Introduction
Atopic dermatitis (AD), or eczema, is a chronic
inflammatory skin disease with a prevalence of 10–20% in children
and 1–3% in adults (1). AD has a
complex etiology that encompasses immunologic responses,
susceptibility factors, environmental triggers and compromised
skin-barrier function (2). AD is
accompanied by symptoms of pruritus, erythema, edema and xerosis
(3), and the underlying
mechanisms of these skin diseases are associated with genetic and
environmental factors of AD pathogenesis (4). Immunoglobulin E (IgE), which has a
key role in the pathogenesis of allergies, is produced by
B-lymphocytes following exposure of a dendritic cell to a foreign
antigen under the control of T-helper lymphocytes (2,4,5).
The association of ~70–85% of human AD to IgE hyper-production has
been demonstrated and the extent of IgE sensitization is directly
associated with the severity of the disease (6). When two or more molecules of IgE
bind to the surface of an immune cell and are simultaneously linked
to its specific allergen, the immune cell immediately releases
pre-formed inflammatory mediators, including histamine, which
induces an immediate allergic response or early phases thereof
(2). Following IgE release, the
immune cells also synthesize newly formed inflammatory molecules,
including leukotriene D4, prostaglandins and cytokines, including
tumor necrosis factor-α (TNF-α), nuclear factor-κB (NF-κB),
interleukin-4 (IL-4), IL-5 and IL-13 (2,7–10).
Among them, the cytokines IL-4 and IL-13 are known as classic
markers of the allergic reaction (10–12). To study the pathogenesis of
allergic contact dermatitis, animal models of AD are used, which
are established by induction of a contact hypersensitivity by
topical application of 2,4-dinitrochlorobenzene (DNCB) to the skin
(13). The allergen DNCB can be
internalized by local antigen-presenting cells, including dermal
dendritic cells and macrophages, is subsequently processed and
presented to T cells in the lymph nodes for activation (5,14),
and can cause AD-like symptoms, including eczema, erythema, scaling
and hemorrhaging in skin lesions (2,6,10,15,16).
Chamaecyparis obtusa (C. obtusa) is a
species of the cypress family and a tropical tree native to the
central part of Japan and the Southern part of Korea. Essential oil
extracted from C. obtusa contains several types of terpene,
including monoterpenes, sesquiterpenes and diterpenes. The major
constituents in extracts of C. obtusa leaves are sabinene,
limonene, bornyl acetate, (+)-borneol, α-terpineol and elemol, and
those in fruit extracts are myrcene, γ-terpinene, p-cymene,
(+)-borneol, α-terpineol and β-caryophyllene (17,18). Although the underlying mechanisms
of action of the essential oil of C. obtusa are yet to be
fully elucidated, the essential oil or terpenes have been used as
anti-microbial agents in foods and cosmetics (18–20). Arima et al (21) demonstrated the anti-bacterial
activity of hinokitiol on staphylococci isolated from atopic
dermatitis lesions, and hinokitiol caused a decrease in the number
of viable bacterial cells from atopic-eczematous lesions. The crude
extract of C. obtusa reduced allergic reactions in a mouse
model of AD (22) and effectively
suppressed the serum levels of IgE, pro-inflammatory cytokines and
mast cell appearance underneath the dermis and hypodermis (22). C. obtusa, which has been
regarded as the most representative medicinal plant, contains
active terpene compounds, which may have pharmacological effects
(23). However, the underlying
mechanisms and precise active components within the composition of
C. obtusa have remained to be fully identified.
The present study hypothesized that the key active
components of C. obtusa (elemol, β-eudesmol and γ-eudesmol;
elemol and γ-eudesmol were extracted from F5-4, and β-eudesmol was
purchased from Sigma-Aldrich, St. Louis, MO, USA) are the effective
in the treatment of symptoms of AD. The anti-atopic properties of
the fractions, sub-fractions and principal components of C.
obtusa were assessed in in vitro and in vivo
models of AD were assessed in order to test their applicability as
pharmaceutical preparations.
Materials and methods
Essential oil of C. obtuse
C. obtusa was collected from the arboretum of
Seoul National University (Gyeonggi, Korea). It was identified and
verified by a wood and forest specialist. The yield of the
essential oil was 3.6%. The essential oil from freshly cut needles
and stems of C. obtusa was obtained by steam distillation
using a manufactured apparatus with a condenser. Distillation (EAMS
9501; Misung Scientific Co. Ltd., Seoul, Korea) was continued for
2–3 h at 100°C and the volatile compounds containing the
water-soluble fraction were allowed to settle for 20 min. The
essential oil layer was separated and finally purified using a
microfilter (pore size, 0.45 µm) and the water vapor
distillation method (24). C.
obtusa oil was then fractionated by silica gel column
chromatography for screening and identification of active
components of the essential oil. For this, the essential oil
(240.40 g) was loaded onto a silica gel column (230–400 mesh,
15×29.5 cm; Merck, Darmstadt, Germany) and eluted with a mixture of
hexane and ethyl acetate (20:1 v/v) at a flow rate of 20 ml/min;
100-ml fractions were collected in Erlenmeyer flasks. The fractions
were pooled into seven groups according to their composition, as
visualized by thin layer chromatography [TLC; silica gel (60
mesh)-precoated glassplate; Merck] using 50% sulfuric acid and 50%
hexane (Sigma-Aldrich), ethyl acetate (Sigma-Aldrich) (8:1, v/v) as
the developing solvent. After concentrating in a rotary vacuum
evaporator (SB-1200; Eyela, Tokyo, Japan), the fractions were
labeled 1–7. Fraction 7 was further fractionated by silica gel
column chromatography. For this, fraction 7 (5 ml) was loaded onto
a silica gel column (60 mesh, 4.5×31 cm; Merck) and eluted with a
mixture of hexane and ethyl acetate (10:1, v/v) at a flow rate of
20 ml/min. A total of 43 fractions (250 ml) were collected in
Erlenmeyer flasks. The residue adsorbed to the silica gel [silica
gel 60 (0.015–0.040 mm), Merck] was re-eluted with 1 liter of ethyl
acetate and labeled fraction 44. The original eluate was pooled
into seven fractions according to composition, as visualized by TLC
(HX41991254; Merck) using 50% sulfuric acid and 50% hexane/ethyl
acetate (8:1, v/v) as the mobile phase. After concentrating with a
rotary vacuum evaporator, the fractions were labeled serially and
used in subsequent experiments. A Mass Spectrometry (GC-MS)
detector for the analysis of the complex chemical structure of the
essential oil was used (stationary phase, DB-5 column 32×0.25 mm;
coating thickness of 0.25 µm; Agilent Technologies, Santa
Clara, CA, USA) and the carrier gas was He at 1 ml/min. The working
conditions were: injection 300°C, detector 250°C. The oven
temperature was increased from 40 to 280 at 5°C/min, with an
initial holding time and a final holding time of 10 min. A split
ratio of 5:1 and a mass range from 50 to 800 m/z was used. Peak
identification was based upon mass spectra comparison with the NIST
08 (National Institute of Standard and Technology) library and with
spectra of injected standards. The identification of the retention
index of individual compounds was based on comparison of their
relative retention times with n-alkane
(C8-C30) mixture in DB-5 column, and by
matching their mass spectra of peaks from NIST 08 (National
Institute Standard Technology) library.
RBL-2H3 cell culture
RBL-2H3 cells (CRL-2256™; American Type Culture
Collection, Manassas, VA, USA) were cultured in 10% fetal bovine
serum (FBS; Gibco-BRL, Life Technologies, Carlsbad, CA, USA) with
Dulbecco’s modified Eagle’s medium (DMEM) (Gibco-BRL) supplemented
with 100 µg/ml streptomycin (Gibco-BRL), 100 U/ml penicillin
(Gibco-BRL) and 5 µg/ml plasmocin (pH 7.4; Invivogen, San
Diego, CA, USA). RBL-2H3 cells were plated and grown to 70–80%
confluence in six-well plastic tissue culture dishes (Nunc™,
Roskilde, Denmark). RBL-2H3 cells were placed at 37°C in a
humidified atmosphere of 95% air and 5% CO2.
RNA extraction and reverse transcription
quantitative polymerase chain reaction (RT-qPCR)
RBL-2H3 cells were grown on 6-well plates
(1×106 cells/well) and experiments were performed 24 h
after plating. The cells were treated with concanavalin A (Con A,
25 µg/ml; Sigma-Aldrich) for 1 h, and then washed 4 times
with Dulbecco’s phosphate buffered-saline (DPBSA; Gibco-BRL). The
cells were then treated with cyclosporin A (CsA, 1 µg/ml;
Sigma-Aldrich) for 1 h. Total RNA was extracted from RBL-2H3 cells
and mouse skin using TRIzol reagent (Invitrogen, Life Technologies)
according to the manufacturer’s instructions. RNA concentrations
were measured using a micro-plate spectrophotometer (Epoch; BioTek
Inc., Winooski, VT, USA) at 260 nm. The RNA quality was evaluated
by electrophoresis in 1% agarose gels (MP Biomedicals, Irvine, CA,
USA). Total RNA (1 µg) was reverse transcribed into
first-strand complementary DNA (cDNA) using Moloney murine leukemia
virus reverse transcriptase (Invitrogen, Life Technologies) and
random primers (9-mer; Takara Bio Inc., Shiga, Japan). Each cDNA
sample (1 µl) was amplified with 10 µl 2X
SYBR® Premix Ex Taq™ (Takara Bio Inc.) and 10 pmol of
each primer. Amplification was performed using a 7300 Real-time PCR
system (Applied Biosystems, Thermo Fisher Scientific, Waltham, MA,
USA) with the following parameters: Denaturation at 95°C for 5 min,
followed by 40 cycles of denaturation at 95°C for 30 sec, annealing
at 60°C for 30 sec, extension at 72°C for 45 sec and final
elongation at 72°C for 10 min. Sequences of the oligonucleotide
primers as shown in Table I.
Relative expression levels in each sample (normalized to that of
β-actin) were determined using RQ software version 1.3 (Applied
Biosystems).
 | Table IOligonucleotide sequences for
quantitative real-time polymerase chain reaction. |
Table I
Oligonucleotide sequences for
quantitative real-time polymerase chain reaction.
| Gene | Primer sequence
(5′-3′) |
|---|
| TNF-α | F:
cctgtagcccacgtcgtag
R: ggagtagacaaggtacaaccc |
| IL-1β | F:
gaaatgccaccttttgacagtg
R: ctggatgctctcatcaggaca |
| IL-4 | F:
tgatgtacctccgtgcttga
R: aggacatggaagtgcaggac |
| IL-6 | F:
ctgcaagagacttccatccag
R: agtggtatagacaggtctgttgg |
| IL-13 | F:
ctggaatccctgaccaacat
R: ccatagcggaaaagttgctt |
| IκBα | F:
gcaatcatccacgaagagaagcc
R: caggatcacagccagctttcagaag |
| β-actin | F:
ttctacaatgagctgcgtgtg
R: accagaggcatacagggaca |
β-hexosaminidase secretion assay
Degranulation was determined by measuring the
release of a granule marker β-hexosaminidase. RBL-2H3 cells were
grown on 48-well plates (2.5×105 cells/well) and
experiments were performed 24 h after plating. Cells were then
treated overnight with 1 µg/ml IgE (Sigma-Aldrich). For
removal of excess IgE prior to stimulation, cells were washed four
times with extracellular buffer (125 mM NaCl, 5 mM KCl, 1.5 mM
CaCl2, 1.5 mM MgCl2 and 20 mmol
4-(2-hydroxyethyl)-1-piperazineethane-sulfonic acid, pH 7.3). The
cells were then stimulated with 800 ng/ml dinitrophenyl human serum
albumin (DNP-HSA; Sigma-Aldrich), suspended in 500 µl
extracellular buffer with 0.1% bovine serum albumin and incubated
at 37°C for 1 h. Following incubation, 50 µl of the
supernatant was incubated with 200 µl of 1 mM
p-nitrophenyl N-acetyl-β-D-glucosamine
(Sigma-Aldrich) in 0.05 M citrate buffer (pH 4.5) for 3 h at 37°C.
The enzyme reaction was terminated by addition of 500 µl
sodium carbonate buffer (0.05 M; pH 10.0) and the optical density
of each reaction was read at 405 nm (SupraMax340; Molecular
Devices, Silicon Valley, CA, USA).
Experimental animals
BALB/c mice (7 weeks old, male, weighing 20–25 g;
total n=30, n=5 per group) were purchased from Koatech (Pyeongtaek,
Gyeonggi, Korea), and were allowed to adapt to laboratory
conditions (temperature: 20±2°C, relative humidity: 50%, light/dark
cycle: 12 h) for 1 week. Mice were fed a standard rodent chow diet
(Nestlé Purina, St Louis, MO, USA), and the mice were euthanized 24
h after the last treatment by ether (Sigma-Aldrich) anesthesia. The
animal experiments were approved by the Chungbuk National
University Animal Care and Use Committee (Chungbuk, Republic of
Korea) and all procedures were performed in accordance with the
Guide for the Care and Use of Laboratory Animals published by the
National Institutes of Health.
Induction of AD-like skin lesions in
DNCB-treated mice
DNCB (Sigma-Aldrich) dissolved in acetone was used
to induce dermatitis in BALB/c mice. Briefly, hair was removed from
a 2×4-cm region spanning from the neck to the pelvis and the dorsal
skins were sensitized with 100 µl 2% DNCB (acetone/olive
oil, 4:1) for three days of the first week. After the first
sensitization, 100 µl 0.5% DNCB was repeatedly applied to
the dorsal skin for an additional eight weeks three times a week.
At the same time, the vehicle (acetone/olive oil, 4:1; negative
control), clobetasol propionate (CP) ointment (a therapeutic
control; Glaxo Operations UK Ltd., Greenford, UK) or elemol (2, 5
and 10%) was evenly applied daily to the entire dorsal skin of the
mice three times a week. No substances were applied to the skin
surface on the last day of the experiment. The mice were then
sacrificed, and the skin, lymph nodes and blood samples were
collected for further analysis.
Measurement of serum IgE
Blood samples were collected directly from the
plexus venes using a capillary tube at the end of the experiment.
Serum was obtained by centrifugation at 3,000 × g for 10 min at 4°C
and stored at −70°C until use. The serum IgE levels were measured
using a mouse IgE ELISA Ready-Set-Go kit (eBiosciences, San Diego,
CA, USA) following the manufacturer’s instructions.
Histopathological analysis
The dermis tissue was fixed by inflating the tissue
with 10% formalin (Junsei Chemical, Tokyo, Japan). The tissues were
then embedded in paraffin, cut into sections (5 microns) and
stained with hematoxylin and eosin (H&E; Sigma-Aldrich). All
tissue samples were examined, photographed and scored in a blinded
fashion under light microscopy (BX51; Olympus, Tokyo, Japan).
Images were captured using an Olympus DP controller and manager at
×100 magnification. To investigate the distribution of mast cells
beneath the dermis and hypodermis, the prepared tissues were
stained with toluidine blue (Sigma-Aldrich), and images were
captured on an Olympus DP controller and manager under a microscope
at ×400 magnification. The number of mast cells in a
1-mm2 area was counted under a microscope at ×400
magnification.
Statistical analysis
Values are expressed as the mean ± standard error of
the mean and were analyzed by one-way analysis of variance followed
by Tukey’s multiple comparison test. Statistical analyses were
performed using GraphPad Prism software v4.0 (GraphPad Software
Inc., La Jolla, CA, USA). P<0.05 was considered to indicate a
statistically significant difference between values.
Results
C. obtusa oil ameliorates skin lesions
and attenuates increases in serum IgE levels in mice with AD
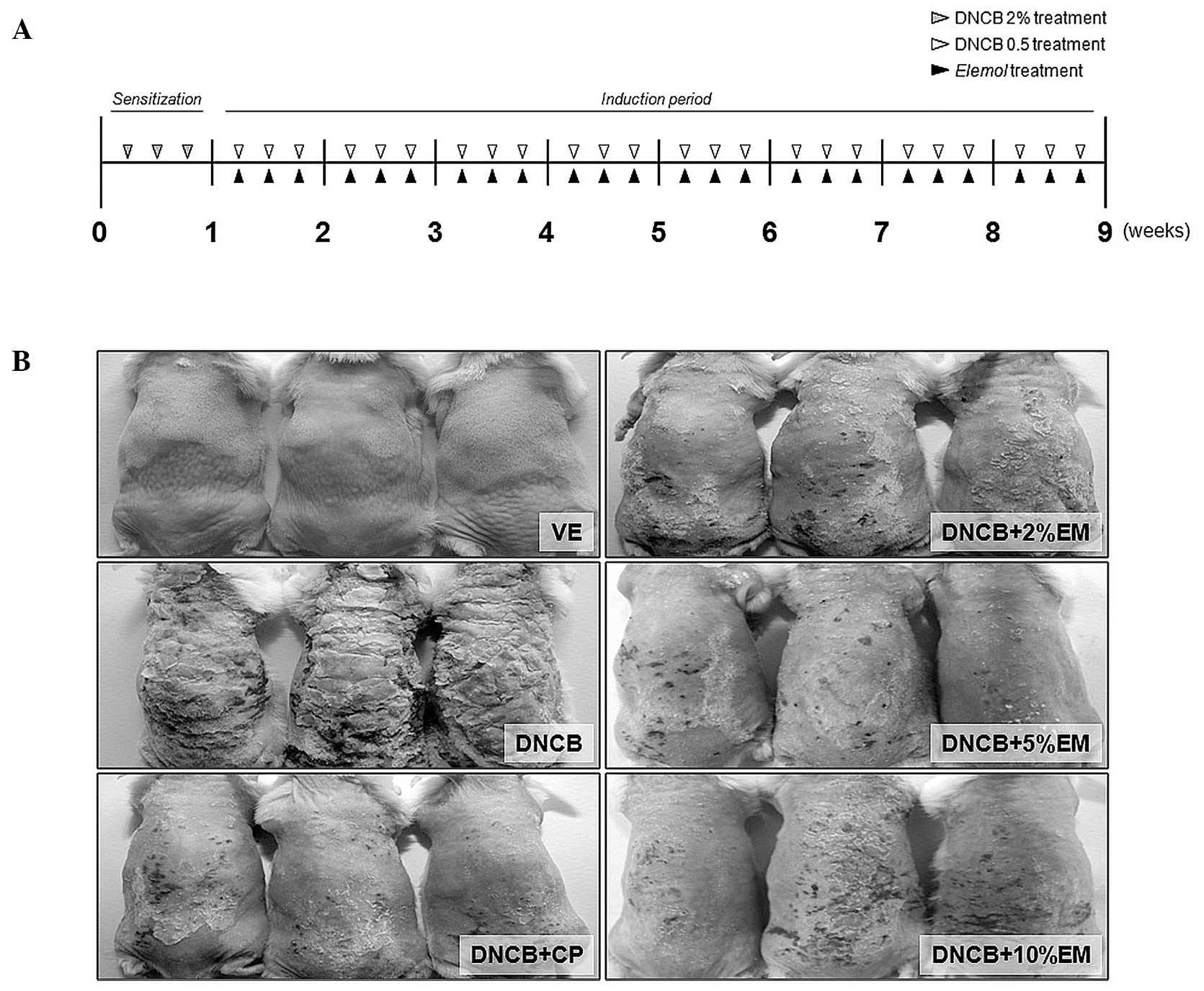
To investigate the anti-allergic effects of elemol
extracted from C. obtusa in a mouse model of AD, skin
lesions were induced in BALB/c mice using multiple topical
applications of DNCB for eight weeks (Fig. 1). However, the topical application
of elemol (2, 5 and 10%) to mice for 1 h after DNCB application
markedly inhibited AD-like skin lesions. Serum IgE levels were
increased (up to 3.5-fold) by DNCB treatment compared to those in
the vehicle-treated group (VE). The elevated serum IgE levels were
decreased in the therapeutic control (CP) treatment, as expected
(Fig. 2). The elevated IgE levels
were also significantly decreased by treatment with elemol (2, 5
and 10%), with the greatest anti-allergenic effect on serum IgE
levels observed with 10% elemol. These results indicated that
elemol attenuated increases of IgE levels in serum, suggesting that
this beneficial compound ameliorated the hyper-allergic reaction in
the mouse model of AD.
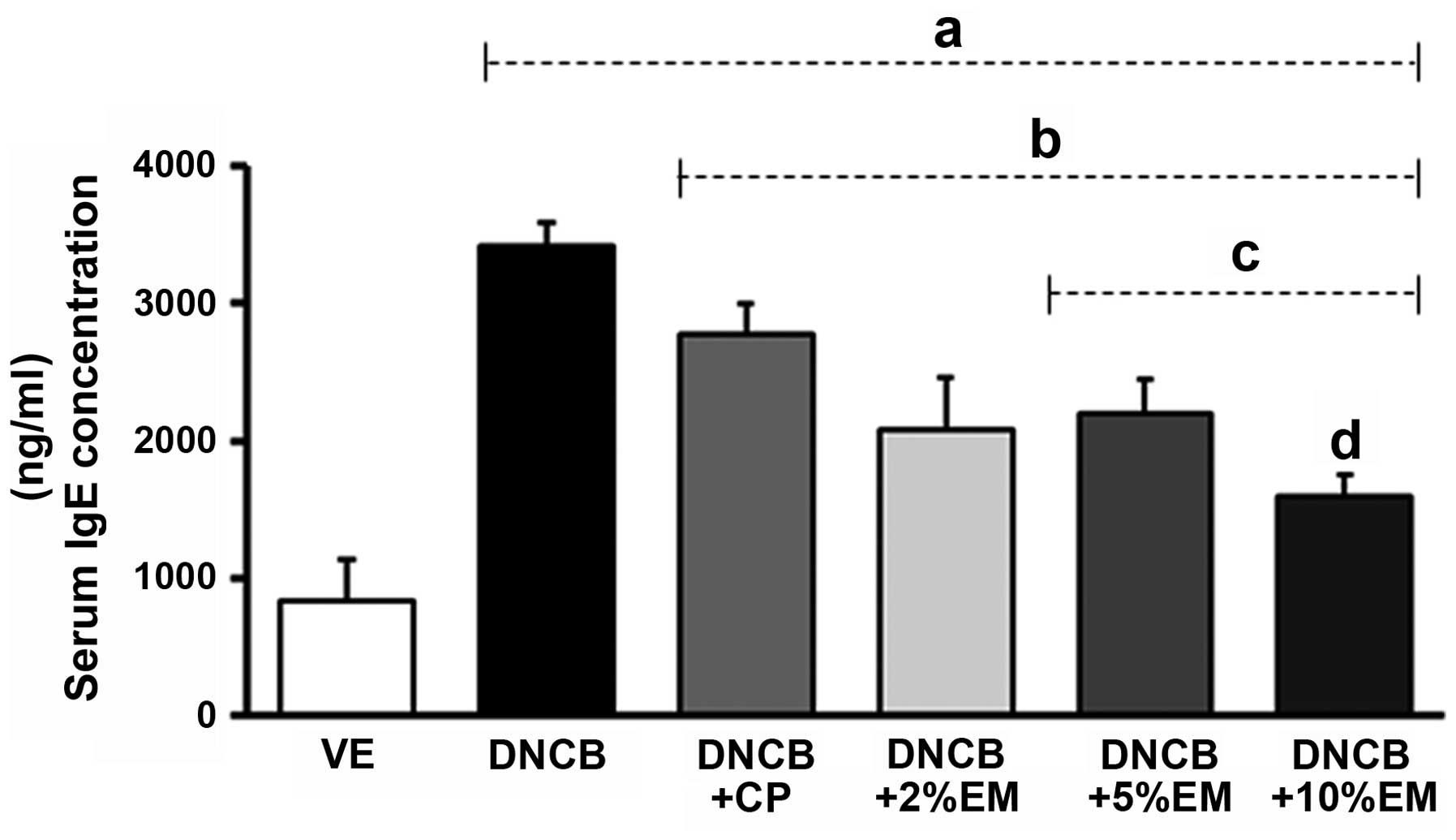 | Figure 2Effects of elemol on serum IgE levels
in DNCB-induced mice. The serum IgE levels in BALB/c mice were
measured at the end of the experiment (after nine weeks) using an
ELISA kit. Groups: VE, vehicle; DNCB, negative control; DNCB + CP,
positive control; DNCB + EM (2, 5 and 7%), experimental groups.
Values are expressed as the mean ± standard deviation.
aP<0.05 vs. VE; bP<0.05 vs.
DNCB-treated group; cP<0.05 vs. DNCB + EM 2%-treated
group; dP<0.05 vs. DNCB + EM 5%-treated group. IgE,
immunoglobulin E; DNCB, 2,4-dinitrochlorobenzene; CP, clobetasol
propionate; EM, elemol. |
C. obtusa oil decreases skin thickness
and mast cell infiltration in mice with AD
For observation of skin thickness and immune cell
infiltration, skin lesions caused by DNCB treatment were collected
and stained with H&E. DNCB induced an increase in skin
thickness compared to that in the vehicle-treated mice, while skin
thickness was decreased in elemol (2, 5 and 10%) or CP-treated mice
(Fig. 3A). Therefore, AD-like
skin treated with elemol at a high concentration (10%) has a
similar potential for recovery compared to that treated with the
positive control, CP. To determine the distribution of mast cells
beneath the dermis and hypodermis of AD-like mice, selected tissues
were stained with toluidine blue after formalin fixation (Fig. 3B). The number of mast cells was
counted under a light microscope and expressed as the number of
cells per square millimeter of dorsal skin (Fig. 3C). The infiltration of mast cells
increased when mice were treated with DNCB only, while the
infiltration was significantly decreased following treatment with 5
and 10% elemol or with CP (Fig.
3C). These findings suggested that elemol may inhibit the
progression of AD-like skin conditions, as demonstrated using the
DNCB-induced mouse model of AD.
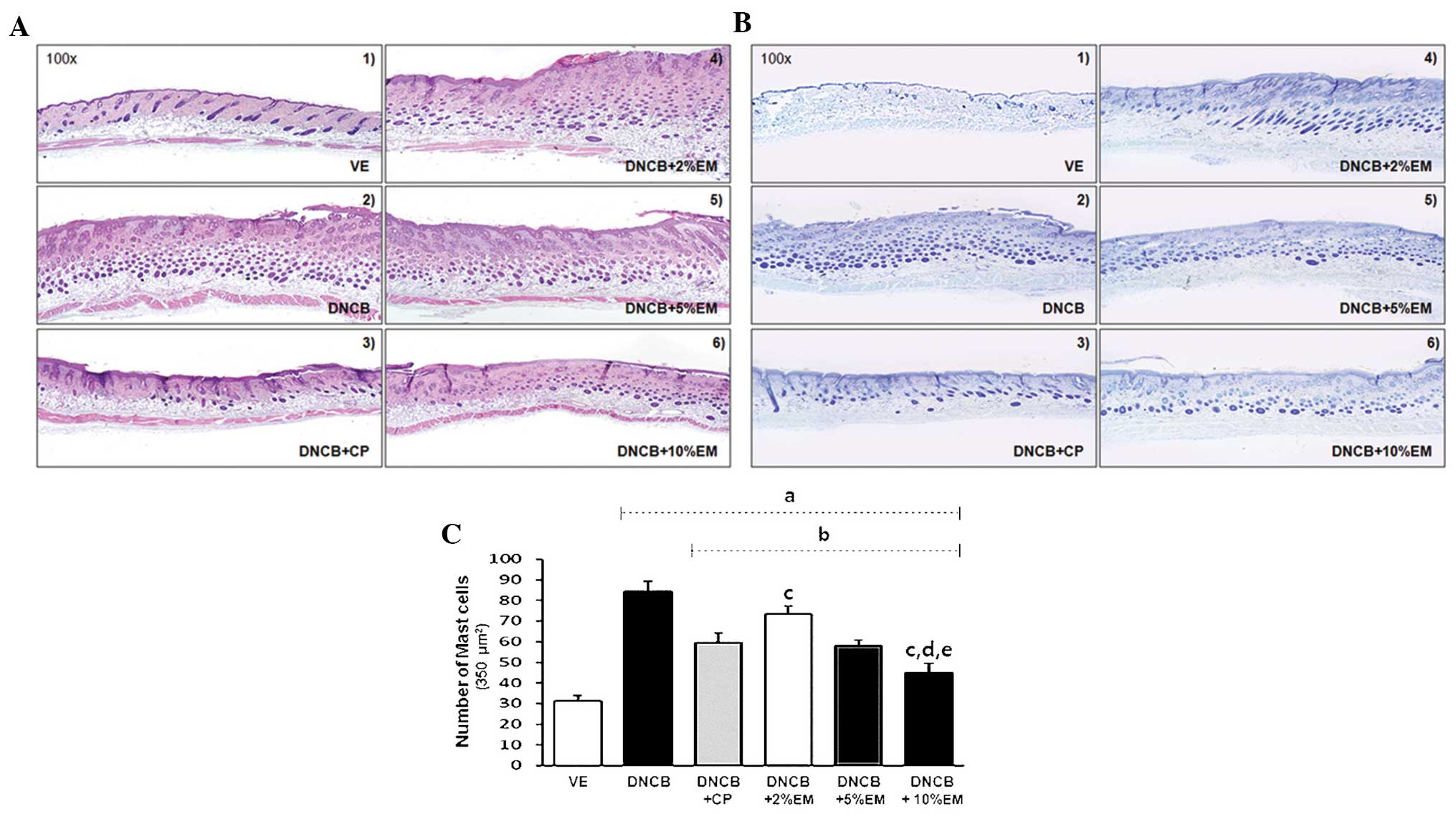 | Figure 3Effects of elemol on histological
dorsal skin lesions of DNCB-treated mice. Histological recovery of
the dorsal skin lesion and mast cell infiltration beneath the
dermis and hypodermis in DNCB- and/or elemol-treated mice. (A)
Hematoxylin and eosin stain; (B) toluidine blue stain
(magnification, ×100). (C) The number of infiltrated mast cells was
calculated under a light microscope (magnification, ×400) and
expressed as the number of cells per square millimeter of dorsal
skin. Groups: VE, vehicle; DNCB, negative control; DNCB + CP,
positive control; DNCB + EM (2, 5 and 7%), experimental groups.
Values are expressed as the mean ± standard deviation.
aP<0.05 vs. VE; bP<0.05 vs.
DNCB-treated group; cP<0.05 vs. DNCB + EM 2%-treated
group; dP<0.05 vs. DNCB + EM 5%-treated group. DNCB,
2,4-dinitrochlorobenzene; CP, clobetasol propionate; EM,
elemol. |
C. obtusa oil reduces the upregulation of
pro-inflammatory cytokines in mice with AD
To determine the effect of elemol on the
pro-inflammatory cytokines TNF-α, IκBα, IL-1β and IL-6, the present
study evaluated the transcriptional expression of these cytokines
in the skin of mice with DNCB-induced AD. As expected, all
cytokines of the skin were induced by DNCB treatment (Fig. 4). The elevated expression of
dermal TNF-α, IκBα, IL-1β and IL-6 mRNA was attenuated in the
positive control group (DNCB + CP). The expression of IL-6 and IκBα
was decreased following treatment with elemol at all concentrations
as compared with that in the DNCB-induced group; furthermore, the
expression of TNF-α and IL-1β mRNA was decreased following
treatment with elemol (2, 5 and 10%) in a dose-dependent manner
compared with that in the DNCB-induced group. These results
suggested that elemol may inhibit the expression of
pro-inflammatory genes in the skin, which may be the underlying
mechanism of the anti-allergenic action of elemol in the mouse
model of AD.
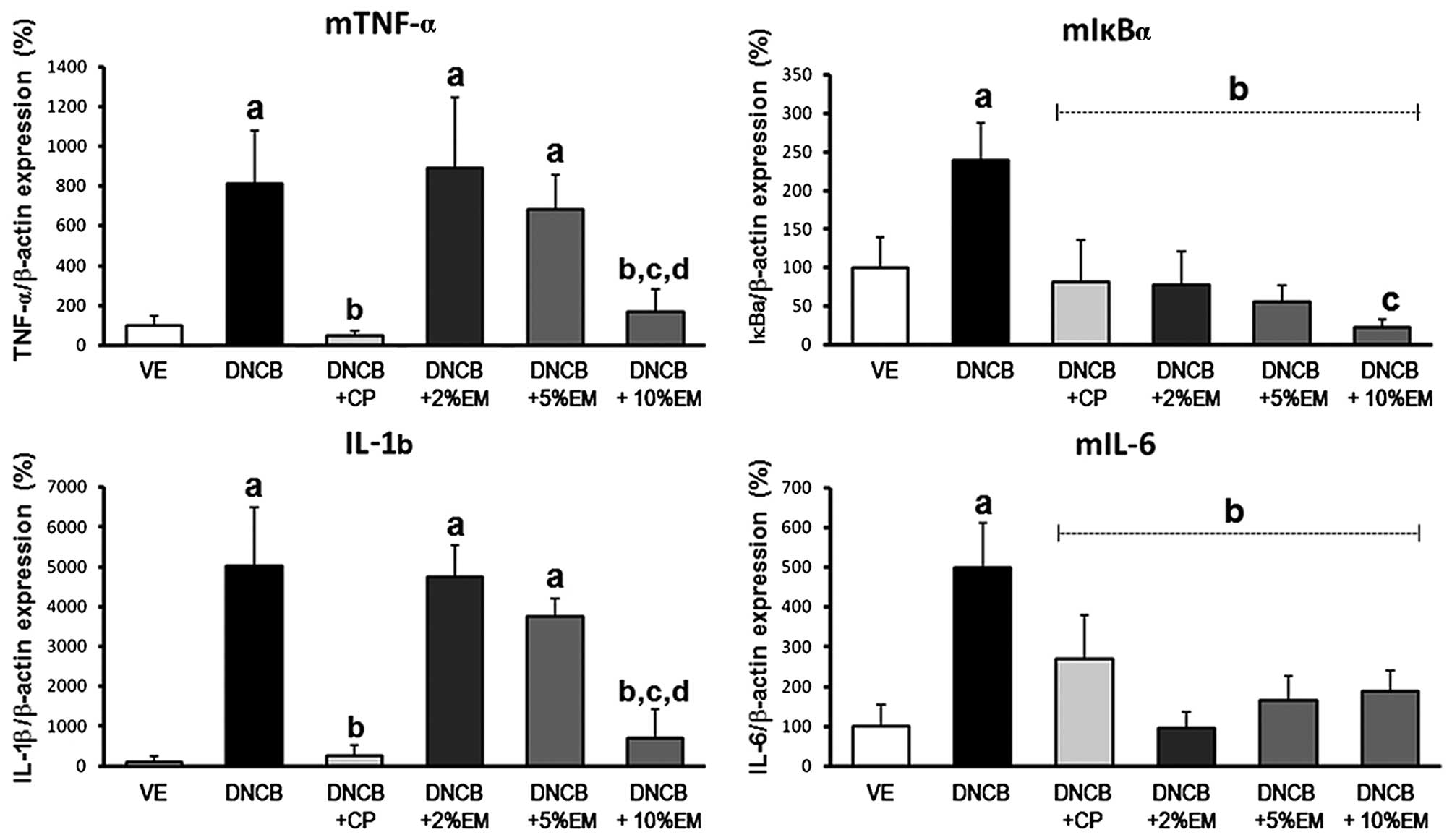 | Figure 4Pro-inflammatory cytokine mRNA
expression in dorsal skin lesions of DNCB-treated mice. Isolated
mRNA was analyzed by real-time reverse transcription polymerase
chain reaction for IL-1β, IL-6, IκBα and TNF-α. Results were
internally confirmed by the comparative cycle threshold method
against β-actin as the standard gene. Groups: VE, vehicle; DNCB,
negative control; DNCB + CP, positive control; DNCB + EM (2, 5 and
7%), experimental groups. Values are expressed as the mean ±
standard deviation. aP<0.05 vs. VE;
bP<0.05 vs. DNCB-treated group; cP<0.05
vs. DNCB + EM 2%-treated group; dP<0.05 vs. DNCB + EM
5%-treated group. DNCB, 2,4-dinitrochlorobenzene; CP, clobetasol
propionate; EM, elemol. |
Effect of the extracts of C. obtusa on atopic
dermatitis models. To investigate the anti-allergenic effect of the
extracts of C. obtusa on the mast cell line RBL-2H3, the
cells were treated with the first fractions (F1, F2, F3, F4, F5, F6
and F7) of C. obtusa oil in the presence of DBP-HSA and
assessed the secretion of β-hexosaminidase, as well as the mRNA
expression of IL-4 and IL-13. Although the release of
β-hexosaminidase showed a significant decrease following treatment
with either of the fractions (F1 to 7), only treatment with F5
resulted in a dose-dependent decrease in the secretion of
β-hexosaminidase (Fig. 5). mRNA
expression of IL-4 and IL-13 was decreased by all fractions
(Figs. 6 and 7). Thus, all fractions extracted from
C. obtusa had an anti-allergenic effect on the RBL-2H3 cell
line and F5 was suggested to be the most effective fraction to
attenuate the secretion of β-hexosaminidase as well as
transcriptional regulation of IL-4 and IL-13.
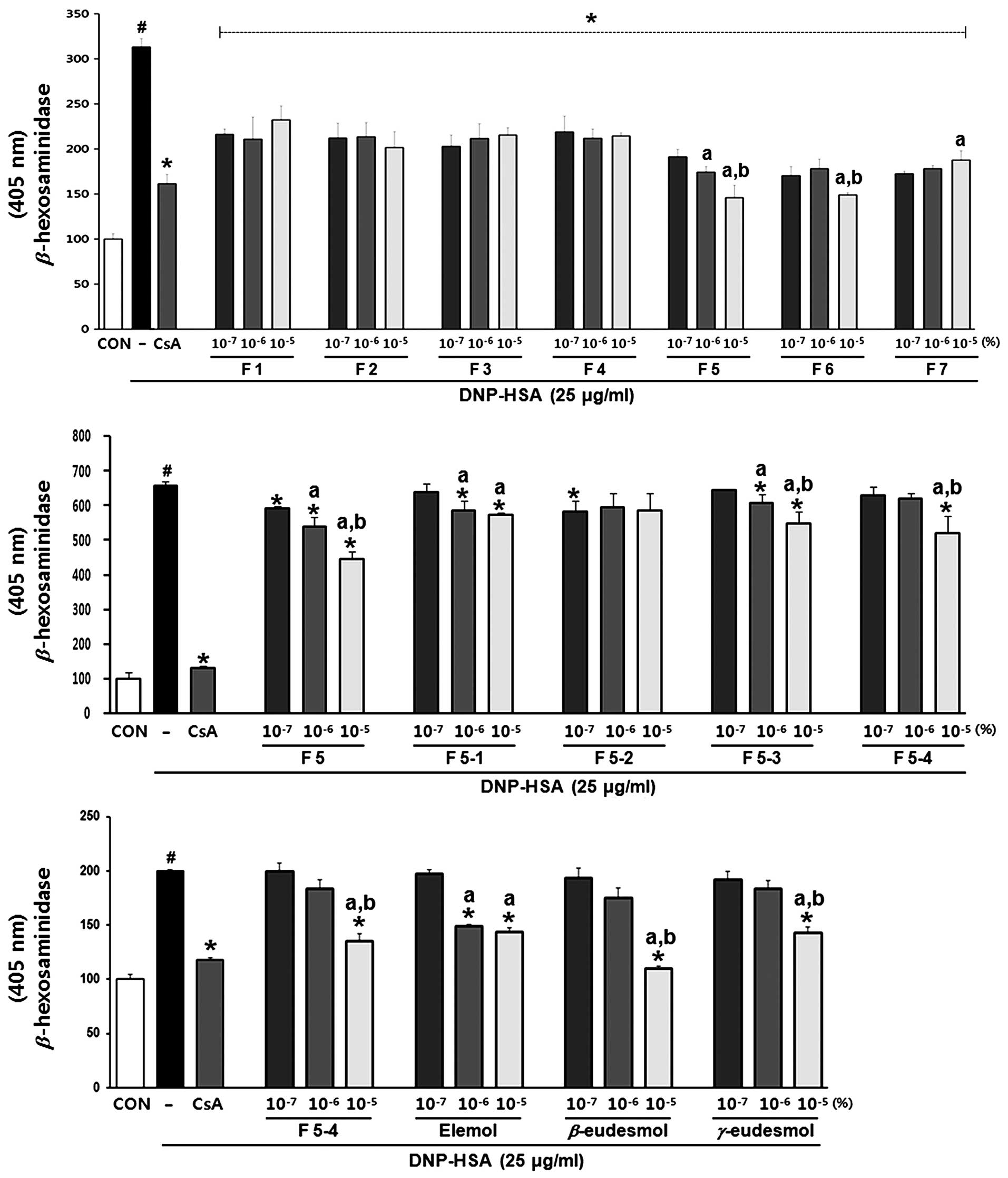 | Figure 5Inhibitory effects of components of
Chamaecyparis obtusa on the release of β-hexosaminidase.
RBL-2H3 cells (2×105 cells/well) were sensitized with 1
µg/ml DNP-specific immunoglobulin E overnight and treated
with varying doses of extract (10−7, 10−6 and
10−5%) for 1 h. Cells were stimulated with 10
µg/ml of DNP-HSA for 1 h. Upper panel, fractions of
Chamaecyparis obtusa (F1, F2, F3, F4, F5, F6 and F7); middle
panel, sub-fractions of F5 (F5-1, F5-2, F5-3 and F5-4); lower
panel, principal components of F5-4 (elemol, β-eudesmol and
γ-eudesmol). Values are expressed as the mean ± standard deviation
(n=3). #P<0.05 vs. untreated group (CON);
*P<0.05 vs. negative control group (−);
aP<0.05 vs. 10−7% treatment group;
bP<0.05 vs. 10−6% treatment group.
DNP-HSA, dinitrophenyl human serum albumin; CON (untreated group),
control; CsA, Cyclosporin A; DNP-HSA (−) treatment only (negative
control). |
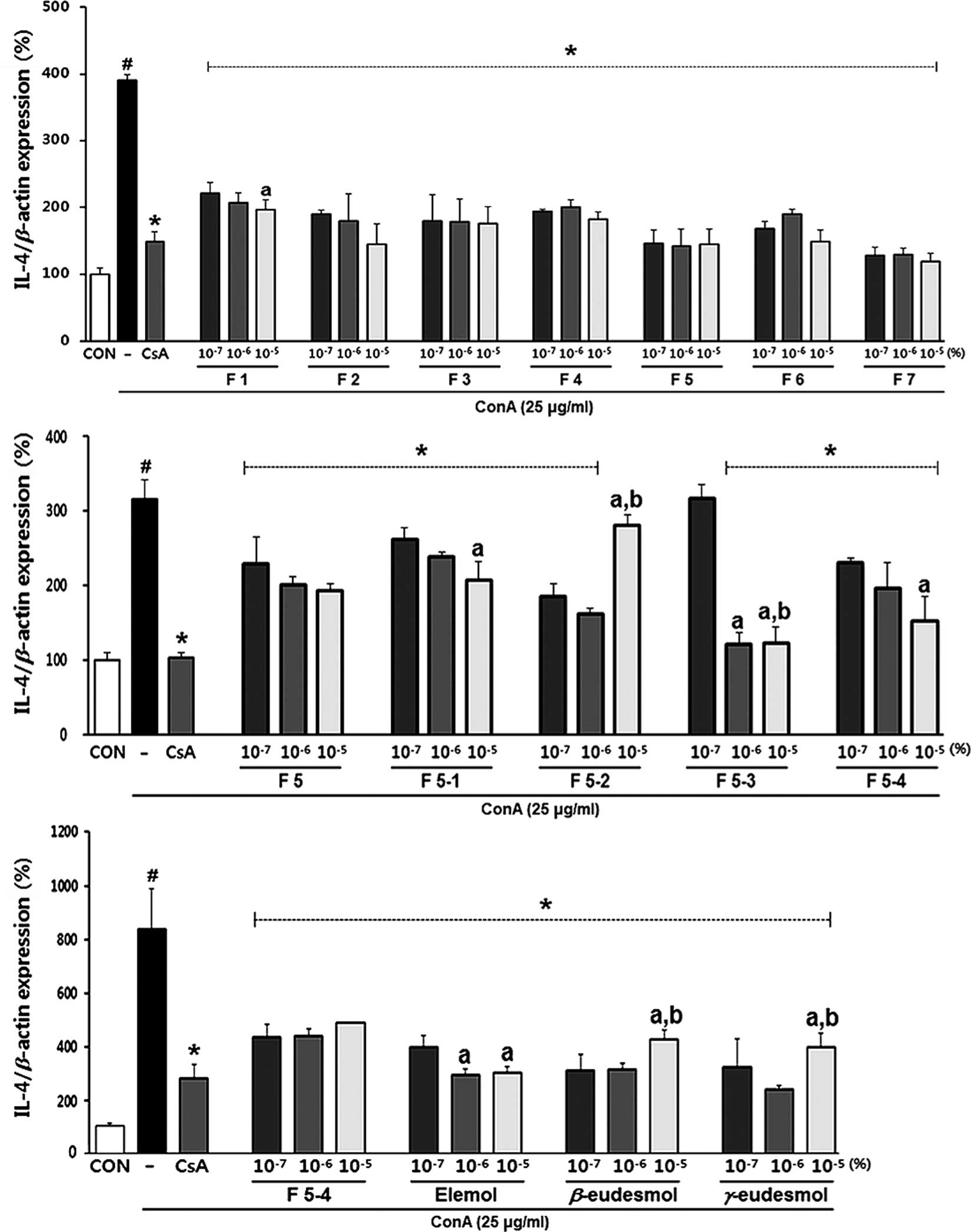 | Figure 6Inhibitory effects of components of
Chamaecyparis obtusa on the mRNA expression levels of IL-4
in sensitized RBL-2H3 cells. Upper panel, fractions of
Chamaecyparis obtusa (F1, F2, F3, F4, F5, F6 and F7); middle
panel, sub-fractions of F5 (F5-1, F5-2, F5-3 and F5-4); lower
panel, principal components of F5-4 (elemol, β-eudesmol and
γ-eudesmol). Values are expressed as the mean ± standard deviation
(n=3). #P<0.05 vs. untreated group (CON);
*P<0.05 vs. negative control group (−);
aP<0.05 vs. 10−7% treatment group;
bP<0.05 vs. 10−6% treatment group. CON
(untreated group), control; CsA, Cyclosporin A; DNP-HSA (−)
treatment only (negative control). |
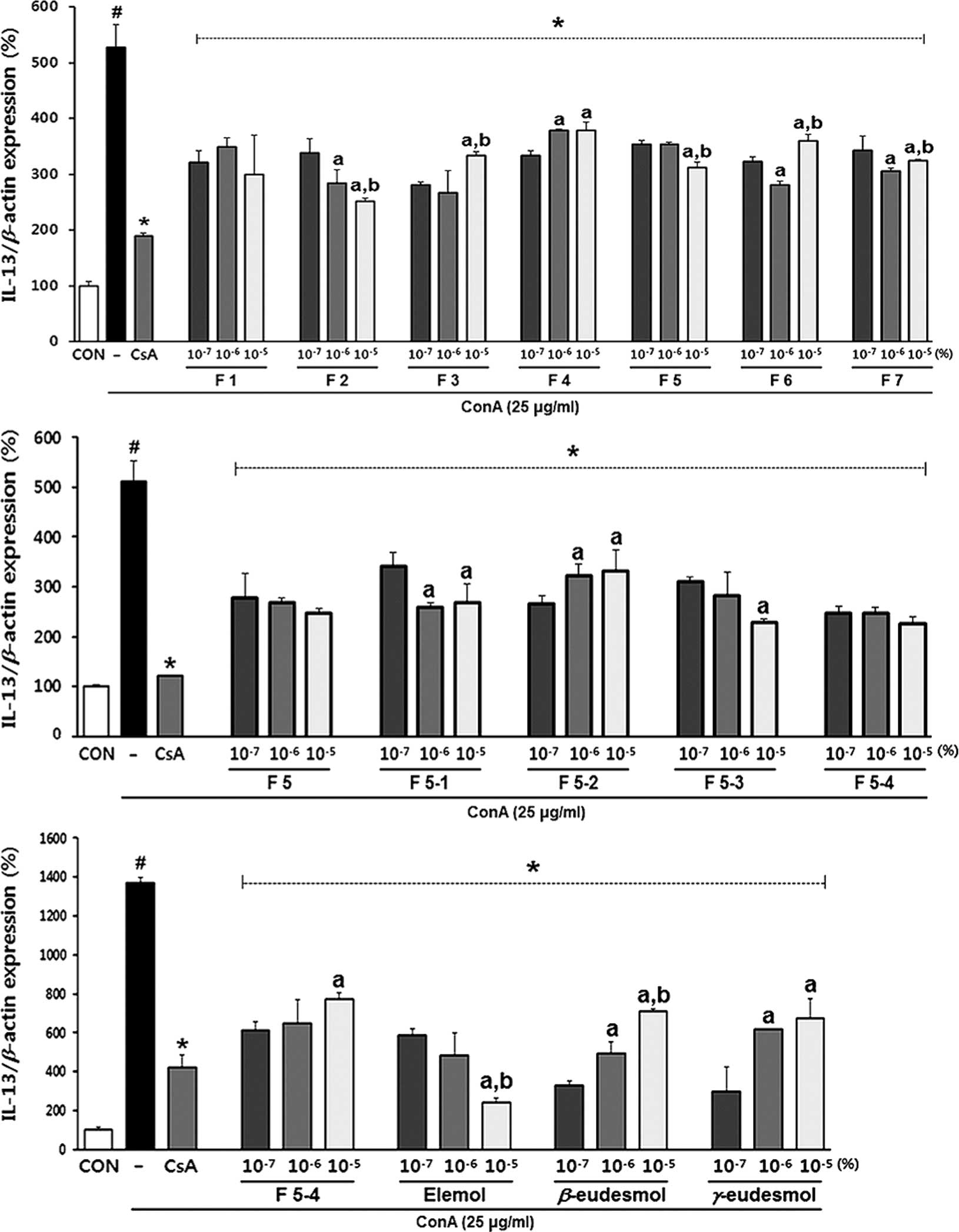 | Figure 7Inhibitory effects of components of
Chamaecyparis obtusa on the mRNA expression levels of IL-13
in sensitized RBL-2H3 cells. Upper panel, fractions of
Chamaecyparis obtusa (F1, F2, F3, F4, F5, F6 and F7); middle
panel, sub-fractions of F5 (F5-1, F5-2, F5-3 and F5-4); lower
panel, principal components of F5-4 (elemol, β-eudesmol and
γ-eudesmol). Values are expressed as the mean ± standard deviation
(n=3). #P<0.05 vs. untreated group (CON);
*P<0.05 vs. negative control group (−);
aP<0.05 vs. 10−7% treatment group;
bP<0.05 vs. 10−6% treatment group. CON
(untreated group), control; CsA, Cyclosporin A; DNP-HSA (−)
treatment only (negative control). |
Furthermore, the present study tested the effects of
sub-fractions of F5 (F5-1, F5-2, F5-3 and F5-4) on the
degranulation and expression of pro-inflammatory cytokines (IL-4
and IL-13) in RBL-2H3 cells. DNP-HSA-mediated β-hexosaminidase
secretion was significantly reduced by all sub-fractions, but not
at all doses (Fig. 5). In the
F5-1 and F5-3 treatment groups, the release of β-hexosaminidase
showed a dose-dependent reduction when compared with that in the
negative control group; however, the lowest dosage
(10−7%) did not affect the release. In the F5-4
treatment group, decreased β-hexosaminidase release was observed
with 10−5% F5-4, while lower doses did not show any
effect (Fig. 5). Furthermore, the
mRNA levels of IL-4 and IL-13 were inhibited by treatment with
sub-fractions of F5 (Figs. 6 and
7). Following treatment with F5-1
and F5-4, the mRNA expression of IL-4 declined in a dose-dependent
manner compared with that in the other groups (Fig. 6). In the F5-2 and F5-3 treatment
groups, IL-4 mRNA expression was also decreased; however, the
effects were not dose-dependent. In parallel with IL-4 mRNA
expression, the levels of IL-13 mRNA were decreased by all F5
sub-fractions (Fig. 7). IL-13
mRNA expression showed a dose-dependent reduction in the F5-3 and
F5-4 treatment groups, while it was reduced in the other groups in
a manner that was not dose-dependent. Based on these results, it is
suggested that all of the F5 sub-fractions exerted anti-allergenic
effects by attenuating increases in β-hexosaminidase activity as
well as IL-4 and IL-13 mRNA expression; in particular, the F5-4
fraction showed stability and efficacy in ameliorating allergic
reactions in RBL-2H3 cells.
In addition to the fractions, the principal
components of the 5–4 fraction, elemol, β-eudesmol and γ-eudesmol,
were also evaluated in RBL-2H3 cells, in which an allergic reaction
was induced (Fig. 5, lower
panel). The β-hexosaminidase levels were downregulated in the
elemol, β-eudesmol and γ-eudesmol treatment groups. Eudesmol β and
γ exhibited anti-β-hexosaminidase activity at high concentration
only (10−5%); however, elemol had a significant effect
at 10−6 and 10−5% (Fig. 5). These results suggested that
C. obtusa oil fractions may alleviate allergic reactions via
reduction of β-hexosaminidase levels as well as IL-4 and IL-13 mRNA
expression in RBL-2H3 cells, and that eudesmol and particularly
elemol are active components exerting these effects.
Discussion
AD, also known as eczema, is a type of skin
inflammatory disease. A variety of defects in the innate immune
system can affect the development and severity of AD. Medications
for AD include oral or topical agents, including emollients,
corticosteroids, calcineurin inhibitors and immunosuppressants
(12). Numerous natural products
are currently being investigated to determine whether they can be
used in the treatment of AD (2).
Corticosteriods may be used for severe flares and when the rash
covers a large part of the body (12,25). Several corticosteriod ointments
are also available for the control of AD-associated symptoms and
are often considered to have greater safety and poorer efficacy
than oral corticosteroids in the treatment of atopic dermatitis
(12,25,26). However, long-term use of oral and
topical corticosteriods is associated with a large number of side
effects and drug intolerance in the endocrine system of the body
(16,25,27,28). To avoid these side effects,
certain medications are prescribed for a short course in an effort
to calm the rash.
Compounds from plants have recently been reported as
alternative therapeutics for anti-AD treatment, and this type of
treatment is expected to prevent the onset of allergic diseases and
ameliorate allergic symptoms (29,30). In the present study, the
basophilic leukemic cell line RBL-2H3 was sensitized with Con A and
mice were induced with DNCB to generate an in vitro and
in vivo model of AD, respectively. These models were
employed to study the anti-allergenic effects of C. obtusa
fractions (F1 to 7), sub-fractions (F5-1 to 5-4) and elemol.
The present study examined β-hexosaminidase release
as well as IL-4 and IL-13 mRNA expression from RBL-2H3 cells after
treatment with 10−7, 10−6 and
10−5% of C. obtusa fractions (F1 to 7),
sub-fractions (F5-1 to 5-4) and elemol. The release of
β-hexosaminidase showed a significant decrease following treatment
with all concentrations of C. obtusa fractions (F1 to 7). In
addition, a decrease in IL-4 and IL-13 mRNA expression following
treatment with all concentrations of fractions F1-7 was observed.
The principal components of C. obtusa, elemol, β-eudesmol
and γ-eudesmol, were identified from the sub-fraction F5-4, which
was particularly potent, using analytical tools. Treatment of
stimulated cells with elemol, β-eudesmol and γ-eudesmol caused
reductions in β-hexosaminidase release as well as IL-4 and IL-13
mRNA expression to a similar extent to that following treatment
with F5-4. However, among the three principal components, the
reduction of IL-4 and IL-13 mRNA expression was dose-dependent in
the elemol-treatment group only. IL-4 and IL-13 are able to
stimulate epithelial cells to produce chemokines, which triggers
several key processes of allergic diseases (15,22,31). The release of β-hexosaminidase
also causes the production of pro-inflammatory and allergenic
cytokines, which can potentiate immune responses through the
subsequent induction of other AD-associated regulatory processes
(11,22,32). The results of the present study
suggested that C. obtusa fractions may ameliorate allergic
reactions via reducing β-hexosaminidase levels and IL-4, IL-13 mRNA
expression, and that elemol is the major active component, at least
with regard to the effect on RBL-2H3 cells.
The existence of T-helper (Th)1/Th2 subsets in Th
lymphocytes provides a framework for understanding the normal and
pathological immune response in allergic responses. In other
studies, Th1- and Th2-associated signaling can mutually regulate
several immune signaling cascades. Therefore, balancing Th1/Th2
signaling may be fundamental for the treatment of AD (33,34). Therapies using herbal medicines
have become increasingly popular in Asia and Europe due to their
successful use over extended time periods. A wide variety of
phenolic substances derived from plants have been reported to exert
marked anti-oxidant and anti-inflammatory activities, which
contribute to their chemopreventive potential (35). In addition, volatile components of
plants have been reported to exhibit various anti-oxidant
activities, which may be responsible for the anti-oxidant effects
of these plants (36). In
previous studies, C. obtusa oil has been shown to possess
anti-microbial and anti-fungal activities (18–20) and has been used to improve the
condition of skin with eczematous lesions in AD caused by mite
antigens. In a previous study, Joo et al (22) reported that C. obtusa oil
attenuated the symptoms of AD in patients with dry scaly skin
lesions by modulating interferon-γ and interleukins.
The present study investigated the effects of elemol
in a DNCB-induced mouse model of AD in vivo. The
DNCB-induced serum IgE levels were significantly decreased by
application of elemol in the mice with AE. In addition, this
treatment resulted in recovery of skin thickness. Topical
application of elemol was shown to result in successful elimination
of AD-associated symptoms, including skin lesions and mast cell
infiltration beneath hypodermis. mRNA expression of cytokines
(IL-1β, IL-6, IκBα and TNF-α) in the skin lesions of DNCB-treated
mice was significantly inhibited by elemol, suggesting that elemol
may contribute to the suppression of the stimulation of T
cell-mediated cytokines.
Over the last 50 years, topical corticosteroids have
been the primary choice for the treatment of AD; however, due to
conditions including skin atrophy, stiriae and perioral dermatitis
in sensitive areas (face or skin fold), corticosteroids are not
suitable for the long-term treatment of AD (37). Recently, new topical calcineurin
inhibitors, including tacrolimus ointment and pimecrolimus cream,
have been used for monotherapy treatment of AD to replace
conventional treatments (such as corticosteroids); however, their
efficacy was not sufficient to successfully treat AD. Therefore, a
large number of patients have turned to alternative medicinal
approaches (38), which include
natural products and herbal medicines. The application of herbal
medicines has a long history due to their use in folk medicine, and
most well-known medications are derived from plants (22,23,29). Although the mechanisms of action
of numerous herbal remedies have not yet been fully elucidated,
their clinical benefit has been proven by a large number of
scientific studies (32,38,39).
In conclusion, the present study demonstrated the
anti-allergenic effects of C. obtusa using an in
vitro as well as an in vivo model of AD. One of the key
components of C. obtusa, elemol, had potent anti-allergenic
activity, particularly in models of AD. Based on the results of the
present study, it appears that elemol may be a potent therapeutic
compound for the treatment of AD, which is effective in controlling
the levels of serum IgE and T cell-derived cytokines, including
IL-1β, IL-6, IκBα and TNF-α, in skin lesions of a mouse model of
AD.
Acknowledgments
This study was supported by a grant from the
National Research Foundation of Korea (NRF) funded by the Korean
Ministry of Education, Science and Technology (MEST; no.
2013R1A2A2A05004582).
References
|
1
|
Adlard BP, Dobbing J and Sands J: A
comparison of the effects of cytosine arabinoside and adenine
arabinoside on some aspects of brain growth and development in the
rat. Br J Pharmacol. 54:33–39. 1975. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Abramovits W: Atopic dermatitis. J Am Acad
Dermatol. 53(Suppl 1): S86–S93. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Shimizu N, Dairiki K, Ogawa S and Kaneko
T: Dietary whey protein hydrolysate suppresses development of
atopic dermatitis-like skin lesions induced by mite antigen in
NC/Nga mice. Allergol Int. 55:185–189. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Kang JS, Lee K, Han SB, Ahn JM, Lee H, Han
MH, Yoon YD, Yoon WK, Park SK and Kim HM: Induction of atopic
eczema/dermatitis syndrome-like skin lesions by repeated topical
application of a crude extract of Dermatophagoides pteronyssinus in
NC/Nga mice. Int Immunopharmacol. 6:1616–1622. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Grabbe S and Schwarz T: Immunoregulatory
mechanisms involved in elicitation of allergic contact
hypersensitivity. Immunol Today. 19:37–44. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Bardana EJ Jr: Immunoglobulin E- (IgE) and
non-IgE-mediated reactions in the pathogenesis of atopic
eczema/dermatitis syndrome (AEDS). Allergy. 59(Suppl 78): 25–29.
2004. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Yu M, Qi X, Moreno JL, Farber DL and
Keegan AD: NF-κB signaling participates in both RANKL- and
IL-4-induced macrophage fusion: Receptor cross-talk leads to
alterations in NF-κB pathways. J Immunol. 187:1797–1806. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Lee SO, Lou W, Nadiminty N, Lin X and Gao
AC: Requirement for NF-(kappa)B in interleukin-4-induced androgen
receptor activation in prostate cancer cells. Prostate. 64:160–167.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Bhushan S, Hossain H, Lu Y, Geisler A,
Tchatalbachev S, Mikulski Z, Schuler G, Klug J, Pilatz A,
Wagenlehner F, et al: Uropathogenic E. coli induce different immune
response in testicular and peritoneal macrophages: Implications for
testicular immune privilege. PLoS One. 6:e284522011. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Georas SN, Guo J, De Fanis U and Casolaro
V: T-helper cell type-2 regulation in allergic disease. Eur Respir
J. 26:1119–1137. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Sohn EH, Jang SA, Joo H, Park S, Kang SC,
Lee CH and Kim SY: Anti-allergic and anti-inflammatory effects of
butanol extract from Arctium Lappa L. Clin Mol Allergy. 9:42011.
View Article : Google Scholar
|
|
12
|
Boguniewicz M and Leung DY: Atopic
dermatitis: A disease of altered skin barrier and immune
dysregulation. Immunol Rev. 242:233–246. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Garrigue JL, Nicolas JF, Fraginals R,
Benezra C, Bour H and Schmitt D: Optimization of the mouse ear
swelling test for in vivo and in vitro studies of weak contact
sensitizers. Contact Dermat. 30:231–237. 1994. View Article : Google Scholar
|
|
14
|
Watanabe H, Unger M, Tuvel B, Wang B and
Sauder DN: Contact hypersensitivity: The mechanism of immune
responses and T cell balance. J Interferon Cytokine Res.
22:407–412. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Gong JH, Shin D, Han SY, Park SH, Kang MK,
Kim JL and Kang YH: Blockade of airway inflammation by kaempferol
via disturbing Tyk-STAT signaling in airway epithelial cells and in
asthmatic mice. Evid Based Complement Alternat Med.
2013:2507252013. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Dharmage SC, Lowe AJ, Matheson MC, Burgess
JA, Allen KJ and Abramson MJ: Atopic dermatitis and the atopic
march revisited. Allergy. 69:17–27. 2014. View Article : Google Scholar
|
|
17
|
Hong CU, Ki CS, Kim NG and Kim YH:
Composition of essential oils from the leaves and the fruits of
Chamaecyparis obtusa and Chamaecyparis pisifera. J Korean Soc Agric
Chem Biotechnol. 44:116–121. 2001.In Korean.
|
|
18
|
Hong EJ, Na KJ, Choi IG, Choi KC and Jeung
EB: Antibacterial and antifungal effects of essential oils from
coniferous trees. Biol Pharm Bull. 27:863–866. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Lee HO, Baek SH and Han DM: Antimicrobial
effects of Chamaecyparis obtusa essential oil. Kor J Appl Microbiol
Biotechnol. 29:253–257. 2001.In Korean.
|
|
20
|
Trust TJ and Coombs RW: Antibacterial
activity of beta-thujaplicin. Can J Microbiol. 19:1341–1346. 1973.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Arima Y, Nakai Y, Hayakawa R and Nishino
T: Antibacterial effect of beta-thujaplicin on staphylococci
isolated from atopic dermatitis: Relationship between changes in
the number of viable bacterial cells and clinical improvement in an
eczematous lesion of atopic dermatitis. J Antimicrob Chemother.
51:113–122. 2003. View Article : Google Scholar
|
|
22
|
Joo SS, Yoo YM, Ko SH, Choi W, Park MJ,
Kang HY, Choi KC, Choi IG and Jeung EB: Effects of essential oil
from Chamaecyparis obtusa on the development of atopic
dermatitis-like skin lesions and the suppression of Th cytokines. J
Dermatol Sci. 60:122–125. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Park D, Jeon JH, Kwon SC, Shin S, Jang JY,
Jeong HS, Lee I, Kim YB and Joo SS: Antioxidative activities of
white rose flower extract and pharmaceutical advantages of its
hexane fraction via free radical scavenging effects. Biochem Cell
Biol. 87:943–952. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Holtzapple MT and Humphrey AE: The effect
of organosolv pretreatment on the enzymatic hydrolysis of poplar.
Biotechnol Bioeng. 26:670–676. 1984. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Gebben HJ: Topical immunomodulators, such
as tacrolimus and pimecrolimus, in the treatment of atopic
dermatitis. Ned Tijdschr Geneeskd. 149:1816–1817. 2005.In
Dutch.
|
|
26
|
McClain RW, Yentzer BA and Feldman SR:
Comparison of skin concentrations following topical versus oral
corticosteroid treatment: Reconsidering the treatment of common
inflammatory dermatoses. J Drugs Dermatol. 8:1076–1079.
2009.PubMed/NCBI
|
|
27
|
Furue M, Terao H, Rikihisa W, Urabe K,
Kinukawa N, Nose Y and Koga T: Clinical dose and adverse effects of
topical steroids in daily management of atopic dermatitis. Br J
Dermatol. 148:128–133. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Hengge UR, Ruzicka T, Schwartz RA and Cork
MJ: Adverse effects of topical glucocorticosteroids. J Am Acad
Dermatol. 54:1–15; quiz 16–18. 2006. View Article : Google Scholar
|
|
29
|
Kawai M, Hirano T, Higa S, Arimitsu J,
Maruta M, Kuwahara Y, Ohkawara T, Hagihara K, Yamadori T, Shima Y,
et al: Flavonoids and related compounds as anti-allergic
substances. Allergol Int. 56:113–123. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Tan HY, Zhang AL, Chen D, Xue CC and Lenon
GB: Chinese herbal medicine for atopic dermatitis: A systematic
review. J Am Acad Dermatol. 69:295–304. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Munitz A, Brandt EB, Mingler M, Finkelman
FD and Rothenberg ME: Distinct roles for IL-13 and IL-4 via IL-13
receptor alpha1 and the type II IL-4 receptor in asthma
pathogenesis. Proc Natl Acad Sci USA. 105:7240–7245. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Wang W, Zhou Q, Liu L and Zou K:
Anti-allergic activity of emodin on IgE-mediated activation in
RBL-2H3 cells. Pharmacol Rep. 64:1216–1222. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Heinzel FP, Sadick MD, Holaday BJ, Coffman
RL and Locksley RM: Reciprocal expression of interferon gamma or
interleukin 4 during the resolution or progression of murine
leishmaniasis. Evidence for expansion of distinct helper T cell
subsets. J Exp Med. 169:59–72. 1989. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Grewe M, Bruijnzeel-Koomen CA, Schöpf E,
Thepen T, Langeveld-Wildschut AG, Ruzicka T and Krutmann J: A role
for Th1 and Th2 cells in the immunopathogenesis of atopic
dermatitis. Immunol Today. 19:359–361. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Surh YJ, Na HK, Lee JY and Keum YS:
Molecular mechanisms underlying anti-tumor promoting activities of
heat-processed Panax ginseng C.A. Meyer. J Korean Med Sci.
16(Suppl): S38–S41. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Jang HW, Ka MH and Lee KG: Antioxidant
activity and characterization of volatile extracts of Capsicum
annuum L. and Allium spp. Flavour Fragrance J. 23:178–184. 2008.
View Article : Google Scholar
|
|
37
|
Thaçi D: Long term management of childhood
atopic dermatitis with calcineurin inhibitors. Hautarzt.
54:418–423. 2003.In German.
|
|
38
|
Vender RB: Alternative treatments for
atopic dermatitis: A selected review. Skin Therapy Lett. 7:1–5.
2002.PubMed/NCBI
|
|
39
|
Yoon S, Lee J and Lee S: The therapeutic
effect of evening primrose oil in atopic dermatitis patients with
dry scaly skin lesions is associated with the normalization of
serum gamma-interferon levels. Skin Pharmacol Appl Skin Physiol.
15:20–25. 2002. View Article : Google Scholar : PubMed/NCBI
|