Introduction
Phimosis and redundant prepuce is one of the common
clinical diseases in urology that affect the normal penile
development (1). It also results in
repeated attacks of acrobystitis, along with symptoms such as
dyspareunia, infection of urinary system and the invasion of
genital system (epididymis, testis, seminal vesicle and prostate)
(1). Long-term stimulation of smegma
praeputii is an important factor that induces carcinoma of penis
and cervical cancer of spouse leading to sexual dysfunction
including premature ejaculation (2–4).
Patients with redundant prepuce often choose operative treatment,
and the traditional circumcision is the most common option.
However, the traditional procedure has disadvantages of lengthy
operation time, large bleeding volume, and unaesthetic incisal
edge. On the other hand, disposable circumcision stitching
instrument operation has the advantages of short operation time,
has less bleeding volume and aesthetic incisal edge, which is
helpful for the harmonious sexual life of patients (5).
The present study conducted disposable circumcision
stitching instrument operation on the patients with phimosis and
redundant prepuce and received a satisfactory curative effect. The
details are reported as follows.
Materials and methods
General data
A total of 102 cases of patients with circumcision
were randomly selected (from June 2013 to December 2014) from the
Department of Plastic and Aesthetic Surgery of our hospital.
Inclusion criteria were: ⅰ) patients with typical phimosis or
redundant prepuce who need operative treatment; ⅱ) normal
development of penis and ⅲ) signed informed consent. Exclusion
criteria were: ⅰ) penis dysplasia and genital tract malformation;
ⅱ) premature ejaculation caused by spermatocystitis, urethritis and
prostatitis; ⅲ) without re-examination and follow-up visit
according to study requirement. Computer software was used to
divide them into the control and observation groups (n=51 per
group). The general data of two groups showed no statistical
significance (P>0.05, Table I).
This study was approved by the Ethics Committee of Shandong
Provincial Hospital. Signed written informed consents were obtained
from all participants before the study.
 | Table I.General data of study objects. |
Table I.
General data of study objects.
| Items | Observation group
n=51 cases | Control group n=51
cases | t/χ2 | P-value |
|---|
| Age (years) | 20-45 | 20-40 |
|
|
| Mean age (years) | 28.86±7.69 | 29.35±8.18 | 0.312 | 0.756 |
| Types (n, %) |
|
|
|
|
| Redundant
prepuce | 38 (78.51) | 35 (68.62) | 0.193 | 0.661 |
|
Phimosis | 13 (21.49) | 16 (31.38) |
|
|
| Degree of education
(n, %) |
|
|
|
|
| Middle
school or below | 11 (21.56) | 9 (17.64) | 0.780 | 0.677 |
| High
school | 26 (50.98) | 24 (47.06) |
|
|
|
| Junior
college or above | 14 (27.45) | 18 (35.29) |
|
|
|
Preoperative preparation
Before operation, the patients in the two groups
received convention blood urine examination. Prepuce cavity and
balanus were washed 1 day before operation. Furthermore, the
patients also received psychological counseling for the elimination
of their nervousness and fear. Before surgery, the surgical sites
of patients were given routine disinfection and drape, with 5–10 ml
of 1% lidocaine to conduct nerve block anesthesia of the penile
base.
Operation methods
Traditional method was applied to the control group.
In this protocol, haemostatic forceps were used to clamp the middle
frenum of the prepuce flank area, and was pulled for cutting the
bilateral prepuce tissue along the parallel site (with a parallel
distance of 5 mm) of coronary sulcus. The prepuce frenum tissue was
kept at approximately 10 mm. Then, electrocoagulation was applied
to stop the bleeding and the incision was sutured after detection
of active hemorrhage.
Disposable circumcision stitching instrument
(produced by Jiangxi Langhe Medical Instrument Co., Ltd., Jiangxi,
China) operation was applied to the observation group. The second,
sixth and tenth migration spots of inner and outer plates of
prepuce were raised by hemostatic forceps. Furthermore, a 30-degree
angle towards the dorsal part between penis axis and the bar axis
of campaniform glans penis base was kept. Ribbon or silk thread was
used for fixation on the rod and to take the safety catch out. The
knob was pressed for 10 sec, to lightly spin and quit the
campaniform glans penis base to stop the bleeding. The pressure was
released after 20 sec to check the suture situation, with pressure
dressing to the incision.
Morphological observation of tissue
specimens
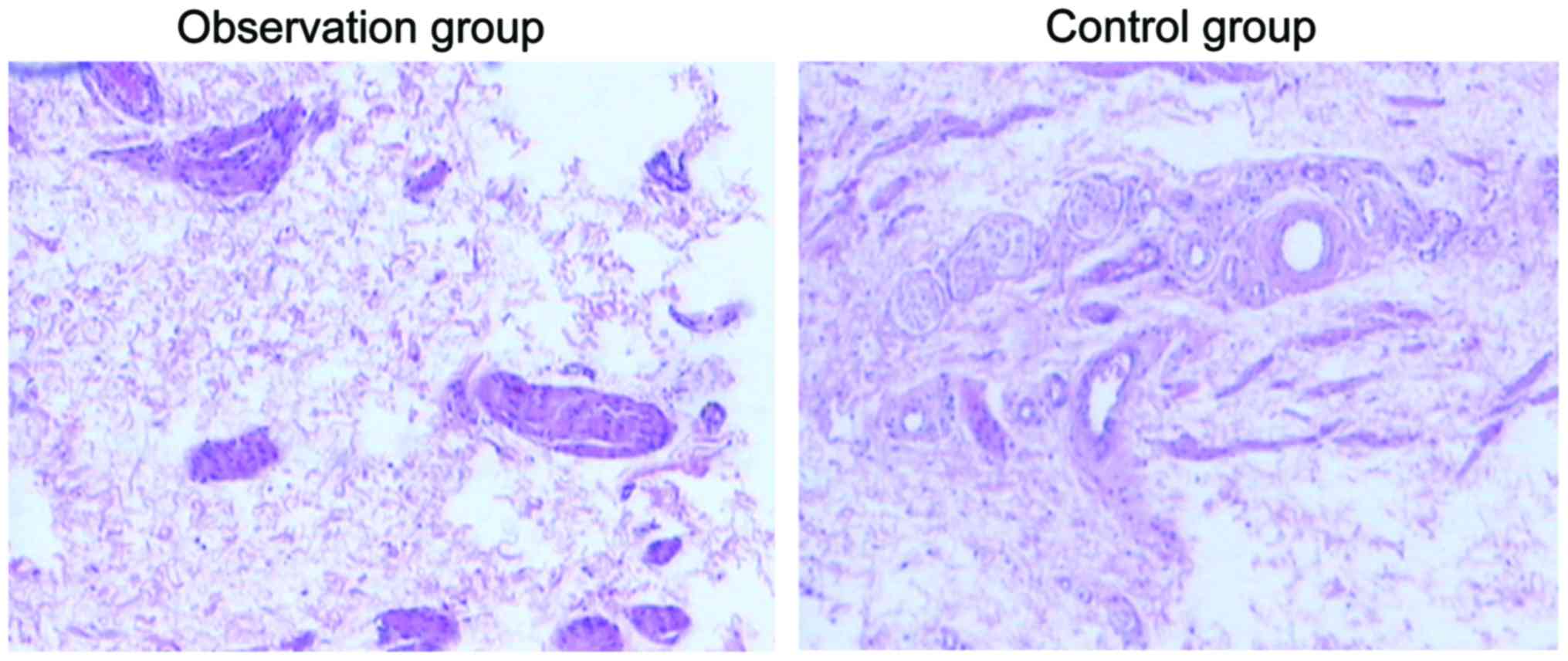
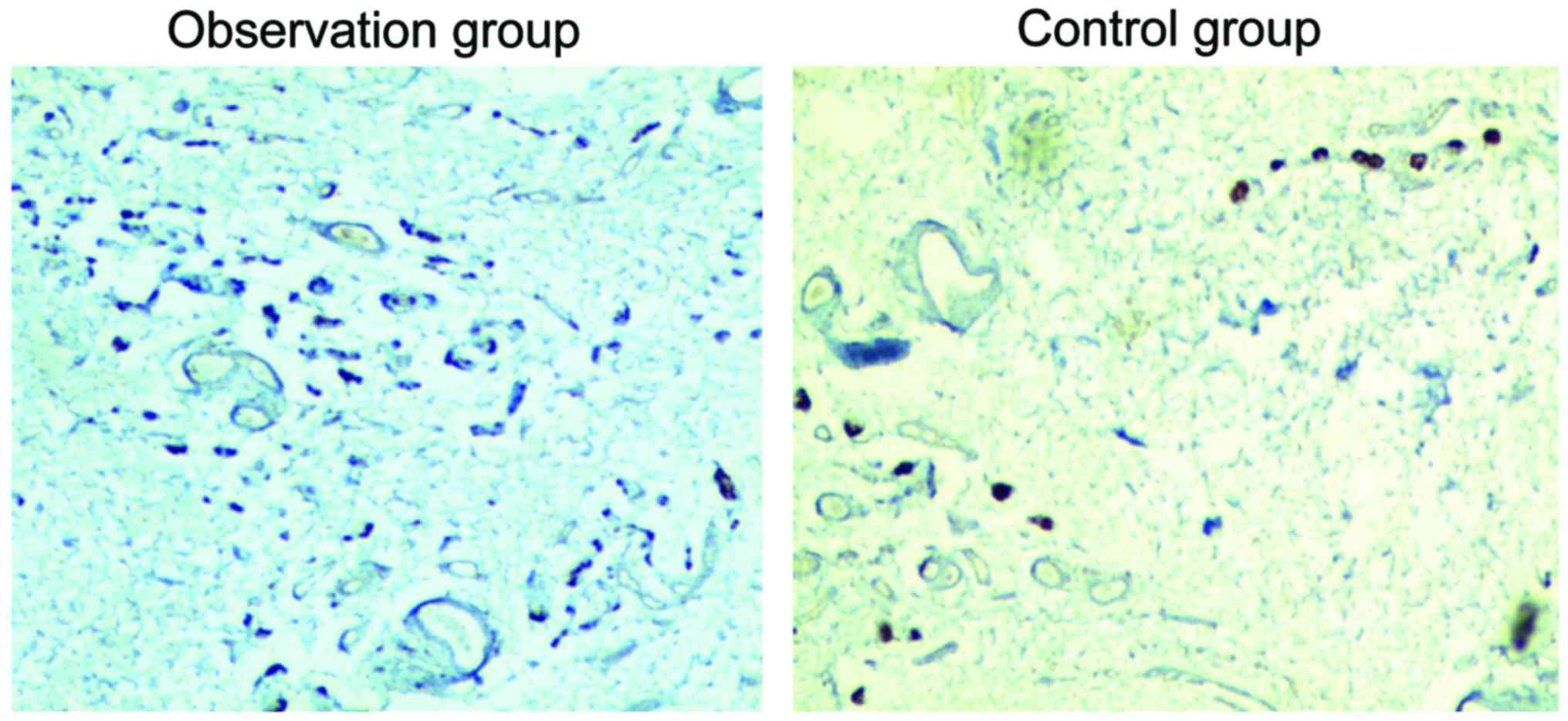
The prepuce tissue specimens of patients in the two
groups were analyzed by standard H&E staining. Under optical
microscope, the form of organization, especially the difference of
vasculature including blood vessel and lymph-vessel of tissue
specimens were observed. S-100 immumohistochemical staining method
was applied to observe the nerve architecture. A 40-time optical
microscope was used to observe the immunohistochemical results.
Postoperative care and follow-up
visit
The patients of the observation group scrubbed the
wound edge using iodophor every day after 1 week of operation. At
the postoperative 6-month follow-up visit, the operation effect,
sexual function and psychological status were evaluated.
Evaluation methods
The operation results and postoperative
complications of the two groups of patients were compared,
including operation time, intra-operative bleeding volume, incision
healing time, postoperative incision infection and incision edema.
VAS scores were recorded to evaluate the pain grade. The Chinese
index of sexual function for premature ejaculation (CIPE) was used
to conduct a questionnaire survey. A 5-grade method of 1–5 scores
was applied to evaluate libido, erectile hardness, ejaculation
incubation, erection hold time, ejaculation control difficulty,
sexual satisfaction of spouses, orgasm frequency of spouse, sexual
self-confidence and self-anxiety level of patients for 6 months
after operation. The total score was 50, which had a positive
relation with sexual function. Furthermore, an Eysenck personality
questionnaire was applied to monitor the psychological states of
patients in the two groups.
Statistical analysis
Software SPSS 19.0 (SPSS, Inc. Chicago, IL, USA) was
utilized to process data. P<0.05 indicates a statistically
significant difference.
Results
Surgery and postoperative
complications
The results of the surgery using the two methods and
their respective postoperative complications were compared. The
intraoperative bleeding volume of patients in the observation group
was significantly less in comparison with the control group.
Operation time and incision healing time of patients in the
observation group was also shorter (P<0.05, Table II). The postoperative complications
of patients in the observation group were significantly lower than
that of the control group (Table
III).
 | Table II.Comparison of postoperative situations
between the two groups of patients. |
Table II.
Comparison of postoperative situations
between the two groups of patients.
| Groups | Cases | Operation time
(min) | Intraoperative
bleeding (ml) | Incision healing time
(days) |
|---|
| Observation
group | 51 | 7.83±1.62 | 1.97±0.63 | 11.23±2.53 |
| Control group | 51 | 19.14±3.57 | 9.57±1.38 | 18.56±3.47 |
| t-test |
| 20.063 | 35.778 | 12.190 |
| P-value |
| <0.0001 | <0.0001 | <0.0001 |
 | Table III.Comparison of postoperative
complications in the two groups. |
Table III.
Comparison of postoperative
complications in the two groups.
| Groups | Cases | Incision
infection | Incision split | Incision edema |
|---|
| Observation
group | 51 | 4 (7.84) | 7 (13.72) | 9 (17.64) |
| Control group | 51 | 0 (0.00) | 1 (1.96) | 2 (3.21) |
| χ2 |
| 14.370 |
|
|
| P-value |
| 0.0002 |
|
|
Morphological results
The morphological observation of tissue specimens
revealed that the blood vessel counting (7.35±2.18) and nerve fiber
counting (15.34±2.46) of tissue specimen in the observation group
were significantly higher than those of the control group
(4.32±1.57 and 9.65±1.48) (P<0.05, Figs. 1 and 2).
Postoperative results
Postoperative VAS score improvement of patients in
the observation group was significantly higher than that of the
control group, and the difference had statistical significance
(P<0.05, Table IV). Furthermore,
the incision aesthetic satisfaction of the observation group was
significantly higher at 98.03%, a degree of satisfaction that was
obviously higher than that of the control group at 76.47%
(P<0.05, Table V).
 | Table IV.Comparison of postoperative VAS scores
of patients in the two groups. |
Table IV.
Comparison of postoperative VAS scores
of patients in the two groups.
| Groups | Cases | 6 h after
operation | 12 h after
operation | 24 h after
operation |
|---|
| Observation
group | 51 | 5.13±1.14 | 3.16±1.13 | 1.85±1.14 |
| Control group | 51 | 7.16±1.23 | 5.33±1.25 | 3.58±1.26 |
| t-test |
| 8.644 | 9.179 | 7.271 |
| P-value |
| <0.0001 | <0.0001 | <0.0001 |
 | Table V.Incision aesthetic satisfaction of
patient in the two groups (n, %). |
Table V.
Incision aesthetic satisfaction of
patient in the two groups (n, %).
| Groups | Cases | Very satisfied | Satisfied | Dissatisfied | Total degree of
satisfaction |
|---|
| Observation
group | 51 | 39 (76.47) | 11 (21.56) | 1 (1.97) | 50 (98.03) |
| Control group | 51 | 19 (3.72) | 20 (39.21) | 12 (23.52) | 39 (76.47) |
| χ2 |
| 29.993 |
|
|
|
| P-value |
| <0.0001 |
|
|
|
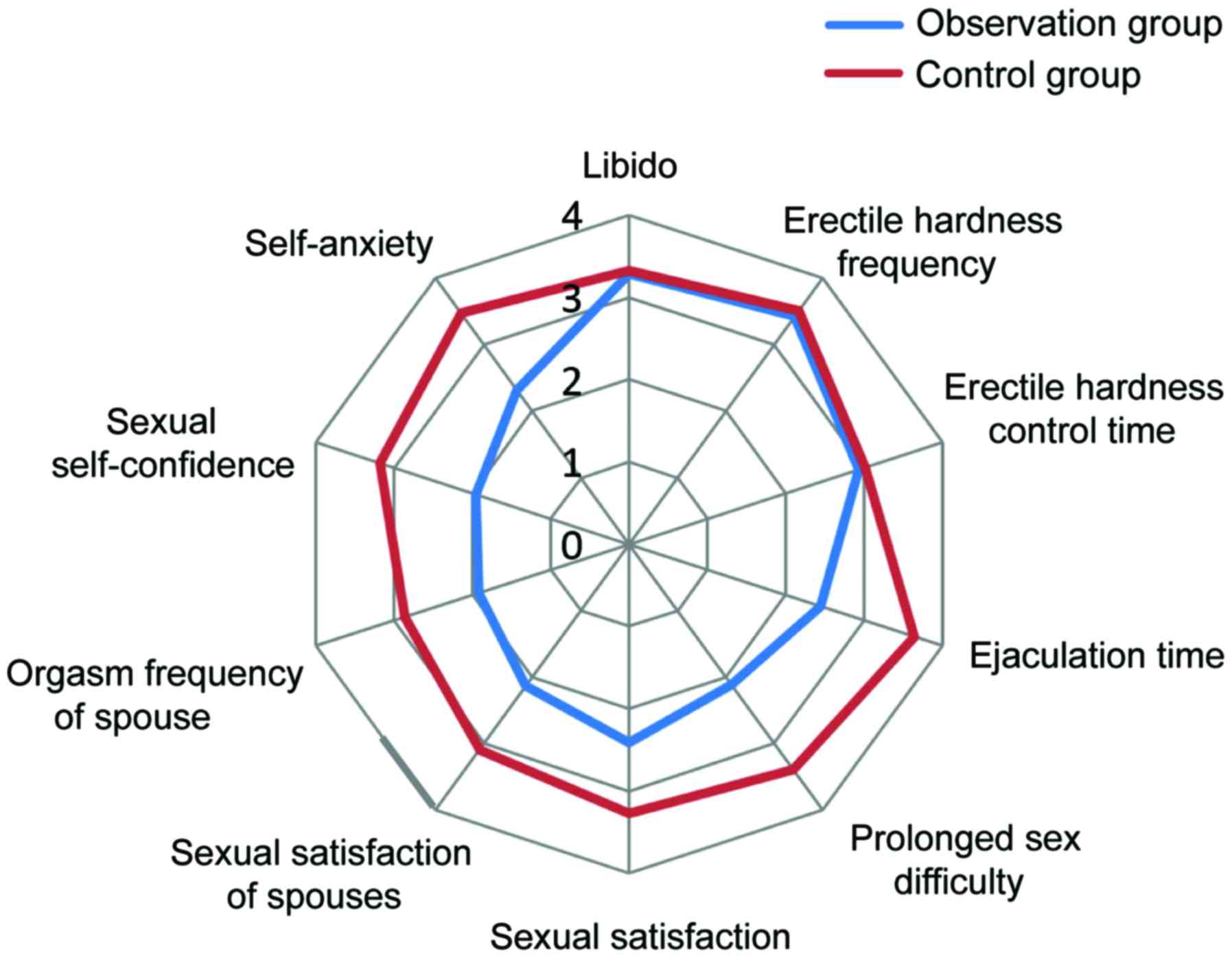
CIPE scores of patients in the two groups 6 months
after operation were compared. The comparison of libido, erectile
hardness frequency and erectile hardness control time of patients
in the two groups had no obvious difference (P>0.05).
Additionally, prolonged sex difficulty and ejaculation time, sexual
satisfaction of spouses, orgasm frequency of spouse, sexual
self-confidence and self-anxiety level of patients in the
observation group were better than those of the control group
(P<0.05), (Fig. 3).
EPQ results
After operation, EPQ of patients in the two groups
were compared. The emotionality, metaphrenia tendency and
dissimulation of the observation group were significantly improved
compared to the control group (P<0.05, Table VI).
 | Table VI.Comparison of EPQ score of patients in
the two groups. |
Table VI.
Comparison of EPQ score of patients in
the two groups.
| Groups | Cases | Introversion and
extroversion | Emotionality | Metaphrenia
tendency | Dissimulation |
|---|
| Observation
group | 51 | 56.95±3.14 | 47.16±3.13 | 39.35±2.14 | 51.13±3.12 |
| Control group | 51 | 47.16±3.23 | 59.33±3.25 | 49.58±2.26 | 56.26±3.17 |
| t-test |
| 15.769 | 19.262 | 23.473 | 8.237 |
| P-value |
| <0.0001 | <0.0001 | <0.0001 | <0.0001 |
Discussion
The growth of phimosis leads to prepuce connecting
with glans closely, which effectively protects the shaft of the
penis and glans. Consequently, immature male children often have
the symptom of redundant prepuce (6,7). The
development of penis, leads to preputial orifice expanding
gradually, and epithelial keratinization separation formation is
covered by glans. After puberty, if the skin of penis still wraps
the glans completely or incompletely, the condition is named
phimosis or redundant prepuce (7–9).
Furthermore, prepuce could be divided into two layers including
inner and outer plate. The cuticle of inner plate is less and its
mucosa surface is moister, which is easily bruised and broken and
integrates with more virus target cells (such as Langerhans cell,
CD4T lymphocyte, macrophage) (10,11).
Langerhans cell belongs to immature dendritic cells, and its
cytoplasm contains a great number of racket and columnar particles.
When the mucosa or skin of some part is infected, Langerhans cells
of root position would identify, capture and dispose the virus and
germ. Therefore, the inner plate is easier to be infected by HIV
than the outer plate (12,13). In a related clinical study, it was
found that the prepuce cavity would form a moist environment for
the patient with phimosis after sexual intercourse, which would
promote the transcription and duplication of the virus HIV.
Circumcision could reduce the infection rate of HIV, especially the
infection rate of HIV from female, up to 60% (14,15).
Traditional operation method is relatively
complicated, and the excision length of inner and outer plate of
prepuce is difficult to control, thus it is not accepted by most
people (16). The present study
results showed that the bleeding of the observation group was less
than that of the control group. Operation time and recovery time of
incision was shorter compared to the control group. The
postoperative complication incidence (5.88%) was also lower than
that of the control group (39.21%), which is closely related to the
advantages of disposable circumcision stitching instrument.
Furthermore, it had less wounds, one main operation and had easy
postoperative care.
HE staining and S-100 protein immunohistochemical
staining were used to observe the histomorphology of the removed
tissue specimens from the patients in the two groups. Blood vessel
counting and nerve fiber counting of tissue specimen in the
observation group were more than those of the control group
(P<0.05). On the other hand, VAS scores 6, 12 and 24 h after
operation of patients in the observation group were significantly
lower than that of the control group (P<0.05). This results in
greater damage to superficial fascia of penis when traditional
operation was applied to wipe out the prepuce, causing damage to
vasculature and nerve fiber. Moreover, it would increase the
incidence of postoperative hematoma, edema and the postoperative
pain degree.
The disposable circumcision stitching instrument
operation only cut the epidermal layer of prepuce, which could
efficiently alleviate complications, such as hematoma and edema. At
the same time, it could effectively prevent the incision of nerve
tissue where nerve fiber distributes densely (17). It also retained the fascia and nerve
tissue between lamina proprias of inner and outer plates of prepuce
as much as possible, to reduce the paresthesia of patients
(18). The results of this study
showed that the sexual dysfunction such as premature ejaculation of
the observation group improved much more than that of the control
group, and the psychological state was also superior in the
observation group (P<0.05). The possible justification for the
above observation could be the direct exposure of glans penis to
the outside and its reduced surface cornification sensitivity after
disposable circumcision stitching instrument operation, leading to
elevated ejaculation threshold. In addition, the disposable method
could keep a favorable tactile function as it improved the quality
of sexual life and the psychological state of patients (19,20).
Collectively, the application of disposable
circumcision stitching instrument operation to circumcision has an
obvious superiority, which is worthy of promoting in clinic.
References
|
1
|
Xie ST, Chen GY, Wei QH, Liu XT, Jiao L
and Tang Y: Outward versus inward placement in Shang Ring
circumcision for phimosis and redundant prepuce in adult men:
Analysis of 527 cases. Zhonghua Nan Ke Xue. 20:325–328. 2014.(In
Chinese). PubMed/NCBI
|
|
2
|
Lei JH, Liu LR, Wei Q, Xue WB, Song TR,
Yan SB, Yang L, Han P and Zhu YC: Circumcision with ‘no-flip Shang
Ring’ and ‘Dorsal Slit’ methods for adult males: A single-centered,
prospective, clinical study. Asian J Androl. 18:798–802. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Larke NL, Thomas SL, dos Santos Silva I
and Weiss HA: Male circumcision and penile cancer: A systematic
review and meta-analysis. Cancer Causes Control. 22:1097–1110.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Namavar MR and Robati B: Removal of
foreskin remnants in circumcised adults for treatment of premature
ejaculation. Urol Ann. 3:87–92. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Pan F, Pan L, Zhang A, Liu Y, Zhang F and
Dai Y: Circumcision with a novel disposable device in Chinese
children: A randomized controlled trial. Int J Urol. 20:220–226.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Abdulwahab-Ahmed A and Mungadi IA:
Techniques of male circumcision. J Surg Tech Case Rep. 5:1–7. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Mavhu W, Frade S, Yongho AM, Farrell M,
Hatzold K, Machaku M, Onyango M, Mugurungi O, Fimbo B, Cherutich P,
et al: Provider attitudes toward the voluntary medical male
circumcision scale-up in Kenya, South Africa, Tanzania and
Zimbabwe. PLoS One. 9:e829112014. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Dias J, Freitas R, Amorim R, Espiridião P,
Xambre L and Ferraz L: Adult circumcision and male sexual health: A
retrospective analysis. Andrologia. 46:459–464. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Jayathunge PH, McBride WJ, MacLaren D,
Kaldor J, Vallely A and Turville S: Male circumcision and HIV
transmission; What do we know? Open AIDS J. 8:31–44. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Fahrbach KM, Barry SM, Anderson MR and
Hope TJ: Enhanced cellular responses and environmental sampling
within inner foreskin explants: Implications for the foreskins role
in HIV transmission. Mucosal Immunol. 3:410–418. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Hirbod T, Bailey RC, Agot K, Moses S,
Ndinya-Achola J, Murugu R, Andersson J, Nilsson J and Broliden K:
Abundant expression of HIV target cells and C-type lectin receptors
in the foreskin tissue of young Kenyan men. Am J Pathol.
176:2798–2805. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Subbiah V and Subbiah IM: Killing two
birds with one stone: BRAF V600E inhibitor therapy for hairy cell
leukemia and Langerhans/dendritic cell sarcoma. Ann Hematol.
92:1149. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Ganor Y and Bomsel M: HIV-1 transmission
in the male genital tract. Am J Reprod Immunol. 65:284–291. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Krieger JN: Male circumcision and HIV
infection risk. World J Urol. 30:3–13. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Peltzer K, Simbayi L, Banyini M and Kekana
Q: HIV risk reduction intervention among medically circumcised
young men in South Africa: A randomized controlled trial. Int J
Behav Med. 19:336–341. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Dinh MH, Fahrbach KM and Hope TJ: The role
of the foreskin in male circumcision: An evidence-based review. Am
J Reprod Immunol. 65:279–283. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Lv BD, Zhang SG, Zhu XW, Zhang J, Chen G,
Chen MF, Shen HL, Pei ZJ and Chen ZD: Disposable circumcision
suture device: Clinical effect and patient satisfaction. Asian J
Androl. 16:453–456. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Cao DH, Dong Q and Wei Q: Commentary on
‘Disposable circumcision suture device: Clinical effect and patient
satisfaction’. Asian J Androl. 17:5162015.PubMed/NCBI
|
|
19
|
Cox G, Krieger JN and Morris BJ:
Histological correlates of penile sexual sensation: Does
circumcision make a difference? Sex Med. 3:76–85. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Homfray V, Tanton C, Mitchell KR, Miller
RF, Field N, Macdowall W, Wellings K, Sonnenberg P, Johnson AM and
Mercer CH: Examining the association between male circumcision and
sexual function: Evidence from a British probability survey. AIDS.
29:1411–1416. 2015. View Article : Google Scholar : PubMed/NCBI
|