Introduction
Endobronchial lipomas are a rare benign tumors
accounting for only 0.1% of all lung neoplasms (1). They are classified into lipoma,
variants of lipoma, heterotopic lipomas, hamartomatous lesions,
infiltrating or diffuse neoplastic or non-neoplastic proliferations
of mature fat and hibernoma (2).
Angiolipoma is a variant of lipoma accounting for 5–17% of all
lipomas and predominantly presents in young adults as subcutaneous
nodules, which are tender or painful on palpation, particularly
during the initial growth period (1–4).
Angiolipoma, however, arising in the bronchus, is extremely rare.
To the best of our knowledge, only one such case has been reported
to date, which was confined to the bronchus intermedius (5). The present study describes a rare case
of a 74-year-old man with a yellowish round mass incidentally
discovered at the orifice of the right lower bronchus during a
routine health check. The mass was resected using a high-frequency
electric snare and argon plasma coagulation through a flexible
bronchoscope under general anesthesia and was proven on
histopathological examination to be an angiolipoma.
Case report
A 74-year-old man was referred to the Department of
Thoracic Surgery of Lanzhou General Hospital (Lanzhou, China) for
treatment of an endobronchial tumor that was incidentally
discovered on chest radiography and computed tomography (CT) during
a routine health check in another hospital, without symptoms. A
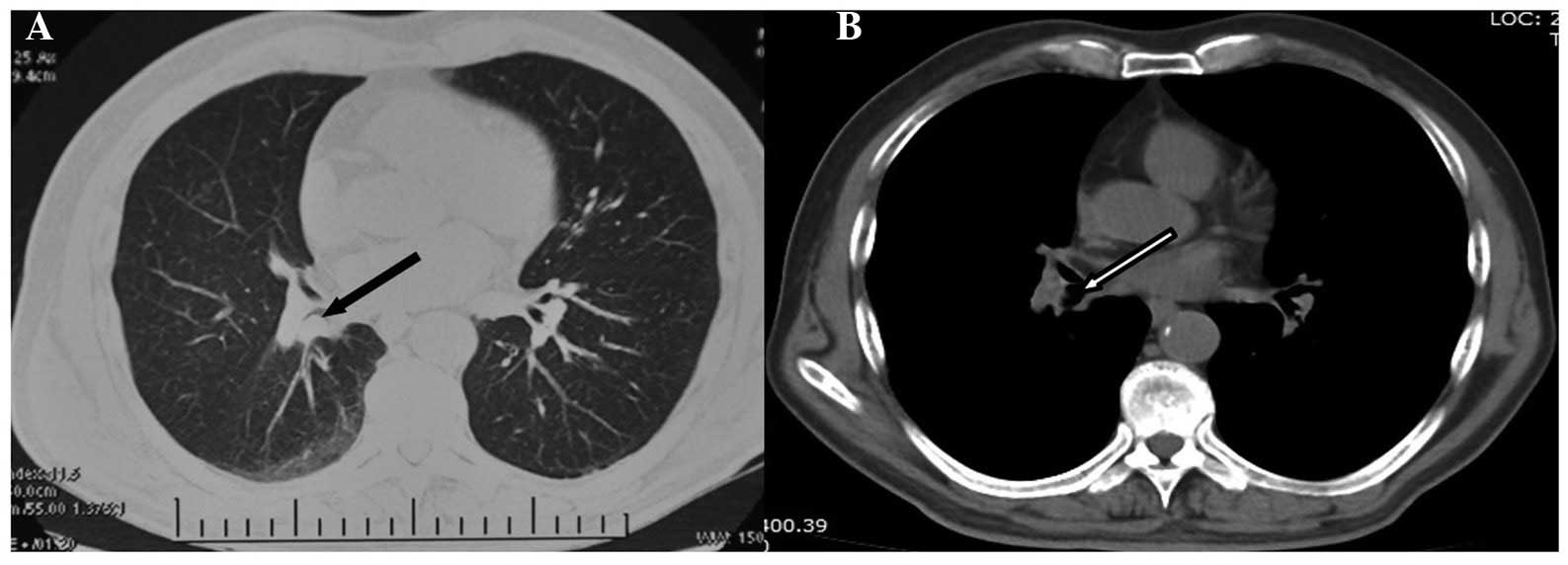
chest CT revealed a round mass, sized ~15×12 mm, occluding the
lumen of the right inferior bronchus, with low attenuation
(Fig. 1). Partial postobstructive
pneumonia in the right lower lobe was also found on the CT scan.
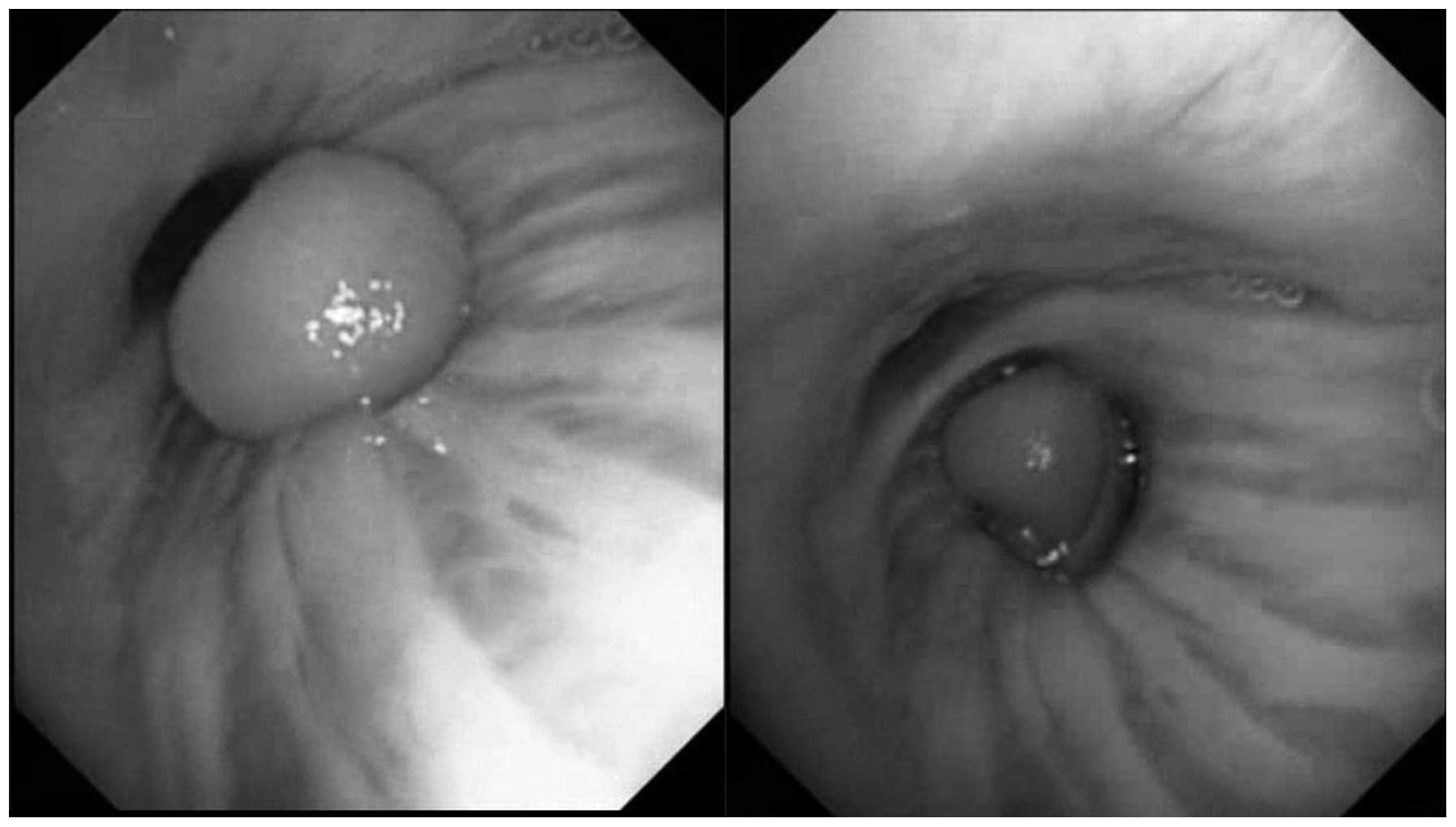
The patient underwent flexible bronchoscopy that confirmed the
presence of a yellowish round pedunculated mass at the orifice of
the right inferior bronchus, which was mobile during breathing and
nearly occluded the bronchial lumen (Fig. 2). As it was difficult to obtain
bioptic specimens from the mass and due to the risk of bleeding,
pathological examination was not performed preoperatively. The
patient had undergone radical resection of gastric carcinoma ~10
years prior, had been diagnosed with diabetes mellitus 1 year
prior, and he was a heavy smoker. Physical examination and
laboratory test results revealed no significant abnormalities.
Bronchoscopic resection of the lesion was performed
during flexible bronchoscopy using a high-frequency electric snare
under general anesthesia. The tumor originated from the membranous
part of the right inferior bronchus. Following removal of the mass,
additional argon plasma coagulation was performed to remove the
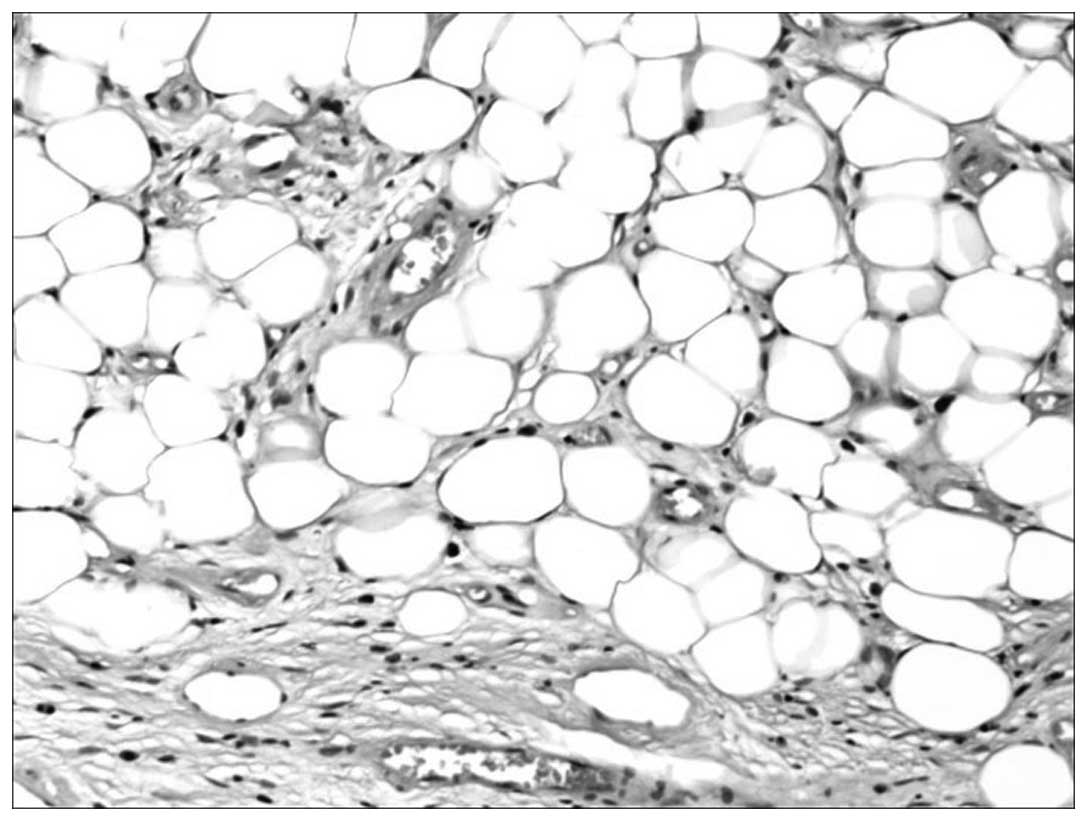
residual tumor base and to control the bleeding. Histologically,
the tumor contained adipose tissue and proliferative blood vessels,
and was diagnosed as angiolipoma (Fig.
3).
The patient's postoperative recovery was uneventful
and he was discharged on the third postoperative day. The patient
has been followed up in the outpatient department for 15 months
with no symptoms or recurrence.
Written informed consent was obtained from the
patient and his family regarding the publication of the case
details and associated images.
Discussion
Angiolipoma was first described as a multiple
subcutaneous tumor and named by Bowen in 1912 (6). In 1960, Howard and Helwig (4) described the clinical and histological
characteristics of angiolipomas that distinguish them from lipomas,
thereby designating angiolipoma as a new entity. Through
cytogenetic analysis, Sciot et al (7) demonstrated a normal karyotype of
angiolipomas, in contrast to the various other types of benign
lipomas, most of which exhibit rather characteristic clonal
chromosomal aberrations, suggesting that the pathogenesis of
angiolipoma differs from that of pure lipomas. Angiolipoma occurs
most commonly in young patients in their second or third decades of
life, and exhibits a male predominance (8). Gonzales-Crussi et al (9) recommended classifying angiolipomas into
two subtypes, namely non-infiltrating and infiltrating. The
non-infiltrating type is more common and is usually
well-encapsulated, just as shown in the present case. The
infiltrating tumors are partially or entirely unencapsulated,
ill-defined and invade adjacent tissues (10).
The pathogenesis of angiolipoma remains unclear.
Trauma, smoking and obesity have been implicated as possible
etiological factors (11,12). Angiolipoma may also be hamartomatous
in nature (12). The patient in the
present case had no history of trauma and was not corpulent, but
was a heavy smoker.
Angiolipomas are mainly located in the subcutaneous
tissues of the trunk and extremities, and are tender or painful on
palpation. Unusual locations reported in the literature, however,
include the brain, breast, intramedullary and epidural spine, foot,
cheek, lip, mediastinum, mandible, ribs, palate, parotid gland and
orbit (12–15). To the best of our knowledge, only one
case of bronchial angiolipoma has been reported in the English
literature to date (5). This
neoplasm is usually slow-growing and presents with symptoms
associated with bronchial obstruction. In our case, the patient was
asymptomatic, as the mass was mobile and did not completely occlude
the lumen.
In the present case, the lesion exhibited low
attenuation in the bronchial lumen on CT examination. The
differential diagnosis should include hamartoma and lipoma.
Angiolipoma may be difficult to distinguish from hamartoma, unless
calcifications are present in the hamartoma, or the ratio of dense
vascular and stromal elements is significantly higher (16). The most characteristic diagnostic
feature of angiolipoma is the presence of adipose tissue and
angiomatous proliferation, as was the case in our patient.
Endobronchial angiolipoma may be resected by
surgical or bronchoscopic methods. In the only previous report of
bronchial angiolipoma, the authors performed successful localized
resection of the lesion and suggested complete surgical resection
was advisable if the patient was able to tolerate the procedure.
However, some scholars consider bronchoscopic resection, which was
employed in the present case, to be the preferred method, as rare
benign tumors characterized by slow growth may carry a low risk of
malignant transformation (11,17,18).
Endoscopic resection includes laser ablation, electrocauterization,
cryorecanalization and electrosurgical snaring (19). Electrosurgical snaring and argon
plasma coagulation are convenient and safe to use for removal of
the lesion by flexible bronchoscopy under general anesthesia, as
described in our case. It was agreed that adjuvant radiation should
not be administered for this benign pathological entity, even in
the infiltrating group (20).
The prognosis of angiolipoma following complete
resection appears to be satisfactory. The patient described in the
present case remained recurrence- and symptom-free at the 15-month
follow-up; however, long-term survival remains to be assessed.
References
|
1
|
Weiss SW and Goldblum JR: Benign
lipomatius tumors. Enzinger and Weiss's Soft Tissue Tumors. 4th.
Mosby; St Louis, MO: pp. 571–639. 2001
|
|
2
|
Ohnishi Y, Watanabe M, Fujii T, Yasui H,
Kubo H and Kakudo K: Infiltrating angiolipoma of the lower lip: A
case report and literature review. Oncol Lett. 9:833–836.
2015.PubMed/NCBI
|
|
3
|
Lin JJ and Lin F: Two entities in
angiolipoma. A study of 459 cases of lipoma with review of
literature on infiltrating angiolipoma. Cancer. 34:720–727. 1974.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Howard WR and Helwig EB: Angiolipoma. Arch
Dermatol. 82:924–931. 1960. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Jiang L, Wang YL, Zhou YM, Xie BX, Wang L,
Ding JA and Jiang GN: Bronchial angiolipoma. Ann Thorac Surg.
88:300–302. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Bowen JT: Multiple subcutaneous
hemangiomas, together with multiplelipomas, occurring in enormous
numbers in an otherwise healthy, muscular subject. Am J Med Sci.
144:189–192. 1912. View Article : Google Scholar
|
|
7
|
Sciot R, Akerman M, Dal Cin P, De Wever I,
Fletcher CD, Mandahl N, Mertens F, Mitelman F, Rosai J, Rydholm A,
et al: Cytogenetic analysis of subcutaneous angiolipoma: further
evidence supporting its difference from ordinary pure lipomas: a
report of the CHAMP Study Group. Am J Surg Pathol. 21:441–444.
1997. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Búa J Arenaz, Luáces R, Franco F Lorenzo,
García-Rozado A, Escudero JL Crespo, Capdevila E Fonseca and
López-Cedrún JL: Angiolipoma in head and neck: Report of two cases
and review of the literature. Int J Oral Maxillofac Surg.
39:610–615. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Gonzalez-Crussi F, Enneking WF and Arean
VM: Infiltrating angiolipoma. J Bone Joint Surg Am. 48:1111–1124.
1966. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Guzey FK, Bas NS, Ozkan N, Karabulut C,
Bas SC and Turgut H: Lumbar extradural infiltrating angiolipoma: A
case report and review of 17 previously reported cases with
infiltrating spinal angiolipomas. Spine J. 7:739–744. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Muraoka M, Oka T, Akamine S, Nagayasu T,
Iseki M, Suyama N and Ayabe H: Endobronchial lipoma: Review of 64
cases reported in Japan. Chest. 123:293–296. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Gerard N and Schultz DA: Angiolipoma of
the upper lip: Report of a case. J Oral Maxillofac Surg.
67:1340–1341. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Kline ME, Patel BU and Agosti SJ:
Noninfiltrating angiolipoma ofthe mediastinum. Radiology.
175:737–738. 1990. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Grivas TB, Savvidou OD, Psarakis SA, Liapi
G, Triantafyllopoulos G, Kovanis I, Alexandropoulos P and Katsiva
V: Forefoot plantar multilobular noninfiltrating angiolipoma: a
case report and review of the literature. World J Surg Oncol.
6:112008. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Sánchez Aniceto G, Salván Saez R and
García Peñin A: Angiolipoma of the cheek: Report of a case. J Oral
Maxillofac Surg. 48:512–515. 1990. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Weill A, del Carpio-O'Donovan R, Tampieri
D, Melanson D and Ethier R: Spinal angiolipomas: CT and MR aspects.
J Comput Assist Tomogr. 15:83–85. 1991. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Nassiri AH, Dutau H, Breen D, Colchen A,
Quiot JJ, Nguyen B and Vergnon JM: GELF Groupe d'Endoscopie de
Langue Française: A multicenter retrospective study
investigatingthe role of interventional bronchoscopictechniques in
the management of endobronchiallipomas. Respiration. 75:79–84.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Choi JC, Yu CM, Ryu YJ, Jeon K, Choi KA,
Kwon OJ and Kim H: The role of endoscopic surgery for completely
obstructive endobronchial benign tumor. Korean J Intern Med.
21:15–19. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Lamprecht B, Hutarew G, Porsch P,
Wegleitner B and Studnicka M: Successful bronchoscopic
cryorecanalization in a case of endobronchial lipoma. Diagn Ther
Endosc. 2011:8456862011. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Gelabert-González M and García-Allut A:
Spinal extradural angiolipoma: Report of two cases and review of
the literature. Eur Spine J. 18:324–335. 2009. View Article : Google Scholar : PubMed/NCBI
|