Introduction
In France, approximately 40% of the newly diagnosed
cancer in female patients is breast cancer. The mapping and
excision of sentinel lymph nodes is the main minimally invasive
technique for cancer staging. The morbidity associated with this
technique is less compared to the axillary dissection (1). The procedure used in routine clinical
practice is clearly defined. Combined blue dye and isotope
injection in the periareolar area allows for the identification of
the sentinel lymph node (SLN) at a higher success rate (2–4).
Thus, the detection subsequent to skin incision in the armpit
involves a nuclear probe. Blue dye, such as patent blue V (PBV), is
used to provide visual guidance during the surgical procedure
(5,6). Potential allergy to PBV dye has
recently been thoroughly studied and severe anaphylaxis is rare,
approximately 0.9% (7). However,
this detection method involves an element of subjectivity and
requires a learning curve on behalf of the surgeon (8).
Currently, attempts have been made to develop
accurate and minimally invasive diagnostic and interventional
tools. Thus, several optical methods are currently being developed
in parallel with conventional methods, such as magnetic resonance
imaging (MRI) (9), positron
emission tomography (PET) (10) or
ultrasound (11), to detect SLN.
The use of tracers with radiocolloid metastable technetium 99
(99mTc) and fluorescent labeling (ICG) is widely
suggested (12). Moreover, the
photoacoustic approach using nanoparticules has increasingly been
considered in several studies (13). However, at present, applications
using these molecules are only used in experimental research and
require prior approval from the sanitary authorities for marketing
and use in routine clinical practice.
In this study, several approaches for SLN detection
were investigated. After the combined isotope and PBV injection, we
aimed to compare the accuracy and success rate using an isotopic
probe for detection of the radiocolloid tracer, and the eye
visibility threshold of the surgeon, as well as a new optical probe
for dye detection. This prototype is based on four laser diodes and
a photodiode detector to automatically detect the presence of PBV.
Each laser diode has a specific wavelength to measure the relative
concentration of chromophores present in the biological tissue such
as PBV, haemoglobin and water. In a previous study, we had
demonstrated that the use of four wavelengths allows for an
accurate measurement of dye absorption (14). The objective of the present study
was to determine the ex vivo applicability of the probe with
the view to develop a new diagnostic tool for the surgeon. The
ultimate goal was to reduce the possibility of false negatives
during the surgical procedure and propose an alternative to the
isotopic detection.
Materials and methods
General
This prospective study was performed in the
Department of Pathology of the Paul Strauss Cancer Center in
Strasbourg (France), given that the prototype used has not yet been
approved by authorities for use in the operating room.
Patients
In total, 24 patients (females with clinical T0 and
T1, N0M0 invasive breast cancer) were enrolled in this preliminary
study. Diagnosis was achieved by pre-operative core biopsy.
Exclusion criteria were pregnancy, ductal carcinoma
in situ, multicentric tumors, inflammatory tumors,
neoadjuvant chemotherapy and metastatic breast cancer. The mean
patient age was 57 years (range, 41–79). The mean body mass index
was 24.7 (range, 15.9–42.5).
Techniques
The patients underwent the same protocol. Initially,
0.2 ml of 11- to 30-MBq 99mTc-labeled sulfur colloid
(Nanocis, Cis Bio International, Saclay, France) was injected into
the periareolar area, 24 h prior to surgery. Breasts were massaged
at the site of injection for 2–3 min to improve the diffusion of
the radiocolloid. Patients had pre-operative lymphoscintigraphy
using a γ-camera. Static images were acquired for ∼10 min, between
30 min and 2 h post-injection, to locate the site of the identified
drained lymph nodes. After anesthesia, PBV (Guerbet,
Aulnay-Sous-Bois, France), was injected periareolarly 5–10 min
before skin incision. The breast was massaged for 2–3 min to
facilitate the diffusion and uptake of the dye. To obtain
PBV-marked surgical sections with visible and invisible to the eye
dye-uptake, decreasing dye volumes ranging from 2 (1 patient) to 1
(3 patients), to 0.5 (2 patients) and, then, 0.25 ml (16 patients)
were injected. In addition, 2 patients, without dye injection, were
included in the protocol as controls. Axillary skin was incised and
a careful dissection was performed to search for blue-stained lymph
nodes.
An intraoperative isotopic probe (Europrobe,
Eurorad, Strasbourg, France) was used to help and guide the
dissection. SLNs were identified in vivo when they were
blue, had radioactive counts or both characteristics. Radioactive
nodes were removed until the background radioactivity of the axilla
was <10% of the ex vivo count of the hottest node
removed.
When the excised nodes arrived at the Department of
Pathology (Paul Strauss Cancer Center), the optical probe prototype
was used on each surgical section to detect dye accumulation in the
SLNs and assess its performance. This measurement was performed
prior to examination (frozen sections). The pathologists were
consulted as to whether they were able to detect blue-stained lymph
nodes visually, and visual assessments were compared with the
information obtained from the probe.
Subsequent to the SLN biopsy, the patients underwent
a lumpectomy, while patients with involved SLN underwent a
hyperectomy combined with axillary lymph node dissection of level I
and II.
Optical probe prototype description
The present study commenced with the development of
a first prototype, demonstrating the feasibility of optical dye
detection using scattered photons (15,16).
However, that optical probe did not completely discriminate between
dye accumulation and other sources of tissue absorption changes,
possibly encountered by surgeons in vivo.
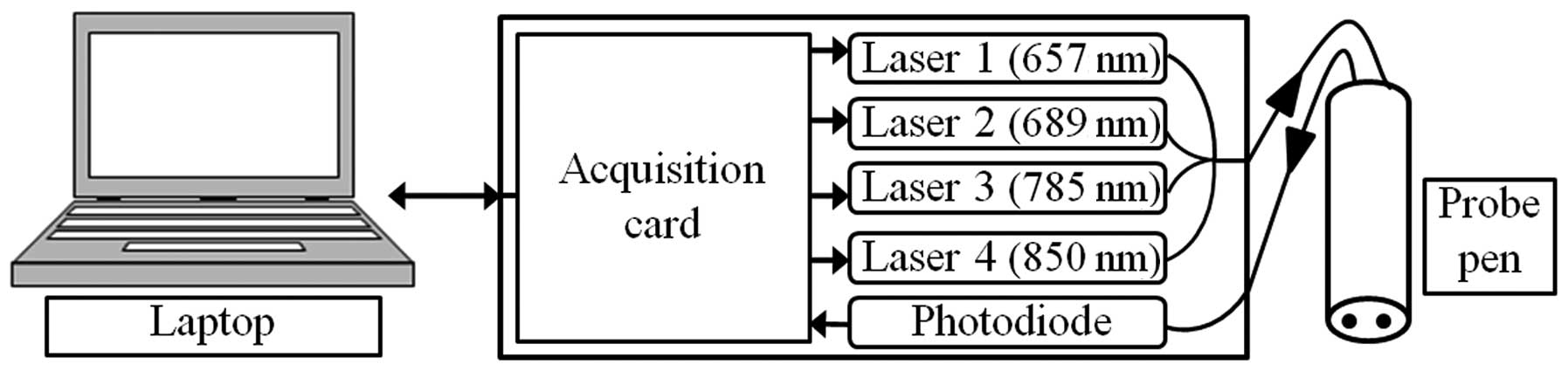
The new probe used in this study was described in
detail by Tellier et al(14). It operates with four laser diode
modules (I.L.E.E. AG, Urdorf, Switzerland), with an average power
of 400 μW, emitting at four different wavelengths (657, 689,
785 and 850 nm). The laser beams are injected in a four-inone
furcated optical fiber with a common output, and are monitored via
a National Instrument (NI USB-6229; National Instrument Crp.,
Austin, TX, USA) multifunction data acquisition (DAQ) module
connected to a laptop via a USB port. Back-scattered photons are
collected with a second fiber, detected by a photodiode (S5106;
Hamamatsu, Hamamatsu City, Japan) and digitalized by the same NI
DAQ module. The sample examined was illuminated with a sterilized
stainless steel probe, including the 2 optical fibers, and placed 4
mm apart (Fig. 1).
The wavelength of 657 nm lies in the absorption band
of PBV. Fig. 2 shows the
absorption spectra of the PBV measured, the oxy-haemoglobin and the
deoxy-haemoglobin, based on the website of the Oregon Medical Laser
Center (17). The extinction
coefficient of deoxy-haemoglobin was clearly higher compared to the
oxy-haemoglobin, at 657 nm. Consequently, a decrease in blood
oxygenation was likely to result in an increased absorption at this
wavelength and be erroneously interpreted as increased optical
absorption by the dye. To avoid such a misinterpretation, three
other laser diodes were incorporated into the probe at 689, 785 and
850 nm in order to measure PBV concentrations, taking blood oxygen
saturation into account.
The laser diodes were modulated at different
frequencies to separate the four components of the measured signal,
by means of a spectral analysis. The absorption coefficients of the
two forms of haemoglobin, as well as of the PBV dye were then
computed to detect a relative PBV concentration in the tissues
(14). This relative concentration
was continuously displayed on the laptop screen, and was equal to
the true concentration multiplied by a coefficient termed as the
differential pathlength factor that varies as a function of the
optical properties of the medium (18), its value ranging from ∼5 to 10 for
the tissues.
Results
Clinical data
The mean number of excised SLNs per patient was 3.3
(range, 1–8). The mean clinical and histopathological tumor size
was 12.6 and 13.1 mm in diameter, respectively.
Pre-operative data are shown in Table I. In 75% of the patients, the
marked node in the axillary area was detected with the γ camera.
Moreover, in four patients lymphoscintigraphy detected two marked
axillary lymph nodes.
 | Table IPre-operative patient data. |
Table I
Pre-operative patient data.
| Patient data | No. of patients | % |
|---|
| Tumor location | | |
| Supero extern | 8 | 33.3 |
| Supero intern | 6 | 25.0 |
| Supero median | 2 | 8.3 |
| Infero extern | 1 | 4.2 |
| Infero median | 1 | 4.2 |
| Equato extern | 4 | 16.7 |
| Equato intern | 1 | 4.2 |
| Retro mammary | 1 | 4.2 |
| Scintigraphy | | |
| Axillary | 18 | 75.0 |
| Axillary
double | 4 | 16.7 |
| Internal
mammary | 1 | 4.2 |
| Axillary + internal
mammary | 1 | 4.2 |
When only one node was visualized, the mean of the
excised sentinel lymph node was 2.7. That number increased to 6.3
when lymphoscintigraphy showed two axillary SLNs. No pathological
metastases were found in SLN in 65 surgical sections (83.3%).
Metastatic disease was found in 13 histopathological specimens (9
with micro- and 4 with macrometastases), originating from 10
patients (Table II). The
histopathological characteristics of the tumor,
Scarff-Bloom-Richardson (SBR) grade, oestrogen receptor,
progesterone receptor, Ki-67 and HER2 are shown in Table III.
 | Table IIResults of the SLN analysis. |
Table II
Results of the SLN analysis.
| Scintigraphy
information | Biopsied SLNs, n | Histological
status | No. of SLNs |
|---|
| Axillary SLN | 48 | Uninvolved | 40 |
| Micrometastases | 7 |
| Macrometastases | 1 |
| Axillary double | 25 | Uninvolved | 23 |
| Micrometastases | 0 |
| Macrometastases | 2 |
| Internal mammary | 3 | Uninvolved | 2 |
| Micrometastases | 1 |
| Macrometastases | 0 |
| Left axillary +
intern mammary | 2 | Uninvolved | 0 |
| Micrometastases | 1 |
| Macrometastases | 1 |
 | Table IIIHistopathological patient
characteristics. |
Table III
Histopathological patient
characteristics.
| Characteristics | No. of patients | % |
|---|
| SBR grade | | |
| I | 10 | 41.7 |
| II | 10 | 41.7 |
| III | 4 | 16.7 |
| Oestrogen
receptor | | |
| Negative | 2 | 8.3 |
| Positive | 22 | 91.7 |
| Progesterone
receptor | | |
| Negative | 3 | 12.5 |
| Positive | 21 | 87.5 |
| Ki-67 (%) | | |
| 0–10 | 7 | 29.2 |
| 11–20 | 9 | 37.5 |
| 21–30 | 3 | 12.5 |
| >30 | 4 | 16.7 |
| Unknown | 1 | 4.2 |
| HER2 | | |
| Negative | 21 | 87.5 |
| Positive | 3 | 12.5 |
Detection results
Measurements were carried out ex vivo in the
Department of Pathology (Paul Strauss Cancer Center) pending
clearance for per-operatory use.
All of the 78 nodes were detected by the isotopic
probe. The 8 SLNs without dye marking were used to validate the
probe, and as such did not yield any relative PBV concentration.
Subsequently, only the 70 excised SLNs marked with PBV were
considered. The dye-marked SLNs were detected by the optical probe,
regardless of the visibility of the dye uptake. Subsequent to
injection of 2, 1, 0.5 and 0.25 ml dye, 3, 7, 6 and 54 SLNs were
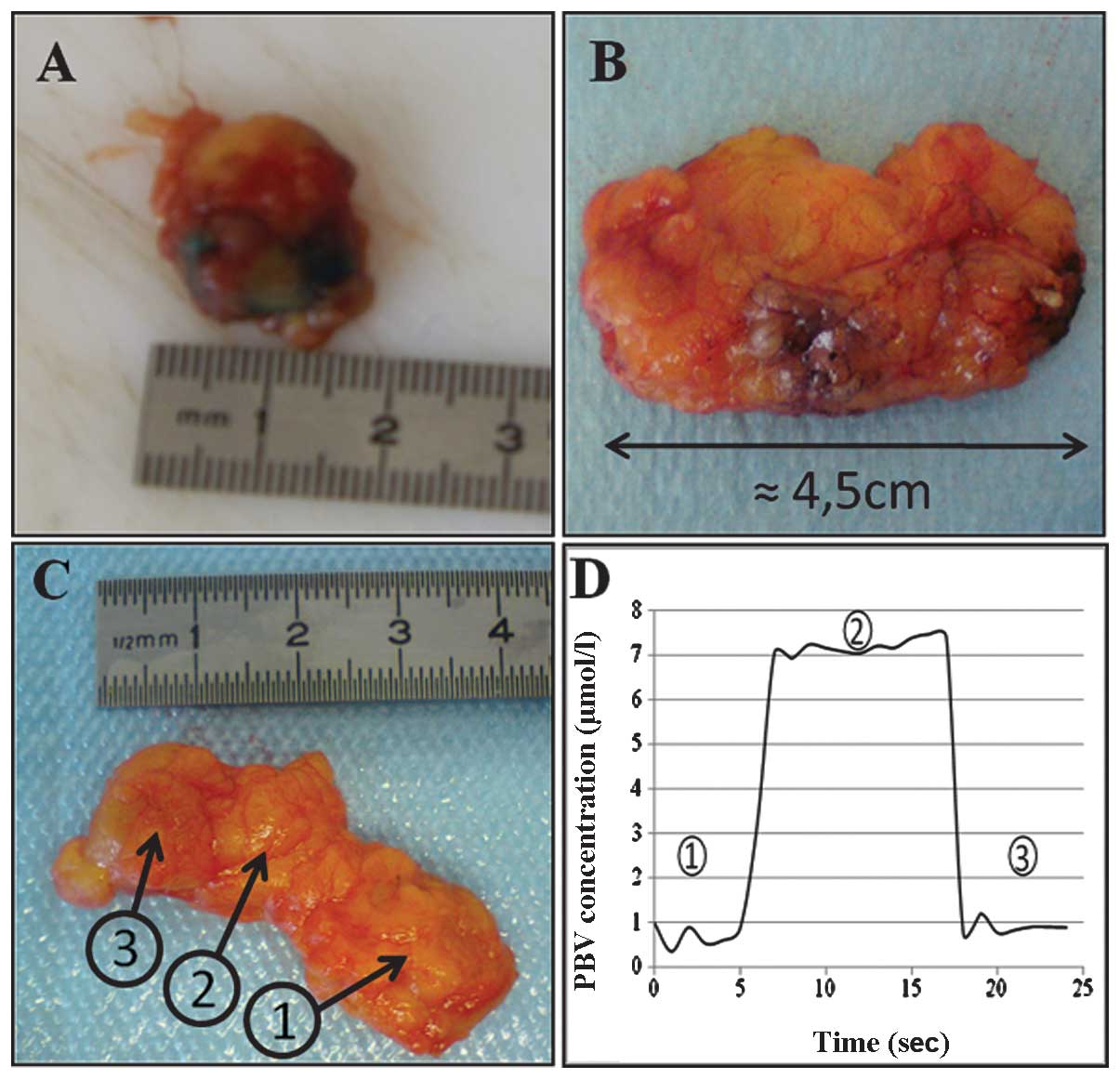
detected, respectively. The visual aspects of the surgical sections
coloured by various PBV quantities are shown in Fig. 3.
For each surgical section and each injection volume
the optical probe was able to detect the presence of exogenous dye
in the tissue sample. However, only 53 nodes (i.e., 67.9%) were
visually detected by the surgeon. Of the total number of excised
nodes, 13 were micro- and macrometastatically involved. All of the
nodes were detected by the isotopic and optical probe, whereas only
9 (69.2%) metastatic nodes were detected by visual inspection
(Table IV).
 | Table IVComparison of the sensibility
detection of dye-marked SLNs. |
Table IV
Comparison of the sensibility
detection of dye-marked SLNs.
| Detection method | Total no. of SLNs
(%) | No. of metastatic
SLNs (%) |
|---|
| Europrobe | 70 (100) | 13 (100) |
| Optical probe | 70 (100) | 13 (100) |
| Surgeon eye | 53 (67.9) | 9 (69.2) |
Fig. 3C is an
example of SLN localization using our optical prototype on a biopsy
sample after a 0.25-ml dye injection. During the measurement, the
probe was initially directed to the part of the excised tissue not
containing the node. When the pen probe was placed in front of the
SLN, dye was observed in the node. Detection occurred from 7 to 17
sec, as shown in Fig. 3D, with the
PBV concentration profile increasing from 1 to 7 μmol/l.
During the final seconds, the probe was not directed to the node
any longer.
The 17 visually undetected nodes varied with respect
to their histological status: 13 were uninvolved, 3 were
micrometastatic and 1 was macrometastatic. One of the nodes was
excised after the injection of 0.5 ml PBV, while the remaining
nodes were excised after the injection of 0.25 ml PBV. To compare
these nodes, only the 16 SLNs marked with 0.25 ml dye were
considered.
In the 16 nodes measured with the probe, the mean
relative PBV concentration was 5.5±1.4 μmol/l. The
individual values were also analyzed as a function of the stage of
metastatic invasion. The mean relative PBV concentration was
5.8±1.8 μmol/l in the 12 uninvolved nodes, 4.9±3.3
μmol/l in the 3 micrometastatic nodes and 4.3±0.5
μmol/l in the single macrometastatic node. Thus, the
standard deviation corresponded to the signal variations detected
during measurement. Although these results showed a low spreading
of values in the sample categories, these data are not sufficient
to establish a possible correlation between the histological status
and relative dye concentration in the SLNs. The number of surgical
sections available for the histological statuses (micro- and
macrometastatic) was not adequate for an appropriate statistical
analysis.
Discussion
The main advantage of the developed optical probe is
its sensitivity in detecting PBV as used in routine clinical
practice for SLN detection.
These experiments demonstrated that the instrument
allowed for the measuring of the relative dye concentration in
surgical sections. Currently, approximately 1% of the nodes are
undetectable when using a radiotracer and a dye during sentinel
lymph node biopsy (19). An
increase in the optical sensitivity using a probe is most likely to
reduce this false negative detection. In this case, optical
detection was effective for each excised node, regardless of the
dye concentration injected, even for the potentially lowest
concentration used in the present study with a view to achieve a
visually undetectable uptake. Upon visual inspection by clinicians
only 53 nodes were detected. The mean relative PBV concentration
was 5.5±1.4 μmol/l measured in the SLNs with visually
undetectable/infravisible dye-mark had a relatively low dispersion.
Detection with the probe was effective for patients with different
clinical status and a good reproducibility.
The dye distribution in different nodes subsequent
to injection of small concentrations of PBV was determined in
previous pre-clinical studies with the present experimental setup
(15). Those results, combined
with the findings of the present study, open promising future
perspectives in the operating room.
These experiments demonstrated the limited extent of
SLN detection. This problem might be overcome by increasing one of
the two following parameters: the source/detector separation and/or
the laser intensities. Time-resolved optical methods also have the
potential of being interesting alternatives to this approach. Being
cost-effective, such techniques increase the extent of the
detection, while improving the spatial resolution. (20).
The present results are promising, suggesting that
the development of an opto-nuclear probe is an interesting approach
to reduce false negative rates. This new technique might be used
during node excision and provides surgeons with a simple diagnostic
tool, without significantly changing their surgical practice.
Additionally, the instrumentation and dye are cost-effective.
In conclusion, there is skin tattoo risk associated
with the injection of the PBV, while decreasing the injected dose
(by a factor 4) might certainly reduce this undesirable side-effect
in patients.
Acknowledgements
This study was conducted with the
financial support of the European Convention ‘Nanomagdye’ EP
7-NMP-2007-SMALL Nr214032, and a research grant from the ANRT
(Agence Nationale pour la Recherche et la Technologie).
References
|
1.
|
Veronesi U, Paganelli G, Viale G, Kuini A,
Zurrida S, Galimberti V, Intra M, Veronesi P, Robertson C,
Maisonneuve P, Renne G, De Cicco C, De Lucia F and Gennari R: A
randomized comparison of sentinel node biopsy with routine axillary
dissection in breast cancer. N Engl J Med. 349:546–553. 2003.
|
|
2.
|
Giuliano AE, Kirgan DM, Guenther JM and
Morton DL: Lymphatic mapping and sentinel lymphadenectomy for
breast cancer. Ann Surg. 220:391–401. 1994.
|
|
3.
|
Rodier JF, Velten M, Wilt M, Martel P,
Ferron G, Vaini-Elies V, Mignotte H, Brémont A, Classe JM, Dravet
F, Routiot T, Tunon de lara C, Avril A, Lorimier G, Fondrinier E,
Houvenaeghel G and Avigdor S: Prospective multicentric randomized
study comparing periareolar and peritumoral injection of
radiotracer and blue dye for the detection of sentinel lymph node
in breast sparing procedures: FRANSENODE trial. J Clin Oncol.
25:3664–3669. 2007.
|
|
4.
|
Garcia-Manero M, Olartecoechea B and Royo
P: Different injection sites of radionuclide for sentinel lymph
node detection in breast cancer: single institution experience. Eur
J Obstet Gynecol. 153:185–187. 2010.
|
|
5.
|
Newton DW, Breen PJ, Brown DE, Mackie JF
and Kluza RB: Physicochemical characteristics of patent blue violet
dye. J Pharm Sci. 70:122–127. 1981.
|
|
6.
|
Radovanovic Z, Golubovic A, Plzak A,
Stojiljkovic B and Radovanovic D: Blue dye versus combined blue
dye-radioactive tracer technique in detection of sentinel lymph
node in breast cancer. Eur J Surg Oncol. 30:913–917. 2004.
|
|
7.
|
Barthelmes L, Goyal A, Newcombe RG,
McNaill F and Mansel RE: Adverse reactions to patent blue V dye -
The NEW START and ALMANAC experience. Eur J Surg Oncol. 36:399–403.
2010.
|
|
8.
|
Rodier JF: Detection of the sentinel node
by the surgeon. Bull Cancer. 89:840–844. 2002.(In French).
|
|
9.
|
Murray AD, Staff RT, Redpath TW, Gilbert
FJ, Ah-See AK, Brookes JA, Miller ID and Payne S: Dynamic contrast
enhanced MRI of the axilla in women with breast cancer: comparison
with pathology of excised nodes. Br J Radiol. 75:220–228. 2002.
|
|
10.
|
Cooper KL, Harnan S, Meng Y, Ward SE,
Fitzgerald P, Papaioannou D, Wyld L, Ingram C, Wilkinson and Lorenz
E: Positron emission tomography (PET) for assessment of axillary
lymph node status in early breast aancer: A systematic review and
meta-analysis. Eur J Surg Oncol. 37:187–198. 2011.
|
|
11.
|
Britton P, Moyle P, Benson JR, Goud A,
Sinnatamby R, Barter S, Gaskarth M, Provenzano E and Wallis M:
Ultrasound of the Axilla : where to look for the sentinel lymph
node. Clin Radiol. 65:373–376. 2010.
|
|
12.
|
Buckle T, van Leeuwen AC, Chin PTK,
Janssen H, Muller SH, Jonkers J and van Leeuwen FW: A
self-assembled multimodal complex for combined pre and
intraoperative imaging of the sentinel lymph node. Nanotechnology.
21:3551012010.
|
|
13.
|
Akers WJ, Kim C, Berezin M, Guo K, Fuhrhop
R, Lanza GM, Fischer GM, Daltrozzo E, Zumbusch A, Cai X, Wang LV
and Achilefu S: Noninvasive photoacoustic and fluorescence sentinel
lymph node identification using dye-loaded perfluorocarbon
nanoparticles. ACS Nano. 5:173–182. 2011.
|
|
14.
|
Tellier F, Rasata R, Simon H, Wilt M,
Rodier JF and Poulet P: Une sonde optique au service du chirurgien
pour la détection du ganglion sentinelle dans le cancer du sein :
‘le troisième œil’. La lettre du sénologue. 51:35–37. 2011.
|
|
15.
|
Tellier F, Rasata R, Simon H, Chabrier R,
Steibel J and Poulet P: Sentinel lymph node detection by an optical
method using scattered photons. Biomed Opt Express. 1:902–910.
2010.
|
|
16.
|
Tellier F, Simon H, Blé FX, Rasata R,
Chabrier R, Steibel J, Rodier JF and Poulet P: Comparison of 2- and
4-wavelength methods for the optical detection of sentinel lymph
node. Proceedings Paper SPIE Munich. 8092: View Article : Google Scholar : 2011.
|
|
17.
|
Prahl S: Oregon Medical Laser Center:
Optical properties spectra. http://omlc.ogi.edu/spectra/index.html,
2011. Accessed March 1, 2011.
|
|
18.
|
Delpy DT, Cope M, van der Zee P, Arridge
S, Wray S and Wyatt J: Estimation of optical pathlength through
tissue from direct time of flight measurement. Phys Med Biol.
33:1433–1442. 1988.
|
|
19.
|
Kang T, Yi M, Hunt KK, Mittendorf EA,
Babiera GV, Kuerer H, Bedrosian I, Hwang RF, Lucci A and
Meric-Bernstam F: Does Blue dye contribute to success of sentinel
node mapping for breast cancer? Ann Surg Oncol. 17:280–285.
2010.
|
|
20.
|
Amouroux M, Uhring W, Pebayle T, Poulet P
and Marlier L: A safe, low-cost and portable instrumentation for
bedside time-resolved picosecond near infrared spectroscopy.
Proceedings Paper SPIE Munich. 7371: View Article : Google Scholar : 2009.
|