Introduction
Cystic lymphangiomas are rare benign tumors that
result from a developmental failure of lymphatic system or
inflammation of lymphatic vessels causing obstruction and
subsequent development of lymphangioma (1-3).
These lesions usually appear in the head, neck and axillary
regions, most often in children (4,5). Less
than 1% of patients present with cystic lymphangiomas in the
mesentery, greater omentum and retroperitoneum (1,3).
Because of this low incidence and absence of symptoms in the
majority of intraabdominal lymphangiomas, these tumors are often
unexpectedly diagnosed in the operative field of other diseases
(6,7).
Most lymphangiomas into the abdominal cavity
originate from the mesentery in which the majority of lymphatic
channels is located. Therefore, intraabdominal lymphangiomas were
previously named as ‘mesenteric cystic lymphangiomas’ (6). However, various locations and sizes of
cystic lymphangiomas have been described. The greater and lesser
omentum, as well as the retroperitoneum are other sites where
cystic lymphangiomas can be found. Differential diagnosis between
cystic lymphangiomas and mesenteric cysts that arise from
mesothelial but not lymphatic tissue is of great importance
(2). Lymphangiomas often behave
aggressively, while mesenteric cysts do not. Histological
examination after surgical excision is often needed to establish
final diagnosis.
In this study, a very rare case of large omental
cystic lymphangioma diagnosed in an adult woman during routine
gynecological examination is described. The aim of this work is to
underline the role of routine gynecological examination and the
importance of full preoperative diagnostic evaluation in cases of
large intraabdominal lesions in order to decide the appropriate
surgical approach and management. The study has been reported in
line with the SCARE criteria (8).
Approval from Leto Maternity Hospital Ethics Committee (no.
42/2018) was given.
Case report
A 40-year-old G2P2 female patient presented, without
symptoms, for routine gynecological examination. She had
obstetrical history of two vaginal deliveries at term, no previous
surgical interventions and medical history of Hashimoto's
thyroiditis without medication.
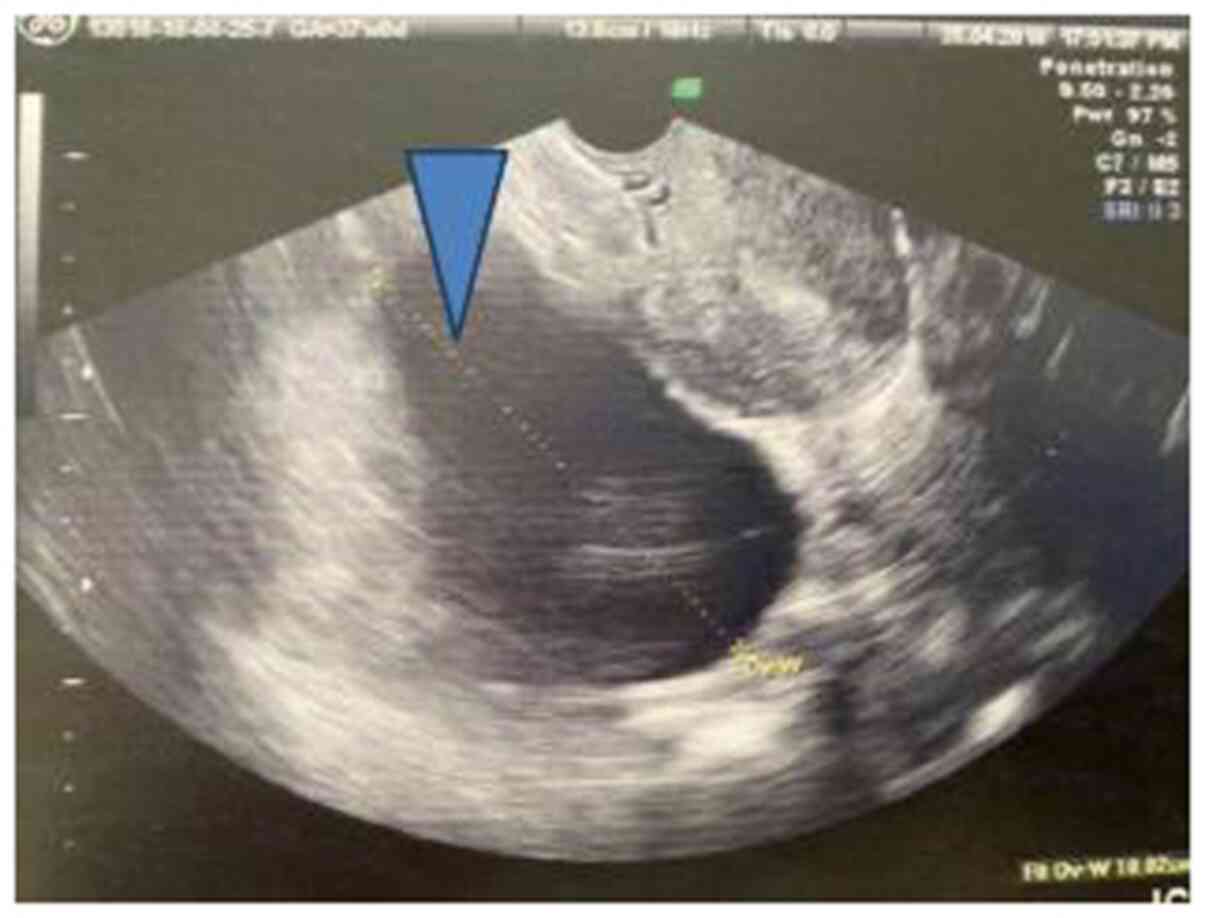
Transvaginal ultrasound examination revealed a
cystic mass, unilocular without solid components or papillary
lesions (maximum diameter of 10 cm) localized at the right
parametrium space, suggestive of large cystic lesion of the right
ovary (Fig. 1). Routine blood
investigations as well as CA-125 marker were into normal ranges
(29.4 U/ml, n.r. <35 U/ml). Further preoperative evaluation with
magnetic resonance imaging (MRI) indicated that the mass was not
arising from the right ovary. It was shown that it was either an
intraabdominal cystic lymphangioma or mesenteric cyst.
Laparotomy, under general anesthesia, via midline
vertical subumbilical incision was done, after obtaining informed
consent from the patient. A large cystic mass originating from the
greater omentum was detected. Complete excision of the lesion after
dissection from the omentum, without need for gastrectomy, was
performed. There was no need for frozen section as the macroscopic
view of the specimen was not suggestive for malignancy.
Histology showed benign vascular cystic lesion, full
of membranoid diaphragms, lymphatic vessels and smooth cells, with
morphological signs suggestive of lymphangioma.
Immunohistochemistry was positive for D2-40 marker, while negative
for Calretinin and CK AE1/AE3. Two lymph nodes that were also
removed were negative for malignant disease.
Post-operative period was uneventful. The patient
was discharged on postoperative day 3 without complications. During
this 2-year follow up period after initial surgery, no recurrence
was identified.
Informed written consent was obtained from the
patient for publication of this case report and accompanying
images.
Discussion
The etiological factors and pathophysiological
mechanisms that lead to lymphangiomas development remain unclear.
As the vast majority of cases occur in children, the hypothesis
that these lesions derive from a congenital abnormality of the
lymphatic system is strongly supported (2). According to this pathophysiological
route lymphangiomas may result from a developmental failure of the
lymphatic system (lymphatic malformation). In our case the patient
was not a child but a 40-year-old female patient without surgical
history. So we have no evidence to identify the chronical presence
of the tumor and its biological behavior, despite the fact that all
previous transvaginal ultrasound examinations were normal.
In addition, our patient was asymptomatic as most
patients with intraabdominal cystic lymphangiomas. This is the
reason for which these masses are often diagnosed in the operative
field of other diseases. However, symptoms including abdominal
distension, pain, nausea and vomiting can be reported as the lesion
progress (3). Potential
complications of intraabdominal cystic lymphangiomas include
infection, torsion, hemorrhage and small bowel obstruction
(9).
Ultrasonography, computed tomography and magnetic
resonance imaging are highly sensitive examinations that can be
useful in preoperative differential diagnosis (10). Lymphangiomas are detected via
ultrasonography as anechoic multilocular cystic masses with
internal septa. In our case a large anechoic cystic mass was found
via transvaginal ultrasonography into the right parametrium space
in attachment with the uterus. This atypical localization of
disease led us to a primary diagnosis of ovarian mass. However,
magnetic resonance imaging revealed that right ovary was not the
site from which this lesion was originating. A differential
diagnosis problem between mesenteric cyst and cystic lymphangioma
was observed after MRI as there are no specific radiological
features to differentiate between these two lesions (2).
In such cases, like ours, pathological examination
is needed in order to confirm diagnosis. Despite being difficult to
differentiate via imaging examinations, these two lesions are
histologically different. Lymphangiomas, as in our case, have an
endothelial lining, foam cells and a wall full of lymphoid tissue,
vessels with smooth muscles and lymphatic spaces, in contrast with
mesenteric cysts which arise from mesothelial tissue.
Total resection of cystic lymphangiomas is
considered as a useful treatment strategy in order to avoid
life-threatening complications of these tumors which have the
potential to grow and invade vital structures. Need for omentectomy
or even gastrectomy has been reported for total removal of cystic
lymphangiomas, depending on the tumors' characteristics, size and
location (6). In our case the
lesion was arising from the greater omentum near to the stomach,
but after dissection, it was removed totally without need for
further surgical intervention.
In conclusion, full preoperative differential
diagnosis evaluation in cases of large intraabdominal lesions is
needed in order to decide the appropriate surgical approach and
management. Computed tomography and magnetic resonance imaging may
add valuable information regarding parameters such as the size,
location, other organ involvement, and solid components within
cysts, that can contribute to preoperative surgical planning.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analysed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
AT contributed to the study concept, design, data
collection, data analysis and writing of the paper. CG was involved
in data collection, data analysis and writing of the paper. KT was
involved in study design and data analysis. IV developed the study
concept and design. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
Approval from Leto Maternity Hospital Ethics
Committee (no. 42/2018) was obtained.
Patient consent for publication
Written consent for publication was obtained from
the patient.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Hamaguchi Y, Arita S, Sugimoto N, Inamoto
O, Takagi H, Kogire M and Kitai T: Laparoscopic resection of
abdominal cystic lymphangioma derived from lesser omentum: Case
report. Medicine (Baltimore). 99(e18641)2020.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Rao TN, Parvathi T and Suvarchala A:
Omental lymphangioma in adults-rare presentation report of a case.
Case Rep Surg. 2012(629482)2012.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Losanoff JE, Richman BW, El-Sherif A,
Rider KD and Jones JW: Mesenteric cystic lymphangioma. J Am Coll
Surg. 196:598–603. 2003.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Kosir MA, Sonnino RE and Gauderer MW:
Pediatric abdominal lymphangiomas: A plea for early recognition. J
Pediatr Surg. 26:1309–1313. 1991.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Makni A, Chebbi F, Fetirich F, Ksantini R,
Bedioui H, Jouini M, Kacem M and Ben Safta Z: Surgical management
of intra-abdominal cystic lymphangioma. Report of 20 cases. World J
Surg. 36:1037–1043. 2012.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Kang BH, Hur H, Joung YS, Kim DK, Kim YB,
Ahn CW, Han SU and Cho YK: Giant mesenteric cystic lymphangioma
originating from the lesser omentum in the abdominal cavity. J
Gastric Cancer. 11:243–247. 2011.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Takiff H, Calabria R, Yin L and Stabile
BE: Mesenteric cysts and intra-abdominal cystic lymphangiomas. Arch
Surg. 120:1266–1269. 1985.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Agha RA, Borrelli MR, Farwana R, Koshy K,
Fowler AJ and Orgill DP: SCARE Group. The SCARE 2018 statement:
Updating consensus surgical CAse REport (SCARE) guidelines. Int J
Surg. 60:132–136. 2018.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Christensen JA, Fuller JW, Hallock JA and
Sherman RT: Mesenteric cysts: A cause of small bowel obstruction in
children. Am Surg. 41:352–354. 1975.PubMed/NCBI
|
|
10
|
Chou YH, Tiu CM, Lui WY and Chang T:
Mesenteric and omental cysts: An ultrasonographic and clinical
study of 15 patients. Gastrointestinal Radiol. 16:311–314.
1991.PubMed/NCBI View Article : Google Scholar
|