Introduction
Bronchogenic cyst is a relatively rare congenital
malformation that develops from abnormal budding of the ventral
foregut during the early stage of gestation (1). Histologically, the cyst wall is covered
by respiratory-type ciliated epithelium that may include cartilage
and bronchial glands (2). The
location of the cyst is dependent on the stage of embryogenesis at
which budding of the foregut occurs (1). The most common location of bronchogenic
cysts is the middle and superior mediastinum, following the lung
parenchyma (1,2). Unusual locations of bronchogenic cysts
include the thymus, pericardium, diaphragm, esophagus, stomach, and
retroperitoneum (3-10).
Intramural esophageal bronchogenic cysts are rare,
and only 25 cases have been reported in the English literature
since 2000 (7,8,11-25).
However, some cases of bronchogenic cysts in the mediastinum
perforating into the esophagus have been described (26). Intramural bronchogenic cysts in the
gastroesophageal junction are extremely rare (only 6 cases have
been reported in the English literature) (27-32),
and because of the rarity of intramural bronchogenic cysts in the
esophagus and gastroesophageal junction, their unique
clinicopathological features have not been well recognized. The
treatment strategy for bronchogenic cyst is complete excision to
avoid recurrence and rare malignant transformation (33,34).
Therefore, accurate pre-operative diagnosis is very important for
treatment.
In this study, we report three new cases of
intramural bronchogenic cysts in the esophagus and gastroesophageal
junction and review the clinicopathological characteristics of
these rare lesions.
Case report
Case 1
A 35-year-old Japanese man presented with dysphagia.
Upper endoscopic examination revealed an esophageal submucosal
tumor. Pre-operative computed tomography (CT) was not available in
our hospital. Subsequently, thoracoscopic enucleation of the tumor
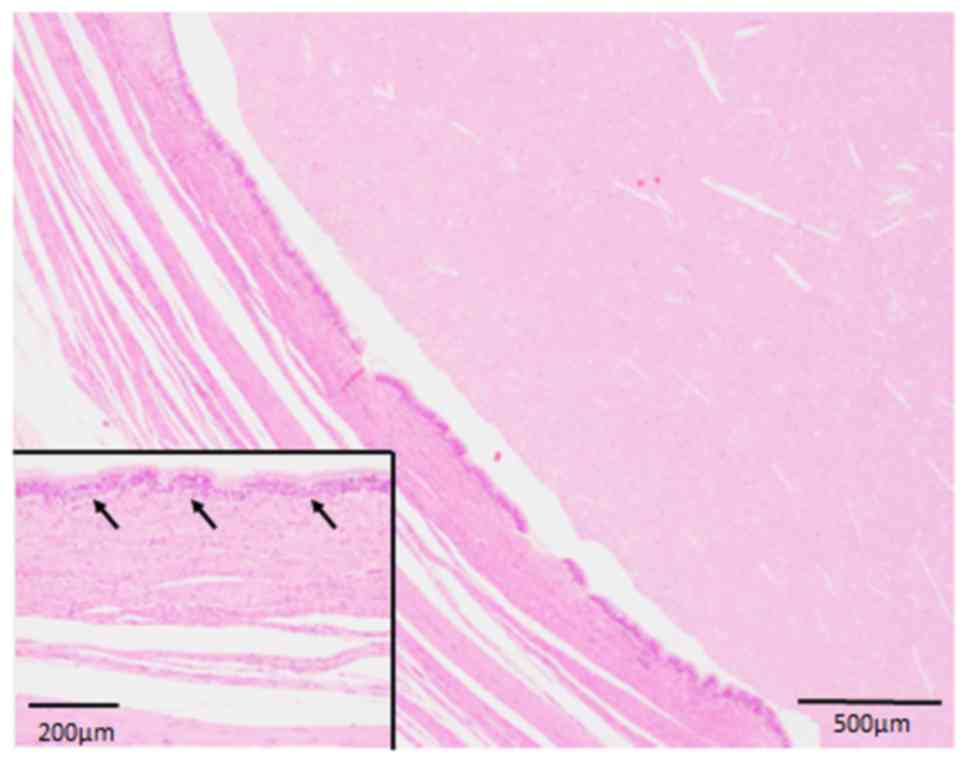
was performed. Histopathological examination indicated that a cyst
(4.5x4x3.5 cm in diameter) was located in the muscularis propria
and contained exudative fluid (Fig.
1). The cyst wall was covered by respiratory type ciliated
epithelium without atypia (Fig. 1
inset). Neither cartilage nor bronchial glands were observed in the
cyst wall. On the basis of these results, the patient was diagnosed
with an intramural esophageal bronchogenic cyst. The post-operative
course was uneventful, and the cyst did not reoccur by CT over 3
years of medical follow-up.
Case 2
A 50-year-old Japanese woman presented with
pharyngeal pain and dysphagia. Upper endoscopic examination
revealed a submucosal tumor in the esophagus, and no surface
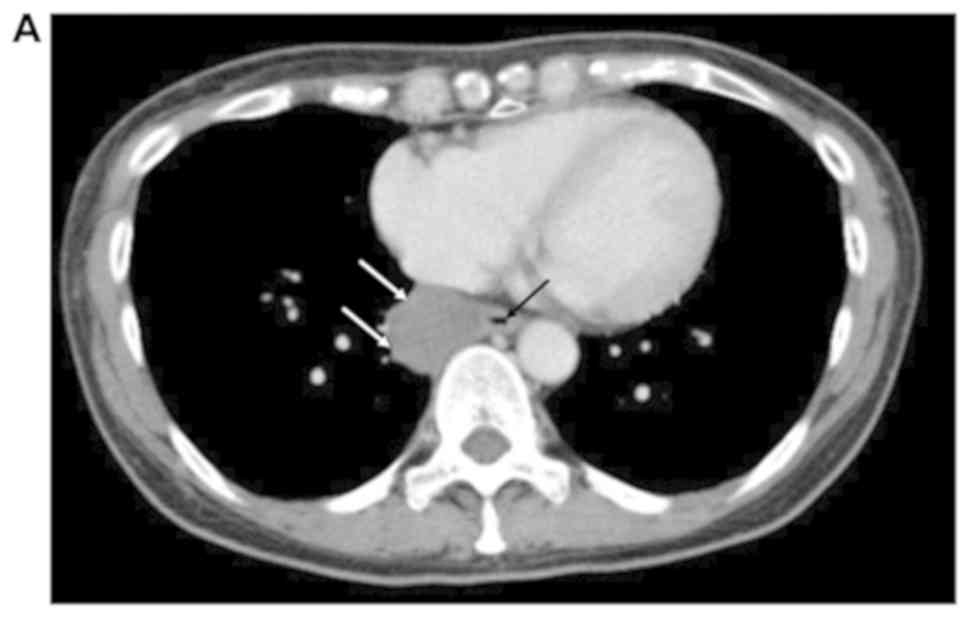
mucosal abnormality was noted. CT demonstrated a submucosal tumor
in the esophagus (Fig. 2A).
Subsequent endoscopic examination showed that the submucosal tumor
was perforating into the esophageal lumen. Therefore, she underwent
thoracoscopic subtotal esophagectomy. Histopathological examination
revealed that the cyst (3.5x2 cm in diameter) was located in the
muscularis propria of the esophagus, and perforated into the
surface squamous mucosa of the esophagus, accompanied by
lymphoplasmacytic infiltration around the cyst (Fig. 2B). The cyst wall was covered by
respiratory-type ciliated epithelium without atypia, and a few
goblet cells were occasionally observed (Fig. 2B, inset). Neither cartilage nor
bronchial glands were observed in the cyst wall. On the basis of
these clinical findings, the patient was diagnosed with an
intramural bronchogenic cyst perforating into the esophageal. The
post-operative course was uneventful, and the patient was free from
recurrence by CT during the 3 months of medical follow-up.
Case 3
A 34-year-old Japanese man presented with heartburn.
Upper endoscopic examination demonstrated that a submucosal tumor
(4.5x3.3 cm in diameter) was located immediately under the
gastroesophageal junction without a remarkable change on the
surface of the gastric mucosa. Pre-operative computed tomography
(CT) was not available in our hospital. Subsequently, enucleation
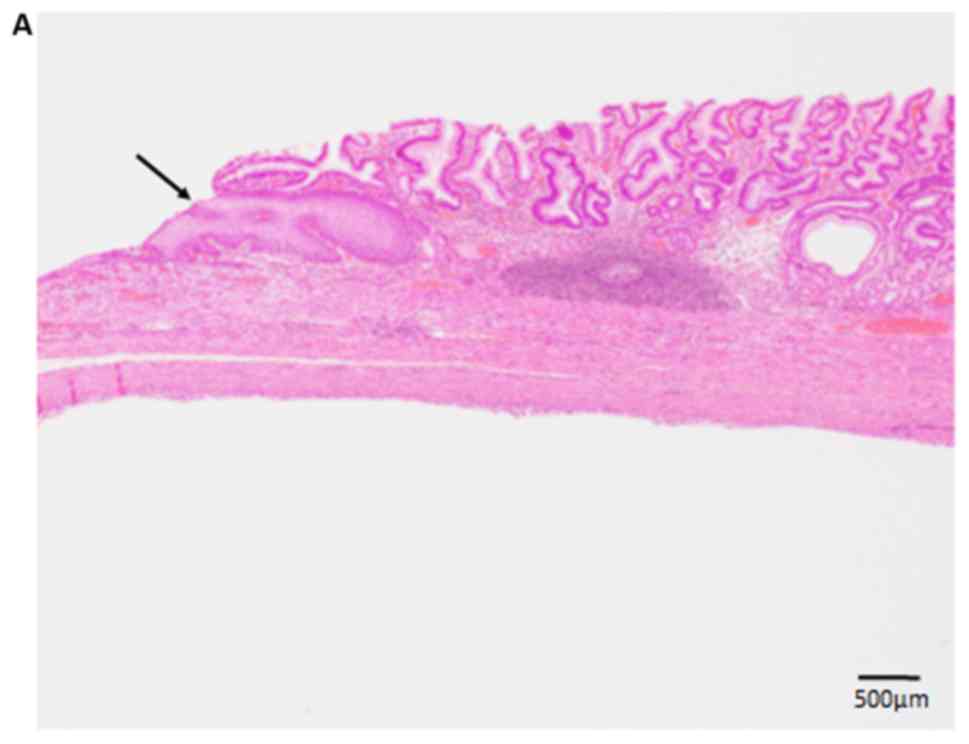
of the tumor was performed. Histopathological analysis showed that
a large cyst was present under the mucosa of the gastroesophageal
junction (Fig. 3A and B) and its wall was covered by
respiratory-type ciliated epithelium without atypia (Fig. 3B, inset). Neither cartilage nor
bronchial glands were observed in the cyst wall. Accordingly, the
patient was diagnosed as intramural bronchogenic cyst in the
gastroesophageal junction. The post-operative course was
uneventful, and the patient was free from recurrence by CT for 1
year of medical follow-up.
Discussion
In this article, we describe the clinicopathological
features of three cases of intramural bronchogenic cysts in the
esophagus and gastroesophageal junction. Table I summarizes the clinicopathological
features of intramural bronchogenic cysts of the esophagus and
gastroesophageal junction that have been reported since 2000.
 | Table IClinicopathological features of
intramural bronchogenic cysts occurring in the esophagus and
gastroesophageal junction. |
Table I
Clinicopathological features of
intramural bronchogenic cysts occurring in the esophagus and
gastroesophageal junction.
| A, Esophagus |
|---|
| Author, year | Case no. | Age | Sex | Size, cm | Chief complaint | Location | Procedure | Histological
features | Outcome | (Refs.) |
|---|
| Cheng et al,
2018 | 1 | 30 years | Male | 8x7x4 | Dysphagia, abdominal
pain | Distal esophagus | Myotomy | Ciliated epithelium,
cartilage, bronchial glands | FFR, 3 months | 7 |
| Lin et al,
2017 | 2 | 20 months | Male | 1.2x1x0.4 | Recurrent
vomitting | Distal esophagus | Laparoscopic
resection | Ciliated epithelium,
cartilage, bronchial glands | FFR 7, months | 11 |
| Han et al,
2016 | 3 | 31 years | Male | 14.5x2.3 | Chest pain,
dysphagia | Para-esophagus | Thoracotomy | Ciliated
epithelium | FFR, 3 months | 12 |
| Altieri et al,
2015 | 4 | 40 years | Female | 3 | abdominal pain | Lower esophagus | Laparoscopic
resection | Ciliated
epithelium | FFR, 2 weeks | 8 |
| Suda et al,
2015 | 5 | 3 days | Male | 2x1 | Inspiratory
stridor | Cervical
esophagus | Myotomy | Ciliated
epithelium | FFR, 9 months | 13 |
| Tang et al,
2014 | 6 | 23 years | Male | 2.5x2 | Chest duscomfort,
dyspnea | Distal esophagus | Endoscopic submucosal
tunnel dissection | Ciliated epithelium,
cartilage, bronchial glands | FFR | 14 |
| Vannucci et
al, 2013 | 7 | 39 years | Female | 25 | Dyspnea, palpable
epigastric mass | Thoracoabdominal | Thoracotomy | NA | FFR, 36 months | 15 |
| Ghobakhlou et
al, 2012 | 8 | 23 years | Female | 3x3 | Dysphagia,
abdominal pain | Distal
esophagus | Thoracotomy | Ciliated
epithelium | FFR | 16 |
| Wang et al,
2012 | 9 | 56 years | Female | 8x7x7 | Chest pain,
dysphagia | Lower
paraesophagus | Thoracotomy | Ciliated
epithelium, cartilage | FFR, 2 years | 17 |
| Barbetakis et
al, 2011 | 10 | 46 years | Male | NA | Dysphagia | Distal
esophagus | VATS | NA | FFR | 18 |
| Chafik et
al, 2011 | 11 | 51 years | Male | 3.6x3.1 | Dysphagia,
pain | Lower
esophagus | Thoracotomy | Ciliated
epithelium, bronchial glands | FFR | 19 |
| Turkyilmaz et
al, 2007 | 12 | 48 years | Male | 3x2x1.5 | Dysphagia | Distal
esophagus | Thoracotomy | Ciliated
epithelium, cartilage | FFR, 6 months | 20 |
| Akutsu et
al, 2006 | 13 | 26 years | Male | NA | Dysphagia | Lower
esophagus | Thoracotomy | Ciliated
epithelium, cartilage | FFR | 21 |
| Ko et al,
2006 | 14 | 21 years | Male | 4 | Dysphagia,
pain | Mid esophagus | VATS | Ciliated
epithelium, cartilage (1/7 case) | FFR, 2 years | 22 |
| Ko et al,
2006 | 15 | 31 years | Female | 3.8 | Dysphagia,
pain | Mid esophagus | Thoracotomy | | FFR, 6 years | 22 |
| Ko et al,
2006 | 16 | 19 years | Female | 3.2 | Dysphagia,
pain | Mid esophagus | Thoracotomy | | FFR, 8 years | 22 |
| Ko et al,
2006 | 17 | 20 years | Female | 3 | Dysphagia, chest
discomfort | Mid esophagus | Thoracotomy | | FFR, 4 years | 22 |
| Ko et al,
2006 | 18 | 34 years | Female | 3.9 | Dysphagia, chest
discomfort | Mid esophagus | Thoracotomy | | FFR, 7 years | 22 |
| Ko et al,
2006 | 19 | 24 years | Female | 3.6 | Dysphagia | Lower
esophagus | VATS | | FFR, 1 year | 22 |
| Ko et al,
2006 | 20 | 60 years | Female | 3.4 | No symptom | Lower
esophagus | Thoracotomy | | FFR, 14 years | 22 |
| Westerterp et
al, 2004 | 21 | 67 years | Male | 6.6 | Odynophagia | Thoracic
esophagus | Esophagectomy | Ciliated
epithelium | FFR | 23 |
| Westerterp et
al, 2004 | 22 | 49 years | Female | 3.1 | Dysphagia | Mid esophagus | Endoscopic mucosal
resection | Ciliated
epithelium | FFR, 1 year | 23 |
| Westerterp et
al, 2004 | 23 | 49 years | Female | 3.3 | No symptom | Esophagus | Local
enuclation | Ciliated
epithelium | FFR, 1 year | 23 |
| Hallani et
al, 2004 | 24 | 64 years | Male | NA | Chest pain | Distal
esophagus | Thoracotomy | NA | FFR | 24 |
| Sashiyama et
al, 2002 | 25 | 34 years | Female | 5 | Dysphagia | Mid esophagus | Endoscopic mucosal
resection | Ciliated
epithelium | FFR | 25 |
| Present study | 26 | 35 years | Male | 4.5x4x3.5 | Dysphagia | Lower
esophagus | Enucleation mucosal
resection | Ciliated
epithelium | FFR, 3 years | - |
| Present study | 27 | 50 years | Female | 3.5x2 | Pharyngeal pain and
dysphagia | Mid esophagus | Thoracoscopic
esophagectomy | Ciliated
epithelium | FFR, 3 months | - |
| B, Gastroesophageal
junction |
| Tonouchi et
al, 2016 | 1 | 32 years | Female | 6 | No symptom | | Laparoscopic
extirpation | Ciliated
epithelium | FFR, 3 months | 27 |
| Kurokawa et
al, 2013 | 2 | 71 years | Male | 3 | Throat
discomfort | | Laparoscopic
resection | Ciliated
epithelium | FFR, 1 year | 28 |
| Ballehaninna et
al, 2013 | 3 | 40 years | Female | 5x3.5 | Dysphagia | | Laparoscopic
resection | Ciliated
epithelium | FFR, 6 months | 29 |
| Fernández et
al, 2011 | 4 | 33 years | Male | 4.5x1.7 | Epigastric and
right upper pain | | Laparoscopic
resection | Ciliated
epithelium | NA | 30 |
| Díaz Nieto et
al, 2010 | 5 | 67 years | Male | 6 | Back pain | | Laparoscopic
resection | Ciliated
epithelium | NA | 31 |
| Melo et al,
2005 | 6 | 39 years | Female | 4x2.5x1 | No symptom | | Laparoscopic
resection | Ciliated
epithelium | FFR | 32 |
| Present study | 7 | 34 years | Male | 4.5x3.3 | Heartburn | | Enucleation | Ciliated
epithelium | FFR, 1 year | - |
Among the 34 patients, men and women were equally
affected. The median age of the patients was 34.5 years with a wide
age distribution (from 3 days to 71 years) (Table I). The most common chief complaint
was dysphagia with discomfort and pain, and no specific complaint
for this lesion is present (Tables I
and II). These symptoms may appear
only when the cysts become larger, leading to compression of the
esophagus and gastrointestinal junction. As most patients have
small asymptomatic cysts (7), the
accurate morbidity of these lesions is unclear.
Histopathologically, the respiratory-type ciliated epithelium was
observed in all cases, and cartilage and bronchial glands were
occasionally found in the cyst wall.
 | Table IISummary of the main characteristics
of intramural bronchogenic cysts. |
Table II
Summary of the main characteristics
of intramural bronchogenic cysts.
| Symptoms | Patients, n | Histology | Patients, n | Procedure | Patients, n |
|---|
| Dysphagia | 19 | Ciliated
epithelium | 31 | Thoracotomy | 13 |
| Pain | 13 | Cartilage | 7 | Laparoscopic
resection | 8 |
| No symptoms | 4 | Bronchial
glands | 4 | VATS | 3 |
| Chest
discomfort | 3 | | | Endoscopic
submucosal resection | 3 |
| Dyspnea | 2 | | | Myotomy | 2 |
Accurate pre-operative diagnosis of bronchogenic
cyst is very important for its appropriate treatment. The diagnosis
of these lesions is challenging because they do not have specific
imaging characteristics. Ko et al (22) reported the imaging characteristics of
7 cases of esophageal bronchogenic cysts. In the report, computed
tomography (CT) revealed that well-defined thin-wall cystic lesions
were present within the esophageal wall. Furthermore, varied cyst
densities were observed (because of the content of the cyst)
without enhancement after administration of a contrast agent, and
no intracystic solid content or abnormal air was identified
(22). However, it may be difficult
to distinguish intramural bronchogenic cysts from mediastinal
masses, including lymphadenopathy or mediastinal tumors, compressed
against the esophageal wall (7,22).
Furthermore, magnetic resonance imaging (MRI) showed variable
signal intensities on T1-weighted images and a homogenous, high
signal intensity on T2-weighted images (25).
Recently, endoscopic ultrasound (EUS) examination
has been recognized as a useful tool for the diagnosis of
bronchogenic cysts (7). EUS can
identify whether the lesions of the esophagus and gastroesophageal
junction are cystic or solid. Moreover, fine-needle aspiration
(FNA) cytological examination using EUS can provide an even more
accurate diagnosis because by this method it is possible to obtain
a sample from the cyst wall. However, EUS-FNA may not be
recommended for all patients with bronchogenic cysts because it can
induce an infection, which would complicate the operation (7). The treatment strategy for bronchogenic
cysts in the esophagus and gastroesophageal junction is complete
resection (7). Therefore, a
combination of the above-mentioned imaging techniques is required
for an accurate pre-operative diagnosis of bronchogenic cyst.
The interesting finding of the present study is that
one of bronchogenic cysts perforated into the esophageal lumen
(Case 2). Only the second endoscopic examination detected the
connection between the cyst and the surface mucosa of the
esophagus. Therefore, secondary inflammation (probably due to
infection) may have led to perforation of the cyst into the
esophageal surface mucosa. Previous studies have already described
an esophageal bronchogenic cyst with a connection to the surface
squamous mucosa (17) and a
mediastinal bronchogenic cyst perforated into the esophageal wall
(26).
In conclusion, we reviewed the clinicopathological
features of bronchogenic cysts in the esophagus and
gastroesophageal junction. No specific symptoms or pre-operative
imaging characteristics were present in this lesion, therefore,
bronchogenic cyst must be added a list of differential diagnosis of
the submucosal tumor of the esophagus and gastroesophageal
junction. As surgical resection is recommended for this lesion,
recognition of the clinicopathological features of bronchogenic
cysts is important for accurate pre-operative diagnosis of this
lesion.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
All data generated or analyzed during this study are
included in this published article.
Authors' contributions
HM, MI and CM conceived and designed the present
study. HM, MI, CM, TM, KI, MS and KT collected and analyzed data.
HM and MI drafted the manuscript and figures. All authors read and
approved the final manuscript.
Ethics approval and consent to
participate
The present study was conducted in accordance with
the Declaration of Helsinki, and the study protocol was approved by
the Institutional Review Board of Kansai Medical University
Hospital (approval no. 2019050). Opt-out consent was obtained from
each participant of this study.
Patient consent for publication
The need for informed consent was waived due to the
retrospective design of the study, and opt-out consent was obtained
from each participant of the present study.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Berrocal T, Madrid C, Novo S, Gutiérrez J,
Arjonilla A and Gómez-León N: Congenital anomalies of the
tracheobronchial tree, lung, and mediastinum: Embryology,
radiology, and pathology. Radiographics. 24(e17)2004.PubMed/NCBI View
Article : Google Scholar
|
|
2
|
Limaïem F, Ayadi-Kaddour A, Djilani H,
Kilani T and El Mezni F: Pulmonary and mediastinal bronchogenic
cysts: A clinicopathologic study of 33 cases. Lung. 186:55–61.
2008.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Hamouri S, Hatamleh M, Alaydi J, Alhadidi
H, Alomari M, Aldaoud N and Darayseh B: Intra-thymic bronchogenic
cyst an extremely rare tumor of anterior mediastinum in adults. J
Cardiothorac Surg. 13(120)2018.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Grozavu C, Fera A, Iliaş M and Pantile D:
Intrapericardial development of a bronchogenic cyst-case report.
Chirurgia (Bucur). 111:345–349. 2016.PubMed/NCBI
|
|
5
|
Simonetti S, Canalís E, Macías L and
Carrasco MA: Clinico-pathological features of the
intradiaphragmatic bronchogenic cysts: Report of a case and review
of the literature. Pathologica. 110:116–120. 2018.PubMed/NCBI
|
|
6
|
Itoh H, Shitamura T, Kataoka H, Ide H,
Akiyama Y, Hamasuna R, Hasui Y, Osada Y and Koono M:
Retroperitoneal bronchogenic cyst: Report of a case and literature
review. Pathol Int. 49:152–155. 1999.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Cheng Y, Chen D, Shi L, Yang W, Sang Y,
Duan S and Chen Y: Surgical treatment of an esophageal bronchogenic
cyst with massive upper digestive tract hematoma without
esophagectomy: A case report and the review of the literature. Ther
Clin Risk Manag. 14:699–707. 2018.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Altieri MS, Zheng R, Pryor AD, Heimann A,
Ahn S and Telem DA: Esophageal bronchogenic cyst and review of the
literature. Surg Endosc. 29:3010–3015. 2015.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Chhaidar A, Ammar H, Abdessayed N, Azzaza
M, Gupta R, Abdennaceur N, Bdioui A, Mokni M and Ali AB: Large
bronchogenic cyst of stomach: A case report. Int J Surg Case Rep.
34:126–129. 2017.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Tu C, Zhu J, Shao C, Mao W, Zhou X, Lin Q,
Li Z, Zhang J, Zhou Q and Chen W: Gastric bronchogenic cysts: A
case report and literature review. Exp Ther Med. 11:1265–1270.
2016.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Lin JS, Yu YR, Chiou EH, Chumpitazi BP,
Schady DA and Brandt ML: Intramural esophageal bronchogenic cyst
mimicking achalasia in a toddler. Pediatr Surg Int. 33:119–123.
2017.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Han C, Lin R, Yu J, Zhang Q, Zhang Y, Liu
J, Ding Z and Hou X: A case report of esophageal bronchogenic cyst
and review of the literature with an emphasis on endoscopic
ultrasonography appearance. Medicine (Baltimore).
95(e3111)2016.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Suda K, Sueyoshi R, Okawada M, Koga H,
Lane GJ, Yamataka A and Doi T: Completely intramural bronchogenic
cyst of the cervical esophagus in a neonate. Pediatr Surg Int.
31:683–687. 2015.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Tang X, Jiang B and Gong W: Endoscopic
submucosal tunnel dissection of a bronchogenic esophageal cyst.
Endoscopy. 46 (Suppl 1):E626–E627. 2014.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Vannucci J, Pecoriello R, Tassi V,
Ceccarelli S and Puma F: Giant thoracoabdominal esophageal
bronchogenic cyst. Dis Esophagus. 26(340)2013.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Ghobakhlou M, Fatemi SR, Dezfouli AA,
Tirgary F and Zali MR: Long-term dysphagia due to bronchogenic cyst
of the esophagus. Endoscopy. 44 (Suppl 2):E129–E130.
2012.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Wang W, Ni Y, Zhang L, Li X, Ke C, Lu Q
and Cheng Q: A case report of para-esophageal bronchogenic cyst
with esophageal communication. J Cardiothorac Surg.
7(94)2012.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Barbetakis N, Asteriou C, Kleontas A,
Papadopoulou F and Tsilikas C: Video-assisted thoracoscopic
resection of a bronchogenic esophageal cyst. J Minim Access Surg.
7:249–252. 2011.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Chafik A, Benjelloun A, Qassif H, El Fikri
A, El Barni R and Zrara I: Intramural esophageal bronchogenic
cysts. Asian Cardiovasc Thorac Ann. 19:69–71. 2011.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Turkyilmaz A, Eroglu A, Subasi M and
Findik G: Intramural esophageal bronchogenic cysts: A review of the
literature. Dis Esophagus. 20:461–465. 2007.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Akutsu Y, Matsubara H, Hayashi H, Okazumi
S, Aoki T, Kozu T and Ochiai T: Endoscope-assisted thoracoscopic
technique for esophageal bronchogenic cyst which presented elevated
CA125. Dig Surg. 23:209–214. 2006.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Ko SF, Hsieh MJ, Lin JW, Huang CC, Li CC,
Cheung YC and Ng SH: Bronchogenic cyst of the esophagus: Clinical
and imaging features of seven cases. Clin Imaging. 30:309–314.
2006.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Westerterp M, van den Berg JG, van
Lanschot JJ and Fockens P: Intramural bronchogenic cysts mimicking
solid tumors. Endoscopy. 36:1119–1122. 2004.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Hallani H, Eslick GD, Cox M, Wyatt JM and
Lee CH: Chest pain? Cause. Lancet. 363(452)2004.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Sashiyama H, Miyazaki S, Okazaki Y, Kaiho
T, Nakajima Y, Hoshino T, Akai T, Nabeya Y, Funami Y, Shimada H, et
al: Esophageal bronchogenic cyst successfully excised by endoscopic
mucosal resection. Gastrointest Endosc. 56:141–145. 2002.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Rubin S, Sandu S, Durand E and Baehrel B:
Diaphragmatic rupture during labour, two years after an
intra-oesophageal rupture of a bronchogenic cyst treated by an
omental wrapping. Interact Cardiovasc Thorac Surg. 9:374–376.
2009.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Tonouchi A, Kinoshita T, Sunagawa H,
Hamakawa T, Kaito A, Shibasaki H, Kuwata T, Seki Y and Nishida T:
Bronchogenic cyst at esophagogastric junction treated by
laparoscopic full-thickness resection and hand-sewn closure: A case
report. Surg Case Rep. 2(41)2016.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Kurokawa T, Yamamoto M, Ueda T, Enomoto T,
Inoue K, Uchida A, Kikuchi K and Ohkohchi N: Gastric bronchogenic
cyst histologically diagnosed after laparoscopic excision: Report
of a case. Int Surg. 98:455–460. 2013.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Ballehaninna UK, Shaw JP and Brichkov I:
Subdiaphragmatic bronchogenic cyst at the gastroesophageal junction
presenting with dysphagia: A case report. Surg Laparosc Endosc
Percutan Tech. 23:e170–e172. 2013.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Fernández JL, Bauza G and McAneny DB:
Minimally invasive management of lesser sac bronchogenic cyst.
JSLS. 15:571–574. 2011.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Díaz Nieto R, Naranjo Torres A, Gómez
Alvarez M, Ruiz Rabelo JF, Pérez Manrique MC, Ciria Bru R, Valverde
Martínez A, Roldán de la Rúa J, Alonso Gómez J and Rufián Peña S:
Intraabdominal bronchogenic cyst. J Gastrointest Surg. 14:756–758.
2010.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Melo N, Pitman MB and Rattner DW:
Bronchogenic cyst of the gastric fundus presenting as a
gastrointestinal stromal tumor. J Laparoendosc Adv Surg Tech A.
15:163–165. 2005.PubMed/NCBI View Article : Google Scholar
|
|
33
|
Fiorelli A, Rambaldi P, Accardo M and
Santini M: Malignant transformation of bronchogenic cyst revealed
by 99mTc-MIBI-SPECT. Asian Cardiovasc Thorac Ann. 20:347–349.
2012.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Taira N, Kawasaki H, Atsumi E, Ichi T,
Kawabata T, Saio M and Yoshimi N: Mucoepidermoid carcinoma of
arising from a bronchogenic cyst of the diaphragm. Ann Thorac
Cardiovasc Surg. 24:247–250. 2018.PubMed/NCBI View Article : Google Scholar
|