Introduction
Although primary tumors of the lacrimal sac are
rare, they can occasionally present as a cause of nasolacrimal duct
obstruction (1,2). When the tumor is confined within the
lacrimal sac without extra-saccular extension, preoperative
diagnosis is often challenging. Computed tomography (CT) and CT
dacryocystography (CT-DCG) can improve the detection rate of
space-occupying lesions within the lacrimal sac (3-5);
however, small intramucosal or submucosal tumors may remain
undetected on imaging. Extranodal marginal zone B-cell lymphoma of
mucosa-associated lymphoid tissue (MALT lymphoma) most commonly
arises in the stomach, salivary glands and ocular adnexa; however,
recent studies have demonstrated that it may also occur in a
variety of non-classical extranodal sites, frequently presenting
with non-specific inflammatory features and leading to diagnostic
delay (6-8).
Among primary lacrimal sac tumors, lymphomas are
rare, and reports of MALT lymphoma are particularly uncommon
(9-12).
In numerous cases, these tumors are misdiagnosed as chronic
dacryocystitis and are managed conservatively for extended periods
of time, rendering pre-operative diagnosis especially difficult.
The present study describes the case of a patient with lacrimal sac
MALT lymphoma which was diagnosed intraoperatively by biopsy;
although the patient exhibited typical symptoms of dacryocystitis,
there were no obvious pre-operative imaging findings suggestive of
a tumor.
Case report
An 83-year-old woman presented to Toyama University
Hospital (Toyama, Japan) in July, 2022 with complaints of
left-sided epiphora and mucopurulent discharge. Upon a
pre-operative physical examination, no palpable mass was detected
in the medial canthus, and gentle pressure over the lacrimal sac
elicited mucopurulent reflux. A pre-operative laboratory evaluation
consisted of routine blood tests, which revealed no clinically
significant abnormalities other than poorly controlled diabetes
mellitus (HbA1c, 8.1%). She had a medical history of diabetes
mellitus, but no history of immunosuppressive therapy or any
malignancy. No bloody discharge was observed. Lacrimal irrigation
revealed the complete obstruction on the left side with purulent
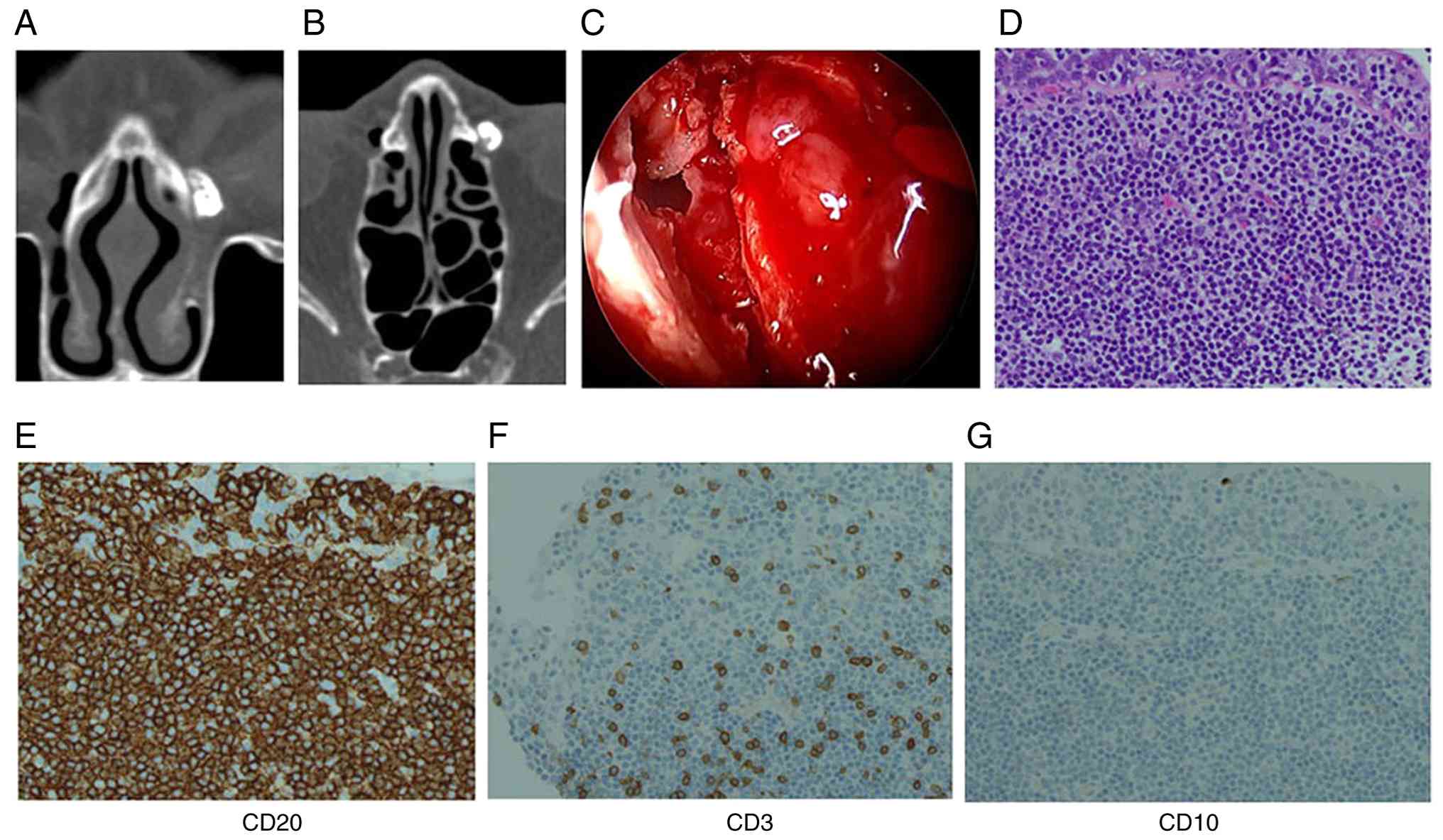
reflux. Representative images of CT-DCG are illustrated in Fig. 1. A coronal plane image is presented
in Fig. 1A and an axial plane image
is illustrated in Fig. 1B, both
demonstrating the lacrimal sac filled with contrast, with a mild
filling defect noted. A mild filling defect was noted, which was
not definitively suggestive of a neoplasm. Endoscopic endonasal
dacryocystorhinostomy (DCR) was performed. Intraoperatively, a
well-circumscribed polypoid mucosal mass was identified within the
lacrimal sac, and a biopsy was obtained (Fig. 1C).
A histopathological examination was performed using
4-µm-thick sections obtained from formalin-fixed, paraffin-embedded
tissue. The specimens were fixed in 10% neutral-buffered formalin
at room temperature for ~24 h. Hematoxylin and eosin staining was
performed according to standard protocols. Staining was carried out
at room temperature. The stained sections were examined using a
standard light microscope routinely used in the pathology
laboratory (manufacturer not recorded). The histopathological
examination revealed a uniform proliferation of small lymphocytes
infiltrating the epithelium (Fig.
1D). In addition, immunohistochemical analysis was performed on
4-µm-thick sections prepared from formalin-fixed, paraffin-embedded
tissue. Following deparaffinization and antigen retrieval using
standard protocols, the sections were incubated with primary
antibodies against CD20, CD10, and CD3. The antibodies used were
commercially available antibodies purchased from Roche Diagnostics
(Ventana Medical Systems): CD20 (clone L26, cat. no. 760-2531),
CD10 (clone SP67, cat. no. 790-4506), and CD3 (clone 2GV6, cat. no.
790-4341). These antibodies are routinely used in th authors'
pathology laboratory. Immunostaining was carried out according to
standard protocols at room temperature, followed by visualization
using a conventional detection system routinely used in our
pathology laboratory; however, the supplier and catalogue number of
the detection system were not recorded at the time of analysis A
commercially available secondary antibody routinely used in our
pathology laboratory was applied; however, the dilution, catalogue
number, supplier, conjugate, and the exact temperature and duration
of incubation were not recorded at the time of analysis. Sections
were counterstained with hematoxylin according to standard
protocols at room temperature. Immunostained sections were examined
using a light microscope (manufacturer not recorded). The
magnification is indicated in the figure legends.
Immunohistochemical staining revealed positive reactivity for CD20,
almost negative for CD10, and scattered CD3-positive reactive
T-cells in the background (Fig.
1E-G), leading to a diagnosis of MALT lymphoma. In the
differential diagnosis, IgG4-related disease, reactive lymphoid
hyperplasia and other types of malignant lymphoma were carefully
considered. IgG4-related disease was considered unlikely as there
were no histopathological features such as dense storiform fibrosis
or obliterative phlebitis, and the patient had no systemic
manifestations suggestive of IgG4-related disease. In addition,
there was no histopathological evidence suggestive of IgG4-related
disease, and serum IgG4 levels were within the normal range.
Reactive lymphoid hyperplasia was excluded based on the presence of
a monotonous proliferation of small lymphoid cells with
lymphoepithelial lesions and the lack of preserved follicular
architecture. Other B-cell lymphomas, including follicular lymphoma
and diffuse large B-cell lymphoma, were considered unlikely due to
the absence of a follicular growth pattern, only a weak and focal
expression of CD10, the lack of high-grade cytological atypia and
low-grade histological features.
Taken together, these morphological and
immunohistochemical findings supported the diagnosis of MALT
lymphoma. Genetic testing and flow cytometry were not performed.
Comprehensive clinical staging was performed to determine whether
the lesion represented primary or secondary involvement. Whole-body
positron emission tomography-computed tomography (PET-CT) was
performed for staging purposes and revealed no evidence of systemic
lymphoma involvement, and a bone marrow examination revealed no
evidence of lymphomatous infiltration. Based on these staging
results, the lesion was diagnosed as a primary lacrimal sac MALT
lymphoma. The patient has been under careful observation without
additional treatment. Follow-up has primarily been performed with
periodic CT scans, and no recurrence has been observed during 24
months of follow-up.
Discussion
In the present case report, the patient exhibited
typical clinical features of dacryocystitis, and CT-DCG revealed
only a mild filling defect within the lacrimal sac, with no
findings suggestive of malignancy. However, the intraoperative
identification of a polypoid lesion prompted a biopsy, which
revealed MALT lymphoma. Primary malignant lymphoma of the lacrimal
sac is rare and often clinically indistinguishable from
inflammatory conditions. MALT lymphoma is known to arise in a wide
range of extranodal sites beyond the classic locations and often
presents with non-specific inflammatory features, which can result
in diagnostic delay. The present case report reflects this
well-recognized diagnostic challenge, with lacrimal sac involvement
mimicking chronic dacryocystitis (6-8).
Accordingly, differentiating primary lacrimal sac MALT lymphoma
from chronic dacryocystitis can be particularly challenging due to
overlapping clinical features.
Suspicious findings that may suggest a lacrimal sac
tumor include a firm medial canthal mass, recurrent dacryocystitis,
bony erosion on imagingand blood-stained epiphora (13). However, these signs are typically
absent in the early stages of disease. Notably, blood-stained
epiphora is uncommon and has been reported to be a non-specific and
infrequent symptom in patients with lacrimal sac malignancies
(13). As demonstrated by the
present case report, some tumors may present without any
characteristic symptoms and are diagnosed incidentally during
surgery. Previous pathological studies analyzing routinely excised
lacrimal sac tissue during DCR have reported that the majority of
cases exhibit non-specific inflammation, with the incidence of
malignant neoplasms ranging from 0 to 3.7% (14-18).
Based on these findings, several studies have suggested that
routine lacrimal sac biopsy during DCR may be unnecessary and
should be reserved for cases with intraoperative findings
suspicious for neoplasm (14-18).
However, the available evidence in the literature remains limited
regarding which specific intraoperative features should prompt a
tissue biopsy.
Previous studies have indicated that 22-38% of
patients with malignant lacrimal sac tumors initially present with
symptoms resembling dacryocystitis (1-3).
Moreover, it has been reported that 60-88% of lacrimal sac tumors
are malignant in nature (12,19).
Among these malignancies, squamous cell carcinoma and malignant
lymphoma are the most common histological types (12,20).
Given these findings, it is essential not to overlook the
possibility of malignancy, even in cases without pre-operative
radiologic or clinical suspicion. In the event that any mass-like
or elevated lesion is observed within the lacrimal sac during
surgery, a proactive and definitive biopsy should be performed. The
key lesson from the case described herein is the potential
diagnostic pitfall in lacrimal sac lesions presenting with symptoms
indistinguishable from chronic dacryocystitis. Even when
pre-operative imaging findings are non-specific, small intramucosal
or submucosal lymphomas may be concealed within the lacrimal sac.
Careful intraoperative inspection of the entire lacrimal sac is
therefore crucial, and any mass-like or elevated lesion should
prompt biopsy to avoid delayed or missed diagnosis.
Where possible, additional diagnostic modalities,
such as flow cytometry and genetic analysis are recommended to
ensure accurate characterization of the lesion. In the case
presented herein, clonality testing was not performed, which
represents a limitation of the present case report. Nevertheless,
the diagnosis was supported by characteristic histopathological and
immunohistochemical findings. This underscores the importance of
careful and thorough intraoperative inspection of the entire
lacrimal sac to avoid missing potentially malignant lesions and
facilitate early diagnosis and appropriate management.
The management of ocular adnexal MALT lymphoma
varies depending on disease stage and institutional practice, and
treatment options may include observation, radiotherapy, or
systemic therapy (6,10).
Based on these findings, even in the absence of
preoperative signs suggestive of a tumor, any mass-like or elevated
lesion identified within the lacrimal sac should be biopsied with
adequate tissue sampling to obtain a definitive diagnosis. In the
present case report, the patient has been followed-up primarily
with periodic CT scans, and no recurrence was observed during 24
months of follow-up. While magnetic resonance imaging may provide
higher soft-tissue contrast and may be considered if clinical
suspicion arises or if CT findings are inconclusive, CT was deemed
sufficient for routine monitoring given the location and size of
the lesion.
The present case report highlights the importance of
maintaining a high index of suspicion for neoplastic disease during
surgical treatment of lacrimal sac disorders. It serves as a
valuable reminder of the clinical significance of thorough
intraoperative evaluation and reinforces the need for vigilance in
the diagnosis and management of lacrimal sac tumors.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The data generated in the present study are not
publicly available in order to protect patient privacy but may be
requested from the corresponding author.
Authors' contributions
TY and AH designed the study, reviewed the clinical
and pathological materials, and wrote and edited the manuscript.
HT, YM and NO reviewed the clinical data material of the patient
and edited the manuscript. TY and AH confirm the authenticity of
all the raw data. All authors have read and approved the final
manuscript.
Ethics approval and consent to
participate
The present case report was conducted in accordance
with the principles of the Declaration of Helsinki. Written
informed consent to participate was obtained from the patient.
Patient consent for publication
Written informed consent was obtained from the
patient for the publication of the present case report and any
accompanying images.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Ryan SJ and Font RL: Primary epithelial
neoplasms of the lacrimal sac. Am J Ophthalmol. 76:73–88.
1973.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Stefanyszyn MA, Hidayat AA, Pe'er JJ and
Flanagan JC: Lacrimal sac tumors. Ophthalmic Plast Reconstr Surg.
10:169–184. 1994.
|
|
3
|
Krishna Y and Coupland SE: Lacrimal sac
tumors-A review. Asia Pac J Ophthalmol (Phila). 6:173–178.
2017.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Ali MJ, Singh S, Naik MN, Kaliki S and
Dave TV: Interactive navigation-guided ophthalmic plastic surgery:
The utility of 3D CT-DCG-guided dacryolocalization in secondary
acquired lacrimal duct obstructions. Clin Ophthalmol. 11:127–133.
2017.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Wang YH, Jiang WH, Tu YH, Zhou GM, Wu WC
and Yu B: Endoscopic dacryocystorhinostomy with mucosal
anastomosing in chronic dacryocystitis with three categories of
ethmoid sinuses. Int J Ophthalmol. 15:1765–1771. 2022.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Segura-Rivera R and Pina-Oviedo S:
Marginal zone lymphoma of extranodal sites: A review with an
emphasis on diagnostic pitfalls and differential diagnosis with
reactive conditions. Hum Pathol. 156(105683)2025.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Fiorentino V, Pizzimenti C, Pierconti F,
Lentini M, Ieni A, Caffo M, Angileri F, Tuccari G, Fadda G, Martini
M and Larocca LM: Unusual localization and clinical presentation of
primary central nervous system extranodal marginal zone B-cell
lymphoma: A case report. Oncol Lett. 26(408)2023.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Chen GP, Lu ZZ, Lu GZ, Zhou Y and Wu SG:
An epidemiological study on survival in lymphoma of
mucosa-associated lymphoid tissue: A comparative analysis by
primary tumor location. J Invest Surg. 38(2523858)2025.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Kitaguchi Y, Takahashi Y, Mupas-Uy J,
Takahashi E and Kakizaki H: Primary marginal zone B-cell lymphoma
of the mucosa-associated lymphoid tissue of the lacrimal sac found
with epiphora: A case report. Case Rep Ophthalmol. 7:148–154.
2016.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Singh S and Ali MJ: Lymphoproliferative
tumors involving the lacrimal drainage system: A major review.
Orbit. 39:276–284. 2020.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Sabundayo MS, Takahashi Y and Kakizaki H:
Lacrimal sac lymphoma: A series of Japanese patients. Eur J
Ophthalmol. 29:678–684. 2019.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Wakasaki T, Yasumatsu R, Tanabe M,
Yoshikawa H, Jiromaru R, Hashimoto K, Matsuo M, Fujimura A and
Nakagawa T: Lacrimal sac tumors: A single-institution experience,
including new insights. In Vivo. 37:1219–1225. 2023.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Singh S and Ali MJ: Primary malignant
epithelial tumors of the lacrimal drainage system: A major review.
Orbit. 40:179–192. 2021.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Knežević M, Stojković M, Jovanović M,
Stanković Z and Rašić DM: A 7-year prospective study of routine
histopathological evaluation of the lacrimal sac wall incisional
biopsy specimens obtained during external dacryocystorhinostomy in
adults and a review of the literature. Med Oncol. 29:396–400.
2012.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Anderson NG, Wojno TH and Grossniklaus HE:
Clinicopathologic findings from lacrimal sac biopsy specimens
obtained during dacryocystorhinostomy. Ophthalmic Plast Reconstr
Surg. 19:173–176. 2003.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Lee-Wing MW and Ashenhurst ME:
Clinicopathologic analysis of 166 patients with primary acquired
nasolacrimal duct obstruction. Ophthalmology. 108:2038–2040.
2001.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Banks C, Scangas GA, Husain Q, Hatton MP,
Fullerton Z and Metson R: The role of routine nasolacrimal sac
biopsy during endoscopic dacryocystorhinostomy. Laryngoscope.
130:584–589. 2020.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Koturović Z, Knežević M and Rašić DM:
Clinical significance of routine lacrimal sac biopsy during
dacryocystorhinostomy: A comprehensive review of literature. Bosn J
Basic Med Sci. 17:1–8. 2017.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Heindl LM, Jünemann AG, Kruse FE and
Holbach LM: Tumors of the lacrimal drainage system. Orbit.
29:298–306. 2010.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Zhao HS, Shi JT and Wei WB: Clinical
analysis of primary malignant lacrimal sac tumors: A case series
study with a comparison to the previously published literature. J
Craniofac Surg. 34:e115–e120. 2023.PubMed/NCBI View Article : Google Scholar
|