Introduction
Atherosclerosis (AS) is a serious disease that
causes hypoxic ischemia of the heart and leads to disordered
collagen metabolism during its progression (1,2).
Multiple studies have revealed that the urotensin II/urotensin
report (UII/UT) system, which is composed of UII and its receptor,
G protein-coupled receptor 14 (GPR14), serves an important role in
various diseases, including AS and heart disease (3,4).
Therefore, the prevention and treatment of AS via regulation of the
UII/UT system may prove to be effective for the improvement of
myocardial collagen metabolism disorders.
The Janus kinase/signal transducer and activator of
transcription (JAK/STAT) pathway is a key cytokine signaling
pathway that regulates various pathophysiological processes,
including inflammation and myocardial fibrosis (5–7). In
addition, the proteolytic enzymes matrix metalloproteinase (MMP)
and tissue inhibitor of matrix metalloproteinase can regulate the
expression of collagen, which serves an important role in
myocardial fibrosis and cardiac dysfunction (8). Study has reported that the JAK2/STAT3
pathway, MMP-2 and MMP-9 are strongly associated with the
prevention of myocardial injury by reducing inflammation and
fibrosis (9). In the present
study, the state of collagen metabolism disorders was monitored in
rats with AS by observing changes in the JAK2/STAT3 pathway and the
MMP-2/TIMP metallopeptidase inhibitor 2 (TIMP-2) protein ratio.
Urantide, a UII receptor antagonist derived from
human UII (hUII), competitively antagonizes the contraction of the
rat thoracic aorta and the mitogenic effect of UII on vascular
smooth muscle cells (10,11). The main reason for conducting the
present study was the fact that little research regarding the
association between the effects of urantide on the prevention and
treatment of AS and AS-related heart disease has been performed.
Based on the successful replication of an AS rat model, it was
demonstrated that urantide was able to significantly reduce
myocardial fibrosis in rats with AS. This effect may have been
associated with the JAK2/STAT3 pathway and the MMP-2/TIMP-2 protein
ratio.
Materials and methods
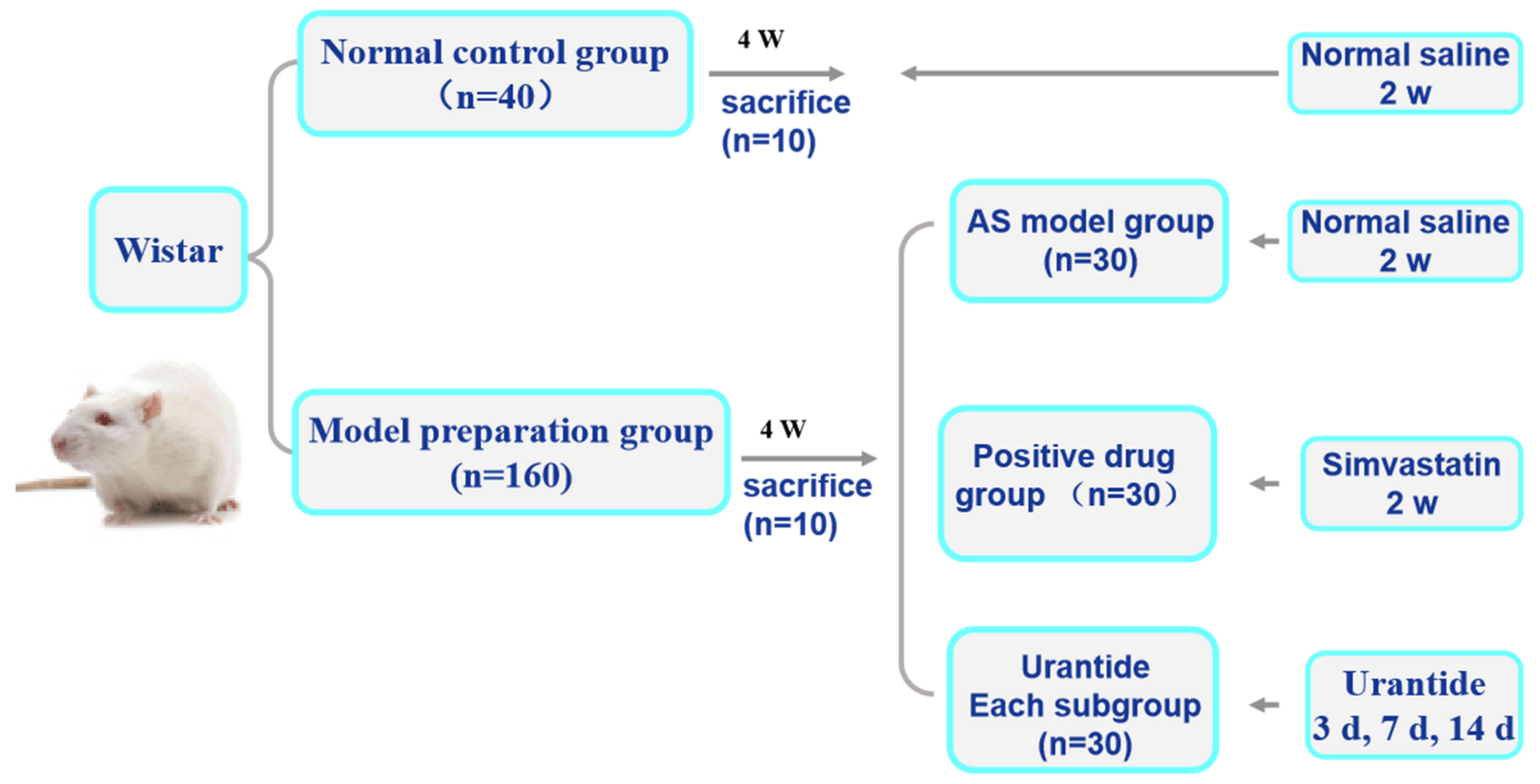
Animals and treatment groups
A total of 200 Wistar male rats (age, 4 weeks)
weighing 180–200 g were obtained from Charles River Laboratories,
Inc. and housed at a constant temperature of 22±2°C with a humidity
of 40–60% and under a 12-h light/dark cycle. The rats were randomly
divided into two groups: A normal control group consisting of 40
rats and an AS model preparation group consisting of 160 rats. Rats
in the normal control group were supplied with normal feed daily
and rats in the AS model preparation group followed a high-fat diet
according to an AS rat preparation method, as previously described
(12,13). The high-fat diet was purchased from
Beijing Keao Xieli Feed Co., Ltd. The experimental period lasted 4
weeks.
An AS rat model was established by intraperitoneal
(i.p.) injection of 150 U/kg vitamin D3 (Harbin Huasheng
Science and Technology Animal Medicine Factory) for 3 days, and
rats were continuous feeding a high-fat diet to damage the arterial
intima (14). In the fourth week,
10 rats from each of the two experimental groups were randomly
sacrificed by i.p. injection of sodium phenobarbital (150 mg/kg) in
order to detect whether the AS rat model had been successfully
replicated. Subsequently, the rats with AS were randomly divided
into the following groups: i) An AS model group (30 rats); ii) a
simvastatin group (30 rats); and iii) three urantide groups (30
rats in each of the three subgroups). Saline (30 µg/kg) was
injected into the tail veins of rats in the normal control group
and the AS model group for 14 consecutive days. Rats in the
simvastatin group were intraperitoneally injected with 5 µg/kg
simvastatin (Lunan Beite Pharmaceutical Co., Ltd.) for 14 days.
Urantide (30 µg/kg; Shanghai Qiangyao Biological Technology Co.,
Ltd.) was injected into the tail veins of rats with AS in the three
urantide groups daily for 3, 7 and 14 days, respectively. In the
present study, the dosages of simvastatin and urantide were based
on two preliminary studies by Zhao et al (10,11).
The rats were given ad libitum access to food and water. The
experimental design is presented in Fig. 1.
Sample collection and testing
All rats were sacrificed using 150 mg/kg sodium
pentobarbital (Tianjin Fuchen Chemical Co., Ltd.). The rat
abdominal aortas were punctured to obtain blood, and following
centrifugation at 1,500 × g for 10 min at 4°C, the supernatant was
stored at −20°C. In the present study, automated biochemical
analysis (BS-480; Shenzhen Mindray Bio-Medical Electronics Co.,
Ltd.) at Hebei Province 266 Hospital was performed to determine
triglyceride (TG), total cholesterol (TC), low-density lipoprotein
(LDL), high-density lipoprotein (HDL) and calcium (Ca2+)
levels.
Morphological evaluation
The thoracic aortas and hearts were dissected from
the rats and divided into two parts; one part was fixed with 4%
paraformaldehyde at 4°C for 24 h for morphological examination,
while the other part was stored directly in liquid nitrogen for
molecular biological detection.
Paraffinized, 4.5-µm sections of rat thoracic aortas
and cardiac tissue were prepared and hematoxylin and eosin
(H&E) staining (Nanchang Yulu Experimental Equipment Co., Ltd.)
was performed according to the manufacturer's instructions. A total
of 10 heart sections were randomly selected from each group. Each
section was examined for evidence of mononuclear and polymorphic
cell infiltration, necrosis and mineralization and given a
histological score of 0 to 4 as follows: i) 0, no change; ii) 1,
changes found in 0–25% of cells; iii) 2, changes found in 26–50% of
cells; iv) 3, changes found in 51–75% of cells; and v) 4, changes
found in 76–100% of cells (15).
Masson trichrome staining and
immunolocalization
Collagen content in the cardiac tissue was
determined using Masson trichrome staining (Fuzhou Maixin Biotech
Co., Ltd.). The ratio of collagen positive area to total area was
calculated using a computer imaging system. The distribution of
phosphorylated (p)-JAK2 (cat. no. ab32101; Abcam), p-STAT3
(phosphorylated-STAT3; cat. no. 9145; Cell Signaling Technology,
Inc.) and collagen type I/III (cat. no. bs-0578R/0948R; Bioss)
proteins was determined using immunofluorescence. The isolated
paraffinized heart sections were dewaxed by xylene, and following
their dehydration, stained for collagen at 22±2°C for 5 min and
incubated with antibodies against p-JAK2 (cat. no. ab32101; Abcam)
and p-STAT3 (cat. no. 9145; Cell Signaling Technology, Inc.) and
collagen type I/III (cat. no. bs-0578R/0548R; BIOSS) at 1:300 at
4°C for 12 h according to a standard protocol (16). Next, the sections which were
immunoblotted for p-JAK2/p-STAT3 and collagen type I/III were
incubated with FITC-labeled goat anti-rabbit IgG antibody (cat. no.
A0562; Beyotime Institute of Biotechnology) at 1:1,000 at 37°C for
60 min. Then, the myocardial collagen volume (%) was calculated
using Image-Pro Plus 6.0 software (Media Cybernetics, Inc.). Images
were captured using a fluorescence microscope (Olympus
Corporation).
Quantification of mRNA expression
levels by reverse transcription-quantitative PCR (RT-qPCR)
Total RNA was extracted from the cardiac tissues
using TRIzol® reagent (Invitrogen; Thermo Fisher
Scientific, Inc.) and quantified by UV spectrophotometry.
Subsequently, total RNA was reverse transcribed into cDNA using a
FastQuant RT kit (Tiangen Biotech Co., Ltd.) at 42°C for 15 min and
95°C for 3 min. qPCR was subsequently performed using the SuperReal
PreMix Plus (SYBR Green) fluorescence quantitative premixing kit
(Tiangen Biotech Co., Ltd.). The related gene primers were
synthesized by Takara Biotechnology Co., Ltd. and their respective
sequences are presented in Table
I. According to the manufacturer's protocol, the following
thermocycling conditions were used for qPCR: 95°C for 15 min,
followed by 40 cycles of 95°C for 10 sec and 60°C for 32 sec. mRNA
expression levels were quantified using the 2−ΔΔCq
method and normalized to the internal reference gene β-actin
(17,18).
 | Table I.Primer sequences used for the reverse
transcription-quantitative PCR analysis of relative mRNA expression
levels. |
Table I.
Primer sequences used for the reverse
transcription-quantitative PCR analysis of relative mRNA expression
levels.
| Gene | Species | Primer sequence
(5′→3′) |
|---|
| UII | Rat | F:
GGAGGAGCTGGAGAGGACTG |
|
|
| R:
GAGTCTCGGCACTGGGATCT |
| GPR14 | Rat | F:
AATGGCTCTAGGGTCCTCCT |
|
|
| R:
AACAGCCTCTGTGATGGACA |
| JAK2 | Rat | F:
TTTGGATCCCTGGATACATACCTGA |
|
|
| R:
TGGCACACACATTCCCATGA |
| STAT3 | Rat | F:
TTTGAGACAGAGGTGTACCACCAAG |
|
|
| R:
ACCACAGGATTGATGCCCAAG |
| MMP-2 | Rat | F:
GGACAGTGACACCACGTGACAA |
|
|
| R:
TTTCCAAAGTGCTGGCAGAATAGAC |
| TIMP-2 | Rat | F:
GACACGCTTAGCATCACCCAGA |
|
|
| R:
CTGTGACCCAGTCCATCCAGAG |
| Collagen I | Rat | F:
CCCTGCTGGAGAAGAAGGAA |
|
|
| R:
AGGAGAACCTTTGGGACCAG |
| Collagen III | Rat | F:
ACTGGTGAACGTGGCTCTAA |
|
|
| R:
GGACCTGGATGTCCACTTGA |
| β-actin | Rat | F:
CAGGCATTGCTGACAGGATG |
|
|
| R:
TGCTGATCCACATCTGCTGG |
Western blot analysis
Western blotting was conducted to evaluate cardiac
protein expression. Total protein was extracted from the heart
tissue using RIPA protein lysate (Beijing Solarbio Science &
Technology Co., Ltd.). Protein content was quantified using the
bicinchoninic acid Protein Concentration assay kit (Beijing
Solarbio Science & Technology Co., Ltd.). A total of 45 µg
protein/lane was separated via 8% SDS-PAGE and transferred to an
immobilon-P PVDF membrane, which was blocked with 5% skimmed milk
powder at 22±2°C for 1.5 h. Next, the membrane was incubated with
primary antibodies against UII (cat. no. orb352970; Biorbyt Ltd.),
GPR14 (cat. no. sc-514460; Santa Cruz Biotechnology, Inc.) and
p-STAT3 (cat. no. 9145; Cell Signaling Technology, Inc.) at a 1:800
dilution; JAK2 and STAT3 (cat. nos. 380903 and 310003; http://www.zen-bio.cn/; Zen Bioscience) at a 1:500
dilution; p-JAK2 (cat. no. ab32101; Abcam) and MMP-2/TIMP-2 (cat.
no. BS1236/1366; https://www.bioworlde.com/Search.aspx?keyword=1366&Category=233&x=7&y=10;
Bioworld Technology, Inc.) at a 1:1,000 dilution; collagen type
I/III (cat. no. bs-0578R/0548R; Bioss) at a 1:500 dilution; or
GAPDH (cat. no. bs-10900R; Bioss) at a 1:1,000 dilution at 4°C for
14–16 h. The membranes were washed with TBST (0.1% Tween-20;
Beijing Solarbio Science & Technology Co., Ltd.) three times
and then incubated with horseradish peroxidase-labeled goat
anti-rabbit or anti-mouse secondary antibodies (cat. no.
074-1056/074-1086; KPL, Inc.) at a 1:5,000 dilution at room
temperature for 1 h. Protein bands were visualized using a
hypersensitive ECL chemiluminescence kit (Beyotime Institute of
Biotechnology). The intensities of each protein band were analyzed
using Image-Pro Plus software (version 6.0; Media Cybernetics,
Inc.) with GAPDH as the loading control.
Statistical analysis
Data are expressed as the mean ± SEM of the mean of
≥3 independent experiments and were analyzed using SPSS software
(version 20; IBM Corp.). The serum index contents, and gene and
protein expression levels in each group of rats were analyzed by
one-way analysis of variance followed by Tukey's post hoc test.
Cardiac injury scores were analysed by Friedman followed by Nemenyi
post hoc test for multiple comparisons. GraphPad Prism (version 7;
GraphPad Software, Inc.) software was used to generate the charts.
P<0.05 was considered to indicate a statistically significant
difference.
Results
Assessing the rat model of AS
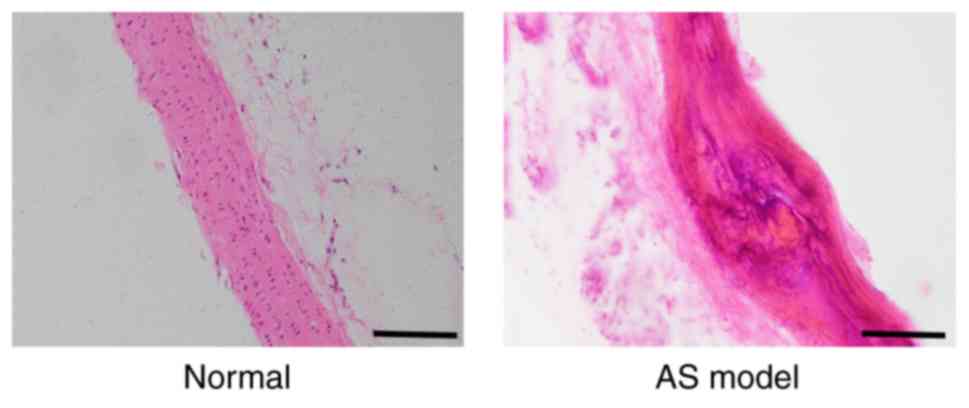
After 4 weeks, the thoracic aortas dissected from
rats in the AS model preparation group were found to contain
diverse characteristics typical of AS lesions, in contrast to the
thoracic aortas of rats in the normal control group. These
characteristics included: i) Intimal inflammatory cell
infiltration; ii) obvious calcification; iii) vascular smooth
muscle cell proliferation and disorder; iv) foam-like cell
formation; v) elastic fiber degeneration; and vi) rupture and
disintegration. The specific results from H&E staining are
presented in Fig. 2.
Blood lipid and
Ca2+levels
Compared with the levels in the normal group, the
serum TG, TC, LDL and Ca2+ levels in the AS model
preparation group were significantly increased, whereas HDL levels
were decreased. Furthermore, the serum TG, TC, LDL and
Ca2+ levels in the simvastatin and urantide groups were
obviously decreased, in contrast to the HDL content, which was
significantly increased. It was revealed that urantide and
simvastatin significantly improved blood lipid and Ca2+
levels in rats with AS. The specific results are displayed in
Table II.
 | Table II.Comparison of the levels of blood
lipid components and Ca2+ in the sera of atherosclerotic
and non-atherosclerotic rats. |
Table II.
Comparison of the levels of blood
lipid components and Ca2+ in the sera of atherosclerotic
and non-atherosclerotic rats.
| Group | TC (mmol/l) | TG (mmol/l) | HDL (mmol/l) | LDL (mmol/l) | Ca2+
(mmol/l) |
|---|
| Normal | 2.07±0.61 | 0.28±0.08 | 2.95±0.93 | 0.27±0.05 | 2.60±0.56 |
| AS model |
11.18±3.12a |
0.77±0.12a |
0.93±0.23a |
1.70±0.31a |
3.95±0.42a |
| Simvastatin |
4.06±1.51a,b |
0.41±0.12b,c |
2.16±0.35b,c |
0.77±0.19a,b |
3.63±0.13a,d |
| Urantide
treatment |
|
|
|
|
|
| 3 days |
7.52±1.59a,b,e |
0.55±0.20a,d,f |
1.48±0.37a,b,e |
1.05±0.31a,b,e |
3.46±0.32a,d |
| 7 days |
5.28±0.59a,b,f |
0.37±0.15b |
1.91±0.66a,d |
0.84±0.27a,b |
3.22±0.29a,b,f |
| 14 days |
8.33±1.43a,b,e |
0.59±0.21a,f |
1.02±0.44a,e |
1.27±0.27a,b,e |
3.68±0.30a |
Cardiac pathological changes in rats
with AS
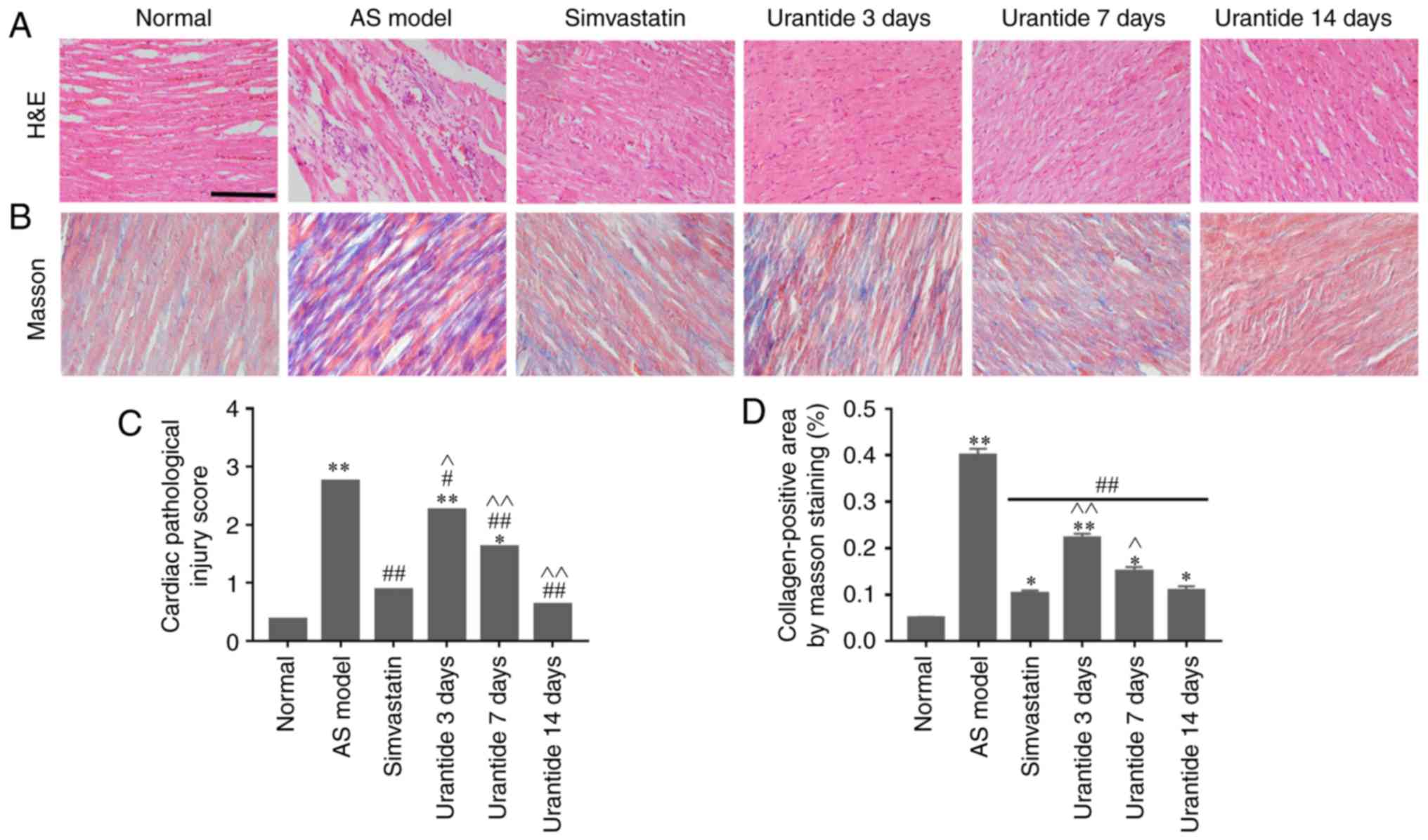
Morphological methods were employed to assess
AS-related cardiac damage and collagen metabolism. In the normal
group, neatly arranged myocardial fibers, oval-shaped and centered
nuclei, no atrophy or hypertrophy of the myocardial cells, and the
microscopic expression of collagen fibers were observed. By
contrast, the AS model preparation group exhibited cardiomyocyte
hypertrophy, interstitial fibrosis, increased neutrophil
infiltration between cells, scattered foam-like cell formation,
hyperemia and abundant fibers (Fig. 3A
and B). Furthermore, both cardiac damage scores and myocardial
collagen volumes were significantly higher in the AS model group
than in the control group (Fig. 3C and
D). Compared with the AS model group, the simvastatin and
urantide groups were shown to have significantly reduced
cardiomyocyte fibrosis and neutrophil infiltration, and lower
cardiac injury scores and myocardial collagen volumes. In addition,
these improvements were positively associated with treatment time
and the effect of 14-day urantide treatment was similar to that
observed in the positive control group.
Alterations in the expression levels
of genes and proteins in cardiac tissue
Molecular biology techniques were used to detect
gene and protein expression in cardiac tissue. Compared with that
in the normal group, the expression of UII, GPR14, JAK2, STAT3,
MMP-2 and collagen type I/III was higher in the cardiac tissue of
the AS model group, whereas TIMP-2 expression was lower.
Furthermore, the expression levels of UII, GPR14, JAK2, STAT3,
MMP-2 and collagen type I/III were downregulated in the cardiac
tissue of rats in the urantide groups compared with the AS model
group; however, TIMP-2 expression was upregulated (Fig. 4A and B). Most importantly, when the
rats with AS received treatment, the protein ratio of p-JAK2/JAK2,
p-STAT3/STAT3 and MMP-2/TIMP-2 was effectively improved as the
corresponding protein ratio decreased after urantide treatment
(Fig. 4Ba and C). Moreover,
improved myocardial collagen metabolism was positively associated
with the urantide treatment time and the effects of urantide were
similar to those of the positive control drug. The specific results
are shown in Fig. 4. However, the
protein ratio of p-JAK2/JAK2 fluctuated at different times of
urantide treatment, and the trend was consistent with serological
indicators. In addition, simvastatin had little effect on the
protein ratio of p-JAK2/JAK2 and p-STAT3/STAT3, as opposed to
urantide treatment. Therefore, the specific mechanism underlying
these effects require further study.
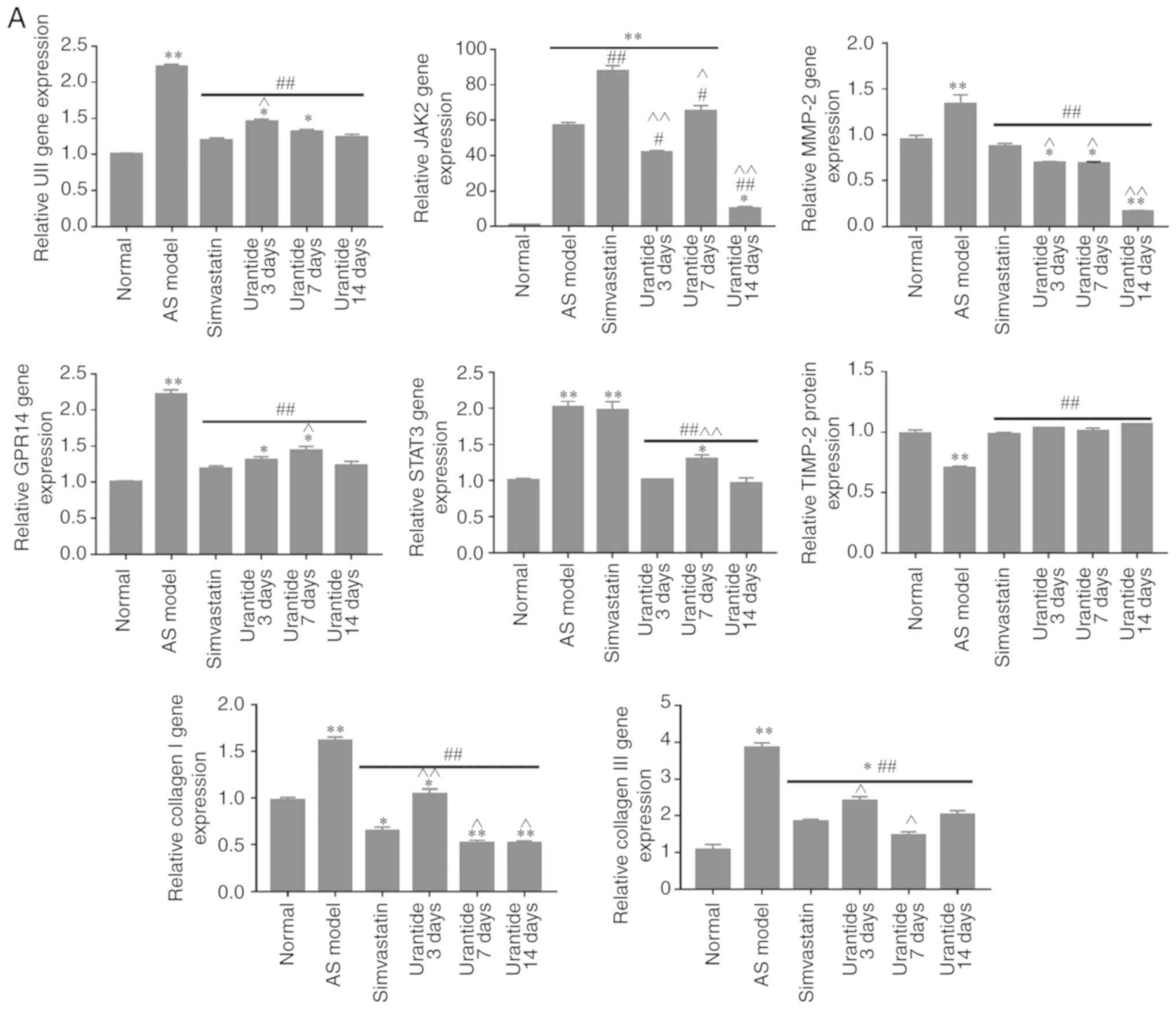 | Figure 4.Effect of urantide on UII/GPR14, the
JAK2/STAT3 pathway and collagen metabolism in the cardiac tissue of
rats with AS. Changes in the expression of the following genes and
proteins with increasing drug administration time: (A) relative
expression level of genes. Changes in the expression of the
following genes and proteins with increasing drug administration
time: (B-a) relative expression level of signaling pathway
proteins, (B-b) relative expression level of collagen metabolism
related proteins and (C) MMP-2/TIMP-2 protein ratio. *P<0.05,
**P<0.01 vs. the normal group; #P<0.05,
##P<0.01 vs. the AS model group;
^P<0.05, ^^P<0.01 vs. the simvastatin
group. Data are presented as the mean ± SEM (n=6–8 rats in each
group). AS, atherosclerosis; UII, urotensin II; G protein-coupled
receptor 14; JAK2, Janus kinase 2; p, phosphorylated; STAT3, signal
transducer and activator of transcription 3; MMP-2, matrix
metalloproteinase 2; TIMP-2, TIMP metallopeptidase inhibitor 2. |
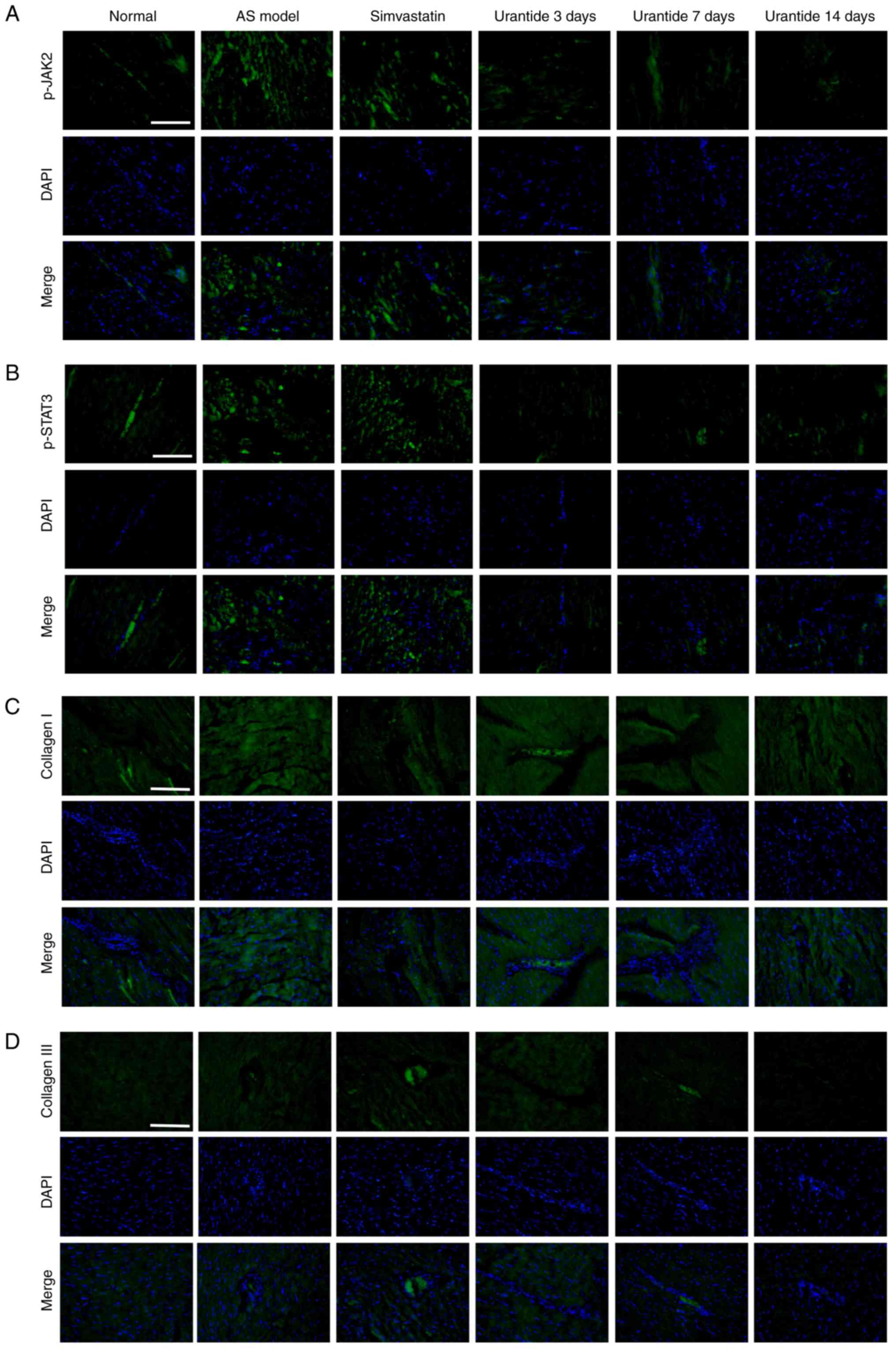
Localization of p-JAK2/p-STAT3 and
collagen type I/III expression in cardiac tissue
Localization of the p-JAK2/p-STAT3 and collagen type
I/III proteins was determined by immunofluorescence. The expression
of p-JAK2, p-STAT3, and collagen types I and III in the cardiac
tissue of rats in the AS model group was increased compared with
the normal group. In addition, vascular and myocardial
degeneration, and necrosis were identified in the AS model group
(Fig. 5). Compare with the AS
model group, the expression levels of p-JAK2, p-STAT3, collagen
types I and III were gradually restored in AS rats treated with
urantide, which mainly exhibited perivascular and myocardial
degeneration and necrosis. Moreover, this effect was positively
associated with treatment time.
Discussion
In the early stages of AS, type III collagen has
been reported to have important compensatory effects on cardiac
rearrangement and muscle bundle formation, which maintain the
normal function of he tissue in the early stage of the disease
(19,20). However, in the advanced stages of
AS, the accumulation of type I collagen in the myocardial
interstitium occludes vasodilation and blood flow (19,21).
It was hypothesized that the effective regulation of disordered
collagen metabolism may have important clinical significance in the
treatment of AS.
The results demonstrated significant hyperlipidemia
and myocardial hypertrophy, neutrophil infiltration, hyperemia and
hemorrhage in the cardiac tissue of rats with AS, accompanied by
abundant collagen. In addition, the UII/UT system in the cardiac
tissue of rats with AS was activated. Luo et al (22) found that UII induces the synthesis
of type I collagen fibers and promotes the occurrence of myocardial
fibrosis in rats. Previous studies performed by the same research
group have reported that urantide had a protective effect on the
thoracic aortas and livers of rats with AS following inhibition of
the UII/UT system (6,23). The possibility of urantide
treatment having a reparative effect on disordered collagen
metabolism caused by AS was further investigated in the present
study.
AS was shown to induce JAK2/STAT3 pathway activation
and MMP-2/TIMP-2 protein ratio imbalance, consequently causing
disordered collagen metabolism mainly due to increased collagen
type I/III expression. This finding is consistent with results from
studies on cardiac pathology and similar to the results of current
studies on myocardial fibrosis (24,25).
Ahn et al (26) reported
that the JAK2/STAT3 pathway may regulate MMP-2 expression, and
promote endometrial cell proliferation and migration. Furthermore,
it has been demonstrated that abnormal proliferation of cardiac
fibroblasts causes an imbalance in the MMP-2/TIMP-2 protein ratio,
leading to disordered collagen metabolism (27,28).
To investigate whether inhibition of the JAK2/STAT3 pathway would
ameliorate the symptoms of myocardial fibrosis, rats with AS were
treated with the peptide urantide.
Recent studies identified that contrast-enhanced
cardiac magnetic resonance imaging of patients with AS indicated
that individuals who had a history of cardiovascular events were
more likely to present with myocardial fibrosis than those who did
not (29,30). In the present study, disordered
collagen metabolism was significantly improved in rats with AS
following treatment. This effect exhibited significant time
dependence. To verify the mechanism of this effect, the UII/UT
system and the JAK2/STAT3 pathway were examined, and it was
determined that they had undergone significant changes. The results
demonstrated that urantide effectively inhibited the expression of
the UII/UT system and the JAK2/STAT3 pathway. Inhibition of the
JAK2/STAT3 pathway may be associated with alleviated symptoms of
myocardial fibrosis, as after urantide treatment the pathological
symptoms of the heart were alleviated, which is consistent with
reports from relevant studies (7,22).
It has been reported that simvastatin is capable of reducing
myocardial fibrosis by downregulating related proteins, including
transforming growth factor, MMP-2, MMP-9, TIMP-1 and TIMP-2
(31). Nevertheless, studies on
the relationship of simvastatin with the JAK2/STAT3 pathway are
limited. Importantly, simvastatin was not found to inhibit the
activation of the JAK2/STAT3 signaling pathway in the cardiac
tissue of rats with AS. The results from the experiment in the
present study are inconsistent with those observed following
administration of simvastatin alone for the treatment of cardiac
hypertrophy (32). To this end,
future studies should establish a rat model of myocardial fibrosis
to further explore the association of simvastatin with the
JAK2/STAT3 signaling pathway.
A recent study by Cho et al (33) indicated that the JAK2/STAT3 pathway
regulates MMP-2 expression, thus follow-up research was conducted
on collagen mechanisms, such as changes in the expression levels of
related MMPs and TIMPs after myocardial fibrosis. Another study by
Wang et al (25)
demonstrated that an imbalance in the MMP-2/TIMP-2 protein ratio
affected the synthesis and degradation of myocardial collagen. In
the present study, an increase in MMP-2 expression was observed in
rats with AS, whereas TIMP-2 expression was decreased. Treatment
with urantide for a prolonged administration time resulted in a
significant improvement in the MMP-2/TIMP-2 protein ratio. By
contrast, the expression levels of collagen type I/III tended to
decrease. The aforementioned findings indicated that the JAK2/STAT3
pathway affected the expression of collagen type I/III by
regulating the balance of MMP-2/TIMP-2, thereby alleviating the
symptoms of disordered collagen metabolism.
In addition, p-JAK2/p-STAT3 and collagen type I/III
were abundantly expressed in AS lesions. Urantide treatment led to
a decrease in the expression and range of these proteins. Moreover,
their localization indicated that the JAK2/STAT3 pathway may be
involved in the process of collagen metabolism.
In summary, the treatment of rats with AS with
urantide was able to relieve cardiac symptoms and also
significantly improve collagen metabolism. The underlying mechanism
responsible for these effects may be antagonization of the UII/UT
system and inhibition of the JAK2/STAT3 pathway by urantide. This
combined mechanism is capable of regulating the balance between
MMP-2/TIMP-2 and decreasing collagen type I/III expression. The
regulation of collagen metabolism was restored and, consequently,
the degree of myocardial fibrosis in rats with AS was reduced. In
addition, differences were identified in the gene and protein
expression levels of collagen I between the 3- and 7-day subgroups
receiving urantide treatment. These differences could be considered
an asynchronous phenomenon, with differences in expression time,
related to the processes of transcription and/or translation.
Regarding this matter, in-depth research should be conducted to
clarify the relevant mechanisms. However, whether the UII/UT system
directly affects the JAK2/STAT3 pathway and how this pathway
regulates collagen metabolism remains unclear. The main limitation
of the present study is the lack of in vitro cell
experiments examining how the UII/UT system affects the JAK2/STAT3
signaling pathway and collagen metabolism. Therefore, the
downstream genes regulated by the JAK2/STAT3 pathway that directly
or indirectly affect collagen metabolism should be studied to
further elucidate the mechanism by which the JAK2/STAT3 pathway
affects collagen metabolism.
Acknowledgements
Not applicable.
Funding
The present study was supported by the Hebei Youth
Talents Project (grant. no. Hebei[2016]9), the Hebei Provincial
Department of Education Outstanding Youth Fund Project (grant. no.
YQ2013005) and the Key Discipline Construction Projects in Hebei
Province (grant. no. Hebei[2013] 4).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author upon reasonable
request.
Authors' contributions
JZ, TW and XS designed the study. TW and XS
performed the experiments. HPC and KL performed the animal model
experiment. JZ, TW, XS, HC and KL analyzed the data. TW and XS
wrote the manuscript. All authors critically reviewed the
manuscript, and read and approved the final version of the
manuscript.
Ethics approval and consent to
participate
All animal procedures were ethically approved by the
Experimental Animal Care and Use Committee of Chengde Medical
University and were conducted in accordance with the National
Institutes of Health Guide for the Care and Use of Laboratory
Animals.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Istratoaie O, OfiTeru AM, Nicola GC, Radu
RI, Florescu C, Mogoant L and Streba CT: Myocardial interstitial
fibrosis-histological and immunohistochemical aspects. Rom J
Morphol Embryol. 56:1473–1480. 2015.PubMed/NCBI
|
|
2
|
Chen X, Tang Y, Gao M, Qin S, Zhou J and
Li X: Prenatal exposure to lipopolysaccharide results in myocardial
fibrosis in rat offspring. Int J Mol Sci. 16:10986–10996. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Ross B, McKendy K and Giaid A: Role of
urotensin II in health and disease. Am J Physiol Regul Integr Comp
Physiol. 298:R1156–R1172. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Leprince J, Chatenet D, Dubessy C,
Fournier A, Pfeiffer B, Scalbert E, Renard P, Pacaud P, Oulyadi H,
Ségalas-Milazzo I, et al: Structure-activity relationships of
urotensin II and URP. Peptides. 29:658–673. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Kiu H and Nicholson SE: Biology and
significance of the JAK/STAT signalling pathways. Growth Factors.
30:88–106. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Liu M, Li Y, Liang B, Li Z, Jiang Z, Chu C
and Yang J: Hydrogen sulfide attenuates myocardial fibrosis in
diabetic rats through the JAK/STAT signaling pathway. Int J Mol
Med. 41:1867–1876. 2018.PubMed/NCBI
|
|
7
|
Zhao L, Wu D, Sang M, Xu Y, Liu Z and Wu
Q: Stachydrine ameliorates isoproterenol-induced cardiac
hypertrophy and fibrosis by suppressing inflammation and oxidative
stress through inhibiting NF-κB and JAK/STAT signaling pathways in
rats. Int Immunopharmacol. 48:102–109. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
El Hajj EC, El Hajj MC, Voloshenyuk TG,
Mouton AJ, Khoutorova E, Molina PE, Gilpin NW and Gardner JD:
Alcohol modulation of cardiac matrix metalloproteinases (MMPs) and
tissue inhibitors of MMPs favors collagen accumulation. Alcohol
Clin Exp Res. 38:448–456. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Bai R, Yin X, Feng X, Cao Y, Wu Y, Zhu Z,
Li C, Tu P and Chai X: Corydalis hendersonii Hemsl. protects
against myocardial injury by attenuating inflammation and fibrosis
via NF-κB and JAK2-STAT3 signaling pathways. J Ethnopharmacol.
207:174–183. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhao J, Zhang SF, Shi Y and Ren LQ:
Effects of urotensin II and its specific receptor antagonist
urantide on rat vascular smooth muscle cells. Bosn J Basic Med Sci.
13:78–83. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Zhao J, Xie LD, Song CJ, Mao XX, Yu HR, Yu
QX, Ren LQ, Shi Y, Xie YQ, Li Y, et al: Urantide improves
atherosclerosis by controlling C-reactive protein, monocyte
chemotactic protein-1 and transforming growth factor-β expression
in rats. Exp Ther Med. 7:1647–1652. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Huang ZY and Yang PY, Almofti MR, Yu YL,
Rui YC and Yang PY: Comparative analysis of the proteome of left
ventricular heart of arteriosclerosis in rat. Life Sci.
75:3103–3115. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Jiao YB, Rui YC, Li TJ, Yang PY and Qiu Y:
Expression of pro-inflammatory and anti-inflammatory cytokines in
brain of atherosclerotic rats and effects of Ginkgo biloba extract.
Acta Pharmacol Sin. 26:835–839. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Gou SH, Liu BJ, Han XF, Wang L, Zhong C,
Liang S, Liu H, Qiang Y, Zhang Y and Ni JM: Anti-atherosclerotic
effect of Fermentum Rubrum and Gynostemma pentaphyllum mixture in
high-fat emulsion- and vitamin D3-induced
atherosclerotic rats. J Chin Med Assoc. 81:398–408. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Rezkalla S, Kloner RA, Khatib FG, Smith FE
and Khatib R: Effect of metoprolol in acure coxsackievirus B3
murine myocarditis. Am Coll Cardiol. 12:412–414. 1988. View Article : Google Scholar
|
|
16
|
Hayes AJ, Hughes CE and Caterson B:
Antibodies and immunohistochemistry in extracellular matrix
research. Methods. 45:10–21. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Li X, Li X, Luo R, Wang W, Wang T and Tang
H: Detection of KIT Genotype in Pigs by TaqMan MGB Real-time
quantitative polymerase chain reaction. DNA Cell Biol. 37:457–464.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Collier P, Watson CJ, van Es MH, Phelan D,
McGorrian C, Tolan M, Ledwidge MT, McDonald KM and Baugh JA:
Getting to the heart of cardiac remodeling; how collagen subtypes
may contribute to phenotype. J Mol Cell Cardiol. 52:148–153. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Lopez B, Gonzalez A, Hermida N, Valencia
F, de Teresa E and Diez J: Role of lysyl oxidase in myocardial
fibrosis: From basic science to clinical aspects. Am J Physiol
Heart Circ Physiol. 299:H1–H9. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Lopez B, Gonzalez A, Varo N, Laviades C,
Querejeta R and Diez J: Biochemical assessment of myocardial
fibrosis in hypertensive heart disease. Hypertension. 38:1222–1226.
2001. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Luo SY, Chen S, Qin YD and Chen ZW:
Urotensin-II Receptor antagonist SB-710411 protects rat heart
against ischemia-reperfusion injury via RhoA/ROCK pathway. PLoS
One. 11:e01460942016. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Zhao J, Yu QX, Kong W, Gao HC, Sun B, Xie
YQ and Ren LQ: The urotensin II receptor antagonist, urantide,
protects against atherosclerosis in rats. Exp Ther Med.
5:1765–1769. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Aboulhoda BE: Age-related remodeling of
the JAK/STAT/SOCS signaling pathway and associated myocardial
changes: From histological to molecular level. Ann Anat. 214:21–30.
2017. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Wang L, Li J and Li D: Losartan reduces
myocardial interstitial fibrosis in diabetic cardiomyopathy rats by
inhibiting JAK/STAT signaling pathway. Int J Clin Exp Patho.
8:466–473. 2015.
|
|
26
|
Ahn JH, Choi YS and Choi JH: Leptin
promotes human endometriotic cell migration and invasion by
up-regulating MMP-2 through the JAK2/STAT3 signaling pathway. Mol
Hum Reprod. 21:792–802. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Wang L, Xu YX, Du XJ, Sun QG and Tian YJ:
Dynamic expression profiles of MMPs/TIMPs and collagen deposition
in mechanically unloaded rat heart: Implications for left
ventricular assist device support-induced cardiac alterations. J
Physiol Biochem. 69:477–485. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Guo C and Piacentini L: Type I
collagen-induced MMP-2 activation coincides with up-regulation of
membrane type 1-matrix metalloproteinase and TIMP-2 in cardiac
fibroblasts. J Biol Chem. 278:46699–46708. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Ambale-Venkatesh B, Liu CY, Liu YC,
Donekal S, Ohyama Y, Sharma RK, Wu CO, Post WS, Hundley GW, Bluemke
DA and Lima JAC: Association of myocardial fibrosis and
cardiovascular events: The multi-ethnic study of atherosclerosis.
Eur Heart J Cardiovasc Imaging. 20:168–176. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Liu CY, Heckbert SR, Lai S,
Ambale-Venkatesh B, Ostovaneh MR, McClelland RL, Lima JAC and
Bluemke DA: Association of Elevated NT-proBNP with myocardial
fibrosis in the Multi-Ethnic study of atherosclerosis (MESA). J Am
Coll Cardiol. 70:3102–3109. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Xing XQ, Xu J, Lu XW, Huang Y and Zhu PL:
Effects of losartan and simvastatin on collagen content, myocardial
expression of MMP-2 mRNA, MMP-9 mRNA and TIMP-1 mRNA, TIMP-2 mRNA
in pressure overload rat hearts. Zhonghua Xin Xue Guan Bing Za Zhi.
37:887–891. 2009.(In Chinese). PubMed/NCBI
|
|
32
|
Al-Rasheed NM, Al-Oteibi MM, Al-Manee RZ,
Al-Shareef SA, Al-Rasheed NM, Hasan IH, Mohamad RA and Mahmoud AM:
Simvastatin prevents isoproterenol-induced cardiac hypertrophy
through modulation of the JAK/STAT pathway. Drug Des Devel Ther.
9:3217–3229. 2015.PubMed/NCBI
|
|
33
|
Cho HJ, Park JH, Nam JH, Chang YC, Park B
and Hoe HS: Ascochlorin suppresses MMP-2-mediated migration and
invasion by targeting FAK and JAK-STAT signaling cascades. J Cell
Biochem. 119:300–313. 2018. View Article : Google Scholar : PubMed/NCBI
|