Introduction
In patients undergoing chemotherapy for
hematological malignancies, neutropenia severity and duration are
important tools to monitor bone marrow recovery, and may
significantly affect the treatment dose intensity, with a possible
impact on disease prognosis (1). In
this setting, other causes of neutropenia may be difficult to
diagnose, possibly leading to therapy delay and undertreatment.
Chronic neutropenia, lasting >3 months, may be primary
(idiopathic or autoimmune) or secondary to other conditions,
including malignancies, chemicals or radiation exposure (2). The present report describes a case of an
acute promyelocytic leukemia (APL) patient who developed a
long-lasting multifactorial neutropenia [associated with
chemotherapy, autoimmunity and large granular lymphocyte (LGL)
expansion], which was difficult to diagnose due to unusual disease
association, and interfered with the leukemia treatment.
Case report
A 53-year-old male patient was referred to the
outpatient service of Fondazione IRCCS Cà Granda, Ospedale Maggiore
Policlinico (Milan, Italy) in March 2013 due to neutropenia
[absolute neutrophil count (ANC), 1.1×103
cells/mm3; normal range,
1.5–6.5×103/mm3) and severe thrombocytopenia
(18×103 cells/mm3; normal range,
130–400×103/mm3). The medical history was
positive for rheumatic fever in his childhood, prostatic
hypertrophy and chronic autoimmune thyroiditis. In 2004, the
patient had been diagnosed with oligoastrocytoma and had been
treated with chemotherapy (vincristine, procarbazine and
lomustine), obtaining persistent remission. During this period, the
patient had an oxcarbazepine drug-induced neutropenia
(1.2×103 cells/mm3), driven by epilepsy
prophylaxis, which recovered upon substitution for levetiracetam.
The patient's platelets and neutrophil levels during the follow-up
are shown in Fig. 1. Physical
examination at presentation revealed diffuse petechiae and an 8-cm
diameter hematoma on the left gluteus. The liver (aspartate
transaminase/alanine transaminase) and kidney (creatinine) values
were normal, as well as the lactate dehydrogenase levels,
coagulation times and fibrinogen; C reactive protein was increased
(7.75 mg/dl; normal range, <0.5 mg/dl), while hepatitis B and C
virus serology was negative. Anti-platelets autoantibodies were
positive at low titer, suggesting primary immune thrombocytopenia.
Thus, first-line intravenous steroid therapy with
methylprednisolone at 1 mg/kg/day was started, but after 7 days,
the blood counts values further declined [hemoglobin (Hb), 10.7
g/dl; normal range, 13.5–17.5 g/dl; neutrophils, 0.9×103
cells/mm3; and platelets, 19×103
cells/mm3], and the fibrinogen values started to
decrease (99 mg/dl; normal range, 165–350 mg/dl). Bone marrow
aspirate revealed 40% infiltrate of myeloid blasts with immune
phenotype and cytogenetics consistent with APL. Fresh frozen plasma
and platelets transfusion were administered, as well as pathogenic
therapy with all-trans retinoic acid (ATRA) and steroids.
Polymerase chain reaction evaluation was positive for the
promyelocytic leukemia protein/retinoic acid receptor α transcript,
and induction chemotherapy with idarubicin (12 mg/m2) in
addition to ATRA was therefore started. Induction was complicated
by neutropenic fever of unknown origin, requiring antimicrobial
broad-spectrum therapy and granulocyte-colony stimulating factor
(G-CSF). At dischargement (April 15th, 2013), the blood counts had
almost recovered (Hb, 10.2 g/dl; ANC, 1.17×103
cells/mm3; and platelets, 107×103
cells/mm3), and bone marrow evaluation revealed complete
hematologic, morphologic, cytogenetic and molecular response. The
first cycle of consolidation chemotherapy with idarubicin alongside
ATRA was then administered. Due to prolonged moderate neutropenia
(ANCs, 0.74×103 cells/mm3 after 2 months),
levetiracetam was temporary stopped, but no ANCs recovery was
observed. In July 2013, as a spontaneous increase in ANCs values
occurred, a second chemotherapy consolidation course with ATRA and
mitoxantrone was administered, which was complicated by severe
febrile neutropenia (ANCs, 0.05×103
cells/mm3) and controlled by intravenous broad-spectrum
antibiotics and G-CSF. However, in November 2013, severe
neutropenia persisted, thus forcing consolidation chemotherapy
interruption and maintenance with ATRA only. In January 2014, a
mild lymphocytosis (absolute lymphocyte count, 6.5×103
cells/mm3) was observed. Peripheral blood flow cytometry
demonstrated a cluster of differentiation (CD)3+
CD8+ CD57+ phenotype in 99% of lymphocytes,
consistent with T-LGL cells. However, no lymphocyte infiltrate was
observed by bone marrow aspirate and histology on April 2014, and
computed tomography scan was negative for splenomegaly and
lymphadenopathies. In addition, anti-neutrophils antibodies were
positive by direct granulocyte immunofluorescence test and negative
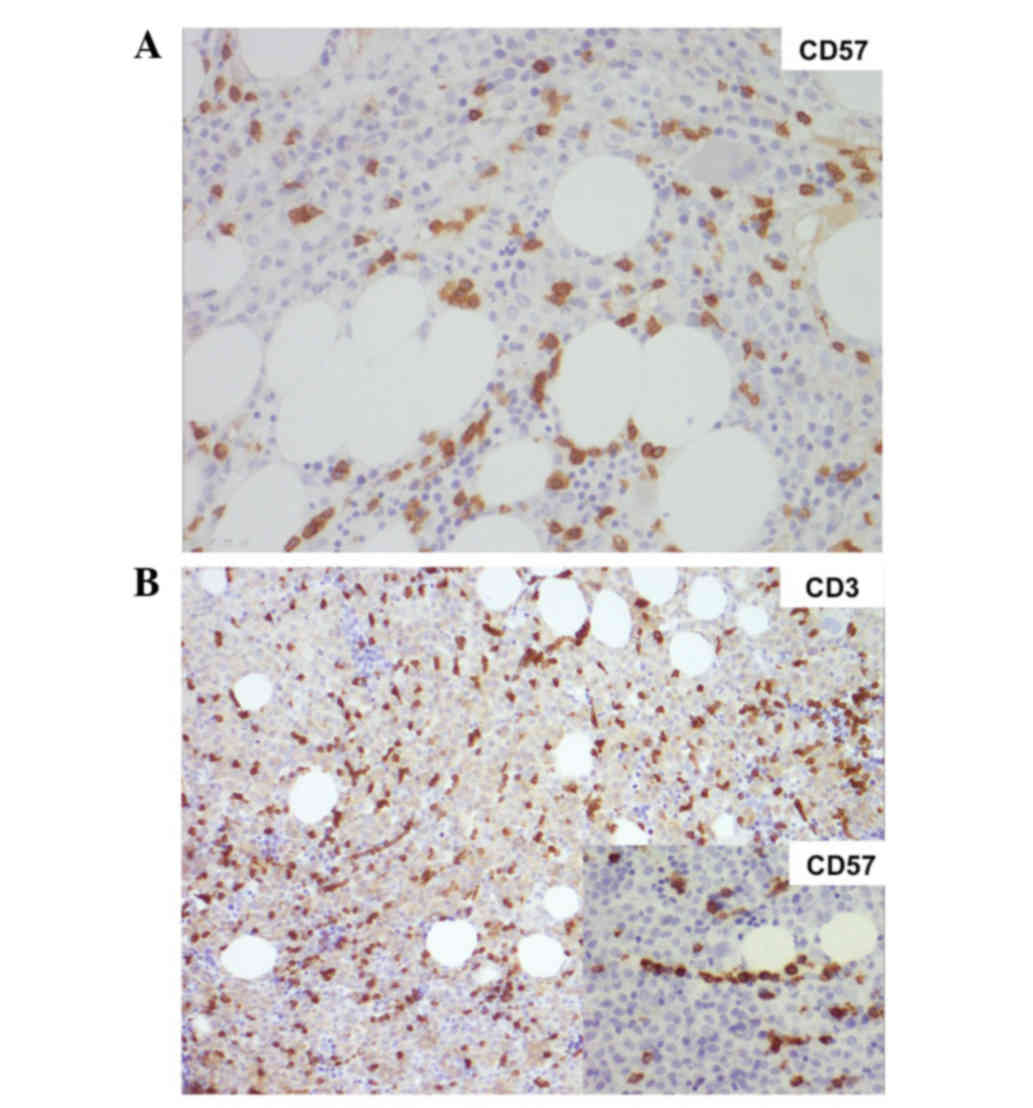
in serum. A year later, bone marrow histology revealed for the
first time a 25% T-LGL infiltrate, consistent with T-LGL chronic
lymphocytic disorder, according to the World Health Organization
criteria (Fig. 2A) (3). From September 2013 to the time of
writing this study, the clinical conditions of the patient remained
stable, with moderate neutropenia and mild LGL lymphocytosis,
without specific therapy (Fig. 1). A
re-evaluation of the bone marrow histology sample obtained at the
time of APL diagnosis was positive for ~10% T-LGL infiltrate, which
was missed at the first pathological evaluation (Fig. 2B).
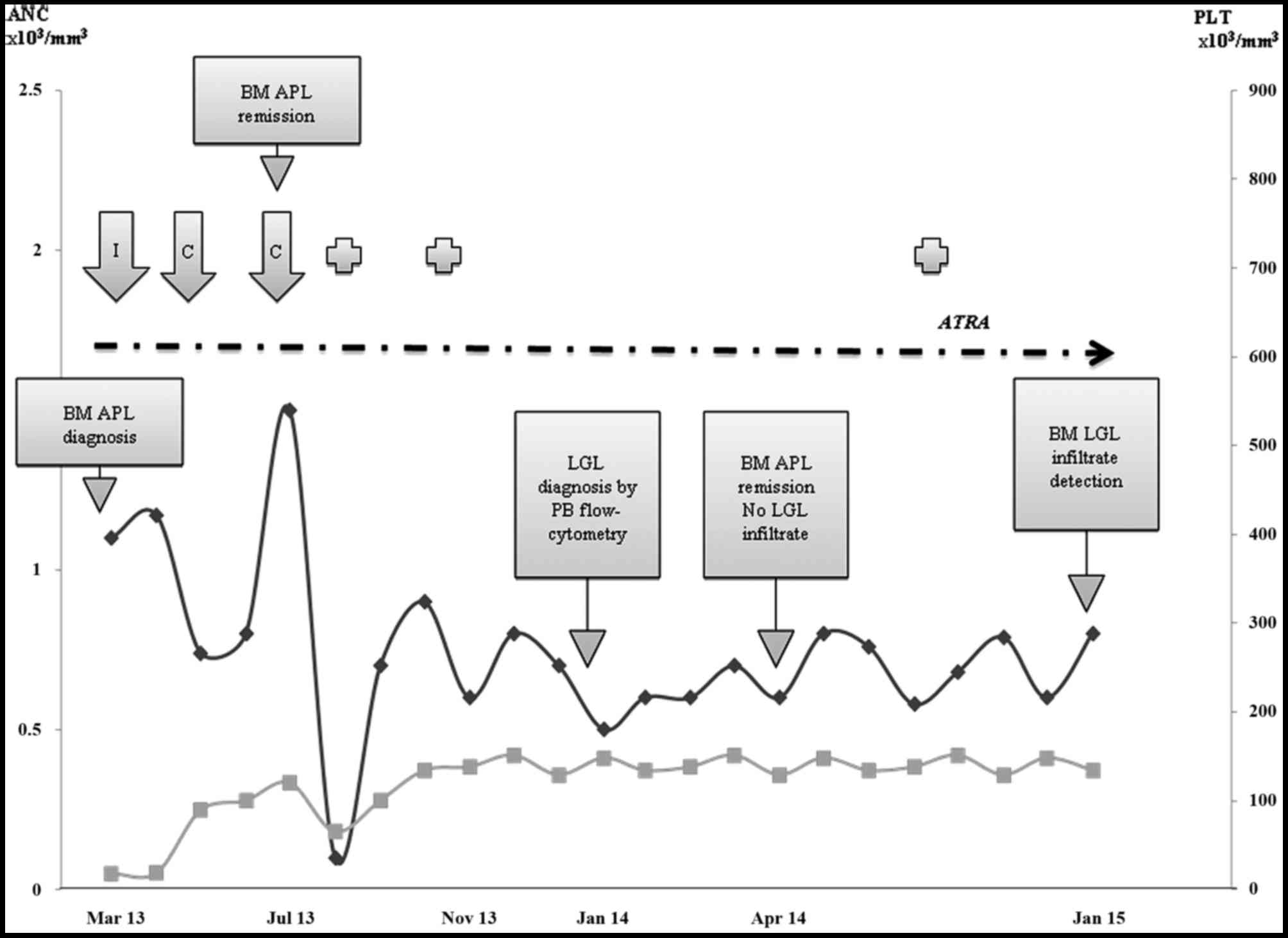 | Figure 1.Patient absolute neutrophil counts
(black line) and platelets (grey line) during the follow-up. Dotted
arrow indicates all-trans retinoic acid treatment, including
induction, consolidation and maintenance. Cross symbol represents
grade 2 infections. ANC, absolute neutrophil counts; BM, bone
marrow; APL, acute promyelocytic leukemia; LGL, large granular
lymphocyte; PB, peripheral blood; ATRA, all-trans retinoic acid;
PLT, platelet; I, induction chemotherapy; C, consolidation
chemotherapy. |
The patient is presently in a good general
condition. Complete remission has been maintained for acute
promyelocytic leukemia for 21 months since the end of therapy, and
the patient undergoes regular clinical check-ups every 6 months.
The patient provided written informed consent.
Discussion
The present study describes a case of three
different causes of cytopenia in the same patient: Acute myeloid
leukemia (AML), autoimmunity and LGL chronic expansion. In
addition, a history of previous chemotherapy and the use of drugs
possibly interfering with ANCs complicated the clinical
setting.
LGL expansion presents with neutropenia in 70–80% of
cases, and it has been reported in ≤35% of patients with idiopathic
cytopenia of uncertain significance (4).
An association between LGL leukemia and solid or
hematological malignancies has been described in various series; in
particular, chronic B-cell dyscrasia is often observed in LGL
patients, including monoclonal gammopathy of undetermined
significance (MGUS), chronic lymphocytic leukemia, monoclonal B
lymphocytosis, hairy cell leukemia and multiple myeloma (5). Additionally, LGL may be associated with
myeloid malignancies such as myelodysplastic syndrome and
myeloproliferative disease (6,7). However,
to the best of our knowledge, the present study is the first report
of an LGL/APL association in the same patient.
Considering the therapeutic approach, no killing was
observed in LGL cells following APL chemotherapy; on the contrary,
LGL clones continued to increase once the marrow leukemic blasts
had been cleared. The prolonged neutropenia observed led to
consolidation and maintenance therapy delay and modification. In
particular, no methotrexate maintenance for APL was administered.
Notably, methotrexate is also used in LGL, and it may have cleared
LGL cells (5). In a recent report of
six LGL/multiple myeloma cases, bortezomib-based therapy was able
to inhibit LGL clones, whereas lenalidomide, which is known to
activate T-natural killer cells, was ineffective (5,6).
In the present case, no LGL specific treatment was
performed. Instead, a patient monitoring approach was preferred due
to the potential side effects of immunosuppression both on
infectious risk and cerebral tumors. Treatment is usually required
in 30–70% of LGL patients due to cytopenia-related manifestations
and/or organomegaly, B symptoms and LGL raising counts (7,8). Notably,
all the infectious episodes observed in the present patient
occurred during induction/consolidation, and were of grade ≤2.
Regarding possible pathogenic mechanisms, it has
been hypothesized that clonal cytotoxic T-cell population could
play a role in antitumor immunosurveillance by controlling
concomitant neoplasia development, as observed in previous MGUS/LGL
cases (5). Otherwise, LGL could
derive from a ‘proliferation escape’ following a chronic immune
response against the concomitant tumor (9). It is difficult to assess whether LGL
expansion is a primary or secondary event, and both conditions have
been described (6). In the present
patient, a posteriori evaluation of the bone marrow
histology from the diagnosis of APL demonstrated that LGL expansion
was already present, suggesting that it may have been an attempt to
control APL tumor growth. Anti-APL chemotherapy and consequent
promyelocytic lysis may have conferred a growing advantage, and may
have ultimately led to a clone expansion of LGL cells. Of note,
there was no peripheral blood lymphocytosis at that time, and a
limited LGL clone is not easy to observe unless specific
immunohistochemistry is performed. Consistently, bone marrow
re-evaluation demonstrated a previously misdiagnosed LGL clone in
patients with chronic idiopathic neutropenia, which subsequently
evolved to LGL chronic expansion (2).
In the patient described in the present case report,
anti-platelets and low titer anti-neutrophils antibodies were
identified at different steps of the disease. Despite the low
sensibility and specificity of the available tests, this may
reflect an immune activation/dysregulation in the course of a
hematological malignancy. Autoantibodies were previously observed
to be positive in several patients, including those with AML. In
particular, antinuclear antibody and anti-DNA positivity were
detected in ≤90% in a study of 39 AML cases (10), and anti-cardiolipin antibodies were
identified in 25 out of 37 AML cases (68%) (11).
In conclusion, in the setting of acute malignancies,
it is important to consider concomitant causes of unexplained
persistent neutropenia. In particular, LGL chronic expansion should
be considered, and ad hoc immunohistochemistry should be performed.
Furthermore, autoimmunity in the context of immune
activation/dysregulation may contribute to the severity of
neutropenia.
References
|
1
|
Morrison VA: Infections in patients with
leukemia and lymphoma. Cancer Treat Res. 161:319–349. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Fattizzo B, Zaninoni A, Consonni D,
Zanella A, Gianelli U, Cortelezzi A and Barcellini W: Is chronic
neutropenia always a benign disease? Evidences from a 5-year
prospective study. Eur J Intern Med. 26:611–655. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Jaffe ES: The 2008 WHO classification of
lymphomas: Implications for clinical practice and translational
research. Hematology Am Soc Hematol Educ Program. 2009:523–531.
2009.
|
|
4
|
Bektas O, Uner A, Aydin SM, Eliacik E, Uz
B, Işık A, Haznedaroğlu IC, Goker H, Sayinalp N, Aksu S, et al:
High frequency of autonomous T-cell proliferation compatible with
T-cell large granular lymphocytic leukemia in patients with
cytopenia of unknown etiology. Int J Hematol. 102:211–217. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Zhang D and Loughran TP Jr: Large granular
lymphocytic leukemia: Molecular pathogenesis, clinical
manifestations, and treatment. Hematology Am Soc Hematol Educ
Program. 2012:652–659. 2012.PubMed/NCBI
|
|
6
|
Cheng J, Talamo G, Malysz J, Ochmann M,
Lamy T and Loughran TP Jr: Report of 6 cases of large granular
lymphocytic leukemia and plasma cell dyscrasia. Clin Lymphoma
Myeloma Leuk. 14:e169–e172. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Lamy T and Loughran TP Jr: How I treat LGL
leukemia. Blood. 117:2764–2774. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Dhodapkar MV, Li CY, Lust JA, Tefferi A
and Phyliky RL: Clinical spectrum of clonal proliferations of
T-large granular lymphocytes: A T-cell clonopathy undetermined
significance? Blood. 84:1620–1627. 1994.PubMed/NCBI
|
|
9
|
Zambello R and Semenzato G: Large granular
lymphocyte disorders: New etiopathogenetic clues as a rationale for
innovative therapeutic approaches. Haematologica. 94:1341–1345.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Kostiala AA, Gripenberg M, Elonen E,
Gripenberg G and Kostiala I: Follow-up of antibodies against
single-stranded DNA in patients with haematological malignancies.
Clin Exp Immunol. 61:15–23. 1985.PubMed/NCBI
|
|
11
|
Lossos IS, BogomolskiYahalom V and Matzner
Y: Anticardiolipin antibodies in acute myeloid leukemia: Prevalence
and clinical significance. Am J Hematol. 57:139–143. 1998.
View Article : Google Scholar : PubMed/NCBI
|