Introduction
Malignant pleural mesothelioma (MPM) is a locally
aggressive tumor with poor prognosis. It is mostly related to
asbestos exposure (1). Most
malignant mesothelioma can be categorized into three histological
subtypes: Epithelioid, sarcomatoid, or biphasic (mixed).
Sarcomatoid and biphasic subtypes have significantly poorer
prognosis and are less responsive to treatment overall (2). To diagnose MPM, the gold standard
procedure is video-assisted thoracic surgery (VATS) biopsy
(3).
Metastasis of a non-hematologic malignancy to the
bone marrow can induce various hematologic abnormalities, which may
be associated with poor prognosis. Metastasis to the bone marrow
most commonly arises from prostate, breast, and lung cancers and
neuroblastoma (4). In contrast,
bone marrow metastasis due to MPM is very rare (5).
Cellular cannibalism is defined as the ability of a
tumor cell to engulf another cell. Several studies have indicated
that this process promotes tumor cell survival under unfavorable
conditions (6). Although this type
of cell-cell interaction has been demonstrated in various
carcinomas, no report has described this phenomenon in a patient
with MPM before. Herein, we describe our experience with an
extremely rare case of MPM with bone marrow metastasis in which
thrombocytopenia was caused by cellular cannibalism.
Case report
A 77-year-old male smoker was referred to our
hospital due to hemothorax. He had a history of dyspnea and cough
20 days before this referral, and exacerbating right chest pain for
several days. He had worked previously as a machine tool
manufacturer and had a history of occupational asbestos exposure. A
blood test results revealed anemia and thrombocytopenia (hemoglobin
level: 6.6 g/dl, white blood cell count:
19.2x103/mm3, and platelet count:
1.9x104/mm3). A chest X-ray revealed
right-sided pleural effusion. Subsequently, a chest tube was
placed, and approximately 2,000 ml of light, bloody pleural
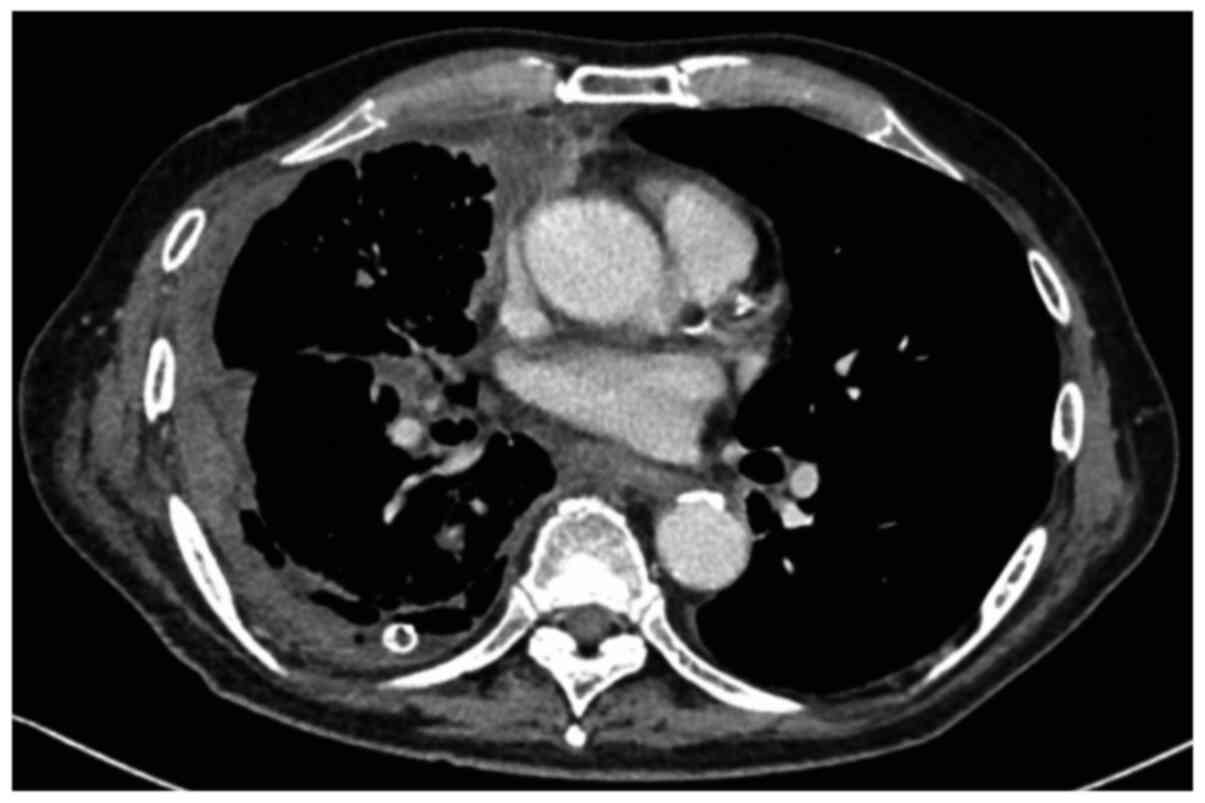
effusion was drained. A computed tomography (CT) scan performed
after tube thoracotomy revealed irregular thickening of the right
pleura (Fig. 1). We performed VATS
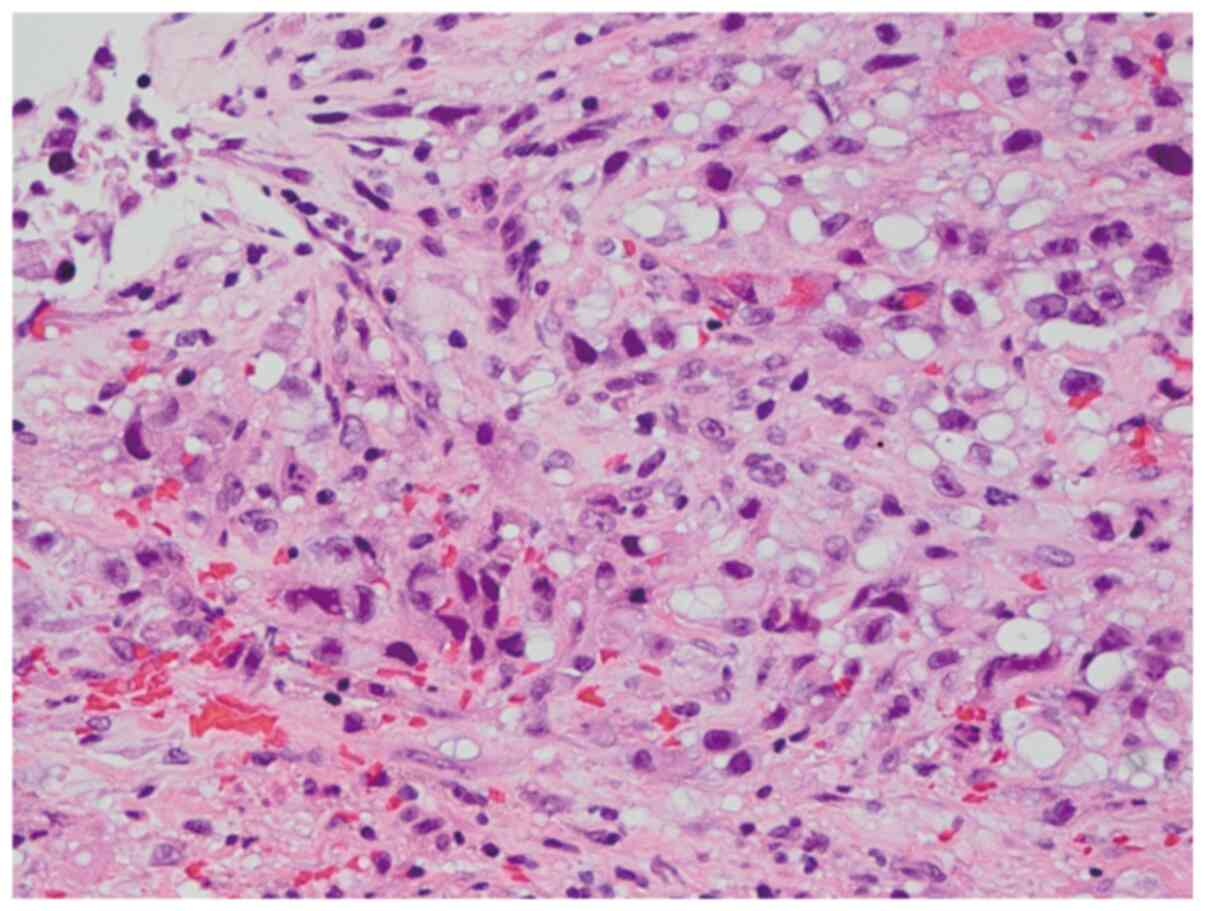
pleural biopsy, and its analysis suggested MPM, sarcomatoid cell
type. Histopathologically, this biopsy specimen contained spindle
tumor cells (Fig. 2), which were
positive for calretinin, D2-40, WT-1, and AE1/AE3 but negative for
S-100, CD34, α-smooth muscle actin, and desmin using an
immunohistochemical analysis.
Although the amount of drainage fluid decreased over
time and had become serous in appearance, the patient's platelet
count did not increase (1.0-3.0x104/mm3)
despite daily transfusions of 10-20 units of platelet concentrate.
In contrast, this patient did not have an abnormal prolonged
prothrombin time or activated partial thromboplastin time through
the whole course of this disease. Therefore, a bone marrow
aspiration was performed to examine the cause of thrombocytopenia.
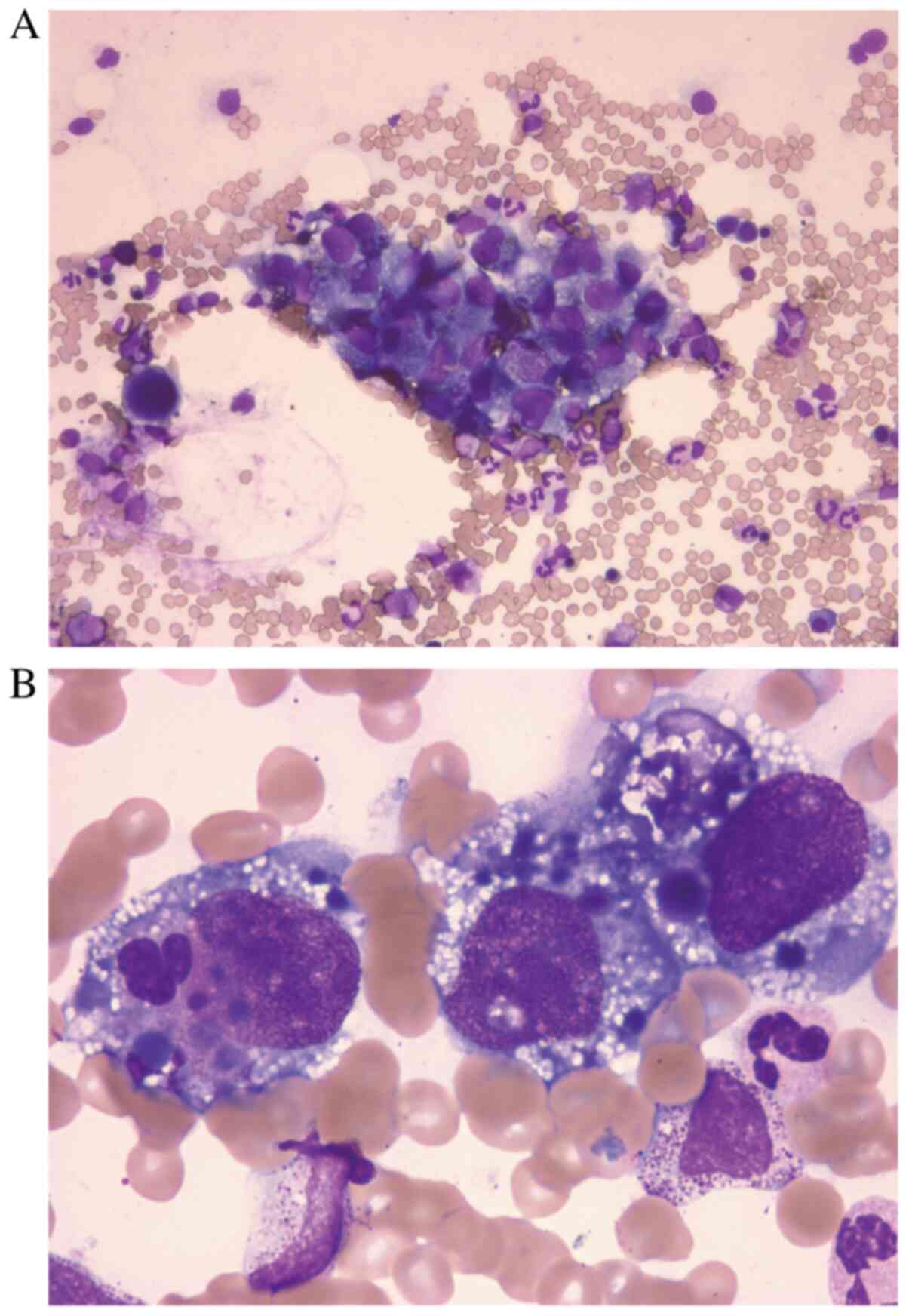
Aspirate smears revealed large, cohesive, and clustered atypical
cells present at a frequency of 2.2% (Fig. 3A). These atypical cells were
negative for esterase and peroxidase. In addition, some of these
atypical cells had engulfed other blood cells, indicating cellular
cannibalism (Fig. 3B).
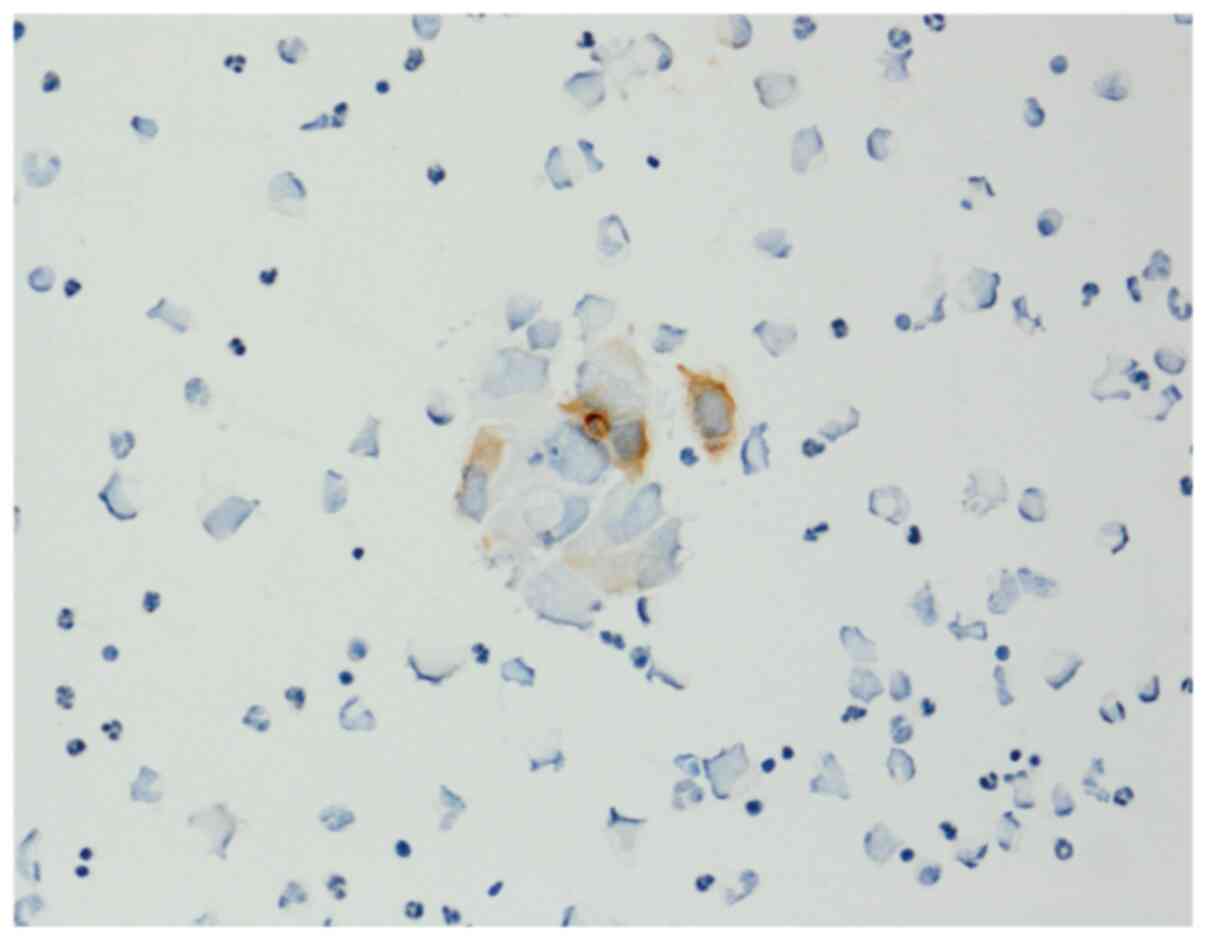
Immunohistochemical staining of this aspiration smear revealed
positivity for AE1/AE3 (Fig. 4).
Consequently, we established a final diagnosis of bone marrow
metastasis of MPM (stage IV) with thrombocytopenia due to cellular
cannibalism. The patient's disease progressed rapidly, and severe
back pain occurred. His consciousness was impaired and he died 11
days after admission.
Discussion
We experienced a rare case of MPM with bone marrow
metastasis in which thrombocytopenia occurred as a consequence of
cellular cannibalism. The interesting and novel findings of this
case include (i) the ability of MPM to metastasize to the bone
marrow and (ii) the ability of metastatic MPM cells to cause
thrombocytopenia due to cellular cannibalism.
MPM is generally considered a locally invasive
tumor, and bone marrow metastasis from MPM is considered an
extremely rare consequence (5). One
study of postmortem records of 318 patients with MPM revealed that
tumors were detected in extrathoracic organs in 55.4% of the cases,
and almost all organs were involved including the liver (31.9%),
spleen (10.8%), thyroid (6.9%), and brain (3.0%). Among those
cases, 13.8% of patients had bone metastasis, whereas no bone
marrow metastasis was detected (7).
In our case, a bone marrow aspiration sample revealed large,
cohesive, and clustered atypical cells that were negative for
esterase and peroxidase. In other words, these atypical cells
differed from bone marrow-derived cells. Immunohistochemically,
these atypical cells were positive for AE1/AE3, which strongly
suggested a bone marrow metastasis due to MPM, rather than
scavenging macrophage.
Although we were unable to confirm presence of other
MPM-specific markers such as calretinin, D2-40, or WT-1 due to
insufficient specimen volume, we definitively detected epithelial
marker expression. Consequently, a malignant tumor with an
epithelial component was present in the bone marrow of this
patient.
Of note, cellular cannibalism describes an ability
of one cell to engulf another living cell (8). This phenomenon is associated with poor
prognosis, and no effective treatment has been identified yet
(6). In vivo, this
phenomenon has been recognized in a wide range of carcinomas,
including breast, cervix, colon, stomach, liver, melanoma,
head-and-neck, and lung malignancies (9). To date, several studies have explored
potential triggers for cellular cannibalism. One in vitro
experiment clarified increased presence of cannibal cells in
metastatic sites relative to primary lesions. Moreover, these
cannibal cells were able to survive under unfavorable conditions,
such as serum starvation or acidity (6). These findings suggest that cellular
cannibalism may provide nutrients and thus enable cancer cells to
proliferate in metastatic organs that are intrinsically unfriendly
to cell survival. Molecular genetic mechanisms for cellular
cannibalistic activity are increasingly being revealed. Cellular
cannibalism could be associated with microenvironment that provokes
drug-resistance. Several studies of this phenomenon have indicated
the potential use of new target anti-tumor strategies (10-12).
In our case, we observed that atypical cells
engulfed other blood cells in the bone marrow. Nuclei collapse of
the apparent normal blood cells was observed indicating cellular
cannibalism. Unfortunately, we could not perform
immunohistochemical staining for apoptosis markers. However,
morphological features of tumor cells engulfing blood cells and
their nuclei collapse highly suggested this phenomenon of cellular
cannibalism. Because we detected no evidence of disseminated
intravascular coagulation (DIC) or other thrombocytopenic
disorders, we assumed that thrombocytopenia in this case was due to
cellular cannibalism caused by metastatic mesothelioma cells in the
bone marrow. Although few cases of thrombocytopenia due to cellular
cannibalism by metastatic cells in the bone marrow have been
reported (Table I) (13-16),
to the best of our knowledge, this is the first reported case
involving a bone marrow metastasis due to MPM.
 | Table IClinical features of
thrombocytopenia-inducing cellular cannibalism due to bone marrow
metastasis. |
Table I
Clinical features of
thrombocytopenia-inducing cellular cannibalism due to bone marrow
metastasis.
| Author (year) | Type of cancer | Age/sex | Clinical
features | Treatment | Outcome | (Refs.) |
|---|
| Falini et al
(1980) | Undifferentiated lung
carcinoma | 51/M | Anemia and
thrombocytopenia | Palliative care | Death (47 days after
admission) | (13) |
| Grier et al
(2011) | Uterine
carcinosarcoma | 72/F | Thrombocytopenia | Not available | Not available | (14) |
| Gonzalez-Molina et
al (2018) | Lung neuroendocrine
carcinoma | 61/F | Pancytopenia | Palliative care | Death (3 weeks after
diagnosis) | (15) |
| Kang et al
(2019) | Urinary bladder small
cell carcinoma | 66/M | Anemia and
thrombocytopenia | Palliative care | Death (intracerebral
hemorrhage, 1 day after diagnosis) | (16) |
In conclusion, we have presented a highly unusual
case. Further clarification of mechanisms underlying cellular
cannibalism by metastatic MPM cells in the bone marrow, with
consequent thrombocytopenia, may identify a promising target for
treatment of bone marrow metastasis. Moreover, these findings could
enable development of more rational and disease-specific strategies
for overcoming poor prognosis associated with MPM.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
MN, YK and KU performed the surgery and
perioperative management of the patient. KN and AM contributed to
acquisition and analysis of hematological data. YM and HS
contributed to acquisition and analysis of pathological data. MN,
YK and KU confirm the authenticity of all the raw data. MN, YK, ST,
WN and KU drafted the manuscript. ST supervised the manuscript
writing, editing and review. ST made a significant contribution to
interpretation of data. WN and KU designed and coordinated the
project and editing the manuscript. All authors read and approved
the final manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Written informed consent for the publication of any
associated data was obtained from the patient prior to his
death.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Robinson BW and Lake RA: Advances in
malignant mesothelioma. N Engl J Med. 353:1591–603. 2005.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Husain AN, Colby T, Ordonez N, Krausz T,
Attanoos R, Beasley MB, Borczuk AC, Butnor K, Cagle PT, Chirieac
LR, et al: Guidelines for pathologic diagnosis of malignant
mesothelioma: 2012 update of the consensus statement from the
International Mesothelioma Interest Group. Arch Pathol Lab Med.
137:647–667. 2013.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Boutin C and Rey F: Thoracoscopy in
pleural malignant mesothelioma: A prospective study of 188
consecutive patients. Part 1: Diagnosis. Cancer. 72:389–393.
1993.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Papac RJ: Bone marrow metastases. A
review. Cancer. 74:2403–2413. 1994.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Ihara H, Harada N, Shimada N, Kanamori K,
Hayashi T, Uekusa T and Takahashi K: Malignant pleural mesothelioma
with bone marrow metastases. Intern Med. 57:2541–2545.
2018.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Lugini L, Matarrese P, Tinari A, Lozupone
F, Federici C, Iessi E, Gentile M, Luciani F, Parmiani G, Rivoltini
L, et al: Cannibalism of live lymphocytes by human metastatic but
not primary melanoma cells. Cancer Res. 66:3629–3638.
2006.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Finn RS, Brims FJH, Gandhi A, Olsen N,
Musk AW, Maskell NA and Lee YCG: Postmortem findings of malignant
pleural mesothelioma: A two-center study of 318 patients. Chest.
142:1267–1273. 2012.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Gupta N, Jadhav K and Shah V:
Emperipolesis, entosis and cell cannibalism: Demystifying the
cloud. J Oral Maxillofac Pathol. 21:92–98. 2017.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Durgan J and Florey O: Cancer cell
cannibalism: Multiple triggers emerge for entosis. Biochim Biophys
Acta Mol Cell Res. 1865:831–841. 2018.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Lozupone F, Perdicchio M, Brambilla D,
Borghi M, Meschini S, Barca S, Marino ML, Logozzi M, Federici C,
Iessi E, et al: The human homologue of Dictyostelium discoideum
phg1A is expressed by human metastatic melanoma cells. EMBO Rep.
10:1348–1354. 2009.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Lozupone F, Borghi M, Marzoli F, Azzarito
T, Matarrese P, Iessi E, Venturi G, Meschini S, Canitano A, Bona R,
et al: TM9SF4 is a novel V-ATPase-interacting protein that
modulates tumor pH alterations associated with drug resistance and
invasiveness of colon cancer cells. Oncogene. 34:5163–5174.
2015.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Fais S and Overholtzer M: Cell-in-cell
phenomena in cancer. Nat Rev Cancer. 18:758–766. 2018.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Falini B, Bucciarelli E, Grignani F and
Martelli MF: Erythrophagocytosis by undifferentiated lung carcinoma
cells. Cancer. 46:1140–1145. 1980.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Grier DD, Anz BM and Sirintrapun SJ:
Hemophagocytic tumor cells in carcinosarcoma bone marrow
metastasis. Am J Hematol. 86(192)2011.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Gonzalez-Molina W, Avila-Polo R,
Morales-Camacho RM, Vargas MT, Bernal R and Prats-Martin C: Bone
marrow erythrocyte and neutrophil phagocytosis and cannibalism by
neuroendocrine carcinoma. Br J Haematol. 183(537)2018.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Kang H, Kim DH, Lee W, Ha J, Ryoo N, Jeon
DS and Jung HR: First case of cellular cannibalism in small-cell
carcinoma of the bladder detected in peripheral blood. Ann Lab Med.
39:400–402. 2009.PubMed/NCBI View Article : Google Scholar
|