Introduction
Hand-foot-syndrome (HFS), which was first reported in 1974(1), is a frequent adverse effect of numerous anti-tumor drugs including chemotherapeutic agents and targeted multi-kinase inhibitors. Especially, patients taking capecitabine therapy are most likely to suffer from HFS. Capecitabine is the first- or second-line treatment for multiple tumor types including gastric, breast and colorectal cancer. However, adjuvant chemotherapy with capecitabine is frequently not completed due to adverse events like as HFS. HFS, that reaches a moderate-to-severe condition (Grade 2 or more), not only impairs their quality of life but also requires discontinuation or postponement of the treatment. Therefore, HFS can affect their prognosis. The mechanism of the capecitabine-induced HFS remains unknown, and there are also no effective strategies to recover from the capecitabine-induced HFS except for its cessation. We here report a single case to help to disentangle the pathophysiological mechanism of the capecitabine-induced HFS.
Case report
A woman in her late 50s, who had received right breast cancer surgery three years before, gradually suffered severe pain and slight motor paralysis of the right upper limb with the brachial plexus infiltration due to the subclavian lymph node metastasis. She developed Complex-regional-pain-syndrome (CRPS; previously known as reflex sympathetic dystrophy) in the right hand, accompanied by edema and anhidrosis. Her CRPS was treated with opioids in combination with neural blockade and physiotherapy in our pain clinic. Soon after, her pain and CRPS-featured signs (i.e., edema, dark purple skin color change) improved, but slight allodynia, sensory loss, partial motor paralysis and hypohidrosis persisted. Then, she was treated with capecitabine (1,500 mg/day, suspended by HFS after 4 courses), which is widely used as the second-line breast cancer chemotherapy. Capecitabine-induced HFS, which are typically characterized as erythema, swelling, numbness, and desquamation, emerged in the distal portions of limbs (equivalent to grade 3) except for the CRPS-affected limb about 3 months after the start of capecitabine treatment. In the CRPS-affected limb, any of these HFS symptoms were not observed and tips of the fingers remained soft and normal (Fig. 1). During chemotherapy, sweat remained stopped in the CPRS-affected limb, and sweat in another hand was almost normal until the onset of HFS. HFS of the residual three limbs improved subsequent to cessation of capecitabin, and the CRPS-affected limb kept normal. Patient was provided with topical steroids.
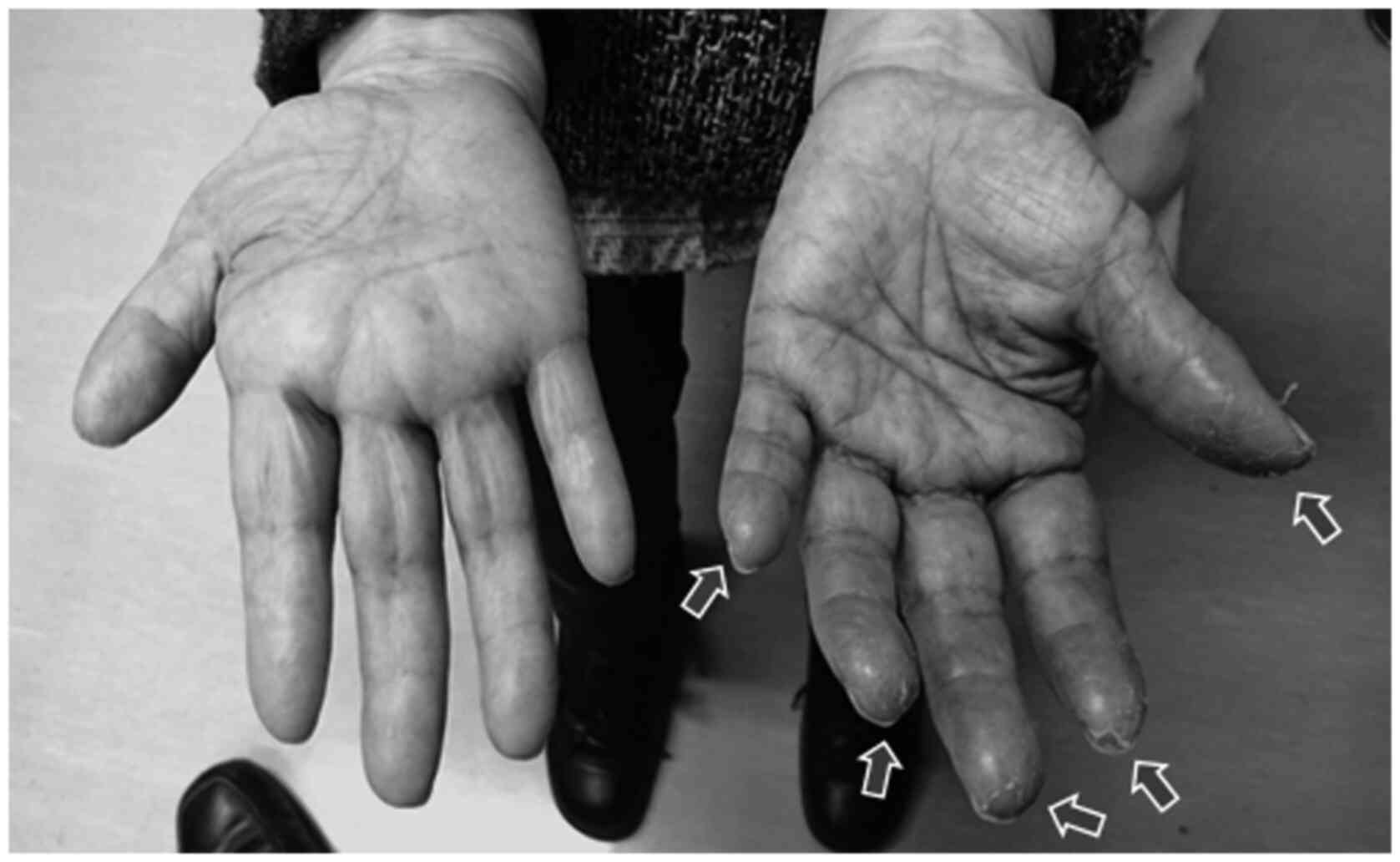 |
Figure 1
Unilateral hand-foot syndrome with capecitabine. The left hand (including both feet) demonstrated typical symptoms of hand-foot syndrome [numbness, pain, pigmentation, desquamation and cracks (arrows)]. These symptoms did not appear in the patient's right hand, which exhibited complex regional pain syndrome with anhidrosis.
|
Discussion
HFS, also known as palmar-plantar erythrodysesthesia, is one of complications, that occurs on the skin (especially the hands and feet) by anti-cancer drug treatments. The main symptoms of HFS begin with sensory abnormalities such as numbness and pain, erythema and swelling in the hands and feet, and subsequently pigmentation, desquamation, ulcers and cracks emerge. There are three levels (Grade 2, which indicates moderate level, affects activities of daily living) of clinical severity in HFS. When it becomes severe (Grade 3), HFS will cause serious problems in activities of daily living. HFS occurs with many chemotherapeutic agents (capecitabine, 5-fluorouracil, docetaxel, cytarabine, doxorubicin, liposomal doxorubicin, etc.) (2), but one of the highest incidences of HFS is capecitabine (e.g., up to 71% for capecitabine) (3). Capecitabine and multi-kinase inhibitors, all of which are approved in recent years, have a high incidence of HFS and thereby markedly affect patient's quality of life (QoL) and activities of daily living (with 17% of capecitabine patients are afflicted with a serious condition) (4). The pathophysiological mechanism of the capecitabine-induced HFS remains still unclear, and therefore causal therapeutic strategies to prevent and treat HFS have not yet been established. HFS becomes more frequent and serious with increased cumulative doses of capecitabine, indicating that HFS in capecitabine therapy represents a cumulative toxicity (5). Most guidelines recommend the dose reduction or deferred treatment, as key prevention and curable strategies (6). Because these recommendations require interruption or discontinuation of the treatment, a greater understanding of its prevention and causal treatment is necessary to improve prognosis of cancer patients receiving capecitabine. Following four mechanisms are mainly proposed as capecitabine-induced HFS. First, cytotoxicity is emerged by mitochondrial dysfunction following to activating the caspase-dependent apoptosis and consequently death of keratinocytes occurs (7). Second, its condensation and exocrine through eccrine sweat-glands, many of which especially locate in the hands and feet, directly induce local tissue injury (8). Third, local trauma to the small vessels due to the mechanical stress on fingertips by daily activities leads to leak capecitabine into the surrounding tissue, and then directly cause local tissue injury (9,10). And finally, the cyclooxygenase-2 (COX-2) overexpression in the tips of fingers by capecitabine might be a potential mediator (11,12).
CRPS is a syndrome in which pain, allodynia and sensory disturbance are usually sustained and mainly caused by trauma and/or nerve injury, with a prevalence of approximately 5.4-26.2 per 100 000 person years (13). In addition to these symptoms, the clinical features include (1) Atrophic change of skin and nails (i.e., keratosis skin thinning and crack) and also bones and muscles, (2) skin color change (redness and/or dark purple pale), (3) skin edema, and (4) hyperhidrosis or anhidrosis/hypohidrosis alternatively (14). The pathophysiological mechanism(s) of CRPS is not completely understood. CRPS is subdivided into two types: One is type 1 without overt nerve injury; and the other is type 2 with overt nerve injury. Because of pain and allodynia in the affected limb, CRPS patients tend to avoid the use of the affected limb.
Our patient was diagnosed as CRPS type 2, according to the clinical diagnostic criteria (15) presenting with continuous pain, skin ‘glittering’ atrophy, incomplete motor paralysis, edema and anhidrosis with overt brachial plexus injury by cancer infiltration. The patient demonstrated less movements of the affected upper limb, because of incomplete paralysis and pain deterioration following the movements. Such disuse of the affected limb might decrease mechanical stress on the affected hand and HFS might not be observed in this patient. Unilateral HFS cases resembling our case were previously reported (16-18). In each case, they are hemiplegic patients after cerebral stroke and developed HFS on the intact-sided hand and foot only. These cases might reinforce the mechanism that HFS develops from mechanical stress. Local trauma to the small vessels due to the mechanical stress on fingertips by daily activities and leakage of capecitabine from injured vessels is suggested as one of mechanisms of HFS. In our case, the CRPS-affected hand was her dominant hand, and moving the affected hand was still routinely executed. Further, the patient was treated with rehabilitation and exercise therapy of the affected hand, but HFS did not develop. Therefore, mechanical stress and small vessels injury would be apart from mechanisms of HFS. Alternatively, patients after stroke or spinal cord injury sometimes demonstrate CRPS-like manifestations, which include anhidrosis/hypohidrosis resembling our case. A local toxic effect of capecitabine is one of the pathomechanism of HFS. The accumulation and excretion through the sweat glands have been suspected to cause the cytotoxic effects on skin sites with increased density of sweat glands. Sweat samples taken one week after oral administration of capecitabine showed substantial increased concentration (19). Considering continuous presentation of anhidrosis/hypohidrosis by CRPS, among the suggested mechanisms of HFS, exocrine of condensed capecitabine through sweat glands would be a promising mechanism to induce HFS.
We here reported that anhidrosis of one hand, caused by the brachial plexus infiltration due to lymph node metastasis of breast cancer, could completely prevent the capecitabine-induced HFS. The patient's symptoms of the affected hand prior to starting capecitabine were not only pain and partial motor paralysis but also anhidrosis, edema and skin colour change, of which met the diagnostic criteria of CRPS. After improving most CRPS manifestations except for anhidrosis, other three hand and feet developed typical symptoms of the HFS, but the CRPS-affected hand did not present HFS and remained soft and normal. After cessation of capecitabine, HFS on the three extremities completely improved and the CRPS-affected hand kept normal. This indicates that exocrine of condensed capecitabine through sweat glands would be a promising mechanism to induce HFS.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Authors' contributions
RI and MS confirm the authenticity of all the raw data. RI obtained the data and wrote the manuscript. MS treated the patient and supervised RI. RI and MS conceived and designed the current study. HA, MK, TE and RT made substantial contributions to the analysis and interpretation of patient data and provided constructive but critical comments to RI. All authors read and approved the final manuscript.
Ethics approval and consent to participate
The University of Tokyo, Clinical Research Review Board approved the report of this case [approval no. 3905-(5)]. Written informed consent was obtained from the case for the current report.
Patient consent for publication
The participant's written consent for the publication of the present case report was obtained. All accompanying images were anonymised.
Competing interests
The authors declare that there are no competing interests.
References
|
1
|
Zuehlke RL: Erythematous eruption of the palms and soles associated with mitotane therapy. Dermatologica. 148:90–92. 1974.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Miller KK, Gorcey L and McLellan BN: Chemotherapy-induced hand-foot syndrome and nail changes: A review of clinical presentation, etiology, pathogenesis, and management. J Am Acad Dermatol. 71:787–794. 2014.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Twelves C, Wong A, Nowacki MP, Abt M, Burris H III, Carrato A, Cassidy J, Cervantes A, Fagerberg J, Georgoulias V, et al: Capecitabine as adjuvant treatment for stage III colon cancer. N Engl J Med. 352:2696–2704. 2005.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Heo YS, Chang HM, Kim TW, Ryu MH, Ahn JH, Kim SB, Lee JS, Kim WK, Cho HK and Kang YK: Hand-foot syndrome in patients treated with capecitabine-containing combination chemotherapy. J Clin Pharmacol. 44:1166–1172. 2004.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Yokokawa T, Kawakami K, Mae Y, Sugita K, Watanabe H, Suzuki K, Suenaga M, Mizunuma N, Yamaguchi T and Hama T: Risk factors exacerbating hand-foot skin reaction induced by capecitabine plus oxaliplatin with or without bevacizumab therapy. Ann Pharmacother. 49:1120–1124. 2015.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Macedo LT, Lima JP, dos Santos LV and Sasse AD: Prevention strategies for chemotherapy-induced hand-foot syndrome: A systematic review and meta-analysis of prospective randomized trials. Support Care Cancer. 22:1585–1593. 2014.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Chen M, Chen J, Peng X, Xu Z, Shao J, Zhu Y, Li G, Zhu H, Yang B, Luo P and He Q: The contribution of keratinocytes in capecitabine-stimulated hand-foot-syndrome. Environ Toxicol Pharmacol. 49:81–88. 2017.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Martschick A, Sehouli J, Patzelt A, Richter H, Jacobi U, Oskay-Ozcelik G, Sterry W and Lademann J: The pathogenetic mechanism of anthracycline-induced palmar-plantar erythrodysesthesia. Anticancer Res. 29:2307–2313. 2009.PubMed/NCBI
|
|
9
|
Saif MW, Elfiky A and Diasio R: Hand-foot syndrome variant in a dihydropyrimidine dehydrogenase-deficient patient treated with capecitabine. Clin Colorectal Cancer. 6:219–223. 2006.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Hoesly FJ, Baker SG, Gunawardane ND and Cotliar JA: Capecitabine-induced hand-foot syndrome complicated by pseudomonal superinfection resulting in bacterial sepsis and death: Case report and review of the literature. Arch Dermatol. 147:1418–1423. 2011.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Lin E, Morris JS and Ayers GD: Effect of celecoxib on capecitabine-induced hand-foot syndrome and antitumor activity. Oncology (Williston Park). 16 (Suppl 14):S31–S37. 2002.PubMed/NCBI
|
|
12
|
Zhang RX, Wu XJ, Wan DS, Lu ZH, Kong LH, Pan ZZ and Chen G: Celecoxib can prevent capecitabine-related hand-foot syndrome in stage II and III colorectal cancer patients: Result of a single-center, prospective randomized phase III trial. Ann Oncol. 23:1348–1353. 2012.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Petersen PB, Mikkelsen KL, Lauritzen JB and Krogsgaard MR: Risk factors for post-treatment complex regional pain syndrome (CRPS): An analysis of 647 cases of CRPS from the Danish patient compensation association. Pain Pract. 18:341–349. 2018.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Galer BS, Bruehl S and Harden RN: IASP diagnostic criteria for complex regional pain syndrome: A preliminary empirical validation study. International association for the study of pain. Clin J Pain. 14:48–54. 1998.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Sumitani M, Shibata M, Sakaue G and Mashimo M: Japanese CRPS Research Group. Development of comprehensive diagnostic criteria for complex regional pain syndrome in the Japanese population. Pain. 150:243–249. 2010.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Almeida da Cruz L, Hoff PM, Ferrari CL and Riechelmann RS: Unilateral hand-foot syndrome: Does it take sides? Case report and literature review. Clin Colorectal Cancer. 11:82–84. 2012.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Disel U, Gürkut O, Abali H, Kaleağasi H, Mertsoylu H, Ozyilkan O and Saif MW: Unilateral hand-foot syndrome: An extraordinary side effect of capecitabine. Cutan Ocul Toxicol. 29:140–142. 2010.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Matsuda S, Koketsu H, Hayakawa M and Nagata N: Unilateral capecitabine-related hand-foot syndrome. Intern Med. 54(2779)2015.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Huang MD, Fuss H, Lademann J, Florek S, Patzelt A, Meinke MC and Jung S: Detection of capecitabine (Xeloda®) on the skin surface after oral administration. J Biomed Opt. 21(47002)2016.PubMed/NCBI View Article : Google Scholar
|















