Introduction
The clinical and pathological picture of lymphomas
covers a wide spectrum, and the rate of occurrence in the oral
cavity is 3–5% (1). Among the
malignant tumors of the oral cavity, lymphomas represent the third
most common type of tumor after squamous cell carcinoma and
salivary gland neoplasms. Lymphomas of the oral cavity mostly arise
from the Waldeyer ring, a lymphoid tissue, and rarely involve the
hard palate, vestibulum and gingival tissue (1,2). The most
common symptoms of lymphoma include pain due to swelling,
difficulty in speech due to ulceration and difficulty when
swallowing. Physical examination may reveal a submucosal mass, a
polypoid mass covered with a smooth mucosa or an ulcerated lesion
(3). The diagnosis may be confirmed
by pathological examination. The treatment of lymphomas depends on
the stage of tumor, the histological type and the age of the
patient, and may involve chemotherapy, radiotherapy or combined
therapy (4,5). In this study, the case of cystic
isolated lymphoma of the base of the tongue in a 48-year-old male
who presented with a sore throat is reported. Written informed
consent was obtained from the patient.
Case report
Patient presentation
In May 2013, a 48-year-old male patient was admitted
to the Ear, Nose and Throat clinic of the Education and Research
Hospital (Erzurum, Turkey) with the complaint of pain for 2 months
and the sensation of a foreign body in the throat. Medical history
revealed that the patient had received antibiotic treatment several
times for these complaints but no improvement had been noted. His
family history revealed no genetic disorders. The patient was a
non-smoker and no alcohol use was noted.
Examinations and findings
An endoscopic laryngeal examination revealed a 1.5×2
cm cystic mass with a wide base and smooth mucosal cover on the
right side of the tongue base extending to the vallecular. Other
laryngeal structures were normal. No cervical lymphadenopathy was
identified by palpation. Findings from other systemic and head and
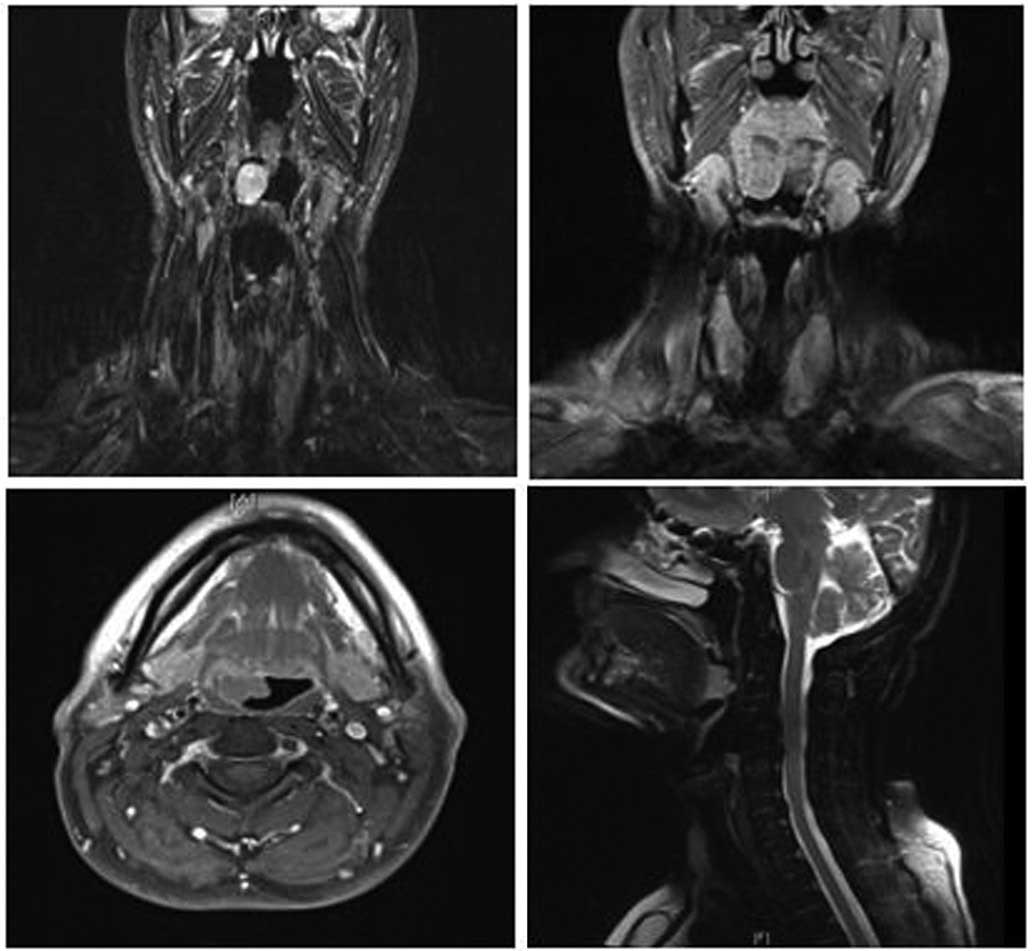
neck examinations were within the normal limits. Neck magnetic
resonance imaging was performed using a MAGNETOM Avanto 1.5T device
(Siemens Aktiengesellschaft, Munich Germany), which revealed a
20×17×16 mm lesion with a cystic component and peripheral minimal
contrast uptake (Fig. 1). The
complete blood count results were as follows: hemoglobin, 15 g/dl;
hematocrit, 45.5%; white blood cells, 7.4×103/ml; red
cell distribution width, 13.7; platelets, 316×103/ml.
ELISA tests for hepatitis and HIV were negative. The chest X-ray
was normal.
Surgery and diagnosis
Under general anesthesia, the mass with its cystic
component extending to the vallecular was excised and wide
incisional biopsy materials were obtained from the vegetative field
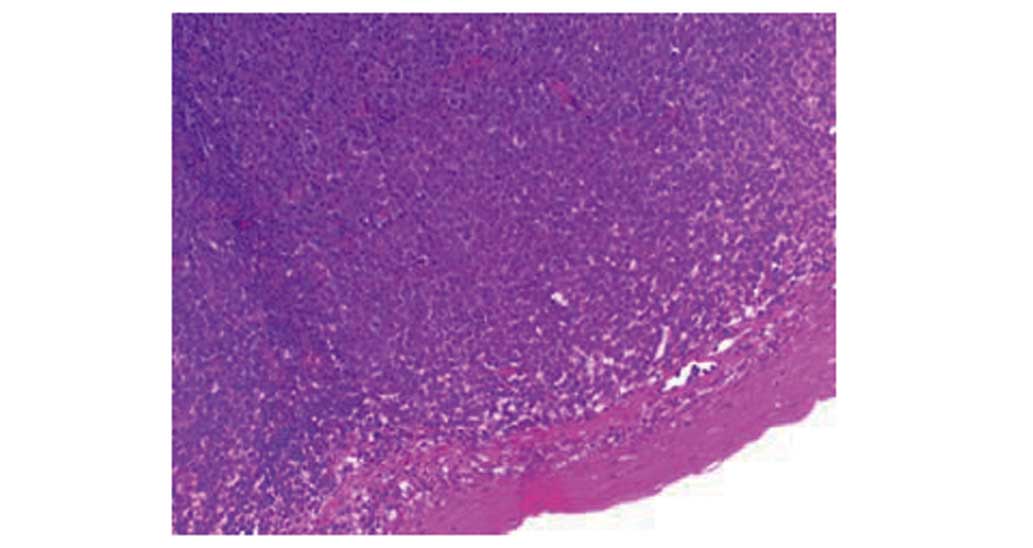
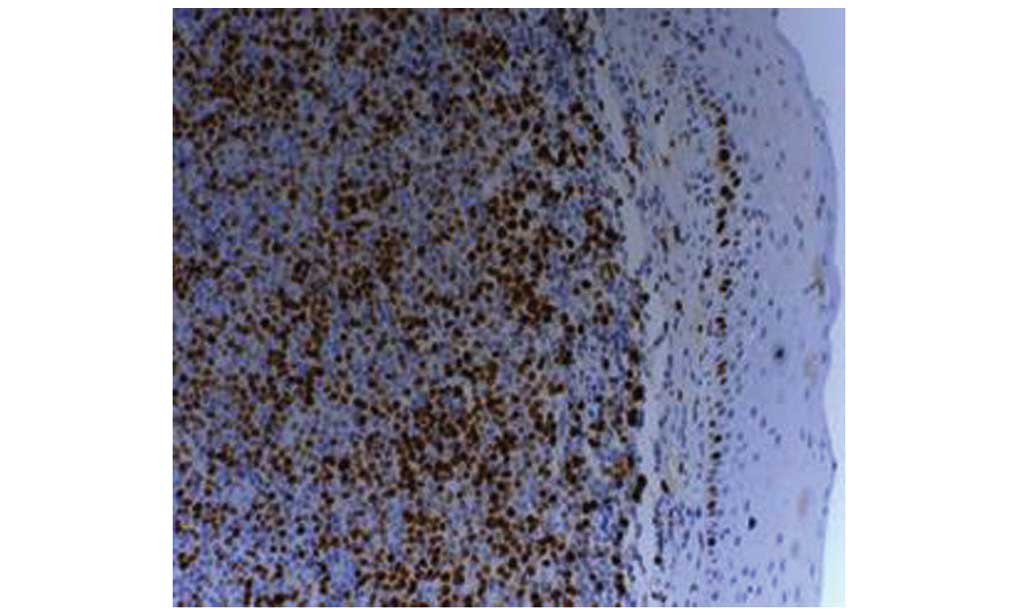
of the cyst base. Pathological and immunophenotypic examination
revealed that CD20, CD19, Bcl-2 and CD10 were positive whereas CD3
was negative. The Ki-67 proliferation index was 85%. Pathological
examination confirmed high-grade diffuse large B-cell lymphoma
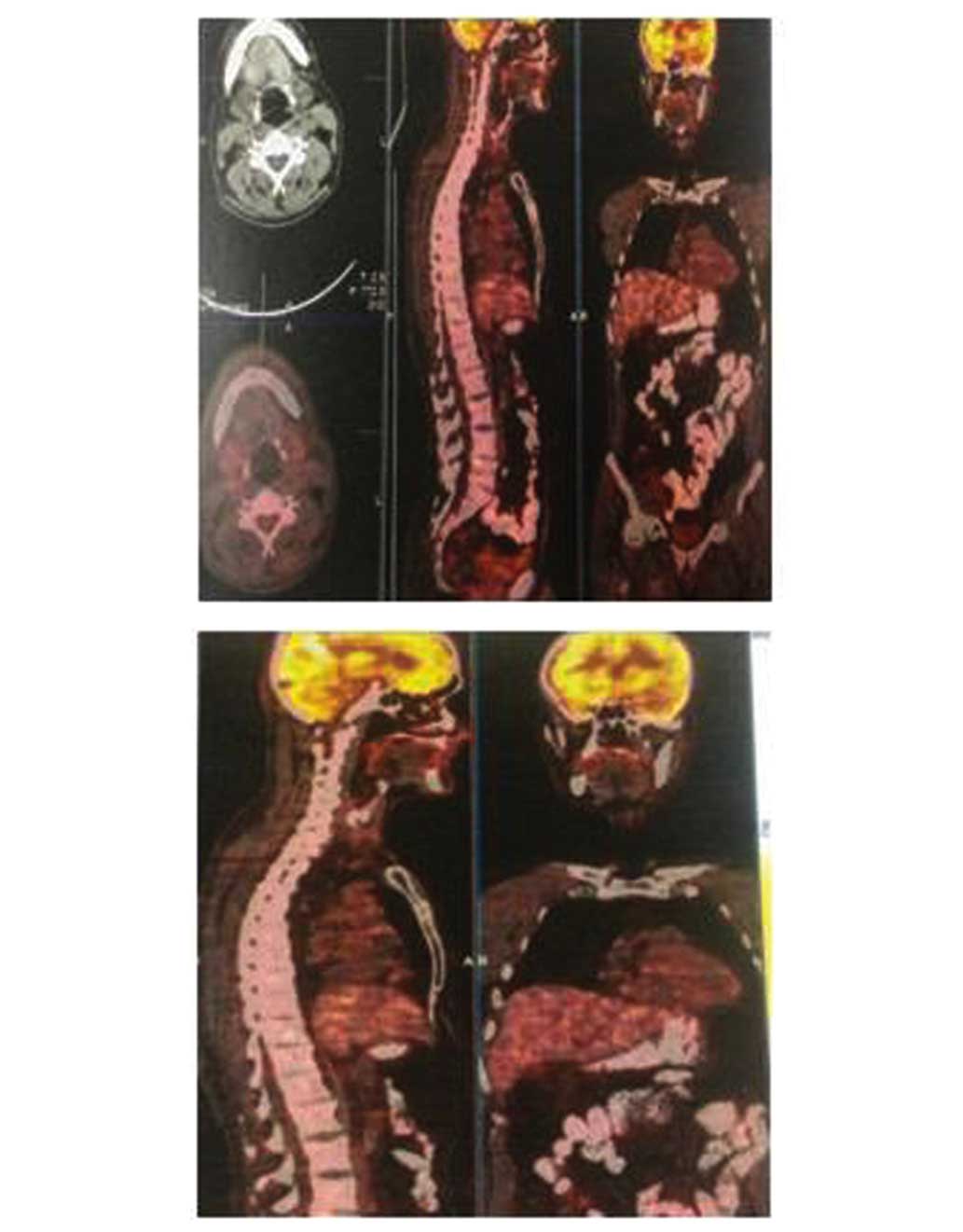
(DLBCL; Figs. 2–4). Pre-treatment positron emission
tomography-computed tomography (PET-CT) using a Siemens Biograph
system (Siemens, Knoxville, TN, USA) demonstrated no focal
involvement (Fig. 5). The patient was
diagnosed with grade 1B DLBCL.
Treatment and follow-up
A four-session rituximab (675 mg/day on day 1),
cyclophosphamide (1,350 mg/day on day 1), doxorubicin (90 mg/day on
day 1), oncovin (1.4 mg/day on day 1) and prednisolone (90 mg/day
on days 1–5) (R-CHOP) multiple chemotherapy regimen followed by
involved-field regional radiotherapy (IFRT) were planned. During
the following 3 months, the four-session (once over a 21 day period
repeated 4 times) R-CHOP chemotherapy and IFRT treatments were
administered without any complications. Follow-up PET-CT imaging
revealed no involvement. No recurrence of the disease was observed
during the 8-month follow-up period.
Discussion
As a lymphoproliferative disease, the occurrence
rate of lymphomas in the oral cavity is 3–5% among all oral
malignancies (1). The most common
location of lymphomas in the oral cavity is Waldeyer's lymphatic
ring, followed by the hard palate, vestibulum and alveoli (3,5). In
Waldeyer's ring, tonsillary (50%), nasopharyngeal and tongue base
involvement is the most common (5).
Isolated non-Hodgkin lymphoma of the tongue base is extremely rare
and the clinical appearance may be a submucosal mass, a polypoid
mass covered with a smooth mucosa or a ulcerated lesion (3,6). In our
case, the tumor was isolated to the tongue base and covered by a
smooth mucosa.
Symptoms of oral lymphomas include pain due to the
effect of the mass, difficulty in speech, and dysphagy or
odinophagy due to ulceration (3,5). The
so-called B-symptoms, including fever, night sweats and weight
loss, are fewer in non-Hodgkin lymphoma compared with Hodgkin
lymphoma, and may not be observed at all (5). In our case, there were no symptoms apart
from sore a throat and the sensation of a foreign body.
There are distinct approaches in the treatment of
oral cavity non-Hodgkin lymphomas. Certain studies suggest multiple
chemotherapy combined with radiotherapy for primary lymphomas of
Waldeyer's ring (2,5,7). A
combined chemotherapy and radiotherapy treatment was also
administered in the present case, and 8 months of follow-up
revealed no recurrence.
In conclusion, although isolated lymphoma of the
base of the tongue is extremely rare, it should always be
considered in patients presenting with a sore throat and the
sensation of a foreign body in the throat. A tongue base
examination should also be performed. Polypoid and cystic masses
covered with a smooth mucosa may mimic benign lesions; thus,
lymphoma should be considered in the differential diagnosis.
References
|
1
|
Lim HJ, Lim JY, Kim YM, Kim CS, Choi SJ,
Yi HG, Choi WG and Lee MH: Primary diffuse large B cell lymphoma of
the base of tongue. J Cancer Res Ther. 8:135–137. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Guastafierro S, Falcone U, Celentano M,
Cappabianca S, Giudice A and Colella G: Primary mantle-cell
non-Hodgkin's lymphoma of the tongue. Int J Hematol. 88:206–208.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Hmidi M, Touiheme N, Elboukhari A, Kettani
M, Elmejareb C and Messary A: Primary B cell lymphoma of the
tongue: a case report. Pan Afr Med J. 12:52012.PubMed/NCBI
|
|
4
|
Terada T: Primary non-Hodgkin B-cell
lymphoma of the tongue. Br J Oral Maxillofac Surg. 49:e18–e19.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Tarhan AE, Akdoğan MV, Haberal AN,
Özlüoğlu LN and Demirhan B: Lymphoma presenting as hypopharynx and
tongue base malıgnancy. KBB-Forum. 3:54–58. 2004.(In Turkish).
|
|
6
|
Jovanovic MB: An exophytic localized
lymphoma of the tongue base. Otolaryngol Head Neck Surg.
139:468–469. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Ezzat AA, Ibrahim EM, El Weshi AN, Khafaga
YM, AlJurf M, Martin JM, Ajarim DS, Bazarbashi SN, Stuart RK and
Zucca E: Localized non-Hodgkin's lymphoma of Waldeyer's ring:
clinical features, management and prognosis of 130 adult patients.
Head Neck. 23:547–558. 2001. View
Article : Google Scholar : PubMed/NCBI
|