Introduction
Gastric cancer (GC) is a prevalent disease globally,
affecting both men and women, with ~990,000 new cases diagnosed
annually, and it is also responsible for 738,000 deaths per year,
making it the third or fourth leading cause of mortality (1-3).
The incidence rates of GC vary according to the sex of the patient
and country, with men being three times more likely to contract the
disease compared with women (1,2).
Developing countries account for ~half of the new cases of GC, with
the highest rates reported in Central and South America, Eastern
Europe and East Asia (China and Japan), and the lowest rates
reported in Australia and New Zealand, Southern Asia, North and
East Africa, North America and Canada (1,4).
In recent decades, an overall decline in the
incidence rate of GC in the majority of countries in the world has
been reported (5). However,
although the incidence of sporadic intestinal GC has decreased, the
incidence of diffuse GC has increased (6,7). The
likelihood of developing GC is influenced by various factors,
including genetics, nutrition, alcohol consumption and smoking,
Helicobacter pylori (H. pylori) infection and
Epstein-Barr virus infection (1).
In the United States, GC constitutes ~1.5% of newly
diagnosed cancer cases annually (8). According to the American Cancer
Society, 26,380 new cases of GC would be diagnosed in 2022, with
15,900 cases in men and 10,480 cases in women, whereas the disease
was anticipated to result in 11,010 deaths, including 6,690 men and
4,400 women (8). Furthermore, the
International Agency for Research on Cancer (IARC) predicted that,
in 2020, the age-standardized incidence rate (ASIR) of GC in Saudi
Arabia would be 2.7 per 100,000 individuals for all ages and sexes,
ranking the nation 15th, whereas the age-standardized mortality
rate (ASMR) would be 2.1 per 100,000 individuals, being ranked
12th. Furthermore, the ASIRs of GC were considerably lower in Saudi
Arabia and Kuwait compared with other Arabian Gulf countries. In
2020, Oman, Qatar, Bahrain and the United Arab Emirates had a
higher reported ASIR for all ages and sexes, with rates of 8.0,
5.2, 4.8 and 4.4, per 100,000 individuals, respectively (9).
The main aim of the present retrospective study was
to assess the incidence of GC in the Saudi population through
analyzing the crude incidence rate (CIR) and ASIR, which were
further classified according the year of diagnosis, age group and
geographical region. To achieve this objective, an observational
descriptive epidemiological investigation of GC was performed,
considering the temporal and regional distribution of cases
recorded in the Saudi Cancer Registry (SCR) between 2004 and
2017.
Materials and methods
Study population
The objective of the present study was to perform a
retrospective observational descriptive epidemiological analysis of
all cases of GC identified in all regions of Saudi Arabia between
January 2004 and December 2017. Owing to the easy accessibility of
GC incidence data in Saudi Arabia through SCR reports, this
observational descriptive epidemiological study did not require
ethical approval. The Saudi Ministry of Health initiated a
population-based cancer registry in 1992, and its records were used
as the foundation for this investigation. The first report on
cancer in Saudi Arabia was released in 2001, and the most precise
cancer reports in Saudi Arabia were published at the beginning of
2004. Moreover, the most current information available from the SCR
was gathered in 2017.
Since 2001, SCR has been releasing reports on cancer
patterns in Saudi Arabia to describe the spread of the disease.
These reports have provided detailed information on the CIRs and
ASIRs, adjusted according to the province in Saudi Arabia, the sex
of the patient and year of diagnosis for 13 administrative regions
between 2004 and 2017(10).
Statistical analysis
The present study employed SPSS version 20.0 (IBM
Corp.) to analyse the data, calculating overall percentages, CIRs
and ASIRs stratified by the sex of the patients, geographical
region and year of diagnosis. The present study used independent
sample t-tests to compare the CIRs and ASIRs of GC between male and
female Saudis. P<0.05 was considered to indicate a statistically
significant difference. Furthermore, the Kruskal-Wallis test was
performed to analyse the CIRs and ASIRs of GC across different
regions of Saudi Arabia. The Dunn post hoc test, often referred to
as the Dunn's test, is a statistical method used in the analysis of
variance (ANOVA) and non-parametric statistics. It is used to
compare multiple pairs of groups when you have identified a
significant difference in a one-way ANOVA or a Kruskal-Wallis test.
The primary purpose of the Dunn post hoc test is to determine which
specific group differences are statistically significant after an
overall significant result in the ANOVA or Kruskal-Wallis test.
Finally, the sex ratio for GC from the age-specific
incidence rates, CIRs and ASIRs were also computed for the present
study.
Data on the trend of GC in the USA from 2004 to 2019
was sourced from the American Cancer Society (https://cancerstatisticscenter.cancer.org/). This was
conducted to compare the GC trend between Saudi Arabia and the USA,
and to determine whether it was on an upward or downward
trajectory. In addition, the age-standardized incidence and
mortality rates of GC for both sexes across all age groups in 2020
were sourced from GLOBOCAN (IARC) (https://gco.iarc.fr/today/home. These data were used
to compare the incidence of GC between different countries
including Saudi Arabia and to identify which countries had the
highest and lowest rates of GC.
Results
GC among Saudi men
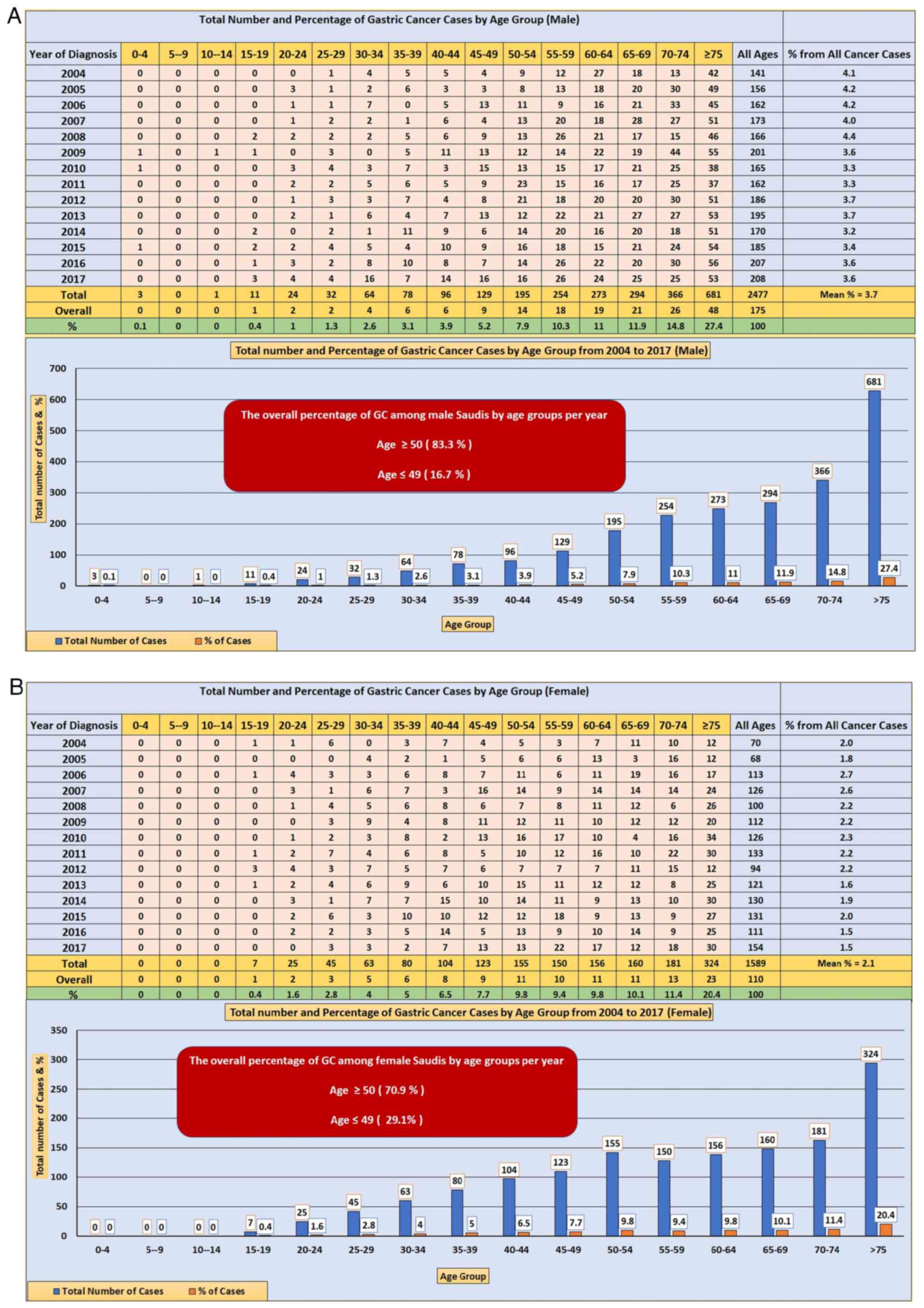
The data revealed the incidence of cases of GC in
Saudi Arabia between January 2004 and December 2017. A total of
2,477 cases of GC were reported during this period, accounting for
an average of 3.7% of all cancer cases. The number of cases ranged
from 141 in 2004 to 208 in 2017, with the corresponding percentages
ranging from 4.1 to 3.6% of all cancer cases during the respective
years. The ASIR for GC demonstrated fluctuations over time,
reaching a peak of 4.4% in 2008 and a low of 3.2% in 2014. The
average number of people suffering from GC was 175 per year.
Interestingly, there was no significant increase or decrease
observed in the incidence of GC during this period, indicating a
stable trend in its occurrence (Fig.
1A).
The mean numbers and percentages of cases of GC in
Saudi Arabian males, divided by the age group, were calculated
using data from the SCR between January 2004 and December 2017. Age
groups were classified using a 5-year class width for those aged
0-4, 5-9, 10-14, 15-19, 20-24 years, and so on, up to ≥75 years old
(the oldest age group). During the study period, GC was frequently
diagnosed in males aged ≥75 years, followed by those aged 70-74
years, accounting for 27.4% of the total (48 overall cases
annually) and 14.8% (26 overall cases annually), respectively.
Nonetheless, the overall percentage of Saudi men aged ≥50 who were
diagnosed with GC was 83.3% between 2004 and 2017. On the other
hand, younger male age groups (0-49 years) had the lowest
occurrences of GC, with an overall proportion of 16.7% (Fig. 1A). Furthermore, there was a high
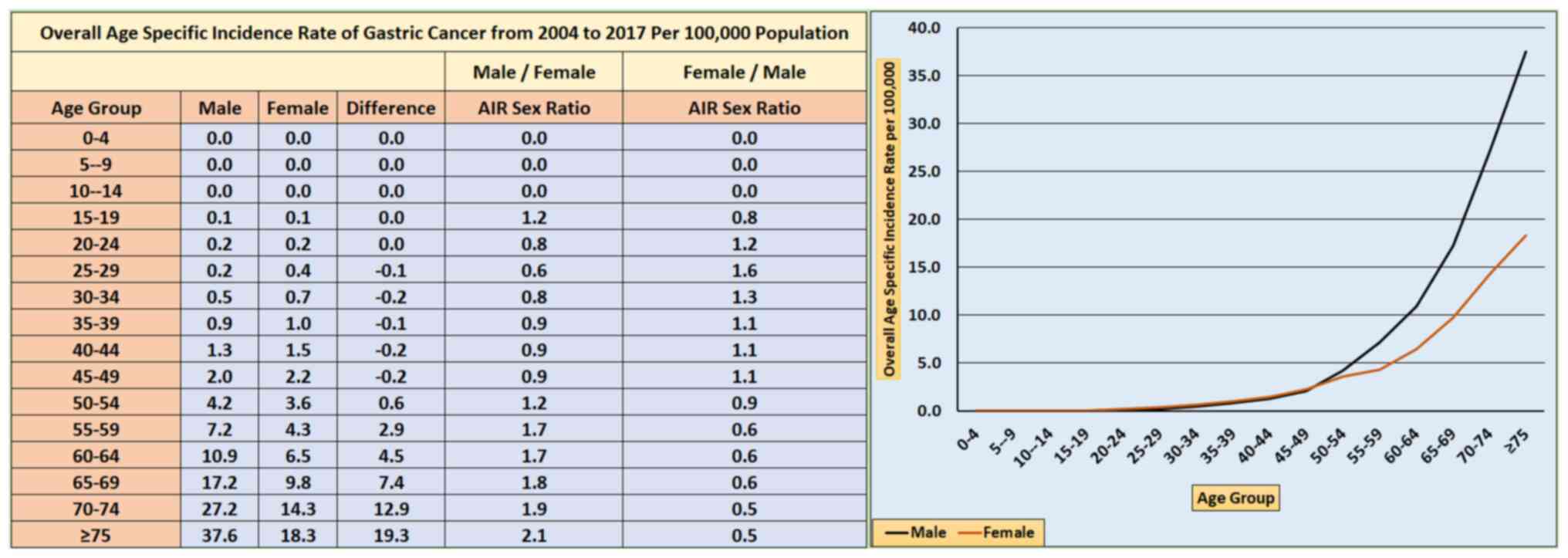
overall age-specific incidence rate of GC among male Saudis. The
average of incidence rate of GC within each age group from 2004 to
2017 showed notable peaks within specific age groups, particularly
among individuals aged ≥75 years, 70-74, 65-69 and 60-64, with
rates of 37.6, 27.2, 17.2 and 10.9 per 100,000 individuals,
respectively. Among Saudi males between the ages of 55 and 64, a
male-to-female ratio for the age-specific incidence rate was
identified that was 2.9 times higher compared with that of females.
Additionally, among Saudi males aged 65-75 years and older, the
overall male-to-female ratio of the age-specific incidence rate for
GC was 3.6 times greater compared with that of females (Fig. 2). Nevertheless, it is important to
note that no significant differences were identified in the
age-specific incidence sex ratio for the 0-54-year age group
(Fig. 2).
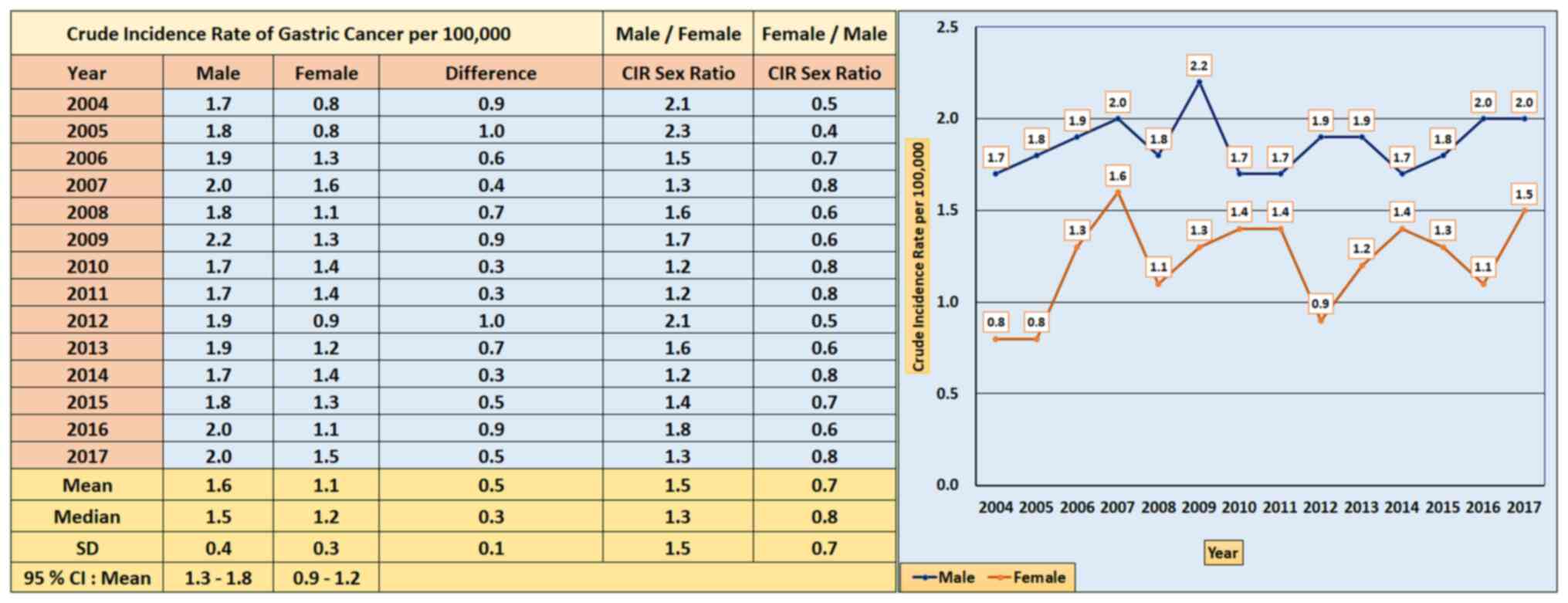
As illustrated in Fig.
3, there was a slight increase in the CIR of cases of GC among
Saudi men between 2004 and 2009, followed by a slight decline from
2009 to 2011, and then a stable trend from 2012-2017. The highest
CIR was reported in 2009 at 2.2 per 100,000 individuals, and the
estimated CIR for 2004 was 1.7 per 100,000 individuals. The overall
CIR of GC among Saudi men between 2004 and 2017 was 1.6 per 100,000
individuals, with a 95% confidence interval (95% CI) of 1.3-1.8.
The t-test for two independent samples indicated that the CIR of GC
in male Saudis was significantly higher compared with females
[t(23)=3.823; P<0.001; data
not shown]. However, the male-to-female overall CIR ratio between
2004 and 2017 per 100,000 individuals was found to be 1.5. The
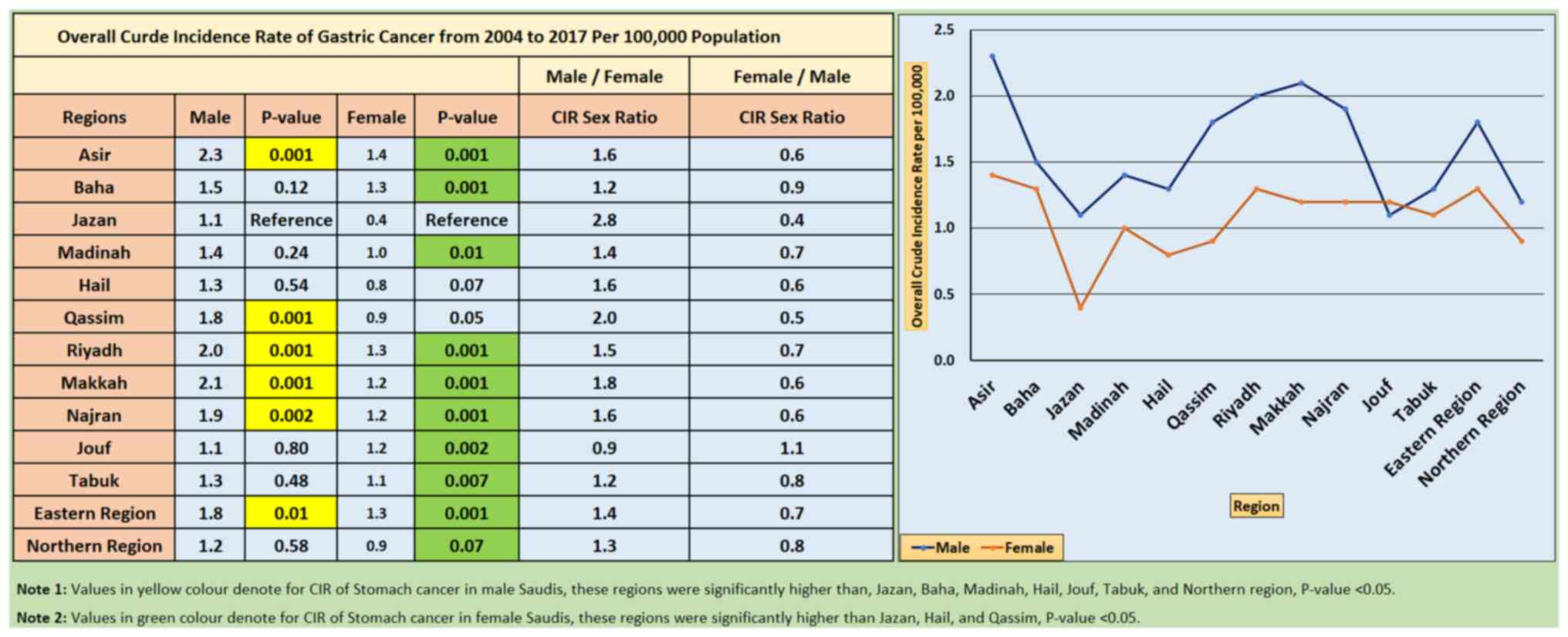
average incidence rate of GC within each region from 2004 to 2017
revealed that the highest overall CIRs for GC among Saudi men were
reported in the regions of Asir, Makkah and Riyadh, at 2.3, 2.1 and
2.0 per 100,000 individuals, respectively. The application of the
Dunn post hoc test in conjunction with the Kruskal-Wallis test
showed that these regions were significantly different compared
with the reference region of Jazan [2(12, N=181)=52.298;
P<0.001; data not shown]. Conversely, the smallest overall CIRs
of GC were reported in the Jazan and Jouf regions, at 1.1 per
100,000 individuals (Fig. 4).
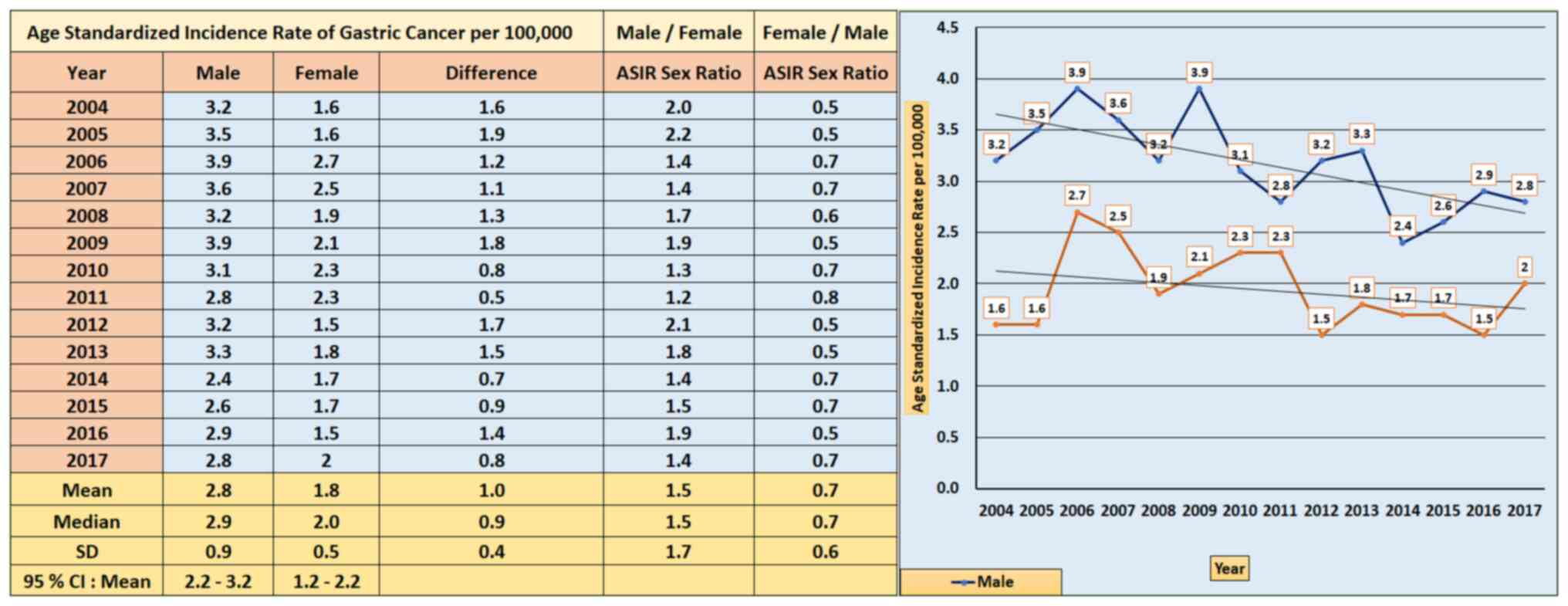
The SCR was subsequently used to determine the ASIRs
of cases of GC among male Saudis, adjusted for the year of
diagnosis between 2004 and 2017 per 100,000 individuals (Fig. 5). The results obtained exhibited a
slight increase between 2004 and 2009, followed by a steady
decrease from 2010-2017. The ASIR of GC was found to be highest in
2006 and 2009 (3.9 per 100,000 individuals), although it decreased
to its lowest rate of 2.4 per 100,000 individuals in 2014. However,
the overall ASIR of GC among Saudi males per 100,000 individuals
between 2004 and 2017 was 2.8 (95% CI; 2.2-3.2). A t-test for two
independent samples indicated that the ASIR of GC in Saudi males
was significantly higher compared with that in females [t(20)=8.823; P<0.001; data not shown].
However, between 2004 and 2017, the overall male-to-female ratio of
ASIR per 100,000 males was 1.5.
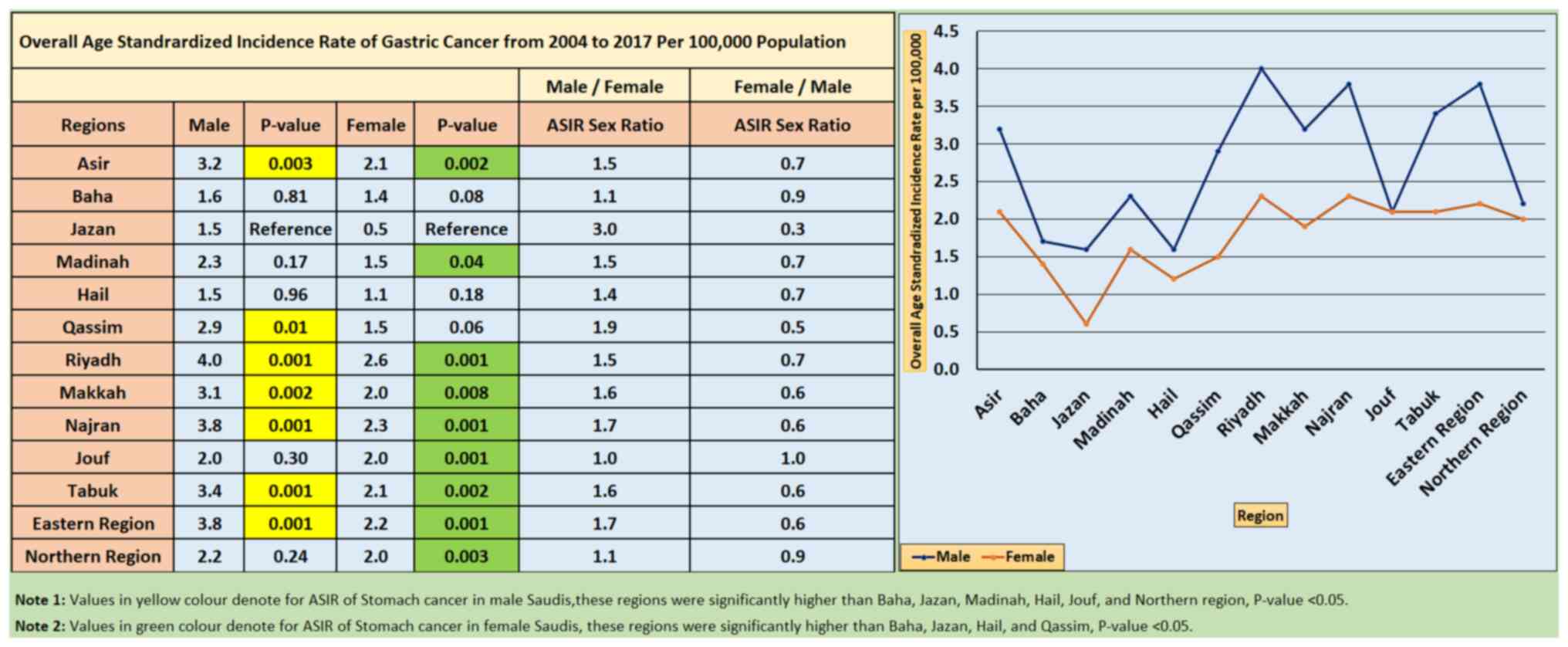
As shown in Fig. 6,
Riyadh, Najran and the Eastern region of Saudi Arabia had the
highest overall ASIRs for GC, with rates of 4.0, 3.8 and 3.8 per
100,000 individuals, respectively. The Kruskal-Wallis test revealed
significant differences among these regions, with the reference
region of Jazan [2(12,N=180)=59.556; P<0.001; data not shown].
By contrast, Jazan, Hail and Baha were the regions that had the
lowest overall ASIRs of GC, with rates of 1.6, 1.5 and 1.5,
respectively.
GC among Saudis women
Between January 2004 and December 2017, a total of
1,589 cases of GC were recorded among Saudi women, accounting for
7.1% of the total diagnosed cancer cases per year. The number of
cases of GC was found to fluctuate over the years, with 70 cases
(2% of all cancer cases) recorded in 2004, and a peak of 133 cases
(2.2% of all cancer cases) in 2011. Between 2012 and 2017, the
number of cases of GC ranged from 186 and 208 per year,
representing a percentage range of 7.5-8.4% per year (Fig. 1B). Among Saudi women, GC was most
commonly diagnosed in those aged ≥75 years, with 23 overall cases
per year (20.4%), followed by those aged 70-74 years, with 13
overall cases per year (11.1%). By contrast, younger females aged
0-49 years were associated with the lowest overall number of cases
of GC, with an average of 29.1% per year. The overall percentage of
women aged 50 years or older diagnosed with GC between 2004 and
2017 was 70.9%. The age-specific incidence rate of GC among Saudi
women was highest in those aged ≥75 years (18.3 per 100,000
individuals), followed by those aged 70-74 (14.3 per 100,000
individuals), 65-69 (9.8 per 100,000 individuals) and 60-64 (6.5
per 100,000 individuals) (Fig.
2).
As shown in Fig. 3,
the CIRs of cases of GC among females in Saudi Arabia, adjusted
according to the year of diagnosis from 2004 to 2017, per 100,000
individuals demonstrated a modest increase between 2004 and 2007, a
small reduction from 2008 to 2012, and a steady trend over the
years 2013-2017. The estimated CIR for 2004 was 0.8 per 100,000
individuals, and the highest CIR reported by the SCR was 1.7 per
100,000 individuals in 2007. Furthermore, the overall CIR of GC
among Saudi women between 2004 and 2017 was 1.1 (95% CI, 0.9-1.2)
per 100,000 individuals. The regions of Asir, Riyadh and the
Eastern region had the highest overall CIRs for GC among Saudi
women, with CIR values identified of 1.4, 1.3 and 1.3,
respectively, per 100,000 individuals. The Kruskal-Wallis test
revealed significant differences between these locations and other
regions of Saudi Arabia [χ2 (12, N=181)=39.689;
P<0.001; data not shown]. By contrast, the region of Jazan had
the lowest overall CIR of GC, at 0.4 per 100,000 individuals
(Fig. 4).
The ASIRs of cases of GC among Saudi women, adjusted
according to the year of diagnosis between 2004 and 2017, were
documented using the SCR (Fig. 5).
Between 2004 and 2006, a modest rise was observed, followed by a
constant trend between 2007 and 2017. In 2006, the ASIR of GC was
the highest at 2.7 per 100,000 individuals; by contrast, in 2012
and 2016, it was the lowest, at 1.5 per 100,000 individuals.
However, the overall ASIR of GC among Saudi women between 2004 and
2017 per 100,000 individuals was 1.8 (95% CI, 1.2-2.2).
Furthermore, the overall ASIR of GC stratified according to the
Saudi Arabian region between 2004 and 2017 per 100,000 individuals
showed that Riyadh, Najran and the Eastern region of Saudi Arabia
had the highest overall ASIR for GC at 2.6, 2.3, and 2.2 per
100,000 individuals, respectively. By contrast, the Jazan region
had the lowest overall ASIR of GC, at 0.5 per 100,000 individuals
(Fig. 6).
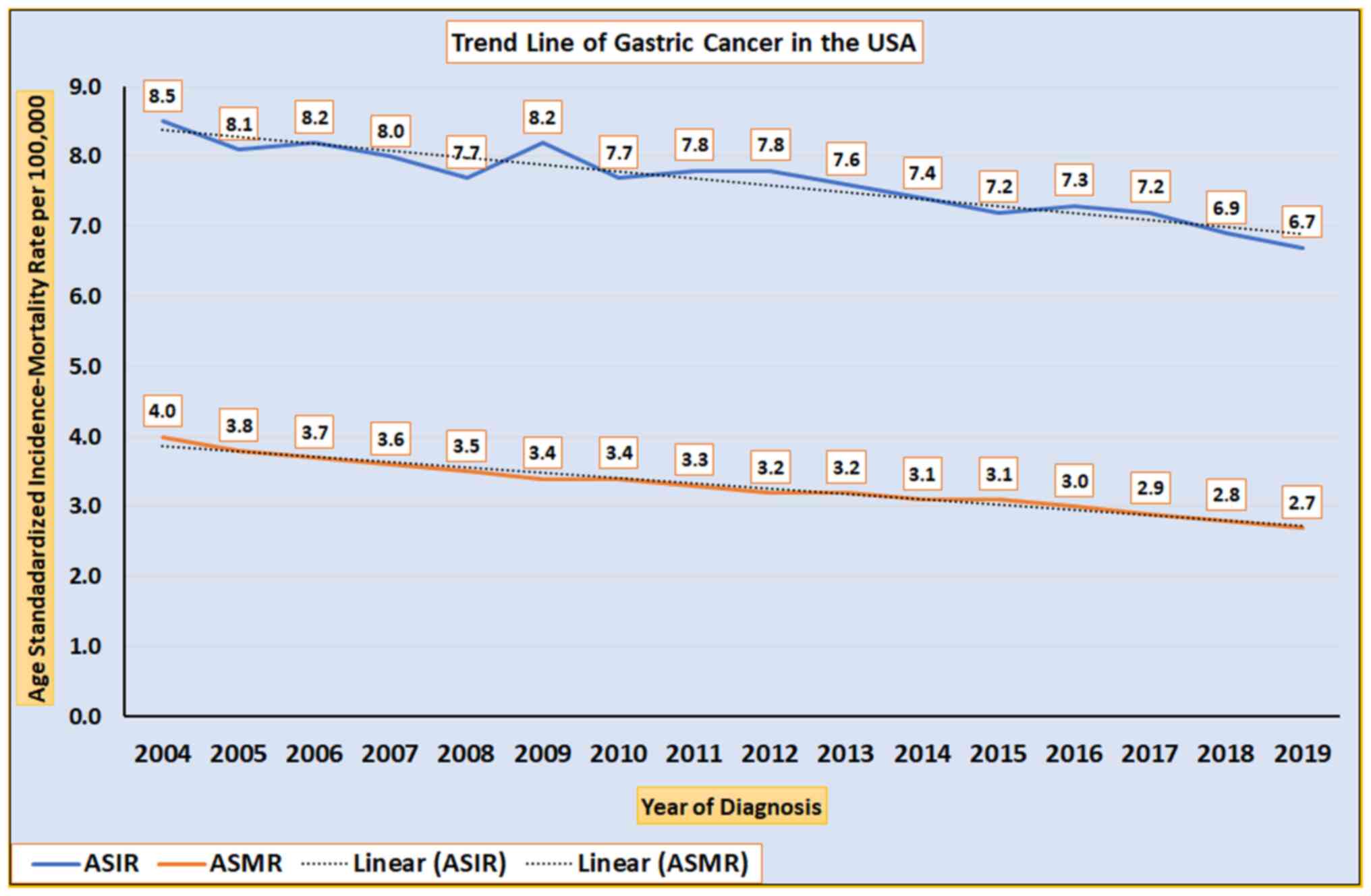
A consistent decline in the ASIR trend of GC for
both the American and Saudi populations from 2004 to 2017 is
illustrated in Fig. 7. The ASIR of
GC in Saudi Arabia stood at 2.7 per 100,000 individuals for both
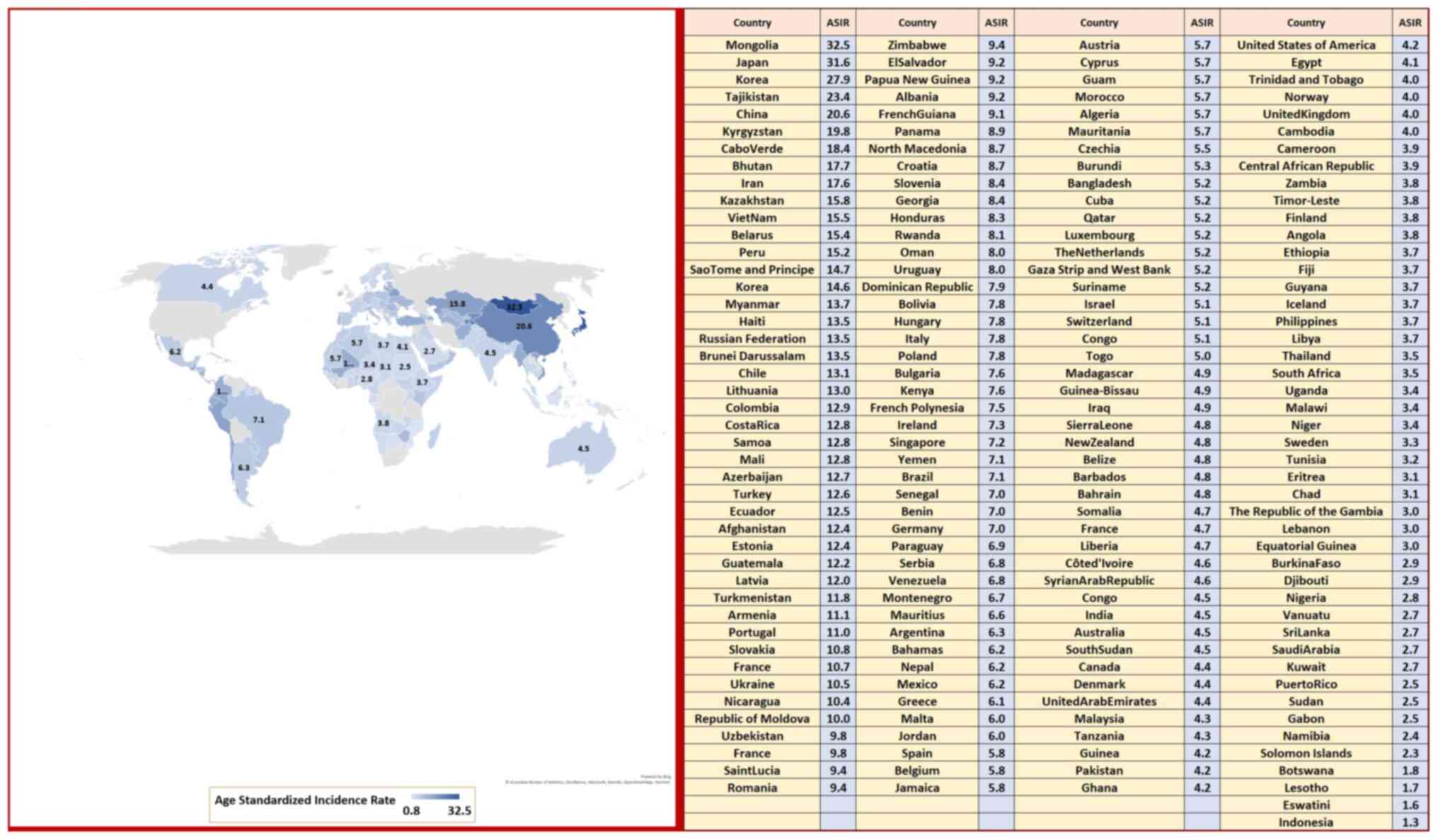
sexes in 2019, notably lower than numerous other countries. Among
Arabian Gulf countries, Oman registered the highest GC rate for
both sexes at 8.0 per 100,000 individuals which was ~2.9 times that
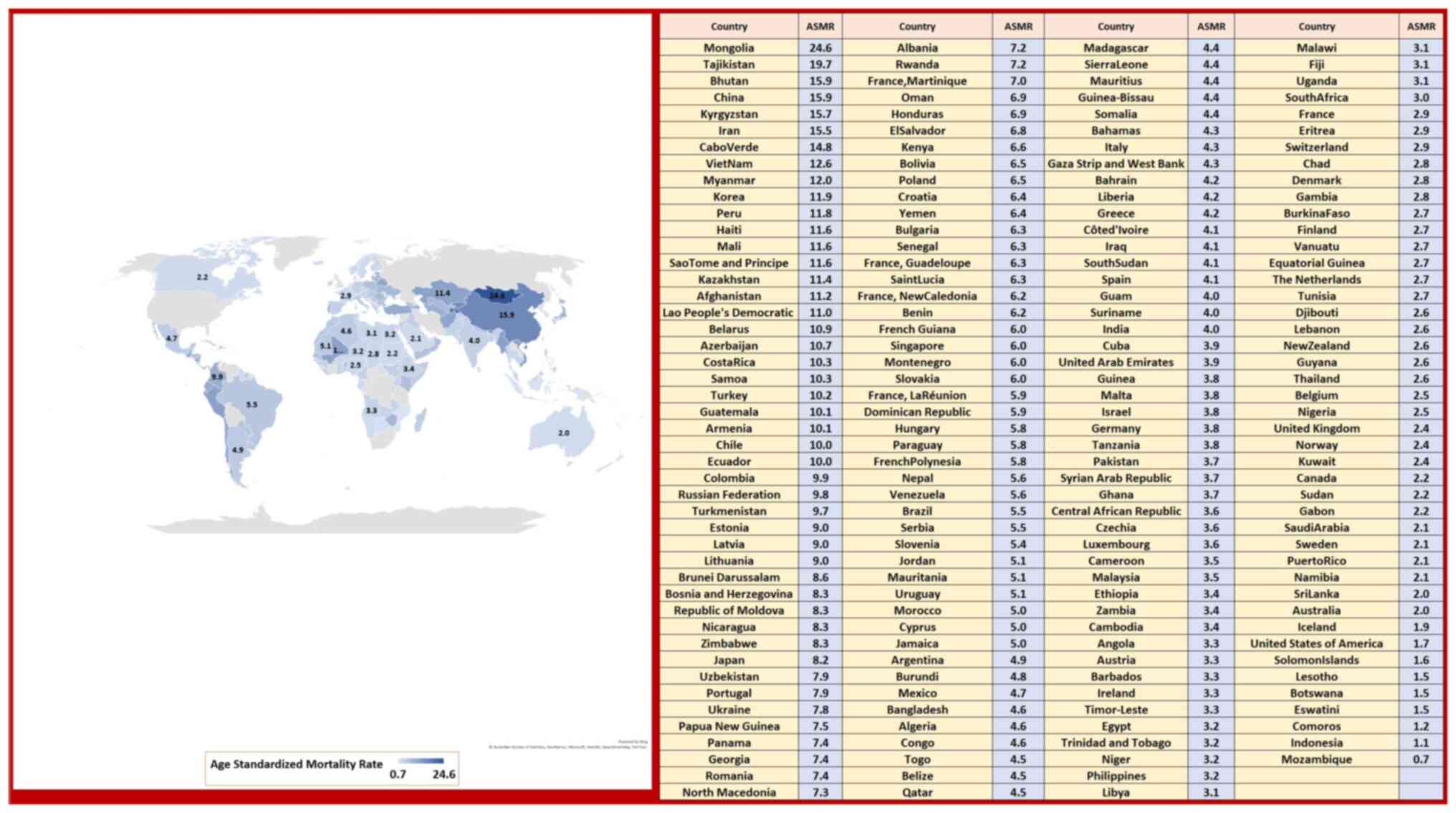
of Saudi Arabia (Fig. 8). The ASMR
for GC in Saudi Arabia was recorded at 2.1 per 100,000 individuals
for both sexes, a slightly lesser rate in comparison with other
Arab nations (Fig. 9). Notably,
Oman showed the peak ASMR for GC among both sexes in the region,
with a rate of 6.9 per 100,000 individuals, which was ~3.2 times
that of Saudi Arabia. The ASIR of Saudi Arabia for GC was
significantly less than countries such as Mongolia (32.5 per
100,000 individuals), Japan (31.6 per 100,000 individuals) and
Korea (27.7 per 100,000 individuals), where the rates were almost 9
to 10-fold higher compared with Saudi Arabia (Fig. 9).
Discussion
It is essential to continuously monitor and update
the CIRs and ASIRs of cases of GC across all regions in Saudi
Arabia. The aim of the present retrospective study was to examine
the trends in CIR and ASIR of GC in Saudi Arabia between 2004 and
2017. To the best of the authors' knowledge, this is the first
descriptive epidemiological study on the spatial and temporal
distribution of GC that has been performed among both men and women
in various regions of Saudi Arabia, based on the PubMed database.
The present study has shed light on the current status of GC
trends, and the significance of the disease, in the Saudi Arabian
population.
The present study identified that, between 2004 and
2017, GC accounted for 3.7 and 2.1% of all cancer cases in Saudi
men and women, respectively, with totals of 175 and 110 cases
confirmed. Furthermore, significantly higher numbers of cases of GC
were observed among individuals aged ≥50 years, with males having
the higher percentage (83.3%) and females having a percentage of
70.9%. On the other hand, individuals ≤49 years old were less
affected by GC, with male and female patients having percentages of
16.7 and 29.0%, respectively. These results are consistent with
previous studies, which reported a median age of diagnosis for GC
of 72 years, and a diagnosis percentage of ~10% in patients under
the age of 45 years (11-13).
GC is a disease that often develops over a long period, which is
associated with risk factors such as chronic infection with H.
pylori, smoking and a diet high in salt and preserved foods.
Therefore, it is not surprising that the majority of cases were
observed in individuals aged ≥50 years, who have had a longer
period of exposure to these risk factors.
The incidence rate of GC in Saudi Arabia was
investigated, and it was detected that this was higher in men
compared with women. Specifically, it was observed that, between
2004 and 2017, the CIR and ASIR values of GC were 2-fold greater in
Saudi men compared with women. This finding was consistent with the
global trend, as the incidence of GC is known to vary according to
sex and geographical location, with men being more commonly
affected than women, and with the risk also increasing with age
(14). In the United States,
previous studies have indicated that the male sex is the most
significant risk factor for the development of GC, with a 2:1
male-to-female ratio predominance (15). Moreover, in developed countries,
men are 2.2 times more likely than women to be diagnosed with GC
(16). The findings of the present
study, along with those of other studies, have highlighted the
significance of the male sex as a predictor of GC. Moreover, the
study conducted by Yang et al (17) investigated not only the incidence
rates, but also the survival rates of patients with metastatic GC,
revealing that male patients had significantly lower survival rates
compared with female patients. This finding suggests that sex may
not only affect the incidence of GC, but also the prognosis and
outcomes of patients with this disease. However, the higher
incidence of GC in males compared with females may be due to
hormonal differences, as estrogen has been revealed to have a
protective effect against GC (18). Additionally, lifestyle factors,
including smoking and alcohol consumption, may also contribute to
this sex difference observed in incidence rates. Overall, the
findings of the present study have highlighted the importance of
early detection and prevention efforts for GC, particularly among
older individuals and males.
The present study also revealed that the ASIR trend
of GC among Saudi men and women dropped steadily between the years
2004 and 2017. This trend is consistent with the gradual decrease
in incidence rates of GC that have been observed throughout the
world in recent decades, including in the United States (Fig. 7) (1,19).
Several factors may have contributed to this decrease, such as
improved standards of hygiene, enhanced food preservation and
increased intake of fresh fruit and vegetables. Additionally, the
widespread implementation of H. pylori eradication programs
may also have contributed a role towards this downward trend
(1,20). The ASIR of GC demonstrated yearly
fluctuations for both males and females, with a gradual increase
between 2004 and 2006, followed by a slight decline in subsequent
years, and furthermore demonstrated sex disparities, as observed
with notably higher ASIR for males in certain years like 2009 and
2013, while ASIR for females was comparatively higher in 2010 and
2011. The observed variations in the ASIR of GC can be attributed
to several reasons. Population dynamics play a role, where changes
in age distributions and demographic factors, such as population
growth, migration patterns and aging populations over the years,
contribute to fluctuations in the ASIR. Additionally, improvements
in diagnostic practices and increased awareness of GC among
healthcare professionals and the public may lead to early detection
and higher incidence rates, resulting in fluctuations in ASIR over
time. Moreover, data completeness and variations in the quality of
data reporting in different years can impact the ASIR results.
Changes in data collection methods, reporting systems, or
healthcare infrastructure may affect the accuracy of recorded
cancer cases, influencing the observed ASIR.
The findings of the present study also indicated
that GC is more prevalent among male and female residents of the
regions Riyadh, Najran and the Eastern region of Saudi Arabia
between 2004 and 2017. This implied that individuals in these
regions are at a higher risk of developing GC. On the other hand,
individuals in Jazan, Saudi Arabia, were less affected by GC,
indicating that they may be exposed to protective factors against
GC compared with individuals in other regions of Saudi Arabia.
However, a more extensive epidemiological study is necessary to
identify the potential risk factors that contribute to the
increased ASIR of GC among Saudi men and women in the Riyadh,
Najran and Eastern regions. In addition, protective factors against
GC in the Jazan region should be investigated.
In Saudi Arabia, the ASIR for GC in 2020 was
estimated to be 2.7% per 100,000 individuals for both sexes, which
is significantly lower compared with other countries. Oman was
found to have the highest rate of GC among both sexes in the
Arabian Gulf, with a rate of 8.0 per 100,000 individuals, which is
2.9 times higher than that of Saudi Arabia (Fig. 8). Moreover, the ASMR of GC in Saudi
Arabia was observed to be 2.1 per 100,000 individuals for both
sexes. This mortality rate was slightly lower compared with other
Arab countries (Fig. 9). However,
Oman had the highest ASMR of GC among both sexes, with a rate of
6.9 per 100,000 individuals, which was 3.2 times higher than that
of Saudi Arabia. The results of the present study have indicated
that the overall ASIR of GC in Saudi Arabia was considerably lower
than in Mongolia (32.5 per 100,000 individuals), Japan (31.6 per
100,000 individuals) and Korea (27.7 per 100,000 individuals),
where the rates were 9 to 10 times higher than in Saudi Arabia
(9).
To the best of the authors' knowledge, the impact of
the COVID-19 pandemic on the incidence rate of GC and those of
other types of cancer in Saudi Arabia has not been studied
extensively. However, it is important to consider that Saudi Arabia
is part of the global community, and therefore the cancer incidence
rates may be subjected to the same types of factors that influence
the trends and effects as are observed in other parts of the world.
The COVID-19 pandemic disrupted healthcare systems, delayed
screenings, diagnoses and altered treatment plans, leading to
potential changes in the patterns of cancer detection and
reporting. One notable effect of the pandemic has been a decrease
in cancer screenings and routine healthcare visits. Numerous
countries implemented lockdown measures and restrictions on
non-essential medical services to curb the spread of the virus.
These actions resulted in the postponement or cancellation of
screenings such as mammograms, Pap smears, colonoscopies and other
tests commonly used for cancer detection. As a consequence, there
has been a decline in cancer diagnoses during the pandemic
(21).
Furthermore, individuals may have been hesitant to
seek medical attention or visit healthcare facilities due to fear
of contracting COVID-19 or overwhelming healthcare systems. This
delay in seeking care could lead to missed or delayed cancer
diagnoses, potentially impacting cancer incidence rates. The impact
of the pandemic on cancer incidence rates may vary according to the
type of cancer involved. Certain cancers, such as breast and
prostate cancer, heavily rely on routine screenings for early
detection. Consequently, their incidence rates may have been more
significantly affected by the pandemic. Other types of cancers,
such as lung or pancreatic cancer, may not be as heavily dependent
on routine screenings, and so their incidence rates could be less
severely affected. However, further research is necessary to
determine the precise magnitude and long-term implications of these
effects (22).
The variations in GC rates in Saudi Arabia over the
studied 14-year period can be attributed to several specific
factors. Notably, significant events in the Saudi healthcare system
could have influenced the GC rates. The substantial investments of
the government in expanding and improving healthcare infrastructure
across the country during this time may have resulted in increased
access to medical facilities, leading to improved screening and
diagnostic services for GC, and consequently, more cases being
detected, potentially causing an apparent increase in GC rates.
Furthermore, changes in lifestyle and dietary habits among the
Saudi population over time may have played a role in the observed
variations in GC rates. The introduction of fast-food chains,
sedentary lifestyles and a shift towards processed foods may have
contributed to an increase in risk factors associated with GC.
Moreover, increased awareness about GC among both the general
population and healthcare professionals could have led to more
frequent screenings and early detection, potentially capturing more
GC cases. Demographic shifts in the Saudi population, such as
increased life expectancy and alterations in age distribution, may
have influenced the overall GC incidence rates, as GC is often
associated with older age groups. Lastly, improvements in
diagnostic techniques and accuracy over time could have led to
improved detection and reporting of GC cases, accounting for some
of the observed variations in GC rates. Overall, these factors
represent crucial aspects to consider when analyzing the
fluctuations in GC rates in Saudi Arabia.
During the period from 2004 to 2017, Saudi Health
Institutions witnessed significant advancements in diagnostic
techniques and enhanced accuracy. These improvements likely
contributed to the observed higher incidence rates and fluctuations
in ASIR of cancer diseases. In this span of time, there were
notable enhancements in medical technology, including the
widespread adoption of advanced imaging modalities such as MRI, CT
scans and digital radiography. These technologies allowed for
earlier and more precise detection of various health conditions,
potentially leading to increased diagnoses of certain diseases.
Moreover, the genetic testing methods became more prevalent
worldwide, enabling healthcare professionals to identify specific
genetic markers associated with diseases (23). Cancer diseases pose a significant
health challenge globally, affecting individuals of various ages
and backgrounds. In the context of Saudi Arabia, where healthcare
advancements have been notable, there has been a remarkable
improvement in life expectancy. The life expectancy in Saudi Arabia
stood at 73 years of age in 2004, and by 2017, it had risen to 76
(https://data.worldbank.org/indicator/SP.DYN.LE00.MA.IN?view=chart).
This increase can be attributed to various factors, including
advancements in medical care, improved access to healthcare
services, and enhanced public health awareness. As life expectancy
continues to rise, addressing the prevalence and impact of cancer
diseases becomes even more crucial, prompting the healthcare system
to further prioritize effective prevention, early detection and
comprehensive treatment strategies to ensure the well-being of the
population.
The present study has provided valuable insights
into the incidence rates of GC in Saudi Arabia and has provided
information which should help inform future research and public
health initiatives. However, it is important to acknowledge the
limitations of the present study, such as the absence of a
comparison group and the inability to assess the statistical
association between potential risk factors and GC. The lack of
information on GC-associated deaths in the SCR reports prevented
the determination of average death rates of GC in various regions
of Saudi Arabia. Additionally, the limitation of not being able to
collect TNM staging information at the initial diagnosis of GC from
the SCR is acknowledged. The SCR only provides TNM staging data for
the top ten cancer types in Saudi Arabia, and GC is not among those
reported. As a result, it was not possible to provide a specific
description of the change in TNM stage in the initial diagnosis of
GC based on SCR data. This limitation is important to note as it
could have implications for the comprehensiveness of the findings
of the present study and the potential impact on public health
research related to cancer in Saudi Arabia. Future studies with a
specific focus on GC and more comprehensive data collection methods
may help address this limitation and provide a deeper understanding
of TNM stage changes in GC diagnoses in the country.
One significant limitation to the present study is
the lack of comparison between the incidence of GC in the years
2004-2017 and 2020-2022, which coincides with the pandemic period.
At present, the SCR has not released the report for the years
2020-2022, and thus, the age-specific incidence rates, CIRs, and
ASIRs of GC in Saudi Arabia during the COVID period are not
available. This limitation hinders the ability to make direct
comparisons between the incidence of GC before and during the
pandemic, which could have provided valuable insights into any
potential impacts or changes in cancer incidence patterns during
this challenging time. However, despite this limitation, the
primary focus of the study on the incidence of GC from 2004 to 2017
offers crucial baseline data and enhances the comprehension of
cancer trends in the pre-pandemic period. By contributing to the
existing literature on GC, the present study has shed light on the
necessity for additional research to identify and address potential
risk factors for this disease in the Saudi population.
Another significant limitation highlighted in the
present study is related to the lack of population coverage data
and the percentage completeness of recorded cancer cases, which can
greatly impact the accuracy and reliability of health-related
statistics, particularly in disease surveillance and public health
research. These limitations have far-reaching implications, leading
to potential underestimation or overestimation of the disease
burden, introducing bias in demographic and epidemiological
profiles, and hindering accurate disease surveillance and outbreak
detection. Moreover, they can impede efforts to monitor health
disparities, allocate resources efficiently and affect the validity
and generalizability of research findings. To address these issues,
it is crucial for health authorities to improve data collection
systems, enhance case reporting completeness and ensure
comprehensive coverage of population data in registration areas
through improved collaboration, accurate recordkeeping, and
advanced health information systems.
In conclusion, the present study has demonstrated
that there has been a small decline in the CIRs and ASIRs of GC in
the Saudi population between 2004 and 2017. Riyadh, Najran and the
Eastern Region were revealed to have the highest overall ASIRs of
GC among male and female Saudis, whereas Jazan had the lowest rates
for both sexes. Between 2004 and 2017, the ratio of cases of GC in
male Saudis was detected to be double that of female Saudis.
Further epidemiological studies, however, are required to determine
the potential risk factors for GC in Saudi Arabia.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets generated and/or analyzed during the
current study are available in the National Health Information
Centre's website, https://nhic.gov.sa/en/eServices/Pages/TumorRegistration.aspx.
Author's contributions
IA contributed in the conceptualization,
methodology, data analysis, visualization, investigation and
supervision of the present study, in the writing and preparation of
the original draft as well as in the writing, reviewing and editing
of the manuscript. IA confirms the authenticity of all the raw
data.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The author declares that he has no competing
interests.
References
|
1
|
Machlowska J, Baj J, Sitarz M, Maciejewski
R and Sitarz R: Gastric cancer: Epidemiology, risk factors,
classification, genomic characteristics and treatment strategies.
Int J Mol Ici. 21(4012)2020.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Ferlay J, Shin HR, Bray F, Forman D,
Mathers C and Parkin DM: Estimates of worldwide burden of cancer in
2008: GLOBOCAN 2008. Int J Cancer. 127:2893–2917. 2010.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Mukkamalla SKR, Recio-Boiles A and Babiker
HM: Gastric cancer. In: StatPearls (Internet). StatPearls
Publishing, Treasure Island, FL, 2022.
|
|
4
|
Ang T and Fock KM: Clinical epidemiology
of gastric cancer. Singapore Med J. 55:621–628. 2014.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Ferro A, Peleteiro B, Malvezzi M, Bosetti
C, Bertuccio P, Levi F, Negri E, La Vecchia C and Lunet N:
Worldwide trends in gastric cancer mortality (1980-2011), with
predictions to. 2015, and incidence by subtype. Eur J Cancer.
50:1330–1344. 2014.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Edwards BK, Noone AM, Mariotto AB, Simard
EP, Boscoe FP, Henley SJ, Jemal A, Cho H, Anderson RN, Kohler BA,
et al: Annual Report to the Nation on the status of cancer,
1975-2010, featuring prevalence of comorbidity and impact on
survival among persons with lung, colorectal, breast, or prostate
cancer. Cancer. 120:1290–1314. 2014.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Kaneko S and Yoshimura T: Time trend
analysis of gastric cancer incidence in Japan by histological
types, 1975-1989. Br J Cancer. 84:400–405. 2001.PubMed/NCBI View Article : Google Scholar
|
|
8
|
American Cancer Society. Key statistics
about stomach cancer. American Cancer Society, Atlanta, GA, 2022.
https://www.cancer.org/cancer/stomach-cancer/about/key-statistics.html.
Accessed September 20, 2022.
|
|
9
|
International Agency for Research on
Cancer (IARC): GLOBOCAN. Maps: Section for Cancer Incidence and
Mortality. IARC, Lyon, 2020. https://gco.iarc.fr/today/home. Accessed September 20,
2020.
|
|
10
|
Saudi Cancer Registry. Cancer Incidence
Report Saudi Arabia 2017. Saudi Cancer Registry, Riyadh, 2017.
|
|
11
|
Kong X, Wang JL, Chen HM and Fang JY:
Comparison of the clinicopathological characteristics of young and
Elderly patients with gastric carcinoma: A meta analysis. J Surg
Oncol. 106:346–352. 2012.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Takatsu Y, Hiki N, Nunobe S, Ohashi M,
Honda M, Yamaguchi T, Nakajima T and Sano T: Clinicopathological
features of gastric cancer in young patients. Gastric Cancer.
19:472–478. 2015.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Milne AN, Sitarz R, Carvalho R, Carneiro F
and Offerhaus GJ: Early onset gastric cancer: On the road to
unraveling gastric carcinogenesis. Curr Mol Med. 7:15–28.
2007.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Forman D and Burley V: Gastric cancer:
Global pattern of the disease and an overview of environmental risk
factors. Best Pract Res Clin Gastroenterol. 20:633–649.
2006.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Suryawala K, Soliman D, Mutyala M, Nageeb
S, Boktor M, Seth A, Aravantagi A, Sheth A, Morris J, Jordan P, et
al: Gastric cancer in women: A regional health-center seven year
retrospective study. World J Gastroenterol. 21:7805–7813.
2015.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Rawla P and Barsouk A: Epidemiology of
gastric cancer: Global trends, risk factors and prevention. Prz
Gastroenterol. 14:26–38. 2019.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Yang D, Hendifar A, Lenz C, Togawa K, Lenz
F, Lurje G, Pohl A, Winder T, Ning Y, Groshen S and Lenz HJ:
Survival of metastatic gastric cancer: Significance of age, sex and
race/ethnicity. J Gastrointest Oncol. 2:77–84. 2011.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Chen C, Gong X, Yang X, Shang X, Du Q,
Liao Q, Xie R, Chen Y and Xu J: The roles of estrogen and estrogen
receptors in gastrointestinal disease (review). Oncol Lett.
18:5673–5680. 2019.PubMed/NCBI View Article : Google Scholar
|
|
19
|
National Cancer Institute (NCI): Cancer of
the stomach-cancer stat facts. NCI, Bethesda, MD, 2022. https://seer.cancer.gov/statfacts/html/stomach.html.
Retrieved September 26, 2022.
|
|
20
|
Sitarz R, Skierucha M, Mielko J, Offerhaus
GJA, Maciejewski R and Polkowski WP: Gastric cancer: Epidemiology,
prevention, classification, and treatment. Cancer Manag Res.
10:239–248. 2018.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Lombe DC, Mwaba CK, Msadabwe SC, Banda L,
Mwale M, Pupwe G, Kamfwa P, Kanduza M, Munkupa H, Maliti B, et al:
Zambia's national cancer centre response to the COVID-19
pandemic-an opportunity for improved care. Ecancermedicalscience.
14(1051)2020.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Kartik A, Garg D and Singh RB:
Implications of reduced health care services for cancer patients in
India and similar resource-limited health care systems during
COVID-19 pandemic. Asia Pac J Public Health. 32:287–288.
2020.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Pulumati A, Pulumati A, Dwarakanath BS,
Verma A and Papineni RVL: Technological advancements in cancer
diagnostics: Improvements and limitations. Cancer Rep (Hoboken).
6(e1764)2023.PubMed/NCBI View Article : Google Scholar
|