Article
Open Access
The effects of rhEPO intervention for perinatal intrauterine herpes virus infection on preventing brain injury in preterm infants
- Authors:
- Ping Tang
- Huijuan Guang
- Ling Huang
-
View Affiliations / Copyright
Affiliations:
Department of Obstetrics, The Second People's Hospital of Liaocheng, Linqing, Shangdong 252601, P.R. China, Department of Obstetrics and Gynecology, Hanzhong Municipal People's Hospital, Hanzhong, Shaanxi 723000, P.R. China, Department VI of Obstetrics, The Central Hospital of Tai'an, Tai'an, Shandong 271000, P.R. China
-
Pages:
271-275
|
Published online on:
October 31, 2017
https://doi.org/10.3892/etm.2017.5412
- Expand metrics +
Metrics:
Total
Views: 0
(Spandidos Publications: | PMC Statistics:
)
Metrics:
Total PDF Downloads: 0
(Spandidos Publications: | PMC Statistics:
)
This article is mentioned in:
Abstract
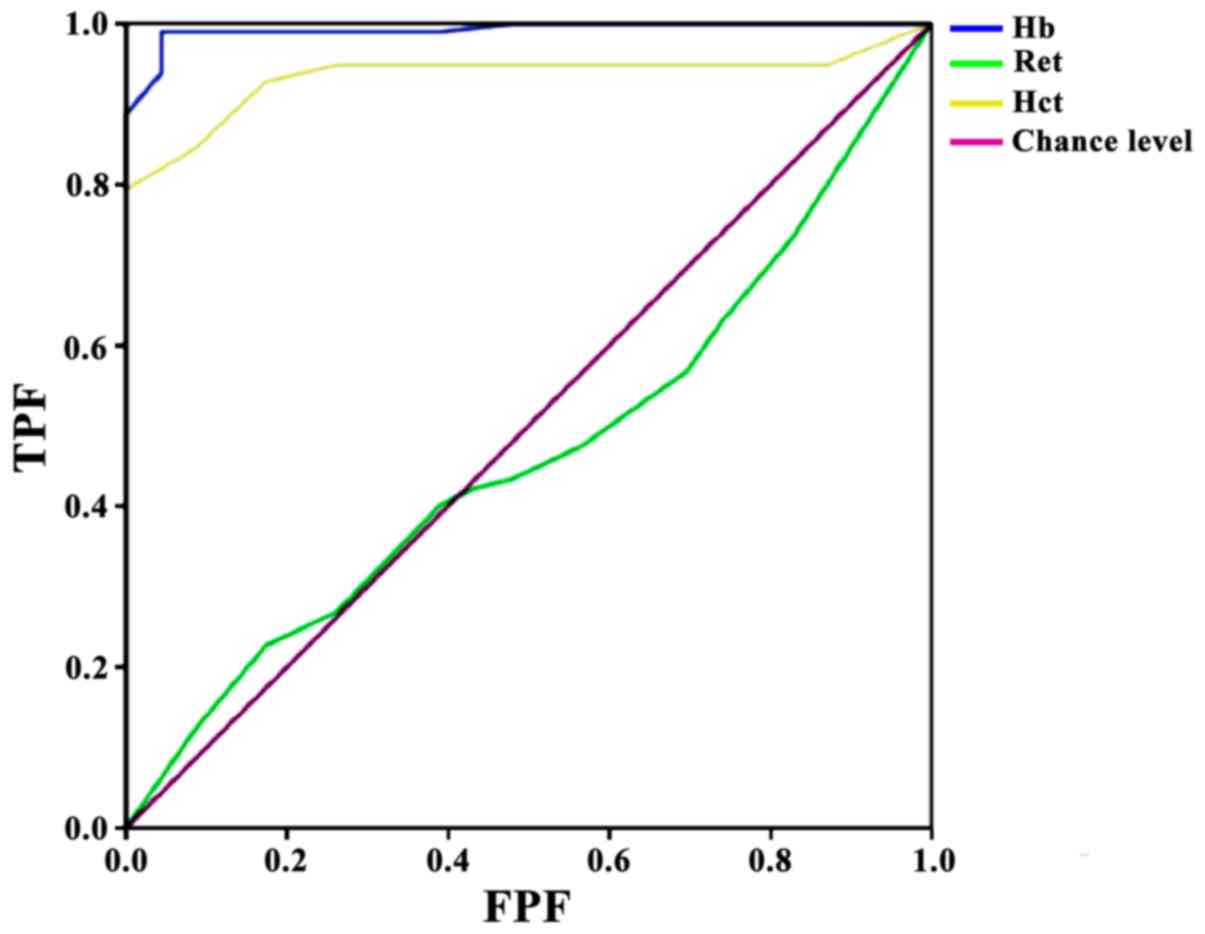
The ability of recombinant human erythropoietin (rhEPO) to protect preterm infants against perinatal intrauterine herpes virus infection-induced brain injury was studied. In total, 120 women infected with perinatal intrauterine herpes virus were randomized into four groups: A, B, C and D, and were given 1,500 IU (mother, pre-partum), 3,000 IU (mother, pre-partum), 250 IU/kg (infant, post-natal), and no rhEPO, respectively. Hemoglobin (Hb), reticulocyte (Ret), hematocrit (Hct), neuron specific enolase (NSE), myelin basic protein (MBP), and S100 protein B (S100B) levels were measured immediately (T0) and at 1 week (T1), 2 weeks (T2), and 4 weeks (T3) post-delivery. Linear regression analysis was performed to analyze inter-indicator correlation, and ROC risk models were established to determine the predictive value of Hb, Ret and Hct for brain injury immediately after delivery. The brain injury incidence rate of group A (10%) was significantly lower than group D (33.3%) and group B (6.7%) significantly lower than groups C (26.7%) and D. At T0, Hb, Ret and Hct in groups A and B were significantly higher than in group C and D, while from T1 to T3, groups A, B and C showed significantly higher values than group D. NSE, MBP and S100B showed an inverse trend, with groups A and B lower at T0 and groups A, B and C lower from T1-T3. Hb and NSE, MBP and S100B were negatively correlated, while no correlation was found between Ret and NSE, MBP and S100B. Finally, Hct and NSE, MBP and S100B were negatively correlated. The optimal cut-off values for Hb and Hct for brain injury diagnosis immediately post-partum were 170 g/l (sensitivity 99%, specificity 95.7%) and 28.5% (sensitivity 79.4%, specificity 100%), respectively. Ret did not show predictive value. In conclusion, pre-partum rhEPO treatment showed greater protective effects than post-natal administration, and this may be the regulation of Hb and Hct levels in post-natal preterm infants. In addition, a dose-dependent effect was displayed.
View References
|
1
|
Barton SK, Tolcos M, Miller SL, Roehr CC,
Schmölzer GM, Davis PG, Moss TJ, LaRosa DA, Hooper SB and Polglase
GR: Unraveling the links between the initiation of ventilation and
brain injury in preterm infants. Front Pediatr. 3:972015.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Pichler M, Staffler A, Bonometti N,
Messner H, Deluca J, Thuile T, Kluge R, Schmuth M and Eisendle K:
Premature newborns with fatal intrauterine herpes simplex virus-1
infection: First report of twins and review of the literature. J
Eur Acad Dermatol Venereol. 29:1216–1220. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Shi J and Mu D: Intrauterine infection and
neonate brain injury. J Clin Pediatr. 33:767–770. 2015.
|
|
4
|
Kashiwagi M, Breymann C, Huch R and Huch
A: Hypertension in a pregnancy with renal anemia after recombinant
human erythropoietin (rhEPO) therapy. Arch Gynecol Obstet.
267:54–56. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Yuan XS, Bian XX, Wei WF, Tang Y and Bao
Q: Effect of recombinant human erythropoietin expressions of
apoptosis genes in rats following traumatic brain injury. Trop J
Pharm Res. 15:695–699. 2016. View Article : Google Scholar
|
|
6
|
Cao Z: Chinese Obstetrics and Gynecology.
2nd. People's Medical Publishing House Co., Ltd.; Beijing: pp.
3792004
|
|
7
|
Kidokoro H, Anderson PJ, Doyle LW,
Woodward LJ, Neil JJ and Inder TE: Brain injury and altered brain
growth in preterm infants: Predictors and prognosis. Pediatrics.
134:e444–e453. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Al-Fadhli M and Saraya M: Herpes Zoster
infection in an infant. J Kuwait Med Assoc. 46:256–257. 2014.
|
|
9
|
Fleiss B, Guillot PV, Titomanlio L, Baud
O, Hagberg H and Gressens P: Stem cell therapy for neonatal brain
injury. Clin Perinatol. 41:133–148. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Chang L and Li W: Intrauterine infection
and preterm infant disease. J Appl Clin Pediatr. 28:1041–1043.
2013.
|
|
11
|
Zhang Z, Li A and Xiao X: Risk factors for
intrauterine infection with hepatitis B virus. Int J Gynaecol
Obstet. 125:158–161. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Kemp MW: Preterm birth, intrauterine
infection, and fetal inflammation. Front Immunol. 5:574. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Bennet L, Booth L and Gunn AJ: Potential
biomarkers for hypoxic-ischemic encephalopathy. Semin Fetal
Neonatal Med. 15:253–260. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Northam GB, Liégeois F, Chong WK, Wyatt JS
and Baldeweg T: Total brain white matter is a major determinant of
IQ in adolescents born preterm. Ann Neurol. 69:702–711. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Thiebaugeorges O, Fresson J, Audibert F,
Guihard-Costa AM, Frydman R and Droulle P: Diagnosis of
small-for-gestational-age fetuses between 24 and 32 weeks, based on
standard sonographic measurements. Ultrasound Obstet Gynecol.
16:49–55. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Uchikura Y, Matsubara K, Matsubara Y, Mori
M, Nabeta M, Hashimoto H, Fujioka T, Hamada K and Nawa A: Nucleated
red blood cells are involved in endothelial progenitor cell
proliferation in umbilical venous blood of preeclamptic patients.
Hypertens Res Pregnancy. 1:46–51. 2013. View Article : Google Scholar
|
|
17
|
Lund A, Lundby C and Olsen NV: High-dose
erythropoietin for tissue protection. Eur J Clin Invest.
44:1230–1238. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Yang W, Cheng Z and Dai H: Calcium
concentration response to uterine ischemia: A comparison of uterine
fibroid cells and adjacent normal myometrial cells. Eur J Obstet
Gynecol Reprod Biol. 174:123–127. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Zhiyuan Q, Qingyong L, Shengming H and Hui
M: Protective effect of rhEPO on tight junctions of cerebral
microvascular endothelial cells early following traumatic brain
injury in rats. Brain Inj. 30:462–467. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Osredkar D, Thoresen M, Maes E, Flatebø T,
Elstad M and Sabir H: Hypothermia is not neuroprotective after
infection-sensitized neonatal hypoxic-ischemic brain injury.
Resuscitation. 85:567–572. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Blackburn S: Brain injury in preterm
infants: Pathogenesis and nursing implications. Newborn Infant Nurs
Rev. 16:8–12. 2016. View Article : Google Scholar
|
|
22
|
Lieber BA, Taylor B, Appelboom G, Prasad
K, Bruce S, Yang A, Bruce E, Christophe B and Connolly ES Jr:
Meta-analysis of telemonitoring to improve HbA1c levels: Promise
for stroke survivors. J Clin Neurosci. 22:807–811. 2015. View Article : Google Scholar : PubMed/NCBI
|