Introduction
Breast cancer is the leading cause of cancer
mortality among females in China, and the incidence of breast
cancer is increasing continuously. Metastasis is the most important
factor that leads to treatment failure and mortality (1). Epithelial-mesenchymal transition
(EMT) and vascularization are known to be key factors in tumor
invasion and metastasis (2).
Vascular endothelial growth factor (VEGF) and matrix
metalloproteinases (MMPs) play important roles in EMT. MMPs promote
tumor invasion and metastasis in breast cancer, thus, facilitate
the departure of epithelial cells from their surrounding tissue.
The underlying mechanisms include the degradation of the
extracellular matrix and intercellular contacts by MMPs (3). A previous study demonstrated that
MMP-9 can accelerate tumor metastasis by promoting
neovascularization and lymphangiogenesis (4). VEGF is also considered to be an
important and effective factor in stimulating vascularization,
which participates in tumor invasion and metastasis (5). A number of studies have described a
correlation between VEGF and MMP-9 levels (6). However, the value of combined
detection of VEGF and MMP-9 levels in breast cancer remains
unclear. Therefore, the aim of the present study was to determine
whether the combined detection of VEGF and MMP-9 is valuable for
the diagnosis, treatment and prognosis of breast cancer. For this
purpose, the levels of VEGF and MMP-9 were compared among breast
cancer patients, fibroadenoma patients and healthy adults using a
lipid-chip based method.
Patients and methods
Patients
A total of 301 breast cancer patients, 83
fibroadenoma patients and 40 healthy adults without
breast-associated diseases were enrolled in the study. All the
cases were female and had been diagnosed between September 2011 and
December 2012 in Jiangsu Province Cancer Hospital (Nanjing, China).
Blood samples were collected from the 301 breast cancer patients,
of which the postoperative pathology was infiltrative ductal
carcinoma (IDC), prior to surgery or any other therapy. Blood
samples were also collected postoperatively from 118 of the 301
patients. The 301 breast cancer patients were aged between 27 and
80 years, with a median age of 51 years. The 118 patients who
underwent surgery had an age range of 28–80 years and the median
age was 51 years. In the fibroadenoma group, the 83 patients were
aged between 19 and 58 years, with a median age of 27 years, while
the 40 healthy adults had an age range of 19–48 years and a median
age of 28 years. According to the Tumor, Node, Metastasis (TNM)
staging criteria from the Union for International Cancer Control
(7th edition) (7), the 301 breast
cancer patients comprised 125 phase I cases, 58 phase II cases, 98
phase III cases and 20 stage IV cases, among which 127 patients
were diagnosed with lymph node metastasis, 166 patients were
without lymph node metastasis and in eight cases, the status of the
lymph node was not detected (without axillary lymph node
dissection). All patients provided informed consent. The
participants serum was obtained by the Ethics Committee of Jiangsu
Cancer Hospital (Nanjing, China) following approval.
Collection and preservation of the
specimens
Venous fasting blood samples (3 ml) were collected
and placed in test tubes without endotoxin or pyrogen. The tubes
were shaken three times and then left at room temperature for 30
min in order for coagulation to occur. The samples were centrifuged
for 10 min at 1,000 × g and the blood serum was extracted and
stored in a refrigerator at −80°C for further analysis. Blood
samples from the breast cancer and fibroadenoma patients were
collected prior to surgery or any other therapy. In the 118 breast
cancer patients that underwent surgery, the blood samples were
collected one month following surgery.
Reagents
Test detection was performed using Luminex
multiplexed assays. FLEXMAP 3D® system consists was
provided by Luminex Corporation (Austin, TX, USA). A Human
Cytokine/Chemokine and Human CVD Panel I kit (Millipore, Billerica,
MA, USA) was used to detect the levels of serum VEGF and MMP-9.
Experimental procedures
For the main experimental procedure of VEGF and
MMP-9, all the above reagents needed to warm to room temperature
(about 20 to 25°C) prior to be used. The placement of standards of
VEGF was 0 (background), 3.2, 16, 80, 400, 2,000 and 10,000 pg/ml
while of MMP-9 was 0 (background), 0.016, 0.08, 0.4, 2.0, 10.0,
50.0 ng/ml, then controls and test specimens were added to the
plate (25 μl per well). The aforementioned procedures were
conducted on ice. Next, 25 μl assay buffer was added to each well.
The specimens were shaken at room temperature; VEGF for 16 h and
MMP-9 for 2 h, ensuring that the procedures were conducted away
from the light. Following washing twice, 25 μl detection antibody
was respectively added to each well and the plates were shaken for
1 h at room temperature. Next, 50 μl
streptavidin-biotin-phycoerythrin medium was added per well and the
specimens were shaken again at room temperature for 30 min. Washed
them twice with wash buffer and sheath fluid (150 μl for VEGF and
100 μl for MMP-9) with 200 μl per well. Added the lotion to the
board after washed it twice. The plates were run with the FLEXMAP
3D™ system and in order to calculate the samples concentration, the
median fluorescence intensity results were analyzed by a weighted
five-parameter logistic method. Three independent experiments were
performed.
Quantitative detection of the protein
levels
It needed warm-up before for 30 min. Instrument
parameters were set as follows: Events, 50; gate, 8,000–15,000;
sample sizes, VEGF 100 μl and MMP-9 50 μl; time out, 60 sec; bead
regions, VEGF 86 and MMP-9 27. The specimens were placed in a
detecting pool, running procedures related to the operation.
Microspheres median fluorescence readings were analyzed using
xPONENT® 4 software (Luminex Corporation) to obtain the
final result. Three independent experiments were performed.
Statistical analysis
Statistical analysis was conducted using SPSS
version 20.0 (IBM, Armonk, NY, USA). As statistical analysis
revealed the data to have a skewed distribution, non-parametric
tests were selected. Comparisons between two groups were performed
using the independent samples Mann-Whitney U test, while
independent samples Kruskal-Wallis one-way analysis of variance was
used for multiple group comparisons. Spearman’s ρ was used to
analyze the correlation between two factors, where r≥0.8 was
considered to indicate a highly significant correlation,
0.5≤r<0.8 was considered to indicate a moderate correlation,
0.3≤r<0.5 was considered to indicate a low correlation and
r<0.3 was considered to indicate a weak or irrelevant
correlation. P<0.05 was considered to indicate a statistically
significant result.
Results
Serum VEGF and MMP-9 levels in the
pretreatment groups of IDC, patients with breast fibroadenoma and
healthy controls
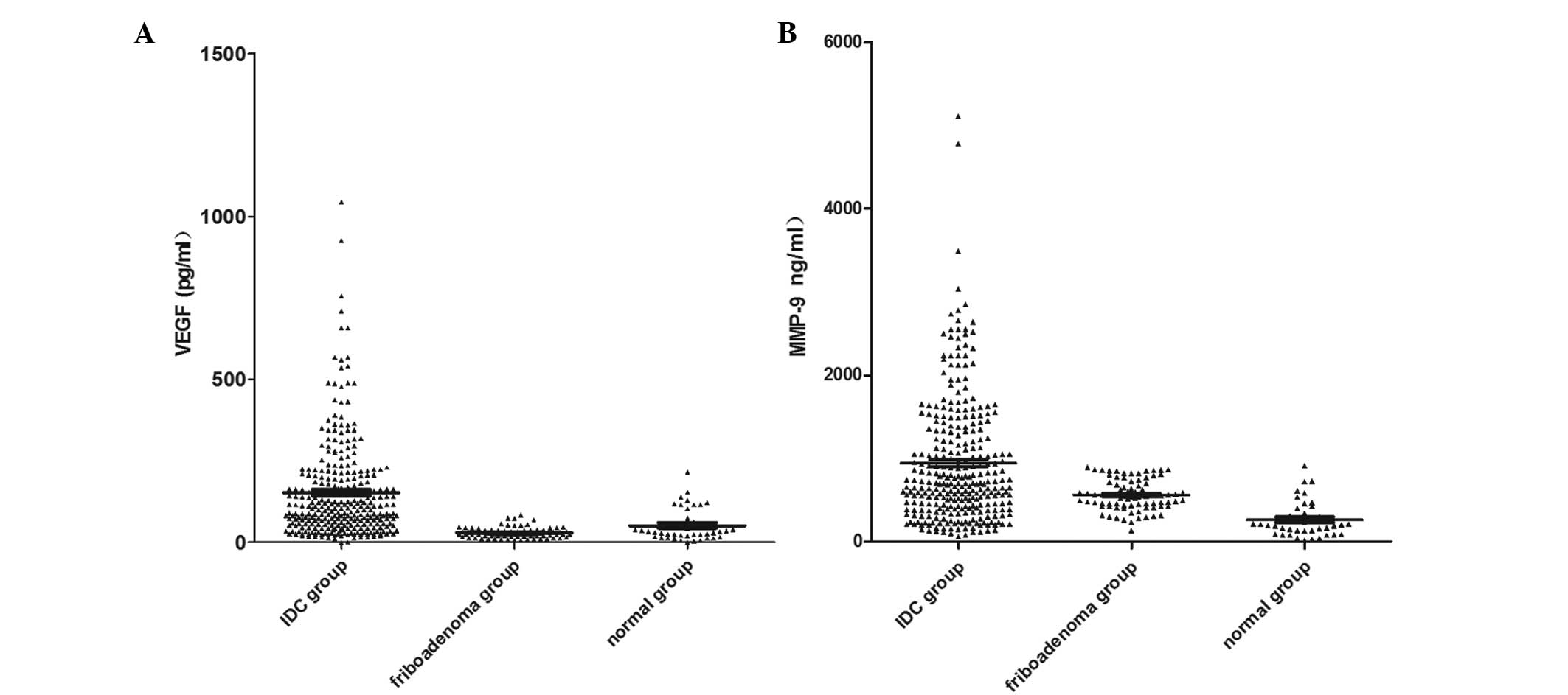
Mean levels of serum VEGF and MMP-9 were
significantly higher in the breast cancer patients when compared
with the levels in the breast fibroadenoma patients and the healthy
controls (Table I; Fig. 1).
 | Table ISerum VEGF and MMP-9 levels in IDC and
breast fibroadenoma patients and healthy adults. |
Table I
Serum VEGF and MMP-9 levels in IDC and
breast fibroadenoma patients and healthy adults.
| Group | VEGF (pg/ml) | MMP-9 (ng/ml) |
|---|
| IDC | 152.76
(<0.025-1044) | 945.09 (63-5112) |
| Preoperative
(n=301) | 180.89 (1-926) | 903.92
(115-3495) |
| Postoperative
(n=118) | 135.26 (6-676) | 680.36 (67-2348) |
| Fibroadenoma
(n=83) | 29.86 (7-84) | 563.59 (135-895) |
| Healthy adults
(n=40) | 52.45
(<0.025-215) | 267.33 (19-916) |
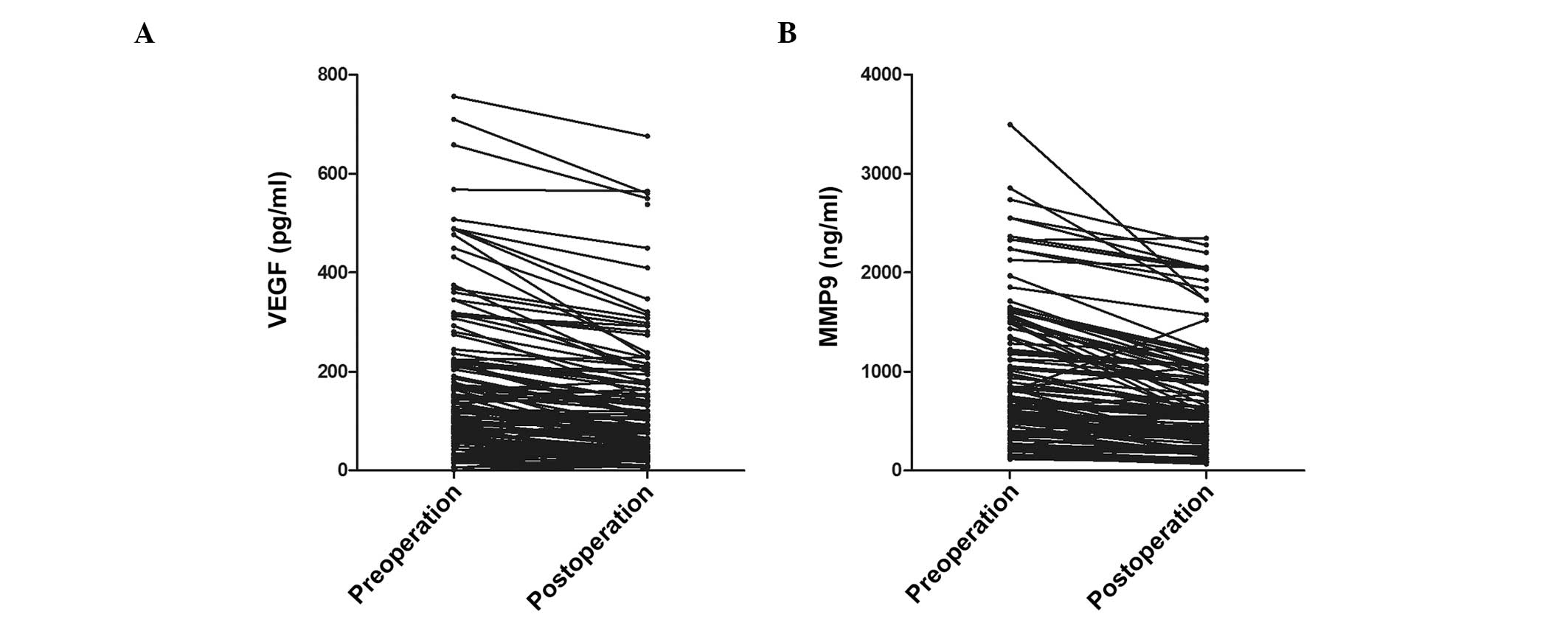
The pre-operation and post-operation levels of VEGF
and MMP-9 were detected respectively. Compared with the
pre-operation group, the levels of VEGF and MMP-9 were all
significantly decreased following surgery. [VEGF: 180.89±167.82 vs.
135.26±131.20 (P<0.05); MMP-9: 903.92±704.76 vs. 680.36±551.77
(P<0.05)] (Fig. 2).
Correlation between serum VEGF and MMP-9
levels and clinicopathological parameters in the pretreatment group
of IDC analysis
The association between serum VEGF and MMP-9 levels
with clinicopathological characteristics in IDC patients (Table II) was analyzed. Serum levels of
VEGF and MMP-9 were closely associated with tumor size
(P<0.001), and the serum levels in patients with stage III or IV
breast cancer were significantly higher than those classified as
TNM stage I or II (P<0.001). In addition, the protein levels of
VEGF and MMP-9 in patients with lymph node metastasis were
significantly higher than those without lymph node metastasis
(P<0.001). However, the serum levels of VEGF and MMP-9 exhibited
no statistically significant difference between the different age
groups in the breast cancer patients (P>0.05).
 | Table IIAssociation between serum MMP-9 and
VEGF levels with clinicopathological characteristics of IDC
patients. |
Table II
Association between serum MMP-9 and
VEGF levels with clinicopathological characteristics of IDC
patients.
| Characteristics | Cases (n) | VEGF (pg/ml) | P-value | MMP-9 (ng/ml) | P-value |
|---|
| Tumor size (cm) | | | <0.001 | | <0.001 |
| <2 | 133 | 96.55 (1-345) | | 524.71 (63-2553) | |
| <5≥2 | 114 | 158.61
(<0.025-1044) | | 1051.40
(101-5112) | |
| ≥5 | 54 | 278.89 (13-926) | | 1756.00
(392-4786) | |
| Clinical stage (UICC
7th) | | | <0.001 | | <0.001 |
| I | 125 | 86.12 (0-488) | | 413.05 (63-833) | |
| II | 58 | 106.14 (10-281) | | 682.33
(125-1377) | |
| III | 98 | 207.2 (13-1044) | | 1435.35
(533-3041) | |
| IV | 20 | 295.55 (52-926) | | 2630.05
(1035-5112) | |
| Lymph node
metastasis | | | 0.001 | | <0.001 |
| Negative | 166 | 93.62 (0-1044) | | 475.77 (63-1377) | |
| Positive | 127 | 231.07 (13-926) | | 1566.80
(445-5112) | |
| Missing | 8 | 136.88 (1-319) | | 813.88
(238-2337) | |
| Age (years) | | | 0.53 | | 0.104 |
| <35 | 21 | 122.38 (10-345) | | 783.38
(125-2553) | |
| <50≥35 | 116 | 154.22 (13-756) | | 1006.11
(82-4786) | |
| ≥50 | 164 | 155.62 (0-1044) | | 922.63 (63-5112) | |
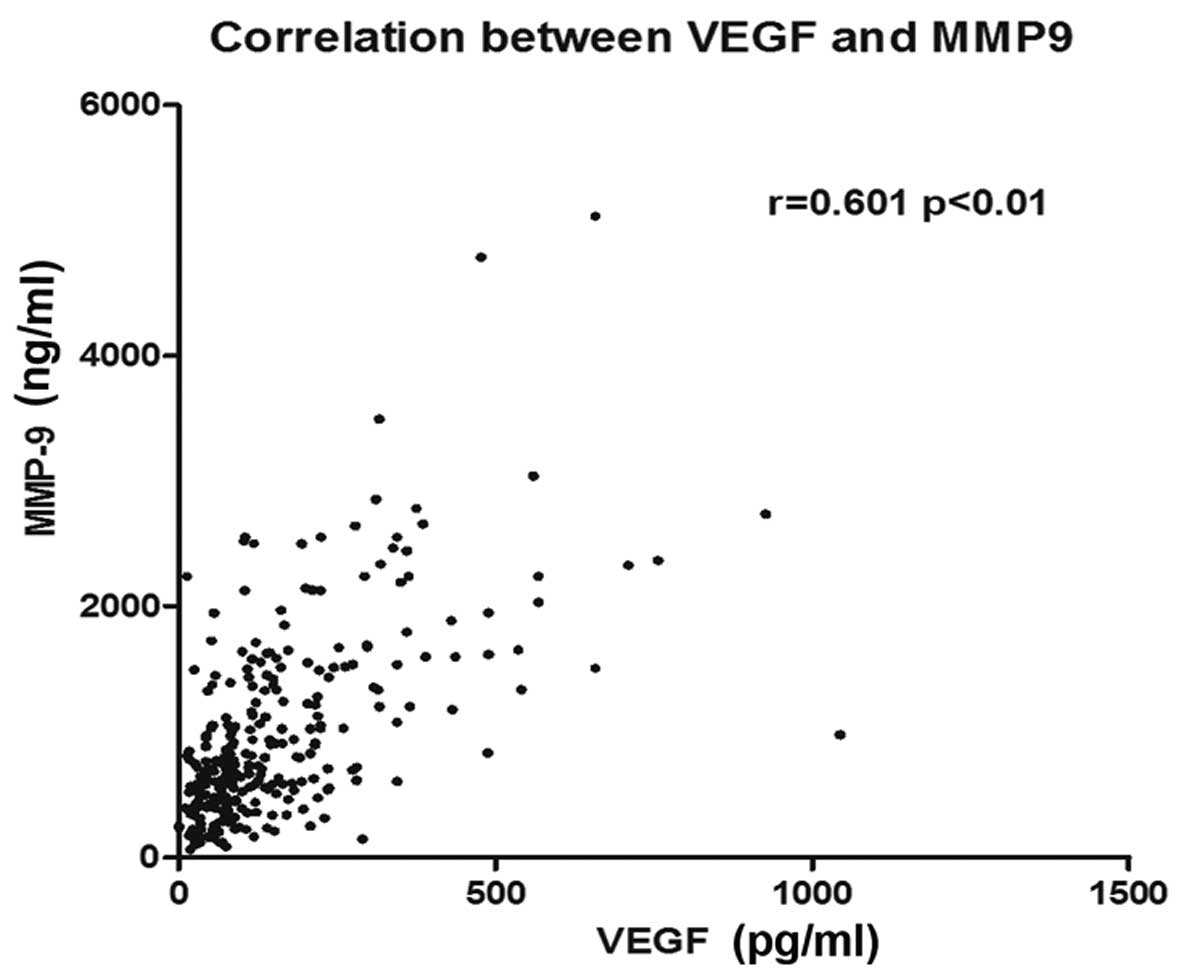
Spearman’s ρ analysis revealed a significant
positive correlation between the serum level of VEGF and serum the
level of MMP-9 (Fig. 3; r=0.601,
P<0.001).
Diagnostic value of VEGF and MMP-9 in the
pretreatment group of NIDC
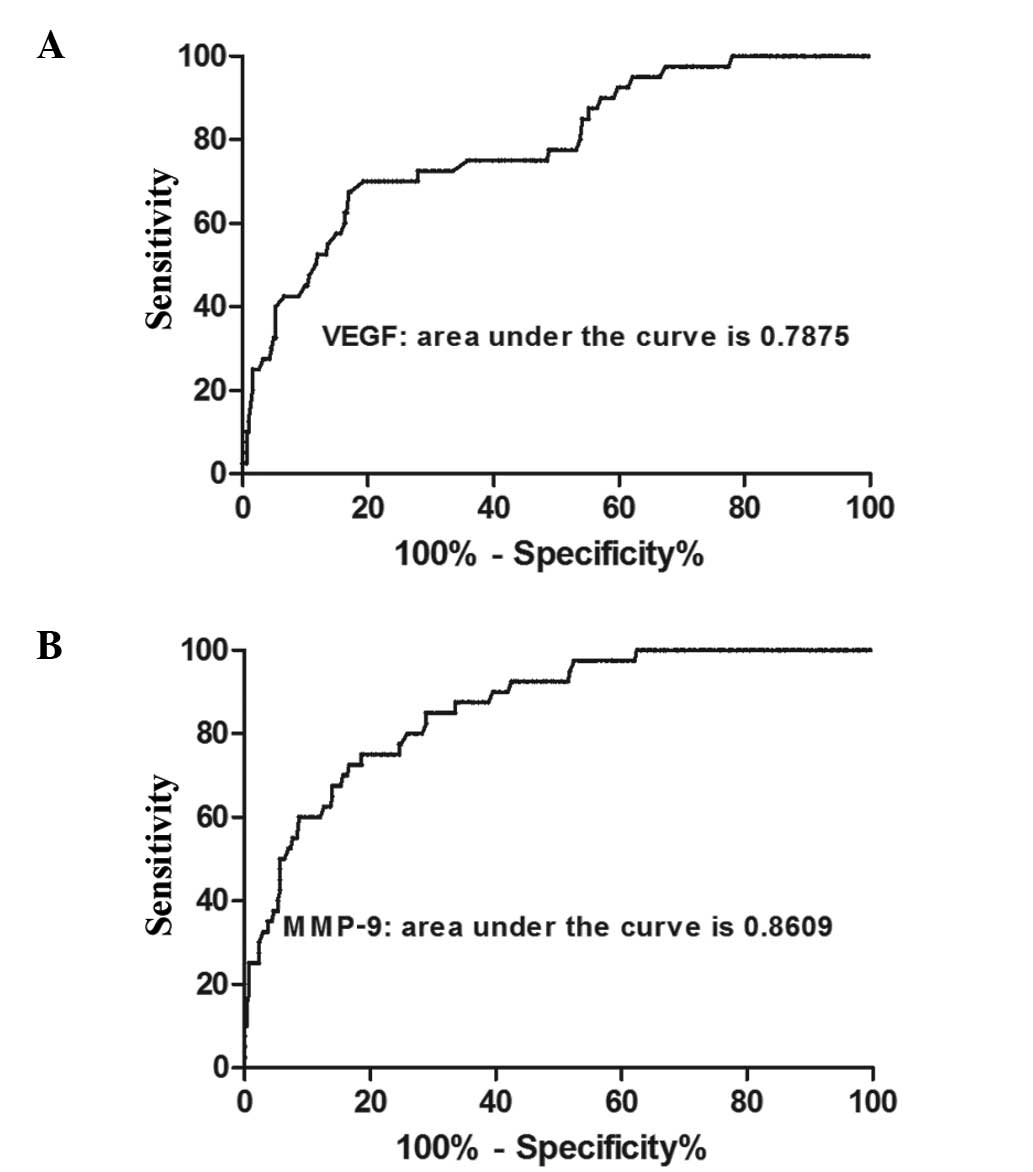
Receiver operating characteristic (ROC) curve
analysis (Fig. 4) revealed the
area under the ROC curve for VEGF was 0.788 (95% confidence
interval, 0.711–0.864), whereas for MMP-9, the area under the ROC
curve was 0.861 (95% confidence interval, 0.806–0.916). Thus, serum
VEGF and MMP-9 levels may be used as markers for the diagnosis of
breast IDC.
Discussion
Angiogenesis is known to be closely associated with
carcinogenesis and tumor development. Neovascularization provides
oxygen and nutrients to tumor cells, and endothelial cells can
promote cell growth in breast carcinoma via paracrine signaling and
the production of carcinogenesis promoters (8). Neovascularization of tumors is the
result of the dynamic equilibrium between two groups of factors
that promote and inhibit vascularization. VEGF is potent in
promoting vascularization (9,10).
It is an endothelial cell specific mitogen that markedly increases
vascular permeability by binding to vascular endothelial growth
factor receptor (VEGFR)-2. When VEGF binds to VEGFR-3, VEGF
activates the Ras/mitogen-activated protein kinase (MAPK) and
related adhesion focal tyrosine kinase signaling transduction
pathways, which promotes lymphangiogenesis of the tumor (11–13).
MMP-9 promotes vascularization of the tumor by upregulating the
bioavailability of VEGF. In addition, MMP-9 can regulate the
stability and permeability of newly formed tumor vessels (14).
In the present study, the levels of VEGF and MMP-9
were compared among IDC patients, fibroadenoma patients and healthy
adults. The results demonstrated that the levels of VEGF and MMP-9
in IDC patients were significantly higher than those in other two
groups. In addition, the levels in the fibroadenoma patients were
slightly higher than those in the healthy adults, although there
was no statistically significant difference. In IDC patients, the
levels of VEGF and MMP-9 were associated with their TNM-staging.
Significantly higher levels of VEGF and MMP-9 were observed in
patients classified as TNM stage III and IV as compared with
patients classified as TNM stage I and II. A previous study
demonstrated that VEGF levels increase in parallel with TNM-staging
(15). In addition, MMP-9 levels
are similar in triple negative breast cancer (TNBC) and in
estrogen-dependent breast cancer (16). These observations are consistent
with the results of the present study.
In the current study, a significant association was
observed between the tumor size and the levels of VEGF and MMP-9,
with levels increasing in parallel with tumor size. Goldhirsch
et al (17) reported that a
tumor size of >2 cm indicated poor prognosis in breast cancer
patients. Tumor size had been regarded as an independent factor for
prognosis of breast cancer. Generally, larger tumors indicate
poorer prognosis when regional lymph node metastasis and distant
metastasis are excluded. Rakha et al (18) also reported that tumor size played
an important role in indicating the prognosis and particularly in
guiding treatment in TNBC (19).
Thus, the levels of VEGF and MMP-9, as a factor in parallel with
tumor size, can also indicate the prognosis in breast cancer. To
exclude the influence of chemotherapeutic drugs, serum was
collected postoperatively and prior to the start of chemotherapy.
The levels of VEGF and MMP-9 were found to decrease as a result of
tumor cytoreduction, thus, it was hypothesized that the levels of
VEGF and MMP-9 may reflect the control of breast cancer.
VEGF can promote the proliferation of epithelial
cells and the permeability of vessels, which facilitates the
invasion and metastasis of tumors. MMP-9 can degrade the basement
membrane, which also leads to metastasis. The incidence of lymph
node metastasis in patients with high levels of VEGF or MMP-9 has
been reported to be higher compared with patients with low levels
of VEGF and MMP-9. In addition, the incidence is higher in patients
with high levels of both factors as compared with a high level of a
single factor (15). In the
present study, the levels of VEGF and MMP-9 were shown to be
significantly higher in patients with lymph node metastasis than in
patients without lymph node metastasis. Thus, we hypothesized that
the levels of VEGF and MMP-9 may be used as risk factors in
predicting lymph node metastasis. In addition, the levels of VEGF
and MMP-9 were significantly higher in IDC patients than in the
fibroadenoma patients and healthy adults, and the level of MMP-9
exhibited a positive correlation with the level of VEGF. These
observations indicate that VEGF induces high expression levels of
MMP-9 by the continuous activation of the MAPK pathway. As a
result, induced EMT of the tumor cells promotes advancement,
invasion and metastasis. However, VEGF may activate mitosis and
facilitate the survival and proliferation of endothelial cells in
the lymph vessels. Thus, the increase in lymphatic vessel density
at the periphery of the tumor may also contribute to invasion and
lymph node metastasis in breast cancer.
The positive correlation between VEGF and MMP-9, as
shown in the present study, was consistent with the results of
previous studies. Riedel et al (20) reported that a synergy existed
between VEGF and MMP-9 levels and that the two factors can be used
as biomarkers to indicate the neovascularization, invasion and
metastasis of tumors. Riedel et al (21) reported a correlation between VEGF
and MMP-9 levels in the neovascularization of head and neck
squamous cell carcinoma. Zucker et al (22) reported that VEGF can promote the
secretion of MMP-9 and increase the activity (23). Thus, combined detection of VEGF and
MMP-9 exhibits a certain value in predicting the invasion and
metastasis of tumors.
Carcinogenesis in breast cancer is a multi-factor
process, and invasion and metastasis involves multiple steps, thus,
is very complicated (24). VEGF
and MMP-9 are important cytokines that participate in the
regulation of the aforementioned processes. Through combined
detection of VEGF and MMP-9, the present study identified that the
levels were correlated with TNM-staging, primary tumor size and
lymph node metastasis in breast cancer. A correlation was also
observed between the two factors. Therefore, combined detection can
play a supporting role in determining TNM-staging and lymph node
metastasis in IDC patients.
In the present study, a lipid chip-based method was
used to detect the serum levels of VEGF and MMP-9. Compared with
pathological methods and ELISA, the lipid chip-based method has
higher sensitivity and accuracy (accurate to 0.01 pg/ml) (25). The liquid environment is more
suitable for maintaining the formation of biomacromolecules and for
the reactions between probes and substrates. The lipid chip-based
method simply requires blood samples, thus, this method has a
number of advantages, including low cost, small wounds, easy
surgery and good repeatability (26).
The present study has certain limitations. Platelets
have been shown to release VEGF into the serum, thus, the level of
VEGF may be influenced by the amount and the activity of platelets.
Therefore, detecting the plasma levels of VEGF and MMP-9, rather
than the serum levels, may be more accurate (27). Further research with more patients
observed over a longer follow-up period is required to confirm the
association between VEGF, MMP-9 and the prognosis of IDC
patients.
References
|
1
|
Liu Y, Cao W, Zhang B, Liu YQ, Wang ZY, Wu
YP, Yu XJ, Zhang XD, Ming PH, Zhou GB and Huang L: The natural
compound magnolol inhibits invasion and exhibits potential in human
breast cancer therapy. Sci Rep. 3:30982013.PubMed/NCBI
|
|
2
|
Charpentier M and Martin S: Interplay of
stem cell characteristics, EMT, and microtentacles in circulating
breast tumor cells. Cancers (Basel). 5:1545–1565. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Chambers AF and Matrisian LM: Changing
views of the role of matrix metalloproteinases in metastasis. J
Natl Cancer Inst. 89:1260–1270. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Peschos D, Damala C, Stefanou D, Tsanou E,
Assimakopoulos D, Vougiouklakis T, Charalabopoulos K and Agnantis
NJ: Expression of matrix metalloproteinase-9 (gelatinase B) in
benign, premalignant and malignant laryngeal lesions. Histol
Histopathol. 21:603–608. 2006.PubMed/NCBI
|
|
5
|
Chang SH, Kanasaki K, Gocheva V, et al:
VEGF-A induces angiogenesis by perturbing the cathepsin-cysteine
protease inhibitor balance in venules, causing basement membrane
degradation and mother vessel formation. Cancer Res. 69:4537–4544.
2009. View Article : Google Scholar
|
|
6
|
Quaranta M, Daniele A, Coviello M, et al:
MMP-2, MMP-9, VEGF and CA 15.3 in breast cancer. Anticancer Res.
27:3593–3600. 2007.
|
|
7
|
Edge SB and Compton CC: The American Joint
Committee on Cancer: the 7th edition of the AJCC cancer staging
manual and the future of TNM. Ann Surg Oncol. 17:1471–1474. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Belugali Nataraj N and Salimath BP:
Crosstalk between VEGF and novel angiogenic protein regulates tumor
angiogenesis and contributes to aggressiveness of breast carcinoma.
Cell Signal. 25:277–294. 2013.PubMed/NCBI
|
|
9
|
Stathopoulos J, Armakolas A, Stathopoulos
GP and Gomatos IP: Plasma VEGF levels in breast cancer patients
with and without metastases. Oncol Lett. 1:739–741. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Recchia F, Candeloro G, Necozione S, et
al: Vascular endothelial growth factor expression and T-regulatory
cells in premenopausal breast cancer. Oncol Lett. 5:1117–1122.
2013.PubMed/NCBI
|
|
11
|
Liu D, Guo H, Li Y, et al: Association
between polymorphisms in the promoter regions of matrix
metalloproteinases (MMPs) and risk of cancer metastasis: a
meta-analysis. PLoS One. 7:e312512012. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Radisky ES and Radisky DC: Matrix
metalloproteinase-induced epithelial-mesenchymal transition in
breast cancer. J Mammary Gland Biol Neoplasia. 15:201–212. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Lohela M, Bry M, Tammela T and Alitalo K:
VEGFs and receptors involved in angiogenesis versus
lymphangiogenesis. Curr Opin Cell Biol. 21:154–165. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Ranuncolo SM, Armanasco E, Cresta C, et
al: Plasma MMP-9 (92 kDa-MMP) activity is useful in the follow-up
and in the assessment of prognosis in breast cancer patients. Int J
Cancer. 106:745–751. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Hao L, Zhang C, Qiu Y, et al:
Recombination of CXCR4, VEGF, and MMP-9 predicting lymph node
metastasis in human breast cancer. Cancer Lett. 253:34–42. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Pellikainen JM, Ropponen KM, Kataja VV, et
al: Expression of matrix metalloproteinase (MMP)-2 and MMP-9 in
breast cancer with a special reference to activator protein-2,
HER2, and prognosis. Clin Cancer Res. 10:7621–7628. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Goldhirsch A, Glick JH, Gelber RD, et al:
Meeting highlights: international expert consensus on the primary
therapy of early breast cancer 2005. Ann Oncol. 16:1569–1583. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Rakha EA, El-Sayed ME, Green AR, et al:
Prognostic markers in triple-negative breast cancer. Cancer.
109:25–32. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Turner N, Tutt A and Ashworth A: Hallmarks
of ‘BRCAness’ in sporadic cancers. Nat Rev Cancer. 4:814–819.
2004.
|
|
20
|
Riedel F, Götte K, Bergler W and Hörmann
K: Inverse correlation of apoptotic and angiogenic markers in
squamous cell carcinoma of the head and neck. Oncol Rep. 8:471–476.
2001.PubMed/NCBI
|
|
21
|
Riedel F, Götte K, Schwalb J, et al:
Expression of 92-kDa type IV collagenase correlates with angiogenic
markers and poor survival in head and neck squamous cell carcinoma.
Int J Oncol. 17:1099–1105. 2000.PubMed/NCBI
|
|
22
|
Zucker S, Mirza H, Conner CE, et al:
Vascular endothelial growth factor induces tissue factor and matrix
metalloproteinase production in endothelial cells: conversion of
prothrombin to thrombin results in progelatinase A activation and
cell proliferation. Int J Cancer. 75:780–786. 1998. View Article : Google Scholar
|
|
23
|
Hawinkels LJ, Zuidwijk K, Verspaget HW, et
al: VEGF release by MMP-9 mediated heparan sulphate cleavage
induces colorectal cancer angiogenesis. Eur J Cancer. 44:1904–1913.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Tang L, Ma X, Tian Q, et al: Inhibition of
angiogenesis and invasion by DMBT is mediated by downregulation of
VEGF and MMP-9 through Akt pathway in MDA-MB-231 breast cancer
cells. Food Chem Toxicol. 56:204–213. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Elshal MF and McCoy JP: Multiplex bead
array assays: performance evaluation and comparison of sensitivity
to ELISA. Methods. 38:317–323. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Sylvester JE and Kron SJ: A bead-based
activity screen for small-molecule inhibitors of signal
transduction in chronic myelogenous leukemia cells. Mol Cancer
Ther. 9:1469–1481. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Reeves KW, Ness RB, Stone RA, et al:
Vascular endothelial growth factor and breast cancer risk. Cancer
Causes Control. 20:375–386. 2009. View Article : Google Scholar : PubMed/NCBI
|