Introduction
Persistent infection with high-risk human
papillomavirus (HPV) types has a critical aetiological role in the
development of cervical intraepithelial neoplasia and cervical
cancer (1). The progression from
low- to high-grade dysplasia and invasive disease is extremely rare
in the absence of HPV (2). A
recently published meta-analysis included 30,848 cases of invasive
cervical cancer; the most frequently found HPV types in descending
order were HPV16, 18, 58, 33, 45, 31, 52, 35, 59, 39, 51 and 56,
with HPV16 and/or 18 associated with 73% of all cases (3). This is in accordance with the HPV
types classified as carcinogenic by the International Agency for
Research on Cancer (4).
The eight most frequent HPV types reported by Li
et al (3) accounted for 91%
of 8,977 HPV-positive cervical cancers of epithelial origin in a
worldwide retrospective cross-sectional study on HPV type
distribution (5). HPV16 and 18 have
been reported to be the causal agents in 65–77% of all cervical
cancers (5,6), and HPV16 is the most prevalent HPV
type in all regions with the exception of Eastern Africa, Japan and
Taiwan, where it is the second most prevalent type following HPV52
(5). In a Swedish study, HPV16 was
detected in 61% of cervical carcinoma in situ (CIS) followed
by HPV33/52/58 in 24%, HPV31 in 13% and HPV18/45 in 12% (7).
In countries with organised cervical cancer
screening programmes, mortality from cervical cancer occurs most
commonly among older females. Despite screening and protocols for
the treatment of cervical intraepithelial neoplasia, which have
existed for several decades, invasive cervical cancer remains
common in females aged ≥50 years. In 2006, >60% of cervical
squamous cell carcinomas (SCCs) in Sweden occurred in
postmenopausal females aged ≥50 years (8) and 86% of all cervical cancer-related
mortalities occurred in females belonging to older age groups
(9,10). It has been shown that HPV testing is
three times as sensitive as cytology to detect CIN2 or worse in
females aged between 50 and 65 years (11). However, diagnostic difficulties
remain, as knowledge with regard to the prevalence of HPV infection
in this age group is limited. For this reason, the understanding of
the correlation between high-risk HPV infection and cervical cancer
in older females is of significant value (12).
The purpose of this study was to identify the
prevalence of HPV16 in females with CIS in the population-based
organised cervical screening programme in Uppsala County, Sweden,
and to describe the age-specific prevalence of multiple HPV
infections, with a focus on older females. The prevalence of HPV16
in females with CIS was also compared with that in females with
SCC.
Patients and methods
Organised cervical cancer screening
programme in Uppsala County, Sweden
The population-based organised cervical screening
programme in Uppsala County, Sweden screens females aged between 25
and 60 years. Within the framework of the programme, ~70,000
females are screened by conventional cytology each year by midwives
in family planning centres. Females with abnormal cytological
findings, using atypical squamous cells of undetermined
significance (ASCUS) as a cut-off, are referred for further
investigation. Females with low-grade cytological abnormalities
[such as ASCUS and low-grade squamous intraepithelial lesions
(SIL)] undergo supplementary HPV testing and have a new cytological
sample taken following a mean follow-up time of approximately three
months, at which time two cervical brushes (MedScand, Malmö,
Sweden) are used to collect cell samples from the ecto- and
endocervix. One brush is spread on a slide for Papanicolaou
staining, while the other is applied to a FTA elute card (filter
paper matrix; cat. no. WB120411; Whatman, Inc., Clifton, NJ, USA)
(13,14). HPV detection is performed using an
hpVIR multiplex real-time polymerase chain reaction (PCR)
assay. Females with persistent ASCUS/low-grade SIL and high-risk
HPV infection at the three-month follow-up, as well as females with
high-grade SIL, are referred for a complete clinical work-up,
including a pelvic examination, colposcopy with directed biopsies
of suspicious areas and repeat cytology.
The SymPathy database (Tieto AB, Malmö, Sweden)
contains information on results obtained at the Department of
Clinical Pathology and Cytology of Uppsala University Hospital
(Uppsala, Sweden). Data therein are identified by specific
topography and morphology codes (Systematized, Nomenclature Of
Medicine; College of American Pathologists, Skokie, IL, USA). The
database of the organised population-based cervical cancer
screening programme of Uppsala County, Sweden includes cytological,
HPV and histological results from all laboratories in the county.
The cytological and histological samples from the screening
programme are stored at the Department of Clinical Pathology and
Cytology of Uppsala University Hospital (Uppsala, Sweden), where
all cytological, HPV and histological testing for the screening
programme is performed. Detailed descriptions of the database
searches for HPV status and HPV screening analysis results have
been published (14).
Briefly, a 3-mm Ø Harris micro punch (GE Healthcare,
Little Chalfont, UK) is used to excise sections from the FTA cards
using the BSD 600 (BSD Robotics, Queensland, Australia)
semi-automatic punch robot. Four punches from each card are then
transferred to a single well in a 96-well plate and washed by
vortexing three times for 5 sec in 200 μl distilled water. The
water is then carefully removed using a pipette. DNA elution is
performed in 50 μl of distilled water at 95°C for 30 min in a
heating block (with a heated lid). A total of 3 μl of the DNA
extract is used as a template in each real-time PCR (14). HPV typing is performed as previously
described, using a real-time PCR assay (13), which detects and quantifies a human
single copy gene [housekeeping gene; homo sapiens
hydroxymethylbilane synthase (HMBS); GenBank accession no.
M95623.1] and the following HPV types, partly in groups: HPV16,
18/45, 31, 33/52/58, 35, 39, 51, 56 and 59. In order to determine
if a sample contains a sufficient amount of material for HPV
testing, a threshold of 10 copies of the nuclear single copy gene
per PCR is used, based on the HMBS analysis. In addition, the
sample has to contain a minimum of 10 HPV copies to render a
positive HPV result (14).
Study population
Females aged between 20 and 65 years with a
histopathological diagnosis of CIS determined between 2010 and 2011
were identified in the Sympathy database. Previous cytological, HPV
and histological results for these females were taken from the
database of the cervical cancer screening programme of Uppsala
County, Sweden. The study population was then restricted to females
with a preceding or concomitantly performed HPV test, separated by
age group and further restricted to females who tested positive for
HPV.
Older females with SCC were used for comparison.
Females aged between 50 and 95 years with a diagnosis of SCC
determined between 2008 and 2011, and a preceding or concomitant
HPV test were identified and included in the study.
Statistical analysis
Data were analysed using the Statistica 6.1 software
(Statsoft, Inc., Tulsa, OK, USA). Pearson’s and Yates’ corrected
χ2 (for n<5) were used to compare proportions.
Ethics statement
The present study was approved by the Uppsala
University Ethics Review Board (Uppsala, Sweden), which determined
that informed consent from the participants was not required, and
was conducted according to the principles expressed in the
Declaration of Helsinki.
Results
HPV types in CIS
Of the 205 females with CIS identified in the
database, 162 (79%) had a previous or concomitant HPV test recorded
in the database of the organised cervical cancer screening
programme. Of those, 156 (96%) tested positive for HPV and were
included in the final analyses. In addition, 35 females with SCC
were also included for comparison. The mean age of females with CIS
was 37 years, (median, 37; range, 20–65 years) and the mean age of
females with SCC was 66 years (median, 62; range 50–95 years).
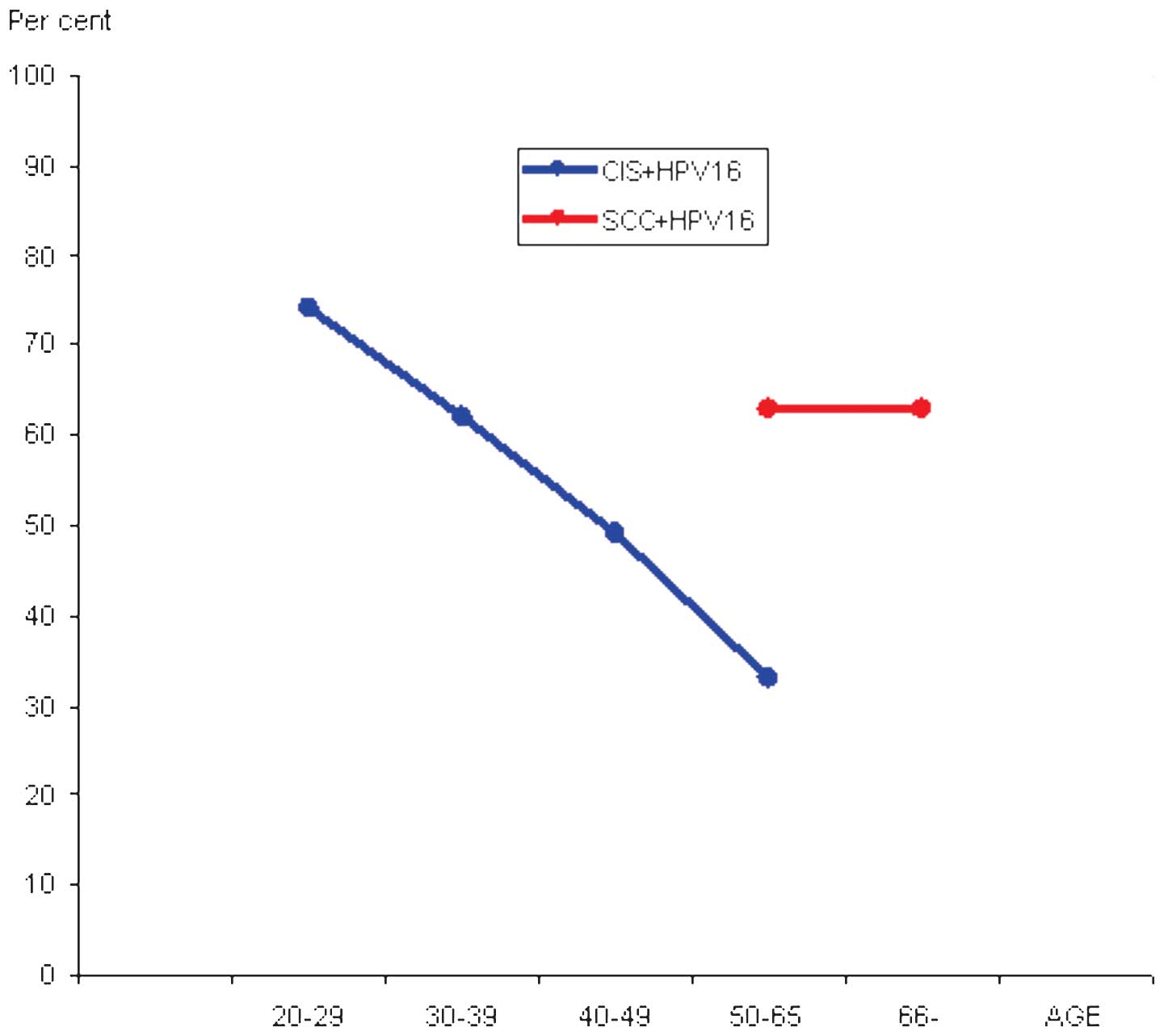
HPV16 was the most common high-risk HPV type in this
study population (n=89; 44.5%). Age-specific HPV16 prevalence
ranged from 73.6% (28/38) in females aged between 20 and 29 years
to 33.3% (7/21) in females aged between 50 and 65 years (P=0.001;
χ2). Whereas HPV18/45 was only identified in 19 (9.5%)
females of the study population (P<0.001 vs. HPV16;
χ2). HPV33/52/58 and HPV31 were also more common than
HPV18. HPV33/52/58 was found in 13.1% of females aged between 20
and 29 years and in 30% of females aged ≥50 years, and the
HPV33/52/58 types were as common as HPV16 in females aged ≥50 years
(30.4%) (Tables I and II and Fig.
1). The importance of high-risk HPV types other than HPV16
varied somewhat with age. In general, HPV33/52/58 and HPV31 were
more frequent among females aged between 20 and 49 years (25.0 and
17.0%, respectively) than HPV18/45, which occurred in 12.0% of the
study population (Table I).
 | Table IDistribution of high-risk HPV types in
156 females with cervical carcinoma in situ. |
Table I
Distribution of high-risk HPV types in
156 females with cervical carcinoma in situ.
| Age, years | HPV16, n | HPV18/45, n | HPV33/52/58, n | HPV31, n | Others, n | Total, n |
|---|
| 20–29 | 28 | 6 | 8 | 8 | 11 | 61 |
| 30–39 | 32 | 5 | 13 | 8 | 8 | 66 |
| 40–49 | 22 | 5 | 11 | 7 | 5 | 50 |
| 50–65 | 7 | 3 | 7 | 3 | 3 | 23 |
| Total (%) | 89 (44.5) | 19 (9.5) | 39 (19.5) | 26 (13.0) | 27 (13.5) | 200a |
 | Table IIOccurrence of HPV16 infection in 156
females with CIS and of multiple HPV infections by age. |
Table II
Occurrence of HPV16 infection in 156
females with CIS and of multiple HPV infections by age.
| Age, years | CIS | HPV16, n (%) | HPV16 with multiple
infections, n (%) |
|---|
| 20–29 | 38 | 28 (73.6) | 10 (35.7) |
| 30–39 | 52 | 32 (61.5) | 5 (15.6) |
| 40–49 | 45 | 22 (48.8) | 1 (2.2) |
| 50–65 | 21 | 7 (33.3) | 1 (4.8) |
| Total | 156 | 89 (57.0) | 17 (19.1) |
Multiple HPV types
Multiple infections were common in this study
population, but more so among the younger females. Overall, 38.9%
of females harboured more than one HPV type, and 26.3% of females
aged between 20 and 29 years harboured more than one high-risk HPV
type, compared with 9.6% of females aged between 30 and 39 years,
and 3.0% of females ages ≥40 years. In HPV16-positive females,
multiple infections were also more prevalent in younger females;
35.6% of females aged between 20 and 29 years, compared with ~7.0%
in females aged ≥40 years (Table
II and Fig. 1).
HPV types in SCC
In total, 30 (85.7%) females with SCC were positive
for high-risk HPV types. HPV16 predominated and occurred in 19
(63.3%) females with SCC, followed by HPV18/45 in six (20.0%)
females. However, multiple HPV infections were not recorded in any
females with SCC (Table III).
 | Table IIIPrevalence of high-risk HPV types in
cervical squamous cell carcinoma of 30 females of ≥50 years of age
(range, 50–95 years) between 2008 and 2011. |
Table III
Prevalence of high-risk HPV types in
cervical squamous cell carcinoma of 30 females of ≥50 years of age
(range, 50–95 years) between 2008 and 2011.
| HPV type | n (%) |
|---|
| 16 | 19 (63.3) |
| 18/45 | 6 (20.0) |
| 31 | 1 (3.33) |
| 33/52/58 | 1 (3.33) |
| 35 | 1 (3.33) |
| 36 | 1 (3.33) |
| 59 | 1 (3.33) |
| Total | 30 (100)a |
The biopsies of the six females with CIS and a
negative HPV test were re-evaluated, but the diagnosis was not
altered. The biopsies of the five females with SCC and a negative
HPV test were also re-evaluated, but in the majority of cases the
biopsies were small, and it was not possible to determine whether
the tumour was of cervical origin, or constituted local metastases
of a tumour with another primary site.
Discussion
This study provides an overview of the HPV type
distribution, and the prevalence of multiple infections encountered
among females of all ages with CIS detected in a population- and
cytology-based cervical cancer screening programme, as well as
among older females with SCC. The prevalence of HPV16 was found to
vary with age in females with CIS, with a significant decreasing
prevalence in older females. Other studies have identified the same
pattern, showing HPV16 as the dominant oncogenic HPV type in CIS
(7,15). In females with CIS aged between 25
and 49 years, 61% were HPV16-positive, a figure identical to that
of a previous study (7). However,
by separating females into age groups and including older females
aged between 50 and 65 years, a clear trend was observed, namely a
markedly significant (P<0.001) decrease in HPV16 positivity to
33% among females with CIS in the oldest age group.
A combination of organised and opportunistic
screening has reduced the incidence of SCC substantially during the
last decades in Sweden (16,17).
However, the sensitivity of cytological screening is lower in older
females (18,19), and it has been indicated that in
spite of a high incidence of cervical cancer in older females, the
value of screening in older age groups is questionable (18). In addition, the sensitivity of
cytology testing has been reported to be lower than HPV testing in
older females (11,19). Consistent with this finding,
countries with organised cervical cancer screening programmes have
a higher occurrence of cervical cancer-related mortality among
females aged ≥50 years (10). For
that reason, the correlation between high-risk HPV infection and
cervical cancer in older females deserves attention, and has been
the object of increased interest (11,19). A
higher risk of premalignant and malignant cervical alterations in
younger, compared with older, HPV16-positive females has been
reported (20). The current study
observed a decreasing importance of HPV16 infection with increasing
age in females with CIS. Conversely, the number of older females
with SCC harbouring HPV16 was unaltered at ~63%. This suggested
that the discrepancy between the number of HPV-positive
premalignant and malignant cervical lesions increases to a
significant degree with age, however, the reason for this is
unknown. It has been reported that a polymorphism of the HPV16 E6
gene is common and special attention has been directed to a L83V
mutation in the HPV16 E6 gene (21,22)
that may affect the oncogenic potential of the virus. Further
studies are required to identify the transformation activity of
various E6 proteins of high-risk HPV types.
In conclusion, HPV testing exhibits a considerably
higher sensitivity to detect CIS compared with conventional
cytology (23), particularly in
older females (11,19). The prevalence of high-risk HPV
infection decreases with age, and in older females is ~6% (12), meaning that the specificity of
primary high-risk HPV testing increases with age. Furthermore, this
specificity can be refined by short-time repeat HPV testing to
identify females with persistent infection, who are at higher risk
of cervical cancer development (24). When launching primary high-risk HPV
testing in older females, the oncogenic potential of various
high-risk HPV types, including the prototypes and their variants,
may be of value (25).
Acknowledgements
The authors would like to thank Mrs. Trudy
Perdrix-Thoma for editing assistance and English language review.
This study was supported by the Swedish Cancer Foundation (grant
nos. 070623, CAN 2007/1044 and 11 0544 CAN 2011/471), the
Karolinska Institute Cancer Strategic Grants (grant no.
5888/05-722), the Swedish Research Council (grant no.
521-2008-2899) and Stockholm County Council (grant no.
20130097).
References
|
1
|
Walboomers JM, Jacobs MV, Manos MM, et al:
Human papillomavirus is a necessary cause of invasive cervical
cancer worldwide. J Pathol. 189:12–19. 1999.
|
|
2
|
Khan MJ, Castle PE, Lorincz AT, et al: The
elevated 10-year risk of cervical precancer and cancer in women
with human papillomavirus (HPV) type 16 or 18 and the possible
utility of type-specific HPV testing in clinical practice. J Natl
Cancer Inst. 97:1072–1079. 2005.
|
|
3
|
Li N, Franceschi S, Howell-Jones R,
Snijders PJ and Clifford GM: Human papillomavirus type distribution
in 30,848 invasive cervical cancers worldwide: Variation by
geographical region, histological type and year of publication. Int
J Cancer. 128:927–935. 2011.
|
|
4
|
Bouvard V, Baan R, Straif K, et al: A
review of human carcinogens - Part B: biological agents. Lancet
Oncol. 10:321–322. 2009.
|
|
5
|
de Sanjose S, Quint WG, Alemany L, et al:
Human papillomavirus genotype attribution in invasive cervical
cancer: a retrospective cross-sectional worldwide study. Lancet
Oncol. 11:1048–1056. 2010.
|
|
6
|
Smith JS, Lindsay L, Hoots B, et al: Human
papillomavirus type distribution in invasive cervical cancer and
high-grade cervical lesions: a meta-analysis update. Int J Cancer.
121:621–632. 2007.
|
|
7
|
Ivansson EL, Gustavsson IM, Wilander E,
Magnusson PK and Gyllensten UB: Temporal trends over 3 decades and
intrafamilial clustering of HPV types in Swedish patients with
cervical cancer in situ. Int J Cancer. 125:2930–2935.
2009.
|
|
8
|
The National Board of Health and Welfare.
Cancer Incidence in Sweden 2008. The National Board of Health and
Welfare; Stockholm, Sweden: 2009, (In Swedish). http://www.socialstyrelsen.se/publikationer2009/2009-12-1.
Accessed December 1, 2009
|
|
9
|
Official Statistics of Sweden
Statistics-Health and Medical Care. Cancer Incidence in Sweden
2009. The National Board of Health and Welfare Centre for
Epidemiology; Stockholm, Sweden: 2010, (In Swedish). http://www.socialstyrelsen.se/publikationer2010/2010-12-17.
Accessed December 17, 2010
|
|
10
|
Official Statistics of Sweden
Statistics-Health and Medical Care. Causes of Death in Sweden 2009.
The National Board of Health and Welfare Centre for Epidemiology;
Stockholm, Sweden: 2011, (In Swedish). http://www.socialstyrelsen.se/publikationer2011/2011-3-22.
Accessed March 22, 2011
|
|
11
|
Gyllensten U, Lindell M, Gustafsson I and
Wilander E: HPV test shows low sensitivity of Pap screen in older
women. Lancet Oncol. 11:509–510. 2010.
|
|
12
|
Gyllensten U, Gustavsson I, Lindell M and
Wilander E: Primary high-risk HPV screening for cervical cancer in
post-menopausal women. Gynecol Oncol. 125:343–345. 2012.
|
|
13
|
Gustavsson I, Juko-Pecirep I, Backlund I,
Wilander E and Gyllensten U: Comparison between the Hybrid Capture
2 and the hpVIR real-time PCR for detection of human papillomavirus
in women with ASCUS or low grade dysplasia. J Clin Virol. 45:85–89.
2009.
|
|
14
|
Gustavsson I, Lindell M, Wilander E,
Strand A and Gyllensten U: Use of FTA card for dry collection,
transportation and storage of cervical cell specimen to detect
high-risk HPV. J Clin Virol. 46:112–116. 2009.
|
|
15
|
de Sanjosé S, Diaz M, Castellsagué X, et
al: Worldwide prevalence and genotype distribution of cervical
human papillomavirus DNA in women with normal cytology: a
meta-analysis. Lancet Infect Dis. 7:453–459. 2007.
|
|
16
|
Bergstrom R, Sparen P and Adami HO: Trends
in cancer of the cervix uteri in Sweden following cytological
screening. Br J Cancer. 81:159–166. 1999.
|
|
17
|
Gunnell AS, Ylitalo N, Sandin S, et al: A
longitudinal Swedish study on screening for squamous cell carcinoma
and adenocarcinoma: evidence of effectiveness and overtreatment.
Cancer Epidemiol Biomarkers Prev. 16:2641–2648. 2007.
|
|
18
|
Gustafsson L, Sparen P, Gustafsson M, et
al: Low efficiency of cytologic screening for cancer in situ
of the cervix in older women. Int J Cancer. 63:804–809. 1995.
|
|
19
|
Lindell M, Sanner K, Wikstrom I and
Wilander E: Self-sampling of vaginal fluid and high-risk human
papillomavirus testing in women aged 50 years or older not
attending Papanicolaou smear screening. BJOG. 119:245–248.
2012.
|
|
20
|
Tanaka H, Karube A, Tanaka T and Nakagomi
O: Much higher risk of premalignant and malignant cervical diseases
in younger women positive for HPV16 than in older women positive
for HPV16. Microbiol Immunol. 45:323–326. 2001.
|
|
21
|
Zehbe I, Wilander E, Delius H and
Tommasino M: Human papillomavirus 16 E6 variants are more prevalent
in invasive cervical carcinoma than the prototype. Cancer Res.
58:829–833. 1998.
|
|
22
|
Richard C, Lanner C, Naryzhny SN, et al:
The immortalizing and transforming ability of two common human
papillomavirus 16 E6 variants with different prevalences in
cervical cancer. Oncogene. 29:3435–3445. 2010.
|
|
23
|
Ronco G, Giorgi-Rossi P, Carozzi F, et al:
Efficacy of human papillomavirus testing for the detection of
invasive cervical cancers and cervical intraepithelial neoplasia: a
randomised controlled trial. Lancet Oncol. 11:249–257. 2010.
|
|
24
|
Leinonen M, Nieminen P, Kotaniemi-Talonen
L, et al: Age-specific evaluation of primary human papillomavirus
screening vs conventional cytology in a randomized setting. J Natl
Cancer Inst. 101:1612–1623. 2009.
|
|
25
|
Katki HA, Kinney WK, Fetterman B, et al:
Cervical cancer risk for women undergoing concurrent testing for
human papillomavirus and cervical cytology: a population-based
study in routine clinical practice. Lancet Oncol. 12:663–672.
2011.
|