Introduction
The majority of the common primary neoplasms which
metastasize to the adrenal gland include melanoma, lung cancer,
breast carcinoma, colon malignant tumor and renal cell carcinoma
(1). In practice, adrenal gland
metastasis normally results from systemic metastasis, particularly
in the advanced stage of the primary neoplasms like breast
carcinoma, and the most common method of metastasis is blood-borne
(2,3).
Breast carcinoma is the most common malignancy in females, while
the primary histological type of the breast cancer is invasive
ductal carcinoma. A report revealed that ~80% of all breast cancer
types are breast invasive ductal carcinomas (4), which normally metastasize to the lung,
liver, bone and brain; however, metastasis to the adrenal gland is
rare (5). Metastasis of breast
carcinoma often leads to a poorer prognosis and a lower 5-year
survival rate (6). Patients who have
solitary adrenal gland metastasis normally have a long-term
survival compared with those who exhibit synchronous metastasis
(7). Laparoscopic adrenalectomy (LA),
the treatment of adrenal gland metastases, has become more and more
acceptable.
The present study reported a rare case of left
adrenal gland metastasis of breast invasive ductal carcinoma, in
good condition, following treatment with LA. This case is the
newest and the sixth to be presented in the literature. The present
study was approved by the Ethics Committee of Peking University
Shenzhen Hospital (Shenzhen, China) and the written informed
consent was provided by the patient.
Case report
A 35-year-old female, who was found to have a mass
located on the left adrenal gland during a routine examination by
positron emission tomography/computed tomography (PET/CT) in
Shenzhen Armed Police Hospital (Shenzhen, China) on May
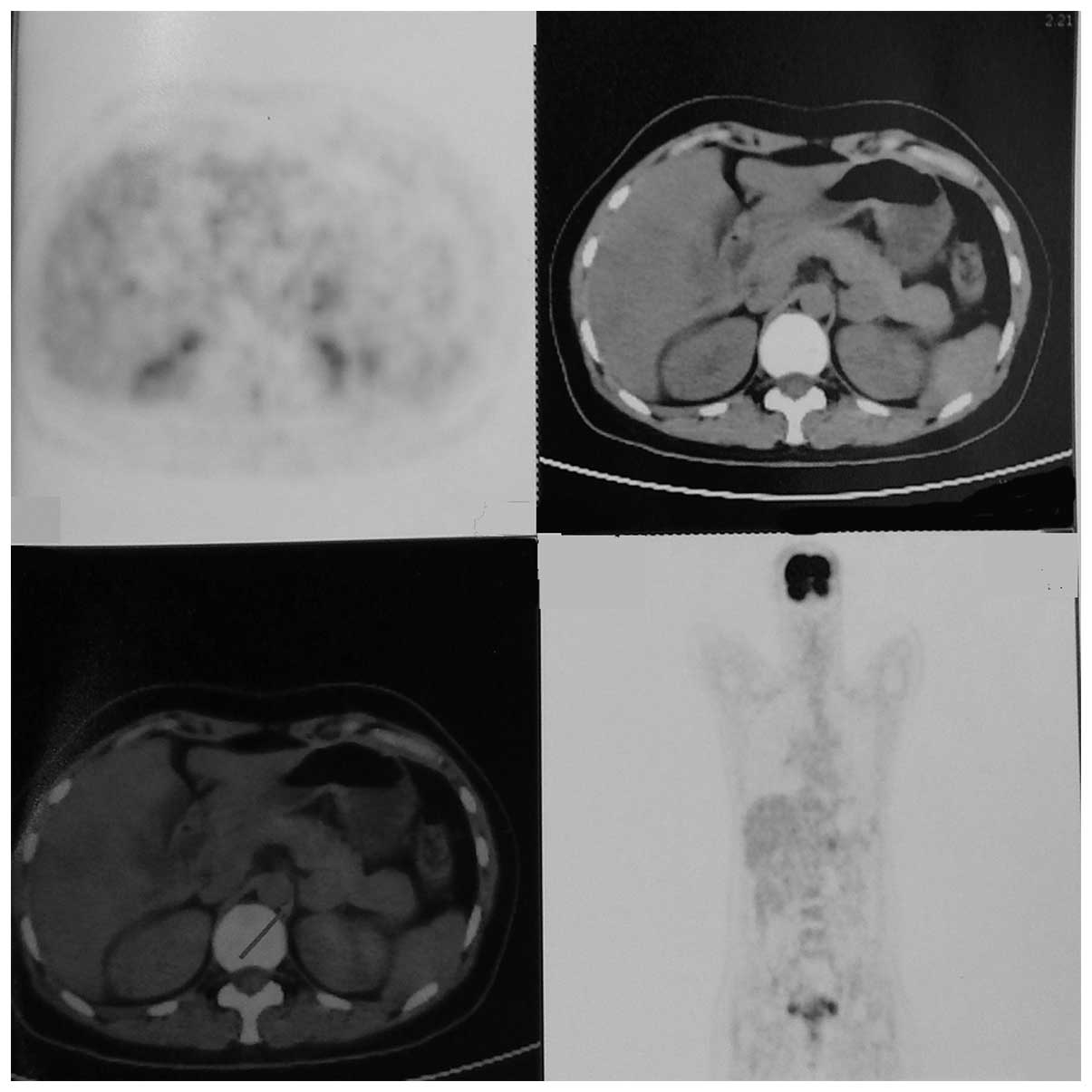
15th 2015. The PET/CT revealed a nodular hypermetabolic
focus located on the left adrenal gland, measuring 2.5×2.6×2.8 cm,
and the maximum standardized uptake value was 3.9 (Fig. 1). Therefore, the possibility of
metastasis was considered. The patient was subsequently admitted to
the Department of Urology, Peaking University Shenzhen Hospital
(Shenzhen, China) for further examination and therapy on June
1st 2015. The patient was diagnosed with left breast
cancer 5 years ago and had undergone mastectomy, followed by
regular chemotherapy and radiotherapy. The patient was asymptomatic
with a normal appetite, no abdominal pain and no weight changes.
Additionally, urinary, respiratory, cardiovascular or
constitutional symptoms were negative. Physical examination
revealed a well-developed and well-nourished female whose pulse,
temperature, blood pressure and respiration rate were all within
normal limits. The chest was clear to percussion and auscultation,
and no masses were palpable on abdominal examination. Laboratory
examinations, including routine hematological examination and
biochemical tests, were within normal limits. The plasma
adrenocorticotropic hormone and cortisol levels were within a
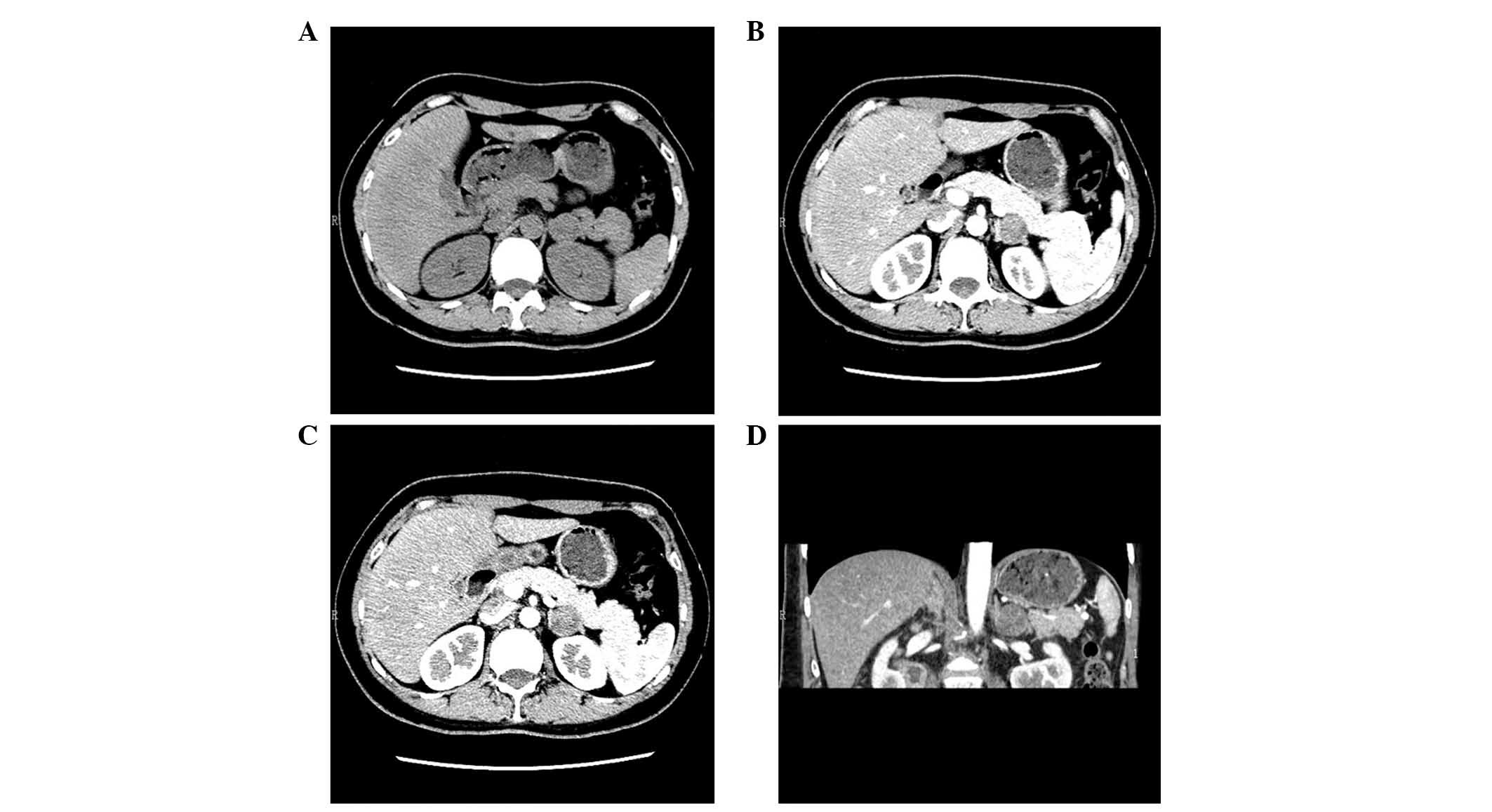
normal range. An adrenal CT scan, enhanced adrenal CT and
three-dimensional imaging were performed, which revealed a
2.1×2.3×2.4 cm round abnormal density shadow [23–26 Hounsfield
units (HU)] in the lateral branches of the left adrenal gland with
clear and smooth edges. Also, the density of the shadow was
heterogeneous (Fig. 2). Enhanced CT
revealed a mild to moderate strengthening of the mass (33–63 HU;
Fig. 2).
The left adrenal gland LA was performed on June
9th 2015. A tumour with clear margin, 2.5 cm in
diameter, was located on the upside of the left kidney and the
tumour exhibited mild adhesion with the surrounding tissue. Normal
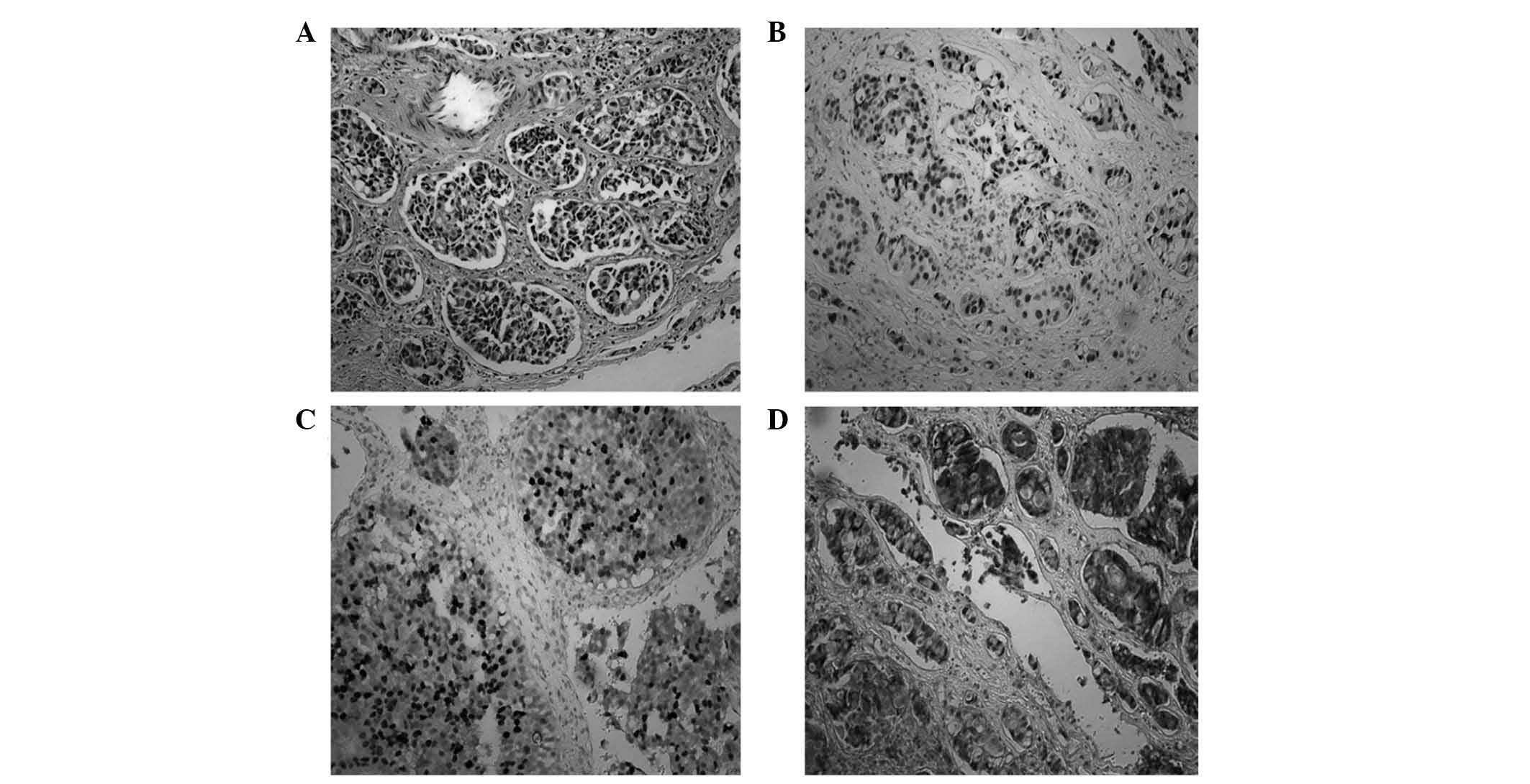
adrenal gland tissue was not observed. The pathological report
revealed irregular nest clusters, adenous duct-like heterotypic
cells in the adrenal gland tissue, the growth of the cells were
infiltrative and piecemeal necrosis was observed (Fig. 3). The result of immunohistochemistry
was as follows: Estrogen receptor (+), progesterone receptor (+)
and human epidermal growth factor-2 (+/++; Fig. 3). The diagnosis of adrenal gland
metastasis of breast invasive ductal carcinoma was subsequently
confirmed.
The patient was discharged on the 7 days
post-operation. At the time of writing, no problems were reported
with the patient.
Discussion
Adrenal gland metastasis, metastasized from breast
invasive ductal carcinoma, are extremely rare. Only 5 cases, to the
best of our knowledge, have been reported previously in the
literature (Table I) (2,5,6,8,9). The present case is the newest and the
sixth in the literature. A previous study by Borst and Ingold
(10), including 2,246 patients with
breast invasive ductal carcinoma, revealed no adrenal gland
metastasis in those patients.
 | Table I.Reported cases of adrenal gland
metastasis of breast invasive ductal carcinoma. |
Table I.
Reported cases of adrenal gland
metastasis of breast invasive ductal carcinoma.
| Case | Authors, year | Age (years) | Tumor size (cm) | Clinical
features | Location |
Immunohistochemistry | (Refs.) |
|---|
| 1 | Liu et al,
2010 | 64 | 6 | Asymptomatic | Left adrenal
gland | C-erbB-2+,
GCDFP-15+, | (5) |
| 2 | Yoshitomi et
al, 2012 | 46 | NA | Asymptomatic | Right adrenal
gland |
E-cadherin+,
CK+ | (2) |
| 3 | Akhtar et al,
2012 | 45 | 2.8 | Pain in abdomen and
shortness of breath | Left adrenal
gland | ER+,
PgR+, HER 2+ | (8) |
| 4 | Eren et al,
2012 | 38 | 4 | Asymptomatic | Left adrenal
gland | NA | (6) |
| 5 | Andjelić-Dekić et
al, 2014 | 58 | NA | Asymptomatic | Left adrenal
gland | HER2+ | (9) |
The majority of patients with adrenal gland
metastases are asymptomatic, while a small proportion of the
patients may present adrenal gland disfunction if the malignant
mass replaces or destroys the normal adrenal gland tissues
(6). Although primary adrenal gland
malignancies like adrenocortical carcinomas usually secrete hormone
excessively and cause certain relative symptoms, or are followed
with other symptoms, including hemorrhage, abdominal distension or
discomfort (11), metastatic adrenal
gland carcinomas are often difficult to identify from primary
adrenal gland malignancies, which can lead to misdiagnosis
(5). Each patient who has a history
of malignance and mass >2 cm in diameter in adrenal gland must
be highly considered as a possible case of adrenal gland metastasis
(1). Normally, a CT scan and magnetic
resonance imaging can be used as a prior option to identify primary
carcinoma and metastases of the adrenal gland (5). The patient in the present case was
asymptomatic with no abdominal pain or other problems; however, she
had a history of left breast carcinoma and a PET/CT revealed a
nodular hypermetabolic focus located on the left adrenal region,
measuring 2.5×2.6×2.8 cm, which was considered as a possible
metastasis.
LA has become the acceptable and is currently the
first option of surgical treatment in adrenal gland tumors
(1) as it has many advantages,
including reduced requirement of analgesia following surgery and
the patient being discharged earlier (11). However, while performing LA to resect
primary carcinoma or metastasis of the adrenal gland,
carcinomatosis and port-site metastasis, which may be caused by
several factors, including the behavior of the tumor, patient's
condition and the operation of surgery, should be taken into
consideration as they have been reported previously (12). It is also important to avoid port-site
metastasis and carcinomatosis when performing LA. Therefore,
whether LA can be widely applied to adrenal gland tumors remains
controversial (13). If it is
necessary to perform adrenalectomy, particularly for bilateral
adrenal gland metastasis, partial adrenalectomy is an alternative
and ideal treatment strategy. When performing partial
adrenalectomy, minimally invasive surgical procedures, including
laparoscopic or robotic procedures, are ideal options, which may
assist in avoiding endocrinological complications caused by
adrenalectomy, including iatrogenic Addison's disease (14). Notably, combining this with
radiotherapy, chemotherapy and hormone replacement therapy can
provide an improved outcome in prolonging survival (5).
In conclusion, a case of adrenal gland metastasis of
breast invasive ductal carcinoma was reported in the present study.
The metastasis of breast carcinoma to the adrenal gland is rare,
therefore it is important to identify metastasis and primary
adrenal gland tumors. Definite diagnosis can be established by CT
and pathological examination. As one of treatments of adrenal gland
metastasis, the role of LA in prolonging survival remains to be
further elucidated in future studies.
Acknowledgements
The present study was supported by the National
Natural Science Foundation of China (no. 81101922), the Science and
Technology Development Fund Project of Shenzhen (nos.
JCYJ20130402114702124 and JCYJ20150403091443329) and the fund of
Guangdong Key medical subject.
References
|
1
|
Suzuki H: Laparoscopic adrenalectomy for
adrenal gland carcinoma and metastases. Curr Opin Urol. 16:47–53.
2006. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Yoshitomi S and Tsuji H: A case of
recurrent breast cancer with solitary adrenal gland metastasis
treated with surgery and endocrine therapy. Gan To Kagaku Ryoho.
39:2074–2076. 2012.(In Japanese). PubMed/NCBI
|
|
3
|
Do YR, Song HS and Kim IH: Adrenalectomy
for metastatic disease to the adrenal gland from gastric cancer:
Report of a case. Korean J Intern Med. 22:18–20. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Toikkanen S, Pylkkänen L and Joensuu H:
Invasive lobular carcinoma of the breast has better short- and
long-term survival than invasive ductal carcinoma. Br J Cancer.
76:1234–1240. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Liu XJ, Shen P, Wang XF, Sun K and Sun FF:
Solitary adrenal gland metastasis from invasive ductal breast
cancer: An uncommon finding. World J Surg Oncol. 8:72010.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Eren OO, Ordu C, Selcuk NA, Akosman C,
Ozturk MA, Ozkan F, Gokce O and Oyan B: Bilateral synchronous
adrenal gland metastasis of invasive ductal carcinoma treated with
multimodality therapy including adrenalectomy and oophorectomy. J
Oncol Pharm Pract. pii: 1078155214551314. 2014.PubMed/NCBI
|
|
7
|
Shen WT, Sturgeon C and Duh QY: From
incidentaloma to adrenocortical carcinoma: The surgical management
of adrenal gland tumors. J Surg Oncol. 89:186–192. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Akhtar K, Sherwani R and Kahkhashan E:
Carcinoma breast metastasis to the suprarenal gland: An unusual
presentation. Pol J Pathol. 63:284–285. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Andjelić-Dekić N, Božović-Spasojević I,
Milošević S, Matijašević M and Karadžić K: A rare case of isolated
adrenal gland metastasis of invasive ductal breast carcinoma. Srp
Arh Celok Lek. 142:597–601. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Borst MJ and Ingold JA: Metastatic
patterns of invasive lobular versus invasive ductal carcinoma of
the breast. Surgery. 114:637–641; discussion 641–642.
1993.PubMed/NCBI
|
|
11
|
Zografos GN, Perysinakis I, Kyrodimou E,
Kassi E and Kaltsas G: Surgical treatment of potentially primary
malignant adrenal gland tumors: An unresolved issue. Hormones
(Athens). 14:47–58. 2015.PubMed/NCBI
|
|
12
|
Kajáry K, Molnár P, Lengyel Z and Szakáll
S Jr: Port-site metastasis after laparoscopic removal of an
isolated adrenal gland metastasis in a patient with breast cancer
detected with FDG PET/CT. Clin Nucl Med. 39:203–205.
2014.PubMed/NCBI
|
|
13
|
Shoji S, Usui Y, Nakano M, Hanai K, Sato
H, Uchida T and Terachi T: Surgical management of metastatic
adrenal gland tumors: Decision-making factors in imaging. Oncol
Lett. 1:967–971. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Öztürk H: Bilateral synchronous adrenal
gland metastases of renal cell carcinoma: A case report and review
of the literature. Oncol Lett. 9:1897–1901. 2015.PubMed/NCBI
|