Spandidos Publications style
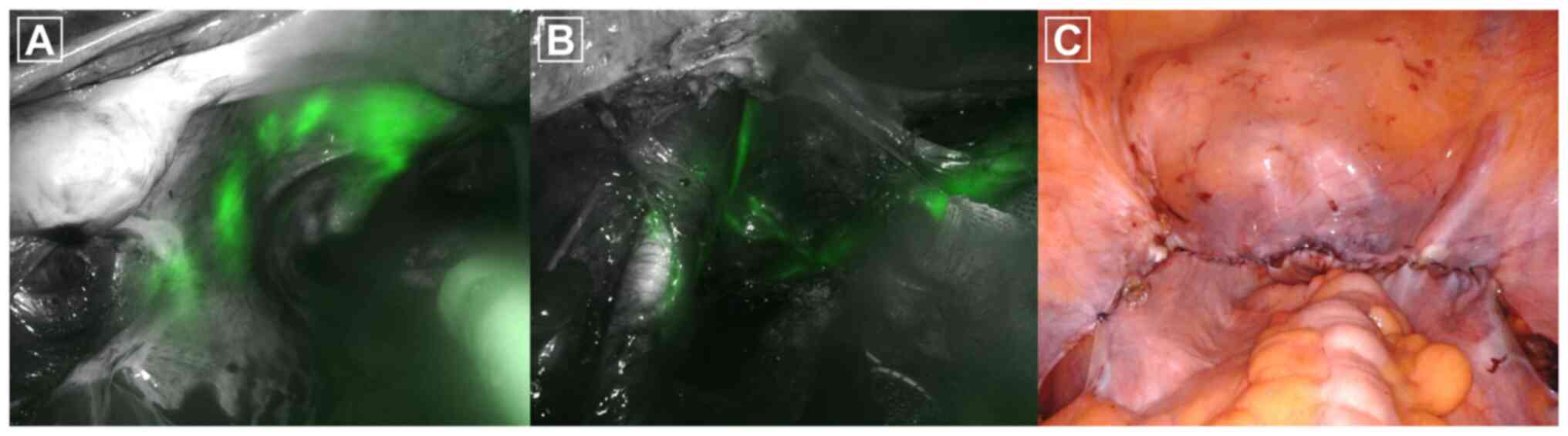
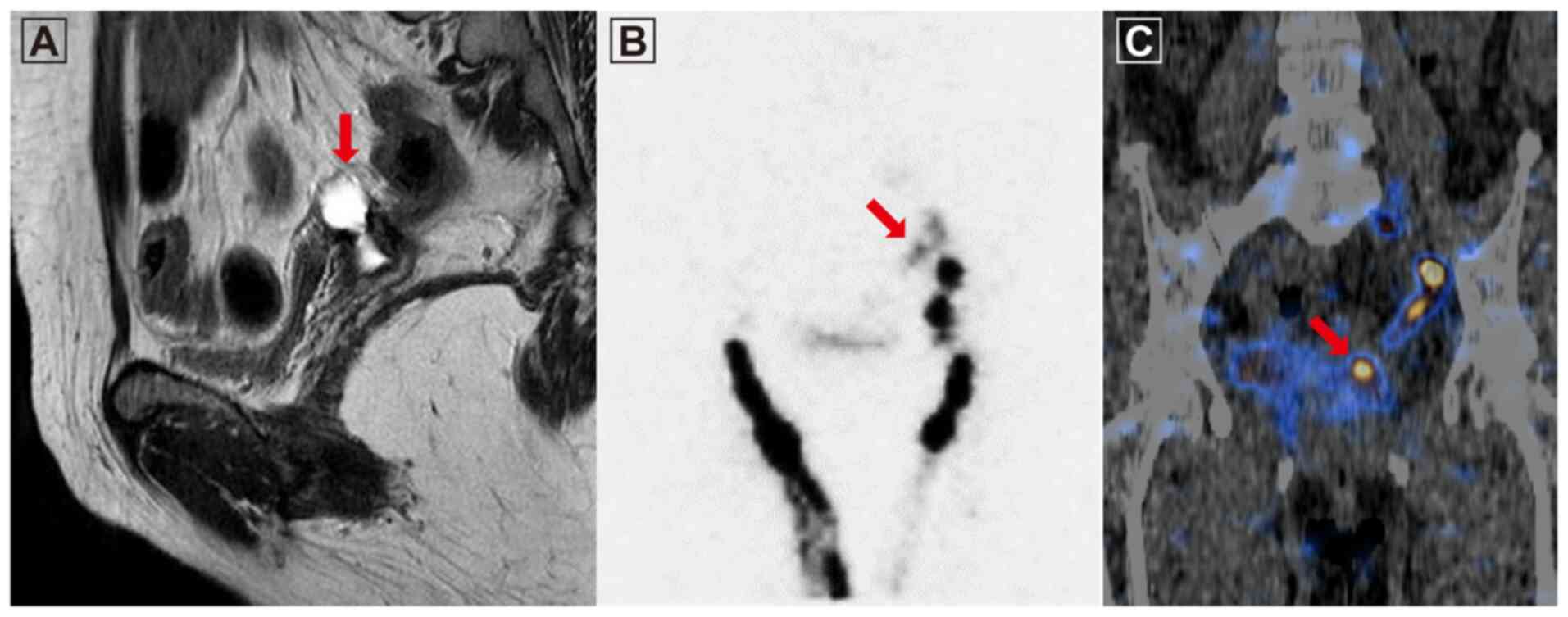
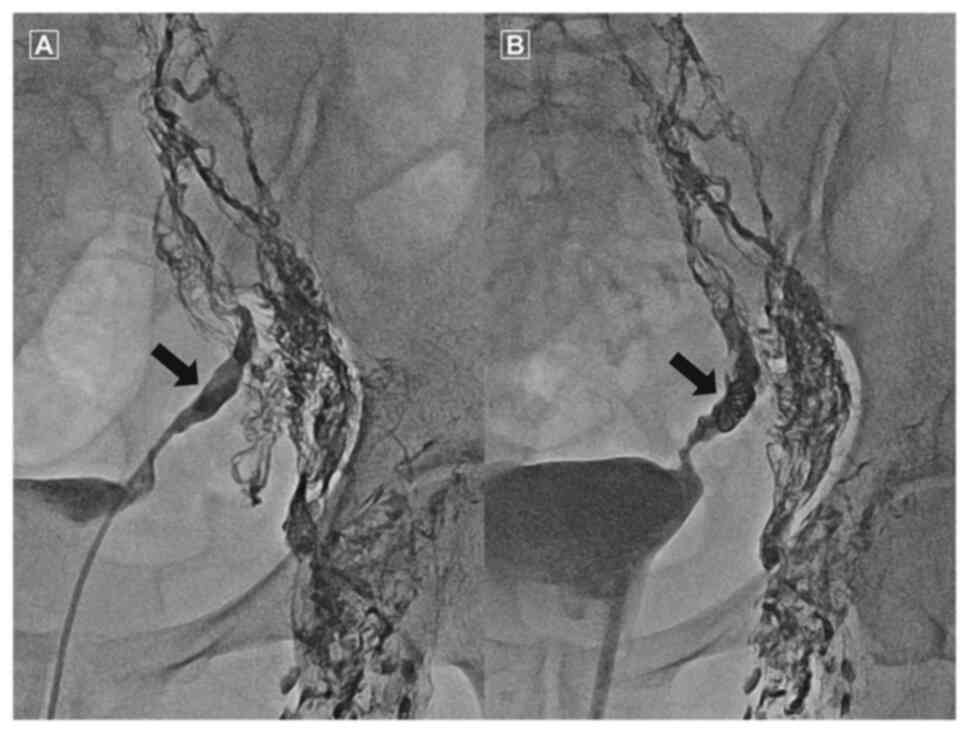
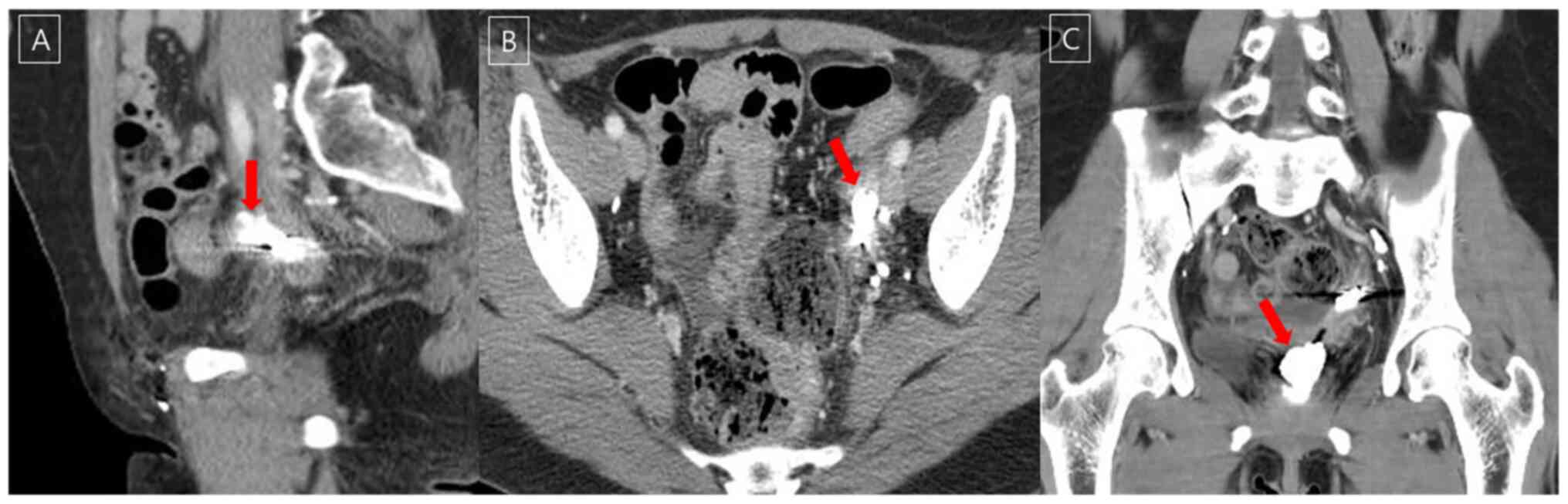
Lee YJ, Lee IJ, Park S, Kim T and Lim MC: Transvaginal lymphatic embolization of the fistula between a pelvic lymphocele and the vaginal stump following radical hysterectomy and sentinel pelvic lymph node biopsy in a patient with cervical cancer: A case report. Mol Clin Oncol 16: 49, 2022.
APA
Lee, Y.J., Lee, I.J., Park, S., Kim, T., & Lim, M.C. (2022). Transvaginal lymphatic embolization of the fistula between a pelvic lymphocele and the vaginal stump following radical hysterectomy and sentinel pelvic lymph node biopsy in a patient with cervical cancer: A case report. Molecular and Clinical Oncology, 16, 49. https://doi.org/10.3892/mco.2021.2482
MLA
Lee, Y. J., Lee, I. J., Park, S., Kim, T., Lim, M. C."Transvaginal lymphatic embolization of the fistula between a pelvic lymphocele and the vaginal stump following radical hysterectomy and sentinel pelvic lymph node biopsy in a patient with cervical cancer: A case report". Molecular and Clinical Oncology 16.2 (2022): 49.
Chicago
Lee, Y. J., Lee, I. J., Park, S., Kim, T., Lim, M. C."Transvaginal lymphatic embolization of the fistula between a pelvic lymphocele and the vaginal stump following radical hysterectomy and sentinel pelvic lymph node biopsy in a patient with cervical cancer: A case report". Molecular and Clinical Oncology 16, no. 2 (2022): 49. https://doi.org/10.3892/mco.2021.2482