Introduction
Osteoclast-like giant cells (OGCs) have been
described in numerous types of malignant tumors, such as
pancreatic, breast, renal, skin, stomach and urinary bladder
(1–6). However, OGCs have rarely been found in
association with uterine cervix neoplasm. To the best of our
knowledge, only three cases of squamous cell carcinoma of the
uterine cervix with OGCs have been reported in the English
literature (7,8). In the three previous cases, all
patients were elderly females (>60 years old) and
irregular postmenopausal bleeding was the most common clinical
symptom observed. The three patients succumbed to the disease
within 14 months of surgery or treatment with radiochemotherapy
(7,8). Therefore, the origination and
prognostic significance of OGCs in squamous cell carcinoma of
uterine cervix are poorly understood. The present study reports a
fourth case of squamous cell carcinoma of the uterine cervix
associated with OGCs, and the clinicopathological features are
discussed. In this study, the case of an 84-year-old female with
irregular vaginal bleeding is presented. A cauliflower-like mass
was identified in the front lip of the uterine cervix by
colposcopy. The patient received palliative radiotherapy and
succumbed to brain metastasis after eight months of follow-up.
Written informed consent was obtained from the patient for
publication of this case report and any accompanying images.
Case report
Clinical data
An 84-year-old post-menopausal female presented to
the Department of Gynaecology at Laishan People’s Hospital (Yantai,
China) with irregular vaginal bleeding of one month, and was then
sent to the Department of Gynaecology at the Affiliated Yantai
Yuhuangding Hospital (Yantai, China). Colposcopy was performed and
a cauliflower-like mass was identified in the front lip of the
uterine cervix. The neoplasm was ~5 cm in diameter and fragile in
texture. Abdominal ultrasound examination showed multiple swollen
lymph nodes surrounding the great vessels. The blood counts,
clinical biochemistry, urine analysis and endocrine profile were
all within normal ranges.
Pathological findings
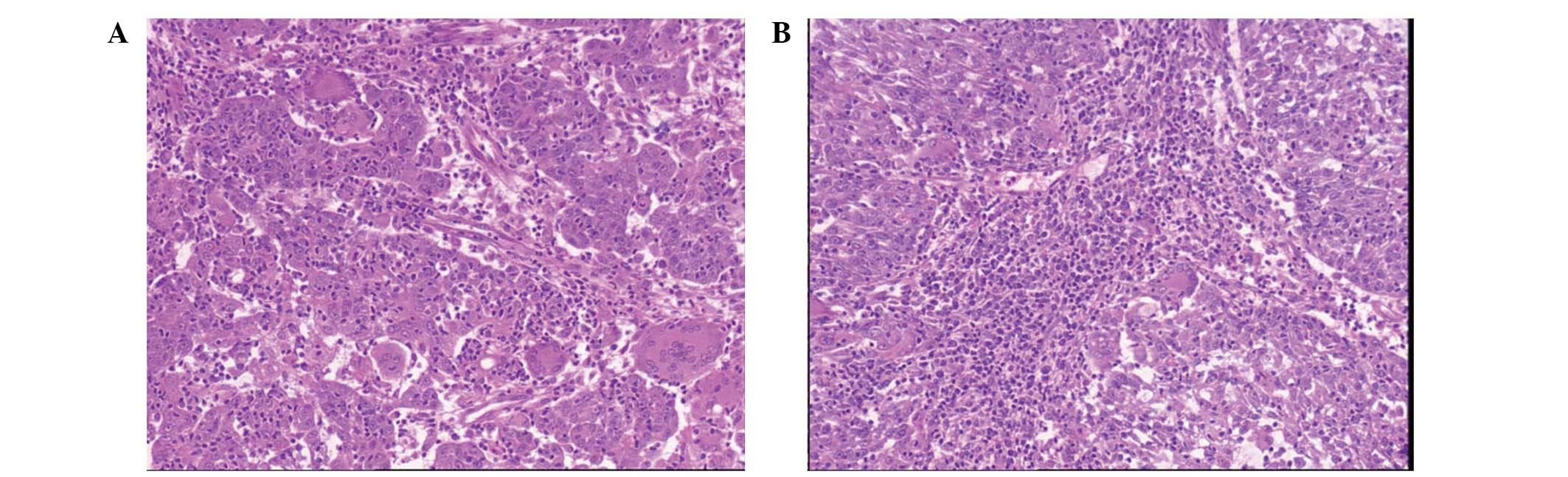
Biopsy was performed and histological findings
showed that epithelial cell nests, ranging in size, had infiltrated
the stroma. The neoplastic cells presented unclear boundaries and
eosinophilic cytoplasm. In addition, the nuclei were atypical and
mitosis was observed. There were no obvious keratin pearls or
intercellular bridges. Among the epithelial cell nests, there were
numerous OGCs with abundant eosinophilic cytoplasm and
multinucleation. The nuclei were bland, monomorphic and round or
oval in shape. The absence of features of cytological atypia and
mitosis distinguished these nuclei from those of the neoplastic
cells (Fig. 1A). There were
numerous lymphatic cells in the epithelial cell nests and
neoplastic stroma (Fig. 1B).
Immunohistochemical findings
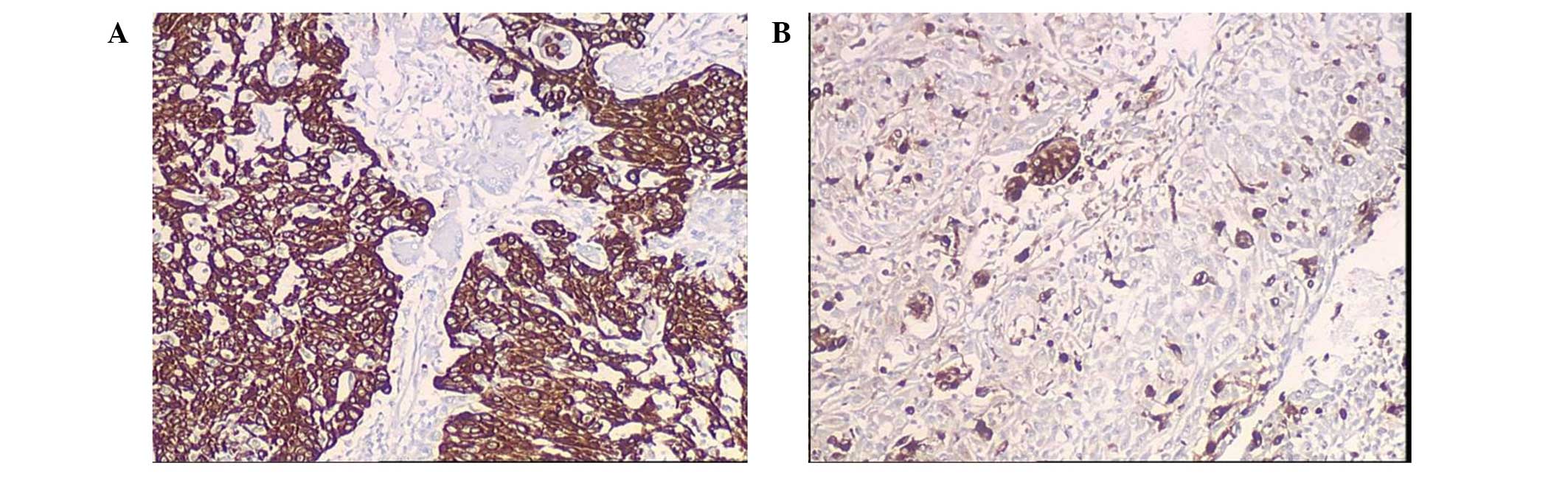
Using immunohistochemical techniques, the neoplastic
cells were identified to be positive for cytokeratin (Fig. 2A); whereas the OGCs were positive
for CD68 (Fig. 2B) and vimentin,
but negative for cytokeratin. The majority of lymphatic cells were
positive for CD3 and only a small number of lymphocytes expressed
CD20. On the basis of the clinical manifestations, histological
features and immunohistochemical findings, a diagnosis of
non-keratinizing squamous carcinoma of the uterine cervix with OGCs
was made. With consideration of the patient’s age, the surgical
treatment was cancelled with the patient’s consent and radiotherapy
was administered instead. The total follow-up period was eight
months. The patient was alive and the size of neoplasm had
decreased prior to the end of radiotherapy, however, the patient
succumbed to brain metastasis of the tumor at eight months of
follow-up.
Discussion
A number of studies have shown that OGCs are a
unique type of microphage emerging from the mesenchymal tissue,
with similar histological features to osteoclasts (3,5,9,10).
However, it was previously thought that OGCs were a type of tumor
cell that originated from the epithelium (2). In the present case, the OGCs were
bland and lacked atypia. Immunohistochemically, the OGCs were
positive for CD68 and vimentin, but negative for cytokeratin. These
results support the hypothesis that OGCs may simply be
immunoreactive cells derived from the mesenchymal tissue. In this
case, it is important to distinguish OGCs from multinucleated
cells, which are known to indicate a poor prognosis (11). The cells of giant cell tumors
exhibit nuclei with hyperchromatism and pleomorphism, while OGCs
are an immunoreactive component with uniform chromatin and no
obvious atypia (11).
OGCs have been described in numerous types of
malignant tumors, such as pancreatic, breast, renal, skin, stomach
and urinary bladder (1–6). The reason for the association of OGCs
with these tumor types may be the chemotaxis of tumor cells or
inflammatory cells. In the present case, numerous lymphocytes,
among which T lymphocytes were predominant, were identified in the
epithelial cell nests and the neoplastic stroma. Therefore, this
finding adds support to the abovementioned theory.
To the best of our knowledge, only three cases of
squamous cell carcinoma associated with OGCs in the uterine cervix
have been reported (7,8), and the clinical information is
presented in Table I. All the
patients were elderly females >60 years of age, and irregular
post-menopausal bleeding was the common clinical manifestation. In
three cases, the mass showed extruding growth, while one case
showed an infiltrated neoplasm. The tumor diameters ranged from 4.5
to 6 cm, and the clinical stage was Ib in all cases according to
the International Federation of Gynecology and Obstetrics staging
for carcinoma of the vulva, cervix, and endometrium (2009)
(12). The type of squamous cell
carcinoma which was accompanied by OGCs was sarcomatoid type or
non-keratinizing type, which are poorly differentiated types of
squamous cell carcinoma. Three patients died within 14 months of
surgery or radio-chemotherapy. One patient survived, but was
followed up for a shorter time period. Although OGCs may be
immunoreactive cells, the presence of OGCs in squamous cell
carcinoma of the uterine cervix appears to be an indicator of poor
prognosis. However, the type of primary tumor appears to be the
main determinant of prognosis, and additional clinical data are
required to determine the significance of these findings.
 | Table IPreviously reported cases of squamous
cell carcinoma associated with OGCs in the uterine cervix. |
Table I
Previously reported cases of squamous
cell carcinoma associated with OGCs in the uterine cervix.
| Case | Author (ref.) | Age, years | Tumor diameter,
cm | Tumor stage | Clinical
manifestation | Growth pattern | Histological type of
SCC | Immumohistochemical
staining of OGC | Treatment | Follow-up/Status |
|---|
| 1 | Pang (7) | 65 | 6 | Ib | IVB | Polypoid mass | Sarcomatoid type | Positive for Kp1 and
CD68; negative for CK and vimentin | Hysterectomy and
lymphadenectomy; radiotherapy and chemotherapy | 7 weeks, DOD |
| 2 | Pang (7) | 61 | 5 | Ib | IVB | Polypoid mass | Sarcomatoid type | Positive for Kp1 and
CD68; negative for CK and vimentin | Hysterectomy and
lymphadenectomy; radiotherapy and chemotherapy | 14 months, DOD |
| 3 | Singh et al
(8) | 60 | 4.5 | Ib | IVB | Infiltrated mass | NK type | Positive for CD68;
negative for CK, EMA and vimentin | Radiotherapy and
chemotherapy | 6 months, ACR |
| 4 | Present case | 84 | 5 | Ib | IVB | Polypoid mass | NK type | Positive for CD68 and
vimentin; negative for CK | Radiotherapy | 8 months, DOD |
Acknowledgements
This study was supported by the Project of
Administration of Traditional Chinese Medicine of Shandong Province
(grant no. 2009222).
References
|
1
|
Molberg KH, Heffess C, Delgado R and
Albores-Saavedra: Undifferentiated carcinoma with osteoclast-like
giant cells of the pancreas and periampullary region. Cancer.
82:1279–1287. 1998.
|
|
2
|
Borg-Grech A, Morris JA and Eyden BP:
Malignant osteoclastoma-like giant cell tumor of the renal pelvis.
Histopathology. 11:415–425. 1987.
|
|
3
|
Shishido-Hara Y, Kurata A, Fujiwara M, et
al: Two cases of breast carcinoma with osteoclastic giant cells:
Are the osteoclastic giant cells pro-tumoural differentiation of
macrophages? Diagn Pathol. 5:552010.
|
|
4
|
Willems S, Carneiro F and Geboes K:
Gastric carcinoma with osteoclast-like giant cells and
lymphoepithelioma-like carcinoma of the stomach: two of a kind?
Histopathology. 47:331–333. 2005.
|
|
5
|
Wooff J, Werner D, Murphy J and Walsh N:
Osteoclast-like giant cell reaction associated with cutaneous
squamous cell carcinoma: a report of 2 cases and review of the
literature. Am J Dermatopathol. 31:282–287. 2009.
|
|
6
|
Behzatoğlu Kemal, Durak Haydar, Canberk
Şule, et al: Giant cell tumor-like lesion of the urinary bladder: a
report of two cases and literature review; giant cell tumor or
undifferentiated carcinoma? Diagn Patho. 4:482009.
|
|
7
|
Pang LC: Sarcomatoid squamous cell
carcinoma of the uterine cervix with osteoclast-like giant cells:
report of two cases. Int J Gynecol Pathol. 17:174–177. 1998.
|
|
8
|
Singh M, Singh S, Mahajan N and Khurana N:
Osteoclastic giant cell rich carcinoma cervix: a rare entity. J
Obstet Gynaecol. 32:499–501. 2012.
|
|
9
|
Li XM, Lin XY, Xu HT, et al: Mediastinal
epithelioid hemangioendothelioma with abundant spindle cells and
osteoclast-like giant cells mimicking malignant fibrous
histiocytoma. Diagn Pathol. 8:1032013.
|
|
10
|
Suh S, Jung CK, Lee YS, et al: Xp11.2
translocation renal cell carcinoma associated with non-neoplastic
osteoclast-like giant cells. Pathol Int. 63:336–338. 2013.
|
|
11
|
Singhal A, Shrago SS, Li SF, et al: Giant
cell tumor of the pancreas: a pathological diagnosis with poor
prognosis. Hepatobiliary Pancreat Dis Int. 9:433–437. 2010.
|
|
12
|
Pecorelli S: Revised FIGO staging for
carcinoma of the vulva, cervix, and endometrium. Int J Gynaecol
Obstet. 105:103–104. 2009.
|