|
1
|
Mobley D, Feibus A and Baum N: Benign
prostatic hyperplasia and urinary symptoms: Evaluation and
treatment. Postgrad Med. 127:301–307. 2015.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Kim EH, Larson JA and Andriole GL:
Management of benign prostatic hyperplasia. Annu Rev Med.
67:137–151. 2016.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Aaron L, Franco OE and Hayward SW: Review
of prostate anatomy and embryology and the etiology of benign
prostatic hyperplasia. Urol Clin North Am. 43:279–288.
2016.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Rauch M and Strunk H: Interventional
treatment of benign prostatic hyperplasia: Embolization of the
testicular vein. Radiologe. 57:652–658. 2017.PubMed/NCBI View Article : Google Scholar : (In German).
|
|
5
|
Bach T, Xia SJ, Yang Y, Mattioli S, Watson
GM, Gross AJ and Herrmann TR: Thulium: YAG 2 mum cw laser
prostatectomy: where do we stand? World J Urol. 28:163–168.
2010.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Nunes R, Oliveira R, Carneiro A, Neto AM,
Antunes AA, Bernardo WM and Silvinato A: Brazilian Society of
Urology. Benign prostatic hyperplasia: Laser prostatectomy (PVP).
Rev Assoc Med Bras (1992). 63:929–940. 2017.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Skagseth E Jr: Retropubic prostatectomy. A
clinical review and follow-up study. Nord Med. 77:621–624.
1967.PubMed/NCBI(In Norwegian).
|
|
8
|
Romero-Otero J, García-González L,
García-Gómez B, Justo-Quintas J, García-Rojo E, González-Padilla
DA, Sopeña-Sutil R, Duarte-Ojeda JM and Rodríguez-Antolín A:
Factors influencing intraoperative blood loss in patients
undergoing holmium laser enucleation of the prostate (HoLEP) for
benign prostatic hyperplasia: A large multicenter analysis.
Urology. 132:177–182. 2019.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Meskawi M, Hueber PA, Valdivieso R,
Karakiewicz PI, Pradere B, Misrai V, Chughtai B and Zorn KC:
Complications and functional outcomes of high-risk patient with
cardiovascular disease on antithrombotic medication treated with
the 532-nm-laser photo-vaporization Greenlight XPS-180 W for benign
prostate hyperplasia. World J Urol. 37:1671–1678. 2019.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Biondi-Zoccai GG, Lotrionte M, Agostoni P,
Abbate A, Fusaro M, Burzotta F, Testa L, Sheiban I and Sangiorgi G:
A systematic review and meta-analysis on the hazards of
discontinuing or not adhering to aspirin among 50,279 patients at
risk for coronary artery disease. Eur Heart J. 27:2667–2674.
2006.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Proietti M, Mairesse GH, Goethals P,
Scavee C, Vijgen J, Blankoff I, Vandekerckhove Y and Lip GY:
Belgian Heart Rhythm Week Investigators. Cerebrovascular disease,
associated risk factors and antithrombotic therapy in a population
screening cohort: Insights from the Belgian Heart Rhythm Week
programme. Eur J Prev Cardiol. 24:328–334. 2017.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Stang A: Critical evaluation of the
Newcastle-Ottawa scale for the assessment of the quality of
nonrandomized studies in meta-analyses. Eur J Epidemiol.
25:603–605. 2010.PubMed/NCBI View Article : Google Scholar
|
|
13
|
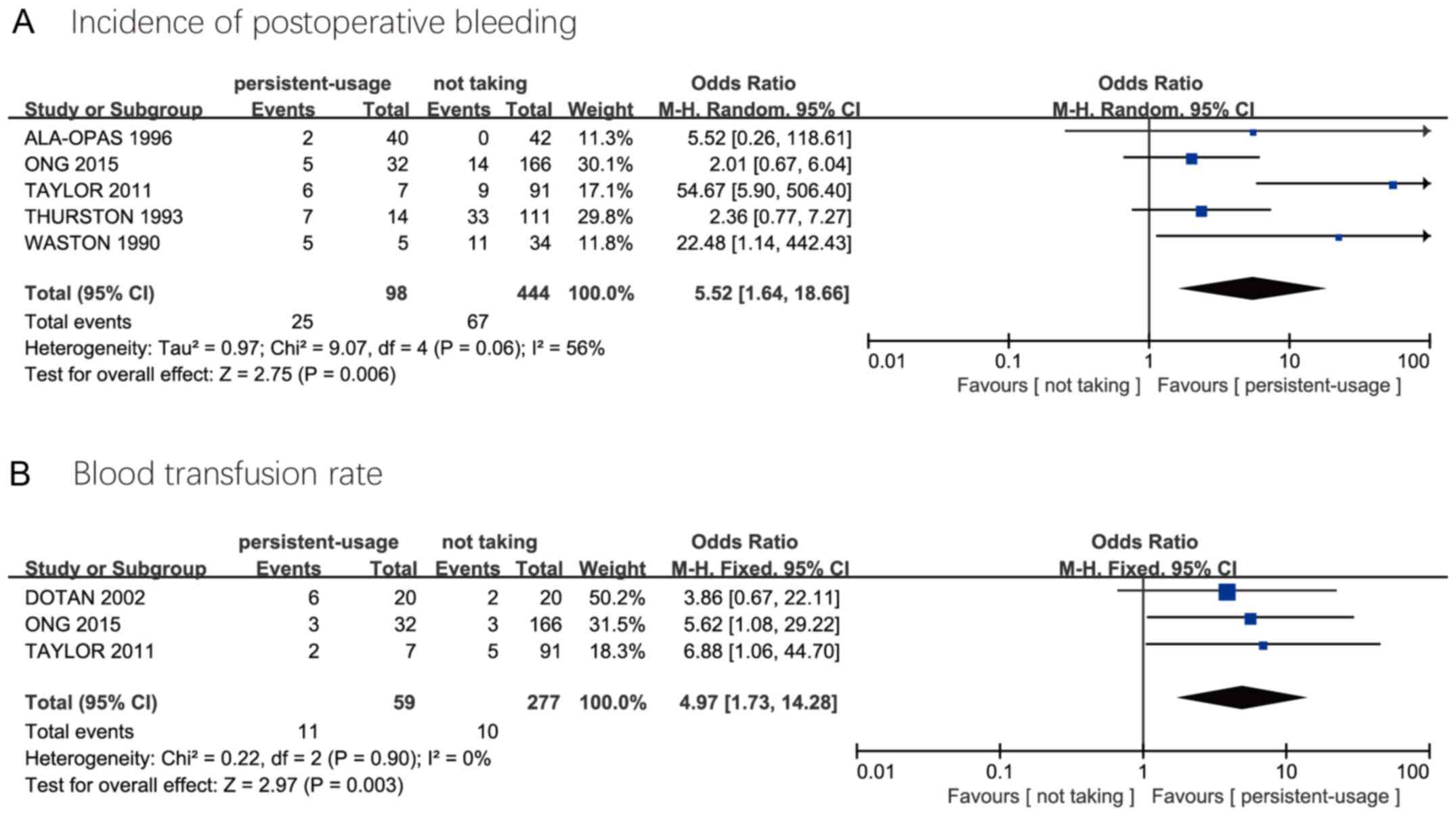
Watson CJ, Deane AM, Doyle PT and Bullock
KN: Identifiable factors in post-prostatectomy haemorrhage: The
role of aspirin. Br J Urol. 66:85–87. 1990.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Thurston AV and Briant SL: Aspirin and
post-prostatectomy haemorrhage. Br J Urol. 71:574–576.
1993.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Ala-Opas MY and Grönlund SS: Blood loss in
long-term aspirin users undergoing transurethral prostatectomy.
Scand J Urol Nephrol. 30:203–206. 1996.PubMed/NCBI View Article : Google Scholar
|
|
16
|
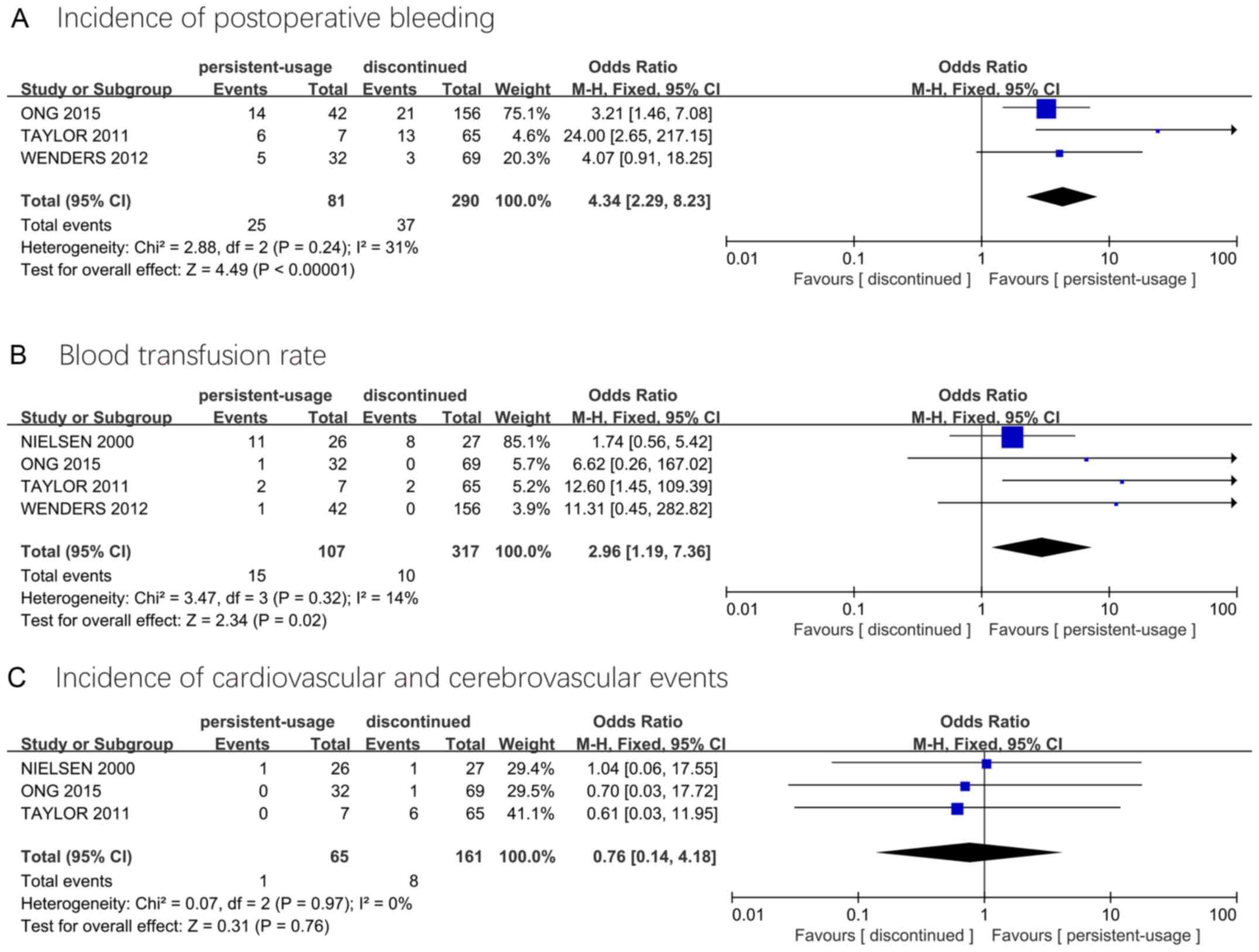
Nielsen JD, Holm-Nielsen A, Jespersen J,
Vinther CC, Settgast IW and Gram J: The effect of low-dose
acetylsalicylic acid on bleeding after transurethral prostatectomy
- a prospective, randomized, double-blind, placebo-controlled
study. Scand J Urol Nephrol. 34:194–198. 2000.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Wenders M, Wenzel O, Nitzke T and Popken
G: Perioperative platelet inhibition in transurethral
interventions: TURP/TURB. Int Braz J Urol. 38:606–610.
2012.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Dotan ZA, Mor Y, Leibovitch I, Varon D,
Golomb J, Duvdevani M and Ramon J: The efficacy and safety of
perioperative low molecular weight heparin substitution in patients
on chronic oral anticoagulant therapy undergoing transurethral
prostatectomy for bladder outlet obstruction. J Urol. 168:610–614.
2002.PubMed/NCBI
|
|
19
|
Taylor K, Filgate R, Guo DY and Macneil F:
A retrospective study to assess the morbidity associated with
transurethral prostatectomy in patients on antiplatelet or
anticoagulant drugs. BJU Int. 108 (Suppl 2):45–50. 2011.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Ong WL, Koh TL, Fletcher J, Gruen R and
Royce P: Perioperative management of antiplatelets and
anticoagulants among patients undergoing elective transurethral
resection of the prostate - A single institution experience. J
Endourol. 29:1321–1327. 2015.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Carmignani L, Macchi A, Ratti D,
Finkelberg E, Casellato S, Bozzini G, Maruccia S, Marenghi C and
Picozzi S: Are histological findings of thulium laser
vapo-enucleation versus transurethral resection of the prostate
comparable? Pathol Oncol Res. 21:1071–1075. 2015.PubMed/NCBI View Article : Google Scholar
|
|
22
|
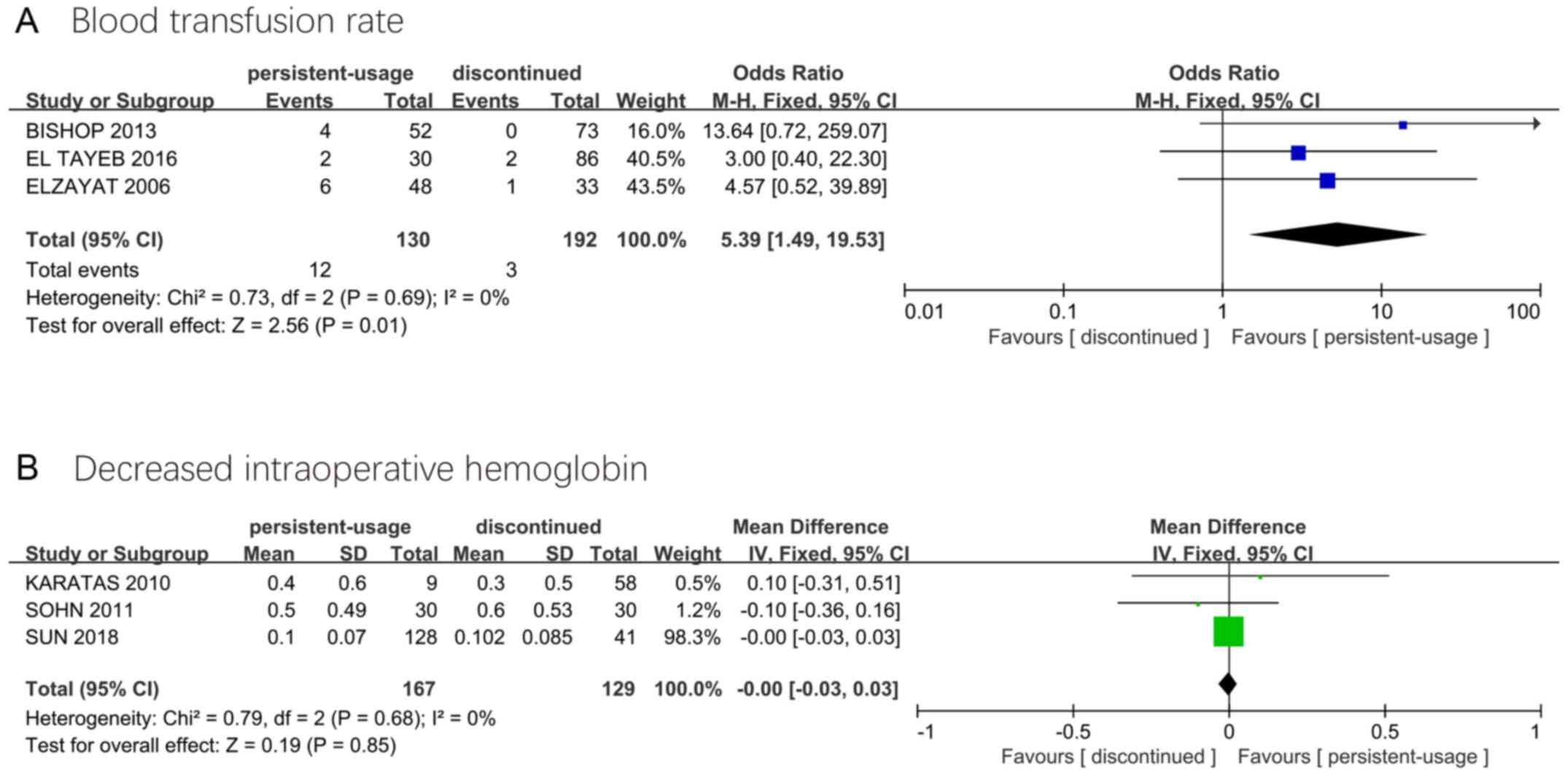
Elzayat E, Habib E and Elhilali M: Holmium
laser enucleation of the prostate in patients on anticoagulant
therapy or with bleeding disorders. J Urol. 175:1428–1432.
2006.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Tyson MD and Lerner LB: Safety of holmium
laser enucleation of the prostate in anticoagulated patients. J
Endourol. 23:1343–1346. 2009.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Bishop CV, Liddell H, Ischia J, Paul E,
Appu S, Frydenberg M and Pham T: Holmium laser enucleation of the
prostate: Comparison of immediate postoperative outcomes in
patients with and without antithrombotic therapy. Curr Urol.
7:28–33. 2013.PubMed/NCBI View Article : Google Scholar
|
|
25
|
El Tayeb MM, Jacob JM, Bhojani N,
Bammerlin E and Lingeman JE: Holmium laser enucleation of the
prostate in patients requiring anticoagulation. J Endourol.
30:805–809. 2016.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Sun J, Shi A, Tong Z and Xue W: Safety and
feasibility study of holmium laser enucleation of the prostate
(HOLEP) on patients receiving dual antiplatelet therapy (DAPT).
World J Urol. 36:271–276. 2018.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Ruszat R, Wyler S, Forster T, Reich O,
Stief CG, Gasser TC, Sulser T and Bachmann A: Safety and
effectiveness of photoselective vaporization of the prostate (PVP)
in patients on ongoing oral anticoagulation. Eur Urol.
51:1031–1038. 2007.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Karatas OF, Alkan E, Horasanli K, Luleci H
and Sarica K: Photoselective vaporization of the prostate in men
with a history of chronic oral anti-coagulation. Int Braz J Urol.
36:190–197. 2010.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Sohn JH, Choi YS, Kim SJ, Cho HJ, Hong SH,
Lee JY, Hwang TK and Kim SW: Effectiveness and safety of
photoselective vaporization of the prostate with the 120 W HPS
Greenlight laser in benign prostatic hyperplasia patients taking
oral anticoagulants. Korean J Urol. 52:178–183. 2011.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Knapp GL, Chalasani V and Woo HH:
Perioperative adverse events in patients on continued
anticoagulation undergoing photoselective vaporisation of the
prostate with the 180-W Greenlight lithium triborate laser. BJU
Int. 119 (Suppl 5):33–38. 2017.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Macchione L, Mucciardi G, Gali' A, Di
Benedetto A, Butticè S and Magno C: Efficacy and safety of prostate
vaporesection using a 120-W 2-µm continuous-wave Tm:YAG laser
(RevoLix 2) in patients on continuous oral anticoagulant or
antiplatelet therapy. Int Urol Nephrol. 45:1545–1551.
2013.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Sener TE, Butticè S, Macchione L, Netsch
C, Tanidir Y, Dragos L, Pappalardo R and Magno C: Thulium laser
vaporesection of the prostate: Can we operate without interrupting
oral antiplatelet/anticoagulant therapy? Investig Clin Urol.
58:192–199. 2017.PubMed/NCBI View Article : Google Scholar
|
|
33
|
Kaciulyte J, Losco L, Maruccia M, Delia G,
Lo Torto F, Di Taranto G, Caputo GG, Berchiolli R, Ribuffo D and
Cigna E: Postsurgical antithrombotic therapy in microsurgery: Our
protocol and literature review. Eur Rev Med Pharmacol Sci.
23:4448–4457. 2019.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Ondeck NT, Bohl DD, McLynn RP, Cui JJ,
Bovonratwet P, Singh K and Grauer JN: Longer operative time is
associated with increased adverse events after anterior cervical
diskectomy and fusion: 15-minute intervals matter. Orthopedics.
41:e483–e488. 2018.PubMed/NCBI View Article : Google Scholar
|
|
35
|
Catanzarite T, Saha S, Pilecki MA, Kim JY
and Milad MP: Longer operative time during benign laparoscopic and
robotic hysterectomy is associated with increased 30-day
perioperative complications. J Minim Invasive Gynecol.
22:1049–1058. 2015.PubMed/NCBI View Article : Google Scholar
|
|
36
|
Bruyère F, Huglo D, Challacombe B, Haillot
O, Valat C and Brichart N: Blood loss comparison during
transurethral resection of prostate and high power GreenLight(™)
laser therapy using isotopic measure of red blood cells volume. J
Endourol. 25:1655–1659. 2011.PubMed/NCBI View Article : Google Scholar
|
|
37
|
Ruszat R, Wyler SF, Seitz M, Lehmann K,
Abe C, Bonkat G, Reich O, Gasser TC and Bachmann A: Comparison of
potassium-titanyl-phosphate laser vaporization of the prostate and
transurethral resection of the prostate: update of a prospective
non-randomized two-centre study. BJU Int. 102:1432–1439.
2008.PubMed/NCBI View Article : Google Scholar
|
|
38
|
Wendt-Nordahl G, Huckele S, Honeck P,
Alken P, Knoll T, Michel MS and Häcker A: Systematic evaluation of
a recently introduced 2-microm continuous-wave thulium laser for
vaporesection of the prostate. J Endourol. 22:1041–1045.
2008.PubMed/NCBI View Article : Google Scholar
|