Introduction
Abdominal pain is one of the most common symptoms
prompting patients to visit hospitals. Among such individuals, a
number of patients have serious diseases and require subsequent
hospitalization or surgery. Diagnosis may consist of acute
appendicitis, intestinal obstruction and other serious conditions
such as bowel necrosis and intestinal volvulus (1). Correct and prompt diagnosis is
essential for the appropriate management of patients. Diagnosis of
patients with abdominal pain is primarily determined by imaging
techniques, such as radiography, abdominal ultrasonography (US),
computed tomography (CT) and magnetic resonance imaging (MRI)
(2). Among these, abdominal US is a
non-invasive procedure, which is readily available at most
hospitals even during off-hours (weekends, nights and holidays) and
may be performed at the bedside (3).
Abdominal US is indispensable for the diagnosis of
diseases in the abdominal cavity in patients with abdominal
symptoms (4,5). In addition, abdominal US is also useful
for the diagnosis of solid organ conditions, including acute
cholangitis, acute cholecystitis and acute pancreatitis (6–8).
Abdominal US is also useful in the diagnosis of bowel disease based
on pathological findings (9,10). Diagnostic criteria with abdominal US
have been established for acute appendicitis and colonic
diverticulitis (11–14) and colorectal cancer may be diagnosed
with abdominal US (15). In numerous
cases, patients are diagnosed by a combination of laboratory data
and diagnostic imaging findings based on symptoms and physical
examination. With regards to diagnostic imaging, CT is recommended
as the first-line procedure (16);
however, CT is not readily available during off-h at the majority
of hospitals. In these cases, abdominal US is the first-line
procedure performed.
On the basis of the aforementioned considerations,
the current study retrospectively analyzed the records of patients
who underwent abdominal US as a first-line diagnostic imaging
procedure in order to evaluate its utility and limitations in
determining the diagnosis of patients presenting with abdominal
symptoms.
Materials and methods
Patients
Medical records were retrospectively analyzed for 76
patients who were subjected to abdominal US as the first-line
diagnostic imaging modality at the National Hospital Organization
Shimoshizu Hospital (Yotsukaido, Japan) from April 2010 to April
2015. Abdominal US was performed at the time of consultation or
during off-hours (weeknights, weekends and holidays). Recruited
patients were restricted to those in which abdominal US was
performed as a first diagnostic approach in order to evaluate the
diagnostic performance solely from abdominal US without any
potentially confounding information from other diagnostic imaging
procedures. Thus, patients were excluded when abdominal US was
performed following another diagnostic imaging procedures, such as
radiography, CT or MRI because the sonographer may have been
informed of the findings obtained. The analyzed patients included
39 males with an average (mean ± standard deviation) age of
65.8±18.8 years and 37 females with an average age of 53.7±19.3
years.
Patients were hospitalized or referred to a
different hospital based on the diagnosis obtained by abdominal US,
the results of blood examinations, clinical findings or diagnostic
imaging following abdominal US. The National Hospital Organization
Shimoshizu Hospital does not have a department of gynecology.
Therefore, patients were referred to another hospital for
gynecological consultation. The referred hospitals were National
Hospital Organization Chiba Medical Center (Chiba, Japan) and
Seirei Sakura Citizen Hospital (Sakura, Japan). During off-hours,
the management of patients was determined on the basis of abdominal
US and clinical symptoms. The present study was approved by the
Ethics Committee of the National Hospital Organization Shimoshizu
Hospital. It was not considered a clinical trial since abdominal US
was performed as a part of routine clinical practice. Written
informed consent for inclusion in the study was waived. Patient
records/information was anonymized and de-identified prior to
analysis.
Abdominal US
Abdominal US was performed by Senior Fellows of the
Japan Society of Ultrasonics in Medicine (Tokyo, Japan; http://www.jsum.or.jp/jsum-e/index.html)
using a SSA-700A US system (Toshiba Medical Systems Corporation,
Ohtawara, Japan) with a 3.75-MHz curved-array probe (PVT-375BT;
Toshiba Medical Systems Corporation) or an 8.0-MHz linear-array
probe (PLT-805AT; Toshiba Medical Systems Corporation).
Diagnostic criteria of diseases
Acute cholangitis is defined as inflammation due to
the obstruction of a bile duct (6).
Findings detectable by abdominal US include bile duct dilatation
and evidence of its etiology, such as stricture, stones or stent
(6). In the present study, in the
absence of these findings, acute cholangitis was not diagnosed by
abdominal US, but was based on a combination of symptoms including
systemic inflammation and cholestasis (6). Acute cholecystitis was diagnosed by a
combination of local and systemic signs of inflammation (7). Abdominal US supported the diagnosis
with findings of distension, wall thickening and sludge in the
gallbladder (7). More specifically,
the finding of a sonographic Murphy sign was considered the most
reliable because it is considered to suggest inflammation of the
gallbladder (17).
Acute pancreatitis is typically diagnosed as
abdominal pain, elevated serum amylase and swelling of the pancreas
by diagnostic imaging (18). In the
current study, acute pancreatitis was diagnosed when abdominal US
revealed a swollen pancreas, fluid collection and inflammation of
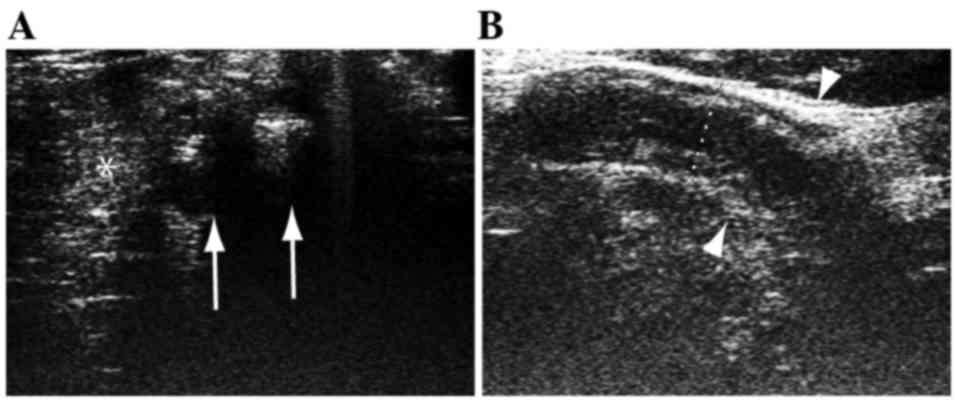
adjacent organs. Acute diverticulitis was diagnosed as diverticulum
with thickened wall and high echo from the surrounding tissue
(Fig. 1A) (12). Acute appendicitis was diagnosed as
swollen appendix with a diameter >10 mm, and thickened wall
(Fig. 1B) (13,14).
Results
Successful diagnosis of patients
Initial diagnosis with abdominal US was in agreement
with the final diagnosis in 66 patients. For the remaining 10
patients, the diagnosis obtained from abdominal US differed from
the final diagnosis. To investigate the performance and limitations
of abdominal US, patients were divided into two groups. The first
included patients in whom abdominal US diagnosis agreed with the
final diagnosis (Table I) and the
other included patients whose initial abdominal US diagnosis
differed from the final diagnosis (Table II).
 | Table I.Diseases successfully diagnosed with
abdominal ultrasonography. |
Table I.
Diseases successfully diagnosed with
abdominal ultrasonography.
| Diagnosis | Number of
patients | Number of
off-houra patients |
|---|
| Acute
cholangitis | 15 | 3 |
| Acute
appendicitis | 11 | 9 |
| Acute
cholecystitis | 7 | 0 |
| Acute
pancreatitis | 7 | 4 |
| Enteritis | 7 | 4 |
| Colonic
diverticulitis | 5 | 3 |
| Ileus | 2 | 2 |
| Colorectal
cancer | 2 | 1 |
| Hepatocellular
carcinoma | 2 | 0 |
| Pancreatic
cancer | 2 | 0 |
| Bile duct cancer | 2 | 1 |
| Bowel
perforation | 2 | 2 |
| Spleen rupture | 1 | 0 |
| Upper
gastrointestinal bleeding | 1 | 1 |
| Total | 66 | 30 |
 | Table II.List of misdiagnosed patients and
speculated causes of misdiagnosis following abdominal
ultrasound. |
Table II.
List of misdiagnosed patients and
speculated causes of misdiagnosis following abdominal
ultrasound.
| Patient number | Gender | Age (years) | Final
diagnosis | Cause of
misdiagnosis | Consultation or
off-hour |
|---|
| 1 | F | 49 | Acute
cholangitis | Bile duct diameter
within normal range | C |
| 2 | M | 69 | Bile duct cancer,
acute cholangitis | Bile duct cancer
not detected due to gas | O |
| 3 | M | 88 | Sigmoid colon
volvulus | Difficult to
examine due to presence of massive gas bubbles | O |
| 4 | F | 87 | Acute
appendicitis | Appendix not
detected | O |
| 5 | M | 39 | Intestinal
anisakiasis | Anisakiasis not
detected | O |
| 6 | F | 89 | Duodena Ulcer | Tentatively
diagnosed as acute cholecystitis due to a positive sonographic
Murphy sign | C |
| 7 | M | 53 | Spontaneous
hemoperitoneum | Nature of ascites
not examined with US | O |
| 8 | F | 40 | Recurrence of
cervical cancer | Presence of a huge
mass in the pelvis of unknown origin | O |
| 9 | F | 48 | Left ovarian
torsion | Torsion not
diagnosed by US | C |
| 10 | F | 57 | Inflammation of
uterus | Inflammation of the
uterus not diagnosed | C |
Colorectal cancer and spleen
rupture
Solid organ diseases, including acute cholangitis,
acute cholecystitis and acute pancreatitis, were correctly
diagnosed by abdominal US. Intestinal diseases, including acute
appendicitis and colonic diverticulitis, were also correctly
diagnosed. Abdominal US was useful for the diagnosis of various
types of cancer, including hepatocellular carcinoma, pancreatic
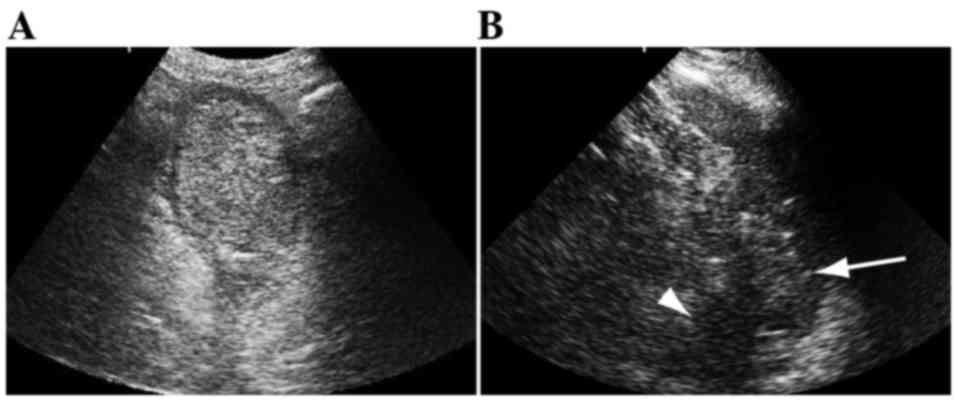
cancer, and colorectal cancer (Fig.
2A). Colorectal cancer findings included irregular shaped wall
thickening and loss of stratification, also referred to as the
‘pseudokidney’ sign (15). Critical
conditions, such as rupture of the spleen, were also successfully
diagnosed with abdominal US (Fig.
2B). Fluid in the abdominal cavity and high echo in the spleen
suggested bleeding and damaging lesions, respectively (19). A total of 30 patients were admitted
outside of regular working h and were subjected to abdominal US.
They were correctly diagnosed without being subjected to CT or
other diagnostic imaging procedures. These results clearly indicate
that abdominal US is useful for the diagnosis of patients
presenting with abdominal symptoms specifically during
off-hours.
Unsuccessful diagnosis of
patients
Table II summarizes
data from those patients who were misdiagnosed by abdominal US and
the potential reasons for misdiagnosis. These patients were
subjected to additional diagnostic imaging procedures and were
hospitalized for treatment because their conditions suggested the
necessity of further management. Two patients were referred to
another hospital for gynecological consultation. All patients
described in Table II were
appropriately managed, according to their condition.
One major cause of misdiagnosis was
intestinal gas
Gas over the site of the disease made the
examination difficult to execute. Gas over the bile duct (patient
2) hindered the detection of bile duct cancer. Gas in the sigmoid
colon made the examination difficult for patient 3.
Unsuccessful diagnosis of acute
appendicitis and duodenal ulcer
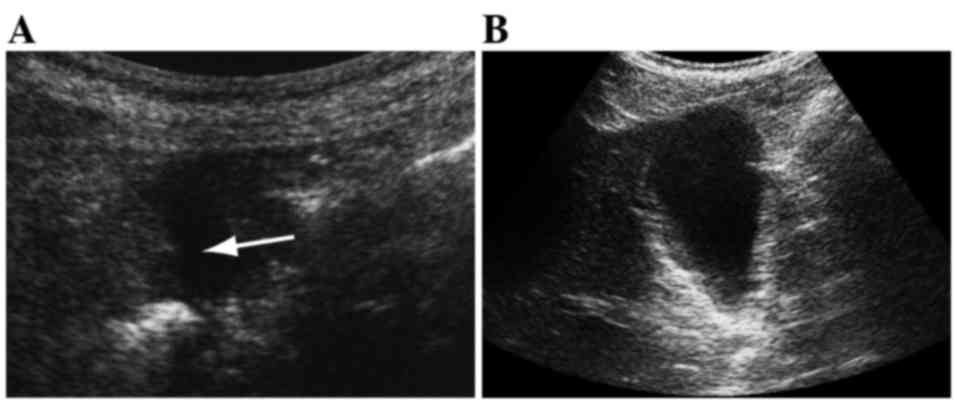
A diagnosis of acute appendicitis was hampered when
it was not possible to detect the appendix (patient 4; Fig. 3A) (20).
A sonographic Murphy sign markedly suggests acute
cholecystitis when abdominal US findings include distension and
wall thickening of the gallbladder (17). Since the duodenum is close to the
gallbladder, the tenderness perceived in duodenal ulcer may
occasionally resemble a sonographic Murphy sign (patient 6;
Fig. 3B).
Unsuccessful diagnosis of
gynecological diseases
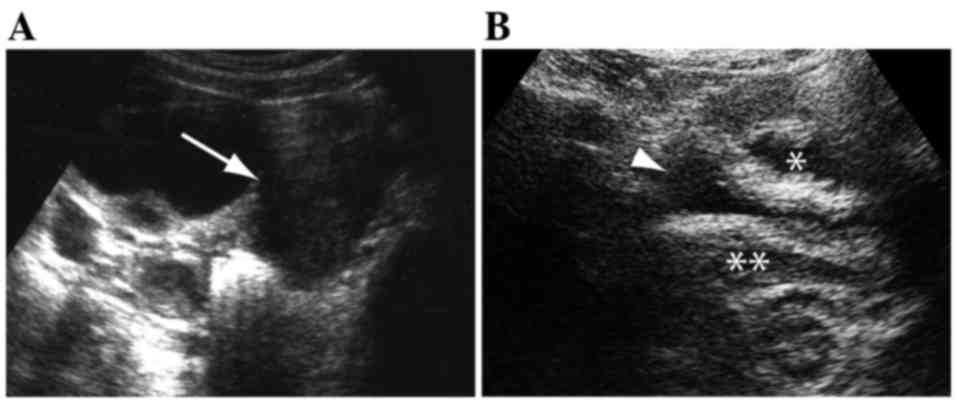
A major difficulty in successful diagnosis with
abdominal US was the presence of gynecological disorders. It was
not difficult to detect a mass in the pelvis (patient 8) or a
cystic lesion in the ovary (patient 9; Fig. 4A), however it was difficult to
diagnose the site or organ of the original lesion, or relative
torsion. The abdominal US clearly illustrated ascites and weakened
peristalsis of the sigmoid colon (patient 10; Fig. 4B), but the correct diagnosis required
subsequent referral to a gynecologist. Thus, these results
suggested that patients should be referred for gynecological
consultation when the abdominal US indicates abnormal findings in
the pelvis, particularly in the ovary and uterus.
Discussion
The presence of gas bubbles makes abdominal US
difficult to perform (21). Large
amounts of gases arise due to perforation and obstruction of the
bowel (22,23). In the current study, bile duct cancer
and sigmoid colon volvulus were not diagnosed using abdominal US
due to the presence of intestinal gas. Sigmoid colon volvulus
requires prompt diagnosis followed by surgical or endoscopic
treatment (24). An upside down
U-shaped loop of dilated bowel is a typical radiological finding
(25). With regards to abdominal US,
findings specific to sigmoid colon volvulus have not been reported
(26). Abdominal US is not,
therefore, suitable for the diagnosis of sigmoid colon volvulus. It
is recommended that patients should be subjected to radiography and
CT when sigmoid colon volvulus is suspected (27).
The diagnosis of acute appendicitis with abdominal
US is challenging when the appendix is unable to be visualized
(20). In such cases, a large amount
of fluid, phlegmon and pericecal inflammatory fat changes are clear
indications for the diagnosis of acute appendicitis (20). In the present study, fluid and high
echo tissues were detected (Fig. 3A)
and these findings suggested acute appendicitis. However, it was
not possible to exclude the diagnosis of colonic diverticulitis or
peritonitis. It was concluded that acute appendicitis is difficult
to diagnose without the direct observation of the appendix.
Abdominal US is useful for gynecologists in the
diagnosis of gynecological emergencies (28). Abnormal findings in the pelvis were
detected in the current study, although a precise diagnosis was
delayed since patients had to be referred to a gynecologist at a
different institution for consultation. Among patients in the
present study, ovarian torsion was the most critical condition.
Ovarian torsion is diagnosed based on clinical symptoms, abdominal
US, CT, and MRI (29). Color Doppler
US reveals absent or diminished central venous flow in patients
with ovarian torsion (5). However, a
diagnosis of ovarian torsion is difficult to achieve (29). A previous report, in addition to the
results from the patients in the current study, has suggested that
gynecological diseases are difficult to correctly diagnose with
abdominal US alone (28). It is
recommended that a patient should be promptly referred to a
gynecologist if an emergency condition is suspected.
One of the limitations of the present study was the
relatively small number of patients examined. The number of
patients was limited as the study was restricted to patients
subjected to abdominal US as the first diagnostic imaging method.
The initial aim of the present study was to evaluate the diagnostic
performance of first-line abdominal US for patients presenting with
abdominal symptoms. If information from the other diagnostic
imaging examinations was available prior to abdominal US, this
information may have interfere with the overall outcome of the
abdominal US.
In the present study, performing an abdominal US was
suitable for the correct diagnosis of patients presenting with
abdominal symptoms. CT is sensitive, but requires exposure to
radiation; abdominal US reduces the necessity of CT, and lowers the
exposure (30). It is recommended
that patients should undergo further diagnostic imaging
examinations when large gas bubbles are observed (31). It is also recommended that patients
should be referred to a gynecologist when gynecological diseases
are suspected.
In conclusion, abdominal US was suitable for the
diagnosis of patients with abdominal symptoms. It is recommended
that further diagnostic imaging be performed for patients with a
large gas bubbles and that patients be referred to a gynecologist
when gynecological diseases are suspected.
References
|
1
|
Paduszynska K, Celnik A and Pomorski L:
Patients subject to surgery due to acute abdominal disorders during
the period between 2001–2004. Pol Przegl Chir. 84:488–494.
2012.PubMed/NCBI
|
|
2
|
Hayes R: Abdominal pain: General imaging
strategies. Eur Radiol. 14:(Suppl 4). L123–L137. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Rozycki GS, Cava RA and Tchorz KM:
Surgeon-performed ultrasound imaging in acute surgical disorders.
Curr Probl Surg. 38:141–212. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Puylaert JB, van der Zant FM and Rijke AM:
Sonography and the acute abdomen: Practical considerations. AJR Am
J Roentgenol. 168:179–186. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Birnbaum BA and Jeffrey RB Jr: CT and
sonographic evaluation of acute right lower quadrant abdominal
pain. AJR Am J Roentgenol. 170:361–371. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Kiriyama S, Takada T, Strasberg SM,
Solomkin JS, Mayumi T, Pitt HA, Gouma DJ, Garden OJ, Büchler MW,
Yokoe M, et al: New diagnostic criteria and severity assessment of
acute cholangitis in revised Tokyo Guidelines. J Hepatobiliary
Pancreat Sci. 19:548–556. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Yokoe M, Takada T, Strasberg SM, Solomkin
JS, Mayumi T, Gomi H, Pitt HA, Gouma DJ, Garden OJ, Büchler MW, et
al: New diagnostic criteria and severity assessment of acute
cholecystitis in revised Tokyo Guidelines. J Hepatobiliary Pancreat
Sci. 19:578–585. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Scaglione M, Casciani E, Pinto A, Andreoli
C, De Vargas M and Gualdi GF: Imaging assessment of acute
pancreatitis: A review. Semin Ultrasound CT MR. 29:322–340. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Maturen KE, Wasnik AP, Kamaya A, Dillman
JR, Kaza RK, Pandya A and Maheshwary RK: Ultrasound imaging of
bowel pathology: Technique and keys to diagnosis in the acute
abdomen. AJR Am J Roentgenol. 197:W1067–W1075. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Puylaert JB: Ultrasound of acute GI tract
conditions. Eur Radiol. 11:1867–1877. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Karul M, Berliner C, Keller S, Tsui TY and
Yamamura J: Imaging of appendicitis in adults. Rofo. 186:551–558.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Puylaert JB: Ultrasound of colon
diverticulitis. Dig Dis. 30:56–59. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Ooms HW, Koumans RK, Ho Kang, You PJ and
Puylaert JB: Ultrasonography in the diagnosis of acute
appendicitis. Br J Surg. 78:315–318. 1991. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Rodgers PM and Verma R: Transabdominal
ultrasound for bowel evaluation. Radiol Clin North Am. 51:133–148.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Tomizawa M, Shinozaki F, Hasegawa R, Fugo
K, Shirai Y, Ichiki N, Sugiyama T, Yamamoto S, Sueishi M and
Yoshida T: Screening ultrasonography is useful for the diagnosis of
gastric and colorectal cancer. Hepatogastroenterology. 60:517–521.
2013.PubMed/NCBI
|
|
16
|
Stoker J, van Randen A, Laméris W and
Boermeester MA: Imaging patients with acute abdominal pain.
Radiology. 253:31–46. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Myrianthefs P, Evodia E, Vlachou I,
Petrocheilou G, Gavala A, Pappa M, Baltopoulos G and Karakitsos D:
Is routine ultrasound examination of the gallbladder justified in
critical care patients? Crit Care Res Pract.
2012:5656172012.PubMed/NCBI
|
|
18
|
Wu BU and Banks PA: Clinical management of
patients with acute pancreatitis. Gastroenterology. 144:1272–1281.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Korner M, Krötz MM, Degenhart C, Pfeifer
KJ, Reiser MF and Linsenmaier U: Current role of emergency US in
patients with major trauma. Radiographics. 28:225–242. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Estey A, Poonai N and Lim R: Appendix not
seen: The predictive value of secondary inflammatory sonographic
signs. Pediatr Emerg Care. 29:435–439. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Hoffmann B, Nurnberg D and Westergaard MC:
Focus on abnormal air: Diagnostic ultrasonography for the acute
abdomen. Eur J Emerg Med. 19:284–291. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Grassi R, Romano S, Pinto A and Romano L:
Gastro-duodenal perforations: Conventional plain film, US and CT
findings in 166 consecutive patients. Eur J Radiol. 50:30–36. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Hucl T: Acute GI obstruction. Best Pract
Res Clin Gastroenterol. 27:691–707. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Yeo HL and Lee SW: Colorectal emergencies:
Review and controversies in the management of large bowel
obstruction. J Gastrointest Surg. 17:2007–2012. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
James B and Kelly B: The abdominal
radiograph. Ulster Med J. 82:179–187. 2013.PubMed/NCBI
|
|
26
|
Lim JH, Ko YT, Lee DH, Lee HW and Lim JW:
Determining the site and causes of colonic obstruction with
sonography. AJR Am J Roentgenol. 163:1113–1117. 1994. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Gingold D and Murrell Z: Management of
colonic volvulus. Clin Colon Rectal Surg. 25:236–244. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Popowski T, Huchon C, Fathallah K,
Falissard B, Dumont A and Fauconnier A: Impact of accreditation
training for residents on sonographic quality in gynecologic
emergencies. J Ultrasound Med. 34:829–835. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Gerscovich EO, Corwin MT, Sekhon S, Runner
GJ and Gandour-Edwards RF: Sonographic appearance of adnexal
torsion, correlation with other imaging modalities, and clinical
history. Ultrasound Q. 30:49–55. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Lameris W, van Randen A, van Es HW, van
Heesewijk JP, van Ramshorst B, Bouma WH, ten Hove W, van Leeuwen
MS, van Keulen EM, Dijkgraaf MG, et al: Imaging strategies for
detection of urgent conditions in patients with acute abdominal
pain: Diagnostic accuracy study. BMJ. 338:b24312009. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Farina R, Catalano O, Stavolo C,
Sandomenico F, Petrillo A and Romano L: Emergency radiology. Radiol
Med. 120:73–84. 2015. View Article : Google Scholar : PubMed/NCBI
|