Introduction
Regorafenib is an oral multi-kinase inhibitor which
targets tumor angiogenesis [vascular endothelial growth factor
receptor (VEGFR)1-3 and TIE2], tumor microenvironment
(platelet-derived growth factor receptor β (PDGFRβ) and fibroblast
growth factor receptor-1), and oncogenesis (c-KIT, RET, RAF-1 and
B-RAF) (1). Based on this mode of
action, regorafenib has a broad spectrum of toxicities (2). To date, however, few reports have
focused on autoimmune adverse events.
Case report
The patient was a Japanese woman who had a past
medical history of chronic immune thrombocytopenic purpura (ITP)
which developed at the age of 38 years and was treated with steroid
therapy, which resulted in remission for more than 20 years without
medication. She was diagnosed with recurrent colon cancer at age 66
years, after primary surgery and adjuvant chemotherapy with
capecitabine plus oxaliplatin. She had received three lines of
palliative chemotherapy including fluorouracil, leucovorin, and
irinotecan (FOLFIRI) plus bevacizumab, panitumumab monotherapy and
trifluridine/tipiracil. Platelet-associated IgG (PAIgG) was not
detected when FOLFIRI plus bevacizumab was initiated. High-grade
thrombocytopenia was not observed during treatment for recurrent
colon cancer.
As a standard therapy in the late-line setting for
recurrent/metastatic colorectal cancer (3,4),
treatment with regorafenib 160 mg orally once daily for 21 days
on/7-days off in a 28-day cycle was initiated at the age of 68
years. Platelet count was 167x109/l on day 1 but dropped
to 61x109/l on day 15, and regorafenib was continued. On
day 18, she vomited blood and presented at the emergency
department. Laboratory examination showed severe thrombocytopenia
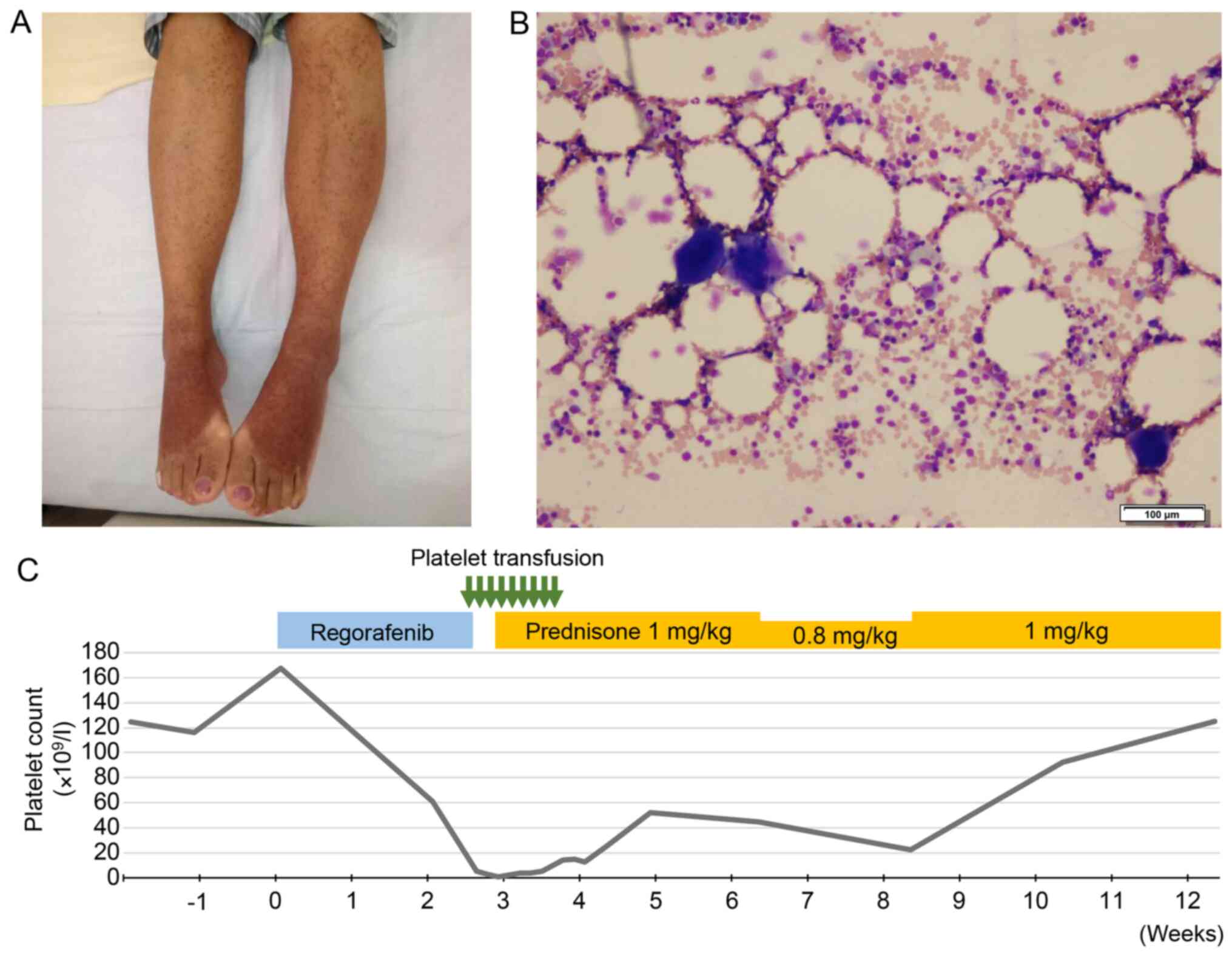
with a platelet count of 5x109/l (Table I). Petechiae and purpura in the
extremities and hemorrhagic blisters in the oral mucosa were also
observed (Fig. 1A). Multiple
platelet transfusions were given, but the response was poor.
Further laboratory examination showed increased PAIgG of 176 ng
(normal range <27.6 ng) and negative IgG for H. pylori
and heparin-induced thrombocytopenia antibody (Table I). There were no clinical
manifestations suggested systemic lupus erythematosus (SLE), such
as arthritis, mucocutaneous involvement or Raynaud's phenomenon.
Diagnostic criteria of SLE were not met. Bone marrow examination
revealed normal hematopoiesis, slightly increased megakaryocytes
and no myelodysplasia or tumor metastasis (Fig. 1B). There was no evidence of other
risk factors for exacerbation of ITP, including a history of taking
any dietary supplements or medications, or viral infections. Taken
together, these findings strongly suggested regorafenib exacerbated
ITP. Regorafenib was permanently discontinued, and prednisone 1
mg/kg/day was administrated on day 21. The hemorrhagic diathesis
resolved one week later, and the severe thrombocytopenia gradually
recovered (Fig. 1C).
 | Table ILaboratory data. |
Table I
Laboratory data.
| Variable | Reference range | Result |
|---|
| White blood cell
count, 100/µl | 33-86 | 50 |
| Red blood cell count,
106/µl | 3.86-4.92 | 2.90 |
| Hemoglobin, g/dl | 11.6-14.8 | 9.3 |
| Hematocrit, % | 35.1-44.4 | 28.4 |
| Platelet count,
109/l | 158-348 | 5 |
| Immature platelet
fraction, % | 1-4.8 | 16.3 |
| APTT, sec | 25.0-38.0 | 31.6 |
| PT, % | 70.0-130.0 | 94.0 |
| Fibrinogen,
mg/dl | 200-400 | 298 |
| D dimer, µg/ml | <1 | 4.1 |
| Lactate
dehydrogenase, U/l | 124-222 | 615 |
| Aspartate
transaminase, U/l | 13-30 | 32 |
| Alanine
aminotransferase, U/l | 7-23 | 17 |
| Total bilirubin,
mg/ml | 0.4-1.5 | 1.6 |
| Creatinine,
mg/dl | 0.46-0.79 | 0.87 |
| Blood urea nitrogen,
mg/dl | 8-20 | 26.8 |
| C-reactive protein,
mg/dl | 0.00-0.14 | 1.55 |
| PA IgG,
ng/107 cells | <27.6 | 176.8 |
| 50% complement
hemolysis, U/ml | 25-51 | 30.2 |
| Complement C3,
mg/dl | 73-138 | 72 |
| Complement C4,
mg/dl | 11-31 | 11 |
| Antinuclear antibody,
IF | <40 | 320x |
| Antinuclear antibody
pattern | | Centromere
pattern |
| HIT antibody,
U/ml | <1 | <0.6 |
| IgG antibody for
H. pylori, U/ml | <10 | 3 |
| Hepatitis B surface
antigen, IU/ml | <0.0049 | <0.003 |
| Hepatitis C virus
antibodies, COI | <0.99 | 0.04 |
| HIV antibody/antigen
combo assay, S/CO | <0.99 | 0.12 |
Discussion
Thrombocytopenia associated with regorafenib is not
rare. A meta-analysis reported incidences of all-grade and
high-grade thrombocytopenia 22 and 3%, respectively (5). Inhibition of VEGFR is a potential
mechanism of regorafenib-induced myelosuppression (6,7).
Conventional thrombocytopenia is associated with bone marrow
hypoplasia and responds to blood transfusion. In the present case,
in contrast, normal hematopoiesis was maintained, and
thrombocytopenia was refractory to platelet transfusion, which is
likely explained by an autoimmune mechanism.
Diagnosis of ITP requires exclusion of a variety of
potential causes for thrombocytopenia. Many conditions which cause
decreased platelet production such as bone marrow damage,
infiltration and replacement of the bone marrow due to malignancies
and myelodysplastic syndromes were excluded by findings form the
bone marrow biopsy in the present case. Drug-induced
thrombocytopenia (DITP) is difficult to be distinguished from ITP.
However, a history of ITP and unrecovered thrombocytopenia after
discontinuation of regorafenib suggested more likely ITP than DITP
(8). Moreover, a very low platelet
count nadir less than 20x109/l, response to steroid and
a positive anti-platelet autoantibody test are supposed to help
precise diagnosis of ITP from expert opinions (9,10).
Based on the above, the diagnosis of ITP was very likely.
ITP is an autoimmune disease which is characterized
by platelet destruction associated with antibodies to platelets and
megakaryocyte dysfunction (11).
The pathogenesis of ITP is complicated and has not been fully
clarified. Recent findings suggest that dysfunction of mesenchymal
stem cells (MSCs) plays an important role (12,13).
MSCs derived from ITP patients (MSCs-ITP) showed impaired
self-proliferative capacity and the loss of immunosuppressive
function. Interestingly, treatment of MSCs-ITP with PDGF-BB, a
ligand of PDGFRβ, could reverse the defect of MSC-ITP in
vitro (13). In this basis,
regorafenib-induced inhibition of PDGF-BB/PDGFRβ signaling might
trigger dysfunction of MSCs, resulting in the exacerbation of ITP.
VEGF/VEGFR signaling is another important target of regorafenib,
however, exacerbation of ITP had not occurred during bevacizumab
containing treatment in the first-line setting at age of 66 years,
which supports the hypothesis above.
Several multi-kinase inhibitors other than
regorafenib also inhibit PDGF/PDGFR signaling, which may exacerbate
ITP. Imatinib and sunitinib have been reported to induce immune
thrombocytopenia (14,15), albeit that these studies did not
investigate the possibility of pre-existing MSC dysfunction.
In conclusion, we report the first case of
regorafenib-induced exacerbation of ITP in remission. This case
report highlights the need for caution with regard to regorafenib
treatment in cancer patients with concomitant ITP.
Acknowledgements
The authors would like to thank Dr Maki Kanzawa
(Department of Diagnostic Pathology, Kobe University Graduate
School of Medicine, Kobe, Japan) for pathological diagnosis.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
SK and YI made substantial contributions to the
conception and design of the study. SK, YI, KY, AH and NK made
substantial contributions to the acquisition of the data. SK, YI
and KY drafted the manuscript. AH, TK, YFuj, YFun, MT, NK, HMa and
HMi made substantial contributions to the analysis and
interpretation of the data and were involved in revising the
manuscript critically for important intellectual content. All
authors read and approved the final manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Written informed consent was obtained from the
patient for publication of the clinical data and images.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Wilhelm SM, Dumas J, Adnane L, Lynch M,
Carter CA, Schütz G, Thierauch KH and Zopf D: Regorafenib (BAY
73-4506): A new oral multikinase inhibitor of angiogenic, stromal
and oncogenic receptor tyrosine kinases with potent preclinical
antitumor activity. Int J Cancer. 129:245–255. 2011.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Krishnamoorthy SK, Relias V, Sebastian S,
Jayaraman V and Saif MW: Management of regorafenib-related
toxicities: A review. Therap Adv Gastroenterol. 8:285–297.
2015.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Grothey A, Van Cutsem E, Sobrero A, Siena
S, Falcone A, Ychou M, Humblet Y, Bouché O, Mineur L, Barone C, et
al: Regorafenib monotherapy for previously treated metastatic
colorectal cancer (CORRECT): An international, multicentre,
randomised, placebo-controlled, phase 3 trial. Lancet. 381:303–312.
2013.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Li J, Qin S, Xu R, Yau TC, Ma B, Pan H, Xu
J, Bai Y, Chi Y, Wang L, et al: Regorafenib plus best supportive
care versus placebo plus best supportive care in Asian patients
with previously treated metastatic colorectal cancer (CONCUR): A
randomised, double-blind, placebo-controlled, phase 3 trial. Lancet
Oncol. 16:619–629. 2015.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Zhao B and Zhao H: Incidence and risk of
hematologic toxicities in cancer patients treated with regorafenib.
Oncotarget. 8:93813–93824. 2017.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Gerber HP, Malik AK, Solar GP, Sherman D,
Liang XH, Meng G, Hong K, Marsters JC and Ferrara N: VEGF regulates
haematopoietic stem cell survival by an internal autocrine loop
mechanism. Nature. 417:954–958. 2002.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Hattori K, Heissig B, Wu Y, Dias S, Tejada
R, Ferris B, Hicklin DJ, Zhu Z, Bohlen P, Witte L, et al: Placental
growth factor reconstitutes hematopoiesis by recruiting VEGFR1(+)
stem cells from bone-marrow microenvironment. Nat Med. 8:841–849.
2002.PubMed/NCBI View
Article : Google Scholar
|
|
8
|
George JN and Aster RH: Drug-induced
thrombocytopenia: Pathogenesis, evaluation, and management.
Hematology Am Soc Hematol Educ Program 153-158, 2009.
|
|
9
|
Salib M, Clayden R, Clare R, Wang G,
Warkentin TE, Crowther MA, Lim W, Nazi I, Kelton JG and Arnold DM:
Difficulties in establishing the diagnosis of immune
thrombocytopenia: An agreement study. Am J Hematol. 91:E327–E329.
2016.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Kelton JG, Vrbensky JR and Arnold DM: How
do we diagnose immune thrombocytopenia in 2018? Hematology Am Soc
Hematol Educ Program. 2018:561–567. 2018.PubMed/NCBI View Article : Google Scholar
|
|
11
|
McMillan R, Wang L, Tomer A, Nichol J and
Pistillo J: Suppression of in vitro megakaryocyte production by
antiplatelet autoantibodies from adult patients with chronic ITP.
Blood. 103:1364–1369. 2004.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Zhang D, Li H, Ma L, Zhang X, Xue F, Zhou
Z, Chi Y, Liu X, Huang Y, Yang Y and Yang R: The defective bone
marrow-derived mesenchymal stem cells in patients with chronic
immune thrombocytopenia. Autoimmunity. 47:519–529. 2014.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Zhang JM, Feng FE, Wang QM, Zhu XL, Fu HX,
Xu LP, Liu KY, Huang XJ and Zhang XH: Platelet-derived growth
factor-BB protects mesenchymal stem cells (MSCs) derived from
immune thrombocytopenia patients against apoptosis and senescence
and maintains MSC-mediated immunosuppression. Stem Cells Transl
Med. 5:1631–1643. 2016.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Radwi M and Cserti-Gazdewich C:
Drug-induced immune thrombocytopenia associated with use of
tyrosine kinase inhibitor imatinib. J Taibah University Med Sci.
10:365–368. 2015.
|
|
15
|
Ansari Z and George MK: Drug-induced
immune-mediated thrombocytopenia secondary to sunitinib in a
patient with metastatic renal cell carcinoma: A case report. J Med
Case Rep. 7(54)2013.PubMed/NCBI View Article : Google Scholar
|