Introduction
Apatinib, a small-molecule tyrosine kinase inhibitor
(TKI), selectively binds to and inhibits vascular endothelial
growth factor receptor-2 (VEGFR-2) (1). This consequently inhibits
VEGF-stimulated endothelial cell migration and proliferation, and
decreases microvascular tumor density (1). Certain pre-clinical and clinical data
have utilized apatinib in the treatment of solid tumors, which has
led to the approval of the drug as a second-line treatment for
patients with advanced gastric tumors in China in 2014(2).
Additionally, apatinib has undergone Phase II/III
clinical trials for non-small-cell lung cancer, esophageal cancer,
hepatocellular carcinoma and breast cancer in China (3-7)
The most common side effects of apatinib are
hypertension, gastrointestinal distress, skin toxicity, fatigue and
elevated transaminases (8). However,
to the best of our knowledge, no studies have examined
hypothyroidism induced by apatinib. Hypothyroidism can lead to
severe consequences if left untreated, including fatigue,
intolerance to cold, acroparesthesia, dryness of the skin and hair,
weight gain, constipation, hoarseness of the voice, typical facial
appearance and prolonged relaxation phase of the tendon reflexes
(9). Therefore, appropriate
monitoring and treatment recommendations in patients receiving
apatinib are critical.
The primary objective of the current study was to
assess the number of patients who accepted thyroid replacement
therapy after commencing treatment with apatinib. The secondary
objective was to investigate thyroid ultrastructure remodeling. To
summarize, the current study evaluated the incidence and severity
of clinically actionable hypothyroidism induced by apatinib.
Materials and methods
Patient selection and therapy
A total of 149 patients with pathologically
diagnosed solid tumors who were treated with apatinib from February
2015 to January 2016 in Shandong Provincial Qianfoshan Hospital
were recruited for the current study. All cases were diagnosed as
stage IIIC or IV and had no standard alternative curative therapy.
Additional eligibility criteria included: Age between 18 and 70
years, no history of other cancers, an Eastern Cooperative Oncology
Group performance status (10)
between 0-3 and a life expectancy of >3 months. Exclusion
criteria was the presence of thyroid disease, other than thyroid
cancer.
At baseline, all patients underwent a computed
tomography scan or magnetic resonance imaging, a thyroid ultrasound
and blood tests. All study subjects had normal hematological,
thyroid, hepatic, renal and cardiac functions prior to treatment
(counts of leukocytes, erythrocytes and thrombocytes; levels of
triiodothyronine, tetraiodothyronine, thyroid stimulating hormone,
lactic dehydrogenase and brain natriuretic peptide; and rates of
alanine transaminase, aspartate aminotransferase and creatinine
clearance were assessed). All these parameters were normal in each
patient.
Evaluation and method
All patients received 500 mg apatinib/day (Jiangsu
Heng Rui Medicine Co., Ltd.) orally until the disease progressed,
except for 3 patients who were administered a dose of 250 mg/day
due to hypertension. Dose reductions occurred often due to
toxicity, as such the doses of 11 patients were reduced to 250
mg/day.
Levels of triiodothyronine (T3; normal range,
3.1-6.8 pmol/l), tetraiodothyronine (T4; normal range, 12-22
pmol/l) and thyroid stimulating hormone (TSH; 0.27-4.2 µIU/ml) were
evaluated monthly. These parameters were evaluated using Elecsys
FT3 III, FT4 III and TSH and Cobase E analyzers supplied by Roche
Diagnostics GmbH. Lower levels of T3 and T4 were <3.1 and 12
pmol/l, respectively. Higher levels of TSH were >4.2 µIU/ml.
Additionally, patients underwent a thyroid
ultrasound every 2 months while receiving apatinib treatment. Their
thyroid function and thyroid ultrastructure was evaluated for at
least 24 months or until death. All patients divided into the
normal thyroid function group (96 cases) and the hypothyroidism
group (53 cases) according to their levels of T3, T4 and TSH.
Efficacy measures included complete response(CR), partial response
(PR), stable disease (SD) and disease control rate (DCR; including
complete response, partial response and sTable disease).
Statistical differences in DCR between the two groups were
analyzed.
Statistical analysis
Statistical analysis of the data was performed using
SPSS (version 18.0; SPSS, Inc.). All quantitative data are
presented as mean ± SD of three independent repeats. Pearson
χ2 test was used for the comparison of parameters.
P<0.05 was considered to indicate a statistically significant
difference. The current study was granted access to information
that could identify individual participants during data collection
through the health information system at Shandong Provincial
Qianfoshan Hospital.
Results
Demographics
The demographic characteristics of 149 patients with
solid tumors are presented in Table
I: Apatinib was administered to patients with gastric, hepatic,
colorectal, pancreatic, lung, breast, ovarian and kidney cancer, as
well as soft tissue sarcoma. A total of 21 cases were diagnosed at
stage IIIc and 128 cases at stage IV.
 | Table IDemographic characteristics of 149
patients with solid tumors. |
Table I
Demographic characteristics of 149
patients with solid tumors.
| Characteristic | Number of cases
(%) |
|---|
| Age (years) | |
|
<65 | 99 (66.44) |
|
≥65 | 50 (33.56) |
| Sex | |
|
Male | 64 (42.95) |
|
Female | 85 (57.05) |
| Primary tumor
site | |
|
Gastric | 54 (36.24) |
|
Hepatic | 13 (8.72) |
|
Colorectal | 12 (8.05) |
|
Pancreatic | 3 (2.01) |
|
Lung | 17 (11.41) |
|
Breast | 16 (10.74) |
|
Ovarian | 18 (12.08) |
|
Kidney | 13 (8.72) |
|
Soft tissue
sarcoma | 3 (2.01) |
| Stage | |
|
IIIc | 21 (14.09) |
|
IV | 128 (85.91) |
| ECOG performance
status | |
|
0-1 | 12 (8.05) |
|
2 | 71 (47.65) |
|
3 | 66 (44.30) |
| Prior therapy | |
|
Chemotherapy | 76 |
|
Radiotherapy | 32 |
|
Surgery | 97 |
|
Tyrosine
kinase inhibitors | 32 |
| Total | 149 |
Toxicity and tolerability
The most frequently observed drug-related adverse
events (AEs) were hypertension, hand-foot syndrome, hypothyroidism,
elevated transaminases, diarrhea, albinism, rash, anorexia, mucosal
ulcers, fatigue and proteinuria. In the current study, only
drug-related hypothyroidism AEs, including hypothyroidism,
ultrastructural changes and fatigue are discussed. A total of 53
(35.57%) patients had hypothyroidism (Table II), which varied from alterations in
THS with normal T3 and T4 (12 cases; 8.05%) to higher TSH with
lower T3 and T4 (41 cases; 27.52%). Thyroid nodules were found in
15 cases (10.07%). A total of 3 cases (2.01%) had thyroid imaging
reporting and data system for ultrasonography scores (11) of 4a/4b/4c and 12 cases (8.05%) had
scores of 1, 2 and 3. Another drug-related AE was fatigue (16.78%;
25 cases of grade 1-2; and 1.34%; 2 cases of grade 3-4).
 | Table IISummary of adverse events in 53
patients with hypothyroidism. |
Table II
Summary of adverse events in 53
patients with hypothyroidism.
| Adverse event | Number of cases
(%) |
|---|
| Hypothyroidism | 53 (35.57) |
|
Normal T3,
T4 and higher TSH | 12 (8.05) |
|
Lower T3, T4
and higher TSH | 41 (27.50) |
| Ultrastructural
changes | 15 (10.07) |
|
Ti-RADs
1/2/3 | 12 (8.05) |
|
Ti-RADs
4a/4b/4c | 3 (2.01) |
| Fatigue | 27 (18.12) |
|
1-2
grades | 25 (16.78) |
|
3-4
grades | 2 (1.34) |
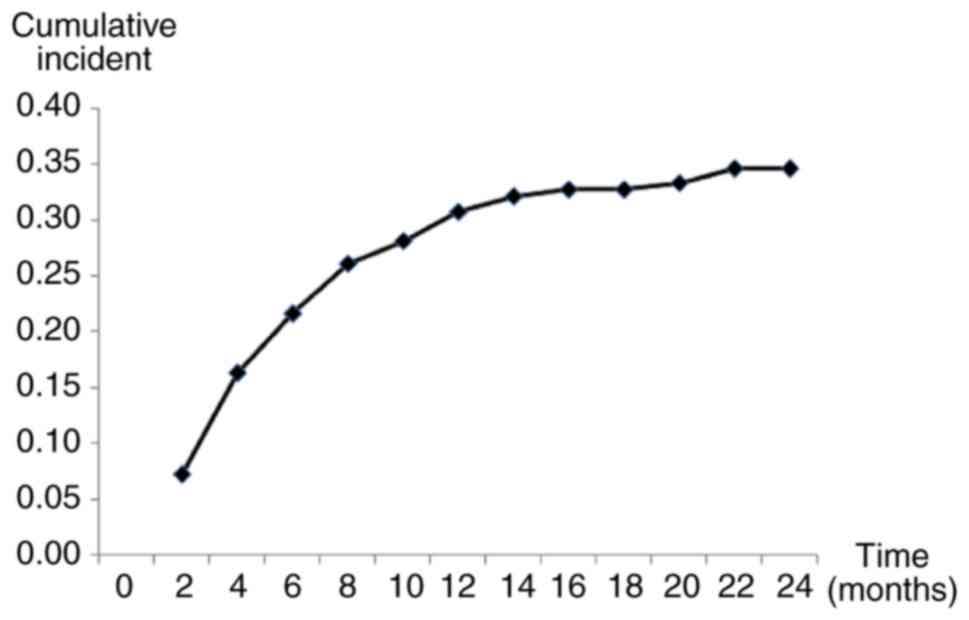
The incidence of hypothyroidism increased gradually
as apatinib treatment duration increased (28.1% at 12 months and
34.6% at 24 months; Fig. 1).
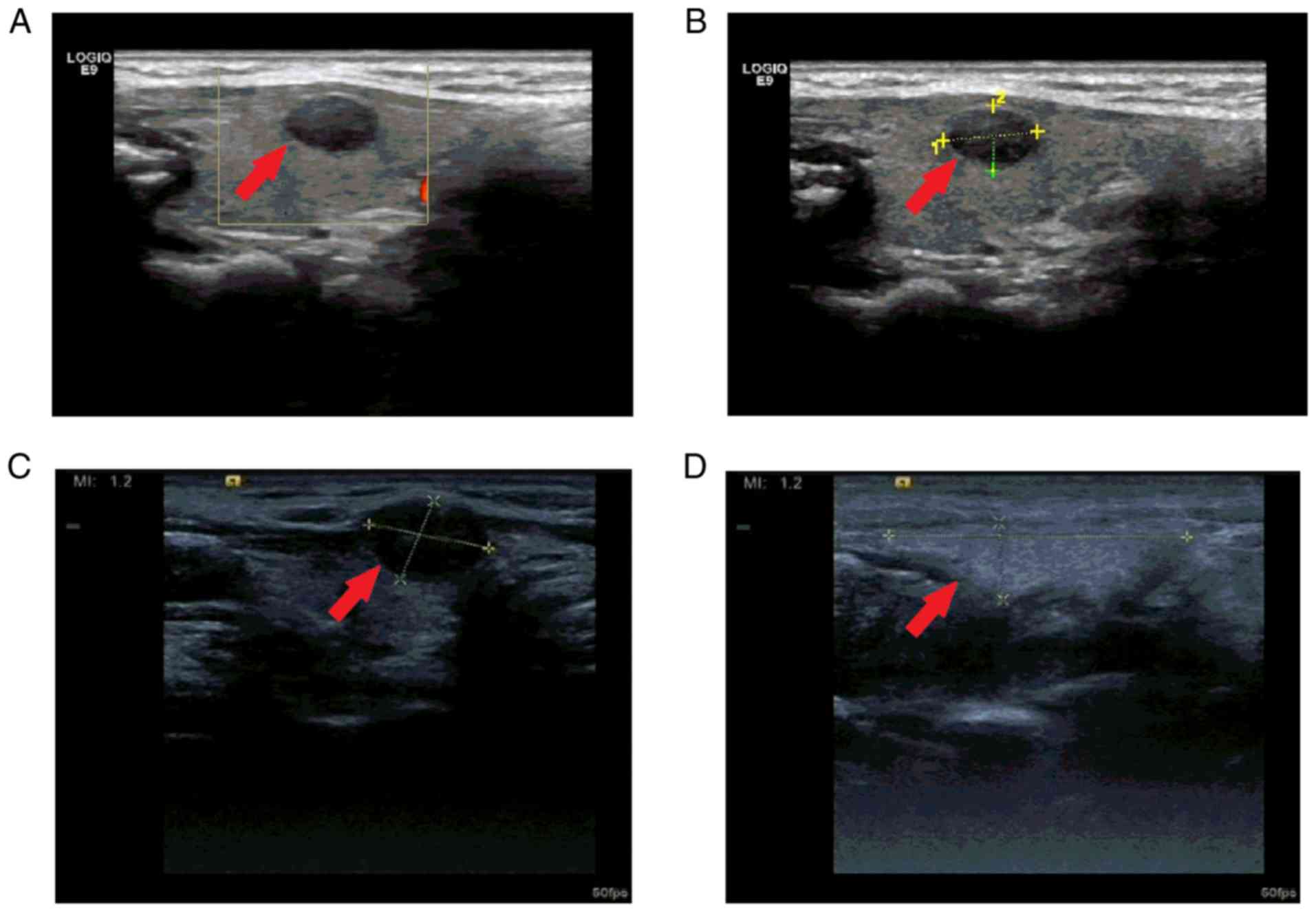
Additionally, 2 cases of ultrastructural changes in the thyroid
gland were reported. However, normal thyroid function was noted in
both cases. Apatinib treatment of 1 year shrunk the thyroid gland
in a patient who had a 9.0x6.0 mm nodule in the right lobe of the
thyroid gland prior to apatinib treatment. The nodule increased to
10.0x8.0 mm after treatment (Fig.
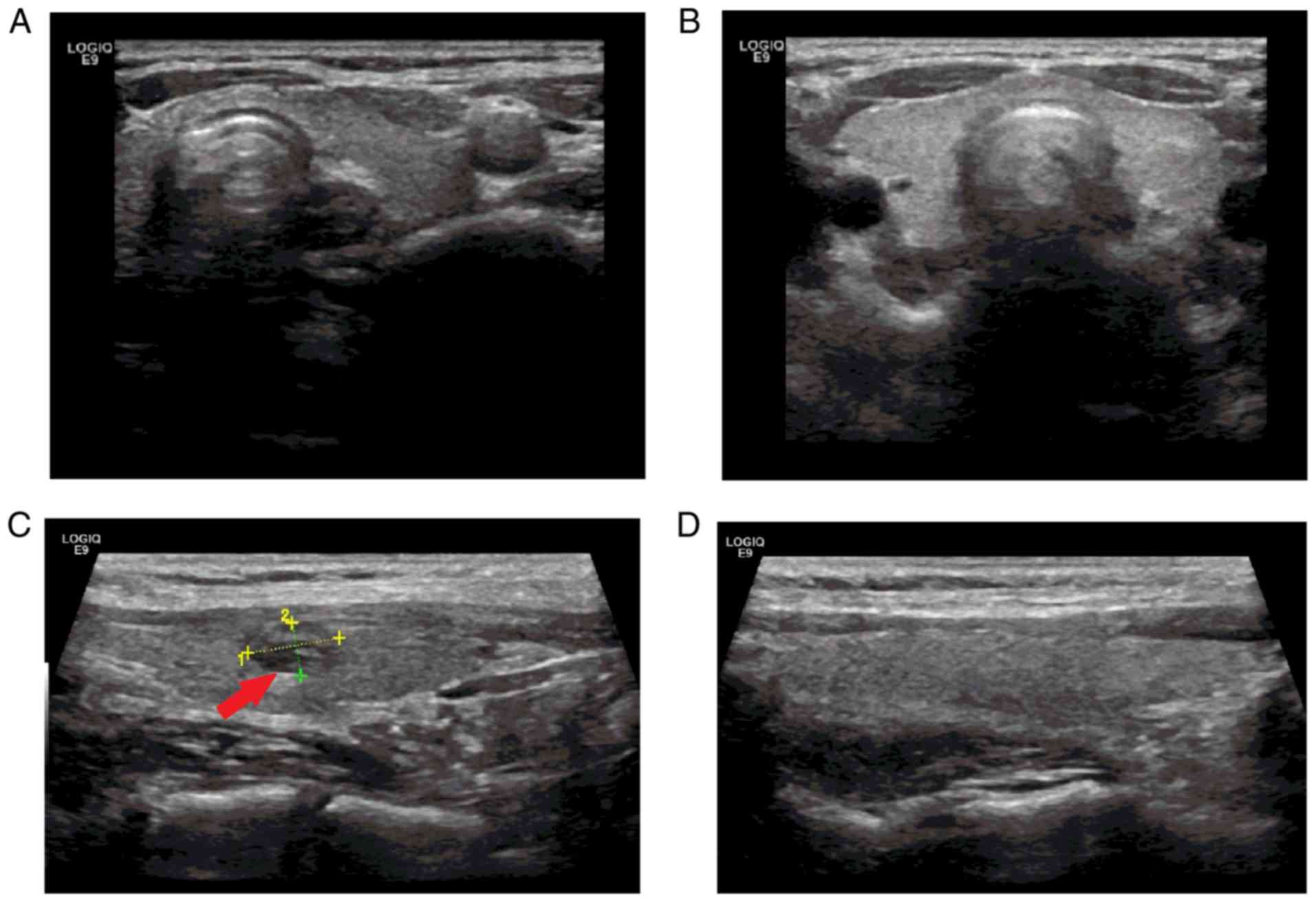
2). Furthermore, after 9 months of apatinib treatment, thyroid
ultrasound revealed two new nodules (3.5x2.0 and 8.4x4.9 mm) in a
second patient who had normal thyroid function prior to treatment
(Fig. 3).
DCR and hypothyroidism
A total of 6 patients attained PR and 28 attained SD
in the normal thyroid function group. In the hypothyroidism group,
2 patients attained PR and 19 attained SD. No significant
difference was noted (P=0.61; Table
III).
 | Table IIIDCR and hypothyroidism. |
Table III
DCR and hypothyroidism.
| Group (no. of
patients) | PR | SD | DCR | P-value |
|---|
| Normal thyroid
function (96) | 6 | 28 | 54 | 0.61 |
| Hypothyroidism
(53) | 2 | 19 | 39.6 | |
Discussion
Since determining the role of VEGF and VEGFR in
carcinogenesis (12,13), therapeutic strategies against these
targets have been widely studied (13-16).
Oral TKIs that inhibit VEGFR (sorafenib, sunitinib, axitinib,
cediranib and pazopanib) have since been elucidated and have been
reported to have similar mechanisms of action and toxicities
(13-16).
The antitumor activity of sorafenib and sunitinib is
mediated through the inhibition of VEGFRs, platelet-derived growth
factor receptor and stem cell factor receptor (17,18).
This inhibition results in apoptotic and antiangiogenic effects.
Sorafenib has been approved for treatment in advanced
hepatocellular carcinoma, metastatic renal cell carcinoma and
radioiodine refractory differentiated thyroid carcinoma (19-21).
Furthermore, sorafenib has also been approved for treatment in
advanced renal cell carcinoma, imatinib-resistant/-intolerant
gastrointestinal stromal tumors and also for certain patients with
progressive, well-differentiated pancreatic neuroendocrine tumors.
Sorafenib and sunitinib are relatively well-tolerated (22,23).
Apatinib has a binding affinity that is 10x higher
than that of sorafenib (24).
Sorafenib and sunitinib were previously demonstrated to cause
hypothyroidism in 6.3-27% and 10-85% of cases, respectively
(25-31).
The severity of hypothyroidism is hypothesized to be associated
with the dose and duration of sorafenib and sunitinib treatment
(26). Certain proposed molecular
mechanisms have been hypothesized for TKI-induced hypothyroidism,
including inhibition of radioactive iodine uptake by the thyroid
gland (32), inhibition of VEGFR
and/or platelet-derived growth factor receptor (25) and via an autoimmune mechanism of
thyroid gland damage, which is supported by the observation of
lymphocytic thyroiditis among certain patients receiving the drug
(33). Lack of treatment can
decrease patients' quality of life (34).
Currently, few studies have assessed the association
between apatinib and thyroid dysfunction. The current study
observed apatinib-related hypothyroidism in numerous patients with
solid tumors. The incidence was similar to the reported incidence
of sorafenib and sunitinib-related hypothyroidism (25-31).
The results of current study indicated that clinicians should
monitor thyroid functions in patients that receive apatinib.
Furthermore, timely supplementation of thyroxine may improve
patient's tolerance and quality of life.
In conclusion, the present study reported data of
the incidence of clinically actionable AEs. Appropriate management
of hypothyroidism may improve the tolerability of apatinib, patient
quality of life and overall survival. However, the present study
had limitations. A statistical significance between the effect of
apatinib and thyroid dysfunction was not established and the
mechanism of apatinib-induced thyroid dysfunction was not assessed.
In future reports, a cohort study concerning the presence of
anti-angiogenesis-related hypothyroidism as a potential biomarker
of antitumor efficacy in patients with metastatic cancer receiving
apatinib should be conducted, followed by a relevant mechanism
study to supplement these limitations.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the present
study are available from the corresponding author on reasonable
request.
Authors' contributions
JX, JL and YL analyzed and interpreted the patient
data regarding hematological and imaging examinations. JX and YL
wrote the manuscript. WZ performed thyroid ultrasound examinations.
All authors read and approved the final manuscript.
Ethics approval and consent to
participate
The current study was designed in accordance with
the legal requirements and principles of the Declaration of
Helsinki and was approved by the Medical Ethics Committee of
Qianfoshan Hospital, affiliated to Shandong University. Written
informed consent was obtained from all patients prior to commencing
the clinical trial.
Patient consent for publication
Written informed consent for publication of any
associated data and accompanying images were obtained from all
patients or their parents, guardians or next of kin.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Scott AJ, Messersmith WA and Jimeno A:
Apatinib: A promising oral antiangiogenic agent in the treatment of
multiple solid tumors. Drugs Today (Barc). 51:223–229.
2015.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Li J, Qin S, Xu J, Guo W, Xiong J, Bai Y,
Sun G, Yang Y, Wang L, Xu N, et al: Apatinib for
chemotherapy-refractory advanced metastatic gastric cancer: Results
from a randomized, placebo-controlled, parallel-arm, phase II
trial. J Clin Oncol. 31:3219–3225. 2013.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Wu F, Zhang S, Xiong A, Gao G, Li W, Cai
W, Su C, Chen X, Zhou F, Zhao J, et al: A phase II clinical trial
of apatinib in pretreated advanced non-squamous non-small-cell lung
cancer. Clin Lung Cancer. 19:e831–e842. 2018.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Li J, Qin S, Xu J, Xiong J, Wu C, Bai Y,
Liu W, Tong J, Liu Y, Xu R, et al: Randomized, double-blind,
placebo-controlled phase III trial of apatinib in patients with
chemotherapy-refractory advanced or metastatic adenocarcinoma of
the stomach or gastroesophageal junction. J Clin Oncol.
34:1448–1454. 2016.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Lu W, Jin XL, Yang C, Du P, Jiang FQ, Ma
JP, Yang J, Xie P and Zhang Z: Comparison of efficacy between TACE
combined with apatinib and TACE alone in the treatment of
intermediate and advanced hepatocellular carcinoma: A single-center
randomized controlled trial. Cancer Biol Ther. 18:433–438.
2017.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Hu X, Zhang J, Xu B, Jiang Z, Ragaz J,
Tong Z, Zhang Q, Wang X, Feng J, Pang D, et al: Multicenter phase
II study of apatinib, a novel VEGFR inhibitor in heavily pretreated
patients with metastatic triple negative breast cancer. Int J
Cancer. 135:1961–1969. 2014.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Hu X, Cao J, Hu W, Wu C, Pan Y, Cai L,
Tong Z, Wang S, Li J, Wang Z, et al: Multicenter phase II study of
apatinib in non-triple-negative metastatic breast cancer. BMC
Cancer. 14(820)2014.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Zhang Y, Han C, Li J, Zhang L, Wang L, Ye
S, Hu Y and Bai L: Efficacy and safety for Apatinib treatment in
advanced gastric cancer: A real world study. Sci Rep.
7(13208)2017.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Evered D and Hall R: Hypothyroidism. Br
Med J. 1:290–293. 1972.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Oken MM, Creech RH, Tormey DC, Horton J,
Davis TE, McFadden ET and Carbone PP: Toxicity and response
criteria of the Eastern cooperative oncology group. Am J Clin
Oncol. 5:649–655. 1982.PubMed/NCBI
|
|
11
|
Park VY, Kim EK, Kwak JY, Yoon JH, Kim MJ
and Moon HJ: Thyroid imaging reporting and data system and
ultrasound elastography: Diagnostic accuracy as a tool in
recommending repeat fine-needle aspiration for solid thyroid
nodules with non-diagnostic fine-needle aspiration cytology.
Ultrasound Med Biol. 42:399–406. 2016.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Chatterjee S, Heukamp LC, Siobal M,
Schottle J, Wieczorek C, Peifer M, Frasca D, Koker M, König K,
Meder L, et al: Tumor VEGF: VEGFR2 autocrine feed-forward loop
triggers angiogenesis in lung cancer. J Clin Invest. 123:1732–1740.
2013.PubMed/NCBI View
Article : Google Scholar
|
|
13
|
Zhang Q, Yu C, Peng S, Xu H, Wright E,
Zhang X, Huo X, Cheng E, Pham TH, Asanuma K, et al: Autocrine VEGF
signaling promotes proliferation of neoplastic Barrett's epithelial
cells through a PLC-dependent pathway. Gastroenterology.
146:461–472 e6. 2014.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Oudard S, Beuselinck B, Decoene J and
Albers P: Sunitinib for the treatment of metastatic renal cell
carcinoma. Cancer Treat Rev. 37:178–184. 2011.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Abdel-Rahman O: Systemic therapy for
hepatocellular carcinoma (HCC): From bench to bedside. J Egypt Natl
Canc Inst. 25:165–171. 2013.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Lin ZZ, Chen BB, Hung YP, Huang PH, Shen
YC, Shao YY, Hsu CH, Cheng AL, Lee RC, Chao Y and Hsu C: A
multicenter phase II study of second-line axitinib for patients
with advanced hepatocellular carcinoma failing first-line sorafenib
monotherapy. Oncologist 2020 (Epub ahead of print).
|
|
17
|
Clark JW, Eder JP, Ryan D, Lathia C and
Lenz HJ: Safety and pharmacokinetics of the dual action Raf kinase
and vascular endothelial growth factor receptor inhibitor, BAY
43-9006, in patients with advanced, refractory solid tumors. Clin
Cancer Res. 11:5472–5480. 2005.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Mendel DB, Laird AD, Xin X, Louie SG,
Christensen JG, Li G, Schreck RE, Abrams TJ, Ngai TJ, Lee LB, et
al: In vivo antitumor activity of SU11248, a novel tyrosine kinase
inhibitor targeting vascular endothelial growth factor and
platelet-derived growth factor receptors: Determination of a
pharmacokinetic/pharmacodynamic relationship. Clin Cancer Res.
9:327–337. 2003.PubMed/NCBI
|
|
19
|
Rovesti G, Orsi G, Faloppi L, Gramantieri
L, Silvestris N, Marisi G, Foschi F, Tamburini E, Andrikou K,
Molinaro E, et al: Sorafenib in patients with hepatocellular
carcinoma: 10 years of real life. Ann Oncol. 30 (Suppl
4)(S57)2019.
|
|
20
|
Flaherty KT, Manola JB, Pins M, McDermott
DF, Atkins MB, Dutcher JJ, George DJ, Margolin KA and DiPaola RS:
BEST: A randomized phase II study of vascular endothelial growth
factor, RAF kinase, and mammalian target of rapamycin combination
targeted therapy with bevacizumab, sorafenib, and temsirolimus in
advanced renal cell carcinoma-a trial of the ECOG-ACRIN cancer
research group (E2804). J Clin Oncol. 33:2384–2391. 2015.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Worden F, Fassnacht M, Shi Y, Hadjieva T,
Bonichon F, Gao M, Fugazzola L, Ando Y, Hasegawa Y, Park DJ, et al:
Safety and tolerability of sorafenib in patients with
radioiodine-refractory thyroid cancer. Endocr Relat Cancer.
22:877–887. 2015.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Thorn CF, Sharma MR, Altman RB and Klein
TE: PharmGKB summary: Pazopanib pathway, pharmacokinetics.
Pharmacogenet Genomics. 27:307–312. 2017.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Doherty KR, Wappel RL, Talbert DR, Trusk
PB, Moran DM, Kramer JW, Brown AM, Shell SA and Bacus S:
Multi-parameter in vitro toxicity testing of crizotinib, sunitinib,
erlotinib, and nilotinib in human cardiomyocytes. Toxicol Appl
Pharmacol. 272:245–255. 2013.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Tian S, Quan H, Xie C, Guo H, Lue F, Xu Y,
Li J and Lou L: YN968D1 is a novel and selective inhibitor of
vascular endothelial growth factor receptor-2 tyrosine kinase with
potent activity in vitro and in vivo. Cancer Sci. 102:1374–1380.
2011.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Mannavola D, Coco P, Vannucchi G,
Bertuelli R, Carletto M, Casali PG, Beck-Peccoz P and Fugazzola L:
A novel tyrosine-kinase selective inhibitor, sunitinib, induces
transient hypothyroidism by blocking iodine uptake. J Clin
Endocrinol Metab. 92:3531–3534. 2007.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Rini BI, Tamaskar I, Shaheen P, Salas R,
Garcia J, Wood L, Reddy S, Dreicer R and Bukowski RM:
Hypothyroidism in patients with metastatic renal cell carcinoma
treated with sunitinib. J Natl Cancer Inst. 99:81–83.
2007.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Wong E, Rosen LS, Mulay M, VanVugt A,
Dinolfo M, Tomoda C, Sugawara M and Hershman JM: Sunitinib induces
hypothyroidism in advanced cancer patients and may inhibit thyroid
peroxidase activity. Thyroid. 17:351–355. 2007.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Tamaskar I, Bukowski R, Elson P,
Ioachimescu AG, Wood L, Dreicer R, Mekhail T, Garcia J and Rini BI:
Thyroid function test abnormalities in patients with metastatic
renal cell carcinoma treated with sorafenib. Ann Oncol. 19:265–268.
2008.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Wolter P, Stefan C, Decallonne B, Dumez H,
Bex M, Carmeliet P and Schöffski P: The clinical implications of
sunitinib-induced hypothyroidism: A prospective evaluation. Br J
Cancer. 99:448–454. 2008.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Clemons J, Gao D, Naam M, Breaker K,
Garfield D and Flaig TW: Thyroid dysfunction in patients treated
with sunitinib or sorafenib. Clin Genitourin Cancer. 10:225–231.
2012.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Feldt S, Schussel K, Quinzler R, Franzmann
A, Czeche S, Ludwig WD and Schulz M: Incidence of thyroid hormone
therapy in patients treated with sunitinib or sorafenib: A cohort
study. Eur J Cancer. 48:974–981. 2012.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Baffert F, Le T, Sennino B, Thurston G,
Kuo CJ, Hu-Lowe D and McDonald DM: Cellular changes in normal blood
capillaries undergoing regression after inhibition of VEGF
signaling. Am J Physiol Heart Circ Physiol. 290:H547–H559.
2006.PubMed/NCBI View Article : Google Scholar
|
|
33
|
Alexandrescu DT, Popoveniuc G, Farzanmehr
H, Dasanu CA, Dawson N and Wartofsky L: Sunitinib-associated
lymphocytic thyroiditis without circulating antithyroid antibodies.
Thyroid. 18:809–812. 2008.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Walko CM, Aubert RE, La-Beck NM, Clore G,
Herrera V, Kourlas H, Epstein RS and McLeod HL:
Pharmacoepidemiology of clinically relevant hypothyroidism and
hypertension from sunitinib and sorafenib. Oncologist. 22:208–212.
2017.PubMed/NCBI View Article : Google Scholar
|