Introduction
Numerous studies have investigated gastric mucosa
associated lymphoid tissue (MALT) lymphoma. It accounts for 20–40%
of extranodal lymphomas and 1–6% of all gastric malignancies
(1–3). Gastric MALT lymphoma is defined as a
distinct clinicopathological entity in the World Health
Organization classification of malignant lymphomas (2,4). It is
widely accepted that Helicobacter pylori (H. pylori)
infection is the primary pathogenic factor stimulating the
development of low-grade, marginal zone B-cell lymphoma of the
stomach. In China, the incidence of H. pylori infection is
high, as is the morbidity rate of patients with gastric MALT
lymphoma (5). There have been few
reports investigating the long-term effect of H. pylori
eradication therapy. Previous studies have demonstrated that H.
pylori eradication leads to the regression of early stage
lymphoma (6–8). However, the traditional strategies used
to treat gastric MALT lymphoma are surgery and chemotherapy.
Long-term follow-up studies investigating the characteristics of
gastric MALT lymphoma and the therapeutic effect of different
treatments remain rare, particularly in China. Therefore, the
current study was conducted on a large number of patients with
gastric MALT lymphoma with the aim of summarizing the
manifestations of the disease and evaluating the effect of H.
pylori eradication on gastric MALT lymphoma.
microRNAs (miRNA) are a group of small noncoding
RNAs 19–24 nucleotides long that regulate gene expression at the
post-transcriptional level (9,10). They
regulate the expression of their target mRNAs by binding to them
(11,12), Previous studies have demonstrated
that miRNAs and their epigenetic mechanisms serve a role in gastric
lymphoma (13,14), however to the best of our knowledge,
the role served by miRNAs in the pathogenesis of gastric MALT
lymphoma remains unknown.
Zinc-finger E-box-binding homeobox (ZEB) 1 and ZEB2
are transcription factors for marginal zone B cells, which induce
the epithelial-mesenchymal transition and promote metastasis in
different types of cancer (15,16). In
H. pylori-positive gastric diffuse large B-cell lymphoma,
the inhibition of ZEB1 by miR-200 leads to a less aggressive form
of the disease (17). However, it
remains unclear whether ZEB2 serves a role in gastric MALT lymphoma
and whether the regulation of ZEB2 is mediated by miRNA. The
current study demonstrates that H. pylori eradication
therapy is effective in the treatment of early gastric MALT
lymphoma.
Materials and methods
Patients
A total of 122 patients (56 females and 66 males;
median age, 56.5 years) with marginal zone B-cell lymphoma of the
primary gastric MALT lymphoma (i.e. disease confined to the stomach
with or without involvement of the paragastric lymph nodes and with
no distant lymph node involvement) who were admitted to Tianjin
Medical University General Hospital (Tianjin, China) were enrolled
in the present study between January 2000 and January 2013. All
patients had stage I1E (confined to the stomach) or II1E
(involvement of paragastric lymph nodes) MALT lymphoma according to
the Ann Arbor classification system modified by Musshoff (6,18,19).
H. pylori status was determined using the rapid urease test,
Giemsa staining or the 13C urea breath test (7). H. pylori infection was classed
as positive if the result of ≥1 test was positive. Gastroendoscopy
was performed in all the 122 patients. The endoscopic type of
gastric lymphoma was classified as superficial, ulcerative or
polypoid based on the classification reported previously (20). Endoscopic ultrasonography (EUS) was
performed to evaluate the depth of tumor invasion and the degree of
perigastric lymphadenopathy in 47 patients.
Initially, 47 patients accepted H. pylori
eradication therapy. First-line treatment consisted of omeprazole
(20 mg; Changzhou Siyao Pharmaceuticals Co., Ltd., Changzhou,
China) or rabeprazole (10 mg; Zhuhai Rundu Pharmacy Ltd., Co.,
Zhuhai, China), amoxicillin (1,000 mg; Beijing Qin Wutian
Pharmaceutical Co., Ltd., Beijing, China) or metronidazole (500 mg;
Qin Wutian Pharmaceutical Co., Ltd.) and clarithromycin (500 mg;
Hainan Puli Pharmacy Co., Ltd., Hainan, China) twice a day for 14
days. Second-line treatment consisted of omeprazole (20 mg) or
rabeprazole (10 mg), levofloxacin (400 mg; Daiichi Saikyo
Pharmaceutical Co., Ltd., Beijing, China) or furazolidone (100 mg;
Shuanghe Pharmaceutical Co., Ltd., Beijing, China) and
clarithromycin (500 mg) or amoxicillin (1,000 mg) twice a day for
14 days. H. pylori status, endoscopic controls and biopsies
were performed 1 month following H. pylori eradication and
were continued every 3 months in the first year, 6 months in the
second year and then once a year from the third year onwards.
The present study was approved by the Ethics
Committee of Tianjin Medical University General Hospital (Tianjin,
China) and written informed consent was obtained from all
participants.
Remission evaluation following H.
pylori eradication
Complete remission (CR) was defined as no
macroscopic findings of lymphoma and negative histology in two
subsequent follow-up investigations. Partial remission (PR) was
defined as normalization or reduction of macroscopic findings,
histological signs of lymphoma regression and no signs of disease
progression. Stable disease (SD) was characterized by unmodified
macroscopy and/or unmodified histology. Progressive disease (PD)
was defined by worsening of macroscopic findings, dissemination of
gastric MALT lymphoma or transformation into DLBCL. Relapse was
defined as persistent histological confirmation of lymphoma
following documentation of CR (4).
Cell lines and reagents
HEK-293T cells, Daudi and U2932 cells (American Type
Culture Collection, Manassas, VA, USA) were cultured in Dulbecco's
modified Eagles medium and NCU-L-4 and Raji cells (American Type
Culture Collection, ATCC; Manassas, VA, USA) were cultured in
RPMI-1640 medium (Invitrogen; Thermo Fisher Scientific, Inc.,
Waltham, MA, USA) with 10% fetal bovine serum (Sigma-Aldrich; Merck
KGaA, Darmstadt, Germany) at 37°C with 5% CO2.
Transfection of cells with miRs
Synthetic hsa-miR-383, scrambled control RNA
(miR-control), hsa-miR-383 inhibitor or negative control RNA
(miR-NC) were purchased from Shanghai GeneChem Co., Ltd. (Shanghai,
China). A total of 3×105 cells were seeded in each well
of 6-well plates and transfected with 2 µg ZEB2 overexpression
construct (Shanghai GenePharma Co., Ltd., Shanghai, China), using
Lipofectamine™ 2000 (Invitrogen; Thermo Fisher
Scientific, Inc.). Transfected cells were harvested for RNA or
protein extraction 1–2 days following treatment.
Reverse transcription quantitative
polymerase chain reaction (RT-qPCR)
Total RNA containing miRNA was extracted from
tissues using a miRNeasy Mini kit (Qiagen China Co., Ltd.,
Shanghai, China). cDNA was synthesized using a miScript Reverse
Transcription kit (Qiagen China Co., Ltd.), following the
manufacturer's instructions. Levels of miRNA expression were
analyzed by quantification using SYBR Green miRNA RT-qPCR on a 7500
Fast Real-Time system (both from Applied Biosystems; Thermo Fisher
Scientific, Inc.). U6 was used for normalization in miRNA studies.
Experiments were performed in triplicate and the results were
expressed as the mean ± standard deviation. The genes expression
was normalized against that of GAPDH and relative fold changes were
calculated using the 2−ΔΔCq (21). The amplification was performed as
follows: Denaturation at 94°C for 20 sec, annealing at 60°C for 45
sec followed by an extension at 72°C for 30 sec for 40 cycles. The
following primers were used: GAPDH forward,
5′-GAGAAGTATGACAACAGCCTC-3′ and reverse,
5′-ATGGACTGTGGTCATGAGTC-3′; and ZEB2 forward,
5′-GTGAGGTCTCCCCGAGGTGT-3′ and reverse,
5′-ATTAGGGTGTGTGCATGATGAAT-3′.
Luciferase reporter assay
Luciferase assays in 293T cells and U2932 cells were
performed with 0.02 mg firefly luciferase reporter construct with
the wild-type ZEB2 pCI-neo-RL-ZEB2 (plasmid #35536) or mutant ZEB2
pCI-neo-RL-ZEB2 200b mut (plasmid #35538) (both from Addgene, Inc.,
Cambridge, MA, USA) and 0.02 mg control vector containing
Renilla luciferase pRL-CMV (Promega Corporation, Madison,
WI, USA) in a 24-well plate. Transfection was conducted using
Lipofectamine 2000. HEK-293T cells and NCU-L-4 cells were
co-transfected with miR-control, miR-383, miR-NC and miR-383
inhibitor at a final concentration of 100 nM. Luciferase activity
was measured using a Luciferase Assay system (Promega Corporation).
A total of 48 h post transfection, the activity of firefly
luciferase was normalized to that of Renilla luciferase.
Each experiment was performed in triplicate.
Western blot analysis
Following transfection, cells were cultured for 2
days and protein was extracted using radioimmunoprecipitation assay
lysis buffer (Promega Corporation). Protein concentration was
determined using the BCA protein assay kit (Thermo Fisher
Scientific, Inc.). A total of 40 µg protein from each group was
loaded per lane and underwent 10% SDS-polyacrylamide gel
electrophoresis. Subsequently, proteins were transferred onto a
PVDF membrane (Merck KGaA). Following blocking with 5% non-fat
dried milk at room temperature for 30 min, membranes were incubated
with primary antibodies against ZEB2 (cat no. ab13222; 1:1,000;
Abcam, Cambridge, UK) and GAPDH (cat no. SC81545; 1:1,000; Santa
Cruz Biotechnology, Inc., Dallas, TX, USA) overnight at 4°C.
Following washing with TBST, membranes were incubated with
peroxidase-conjugated goat anti-rabbit secondary antibodies (cat
no. sc-2004, 1:5,000; Santa Cruz Biotechnology, Inc.) at room
temperature for 1 h. Immunoreactive bands were analyzed using the
ECL chemiluminescence system (Thermo Fisher Scientific, Inc.) and
quantified using ImageI software (version 2x; Rawak Software, Inc.,
Stuttgart, Germany).
MTT assay
An MTT assay was performed to determine the
viability of cancer cells. The transfected cells were seeded in
triplicate in a 96-well plate, at a concentration of 500
cells/well. At 24, 48, 72 and 96 h following transfection, 20 µl
MTT (5 mg/ml; Sigma-Aldrich; Merck KGaA) was added to each well and
the cells were further incubated for 4 h at 37°C prior to harvest.
A total of 150 µl dimethyl sulfoxide was used to terminate the
reaction and absorbance was measured at a wavelength of 570 nm
using a microplate reader.
Statistical analysis
Statistical analysis was conducted using the SPSS
17.0 software (SPSS Inc., Chicago, IL, USA) and differences between
groups were assessed using Student's t-test. Survival time was
calculated according to the revised criteria for malignant lymphoma
from the time of diagnosis to that of mortality from any cause or
lost follow-up (22). Follow-up was
calculated as the median time to censoring using reverse
Kaplan-Meier analysis and survival curves were estimated using the
Kaplan-Meier method. RT-qPCR and the luciferase reporter assay were
performed in triplicate. Data are presented as the mean ± standard
deviation and P<0.05 was considered to indicate a statistically
significant difference.
Results
Patient characteristics
The characteristics of the patients participating in
the current study are presented in Table
I. The median age of initial diagnosis was 56.5 years (range,
19–84 years) and 54.1% of the patients were male. All patients
exhibited gastrointestinal symptoms. The most common symptom
experienced was epigastric pain (39.4%), however abdominal
discomfort (23.8%) and bleeding (15.6%) were also common. MALT
lymphoma was most often localized in the antrum of patients (40.2%)
and was determined as multifocal (situated at two different sites
out of the antrum, body and fundus) in 26.2% of patients. Results
indicated that from all the 122 patients who underwent
gastroendoscopy, 46.7% of tumors were classified as ulcerative
type, 20.5% as superficial and 32.8% as polypoid. Among the 122
patients, 97 of them tested positive for H. pylori. With the
exception of those 75 patients who decided to undergo the surgery
or the chemotherapy, 47 received the H. pylori eradication
treatment following diagnosis (Table
I).
 | Table I.Clinical manifestations of gastric
mucosa associated lymphoid tissue lymphoma at diagnosis. |
Table I.
Clinical manifestations of gastric
mucosa associated lymphoid tissue lymphoma at diagnosis.
| Features | n (%) |
|---|
| Age (years) |
|
|
≥60 | 52 (42.6) |
|
<60 | 70 (57.4) |
| Sex |
|
|
Female | 56 (45.9) |
|
Male | 66 (54.1) |
| Symptoms |
|
|
Epigastric pain | 48 (39.4) |
|
Abdominal discomfort | 29 (23.8) |
|
Bleeding | 19 (15.6) |
|
Abdominal distention | 11 (9.0) |
| Poor
appetite | 8 (6.5) |
| Nausea
and vomiting | 7 (5.7) |
| Helicobacter
pylori status |
|
|
Positive | 97 (79.5) |
|
Negative | 25 (20.5) |
| Gastric
location |
|
|
Antrum | 49 (40.2) |
|
Body | 27 (22.1) |
|
Fudus | 14 (11.5) |
|
Multifocal | 32 (26.2) |
| Endoscopic
type |
|
|
Ulcerative | 57 (46.7) |
|
Superficial | 25 (20.5) |
|
Polypoid | 40 (32.8) |
Treatment outcomes
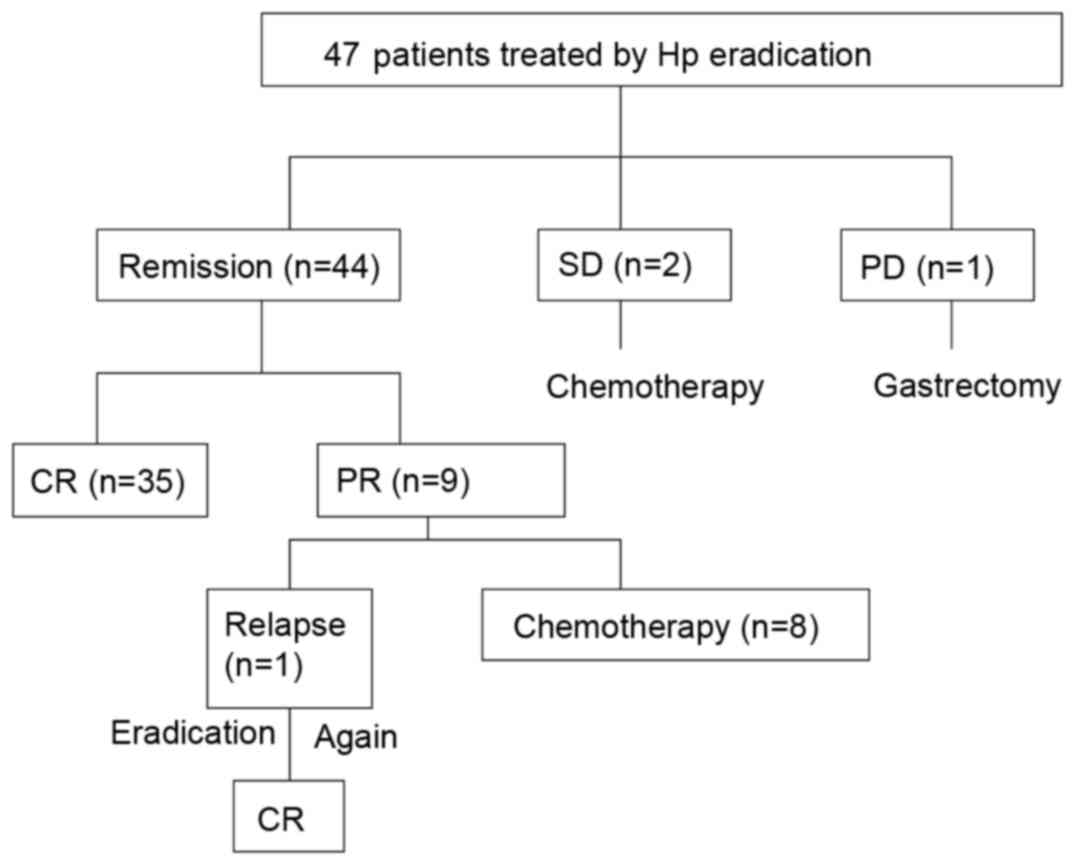
The clinical course following eradication of H.
pylori is summarized in Fig. 1.
A total of 47 patients received H. pylori eradication
treatment. All these patients were infected with H. pylori,
their median age was 52 years old (range, 24–69 years old) and they
all underwent EUS. Among the 47 patients, the depth of lymphoma
infiltration in the gastric wall was: The mucosa in 13,
subcutaneous in 14, muscularis propria in 13 and the entire gastric
wall in 7 patients. The paragastric lymph nodes were involved in
the case of 1 patient with lymphoma that had infiltrated the entire
gastric wall. Overall, lymphoma remission was achieved in 44/47
(93.6%) patients and 35/47 patients achieved CR (74.4%). The median
time taken to achieve CR was 4 months (range, 3–7 months). Among
the 9 patients that achieved PR, 8 chose to undergo chemotherapy
and 1 patient experienced relapse. Following relapse, this patient
underwent further H. pylori eradication and achieved CR in 4
months. A total of 2 out of 47 patients continued to exhibit SD
following H. pylori eradication and subsequently underwent
chemotherapy 6 months later. One patient presented with DLBCL
following H. pylori eradication treatment and subsequently
underwent a gastrectomy (Fig.
1).
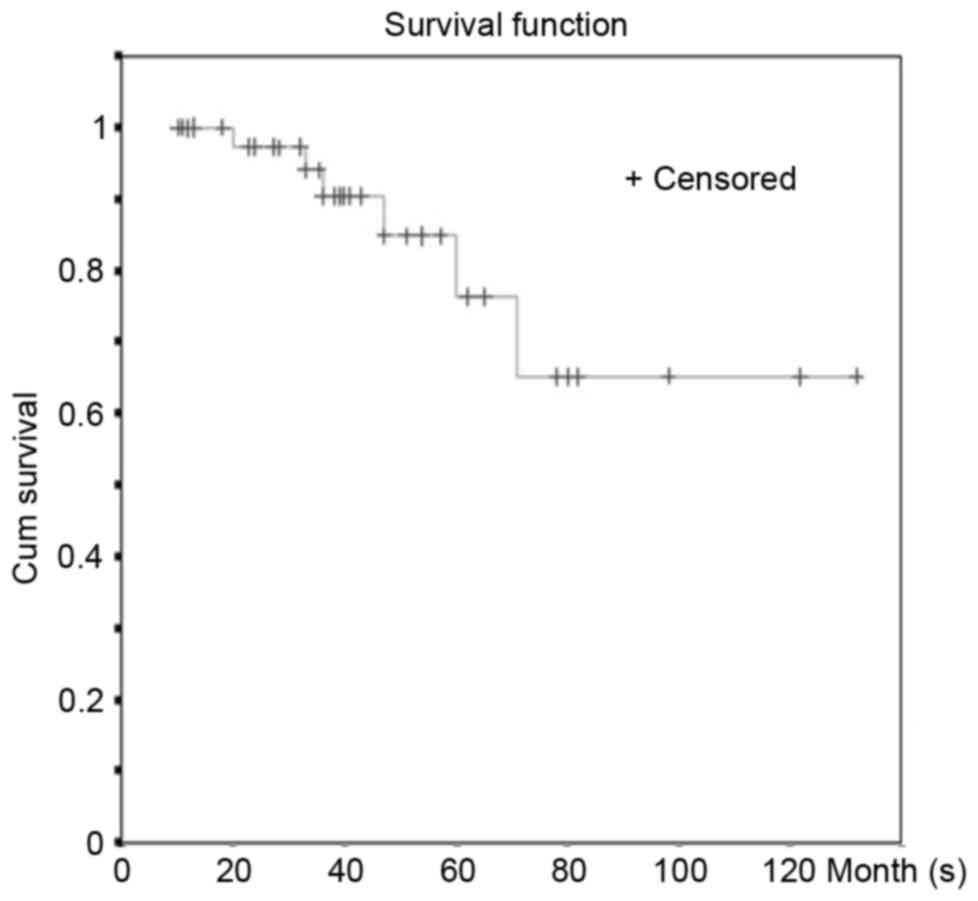
Overall survival
All mortalities, regardless of cause, were recorded.
The results presented are a conservative estimate of survival in
patients with gastric MALT lymphoma. The median follow-up time was
38 months (range, 10–132 months; Kaplan-Meier analysis; Fig. 2). Among the 47 patients, 7 succumbed.
One patient with PD (DLBC lymphoma) succumbed 20 months following
surgery. Another patient with SD also succumbed 36 months following
surgery due to a progression of lymphoma. Other causes of mortality
included coronary syndrome (n=2), stroke (n=2) and chest infection
(n=1). The estimated 3-year survival rate was 90.3% and the 5-year
survival rate was 76.2%.
Expression of miR-383 is downregulated
in gastric MALT lymphoma and cell lines
miR-383 is a tumor suppressor in various types of
cancer, therefore the present study was conducted to identify
whether miR-383 contributes to the progression of gastric MALT
lymphoma. RT-qPCR was conducted to measure miR-383 expression in 47
cases of gastric MALT lymphoma. miR-383 expression in gastric MALT
lymphoma lesions was significantly lower than in the corresponding
non-tumor gastric mucosae (P<0.01; Fig. 3A). miR-383 expression in malignant
lymphoma cell lines was also examined using RT-qPCR. The results
demonstrated that miR-383 was significantly downregulated in the
NCU-L-4, Raji, Daudi lymphoma and U2932 cells compared with
HEK-293T cells (P<0.05; Fig. 3B).
To identify the role of miR-383 in gastric MALT lymphoma, the
expression of miR-383 was measured in HEK-293T and NCU-L-4 cells
transfected with miR-control, miR-383, miR-NC and miR-383 inhibitor
(Fig. 3C and D). The overexpression
or knockdown efficiency was demonstrated. As compared with the
miR-control, miR-183 significantly increased the expression levels
of miR-183 (P<0.05). Furthermore, compared with the miR-NC,
miR-383 inhibitor significantly reduced the miR-183 expression
levels (P<0.05) in HEK-293T cells and NCU-L-4 cells.
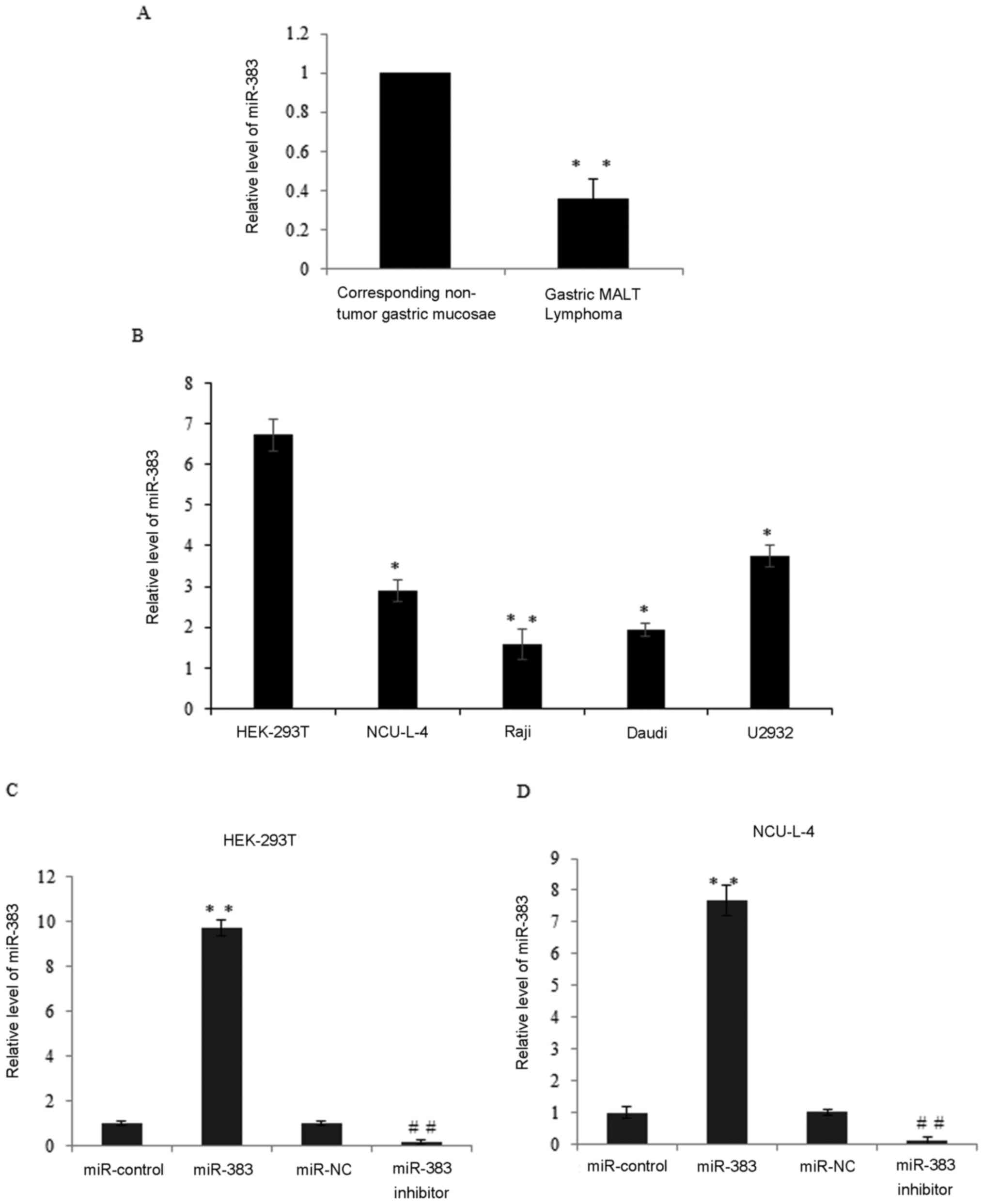 | Figure 3.Expression of miR-383 is
downregulated in gastric MALT lymphoma and cell lines. (A)
Expression of miR-383 in 47 cases of gastric MALT lymphoma and
corresponding non-tumor gastric mucosae by RT-qPCR. **P<0.01 vs.
corresponding non-tumor gastric mucosae. (B) Relative miR-383
expression was detected in the NCU-L-4, Raji, Daudi lymphoma and
U2932 cells compared with HEK-293T cells by RT-qPCR; U6 was used as
an internal control. *P<0.05, **P<0.01 vs. HEK-293T. (C)
Relative miR-383 expression was detected in miR-control, miR-383,
miR-NC and miR-383 inhibitor transfected HEK-293T cells by RT-qPCR.
**P<0.01 vs. miR-control and ##P<0.01 vs. miR-NC.
(D) Relative miR-383 expression was detected in miR-control,
miR-383, miR-NC and miR-383 inhibitor transfected NCU-L-4 cells by
RT-qPCR. **P<0.01 vs. miR-control and ##P<0.01 vs.
miR-NC. Results are presented as the mean ± standard deviation.
miR-383, microRNA-383; MALT, mucosa associated lymphoid tissue;
RT-qPCR, reverse transcription quantitative polymerase chain
reaction. |
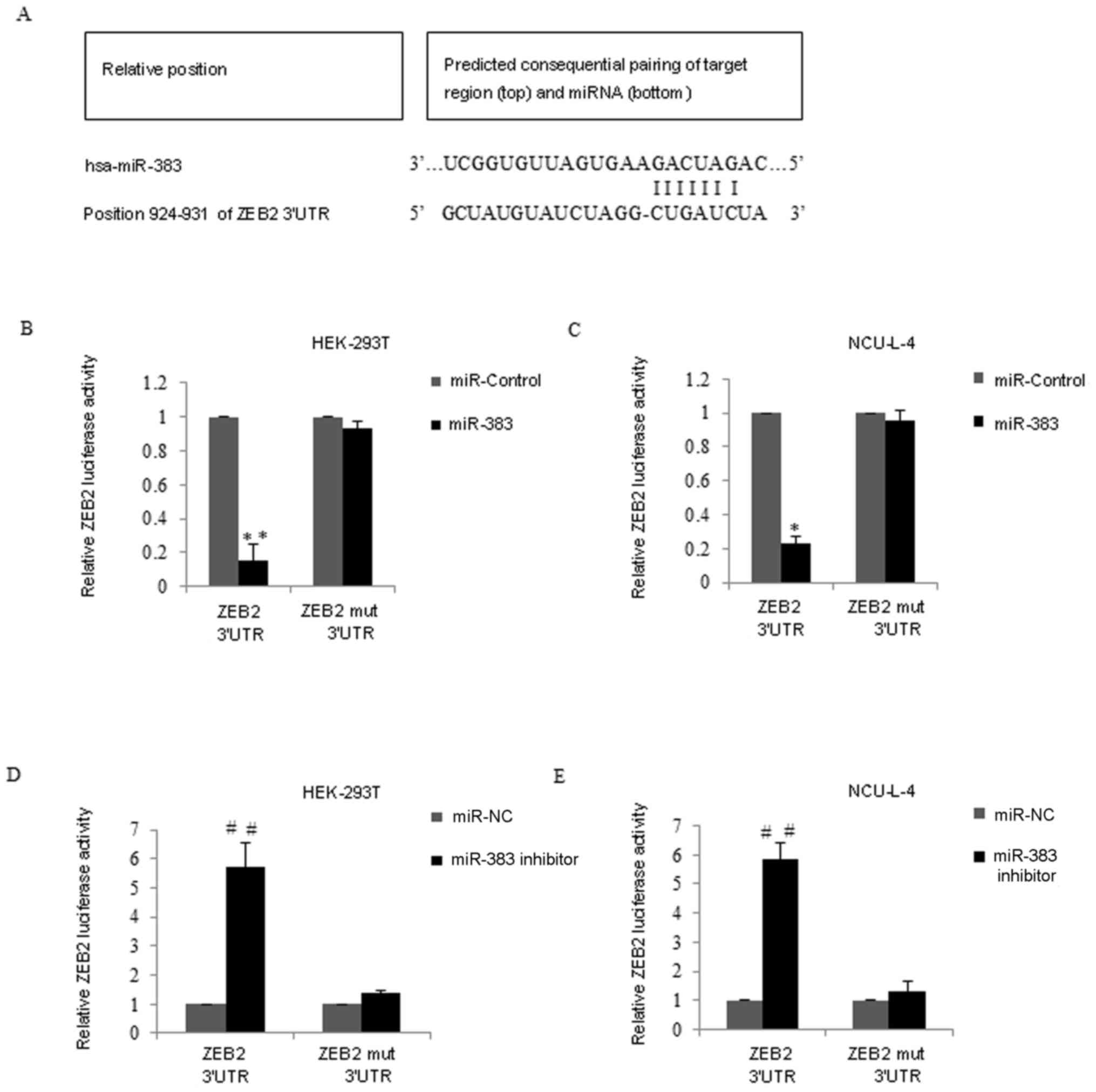
Validation of ZEB2 as a direct target
of miR-383
It was hypothesized that miR-383 may be a tumor
suppressor in gastric MALT lymphoma therefore, the target gene of
miR-383 was screened using TargetScan 6.2 (http://www.targetscan.org). ZEB2 was considered to be
a potential target with miR-383-binding sites (Fig. 4A). To confirm this possibility, the
ZEB2 3′UTR wild-type (wt) or ZEB2 mutant site (ZEB2 3′ UTR-mut) was
cotransfected with miR-383 mimics into HEK-293T cells (Fig. 4B) and NCU-L-4 cells (Fig. 4C). Compared with the miR-control
group, the luciferase reporter activity of the cells containing the
ZEB2-UTR-wt was significantly decreased in HEK-293T and NCU-L-4
miR-383 transfected cells (P<0.01; Fig. 4B; P<0.05; Fig. 4C). However, the luciferase activity
of the ZEB2 3′-UTR-mut reporter was unaffected by the simultaneous
transfection of miR-383 in the two cell lines. By contrast,
co-transfection of ZEB2 3′UTR wt and miR-383 inhibitor into
HEK-293T cells and NCU-L-4 cells resulted in significantly higher
luciferase activity compared with the miR-NC groups (P<0.01)
however, ZEB2 3′-UTR-mut reporter activity was unaffected following
transfection with miR-383 inhibitor (Fig. 4D and E).
miR-383 inhibits proliferation through
the repression of ZEB2 expression
Consistent with the results of the luciferase report
assay, RT-qPCR was used to measure expression of ZEB2 mRNA in
HEK-293T and NCU-L-4 cells transfected with miR-control, miR-383,
miR-NC and miR-383 inhibitor (Fig. 5A
and B). Compared with the control and NC groups, overexpression
of miR-383 significantly inhibited ZEB2 expression (both P<0.01;
Fig. 5A and B). By contrast,
inhibition of miR-383 significantly increased ZEB2 expression in
HEK-293T and NCU-L-4 cells (P<0.01; Fig. 5A; P<0.05; Fig. 5B). Western blot analysis was also
used to measure levels of ZEB2 mRNA in the two cell lines and a
similar trend was observed (data not shown).
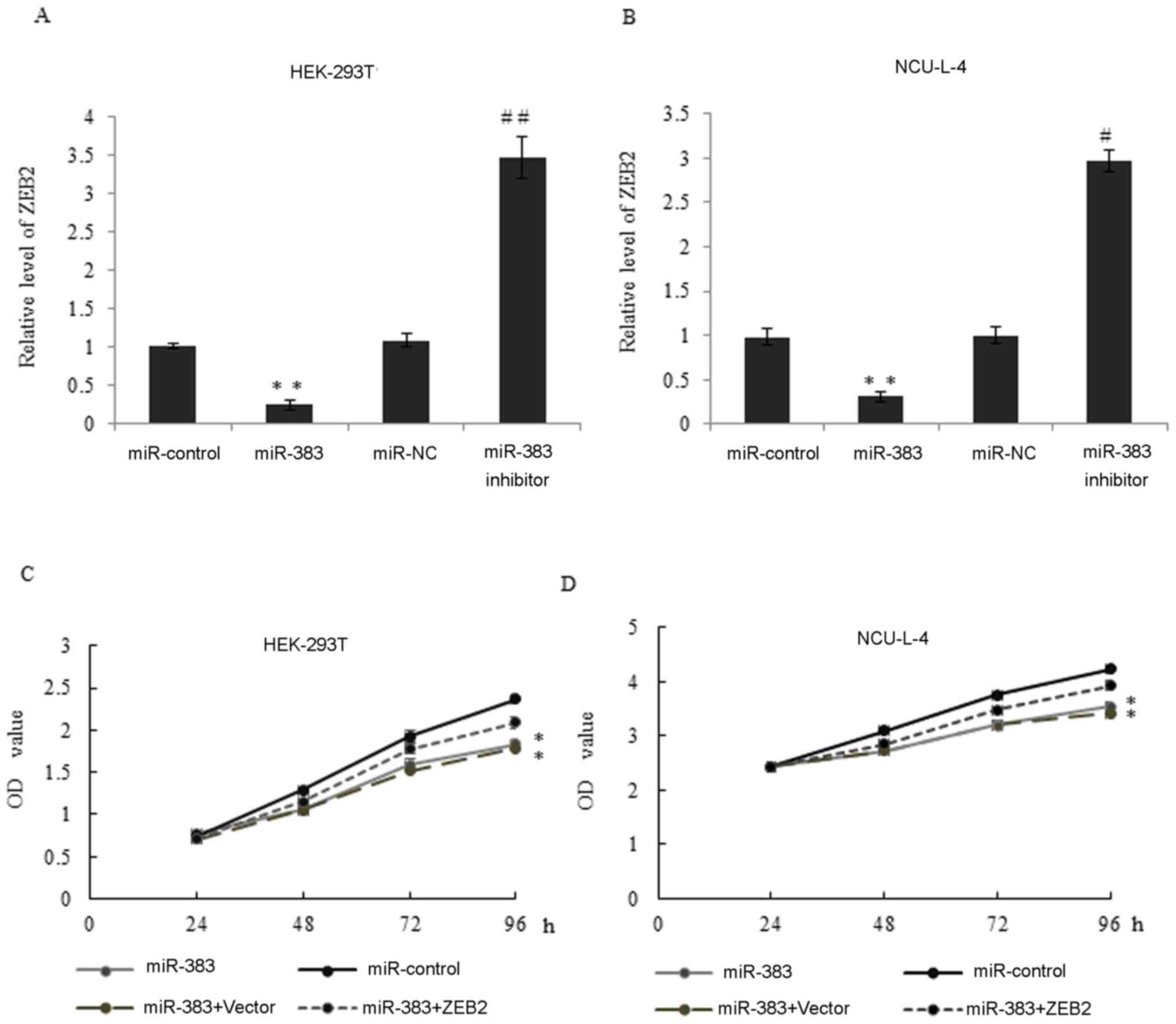 | Figure 5.miR-383 inhibits proliferation
through the repression of ZEB2 expression. (A) The expression of
ZEB2 mRNA in HEK-293T cells transfected with miR-control, miR-383,
miR-NC or miR-383 inhibitor was measured. *P<0.05, **P<0.01,
vs. miR-control. #P<0.05, ##P<0.01 vs.
miR-NC. (B) The level of ZEB2 mRNA expression in NCU-L-4 cells
transfected with miR-control, miR-383, miR-NC or miR-383 inhibitor
was measured. *P<0.05, **P<0.01, vs. miR-control.
#P<0.05, ##P<0.01 vs. miR-NC. (C) Cell
viability was assessed in miR-control, miR-383, miR-383 plus vector
and miR-383 + ZEB2 overexpression construct transfected HEK-293T
cells by MTT assay at 0, 24, 48, 72 and 96 h time points.
*P<0.05, **P<0.01 vs. miR-control. (D) The relative MTT assay
was performed in NCU-L-4 cells. Results are presented at the mean ±
standard deviation. miR-383, microRNA-383; ZEB2, zinc-finger
E-box-binding homeobox 2; NC, negative control. |
To examine whether miR-383 regulates cancer cell
proliferation by suppressing ZEB2 in vitro, an MTT assay was
performed in HEK-293T and NCU-L-4 cells transfected with
miR-control, miR-383, miR-383+vector and miR-383+ZEB2
overexpression vector. The overexpression of miR-383 significantly
inhibited the viability of cells compared with the miR-control
group and this may also be blocked by the additional ZEB2
overexpression (Fig. 5C and D).
Therefore, miR-383 may inhibit the proliferation of cancer cell
lines by suppressing ZEB2 expression in vitro.
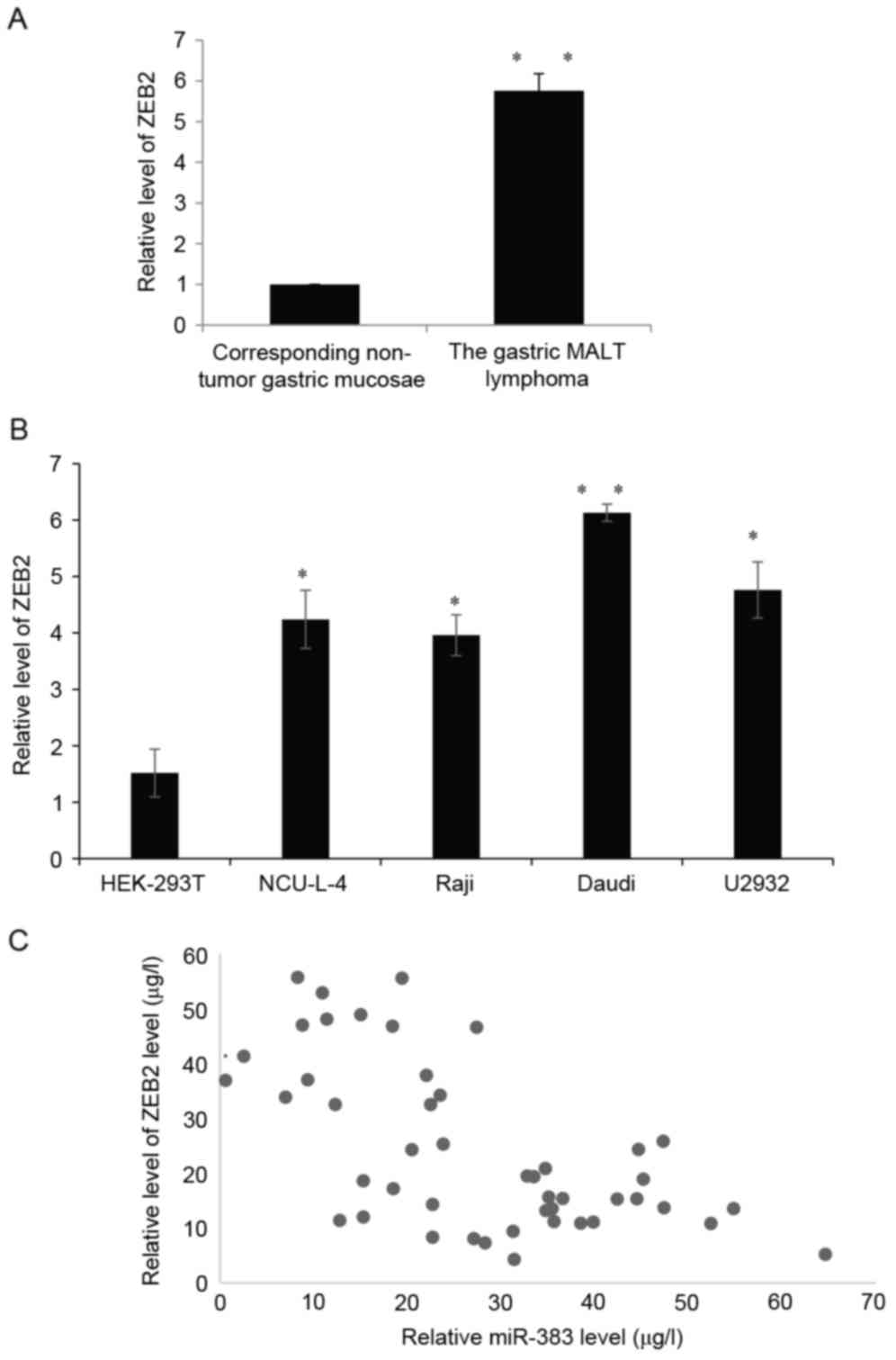
The expression of ZEB2 is upregulated
and is negatively associated with miR-383 expression
The expression of ZEB2 mRNA in patients with gastric
MALT lymphoma was measured (Fig.
6A). The expression of ZEB2 mRNA was significantly increased in
gastric MALT lymphoma tumor tissues compared with corresponding
non-tumor tissues (P<0.01; Fig.
6A). In addition, the expression of ZEB2 mRNA in NCU-L-4, Raji,
Daudi lymphoma and U2932 cells was measured and compared with
expression in HEK-293T cells. The expression of ZEB2 mRNA was also
increased in those cancer cell lines compared with the HEK-293T
cells (all P<0.05; Fig. 6B).
Furthermore, there was an inverse association between the
expression of ZEB2 mRNA and miR-383 in clinical gastric MALT
lymphoma tissues (Fig. 6C). These
results indicate that miR-383 may directly target ZEB2 by
interacting with its 3′-UTR binding site, thus regulating the
endogenous expression of ZEB2 at the transcriptional and
translational levels.
Discussion
Previous studies have demonstrated that H.
pylori infection serves a role in the pathogenesis of MALT
lymphomas of the gastrointestinal tract. Asenjo and Gisbert
(23) indicated that the infection
rate of H. pylori in patients with gastric MALT lymphoma
patients was 90% compared with the 79.5% infection rate observed in
the present study. This difference between rates may be due to the
different dietary habits of patients in the respective countries in
which the studies were conducted.
H. pylori infection stimulates immune
lymphocytes in the gastric mucosa and induces the formation of
MALTs, from which MALT lymphomas of B-cell origin develop.
Cytotoxin-associated gene A may be translocated into human B
lymphocytes through the bacterial type-IV secretion system. H.
pylori colonization induces systemic and mucosal immune
responses (24). Bacterial
colonization of the gastric mucosa triggers lymphoid infiltration
(25) and the formation of acquired
MALTs. H. pylori infection induces and sustains an actively
proliferating B-cell population via direct and indirect immunologic
stimulation and infiltrating T cells serve an important role in the
development of MALT lymphomas (24,26).
Thus, gastric MALT lymphoma may be the only malignant tumor induced
by bacteria infection.
The diagnosis of gastric MALT lymphoma depends
primarily on endoscopic and pathological examination. However, it
is difficult to distinguish between gastric MALT lymphoma, gastric
ulcer, gastritis and gastric cancer as they exhibit similar
endoscopic characteristics and sometimes the pathologic results
reveal inflammation, which may be a result of insufficient or
inadequate biopsy materials. The clinical symptoms of gastric MALT
lymphoma are non-specific and include epigastric pain, abdominal
discomfort and bleeding. Lymphoma is often localized in the antrum,
body and multifocal sites of the stomach and the common endoscopic
types are ulcer, erosion and mucosa edema (27). A large number of biopsies should be
taken from visible lesions and normal mucosa. In cases where
gastric MALT lymphoma is suspected but insufficient or inadequate
initial biopsy materials have been obtained, an EUS and endoscopic
mucosa resection may be required (28). Previous studies have recommended
examining patients for signs of translocation t (11;18) (4,27),
however, this testing is not common in the institution in which the
current study was performed. The fact that none of the patients
participating in the current study were tested for translocation t
(11;18) was a limitation.
Insufficient knowledge of the association between
H. pylori and gastric MALT lymphoma and patient concerns
leads to a large proportion of patients initially choosing surgery
or chemotherapy to treat gastric MALT lymphoma, which was the case
in the present study. Extranodal marginal zone lymphoma of gastric
MALT lymphoma has been defined as a distinct clinicopathological
entity in the World Health Organization's classification of
malignant lymphomas (2). Early
low-grade gastric MALT lymphoma rarely transforms into secondary
DLBCL or progresses beyond the stomach (3,2). Without
transformation or progression, patients with early low-grade
gastric MALT lymphoma rarely succumb and should be treated
conservatively (29). Furthermore,
it has been demonstrated that H. pylori eradication may
induce the regression of low-grade gastric MALT lymphoma in the
majority of patients (27). In the
present study, CR was achieved in 74.4% of the patients who
underwent H. pylori eradication. It is essential to evaluate
the lymphoma response following effective H. pylori
eradication. CR is usually achieved within 6–12 months following
eradication, however in some cases, this may be delayed up to 24–72
months (7). In the present study,
the median time taken to achieve CR was 4 months (range, 3–7
months), which is shorter than the length of time cited in previous
studies (3,8). This may have been due to patients
opting to undergo chemotherapy or surgery when CR was not achieved
6 months following eradication, rather than maintaining a ‘watch
and wait’ strategy. The 3-year survival rate was 90.3% and the
5-year survival rate was 76.2%. This is consistent with previous
studies conducted in different countries (3,5,6). Recently, it has been demonstrated that
patients with H. pylori-negative gastric MALT lymphomas
achieve CR following exclusive anti-H. pylori treatment
(30).
The role of miRNAs and epigenetic mechanisms in
primary gastric mucosa-associated lymphoid tissue lymphoma are
being increasingly studied to improve understanding of its
pathogenesis, prognosis and treatment (31,32).
miR-383 has been identified as a tumor suppressor and potential
prognostic biomarker in human non-small cell lung cancer (33). miR-383 inhibits anchorage-independent
growth and induces glioma cell cycle arrest by targeting cyclin D1
(34). It is also associated with
male infertility and inhibits testicular embryonal carcinoma cell
proliferation by targeting interferon regulatory factor 1 (35). However, it has remains unknown
whether miR-138 serves a function in the progression of gastric
MALT lymphomas and what its target gene is.
To the best of our knowledge, the current study is
the first to investigate the function of miR-383 and demonstrate
that miR-383 inhibits ZEB2 in H. pylori-positive gastric
MALT lymphoma. In the present study, 1 patient relapsed 3 months
following achievement of PR and eradication treatment. This patient
received further H. pylori eradication treatment and
achieved CR in 4 months. The mechanism of lymphoma relapse may be
associated with the re-infection of H. pylori, however this
remains to be determined.
In conclusion, the results of the current study
demonstrate that patients with stage I or II gastric MALT lymphoma
may receive H. pylori eradication as a first-line treatment.
Patients achieving CR following H. pylori eradication may be
managed by follow-up endoscopy with multiple biopsies every 1–2
years. Other treatments, including chemotherapy and surgery, may be
adopted if there is no change following eradication. Furthermore,
the inhibition of ZEB2 by miR-383 contributes to a less aggressive
form of the disease.
References
|
1
|
Nakamura S, Matsumoto T, Iida M, Yao T and
Tsuneyoshi M: Primary gastrointestinal lymphoma in Japan: A
clinicopathologic analysis of 455 patients with special reference
to its time trends. Cancer. 97:2462–2473. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Sabattini E, Bacci F, Sagramoso C and
Pileri SA: WHO classification of tumours of haematopoietic and
lymphoid tissues in 2008: An overview. Pathologica. 102:83–87.
2010.PubMed/NCBI
|
|
3
|
Nakamura S, Sugiyama T, Matsumoto T,
Iijima K, Ono S, Tajika M, Tari A, Kitadai Y, Matsumoto H, Nagaya
T, et al: Long-term clinical outcome of gastric MALT lymphoma after
eradication of Helicobacter pylori: A multicentre cohort follow-up
study of 420 patients in Japan. Gut. 61:507–513. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Ruskoné-Fourmestraux A, Fischbach W,
Aleman BM, Boot H, Du MQ, Megraud F, Montalban C, Raderer M, Savio
A and Wotherspoon A; EGILS group, : EGILS consensus report. Gastric
extranodal marginal zone B-cell lymphoma of MALT. Gut. 60:747–758.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Cheng KS, Chan YK and Yeung YW: Treatment
outcome of gastric extra-nodal marginal zone B-cell lymphoma of
mucosa-associated lymphoid tissue type in the Hong Kong Chinese
population: A single centre experience. J Gastrointest Oncol.
4:198–202. 2013.PubMed/NCBI
|
|
6
|
Andriani A, Miedico A, Tedeschi L, Patti
C, Di Raimondo F, Leone M, Schinocca L, Romanelli A, Bonanno G,
Linea C, et al: Management and long-term follow-up of early stage
H. pylori-associated gastric MALT-lymphoma in clinical practice: An
Italian, multicentre study. Dig Liver Dis. 41:467–473. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Fischbach W, Goebeler-Kolve ME, Dragosics
B, Greiner A and Stolte M: Long term outcome of patients with
gastric marginal zone B cell lymphoma of mucosa associated lymphoid
tissue (MALT) following exclusive Helicobacter pylori eradication
therapy: Experience from a large prospective series. Gut. 53:34–37.
2004. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Wündisch T, Thiede C, Morgner A, Dempfle
A, Günther A, Liu H, Ye H, Du MQ, Kim TD, Bayerdörffer E, et al:
Long-term follow-up of gastric MALT lymphoma after Helicobacter
pylori eradication. J Clin Oncol. 23:8018–8024. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Ke XS, Liu CM, Liu DP and Liang CC:
MicroRNAs: Key participants in gene regulatory networks. Curr Opin
Chem Biol. 7:516–523. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Herranz H and Cohen SM: MicroRNAs and gene
regulatory networks: Managing the impact of noise in biological
systems. Genes Dev. 24:1339–1344. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Lytle JR, Yario TA and Steitz JA: Target
mRNAs are repressed as efficiently by microRNA-binding sites in the
5′ UTR as in the 3′ UTR. Proc Natl Acad Sci USA. 104:pp. 9667–9672.
2007; View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Standart N and Jackson RJ: MicroRNAs
repress translation of m7Gppp-capped target mRNAs in vitro by
inhibiting initiation and promoting deadenylation. Genes Dev.
21:1975–1982. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Matsushima K, Isomoto H, Inoue N, Nakayama
T, Hayashi T, Nakayama M, Nakao K, Hirayama T and Kohno S: MicroRNA
signatures in Helicobacter pylori-infected gastric mucosa. Int J
Cancer. 128:361–370. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Gebauer N, Kuba J, Senft A, Schillert A,
Bernard V and Thorns C: MicroRNA-150 is up-regulated in extranodal
marginal zone lymphoma of MALT type. Cancer Genomics Proteomics.
11:51–56. 2014.PubMed/NCBI
|
|
15
|
Brabletz S and Brabletz T: The ZEB/miR-200
feedback loop - a motor of cellular plasticity in development and
cancer? EMBO Rep. 11:670–677. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Si W, Huang W, Zheng Y, Yang Y, Liu X,
Shan L, Zhou X, Wang Y, Su D, Gao J, et al: Dysfunction of the
reciprocal feedback loop between GATA3- and ZEB2-nucleated
repression programs contributes to breast cancer metastasis. Cancer
Cell. 27:822–836. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Huang WT, Kuo SH, Cheng AL and Lin CW:
Inhibition of ZEB1 by miR-200 characterizes Helicobacter
pylori-positive gastric diffuse large B-cell lymphoma with a less
aggressive behavior. Mod Pathol. 27:1116–1125. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Bartl R, Frisch B, Burkhardt R, Kettner G,
Mahl G, Fateh-Moghadam A and Sund M: Assessment of bone marrow
histology in the malignant lymphomas (non-Hodgkin's): Correlation
with clinical factors for diagnosis, prognosis, classification and
staging. Br J Haematol. 51:511–530. 1982. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Musshoff K: Clinical staging
classification of non-Hodgkin's lymphomas. Strahlentherapie.
153:218–221. 1977.(In German). PubMed/NCBI
|
|
20
|
Roseau G: Role of echoendoscopy in the
study of gastric diseases with fold thickening and in gastric
lymphomas. Gastroenterol Hepatol. 25:19–25. 2002.(In Spanish).
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Cheson BD, Pfistner B, Juweid ME, Gascoyne
RD, Specht L, Horning SJ, Coiffier B, Fisher RI, Hagenbeek A, Zucca
E, et al: Revised response criteria for malignant lymphoma. J Clin
Oncol. 25:579–586. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Asenjo LM and Gisbert JP: Prevalence of
Helicobacter pylori infection in gastric MALT lymphoma: A
systematic review. Rev Esp Enferm Dig. 99:398–404. 2007.(In
Spanish). View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Lin WC, Tsai HF, Kuo SH, Wu MS, Lin CW,
Hsu PI, Cheng AL and Hsu PN: Translocation of Helicobacter pylori
CagA into Human B lymphocytes, the origin of mucosa-associated
lymphoid tissue lymphoma. Cancer Res. 70:5740–5748. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Wu YY, Tsai HF, Lin WC, Hsu PI, Shun CT,
Wu MS and Hsu PN: Upregulation of CCL20 and recruitment of CCR6+
gastric infiltrating lymphocytes in Helicobacter pylori gastritis.
Infect Immun. 75:4357–4363. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Tasaki K, Shichishima A, Furuta M, Yoshida
S, Nakamura N and Abe M: CD5-positive mucosa-associated lymphoid
tissue (MALT) lymphoma of ocular adnexal origin: Usefulness of
fluorescence in situ hybridization for distinction between mantle
cell lymphoma and MALT lymphoma. Pathol Int. 57:101–107. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Stathis A, Chini C, Bertoni F, Proserpio
I, Capella C, Mazzucchelli L, Pedrinis E, Cavalli F, Pinotti G and
Zucca E: Long-term outcome following Helicobacter pylori
eradication in a retrospective study of 105 patients with localized
gastric marginal zone B-cell lymphoma of MALT type. Ann Oncol.
20:1086–1093. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Zucca E and Dreyling M; ESMO Guidelines
Working Group, : Gastric marginal zone lymphoma of MALT type: ESMO
clinical practice guidelines for diagnosis, treatment and
follow-up. Ann Oncol. 5 Suppl 21:v175–v176. 2010. View Article : Google Scholar
|
|
29
|
Liu TY, Dei PH, Kuo SH and Lin CW: Early
low-grade gastric MALToma rarely transforms into diffuse large cell
lymphoma or progresses beyond the stomach and regional lymph nodes.
J Formos Med Assoc. 109:463–471. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Gong EJ, Ahn JY, Jung HY, Park H, Ko YB,
Na HK, Jung KW, Kim do H, Lee JH, Choi KD, et al: Helicobacter
pylori eradication therapy is effective as the initial treatment
for patients with H. pylori-negative and disseminated gastric
Mucosa-Ass. Gut Liver. 10:706–713. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Vasilatou D, Sioulas AD, Pappa V,
Papanikolaou IS, Triantafyllou K, Dimitriadis GD and Papageorgiou
SG: The role of miRNAs and epigenetic mechanisms in primary gastric
mucosa-associated lymphoid tissue lymphoma. Future Oncol.
12:1587–1593. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Thorns C, Kuba J, Bernard V, Senft A,
Szymczak S, Feller AC and Bernd HW: Deregulation of a distinct set
of microRNAs is associated with transformation of gastritis into
MALT lymphoma. Virchows Arch. 460:371–377. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Shang Y, Zang A, Li J, Jia Y, Li X, Zhang
L, Huo R, Yang J, Feng J, Ge K, et al: MicroRNA-383 is a tumor
suppressor and potential prognostic biomarker in human non-small
cell lung caner. Biomed Pharmacother. 83:1175–1181. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Xu Z, Zeng X, Tian D, Xu H, Cai Q, Wang J
and Chen Q: MicroRNA-383 inhibits anchorage-independent growth and
induces cell cycle arrest of glioma cells by targeting CCND1.
Biochem Biophys Res Commun. 453:833–838. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Lian J, Tian H, Liu L, Zhang XS, Li WQ,
Deng YM, Yao GD, Yin MM and Sun F: Downregulation of microRNA-383
is associated with male infertility and promotes testicular
embryonal carcinoma cell proliferation by targeting IRF1. Cell
Death Dis. 1:e942010. View Article : Google Scholar : PubMed/NCBI
|