) | 0.742 | 0.690 |
|
Female | 29 (48.33) | 25 (41.67) | 42 (42.00) |
|
|
| Age (years) |
7.2±1.8 |
7.5±1.9 |
7.0±1.5 | 1.624 | 0.200 |
| BMI
(kg/m2) | 15.12±1.25 | 14.82±1.42 | 14.98±1.62 | 0.623 | 0.537 |
| Average course of
disease (years) |
1.25±0.35 |
1.28±0.29 |
| 0.511 | 0.610 |
| Seizure frequency
(times/years) |
2.48±1.22 |
2.52±1.35 |
| 0.170 | 0.865 |
| Epileptic seizure
type |
| Simple
partial seizure | 23 (38.33) | 25 (41.67) |
| 1.110 | 0.893 |
| Complex
partial seizure | 11 (18.33) | 9
(15.00) |
|
|
|
|
Tonic-clonic seizure | 10 (16.67) | 11 (18.33) |
|
|
|
| Tonic
seizure | 7
(11.67) | 9
(15.00) |
|
|
|
|
Lennox-Gastaut syndrome | 9
(15.00) | 6
(10.00) |
|
|
|
| Place of
residence |
|
Urban | 35 (58.33) | 30 (50.00) | 58 (58.00) | 1.170 | 0.557 |
|
Rural | 25 (41.67) | 30 (50.00) | 42 (42.00) |
|
|
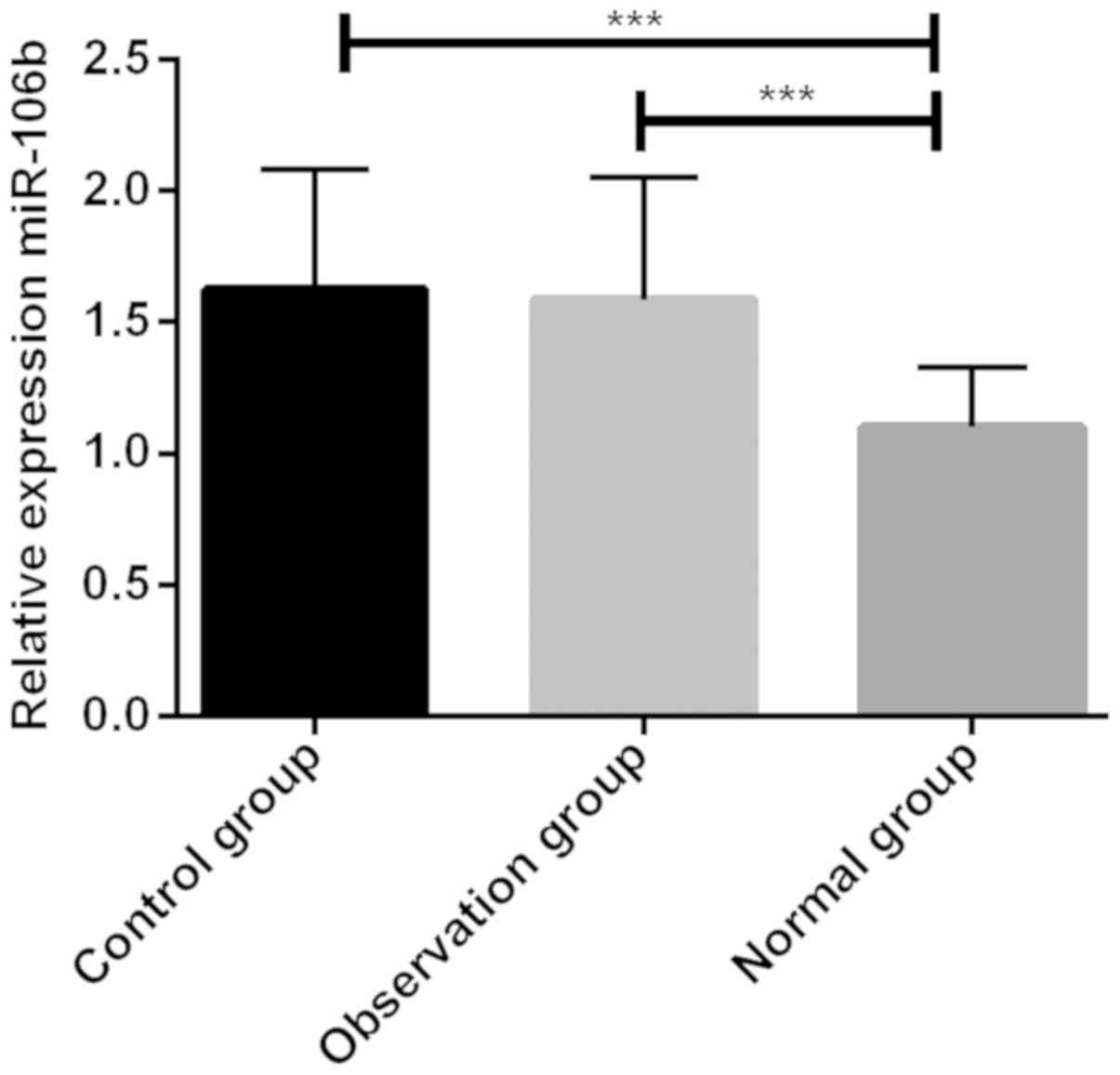
Relative expression of serum miR-106b
in three groups of children
The expression of serum miR-106b in children before
treatment was detected. Before treatment, the expression of serum
miR-106b in the control group and the observation group was
significantly higher than that in the normal group, with a
significant difference (P<0.05); there was no statistically
significant difference between the control group and the
observation group (P>0.05) (Fig.
1). The expression of serum miR-106b in the two groups after
treatment was significantly lower than that before treatment
(P<0.05); after treatment, the relative expression of serum
miR-106b in the control group was significantly higher than that in
the observation group, with a statistically significant difference
(P<0.05). The difference of miR-106b during the treatment was
compared. The difference in the control group was smaller than that
in the observation group, with a statistically significant
difference (P<0.05) (Tables IV
and V).
 | Table IV.Relative expression of miR-106b in
two groups of children before and after treatment. |
Table IV.
Relative expression of miR-106b in
two groups of children before and after treatment.
|
| Relative expression
of miR-106b |
|
|
|---|
|
|
|
|
|
|---|
| Group | Before
treatment | After
treatment | t value | P-value |
|---|
| Control group
(n=60) | 1.627±0.456 | 1.454±0.302 |
7.508 | <0.001 |
| Observation group
(n=60) | 1.586±0.466 | 1.244±0.256 | 12.205 | <0.001 |
| t value | 0.487 | 4.109 |
|
|
| P-value | 0.627 | <0.001 |
|
|
 | Table V.Comparison of difference in relative
expression of miR-106b between the two groups before and after
treatment. |
Table V.
Comparison of difference in relative
expression of miR-106b between the two groups before and after
treatment.
| Score | Control group
(n=110) | Observation group
(n=110) | t value | P-value |
|---|
| Difference in
relative expression of miR-106b | 0.172±0.128 | 0.342±0.217 | 5.227 | <0.001 |
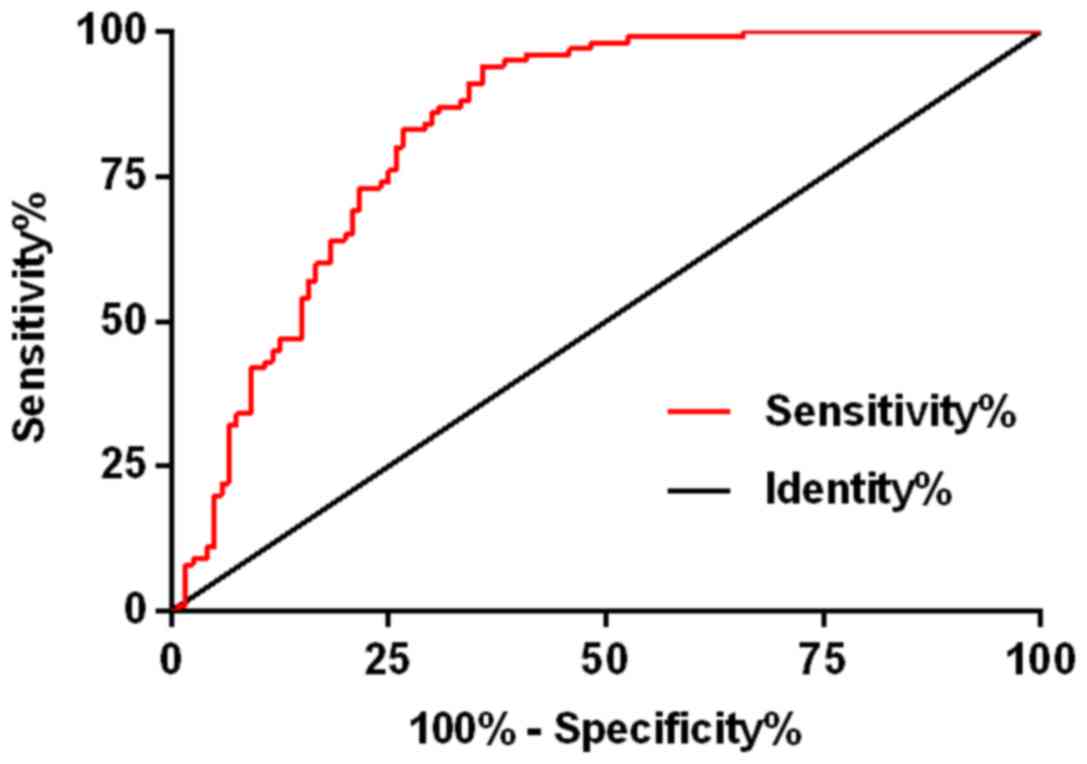
Diagnostic value of miR-106b in
children with epilepsy
The serum miR-106b before treatment was detected in
healthy children and in children with epilepsy. The area under
curve (AUC) of miR-106b was 0.833, 95% CI: 0.779 to 0.887 the
cut-off: 1.442. The sensitivity, the specificity and the Youden
index were 94.00, 64.17, and 58.17%, respectively (Fig. 2).
Relationship between clinical efficacy
and miR-106b in two groups of children
The clinical efficacy in the two groups of children
was compared. In the control group, there were 8 children cured, 20
children with marked effect, 18 children with effect and 14
children with invalidity. In the observation group, there were 15
children cured, 27 children with marked effect, 10 children with
effect and 8 children with invalidity. The results of comparison
showed that the clinical efficacy in the observation group was
significantly better than that in the control group, with a
statistically significant difference (P<0.05) (Table VI). The relationship between
miR-106b and different clinical efficacy was analyzed. Spearman
test showed that the expression of miR-106b gradually decreased
with the continuous improvement of the clinical efficacy
(P<0.05) (Table VII).
 | Table VI.Clinical efficacy in two groups of
children. |
Table VI.
Clinical efficacy in two groups of
children.
| Groups | Cured | Markedly
effective | Effective | Invalid | Z value | P-value |
|---|
| Control (n=60) | 8
(13.33) | 20 (33.33) | 18 (30.00) | 14 (23.33) | −2.525 | 0.012 |
| Observation
(n=60) | 15 (25.00) | 27 (45.00) | 10 (16.67) | 8
(13.33) |
|
|
 | Table VII.Relationship between clinical
efficacy and miR-106b. |
Table VII.
Relationship between clinical
efficacy and miR-106b.
| Efficacy grade | n | Relative expression
of miR-106b | r value | P-value |
|---|
| Cured | 23 | 1.124±0.394 |
|
|
| Markedly
effective | 47 | 1.319±0.284 | 0.784 | <0.001 |
| Effective | 28 | 1.239±0.298 |
|
|
| Invalid | 22 | 1.658±0.207 |
|
|
ADR statistics
According to the ADR statistics, in the control
group, there were 3 children with nausea, 4 children with vomiting,
2 children with hypersomnia, 5 children with anorexia, 3 children
with dizziness and 3 children with liver function damage. In the
observation group, there were 2 children with nausea, 3 children
with vomiting, 2 children with hypersomnia, 3 children with
anorexia, 2 children with dizziness and 2 children with liver
function damage. The results of comparison showed that there was no
statistically significant difference in the ADR between the two
groups (P>0.05) (Table
VIII).
 | Table VIII.ADR statistics. |
Table VIII.
ADR statistics.
| Groups | Nausea | Vomiting | Hypersomnia | Anorexia | Dizziness | Liver function
damage |
|---|
| Control (n=60) | 3 (5.00) | 4 (6.67) | 2 (3.33) | 5 (8.33) | 3 (5.00) | 3 (5.00) |
| Observation
(n=60) | 2 (3.33) | 3 (5.00) | 2 (3.33) | 3 (5.00) | 2 (3.33) | 2 (3.33) |
| χ2
value | 0.209 | 0.152 | 0 | 0.536 | 0.209 | 0.209 |
| P-value | 0.648 | 0.697 | 1 | 0.464 | 0.648 | 0.648 |
Discussion
Epilepsy is a common syndrome in neurology (15). It has been reported that
approximately 9 million people are affected by epilepsy in China,
the population of which is mainly children and the elderly
(16,17). Compared with the elderly, the child's
brain is at the developmental stage. Recurrent and transient tonic
and clonic seizures for a long time easily cause hypoxia in the
brain. Without timely intervention, the neurons of the child are
damaged as the disease progresses, seriously affecting the
intelligence and the daily life of the child. Therefore, the
treatment of pediatric epilepsy is increasingly valued (18).
In this study, LEV and SV were used to treat
children with epilepsy, and their clinical efficacy was observed.
SV is the most commonly used broad-spectrum antiepileptic drug for
the clinical treatment of epilepsy in clinical practice (19). Although the drug is effective, it is
metabolized by the liver and may cause liver function damage in
children. Besides, the anti-epileptic treatment process is long and
prone to various adverse reactions, which increases the treatment
pain and reduces the treatment compliance of the child, resulting
in unsatisfactory expected effect (20). Guo et al (21), reported that the long-term use of SV
has a serious impact on growth and osteopenia in children with
epilepsy. LEV is a new broad-spectrum antiepileptic drug for the
treatment of epilepsy (22). There
is a study showing that it has a lower effect on liver enzymes and
creatine kinase in children (23).
The clinical efficacy in the two groups of children after treatment
was first observed. The improvement of the disease condition in the
observation group was significantly better than that in the control
group. In the study by Tan and Appleton (24), 26 children with epilepsy aged under
10 years were treated with LEV alone, and 61% of them had a good
response to LEV, with the seizure frequency reduced by at least
50%. In addition, 2 children with refractory epilepsy had no
seizure after medication. In this study, the effective rate of LEV
combined with SV for the treatment of children was 93.64%, and the
efficacy was significantly better than that of single medication.
This suggests that the combined medication can effectively improve
the condition of the child. Then, the adverse events during the
treatment were compared between the two groups. There was no
difference in the ADR between the two groups. This suggests that
LEV and SV have good efficacy in the treatment of children with
epilepsy, and have small adverse reactions.
miR-106b is an important member of the miR-17 family
and differentially expressed in tumor and cardiovascular diseases
(25,26). According to Cava et al
(27), highly expressed in the serum
of patients with epilepsy, miR-106b is expected to become a new
diagnostic indicator. However, there is no relevant research on
whether it can be a prognostic indicator in the treatment of
epilepsy. Therefore, in this study, whether miR-106b can be used as
a prognostic indicator in the treatment of children with epilepsy
was investigated. The expression of serum miR-106b in children with
epilepsy was first detected. The expression of serum miR-106b in
the control group and the observation group was significantly
higher than that in the normal group, consistent with the results
of Pitkänen et al (28).
Subsequently, the ROC curve was plotted. In the study by An et
al (29), the AUC of miR-106b
was 0.786, 95% CI: 0.693–0.824, while the AUC was 0.882, 95% CI:
0.839–0.926 in the study by Wang et al (30), consistent with the results of this
study. In the present study, the AUC of miR-106b was 0.833, 95% CI:
0.779–0.887. These findings suggest that miR-106b can be used as a
potential diagnostic indicator for children with epilepsy. Finally,
the correlation analysis between the clinical efficacy and the
expression of miR-106b in children was performed. The expression of
miR-106b in children after treatment gradually decreased with the
improvement of the disease, suggesting that miR-106b is expected to
be a potential prognostic indicator for children with epilepsy
after treatment.
This study showed the clinical efficacy of LEV
combined with SV in children with epilepsy. The combination of the
two drugs effectively improves the condition of the child, and does
not increase the clinical ADR. The expression of serum miR-106b in
children was detected. miR-106b was highly expressed in children
with epilepsy. The expression of serum miR-106b in children can be
used as a prognostic indicator. However, there are still
limitations in this study. First, the children were not followed up
for a long time, and the specific improvement of them remains
unclear. Secondly, the specific mechanism of LEV combined with SV
on improving of the expression of miR-106b in children needs
further investigation.
In summary, LEV combined with SV is effective in the
treatment of children with epilepsy, and does not increase the
clinical ADR. The expression of serum miR-106b in children can be
used as a clinical prognostic indicator and a potential diagnostic
indicator.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the present
study are available from the corresponding author on reasonable
request.
Authors' contributions
JZ wrote the manuscript. JZ and YS were responsible
for PCR. YZ and DZ assisted with the clinical efficacy analysis. JC
and XL were responsible for the statistical analysis. All the
authors read and approved the final manuscript.
Ethics approval and consent to
participate
The study was approved by the Ethics Committee of
Xuzhou Children's Hospital, Xuzhou Medical University (Xuzhou,
China). Patients who participated in this research, had complete
clinical data. The family members of the children were informed of
this study and signed an informed consent form.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Berg AT and Scheffer IE: New concepts in
classification of the epilepsies: Entering the 21st century.
Epilepsia. 52:1058–1062. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Russ SA, Larson K and Halfon N: A national
profile of childhood epilepsy and seizure disorder. Pediatrics.
129:256–264. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Theodore WH, Spencer SS, Wiebe S, Langfitt
JT, Ali A, Shafer PO, Berg AT and Vickrey BG: Epilepsy in North
America: A report prepared under the auspices of the global
campaign against epilepsy, the International Bureau for Epilepsy,
the International League Against Epilepsy, and the World Health
Organization. Epilepsia. 47:1700–1722. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Mac TL, Tran DS, Quet F, Odermatt P, Preux
PM and Tan CT: Epidemiology, aetiology, and clinical management of
epilepsy in Asia: A systematic review. Lancet Neurol. 6:533–543.
2007. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Glennon JM, Weiss-Croft L, Harrison S,
Cross JH, Boyd SG and Baldeweg T: Interictal epileptiform
discharges have an independent association with cognitive
impairment in children with lesional epilepsy. Epilepsia.
57:1436–1442. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Belcastro V, Costa C, Galletti F, Autuori
A, Pierguidi L, Pisani F, Calabresi P and Parnetti L: Levetiracetam
in newly diagnosed late-onset post-stroke seizures: A prospective
observational study. Epilepsy Res. 82:223–226. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Chen L, Feng P, Wang J, Liu L and Zhou D:
Intravenous sodium valproate in mainland China for the treatment of
diazepam refractory convulsive status epilepticus. J Clin Neurosci.
16:524–526. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Ha M and Kim VN: Regulation of microRNA
biogenesis. Nat Rev Mol Cell Biol. 15:509–524. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Condorelli G, Latronico MV and Cavarretta
E: microRNAs in cardiovascular diseases: Current knowledge and the
road ahead. J Am Coll Cardiol. 63:2177–2187. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Lin S and Gregory RI: MicroRNA biogenesis
pathways in cancer. Nat Rev Cancer. 15:321–333. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Sun Y, Luo ZM, Guo XM, Su DF and Liu X: An
updated role of microRNA-124 in central nervous system disorders: A
review. Front Cell Neurosci. 9:1932015. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Sun J, Cheng W, Liu L, Tao S, Xia Z, Qi L
and Huang M: Identification of serum miRNAs differentially
expressed in human epilepsy at seizure onset and post-seizure. Mol
Med Rep. 14:5318–5324. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Healy F and Panitch HB: Pulmonary
complications of pediatric neurological diseases. Pediatr Ann.
39:216–224. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Livak KJ and Schmittgen TD: Analysis of
relative geneexpression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Fisher RS, Acevedo C, Arzimanoglou A,
Bogacz A, Cross JH, Elger CE, Engel J Jr, Forsgren L, French JA,
Glynn M, et al: ILAE official report: A practical clinical
definition of epilepsy. Epilepsia. 55:475–482. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Singh A and Trevick S: The epidemiology of
global epilepsy. Neurol Clin. 34:837–847. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Ollenberger GP, Byrne AJ, Berlangieri SU,
Rowe CC, Pathmaraj K, Reutens DC, Berkovic SF, Scheffer IE and
Scott AM: Assessment of the role of FDG PET in the diagnosis and
management of children with refractory epilepsy. Eur J Nucl Med Mol
Imaging. 32:1311–1316. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Lagunju IA, Oyinlade AO and Babatunde OD:
Seizure-related injuries in children and adolescents with epilepsy.
Epilepsy Behav. 54:131–134. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Stephen LJ, Kwan P, Shapiro D, Dominiczak
M and Brodie MJ: Hormone profiles in young adults with epilepsy
treated with sodium valproate or lamotrigine monotherapy.
Epilepsia. 42:1002–1006. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Fisher K, Vuppalanchi R and Saxena R:
Drug-induced liver injury. Arch Pathol Lab Med. 139:876–887. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Guo CY, Ronen GM and Atkinson SA:
Long-term valproate and lamotrigine treatment may be a marker for
reduced growth and bone mass in children with epilepsy. Epilepsia.
42:1141–1147. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Weijenberg A, Brouwer OF and Callenbach
PM: Levetiracetam monotherapy in children with epilepsy: A
systematic review. CNS Drugs. 29:371–382. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Attilakos A, Dinopoulos A, Paschalidou M,
Tsirouda M, Prasouli A, Siafakas N and Garoufi A: Effect of
levetiracetam monotherapy on liver enzymes and creatine kinase
concentrations in children with epilepsy: A prospective study. J
Clin Neurol. 14:594–595. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Tan MJ and Appleton RE: Efficacy and
tolerability of levetiracetam in children aged 10 years and
younger: A clinical experience. Seizure. 13:142–145. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Moshiri F, Salvi A, Gramantieri L,
Sangiovanni A, Guerriero P, De Petro G, Bassi C, Lupini L, Sattari
A, Cheung D, et al: Circulating miR-106b-3p, miR-101-3p and
miR-1246 as diagnostic biomarkers of hepatocellular carcinoma.
Oncotarget. 9:15350–15364. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Wronska A, Kurkowska-Jastrzebska I and
Santulli G: Application of microRNAs in diagnosis and treatment of
cardiovascular disease. Acta Physiol (Oxf). 213:60–83. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Cava C, Manna I, Gambardella A, Bertoli G
and Castiglioni I: Potential role of miRNAs as theranostic
biomarkers of epilepsy. Mol Ther Nucleic Acids. 13:275–290. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Pitkänen A, Löscher W, Vezzani A, Becker
AJ, Simonato M, Lukasiuk K, Gröhn O, Bankstahl JP, Friedman A,
Aronica E, et al: Advances in the development of biomarkers for
epilepsy. Lancet Neurol. 15:843–856. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
An N, Zhao W, Liu Y, Yang X and Chen P:
Elevated serum miR-106b and miR-146a in patients with focal and
generalized epilepsy. Epilepsy Res. 127:311–316. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Wang J, Yu JT, Tan L, Tian Y, Ma J, Tan
CC, Wang HF, Liu Y, Tan MS, Jiang T, et al: Genome-wide circulating
microRNA expression profiling indicates biomarkers for epilepsy.
Sci Rep. 5:95222015. View Article : Google Scholar : PubMed/NCBI
|