Introduction
Bronchogenic cyst (BC) is a type of congenital cyst
occurring during embryogenesis due to preintestinal malformations
(1). BC is relatively rare, with a
prevalence rate of 1/68,000-1/42,000(2). Nearly 90% of BC cases have been
reported in the mediastinum, particularly in the posterior
(3). BC of the stomach has been
rarely reported (4). Due to the
heterogeneous clinical presentations and no specific manifestations
of BC of the stomach, this disease is frequently misdiagnosed as
gastrointestinal stromal tumor (GIST). The present study
retrospectively reported on a case of BC of the stomach and
reviewed previously published case reports on this rare
condition.
Case report
A 68-year-old Chinese male was admitted to the
Department of Hepatobiliary Surgery, The Affiliated Hospital of
Southwest Medical University, China in December 2019 due to a
spleen and stomach space mass detected incidentally upon a routine
health examination. The patient had been in good health, denying
any anorexia, nausea, vomiting, diarrhea or constipation. There was
no history of weight loss or fever. The patient's medical history
included hypertension for ~10 years. There were no obvious signs of
pain or tenderness and no lumps to palpate during the physical
examination. Blood routine and tumor markers were within the normal
range. Abdominal ultrasound revealed a heterogeneous lesion in the
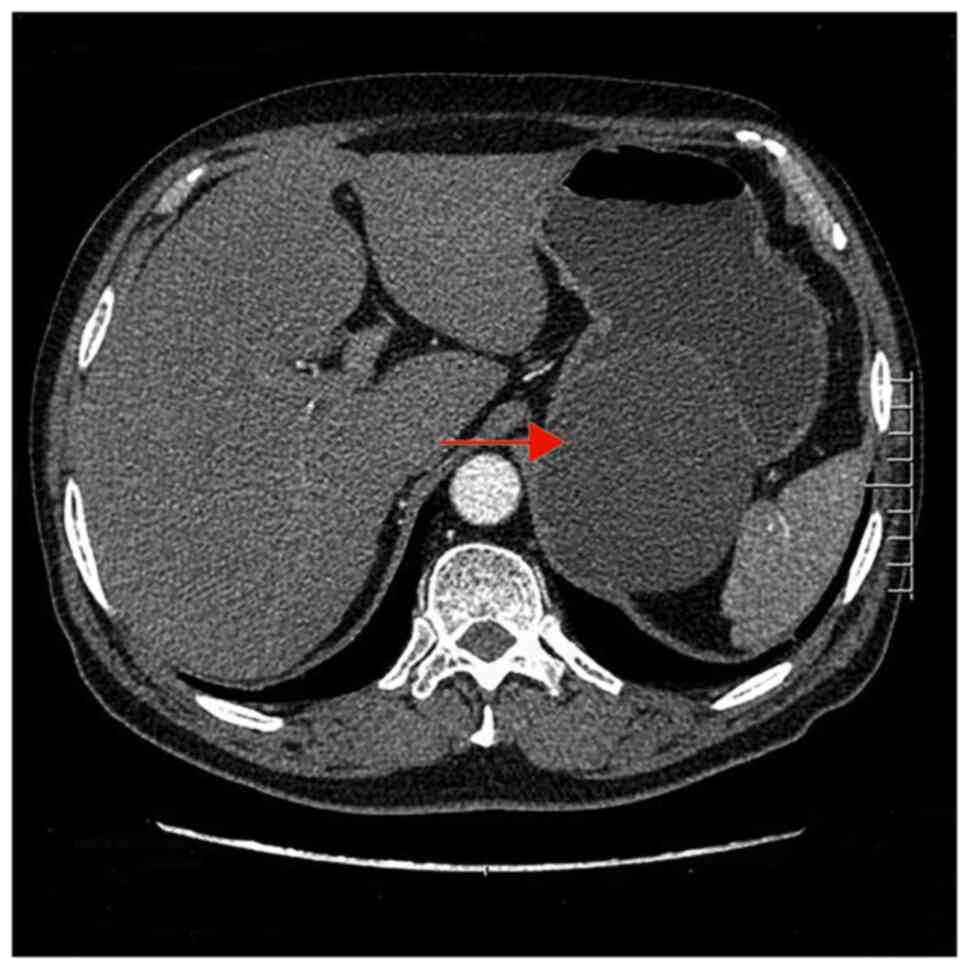
spleen and stomach space measuring 10.0x8.2x7.3 cm. CT displayed a
well-defined, 9.5x8.4x7.8 cm ovate homogenous lesion attached to
the fundus of the stomach, with a CT value of ~17 HU. The density
was uniform, and spot-shaped calcifications were visible on the
edges. The edges were clear and no obvious enhancement was seen on
enhanced CT (Fig. 1). As the
patient rejected endoscopy, no endoscopy was performed prior to the
operation. The preoperative diagnosis was retroperitoneal mass.
During abdominal exploration, an 10x8x8 cm cyst originating from
the bottom of the stomach, with thin walls and smooth edges, was
encountered. It had a clear boundary with the posterior peritoneum
and surrounding organs. The area of adhesion to the stomach was
~2.1x2.3 cm. Cystic lesions were isolated and were not connected to
the stomach cavity. The capsule was filled with yellow-white
mucous, gelatinous contents. Considering the close relationship
between the cyst and the stomach, the final decision was to remove
the cyst at the bottom of the stomach and repair the stomach wall.
The cysts originated from the serous muscle layer of the gastric
wall. The cyst was separated and completely removed. The gastric
muscle was repaired by intermittent suture. For histopathology, the
tissue of the cyst wall was selected while avoiding the calcified
part. Histopathology was performed according to standard protocols.
The sample was fixed with 15% formaldehyde at room temperature for
24 h, washed for 20 min after fixation and then embedded in
paraffin. Subsequently, the specimen was cut into 50-µm slices and
the cut slices were flattened in hot water, attached to a glass
slide and dried in a 45˚C thermostat. Xylene was used to remove the
paraffin wax from the slices, followed by rehydration with a
descending series of graded alcohols. Finally, the sample was
immersed in distilled water and stained with hematoxylin and eosin
(H&E) at 60˚C for 30 min. The transparent slices were mounted
with coverslips with and sealed with gum before they were observed
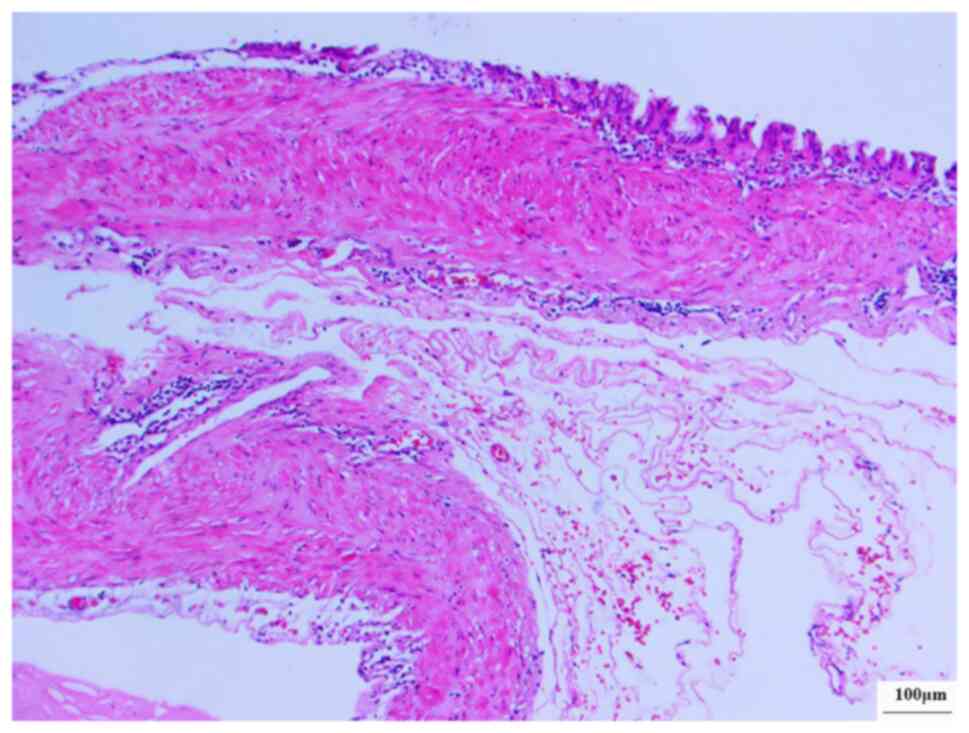
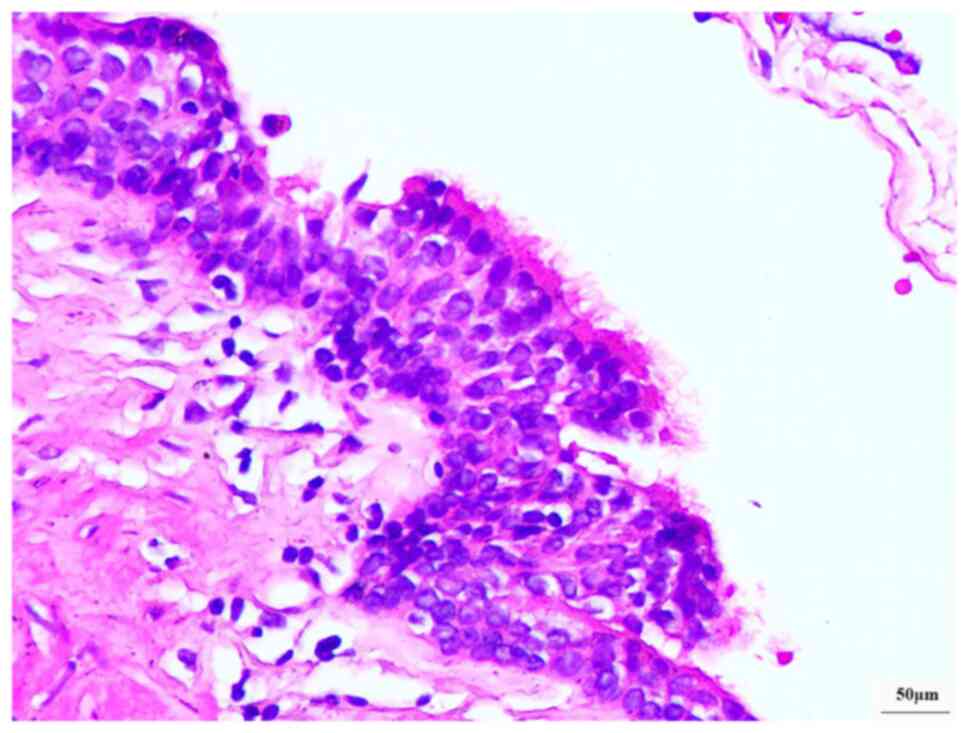
under the light microscope. Histopathological examination of the
resected specimen revealed that the cyst wall was lined by
pseudostratified ciliated columnar epithelium and was without
cellular atypia (Figs. 2 and
3). Based on the abovementioned
pathologic features, the patient was diagnosed with BC of the
stomach. The patient's recovery was smooth and he was discharged
after 8 days.
Discussion
Congenital cyst is a rare type of benign gastric
lesion. Several types of congenital cyst have been reported in the
literature, including foregut cysts, gastric replication cysts and
bronchial cysts. The difference between them is the type of lining
epithelium and surrounding layers, which may contain smooth muscle,
cartilage, bronchial glands or may not be present. BC is a term
traditionally used to describe pseudostratified columnar or
cuboidal ciliated (respiratory) epithelium with cartilage or
glandular tissue on the inner wall of the cyst (5). BC is a type of foregut-derived
dysplasia, most commonly in the mediastinum, and is rarely seen in
the abdomen or retroperitoneum (6).
Because they are produced by abnormal budding of the original
tracheobronchial tree, they are usually located in the mediastinum
or lung parenchyma (7). However, in
some cases, they may detach and migrate to the abdomen. Depending
on the degree of migration, they can be found anywhere in the
abdominal cavity, including the ileal mesentery and hepatogastric
ligament (8,9). The occurrence of BC in the stomach
wall is very rare.
The current knowledge regarding the clinical
features and optimal treatment of BC of the stomach is limited. A
systematic review of the PubMed database was performed using the
following keywords: [bronchogenic cysts (Title)] and [stomach
(Title)], but it yielded only 10 potentially relevant articles.
Exclusion of articles without full text (n=3, English language)
resulted in a final count of 6 articles, describing 8 cases
(10-15),
including the present case (Table
I). BC of the stomach appeared to be a disease detected in
older individuals (from 37 to 68 years of age) and there was no
gender difference (4 females and 4 males). Cysts ranged in diameter
from 1.5 to 15 cm. They were mostly located on the lesser curved
side of the stomach and the second most frequent location was at
the bottom and back of the stomach. Upper abdominal pain, nausea
and vomiting were the most common complaints and symptoms. These
are consistent with the findings described in the present report.
Symptoms are usually related to enlarged cysts, secondary
infections, perforations or compression of adjacent structures.
 | Table IPreviously reported cases of
bronchogenic cyst of the stomach. |
Table I
Previously reported cases of
bronchogenic cyst of the stomach.
| First author
(year) | Age (years)/sex | Diameter (mm) | Symptoms | Location | Treatment | Outcome | (Refs.) |
|---|
| Keohane (1988) | 64/F | 150 | Epigastric pain | Posterior | Resection | NR | (10) |
| Song (2005) | 62/F | 15 | - | U/less | Resection | NR | (11) |
| Shibahara (2009) | 43/M | 90 | Epigastric pain | U/less | Resection | NR | (12) |
| Yang (2013) | 50/M | 75 | - | Fundus | Resection | Alive/24 mo | (13) |
| Yang (2013) | 37/F | 100 | - | Posterior | Resection | NR | (13) |
| Chhaidar (2017) | 65/M | 80 | Epigastric pain | U/less | Resection | Alive/24 mo | (5) |
| Han (2019) | 62/F | 60 | Epigastric pain | U/less | Resection | NR | (14) |
| Present study
(2020) | 68/M | 100 | - | Fundus | Resection | Alive/to date | (-) |
To date, the etiology and mechanisms of BC of the
stomach remain to be fully elucidated. The occurrence of BC in the
abdominal cavity may be explained as follows: In the early
embryonic stage, the thoracic cavity and the abdominal cavity are
connected by a pericardial abdominal cavity tube, and the abdominal
cavity is divided into two separate cavities by fusion of the
pleura and the peritoneum, which is a component of the diaphragm.
In cases developing BC, the abnormal buds of the tracheobronchial
tree were cutoff and migrated to the abdomen (13).
Accurate preoperative diagnosis remains a challenge
and there are no characteristic changes in laboratory tests. No
distinctive radiologic characteristics were apparent. On
conventional imaging, such as CT, BC lesions present as definite
cystic lesions with or without calcification (16). On MRI, lesions appear as equal to
high intensity on T1-weighted images and high intensity on
T2-weighted images (1,15,16).
However, these imaging features are similar to GIST and are
frequently misdiagnosed. Endoscopic ultrasonography (EUS) may help
determine the exact location of the cyst in the stomach wall. CT-
or EUS-guided biopsy may reveal mucus-like substances, providing
clues for correct diagnosis It should be performed as an important
supplementary method to secure a definitive diagnosis in some cases
(3,16). Possible complications include
recurrence, ulceration, infection and hemorrhage.
To date, due to the small number of cases reported
worldwide, no optimal treatment strategy for the clinical
management of BC of the stomach has been established. In the
reported cases, all patients underwent surgical resection of the BC
of the stomach, and BC of the stomach with malignant transformation
was rare. The possible pathology may be as follows: Chronic
inflammation, repeated erosion and regeneration may lead to
atypical hyperplasia or canceration (12,17).
Most patients with non-cancerous BC recovered well after surgery
and there was no recurrence or metastasis during the follow-up.
A limitation of the present study was that no
intraoperative images and photos of resected specimens were
acquired. So far, there is no standard treatment for this rare
disease. The review of the relevant literature as part of the
present study indicated that surgery may be the best choice for
diagnosis and treatment, as long as the patient's physical
condition allows, but the choice of treatment should be based on
the size, location and number of cystic lesions and the patient's
physical condition. Further reports will enhance the current
understanding of this rare disease and help improve its
management.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
BS analyzed the data, drafted the manuscript and
critically revised the draft. AKW analyzed the data and critically
discussed the results. HC and XKY performed the literature search
and selection. BLQ performed the pathological analysis. YJ
collected the clinical data. WGF and QL performed the operation and
discussed the manuscript. WGF and JL were involved in the
conception of the study and finalized the draft. All authors read
and approved the final manuscript.
Ethics approval and consent to
participate
The present study was approved by the Ethics
Committee of The Affiliated Hospital of Southwest Medical
University (Luzhou, China; approval reference no. KY2019053).
Patient consent for publication
Written consent was provided by the patient for the
publication of his data and images.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Tu C, Zhu J, Shao C, Mao W, Zhou X, Lin Q,
Li Z, Zhang J, Zhou Q and Chen W: Gastric bronchogenic cysts: A
case report and literature review. Exp Ther Med. 11:1265–1270.
2016.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Limaïem F, Ayadi-Kaddour A, Djilani H,
Kilani T and El Mezni F: Pulmonary and mediastinal bronchogenic
cysts: A clinicopathologic study of 33 cases. Lung. 186:55–61.
2008.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Sato M, Irisawa A, Bhutani MS, Schnadig V,
Takagi T, Shibukawa G, Wakatsuki T, Imamura H, Takahashi Y, Sato A,
et al: Gastric bronchogenic cyst diagnosed by endosonographically
guided fine needle aspiration biopsy. J Clin Ultrasound.
36:237–239. 2008.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Hedayati N, Cai DX and Mchenry CR:
Subdiaphragmatic bronchogenic cyst masquerading as an ‘adrenal
incidentaloma’. J Gastrointest Surg. 7:802–804. 2003.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Chhaidar A, Ammar H, Abdessayed N, Azzaza
M, Gupta R, Abdennaceur N, Bdioui A, Mokni M and Ali AB: Large
bronchogenic cyst of stomach: A case report. Int J Surg Case Rep.
34:126–129. 2017.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Liang MK, Yee HT, Song JW and Marks JL:
Subdiaphragmatic bronchogenic cysts: A comprehensive review of the
literature. Am Surg. 71:1034–1041. 2005.PubMed/NCBI
|
|
7
|
Aktoğu S, Yuncu G, Halilçolar H, Ermete S
and Buduneli T: Bronchogenic cysts: Clinicopathological
presentation and treatment. Eur Respir. 9:2017–2021.
1996.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Petrina A, Boselli C, Cirocchi R,
Covarelli P, Eugeni E, Badolato M, Finocchi L, Trastulli S and Noya
G: Bronchogenic cyst of the ileal mesentery: A case report and a
review of literature. J Med Case Rep. 4(313)2010.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Gou Y, Wang YG, Fang H, Xu X, Yu W, Zhang
K and Yu Y: Bronchogenic cyst in the hepatogastric ligament
masquerading as an esophageal mesenchymal tumor: A case report. Int
J Clin Exp Pathol. 8:15307–15311. 2015.PubMed/NCBI
|
|
10
|
Keohane ME, Schwartz I, Freed J and Dische
R: Subdiaphragmatic bronchogenic cyst with communication to the
stomach: A case report. Hum Pathol. 19:868–871. 1988.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Song SY, Noh JH, Lee SJ and Son HJ:
Bronchogenic cyst of the stomach masquerading as benign stromal
tumor. Pathol Int. 55:87–91. 2005.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Shibahara H, Arai T, Yokoi S and Hayakawa
S: Bronchogenic cyst of the stomach involved with gastric
adenocarcinoma. Clin J Gastroenterol. 2:80–84. 2009.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Yang X and Guo K: Bronchogenic cyst of
stomach: Two cases report and review of the English literature.
Wien Klin Wochenschr. 125:283–287. 2013.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Han WG, Xue HD and Pan WD: Bronchogenic
cyst of stomach: Report of one case. Zhongguo Yi Xue Ke Xue Yuan
Xue Bao. 41:572–574. 2019.PubMed/NCBI View Article : Google Scholar : (In Chinese).
|
|
15
|
Sun L, Lu L, Fu W, Li W and Liu T: Gastric
bronchogenic cyst presenting as a gastrointestinal stromal tumor.
Int J Clin Exp Pathol. 8:13606–13612. 2015.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Belli S, Noyan T, Kayaselçuk F and Erbay
G: Gastric duplication (bronchogenic) cyst mimicking a
gastrointestinal stromal tumour. Ulus Cerrahi Derg. 29:35–37.
2013.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Murakami M, Machida M, Kobayashi Y, Ogura
J, Ichikawa T and Kumazaki T: Retroperitoneal bronchogenic cyst: CT
and MR imaging. Abdom Imaging. 25:444–447. 2000.PubMed/NCBI View Article : Google Scholar
|