Introduction
According to international literature data, a wound
is defined as a condition that disrupts the integrity of the
membranes (skin or mucosa), a physical trauma induced by factors,
such as cuts, abrasions or burns. Wounds that tend to become
chronic (microorganism origin) are a concern in developed
countries, as they are associated with high costs and a negative
impact on the quality of life of affected individuals. In
particular, biofilm formation is considered one of the most
critical factors in the chronicity of wounds (1). By forming a biofilm
(polysaccharide-based), microorganisms form a polymicrobial complex
structure that allows attachment to living and non-living surfaces,
and thus adhere to the wound surface (2). It has been determined that bacteria
able to develop a biofilm structure are more resistant to
antibiotics (3,4). Staphylococcus aureus, which is
responsible for the majority of nosocomial infections, is a
cocci-like non-encapsulated bacterium under a Gram-positive
coloration. As demonstrated below, the antibiotic susceptibility of
methicillin-resistant Staphylococcus aureus (MRSA) was determined
according to European Committee on Antimicrobial Susceptibility
Testing (EUCAST) criteria (5).
MRSA was sensitive to amikacin (30 µg/ml), fusidic acid (10 µg/ml),
gentamicin (10 µg/ml), levoflaxacin (5 µg/ml), linezolid (10
µg/ml), penicillin (1 µg/ml), trimethoprim sulfamethoxazole
(1.25+23.75 µg/ml) and it exhibited resistance to ciprofloxacin (5
µg/ml) (intermediate), erythromycin (30 µg/ml), clindamycin (2
µg/ml) and tetracycline (30 µg/ml).
Methicillin is an effective antibiotic used in the
treatment of Staphylococcus aureus; however, some strains are
methicillin-resistant (MRSA). MRSA infections are usually observed
in open wounds in hospitalized patients (6). Chronic biofilm-associated infections
caused by Staphylococcus aureus often lead to a significant
increase in morbidity and mortality rates, particularly when
associated with permanent medical devices (6,7).
Biofilm plays a role in the adhesion of microorganisms to a
surface. It is a layer of extracellular polymeric structures formed
by the microorganism, environmental organic and inorganic
substances and proteins. The biofilm formed by microorganisms
protects them from phagocytosis and antibiotics. Therefore, it
leads to sepsis and chronic infections. The icaA and icaD genes are
important in the biofilm layer in the structure of Staphylococcus
aureus. One of the proteins produced by the icaA and icaD genes,
the ‘biofilm-associated protein’ is one of the necessary structures
for the biofilm formation of Staphylococcus aureus (7). In addition, the presence of biofilms
on chronic wounds inducing community-acquired Staphylococcus aureus
has been reported as 78.2% in wound studies (8). Chronic wound biofilms represent a
significant treatment challenge by demonstrating recalcitrance
towards antimicrobial agents. In addition, the delayed wound
healing process caused by biofilm is one of the main reasons.
Staphylococcus aureus and its associated biofilm are among the
dominant causes of persistent infections in chronic wounds. After
MRSA attaches to cells, the biofilm develops into a ‘mat’ composed
of an extracellular DNA (eDNA) and proteinaceous matrix. After
reaching confluency, a period of cell mass egress occurs, in which
a subpopulation of cells is released from the biofilm via
nuclease-mediated eDNA degradation to allow the formation of
three-dimensional microcolonies consisting of different foci of
cells that remain attached during the exit phase. This stage is
characterized by rapid cell division, forming robust aggregates of
proteins, including phenol-soluble modulins and eDNA (9).
Therefore, in recent years, the increasing
antibiotic resistance, the increase in biofilm formation and
recurrent wounds cases have led to the search for alternative
compounds to stimulate/improve the outcomes of antibiotic
treatment. Recently, various antibacterial studies with boron and
boron compounds have attracted attention (10–14).
The ability of boron to form covalent bonds with
carbon renders it very useful in the drug discovery process.
Trivalent boron derivatives have a trigonal planar structure and
are electrophiles. By accepting a pair of electrons, they convert
in a tetrahedral configuration and become nucleophile agents. This
transformation explains the capacity of various boron derivatives
to inhibit a large array of enzymes (15,16). Bortezomib is a boronic acid
derivative approved by the FDA as an anticancer treatment, acting
as a proteasome inhibitor (17).
An alkaline type of boron, potassium metaborate, which is one of
the most critical boron compounds, is a solvent for casein and an
important additive in the fabrication processes for stainless steel
and other non-ferrous metals (18).
Boron compounds are used effectively especially in
vaginal yeast infections caused by dimorphic fungus Candida
albicans (19). It has been
reported that the application of 3% boric acid to deep wounds
significantly contributes to the healing cascade and the reduction
of hospital duration in intensive care units (20,21). Sodium pentaborate has been proven
to increase collagen deposition and favor wound contraction in
vitro, as well as to increase cell migration, superoxide dismutase
activity and the expression levels of gene associated with vital
wound healing (22). The same
formulation has been found to increase the healing of burn wounds
by increasing capillary density and fibroblastic activity (23,24). In light of all this information,
the present study aimed to examine the effects of boric acid and
potassium metaborate on the healing process of MRSA-derived wounds,
using a cell culture method. For the evaluation of the efficacy of
the test compounds, redox stress parameters, as well as
inflammation ones were employed.
Materials and methods
MRSA strain
Community-acquired MRSA bacteria were isolated from
a chronic non-healing wound sample which was sent to the Medical
Microbiology Laboratory of Ataturk University (Erzurum, Turkey).
The VITEK 2 system uses a fluorogenic methodology for organism
identification and a turbidimetric method for susceptibility
testing. MRSA bacteria isolated from a patient sample, for which
ethical approval was obtained from the Ataturk University Faculty
of Medicine Clinical Research Ethics Committee (decision date,
04.11.2021; decision no. 23; and meeting no. 07) was used in the
study. All necessary consents and permissions were obtained for the
patient samples used in the study. The ethics committee document
obtained from the authors' institution includes all consent forms.
The wound sample sent to the clinical microbiology laboratory was
evaluated as a community-acquired agent. The causes of this
(culture positivity outside the hospital or within the first 48 h
of hospitalization, no previous MRSA infection or colonization,
hospitalization over the past year, residing in a nursing home, no
surgery and indwelling catheter or crossing the skin, or the
absence of a medical device) were taken into account. Bacteria were
selected according to these criteria.
Reagents and chemicals. Boric acid, potassium
metaborate, Dulbecco's modified Eagle's medium (DMEM),
phosphate-buffered saline (PBS), fetal calf serum (FCS), antibiotic
antimitotic solution (×100), L glutamine, trypsin-EDTA,
paraformaldehyde and ethanol were obtained from MilliporeSigma.
Experimental design
The experiment was designed in two different parts:
The first part consisted of the evaluation of the boric acid (39,
78, 156, 312, 625, 1,250, 5,000 and 10,000 µg/ml) and potassium
metaborate (9.4, 18.75, 37.5, 75, 150, 300, 600, 1,200 and 2,400
µg/ml) minimal inhibitory concentration (MIC) and cell (fibroblast)
culture toxicity. The antibacterial effects of boric acid and
potassium metaborate were analyzed according to the recommendations
of the National Committee for Clinical Laboratory Standards (NCCLS)
(25). Community-acquired MRSA
bacteria were isolated from a chronic non-healing wound sample sent
to the Medical Microbiology Laboratory of Ataturk University (as
aforementioned). MRSA strains were used for the test. In
microbiology, the MIC is the lowest concentration of an
antimicrobial that inhibits the visible growth of a microorganism
following overnight incubation. MICs were defined as the lowest
concentration of boric acid and potassium metaborate inhibiting the
visible growth of the bacteria. The MICs of boric acid and
potassium metaborate were conventionally determined in triplicate,
for each bacterial strain by the microdilution broth method as
described by the NCCLS (25).
Serial dilutions of both boric acid and potassium metaborate were
prepared in microdilution with concentrations ranging between 10
mg/ml (40 mM) and 0.02 mg/ml (40 mM). 0.62 mg/ml potassium
metaborate and, 2.5 mg/ml boric acid showed minimal inhibition on
MRSA.
In the second step, a Methicillin resistant
Staphylococcus aureus wound model was induced, using a fibroblast
cell line; boric acid (1,250 µg/ml) and potassium metaborate (600
µg/ml) were applied for 24 h treatments. These concentrations were
preferred as these did not exhibit toxicity at these ranges. After
the end of experiment,
3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT)
assay, as well as total antioxidant capacity (TAC), total oxidant
status (TOS), glutathione reductase (Gr), lactate dehydrogenase
(LDH) and immunohistochemical analyses were performed (Fig. 1).
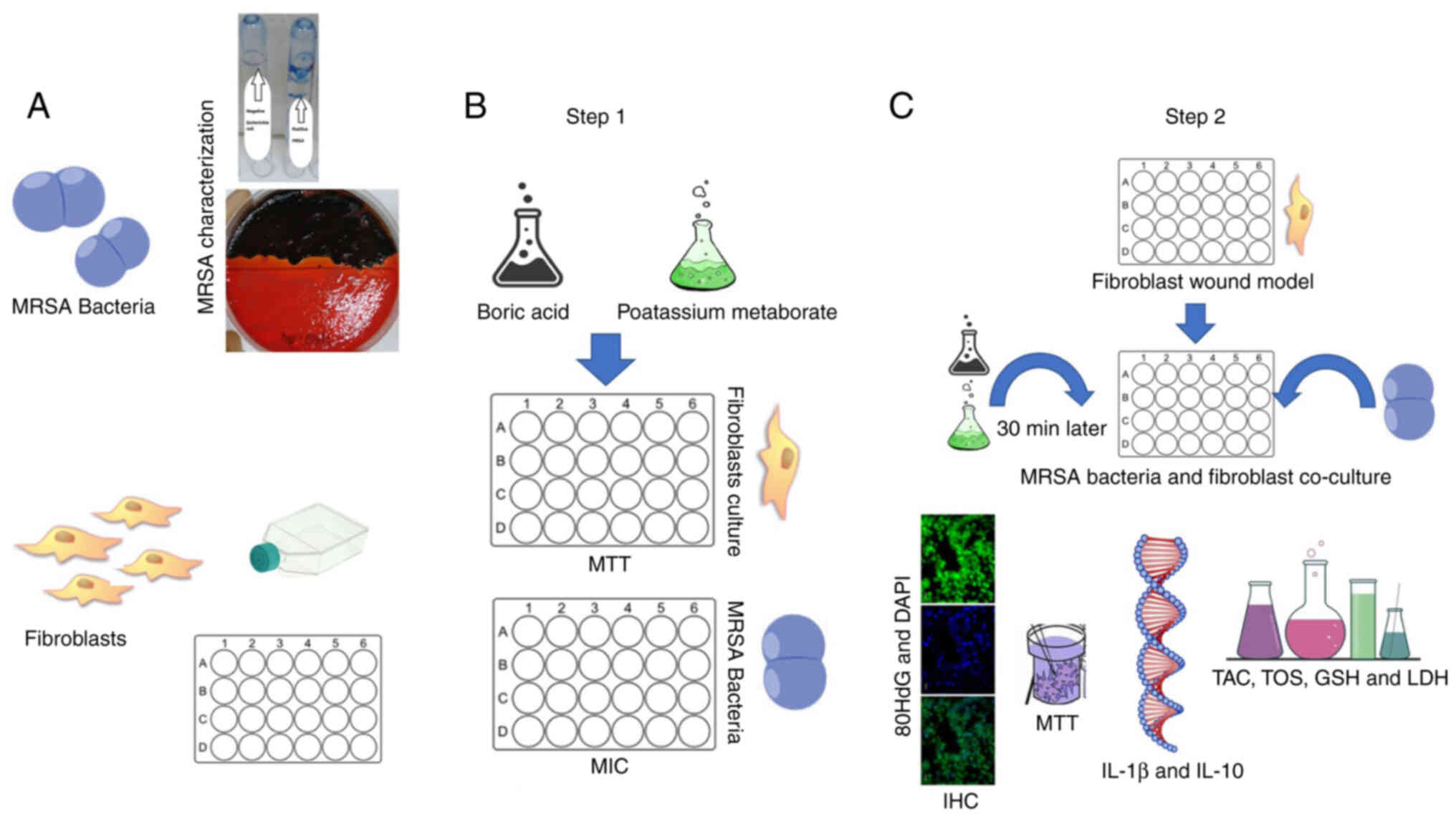 | Figure 1.Experimental design. (A) MRSA
bacterial characterization and fibroblast culture was made; (B)
Step 1: Boric acid (1,250 µg/ml) and potassium metaborate (600
µg/ml) toxicity tests for concentration and MRSA bacteria MIC were
assessed. (C) Step 2: Wound model was prepared than bacteria used
for co-culture and after 30 min the treatment were added; 24 h
later, MTT assay, TOS and TAC, LDH, Gr, immunofluorescence, and
IL-1β and IL-10 expression analyses were performed. MRSA,
methicillin-resistant Staphylococcus aureus; MIC, minimal
inhibitory concentration; TOS, total oxidant status; TAC, total
antioxidant capacity; LDH, lactate dehydrogenase; GSH,
glutathione. |
Cells and cell cultures
For the present study, fibroblast cell (L929,
CRL-6364, ATCC) cultures were obtained from the Department of
Medical Pharmacology of Ataturk University (Erzurum, Turkey).
Briefly, the cells were re-suspended in fresh medium
(DMEM), fetal bovine serum (FBS) 10% and antibiotic 1% (penicillin,
streptomycin and amphotericin B) (MilliporeSigma). The cells were
then seeded in 24 well plates (Corning, Inc.) and stored in an
incubator (5% CO2; 37°C), as previously described
(21). After obtaining 85%
confluency, the wound model was created using 100-µl yellow pipet
tip. According to the McFarland 0.5 scale, the bacterial suspension
was then added to the cell culture. After 30 min, treatment with
boric acid (1,250 µg/ml) and potassium metaborate (600 µg/ml) was
applied for 24 h.
MTT assay
At the end of the two parts of the experiment
(following 24 h of treatment with boric acid and potassium
metaborate), 10 µl MTT solution (MilliporeSigma) were added to each
well plate and the samples were incubated for 4 h; 100 µl DMSO
(MilliporeSigma) was incorporated into all wells to dissolve the
formazan crystals. The optical density of the solutions was read at
570 nm using a Multiskan™ GO microplate spectrophotometer (23).
The extraction buffer was considered as a blank and
the optical density in the control group (untreated cells) was
considered as 100% viability. The relative cell viability (%) was
calculated as (A570 of treated samples/A570 of untreated samples)
×100.
Evaluation of TOS and TAC
TOS and TAC (Rel Assay Diagnostics) evaluations were
performed on cell supernatants according to the manufacturer's
instructions (Multiskan™ GO microplate spectrophotometer).
For the TOS assay, the oxidants from the biological
sample oxidize the ferrous ion-chelator complex to ferric ion; the
ferric ions form a complex with a chromogen and the color intensity
is evaluated spectrophotometrically (530 nm), with calibration
being performed using hydrogen peroxide (Rel Assay
Diagnostics).
In the TAS assay, antioxidants in the cell medium
reduce the colored 2,2′-azino-bis(3-ethylbenzothiazoline-6-sulfonic
acid) (ABTS) (radical to colorless reduced ABTS form; the dynamics
of absorbance at 660 nm are associated with the total antioxidant
level in the sample). For calibration of the assessment, a stable
antioxidant standard solution (Trolox) (Rel Assay Diagnostics) was
used.
Gr and LDH assay
Glutathione plays a key role in oxidative stress and
Gr is responsible for maintaining the supply of reduced
glutathione. On the other hand, LDH plays a critical role in the
cell energy process and LDH assay is generally used to screen for
tissue damage. Supernatants stored at −80°C were used for the
evaluation of LDH (Elabscience), as well as Gr activities, using
commercial ELISA kits, according to the manufacturer indications
(cat. no. E-EL-R0026, Elabscience) The absorbance was measured
using a reader (Multiskan™ GO microplate spectrophotometer).
MRSA identification
Community-acquired MRSA bacteria were isolated from
a chronic non-healing wound sample which was sent to the Ataturk
University Medical Microbiology Laboratory and included in the
study. The sample was inoculated on 5% sheep blood, McConkey agar
and mannitol salt agar (MSA) (MilliporeSigma) media and incubated
at 37°C for 24–48 h. The transplanted plates were examined using
the Gram staining (MilliporeSigma) method as follows: i) Applying a
primary stain (crystal violet) (MilliporeSigma) to a heat-fixed
smear of a bacterial culture (1 min, 25°C); ii) the addition of
iodine, which binds to crystal violet and traps it in the cell (1
min, 25°C); iii) rapid decolorization with ethanol or acetone (10
sec, 25°C); iv) counterstaining with safranin (MilliporeSigma) (1
min at room temperature) (26) at
the end of the 48-h time point.
The distinction between the causative microorganism
and the contaminant of the growth was decided according to the
results of direct microscopic examination. At the same time,
Gram-stained preparations were prepared from the wound sample; ×100
objective microorganism morphology was evaluated under a light
microscope (Leica DM300; Leica Microsystems GmbH). The MRSA strain
was detected by appropriate conventional tests.
Determination of microorganism
antibacterial susceptibility
The automated system VITEK 2 (bioMérieux) was used.
The VITEK 2 system uses a fluorogenic methodology for organism
identification and a turbidimetric method for susceptibility
testing. Available test kits include Gram-negative Bacillus
identification, Gram-positive cocci identification, Gram-negative
susceptibility and Gram-positive susceptibility; sensitivities were
interpreted according to EUCAST criteria (5).
Kirby-Bauer disk diffusion method
MRSA colonies, which were cultured for 24 h, were
inoculated into Mueller-Hinton medium (MilliporeSigma) with a swab
after adjusting the appropriate turbidity in sterile saline with
the McFarland 0.5 chart. Subsequently, Sterile Paper discs (6 mm in
diameter; Oxoid Antibacterial Susceptibility Blank Test Disc, Oxoid
Limited) were impregnated with 20 µg/ml and placed in
Mueller-Hinton medium. Zone diameters were measured following 24 h
and 37°C of incubation.
Determination of the MIC
The antibacterial effects of boric acid and
potassium metaborate were analyzed according to the recommendations
of the NCCLS (25). MRSA strains
were used for the test.
The MICs of boric acid and potassium metaborate were
conventionally determined in triplicate for each strain by the
microdilution broth method as described by the NCCLS (25). Serial dilutions of both boric acid
and potassium metaborate were prepared in microdilution with
concentrations ranging between 10 mg/ml (40 mM) and 0.02 mg/ml (40
mM). These concentration ranges were determined by experimentation
and by Yılmaz (27). Due to the
lack of sufficient resources in the literature, the appropriate
concentration range was determined as done in the present study.
The concentration ranges have been previously described by Yılmaz
(27). MRSA colonies prepared
according to the McFarland 0.5 scale with serial dilutions were
inoculated to all wells as 100 µl. Subsequently, 100 µl tryptic soy
broth (TSB) (MilliporeSigma) medium and a solution of boric acid
and potassium metaborate were added to the wells by dilution. The
last two wells consisted of the positive control containing the
microorganism and medium, and the negative control containing the
medium and boron derivatives. The samples were incubated for 24 h
at 37°C. MIC values were determined depending on the formation of
agglutination.
Biofilm evaluation using the
microplate method
The MRSA strain was incubated in TSB medium at 37°C
for 18–24 h. Bacterial suspensions were prepared by standardizing
them according to the McFarland 0.5 chart; 100 µl were added to the
flat-bottomed wells and incubated at 37°C for 24 h. At the end of
the incubation period, the wells were washed with distilled water
and the cell residues associated with the biofilm were stained with
1% crystal violet (MilliporeSigma) for 37°C for 15 min. Biofilms
observed in bacteria were photographed after the excess dye was
washed off with water. To quantitatively determine biofilm
formation, optical densities were measured on an ELISA reader
(Biotek ELX800; BioTek Instruments, Inc.) at OD 450 - OD 630 nm.
During the test, sterile TSB was used as a negative control. The E.
coli ATCC 25922 bacterial strain obtained from Ataturk University
Medical Faculty Medical Microbiology Laboratory was used as a
negative control.
Biofilm evaluation using the tube
method
A single colony was taken from MRSA pure cultures,
inoculated into 5 ml TSB medium containing 0.25% glucose, and
incubated at 37°C for 24 h. Subsequently, the tube contents were
emptied and kept at room temperature for 30 min with 1% saffron
(MilliporeSigma) solution. At the end of this period, the dye was
poured, and the tubes were washed twice with sterile PBS. The tubes
were inverted and allowed to dry on blotting paper. The following
day, the evaluation was performed (+), (++), (+++) and (−)
according to the formation and density of a colored film layer on
the inner surface of the tube. The E. coli bacterial strain was
used as a negative control. All tests were performed as three
repetitions, as previously described (22).
Biofilm evaluation using the Congo red
agar method
Congo red medium was prepared to contain 50 g
sucrose, 37 g brain heart infusion (BHI) agar (MilliporeSigma) and
0.8 g Congo red (MilliporeSigma) per liter. Following inoculation
on MRSA Congo red agar, incubation was performed at 37°C for 24 h.
As a result of incubation, the strains forming dry crystallized
black colonies were evaluated as biofilm-positive, and the strains
forming red or pink colonies were evaluated as biofilm-negative.
The E. coli bacterial strain was used as a negative control. This
experiment was studied in two repeats; three methods are used to
determine the presence of in vitro biofilm in the microbiological
analysis. The presence of biofilm was detected using in vitro
methods, as previously described (22).
RNA isolation and cDNA synthesis
The RNA of cells was isolated using the High Pure
RNA Isolation kit (cat. no. 11828665001, E.Z.N.A.®;
Roche Diagnostics). The RNA concentration was measured using a
NanoDrop 2000c Spectrophotometer (Thermo Fisher Scientific, Inc.).
RNA samples for cDNA were performed using the Transcriptor First
Strand cDNA Synthesis kit (cat. no. 04896866001, Roche Diagnostics)
according to the specified protocol (28).
Quantitative PCR (qPCR)
qPCR was performed using primers constructed for
IL-1β, IL-10 and β-actin. Briefly, 1 µl Primer Probe mix, 3 µl of
cDNA, 3 µl of Fast Start Essential DNA Probes Master mix (Roche
Diagnostics) and 13.25 µl distilled water were added to each tube
to be used (final volume is 20 µl). The PCR cycling conditions were
as follows: 5 min at 95°C, 10 sec at 95°C and 30 sec at 60°C,
covering a period of 45 cycles. The results were calculated by
calculating the 2−ΔΔCq values (22). The primers used were as follows:
β-actin forward, 5′-ATGGATGACGATATCGCTGCG-3′ and reverse,
5′-CTAGAAGCACTTGCGGTGCA-3′; IL-1β forward,
5′-ATGGCAACTGTTCCTGAACT-3′ and reverse,
5′-TTAGGAAGACACAGATTCCAT-3′; and IL-10 forward,
5′-ATGCCTGGCTCAGCACTGC-3′ and reverse,
5′-TTAGCTTTTCATTTTGATCATCA-3′.
Immunofluorescence analysis
The cells cultivated in cell culture were incubated
at room temperature for 30 min in paraformaldehyde solution. The
cells were then maintained in 3% H2O2 for 5
min; 0.1% Triton-X solution was then dripped onto the cells washed
with PBS and maintained for 15 min. After the incubation period,
protein blocks were dripped onto the cells and kept in the dark for
5 min. The primary antibody (8-OHdG; dilution ratio, 1/100; cat.
no. sc-66036, Santa Cruz Biotechnology, Inc.) was then dropped and
incubated at room temperature for 30 min in accordance with the
instructions for use. Immunofluorescence secondary antibody was
used as a secondary marker (FITC; dilution ratio, 1/500; cat. no.
ab6785, Abcam) and kept in the dark for 45 min (room temperature).
Subsequently, DAPI with mounting medium (dilution ratio, 1/200;
cat. no. D1306, MilliporeSigma) was dripped onto the sections and
kept in the dark for 5 min (room temperature), and the sections
were closed with a coverslip. The stained sections were examined
under a fluorescence microscope (Zeiss Axio; Zeiss AG).
Statistical analysis
The results were calculated as the mean ± standard
error. Statistical comparisons between groups were performed using
one-way ANOVA with Tukey's HSD test. For statistical analyzes, all
calculations were performed using SPSS 20 software (IMP Corp.). A
value of P<0.05 was considered to indicate a statistically
significant difference in all tests. In order to determine the
intensity of positive staining from the images obtained as a result
of the dyeing; five random areas were selected from each image and
evaluated in the ZEISS Zen Imaging Software program (Blue edition)
(Zeiss AG). Data were statistically defined as the mean and
standard deviation (mean ± SD) for % area. The one-way ANOVA test
(Fig. 8) was performed to compare
positive immune-reactive cells and immune-positive stained areas
with the healthy controls. As a result of the test, a value of
P<0.05 was considered to indicate a statistically significant
difference.
Results
Cell viability
The evaluation was performed in two steps. In the
first step, the toxicological effects of boric acid and potassium
metaborate on the fibroblast cell line were evaluated. In the
second step, the effects of the MIC on the fibroblast cell line
were determined. In the present study, after the cells reached the
appropriate density (80%), MRSA bacteria were added to the wound
line. After 30 min, boric acid and potassium metaborate were added
to the culture and the results of cell viability assay after 24
hours were determined (Figs. 2
and 3).
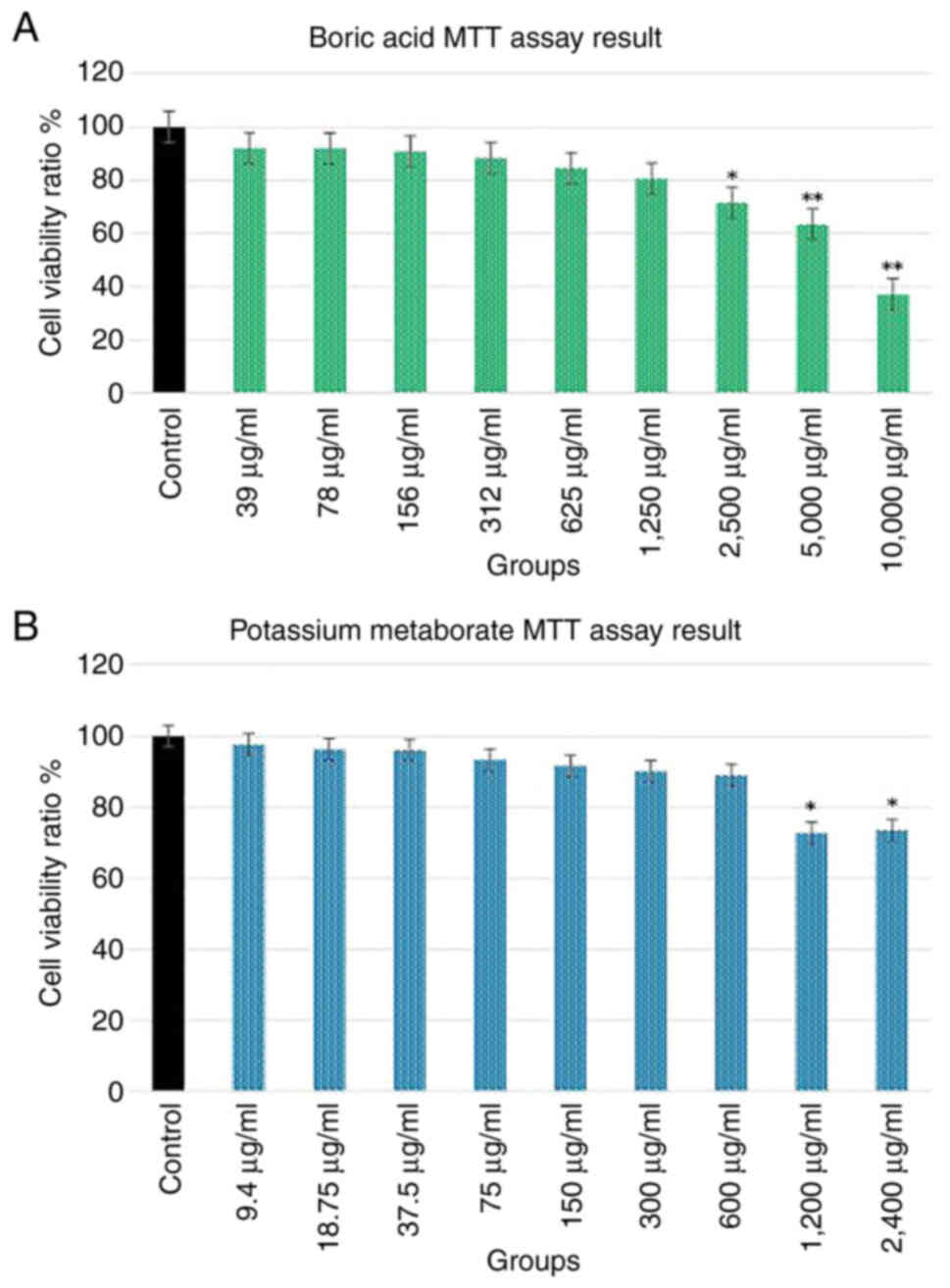
According to the results obtained, cell viability
decreased significantly with either boric acid (2,500 to 10,000
µg/ml) and potassium metaborate (1,200 and 2,400 µg/ml) (Fig. 2).
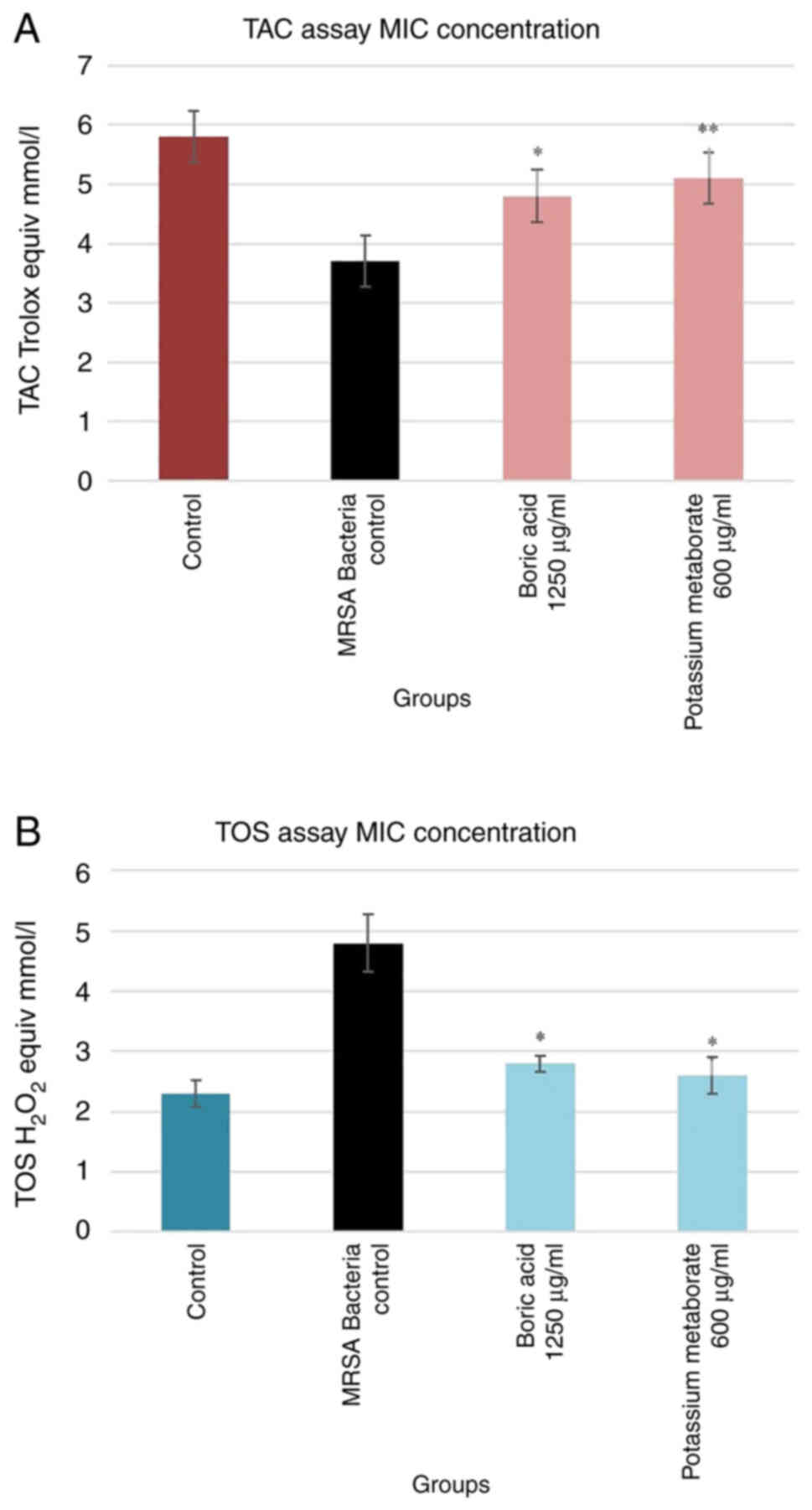
TAC and TOS in the wound model
The results revealed that there was a significant
difference between boric acid and potassium metaborate in both the
TAC and TOS assays compared to the bacteria control group.
Potassium metaborate was more effective (0.3 trolox equiv/mmol/l)
than boric acid concerning its antioxidant capacity; the oxidant
status was similar (Fig. 4).
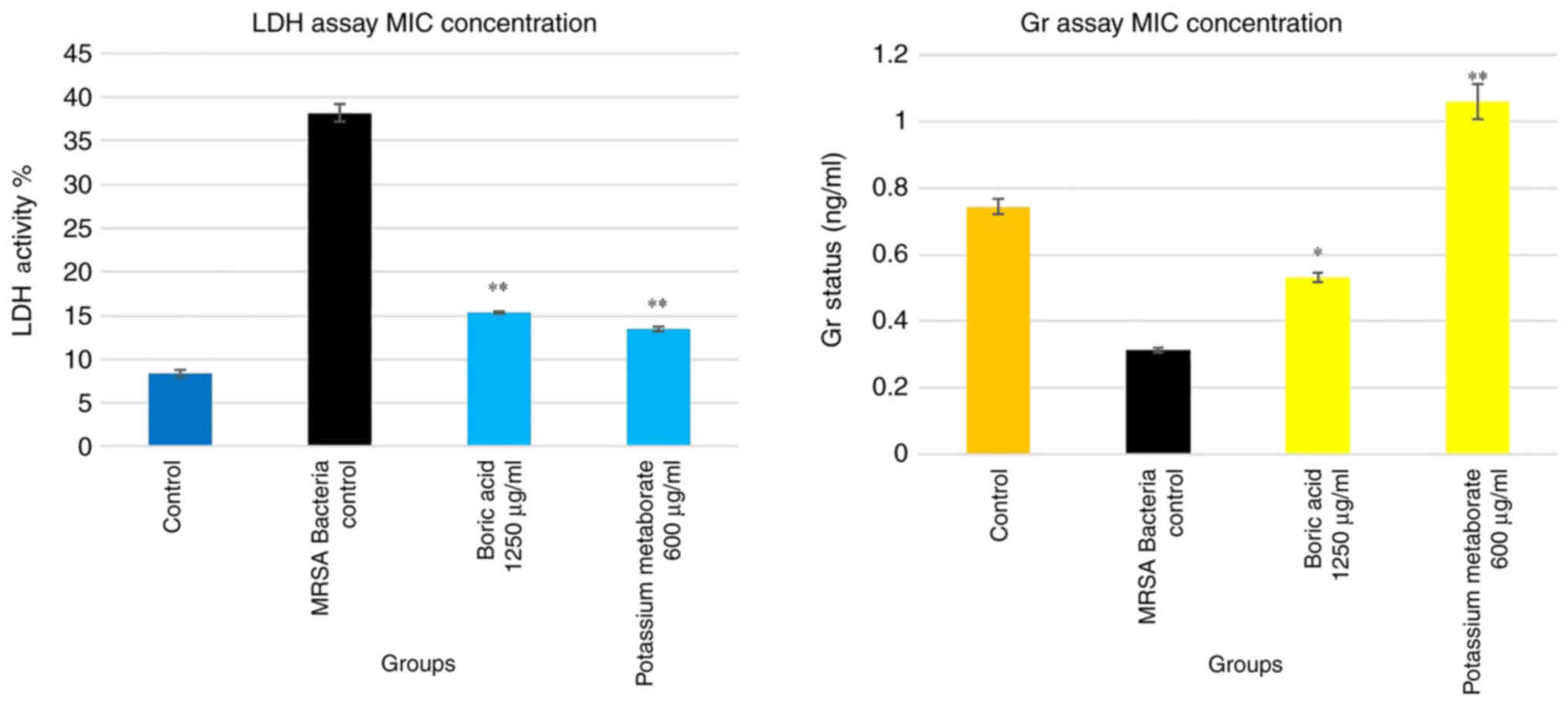
LDH and Gr concentrations in the wound
model
LDH can be used as a marker of cell death, and Gr
marker is a critical molecule in resisting in oxidative stress
(Fig. 5). The MRSA control group
exhibited an LDH level up to 7- and 2-fold higher than that of the
control and treatment groups, respectively. In addition, boric acid
and potassium metaborate reduced the LDH level to a value similar
to that obtained for the control group (the percentage of LDH
activity was measured by the ratio [absorbance of the
sample/absorbance of maximum activity) ×100 (25)]. The results of Gr assay revealed
that MRSA decreased the Gr level compared to the control group
(26). Potassium metaborate
increased the Gr status more effectively (2-fold greater) than
boric acid. Although the Gr level increased with boric acid, this
increase was not as prominent as that observed in the control group
(Fig. 5).
Antibiotic susceptibility
The antibiotic susceptibility results obtained from
the automated system VITEK 2 device were interpreted according to
the EUCAST criteria (5). The
susceptibility to all antibiotics is presented in Table I.
 | Table I.Antibiotic susceptibility. |
Table I.
Antibiotic susceptibility.
| Antibiotic | S | I | R |
|---|
| Amikacin (30
µg/ml) | X |
|
|
| Erythromycin (30
µg/ml) |
|
| X |
| Fusidic acid (10
µg/ml) | X |
|
|
| Gentamicin (10
µg/ml) | X |
|
|
| Clindamycin (2
µg/ml) |
|
| X |
| Levofloxacin (5
µg/ml) | X |
|
|
| Linezolid (10
µg/ml) | X |
|
|
| Penicillin (1
µg/ml) | X |
|
|
| Ciprofloxacin (5
µg/ml) |
| X |
|
| Tetracycline (30
µg/ml) |
|
| X |
| Trimethoprim
sulfamethoxazole | X |
|
|
| (1.25+23.75
µg/ml) |
|
|
|
The antibiotic susceptibility of the MRSA bacteria
was determined according to the EUCAST criteria. According to these
criteria, the bacteria were sensitive to amikacin (30 µg/ml),
fusidic acid (10 µg/ml), gentamicin (10 µg/ml), levoflaxacin (5
µg/ml), linezolid (10 µg/ml), penicillin (1 µg/ml), trimethoprim
sulfamethoxazole (1.25 +23.75 µg/ml) and ciprofloxacin (5 µg/ml)
(intermediate), and were resistant to erythromycin (30 µg/ml),
clindamycin (2 µg/ml) and tetracycline (30 µg/ml).
Kirby-Bauer disk diffusion method
results
Sterile Paper discs (6 mm in diameter, Oxoid
Antibacterial Susceptibility Blank Test Disc) were impregnated with
20 µg/ml and placed in Mueller-Hinton medium. Zone diameters were
measured following 24 h of incubation. After 24 h of incubation
according to the Kirby-Bauer disk diffusion results, boric acid
formed a 25 mm diameter zone, while potassium metaborate formed a
12 mm diameter zone in the antibiogram for MRSA. The generated zone
diameter sensitivities are presented in Table II and Fig. 6. The MRSA bacteria were found to
be sensitive to boric acid (20 µg/ml), and to exhibit resistance to
potassium metaborate (20 µg/ml).
 | Table II.Boric acid and potassium metaborate
susceptibility. |
Table II.
Boric acid and potassium metaborate
susceptibility.
| Boron
compounds | S | I | R |
|---|
| Boric acid (20
µg/ml) | X |
|
|
| Potassium
metaborate (20 µg/ml) |
|
| X |
MIC values of boron compounds
The final concentration of the boron compounds was
determined as 20 mg/ml. The MIC values were measured by dilution
(20–0.039 mg/ml) from the solution. As a result of the dilution, it
was determined that potassium metaborate (0.62 mg/ml) and boric
acid (2.5 mg/ml) inhibited the growth of bacteria. Boron compounds
exhibited an effect on bacteria in these value ranges.
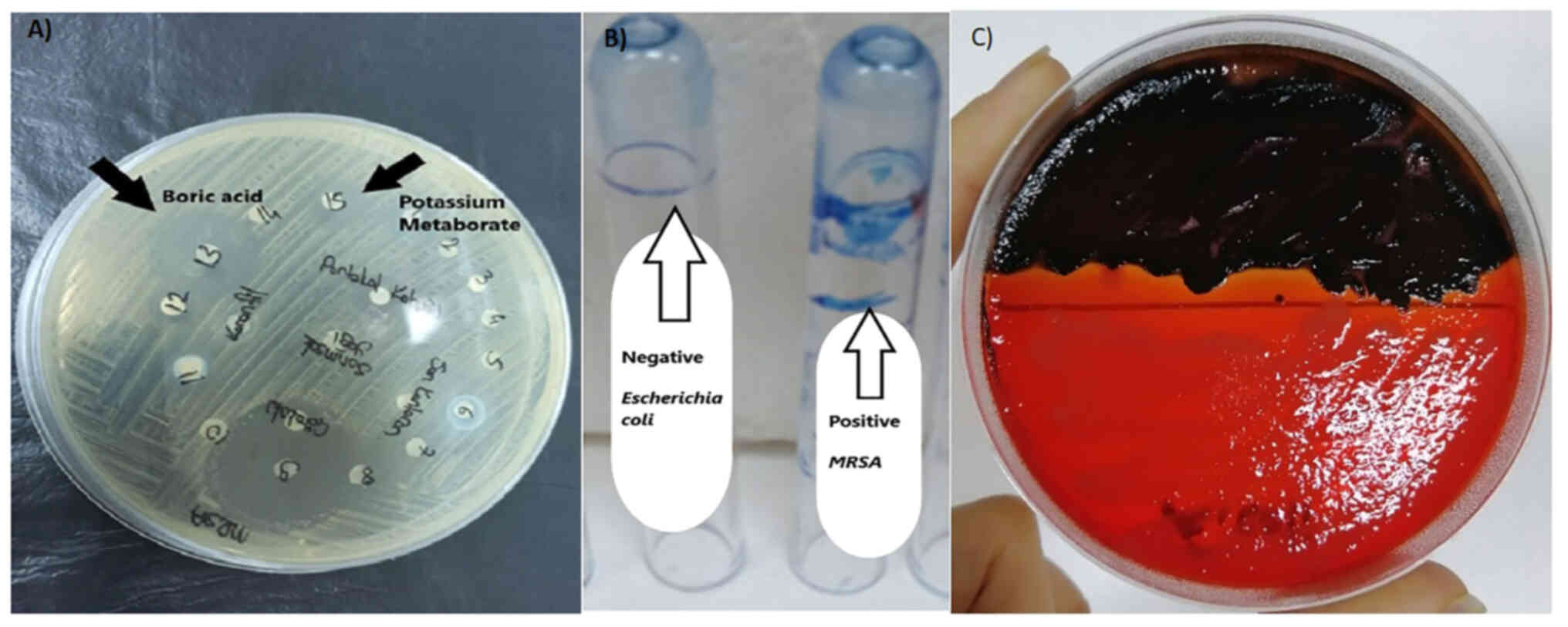
Biofilm assay
Three tests are used to detect the presence of
biofilm as follows: In the tube test, the presence of biofilm was
detected by residues of the safranin solution. MRSA cones treated
with 1% safranin solution were evaluated as strong positive (+++)
according to the formation and density of a colored film layer on
the inner surface of the tube. The biofilm feature in the tube test
is illustrated in Fig. 6.
To quantitatively determine biofilm formation, the
optical densities of microplates with ELISA wells were measured at
OD 450 - OD 630 OD nm using an ELISA reader. During the test,
sterile TSB was examined and evaluated as a negative control. As
regards the use of boric acid on the MRSA colonies, the absorbance
values were established at a wavelength of 0.315 nm and at a
wavelength of 0.131 nm for potassium metaborate. As a negative
control, the OD value was determined as 0.045 nm in E. coli
(Tables III and IV).
 | Table III.The results of the biofilm feature of
MRSA with the three methods. |
Table III.
The results of the biofilm feature of
MRSA with the three methods.
| Microorganism
type/method | Tube test
method | Microplate
method | Congo red agar
method |
|---|
| MRSA | (+++) | 0.315 nm | Dry crystallized
black colony |
| Escherichia coli
ATCC 25922 | (−) | 0.045 nm | White/Pink
Colony |
 | Table IV.OD values of MRSA boric acid and
potassium metaborate. |
Table IV.
OD values of MRSA boric acid and
potassium metaborate.
| Microorganism
type/compound | OD value | Positive
control | Negative
control |
|---|
| MRSA/Boric
acid | 0.315 nm | 0.255 nm | 0.216 nm |
| MRSA/Potassium
metaborate | 0.131 nm | 0.106 nm | 0.11 nm |
| Escherichia coli
ATCC 25922/Boric acid | 0.045 nm | 0.101 nm | 0.048 nm |
| Escherichia coli
ATCC 25922/Potassium metaborate | 0.060 nm | 0.075 nm | 0.063 nm |
Strains that formed dry crystalline black colonies
on the surface of the medium as a result of incubation were
evaluated as biofilm-positive. The results of the three methods
applied to the MRSA colonies are presented in Table III. In addition, morphological
images in Congo red medium are illustrated in Fig. 6. The E. coli colony was cultivated
as a negative control (Tables
III and IV).
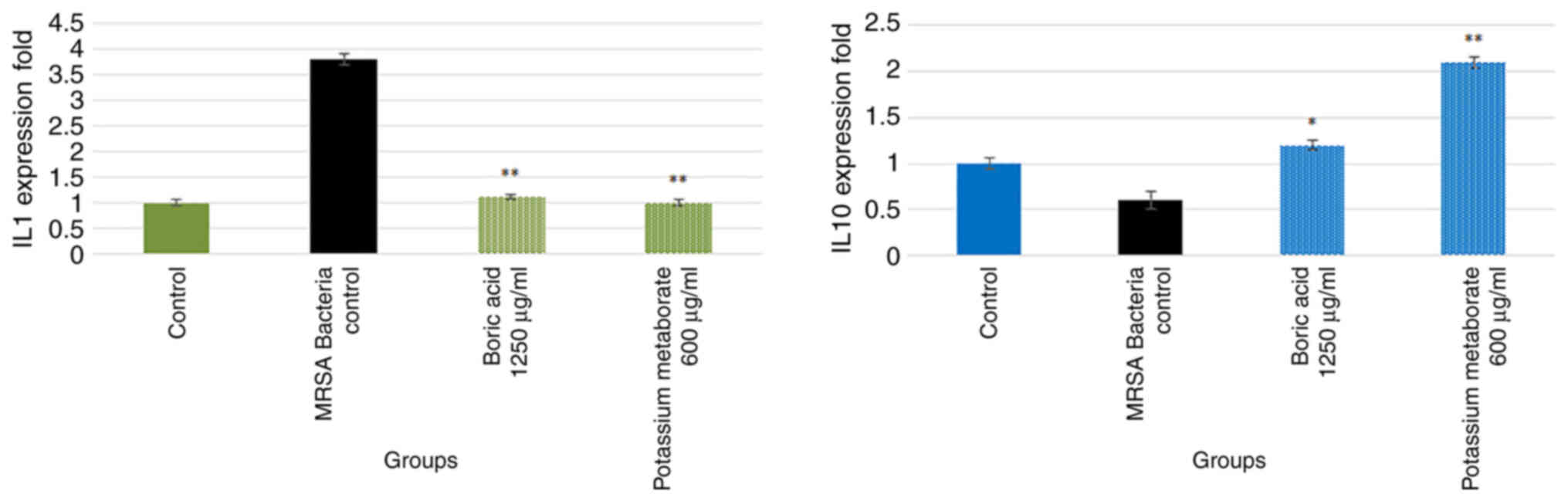
IL-1β and IL-10 gene expression
IL-1β levels were determined as a marker of
inflammation and IL-10 levels were determined as it has
anti-inflammatory properties (Fig.
7). The results revealed an almost 4.5-fold increase in the
levels of IL-1β in the bacteria group compared to the control
group. However, treatments with boric acid and potassium metaborate
significantly reduced IL-1β expression (P<0.001). In addition,
the IL-110 level decreased in the bacteria group by almost
0.2-fold; treatment with boric acid increased IL-10 expression
level to levels similar to those of the control group. However,
potassium metaborate increased the IL-10 expression level by almost
1-fold compared to the bacteria control group (Fig. 7).
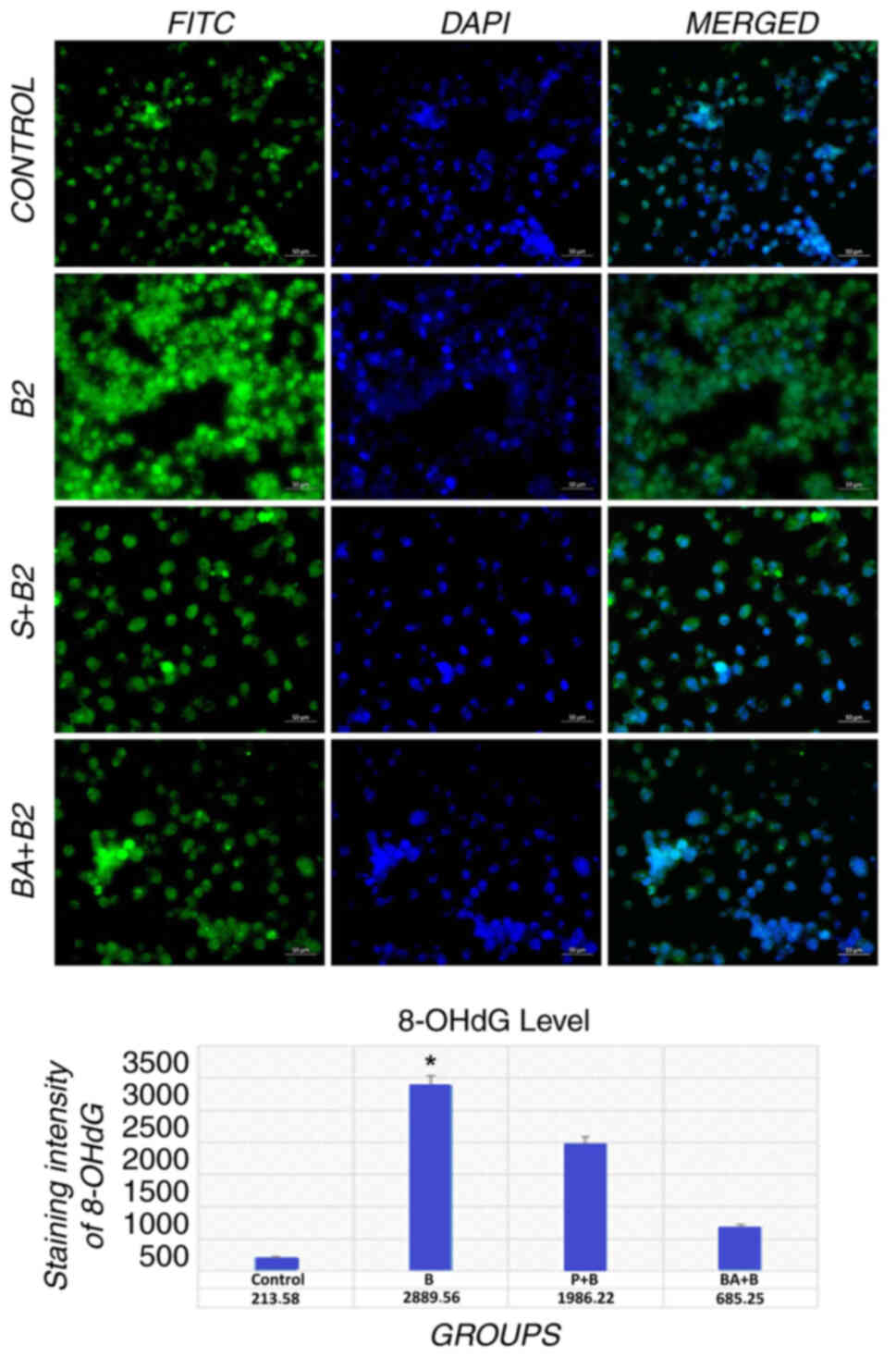
Immunohistochemical evaluation
In mitochondrial and nuclear DNA,
8-hydroxy-2′-deoxyguanosine is the predominant form of free
radical-induced oxidative lesions, and thus, it serves as a marker
of oxidative stress (23). In
line with the previous findings (MTT and LDH test), a significant
concentration-dependent increase in the 8-OHdG fluorescent signal
was observed in the bacteria control group (Fig. 8).
These results further support the data related to
the oxidant abilities of MRSA bacteria already observed in TAS and
TOS assays, demonstrating how boric acid and potassium metaborate
are able to reduce 8-OHdG, as one of the major products of DNA
oxidation and, consequently, of DNA damage accumulation and
fibroblast cell death. In particular, a mild-moderate fluorescence
signal intensity was observed with boric acid compared to potassium
metaborate, while marked signal intensities were observed in the
bacteria control group (Fig. 8)
(29,30).
Discussion
MRSA strains have begun to exhibit multi-drug
resistance with their biofilm structure and virulence factors. This
situation causes problems in treatment protocols with conventional
antibiotics, forcing the elimination of MRSA infections (24). The World Health Organization (WHO)
categorized MRSA strains as a high priority pathogen in 2017
(31). MRSA is the most
frequently isolated agent in wound samples, particularly from
diabetic foot wound samples. The higher antibiotic concentration
(almost 100-fold) of vancomycin and gentamicin used has been shown
to prevent the penetration of antibiotics by acting on the biofilm
(32,33). As a result of this situation, it
is important to investigate molecules to prevent biofilm formation.
Thus, in the present study, the antibacterial effects of boron
compounds (potassium metaborate and boric acid) were evaluated
(34).
In the present study, 600 µg/ml potassium metaborate
and 1,250 µg/ml boric acid exhibited a minimal inhibition of MRSA
as a result of dilution with the final concentration of 20 mg/ml
boron compounds. Yılmaz (27)
found the MIC value of 3.80 mg/ml when examining the effect of
boric acid and borax on the S. aureus ATCC 25923 strain. Similarly,
Sayın et al (35) found that the
MIC value of 3.09 mg/ml when examining the antibacterial and
biofilm effects of boric acid on the S. aureus ATCC 25923 strain.
When common boric acid was compared in the present study, the
closest MIC value was found. In the present study, dry black
colonies were observed in Congo red medium. Tge OD value was
determined at 0.315 and 630 nm using an ELISA reader in tube test
(+++) and microplate method.
The inhibition concentration of boron derivatives
was applied to the bacteria contaminated wound model (fibroblast
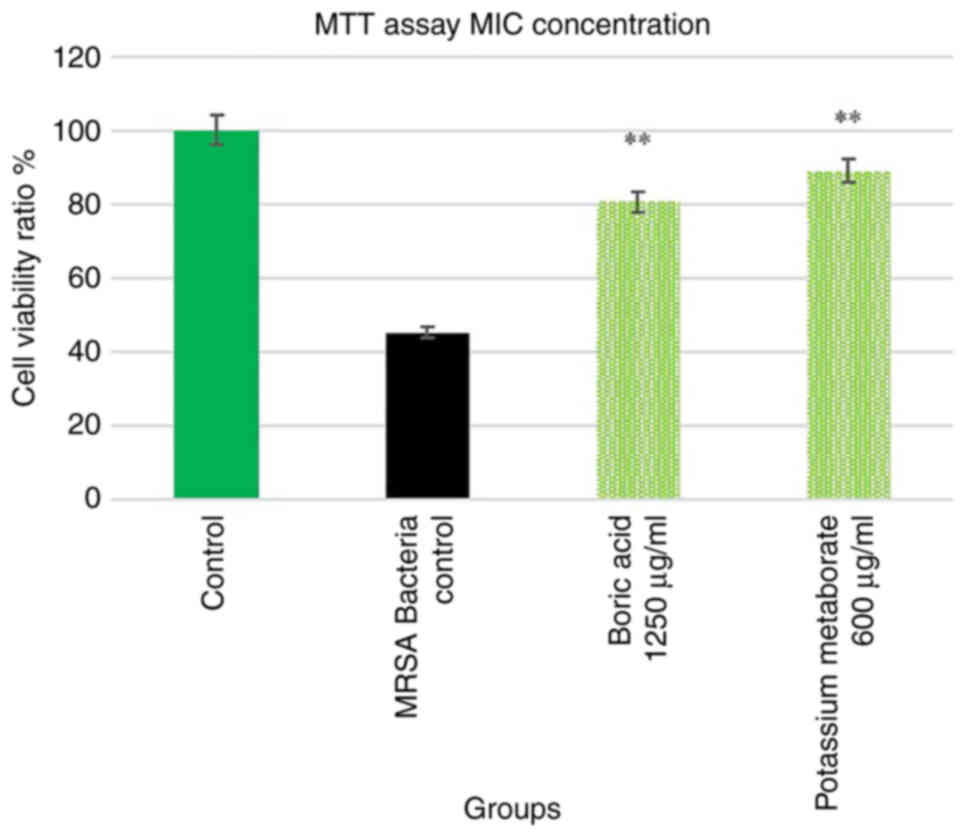
wound model with MRSA contamination). In the experiment, the cell
viability ratio was determined using MTT assay. The control group
with MRSA contamination exhibited a decreased fibroblast viability
ratio by almost 60%. Treatment with boric acid and potassium
metaborate inhibited MRSA toxicity and increased cell viability by
up to 35 and 45% respectively. By contrast, the LDH level in the
boron treatment groups exhibited a decrease. There is an
association between LDH activity and TOS. MRSA dominantly led to
increased cytotoxicity by inducing cell stress and oxidative damage
(was be detected by an increase in LDH and TOS levels, whereas Gr
and TAC levels exhibited a notable decrease) as well as biofilm
formation. An important advantage of these compounds is their high
solubility in water and a relatively good cell permeability. Nisha
et al (36) demonstrated that a
boric acid mouth rinse solution significantly reduced bacteria
compared to the control group. The inhibition of MRSA activity in
the wound model led to an increased glutathione reductase level.
Martínez et al (37) demonstrated
that MRSA induced DNA fragmentation and apoptosis by increasing
oxidative stress. In addition, they demonstrated a decrease in
oxidative stress levels, leading to an increase in the cell
viability ratio. The present study demonstrated that boron
components improved the Gr and TAC levels and also revealed that
cells can tolerate stress induced by MRSA bacteria (as a result the
cytotoxicity decreases significantly).
In addition, Idiz et al (38) demonstrated that boric acid
significantly reduced IL-1β levels in rats using hydroalcoholic
extract during the liposaccharide-associated acute inflammatory
response. Boric acid also increased the IL-10 expression level at
the same time. The mechanisms of action of boron components have
not yet been fully elucidate; however, their suppressive effects on
free radicals and the elevation of the antioxidant capacity have
been well-described. Another study also demonstrated that potassium
metaborate and boric acid decreased pro-inflammatory cytokine
levels (IL-1β) and increased IL-10 levels significantly (39). Another parameter for evaluation
oxidative stress is DNA damage.
The present study examined a wound model using the
DNA fragmentation marker, 8-OHdG (immunohistochemical staining).
The fibroblast intracytoplasmic 8-OHdG expression level was high in
the MRSA group (P<0.05). The treatment groups exhibited
decreased 8-OHdG expression levels, particularly the boric acid
group. The DNA fragmentation level decreased significantly compared
to the MRSA group. Geyikoglu et al (40) demonstrated that boric acid
decreased the 8-OHdG expression level in ischemia reperfusion
injury by acting as an antioxidant, anti-inflammatory and
antiapoptotic agent. The results of TAC, TOS and LDH assays
supported the results from the 8-OHdG staining assay (41,42).
A positive finding of the present study is that it
demonstrated that boron compounds exhibit antimicrobial activity
against MRSA. The present study determined biofilm formation using
three methods. However, some limitations of the present study were
that although biofilm formation was demonstrated phenotypically,
molecular biofilm-forming gene regions were not detected due to
unavailable economic conditions.
In conclusion, the results of the present study
suggest that boric acid and potassium borate substances can be
effective on the tested microorganisms. Further studies on the
effects of these microorganisms using various concentrations and
treatment durations are required. However, considering that
potassium metaborate has not been previously studied, at least to
the best of our knowledge, the findings of the present study may
shed light on to resistance to these microorganisms and may aid
future research into microbial resistance.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
DC, ATa, SB, SG, AY, YY, FYe, SY, IB, SK, FYi, AH,
OC, DM, GMN, DAS and ATs were involved in the study methodology and
analysis, as well as in the writing, reviewing and editing of the
manuscript. All authors have read and approved the final
manuscript. DC and ATa confirm the authenticity of all the raw
data.
Ethics approval and consent to
participate
Methicillin-resistant Staphylococcus aureus bacteria
isolated from the patient sample, for which ethical approval was
obtained with the Ataturk University Faculty of Medicine Clinical
Research Ethics Committee (decision date, 04.11.2021; decision no.
23; and meeting no. 07) was used in the study. All necessary
consents and permissions were obtained for the patient samples used
in the study. The ethics committee document obtained from the
authors' institution includes all consent forms.
Patient consent for publication
Not applicable.
Competing interests
DAS is the Editor-in-Chief for the journal, but had
no personal involvement in the reviewing process, or any influence
in terms of adjudicating on the final decision, for this article.
The other authors declare that they have no competing
interests.
References
|
1
|
Macdonald J and Asiedu K: WAWLC: World
alliance for wound and lymphedema care. Wounds. 22:55–59.
2010.PubMed/NCBI
|
|
2
|
Hill KE, Malic S, McKee R, Rennison T,
Harding KG, Williams DW and Thomas DW: An in vitro model of chronic
wound biofilms to test wound dressings and assess antimicrobial
susceptibilities. J Antimicrob Chemother. 65:1195–1206. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Yarwood JM and Schlievert PM: Quorum
sensing in staphylococcus infections. J Clin Invest. 112:1620–1625.
2003. View Article : Google Scholar
|
|
4
|
Larsen JA and Overstreet J: Pulsed radio
frequency energy in the treatment of complex diabetic foot wounds:
Two cases. J Wound Ostomy Continence Nurs. 35:523–527. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
European Committee on Antimicrobial
Susceptibility Testing (EUCAST), . Breakpoint tables for
interpretation of MICs and zone diameters. Version 12.0. EUCAST;
Växjö: 2022, https://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/Breakpoint_tables/v_12.0_Breakpoint_Tables.pdfJanuary
1–2022
|
|
6
|
Selim S: Mechanisms of gram-positive
vancomycin resistance (Review). Biomed Rep. 16:72022. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Manandhar S, Singh A, Varma A, Pandey S
and Shrivastava N: Biofilm producing clinical staphylococcus aureus
isolates augmented prevalence of antibiotic resistant cases in
tertiary care hospitals of Nepal. Front Microbiol. 9:27492018.
View Article : Google Scholar
|
|
8
|
Malone M, Bjarnsholt T, McBain AJ, James
GA, Stoodley P, Leaper D, Tachi M, Schultz G, Swanson T and Wolcott
RD: The prevalence of biofilms in chronic wounds: a systematic
review and meta-analysis of published data. J Wound Care. 26:20–25.
2017. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Moormeier DE and Bayles KW: Staphylococcus
aureus biofilm: A complex developmental organism. Mol Microbiol.
104:365–376. 2017. View Article : Google Scholar
|
|
10
|
Irschik H, Schummer D, Gerth K, Höfle G
and Reichenbach H: The tartrolons, new boron-containing antibiotics
from a myxobacterium, Sorangium cellulosum. J Antibiot (Tokyo).
48:26–30. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Soriano-Ursúa MA, Das BC and
TrujILlo-Ferrara JG: Boron-containing compounds: Chemico-biological
properties and expanding medicinal potential in prevention,
diagnosis and therapy. Expert Opin Ther Pat. 24:485–500. 2014.
View Article : Google Scholar
|
|
12
|
Field MC, Horn D, Fairlamb AH, Ferguson
MA, Gray DW, Read KD, De Rycker M, Torrie LS, Wyatt PG, Wyllie S
and Gilbert IH: Anti-trypanosomatid drug discovery: An ongoing
challenge and a continuing need. Nat Rev Microbiol. 15:217–231.
2017. View Article : Google Scholar
|
|
13
|
Wall RJ, Rico E, Lukac I, Zuccotto F, Elg
S, Gilbert IH, Freund Y, Alley MR, Field MC, Wyllie S and Horn D:
Clinical and veterinary trypanocidal benzoxaboroles target CPSF3.
Proc Natl Acad Sci USA. 115:9616–9621. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Castanheira M, Huband MD, Mendes RE and
Flamm RK: Meropenem-vaborbactam tested against contemporary
gram-negative isolates collected worldwide during 2014, including
carbapenem-resistant, KPC-producing, multidrug-resistant, and
extensively drug-resistant enterobacteriaceae. Antimicrob Agents
Chemother. 61:e00567–17. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Yang F, Zhu M, Zhang J and Zhou H:
Synthesis of biologically active boron-containing compounds.
Medchemcomm. 9:201–211. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Das BC, Thapa P, Karki R, Schinke C, Das
S, Kambhampati S, Banerjee SK, Van Veldhuizen P, Verma A, Weiss LM
and Evans T: Boron chemicals in diagnosis and therapeutics. Future
Med Chem. 5:653–676. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Jiang L, Zhao YM and Yang MZ: Inhibition
of autophagy enhances apoptosis induced by bortezomib in AML cells.
Oncol Lett. 21:1092021. View Article : Google Scholar
|
|
18
|
Tanaka M and Fujiwara T: Physiological
roles and transport mechanisms of boron: Perspectives from plants.
Pflugers Arch. 456:671–677. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Iavazzo C, Gkegkes ID, Zarkada IM and
Falagas ME: Boric acid for recurrent vulvovaginal candidiasis: The
clinical evidence. J Womens Health (Larchmt). 20:1245–1255. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Borrelly J, Blech MF, Grosdidier G,
Martin-Thomas C and Hartemann P: Contribution of a 3% solution of
boric acid in the treatment of deep wounds with loss of substance.
Ann Chir Plast Esthet. 36:65–9. 1991.(In French).
|
|
21
|
Nzietchueng RM, Dousset B, Franck P,
Benderdour M, Nabet P and Hess K: Mechanisms implicated in the
effects of boron on wound healing. J Trace Elem Med Biol.
16:239–244. 2002. View Article : Google Scholar
|
|
22
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(−Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Valavanidis A, Vlachogianni T and Fiotakis
C: 8-hydroxy-2-deoxyguanosine (8-OHdG): A critical biomarker of
oxidative stress and carcinogenesis. J Environ Sci Health C Environ
Carcinog Ecotoxical Rev. 27:120–139. 2009. View Article : Google Scholar
|
|
24
|
Demirci S, Doğan A, Karakuş E, Halıcı Z,
Topçu A, Demirci E and Sahin F: Boron and poloxamer (F68 and F127)
containing hydrogel formulation for burn wound healing. Biol Trace
Elem Res. 168:169–180. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
National Committee for Clinical Laboratory
Standards (NCCLS), . Performance standards for antimicrobial disk
susceptibility tests. Approved standard. NCCLS document M2-A5.
NCCLS; Villanova, PA: pp. 138–144. 1993
|
|
26
|
O'Toole GA: Classic spotlight: How the
gram stain works. J Bacteriol. 198:31282016. View Article : Google Scholar
|
|
27
|
Yilmaz MT: Minimum inhibitory and minimum
bactericidal concentrations of boron compounds against several
bacterial strains. Turk J Med Sci. 42:1423–1429. 2012.
|
|
28
|
Çomaklı S, Sevim Ç, Kontadakis G, Doğan E,
Taghizadehghalehjoughi A, Özkaraca M, Aschner M, Nikolouzakis TK
and Tsatsakis A: Acute glufosinate-based herbicide treatment in
rats leads to increased ocular interleukin-1β and c-Fos protein
levels, as well as intraocular pressure. Toxicol Rep. 6:155–160.
2019. View Article : Google Scholar
|
|
29
|
Kinoshita PF, Yshii LM, Orellana A, Paixão
AG, Vasconcelos AR, Lima LS, Kawamoto EM and Scavone C: Alpha 2
Na+, K+-ATPase silencing induces loss of inflammatory response and
ouabain protection in glial cells. Sci Rep. 7:48942017. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Shinde DB, Koratkar SS, Sharma N and
Shitole AA: Antioxidant activity and antiproliferative action of
methanolic extract of liquorice (Glycyrrhiza Glabra) in Hepg2 cell
line. Int J Pharm Pharmaceut Sci. 8:293–298. 2016. View Article : Google Scholar
|
|
31
|
World Health Organization (WHO), . Global
Priority List of Antibiotic-Resistant Bacteria to Guide Research,
Discovery, and Development of New Antibiotics. WHO; Geneva: 2017,
https://www.who.int/news/item/27-02-2017-who-publishes-list-of-bacteria-for-which-new-antibiotics-are-urgently-neededJuly
5–2022
|
|
32
|
Suci PA, Mittelman MW, Yu FP and Geesey
GG: Investigation of ciprofloxacin penetration into pseudomonas
aeruginosa biofilms. Antimicrob Agents Chemother. 38:2125–2133.
1994. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Rachid S, Ohlsen K, Witte W, Hacker J and
Ziebuhr W: Effect of subinhibitory antibiotic concentrations on
polysaccharide intercellular adhesin expression in biofilm-forming
Staphylococcus epidermidis. Antimicrob Agents Chemother.
44:3357–3363. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Ni N, Li M, Wang J and Wang B: Inhibitors
and antagonists of bacterial quorum sensing. Med Res Rev.
29:65–124. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Sayin Z, Ucan US and Sakmanoglu A:
Antibacterial and antibiofilm effects of boron on different
bacteria. Biol Trace Elem Res. 173:241–246. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Nisha S, Shivamallu AB, Gujjari SK,
Shashikumar P, Ali NM and Kulkarni M: Efficacy of preprocedural
boric acid mouthrinse in reducing viable bacteria in dental
aerosols produced during ultrasonic scaling. Contemp Clin Dent.
12:282–288. 2021. View Article : Google Scholar
|
|
37
|
Martínez SR, Aiassa V, Sola C and Becerra
MC: Oxidative stress response in reference and clinical
Staphylococcus aureus strains under Linezolid exposure. J Glob
Antimicrob Resist. 22:257–262. 2020. View Article : Google Scholar
|
|
38
|
Idiz UO, Aysan E, Firat D, Ercan C,
Demirci S and Sahin F: Effects of boric acid-linked ampicillin on
the rat intra-abdominal sepsis model. Pak J Pharm Sci. 32:477–481.
2019.
|
|
39
|
Tekeli H, Asıcı GSE and Bildik A:
Anti-inflammatory effect of boric acid on cytokines in
ovariectomy-induced rats. Cell Mol Biol. 67:313–320. 2022.
View Article : Google Scholar
|
|
40
|
Geyikoglu F, Koc K, Erol HS, Colak S, Ayer
H, Jama S, Eser G, Dortbudak MB and Saglam YS: The propolis and
boric acid can be highly suitable, alone/or as a combinatory
approach on ovary ischemia-reperfusion injury. Arch Gynecol Obstet.
300:1405–1412. 2019. View Article : Google Scholar
|
|
41
|
Yu J, Yang Y, Li S and Meng P: Salinomycin
triggers prostate cancer cell apoptosis by inducing oxidative and
endoplasmic reticulum stress via suppressing Nrf2 signaling. Exp
Ther Med. 22:9462021. View Article : Google Scholar : PubMed/NCBI
|
|
42
|
Skaperda Z, Kyriazis D.I, Vardakas P,
Tekos F, Antoniou K, Giannakeas N and Kouretas D: In vitro
antioxidant properties of herb decoction extracts derived from
Epirus, Greece. Int J Funct Nutr. 2:112021. View Article : Google Scholar
|