Introduction
Non-medullary thyroid carcinoma (NMTC) originating
from thyroid epithelial cells accounts for >90% of all thyroid
malignancies (1). Patients with NMTC
usually demonstrate a good prognosis, with a 10-year survival rate
of 80–95% (2). However, 4–23% of
patients will present with distant metastases (DM) at the time of
diagnosis or over the course of their disease (3–8). Our
previous study reported a 6.8% rate of DM for all patients with
NMTC who were treated and followed-up at our institution (9). The presence of DM is associated with a
poor prognosis, constituting the most frequent cause of thyroid
cancer-associated mortality (8–10). The
most common sites of DTC metastases are the lungs and the bones,
followed by the brain and the liver (11). While the 10-year survival rate in the
whole population of NMTC patients with DM may reach ~50% (12), intracranial DM are associated with a
median survival time of <1 year (13,14). Data
on the optimal management of brain metastases in this setting and
the factors affecting outcome remain limited. In potentially
curable patients with isolated brain metastases, surgical excision
is indicated, while the administration of 131-iodine therapy for
radioiodine-responsive disease and external-beam radiation therapy
(EBRT) may partially control disease progression in selected
patients. Data regarding the role of systemic therapy with kinase
inhibitors are limited (15).
Furthermore, rates of brain metastases occurrence
may be underestimated. While patients may present with headaches or
various neurological symptoms, intracranial metastasis may be
asymptomatic. According to a previous study, asymptomatic brain
metastases were diagnosed incidentally during systemic brain
imaging prior to prescription of tyrosine kinase inhibitors in
15.4% of patients with NMTC and distant metastases (13). De Figueiredo et al (13) suggested, in agreement with others
(16–19), that surgical intervention, EBRT and
stereotactic radiosurgery (SRS) may prolong survival in this group
of patients.
The aim of the present study was to evaluate a
series of patients with NMTC-associated brain metastases who were
treated and subsequently followed-up at a single tertiary medical
center.
Patients and methods
The electronic database of the Rabin Medical Center
Thyroid Cancer Registry and the Head and Neck Tumor Unit, Beilinson
Hospital (Petach Tikva, Israel) was searched for all patients
diagnosed and treated for NMTC with distant metastases between 1970
and 2014. A total of 10 patients with brain metastases, confirmed
by computerized tomography or magnetic resonance imaging, were
identified and formed the study group. Patients with anaplastic
cancer were excluded. The medical records of the eligible patients
were reviewed for data on clinical characteristics, histological
type of primary tumor, sites of distant metastases, diagnosis and
treatment of brain metastases, time intervals for diagnosis and
treatment of the brain metastasis, disease outcome and
tumor-node-metastasis staging of the thyroid cancer, according to
the American Joint Committee on Cancer (seventh edition) (20). The study protocol was approved by the
Institutional Ethics Board of Rabin Medical Center, Beilinson
Hospital.
Statistical analysis
Categorical variables are presented as numbers and
percentage, and continuous variables as means and standard
deviations or medians with ranges. Categorical variables were
compared using χ2 test, and continuous variables using
unpaired Student's t-test or Mann Whitney U-test, as appropriate.
The product-limit estimate method (Kaplan-Meier) was used to
estimate survival in the cohort of patients with distant
metastases, and the log-rank test was used to compare survival
curves. P<0.05 was considered to indicate a statistically
significant difference. All analyses were conducted using SAS
Software, version 9.4 (SAS Institute, Inc., Cary, NC, USA).
Results
Baseline patient characteristics and
clinicopathological findings
Clinicopathological characteristics of patients are
presented in Table I. Of the 172
patients diagnosed and treated for NMTC with distant metastases
during the study period, 10 (5.8%) possessed brain metastases. This
included 6 female and 4 male patients with a median age of 53.5
years (range, 18–81 years). The median follow-up time from primary
diagnosis was 84 months (7 years; range, 1–25 years). Histological
analysis of the primary tumor revealed papillary thyroid carcinoma
(PTC)-classical variant in 3 patients, and PTC-follicular variant
in 3 patients. The remaining 4 patients exhibited an aggressive
variant, including poorly differentiated and follicular in 2, tall
cell in 1, and insular in 1 patient. Tumor stage was determined to
be pT4 in 5 patients, pT3 in 2 patients, pT2 in 2 patients and
unknown in the remaining patient (20). Extra-thyroidal extension was
documented in 7/9 patients (78%). A total of 6 patients (60%)
demonstrated nodal involvement, and 5 (50%) possessed distant
metastases at diagnosis.
 | Table I.Baseline features and
clinicopathological findings in patients with non-medullary thyroid
carcinoma-associated brain metastases. |
Table I.
Baseline features and
clinicopathological findings in patients with non-medullary thyroid
carcinoma-associated brain metastases.
| Patient no. | Sex | Age, years | Histopathology | Thyroidectomy | RAI | Tumor size, mm | ETE | N1 | M1 | Sequence of
metastasis |
|---|
| 1 | F | 64 | PTC | Yes | Yes | 55 | Yes | Yes | No | Lung>brain |
| 2 | M | 56 | PTC-FV | Yes | Yes | 20 | No | Yes | Lung | Lung>bone,
brain |
| 3 | F | 30 | PTC-FV + poorly
diff. | Yes | Yes | 75 | Yes | No | Lung, bone,
liver | Lung, bone,
liver>brain |
| 4 | F | 32 | Tall cell | Yes (hemi) | Yes | 29 | Yes | Yes | No |
Lung>bone>brain |
| 5 | F | 60 | PTC-FV + poorly
diff. | Yes | Yes | 35 | Yes | No | Bone, lung |
Lung>bone>brain |
| 6 | M | 36 | PTC-FV | Yes | Yes | Uk | Yes | No | No |
Lung>bone>brain |
| 7 | F | 18 | PTC-FV | Yes | Yes | 35 | Yes | Yes | Lung, brain |
|
| 8 | M | 48 | Insular | Yes | Yes | 35 | No | No | No |
Lung>brain>bone |
| 9 | M | 81 | PTC | Yes | Yes | 32 | Yes | Yes | Lung, bones |
Lung>bone>brain |
| 10 | F | 55 | PTC | Yes | Uk | Uk | Uk | Yes | No | Lung>brain |
All 10 patients exhibited associated lung
metastases, which preceded the brain metastases in 9 cases and
occurred synchronously with the brain metastases in 1 case. A total
of 7 patients (70%) demonstrated bone metastases, which preceded
the brain metastases in 5 cases, was synchronous in 1 case and was
metachronous in 1 case. In 1 patient with lung and bone metastases,
liver metastases were also detected, all of which were identified
at initial diagnosis.
Clinical, biochemical and radiological
characteristics of brain metastases
Data on the diagnosis and management of brain
metastases from non-medullary carcinoma are presented in Table II. The median interval from
thyroidectomy to diagnosis of brain metastases was 40 months
(range, 9–207 months). Brain metastases were detected at initial
presentation in 1 patient.
 | Table II.Diagnosis and management of brain
metastases from non-medullary carcinoma. |
Table II.
Diagnosis and management of brain
metastases from non-medullary carcinoma.
|
|
|
|
| Treatment |
|
|
|
|
|---|
|
|
|
|
|
|
|
|
|
|
|---|
| Patient no. | Symptoms | Features | Thyroglobulin,
ng/ml | Surgery | RT | RAI | TKI | Treatment
sequence | Overall follow-up,
months | Follow-up since BM,
months | Last status |
|---|
| 1 | Hemiparesis | >1 cm | <0.2
Ab-positive | Yes | EBRT | Yes | No |
RAI>surgery>RT | 32 | 24 | DOD |
| 2 | None | >1 cm | 1,258 | No | EBRT + SRS | Yes | No | RT>RAI | 60 | 26 | DOD |
| 3 | None | >1 cm, Mf,
Bi | 143,751 | No | SRS | Yes | Yes |
RT>RAI>TKI | 36 | 2 | DOD |
| 4 | Diplopia | >1 cm, Mf,
Bi | 521 | No | EBRT + SRS | No | Yes | RT>TKI | 108 | 4 | DOD |
| 5 | None | <1 cm, Mf,
Bi | 1,496 | No | SRS | No | No | RT | 240 | 32 | AWD |
| 6 | Nausea | >1 cm, Mf,
Bi | Uk | Yes | SRS | No | No | Surgery>RT | 264 | 18 | DOD |
| 7 | Hemiparesis | Uk | Uk | Yes | EBRT | Yes | No |
Surgery>RAI>RT | 300 | 300 | AWD |
| 8 | Hemiparesis | >1 cm | 2,182 | Yes | EBRT | No | No | Surgery>RT | 48 | 15 | DOD |
| 9 | Delirium | >1 cm | 2,800 | No | No | No | No | None | 12 | 2 | DOD |
| 10 | Vertigo,
vomiting | >1 cm | 4.2
Ab-positive | No | EBRT | No | No | RT | 120 | 12 | DOD |
A total of 7 patients presented with neurological
symptoms, primarily motor deficits, followed by nausea, headaches
and delirium. The remaining 3 patients were asymptomatic and the
brain metastases in these cases were diagnosed incidentally by
computed tomography or magnetic resonance imaging during systemic
evaluation of other distant metastases. Additionally, 4 patients
exhibited >1 brain lesion. Macroscopic lesions (≥1 cm) were
identified in 8 patients and bilateral lesions were detected in 4
patients (3 with macroscopic lesions). Brain imaging results from 1
patient (treated in 1990) were unknown. A total of 6 patients
presented with high thyroglobulin levels (threshold value, >0.2
ng/ml) at diagnosis of the brain metastasis (mean, 1,496±874
ng/ml). Positive anti-thyroglobulin antibodies limited the accuracy
of thyroglobulin measurement in 2 patients, and the data were
missing in the remaining 2 patients.
Treatment of brain metastases
The data on treatment and prognosis of brain
metastases are presented in Table
II. Treatment for NMTC consisted of thyroidectomy (total or
hemi) and subsequent radioactive iodine (RAI) in all patients. No
information on RAI were available in the medical chart of patient
no. 10 operated at another hospital. In 4 patients, EBRT was
delivered to the primary tumor bed. Treatment of the brain
metastases consisted of surgery in 4 patients, radiotherapy
delivered directly to the lesion in 8 patients and RAI in 4
patients, alone or in combination. Surgery was combined with EBRT
in 1 patient, with SRS in 1, and with EBRT and RAI in 2. One
patient each underwent only EBRT or SRS, and 1, ERBT + SRS and RAI.
Patient no. 3 received tyrosine kinase inhibitors in combination
with SRS and RAI, and patient no. 4 in combination with
radiotherapy. In patient no. 9, the brain metastases were not
treated due to a poor performance status. The thyroid was confirmed
by histology to be the origin of the brain metastases in 4 patients
following surgical resection.
Disease outcomes
Median overall survival time following diagnosis of
brain metastasis was 15 months (range, 2–59 months). A total of 6
patients survived for >12 months, of whom 2 remained alive at
their last follow-up (duration of follow-up from brain metastases
diagnosis, 32 and 300 months, respectively). Mortality in the
remaining patients was due to progression of the brain lesions in 5
patients and worsening of pulmonary metastases in 3 patients.
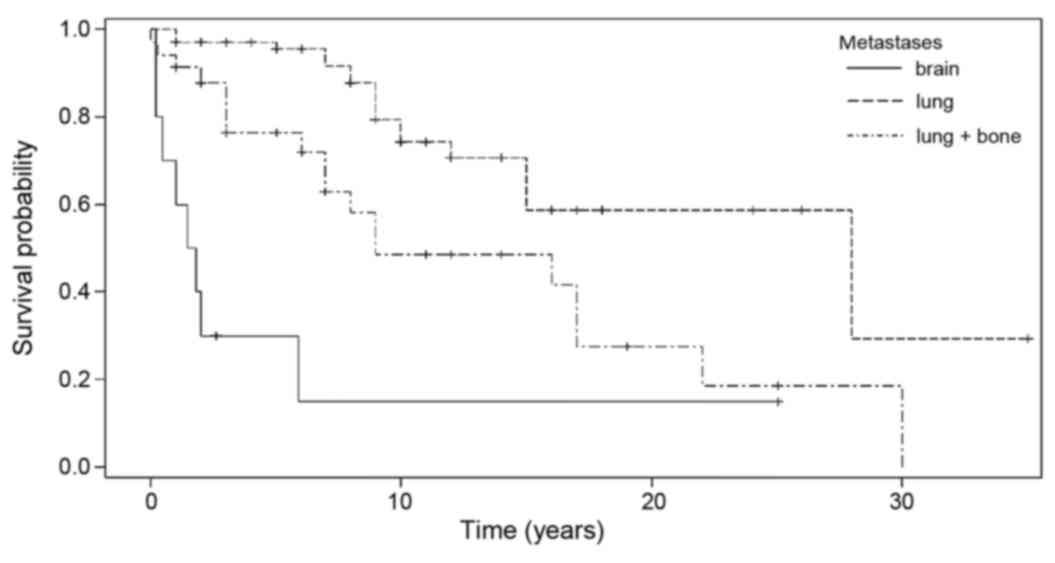
Median survival time was markedly increased in
patients who underwent surgical resection and/or external
radiotherapy (28 months) compared with patients who did not (4
months). The small sample size of the study precluded an analysis
of survival by type of treatment. Mean survival time in the
patients with brain metastases (2.5 years) was significantly
decreased compared with the other patients with NMTC with distant
metastases only in the lungs (20.6 years; P<0.0001) (Fig. 1).
Patient no. 7 (Tables
I and II) was the only patient
in whom brain metastasis was diagnosed prior to diagnosis of the
primary tumor. Following total thyroidectomy and radioiodine
treatment, the patient underwent five neurosurgeries followed by
EBRT. Despite severe disability, the patient received a bachelor's
degree in social work and, at the age of 41 years, successfully
gave birth by caesarean section. She remains alive, after a
follow-up of 25 years.
Discussion
The present study demonstrated that the brain is a
relatively frequent site of secondary metastases in patients with
NMTC and distant metastases, reaching rates of ~6%. This finding is
in agreement with previous studies comprising large cohorts of
>600 patients with NMTC (21–25),
including our previous study (9). In
the present study, all the patients exhibited lung metastases and
the majority also possessed bone metastases. Hematogenic spread of
tumor cells may explain the association observed between
intracranial involvement and lung metastases. Notably, a high rate
of extrathyroidal extension (78%) was observed in this cohort of
patients. As such, clinicians should consider this risk and
investigate the possibility of intracranial involvement as early as
possible in patients with NMTC and distant metastases in order to
minimize clinical deterioration. The considerable proportion (30%)
of asymptomatic brain lesions in the present study justifies the
use of brain imaging in all patients with disseminated disease.
Serum thyroglobulin levels were high (1,496±874
ng/ml) in all patients with brain metastases who were negative for
anti-thyroglobulin antibodies, confirming the differentiated nature
of the thyroid cancer. Practically, however, a high thyroglobulin
level is a problematic indicator to suspect brain metastases given
that all the patients in the present study had distant metastases
in other sites. For the same reason, high serum thyroglobulin
levels cannot serve as an indicator of response to therapy.
The median survival time of 15 months in the present
cohort is longer compared with those reported in other studies,
namely 7.1 months (13), 9.4 months
(25) and 12.4 months (24). This difference in survival time may be
attributable to the relatively young age of the patients in the
present study (median, 53.5 years) compared with those in previous
studies (with median ages of 59 and 63 years) (13,17,24,26),
the exclusion of patients with anaplastic-type cancer from the
present study, and the aggressive treatment approach employed in
the present study. For example, patient no. 7 underwent five
neurosurgeries in addition to EBRT and RAI. The use of stereotactic
radiotherapy in patients with a limited number of brain foci has
been increasing, because it allows for the delivery of a large dose
to the target mass while minimizing damage to normal brain tissue
(17). Treatment with SRS alone or in
addition to whole-body radiation therapy has been demonstrated to
achieve a local control rate of 96% without any
procedure-associated complications (18). In the present study cohort, the
patients who were treated for brain metastases with surgery and/or
radiation achieved a longer survival time compared with untreated
patients (patient nos. 4 and 9), similar to previous studies
(13,17,18). In a
recent study by Choi et al (26), the median overall survival time
following diagnosis of brain metastases was 16.7 months in treated
patients compared with 2.6 months in untreated patients.
The results of the present study should be
interpreted with caution due to the retrospective design of the
study and the inclusion of only a small sample of patients from a
single institution. However, due to the rarity of NMTC with brain
metastases and the lack of data from prospective studies,
management decisions currently rely on case reports and
retrospective studies (23). The
present study is of interest due to the improved outcome achieved
in the aggressively treated patients, the high association observed
between brain metastases and lung metastases in NMTC and the high
incidence of incidentally diagnosed brain metastases.
In conclusion, the present study demonstrates that a
higher-than-expected proportion of patients with lung and bone
metastases from NMTC also exhibit brain metastases. Therefore,
systemic screening should be considered for all patients with
disseminated NMTC. Surgical resection of all operable metastatic
lesions with multidisciplinary adjuvant treatment is critical to
improve patient survival.
References
|
1
|
Chen AY, Jemal A and Ward EM: Increasing
incidence of differentiated thyroid cancer in the united states,
1988–2005. Cancer. 115:3801–3807. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Schlumberger MJ: Papillary and follicular
thyroid carcinoma. N Engl J Med. 338:297–306. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Massin JP, Savoie JC, Garnier H, Guiraudon
G, Leger FA and Bacourt F: Pulmonary metastases in differentiated
thyroid carcinoma. Study of 58 cases with implications for the
primary tumor treatment. Cancer. 53:982–992. 1984. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Ruegemer JJ, Hay ID, Bergstralh EJ, Ryan
JJ, Offord KP and Gorman CA: Distant metastases in differentiated
thyroid carcinoma: A multivariate analysis of prognostic variables.
J Clin Endocrinol Metab. 67:501–508. 1988. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Casara D, Rubello D, Saladini G, Gallo V,
Masarotto G and Busnardo B: Distant metastases in differentiated
thyroid cancer: Long-term results of radioiodine treatment and
statistical analysis of prognostic factors in 214 patients. Tumori.
77:432–436. 1991.PubMed/NCBI
|
|
6
|
Samaan NA, Schultz PN, Haynie TP and
Ordonez NG: Pulmonary metastasis of differentiated thyroid
carcinoma: Treatment results in 101 patients. J Clin Endocrinol
Metab. 60:376–380. 1985. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Jonklaas J, Sarlis NJ, Litofsky D, Ain KB,
Bigos ST, Brierley JD, Cooper DS, Haugen BR, Ladenson PW, Magner J,
et al: Outcomes of patients with differentiated thyroid carcinoma
following initial therapy. Thyroid. 16:1229–1242. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Lang BH, Wong KP, Cheung CY, Wan KY and Lo
CY: Evaluating the prognostic factors associated with cancer
specific survival of differentiated thyroid carcinoma presenting
with distant metastasis. Ann Surg Oncol. 20:1329–1335. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Hirsch D, Levy S, Tsvetov G, Gorstein A,
Slutzky-Shraga I, Akirov A, Robenshtok E, Shimon I and Benbassat
CA: Long term outcomes and prognostic factors in patients with
differentiated thyroid cancer and distant metastases. Endocr Pract.
13–Jul;2017.(Epub ahead of print). View Article : Google Scholar
|
|
10
|
Dinneen SF, Valimaki MJ, Bergstralh EJ,
Goellner JR, Gorman CA and Hay ID: Distant metastases in papillary
thyroid carcinoma: 100 cases observed at one institution during 5
decades. J Clin Endocrinol Metab. 80:2041–2045. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Hoie J, Stenwig AE, Kullmann G and
Lindegaard M: Distant metastases in papillary thyroid cancer. A
review of 91 patients. Cancer. 61:1–6. 1988. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Clark JR, Lai P, Hall F, Borglund A, Eski
S and Freeman JL: Variables predicting distant metastases in
thyroid cancer. Laryngoscope. 115:661–667. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
de Figueiredo B Henriques, Godbert Y,
Soubeyran I, Carrat X, Lagarde P, Cazeau AL, Italiano A, Sargos P,
Kantor G, Loiseau H and Bonichon F: Brain metastases from thyroid
carcinoma: A retrospective study of 21 patients. Thyroid.
24:270–277. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Samuel AM and Shah DH: Brain metastases in
well-differentiated carcinoma of the thyroid. Tumori. 83:608–610.
1997.PubMed/NCBI
|
|
15
|
Haugen BR, Alexander EK, Bible KC, Doherty
GM, Mandel SJ, Nikiforov YE, Pacini F, Randolph GW, Sawka AM,
Schlumberger M, et al: 2015 American thyroid association management
guidelines for adult patients with thyroid nodules and
differentiated thyroid cancer: The american thyroid association
guidelines task fork on thyroid nodules and differentiated thyroid
cancer. Thyroid. 26:1–133. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Salvati M, Frati A, Rocchi G, Masciangelo
R, Antonaci A, Gagliardi FM and Defini R: Single brain metastasis
from thyroid cancer: Report of twelve cases and review of the
literature. J Neurooncol. 51:33–40. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Bernard DM, Sperduto PW, Souhami L, Jensen
AW and Roberge D: Stereotactic radiosurgery in the management of
brain metastases from primary thyroid cancers. J Neurooncol.
98:249–252. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Kim IY, Kondziolka D, Niranjan A,
Flickinger JC and Lunsford LD: Gamma knife radiosurgery for
metastatic brain tumors from primary thyroid cancers. J Neurooncol.
93:355–359. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
McWilliams RR, Giannini C, Hay ID,
Atkinson JL, Stafford SI and Buckner JC: Management of brain
metastases from thyroid carcinoma: A study of 16 pathologically
confirmed cases over 25 years. Cancer. 98:356–362. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Edge S and Compton C: The american joint
committee on cancer: The seventh edition of the AJCC cancer staging
manual and the future of TNM. Ann Surg Oncol. 17:1471–1474. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Kim KM, Park JB, Bae KS and Kang SJ:
Analysis of prognostic factors in patients with multiple
recurrences of papillary thyroid carcinoma. Surg Oncol. 21:185–190.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Nixon IJ, Whitcher MM, Palmer FL, Tuttle
MR, Shaha AR, Shan JP, Patel SG and Ganly I: The impact of distant
metastases at presentation on prognosis in patients with
differentiated carcinoma of the thyroid gland. Thyroid. 22:884–889.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Hay ID: Brain metastases from papillary
thyroid carcinoma. Arch Intern Med. 147:607–611. 1987. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Chiu AC, Delpassand ES and Sherman SI:
Prognosis and treatment of brain metastases in thyroid carcinoma. J
Clin Endocrinol Metab. 82:3637–3642. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Misaki T, Iwata M, Kasagi K and Konishi J:
Brain metastases from differentiated thyroid cancer in patients
treated with radioiodine for bone and lung lesions. Ann Nucl Med.
14:111–114. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Choi J, Kim JW, Keum YS and Lee IJ: The
largest known survival analysis of patients with brain metastasis
from thyroid cancer based on prognostic groups. PLoS One.
11:e01547392016. View Article : Google Scholar : PubMed/NCBI
|