Introduction
Multiple endocrine neoplasia type 1 (MEN1), is a
rare autosomal dominant disease, linked to a mutation of a tumor
suppressor gene encoding for the protein menin. Tumors occur in
parathyroids, pancreas and pituitary, with a variable phenotype.
Alport syndrome, a recessive X-linked disease is due to mutations
of the genes, encoding for the procollagen IV, usually leading to
end-stage chronic kidney disease. Neurosensory deafness, abnormally
colored retina and misshapen lenses are the other most relevant
features of the syndrome. The patient we describe herein was
carrying both these rare diseases. The clinical challenge we had to
face was to establish the eligibility of the patient to kidney and
possibly pancreas transplantation.
Case report
We report on a 36 year-old man affected by MEN1,
namely with primary hyperparathyroidism (PHPT) and non-secreting
neuroendocrine pancreatic tumor and concomitant Alport syndrome
with end-stage chronic kidney disease. At the age of 10, following
the diagnosis of Alport syndrome in the mother's lineage, the
patient underwent a kidney biopsy which showed a histologic picture
of Alport syndrome. Five years later, because of increasing
proteinuria, angiotensin converting enzyme inhibitor treatment was
started. The renal function progressively deteriorated up to
end-stage renal failure and, at the age of 32, hemodialysis was
started. The diagnosis of Alport syndrome was confirmed by genetic
analysis. Familial PHPT was diagnosed in his father's kindred when
the patient was 30 year-old, and MEN1 genetic analysis revealed an
uncommon complete deletion of the MEN gene in both the patient and
his father. One year later, PHPT was also diagnosed in the patient
who underwent surgical removal of the right superior, left superior
and left inferior parathyroid glands. After surgery, cinacalcet
therapy (30 mg/daily) was started. The patient was referred to our
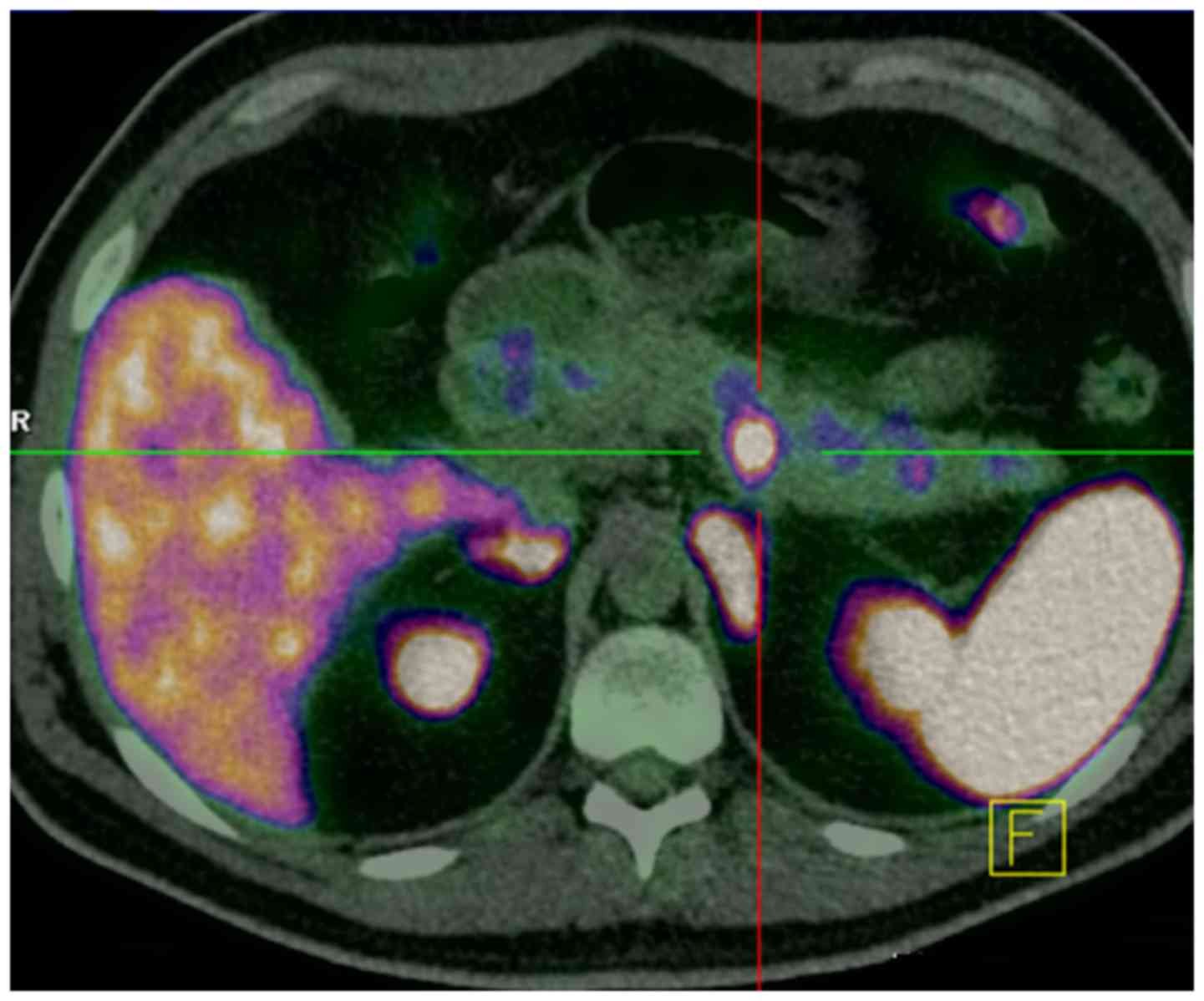
hospital for further evaluation. A whole-body CT scan, performed as
part of the work out of the MEN1 syndrome, showed multiple
pancreatic lesions that were positive at the Gallium-68 Dotatoc PET
scan (Fig. 1). Neuroendocrine
markers were increased (Table I,
column 1). However, treatment with proton pump inhibitor and
end-stage renal failure lessened reliability of their measurement.
In 2014, at the age of 32, the patient underwent
duodenopancreatectomy plus lymphadenectomy. Histology showed
multiple foci of neuroendocrine tumors of intermediate grade (G2)
widespread in the pancreas, with vascular invasion, 2 mitosis/10
high-power fields, immunostaining positive for Ki67 (5%),
chromogranin, CD56, insulin and negative for glucagon; no lymph
nodes metastases were present (ENETS: pT2N0G2; AJCC: cT1N0M0).
After duodenopancreatectomy, treatment with insulin for secondary
diabetes was started. After recovering from pancreatic surgery, in
2016, at the age of 36 years, the patient was evaluated for
eligibility to kidney and possibly pancreas transplantation. At
admission he was in good conditions. Daily treatment consisted of
cinacalcet 30 mg, sevelamer 4,800 mg, lispro 30 IU, degludec 6 IU,
pancreolipase 60,000 IU, cardioaspirin 100 mg, esomeprazol 40 mg.
Laboratory findings are shown in Table
I (column 2). Neck ultrasound and tc-99m sestamibi scan showed
a hyperplastic right inferior parathyroid (diameter: 20 mm).
Abdominal CT scan, Gallium-68 Dotatoc PET scan and pituitary MRI
were all unremarkable.
 | Table I.Laboratory findings before and after
duodenopancreatectomy. |
Table I.
Laboratory findings before and after
duodenopancreatectomy.
|
| Column 1 (before
surgery) | Column 2 (after
surgery) | Normal range |
|---|
| Glucose (mg/dl) | 73 | 121a | 74–109 |
| Hemoglobin A1c
(mmol/mol) | NA | 38a | 20–38 |
| Chromogranin A
(ng/ml) | 1680 | NA | <100 |
| Neuron Specific
Enolase (ng/ml) | 17.6 | 12.3 | <12.5 |
| Glucagon (pg/ml) | 1799 | 298 | 25–250 |
| Gastrin (pg/ml) | 255 | NA | 25–111 |
| Histamine
(mcmol/l) | 10.6 | NA | <10 |
| Calcium (mg/dl) | 10.1b | 8.6–9.7c | 8.6–10.2 |
| Phosphorus
(mg/dl) | 5.8 | 7.3 | 2.7–4.5 |
| Albumin (g/dl) | 4.58 | 4 | 3,5-5,5 |
| PTH (pg/ml) | 311b | 248-283c | 8–40 |
| 25 OH Vitamin D
(ng/ml) | 16.5 | 8.8 | 30–150 |
| 1-25 OH2
Vitamin D (pg/ml) | NA | 17 | 20–67 |
| Bone Alkaline
Phosphatase (mcg/l) | 13 | 43 | 2–15 |
| C-Terminal
Telopeptide (ng/ml) | >6 | >6 | 0.115–0.748 |
| Osteocalcin
(ng/ml) | >200 | >200 | 6.8–34 |
| ACTH (pg/ml) | 31 | NA | 10–50 |
| Cortisol
(mcg/dl) | 13.2 | NA | 6.7–22.6 |
| IGF-1 (ng/ml) | 166 | NA | 77–250 |
| GH (ng/ml) | 0.08 | NA | 0.01–3.6 |
| FSH (mUI/ml) | 5.7 | NA | 1.3–19.5 |
| LH (mUI/ml) | 4.9 | NA | 1.4–12.7 |
| Testosteron
(ng/ml) | 2.7 | NA | 1.75–7.8 |
Discussion
MEN1, an autosomal dominant disease, presents with a
low incidence (2–4/1,000,000 cases per year) but a very high
penetrance. It is linked to a mutation of a tumor suppressor gene
on the long arm (q) of chromosome 11 at position 13.1 encoding for
the protein menin. Tumors occur in parathyroids, pancreas and
pituitary, with a variable phenotype. Alport syndrome, a recessive
X-linked disease with an incidence of 1/50,000 per year, is due to
mutations of the COL4A3, A4 and A5 genes,
encoding for the procollagen IV. Neurosensory deafness, abnormally
colored retina and misshapen lenses are the most relevant features
of the syndrome. The patient we describe herein was carrying both
these rare diseases. The clinical challenge we had to face was to
establish the eligibility of the patient to kidney and possibly
pancreas transplantation. To address this question we had to take
into account several considerations, that will be addressed
thereafter. It is generally agreed that only patients with no
evidence of tumor are eligible to organ transplantation. We had
therefore to establish that the neuroendocrine pancreatic tumor was
on remission, on the basis of undetectable serum markers and
negative imaging. Unfortunately, we could not rely on measurement
of chromogranine because of coexistent modifiable (PPI treatment)
and non-modifiable (end-stage chronic kidney disease) interfering
factors. Measurement of glucagon, which was very high before
duodenopancreatectomy, was not informative for several reasons.
Indeed, hyperglucagonemia can be observed in end stage renal
failure (1), glucagon might have an
extra-pancreatic origins and, in addition, the results of its
measurement are often discordant (2). Older age, high-grade tumor, high
expression of Ki67, number of metastatic lymph nodes and
tumor-related symptoms are all negative prognostic factors for the
recurrence of neuroendocrine tumors (3). Our patient was young and presented with
a low/intermediate malignancy grade tumor with low grade of Ki67
expression. It has been reported that pancreatic neuroendocrine
tumors in patients with MEN1 have a better prognosis compared to
sporadic forms, even in case of recurrence (4). Moreover, because imaging studies were
negative two years after duodenopancreatectomy, we concluded that
the likelihood that the pancreatic tumor was on remission was high.
The outcome of cancer in remission in patients undergoing organ
transplantation is uncertain. A recent meta-analysis of all-organ
transplanted patients has shown a higher mortality rate (HR 3.13;
95% CI, 2.29–4.27) and a higher risk of other neoplasia (HR 1.92;
95% CI, 1.52–2.42) in those cured from a concomitant cancer than in
transplanted, non-neoplastic patients (5). In keeping with their low prevalence, no
data on the prevalence of neuroendocrine tumors in all-organ
transplanted patients has been reported. Available data indicates
that the recurrence rate of cancer in transplanted patients ranges
between 5 and 21%, and is strictly related to the lag between
cancer remission and kidney transplantation as well as type of
tumors, multiple myeloma, breast cancer and kidney cancer showing
the higher recurrence rate (6). The
suggested lag between cancer remission and eligibility to kidney
transplantation varies according to the different guidelines and
depends upon to the type of the tumor. No data about patients with
neuroendocrine tumors undergoing kidney transplantation are
currently available. One should also take in mind that the
mortality rate, particularly because of cardiovascular
complications, is higher in hemodialyzed patients than in the
general population. According to a recent report, the duration of
hemodialysis influences the outcome of patients with end-stage
kidney disease (7). Because our
patient was on hemodialysis for 3 years, his life expectancy was
reduced by 8–20% (7). In addition,
chronic kidney disease and dialysis are independent risk factors
for the occurrence of new tumors (8), in particular lung and urinary tract
cancer (9). We did not consider
pancreatic transplantation as urgent as kidney transplantation
because hyperglicemia was well managed by insulin treatment. In
addition, compared to kidney transplantation, pancreatic
transplantation requires a higher immunosuppressive treatment,
which could negatively affect the outcome of the neuroendocrine
pancreatic tumor. Immunosuppressive therapy by itself increases
tumor incidence and recurrences, the longer the treatment the
higher the incidence of tumors (10). Finally, while establishing
eligibility to kidney transplantation, we had to take into
consideration the concomitant hyperparathyroidism. The finding of
normal serum calcium and high PTH fifteen days after the withdrawal
of cinacalcet was in keeping with the end-stage renal disease and
ruled out persistent primary hyperparathyroidism. Therefore an
additional parathyroidectomy was not taken into consideration. In
addition, post-surgical hypoparathyroidism usually worsens the
adynamic bone state typical of uremic patients (11) and requires a strict adherence to
medications to avoid hypocalcemia. We foresaw that a possible
further rise in serum calcium would require a medical treatment in
order to defer parathyroidectomy as long as possible. We concluded
in favor of the eligibility of the patient for kidney
transplantation for the following reasons: i) the remission of the
pancreatic tumor ant its low risk of recurrence; ii) the higher
mortality in end-stage renal failure overcomes the increased risk
of recurrence of the pancreatic tumor after kidney transplantation;
and iii) no evidence of hypercalcemia.
Acknowledgements
A.M. contributed to this paper as recipient of the
PhD program in Clinical and Translational Science of the University
of Pisa. We would like to thank Ministero dell' Istruzione, dell'
Università e della Ricerca (MIUR, investigator grant 2015 project
code PRIN 2015HPMLFY) for the continuing research support.
References
|
1
|
Bilbrey GL, Faloona GR, White MG and
Knochel JP: Hyperglucagonemia of renal failure. J Clin Invest.
53:841–847. 1974. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Wewer Albrechtsen NJ, Hartmann B, Veedfald
S, Windeløv JA, Plamboeck A, Bojsen-Møller KN, Idorn T,
Feldt-Rasmussen B, Knop FK, Vilsbøll T, et al: Hyperglucagonaemia
analysed by glucagon sandwich ELISA: Nonspecific interference or
truly elevated levels? Diabetologia. 57:1919–1926. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Falconi M, Eriksson B, Kaltsas G, Bartsch
DK, Capdevila J, Caplin M, Kos-Kudla B, Kwekkeboom D, Rindi G,
Klöppel G, et al: ENETS consensus guidelines update for the
management of patients with functional pancreatic neuroendocrine
tumors and non-functional pancreatic neuroendocrine tumors.
Neuroendocrinology. 103:153–171. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Rindi G, Falconi M, Klersy C, Albarello L,
Boninsegna L, Buchler MW, Capella C, Caplin M, Couvelard A,
Doglioni C, et al: TNM staging of neoplasms of the endocrine
pancreas: Results from a large international cohort study. J Natl
Cancer Inst. 104:764–777. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Acuna SA, Huang JW, Daly C, Shah PS, Kim
SJ and Baxter NN: Outcomes of solid organ transplant recipients
with preexisting malignancies in remission: A systematic review and
meta-analysis. Transplantation. 101:471–481. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Chapman JR, Sheil AG and Disney AP:
Recurrence of cancer after renal transplantation. Transplant Proc.
33:pp. 1830–1831. 2001; View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Orandi BJ, Luo X, Massie AB, Garonzik-Wang
JM, Lonze BE, Ahmed R, Van Arendonk KJ, Stegall MD, Jordan SC,
Oberholzer J, et al: Survival benefit with kidney transplants from
HLA-incompatible live donors. N Engl J Med. 374:940–950. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Vajdic CM, McDonald SP, McCredie MR, van
Leeuwen MT, Stewart JH, Law M, Chapman JR, Webster AC, Kaldor JM
and Grulich AE: Cancer incidence before and after kidney
transplantation. JAMA. 296:2823–2831. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Wong G, Hayen A, Chapman JR, Webster AC,
Wang JJ, Mitchell P and Craig JC: Association of CKD and cancer
risk in older people. J Am Soc Nephrol. 20:1341–1350. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Mortaz E, Tabarsi P, Mansouri D, Khosravi
A, Garssen J, Velayati A and Adcock IM: Cancers related to
immunodeficiencies: Update and perspectives. Front Immunol.
7:3652016. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Drüeke TB and Massy ZA: Changing bone
patterns with progression of chronic kidney disease. Kidney Int.
89:289–302. 2016. View Article : Google Scholar : PubMed/NCBI
|