Article
Extragastrointestinal stromal tumors: Computed tomography and magnetic resonance imaging findings
- Authors:
- Jingqi Zhu
- Zhangwei Yang
- Guangyu Tang
- Zhongqiu Wang
-
View Affiliations / Copyright
Affiliations:
Department of Radiology, Shanghai Tenth People's Hospital, Tongji University School of Medicine, Shanghai 200072, P.R. China, Department of Radiology, East Hospital, Tongji University School of Medicine, Shanghai 200120, P.R. China
-
Pages:
201-208
|
Published online on:
November 12, 2014
https://doi.org/10.3892/ol.2014.2705
- Expand metrics +
Metrics:
Total
Views: 0
(Spandidos Publications: | PMC Statistics:
)
Metrics:
Total PDF Downloads: 0
(Spandidos Publications: | PMC Statistics:
)
This article is mentioned in:
Abstract
Extragastrointestinal stromal tumors (EGISTs) are rare mesenchymal tumors that originate outside the gastrointestinal tract. The aim of the present study was to investigate the computed tomography (CT) and magnetic resonance imaging (MRI) features of EGISTs and analyze the correlations between radiological findings and pathological features. CT and MRI images of 24 patients with EGISTs were reviewed retrospectively. Patient demographics and tumor characteristics, including localization, size, contours, borders, cystic‑necrotic components, calcification, hemorrhage, tumor vessels, attenuation and intensity, degree and pattern of enhancement, ascites, tumor invasion, lymphadenopathy and distant metastasis were recorded. Statistical analyses to compare the radiological characteristics of low‑ and high‑grade EGISTs were performed with χ2 or Fisher's exact tests. The mean patient age at the time of presentation was 53 years. A total of 24 EGISTs were detected, originating in the omentum (n=4), mesentery (n=19) and retroperitoneum (n=1), respectively. The EGISTs displayed a predominantly spindle cell subtype (87.5%; 21/24). The majority of the EGISTs appeared as large (>10 cm; 70.8%; 17/24), round or oval (66.7%; 16/24), cystic‑solid (87.5%; 21/24) and ill‑defined (66.7%; 16/24) soft‑tissue masses. The EGISTs were hypodense (69.6%; 16/23) or isodense (30.4%; 7/23) on CT images, hypointense (50%; 3/6), isointense (33.3%; 2/6) or hyperintense (16.7%; 1/6) on T1‑weighted imaging (T1WI), and hyperintense on T2WI (100%; 6/6) and diffusion‑WI (DWI; 100%; 6/6). A total of 54.2% (13/24) of the EGISTs displayed tumor vessels. Overall, 95.8% (23/24) of the masses showed marked enhancement and 87.5% (21/24) demonstrated heterogeneous enhancement. Calcification, hemorrhage, ascites and lymphadenopathy were rare characteristics in the EGISTs. Distant metastases were present in 10 patients (41.7%). The size, borders, tumor vessels and distant metastasis correlated with high‑grade EGISTs [>5 mitoses/50 high‑power fields (HPFs)] (P<0.05). The results of the present study indicated that clinical and radiological features, including advanced age, a large tumor size, cystic‑necrotic components, rare lymphadenopathy, a heterogeneous enhancement pattern and hepatic metastasis may aid in the diagnosis of EGISTs. Radiological characteristics, such as a large size (>10 cm), ill‑defined borders, tumor vessels and distant metastasis, can provide useful information in identifying the malignant behavior of EGISTs.
View Figures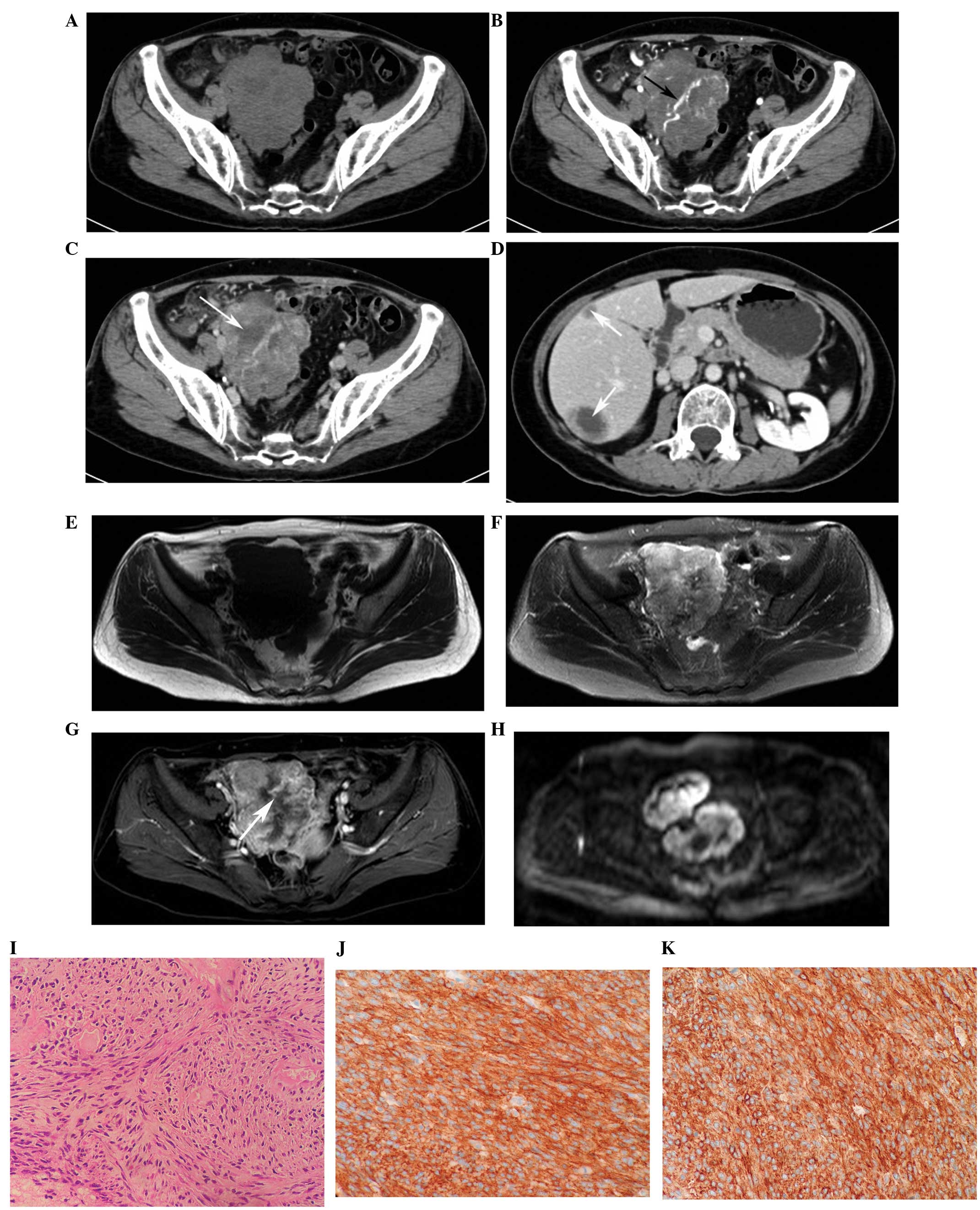 |
Figure 1
|
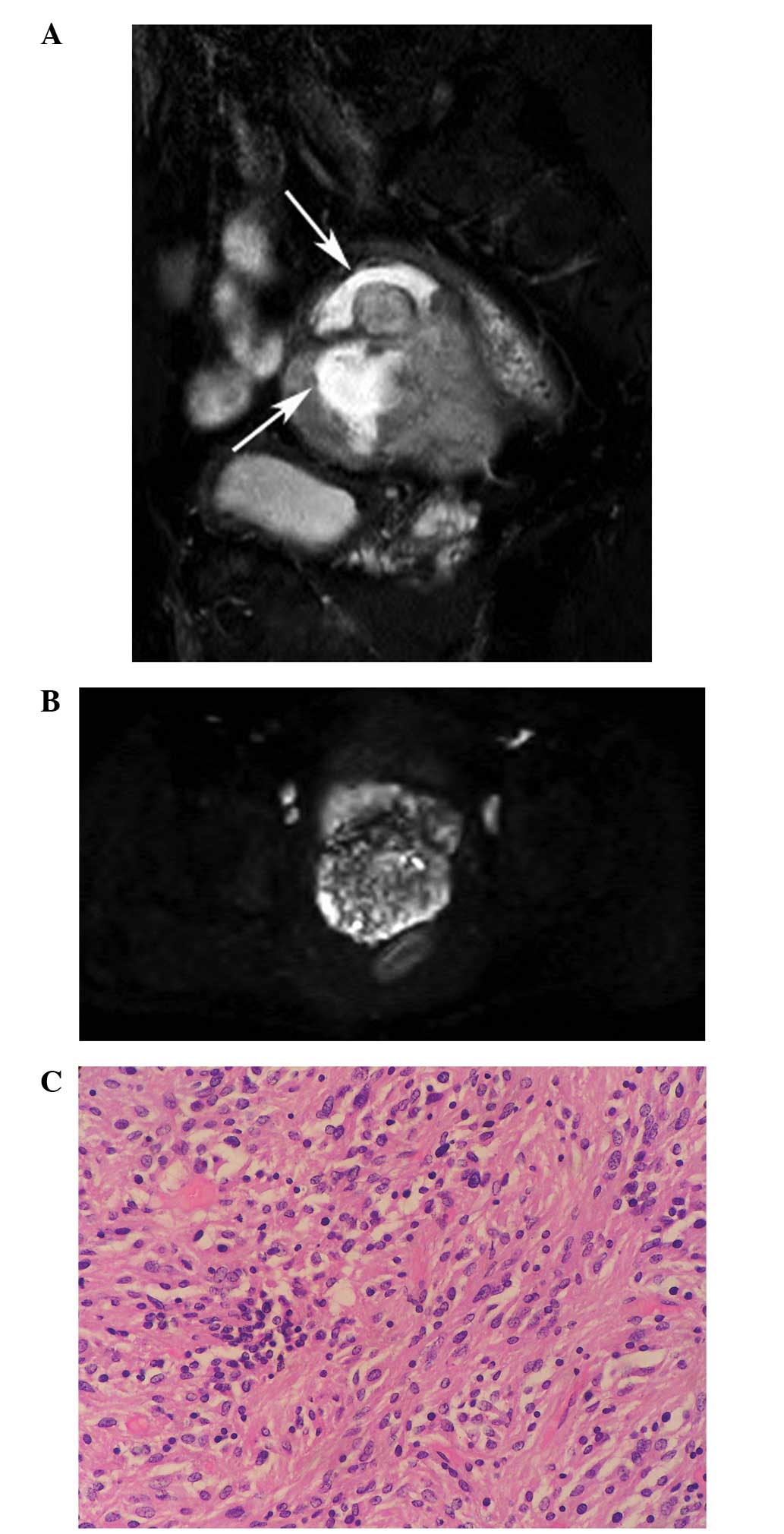 |
Figure 2
|
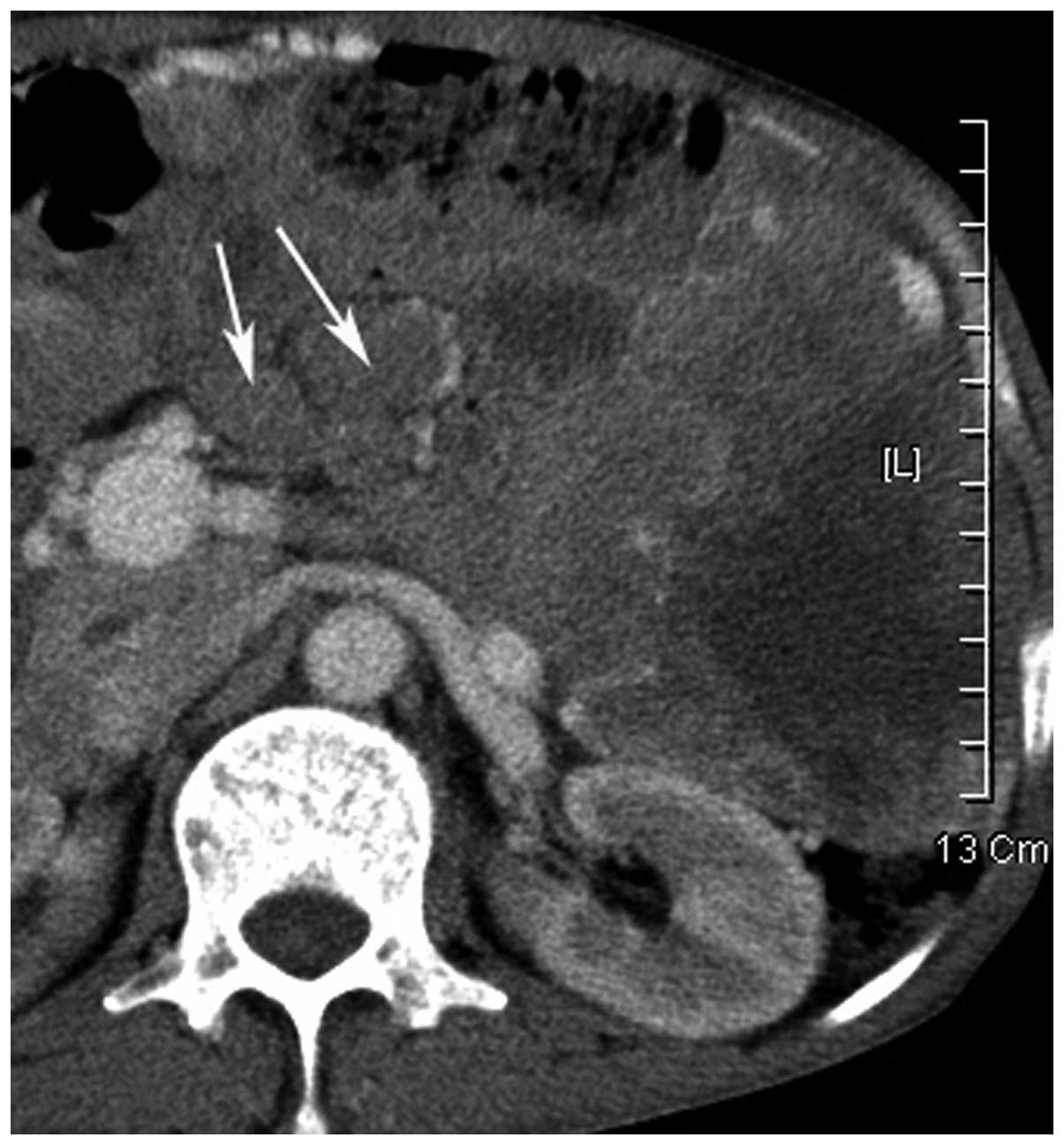 |
Figure 3
|
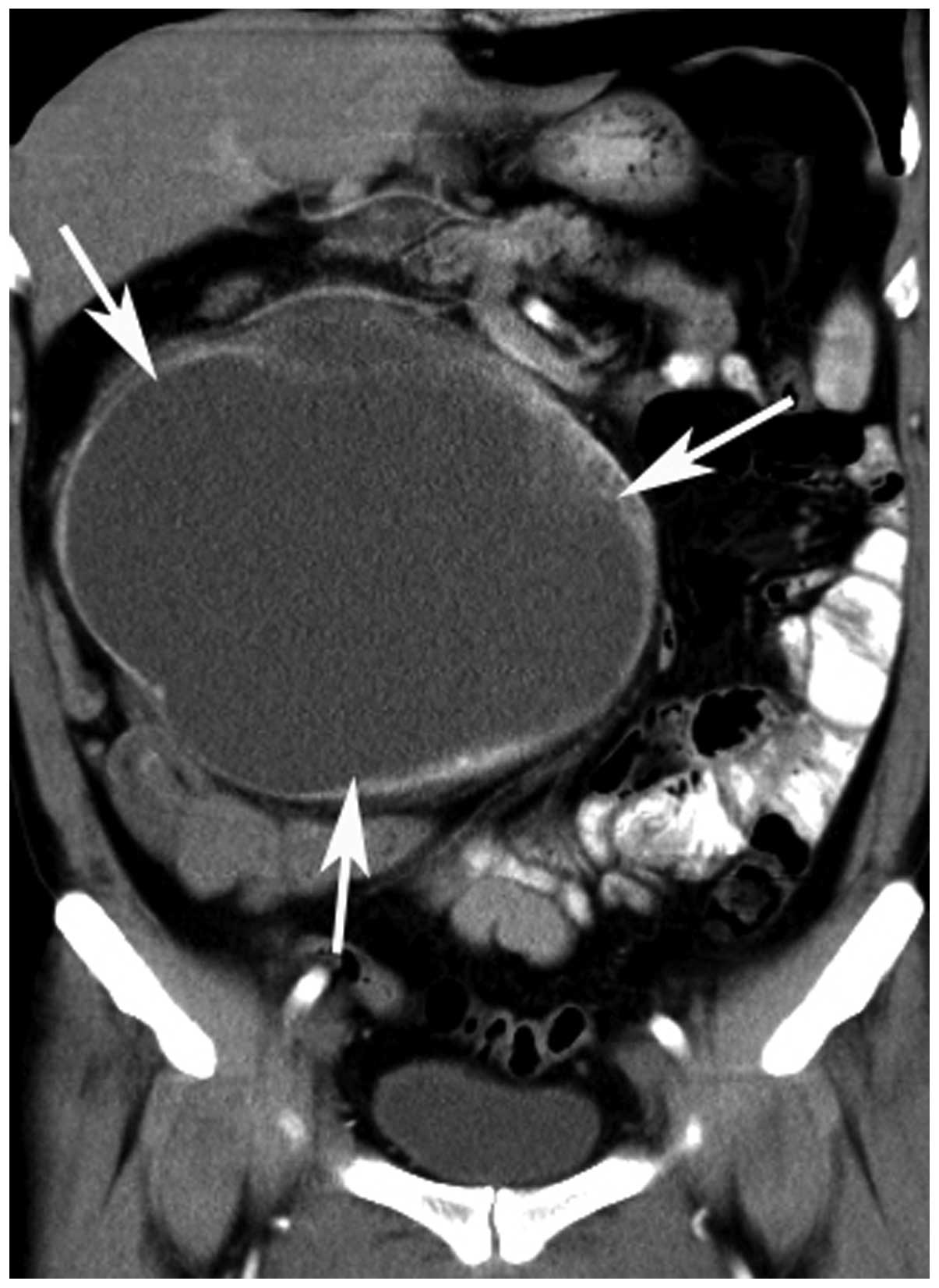 |
Figure 4
|
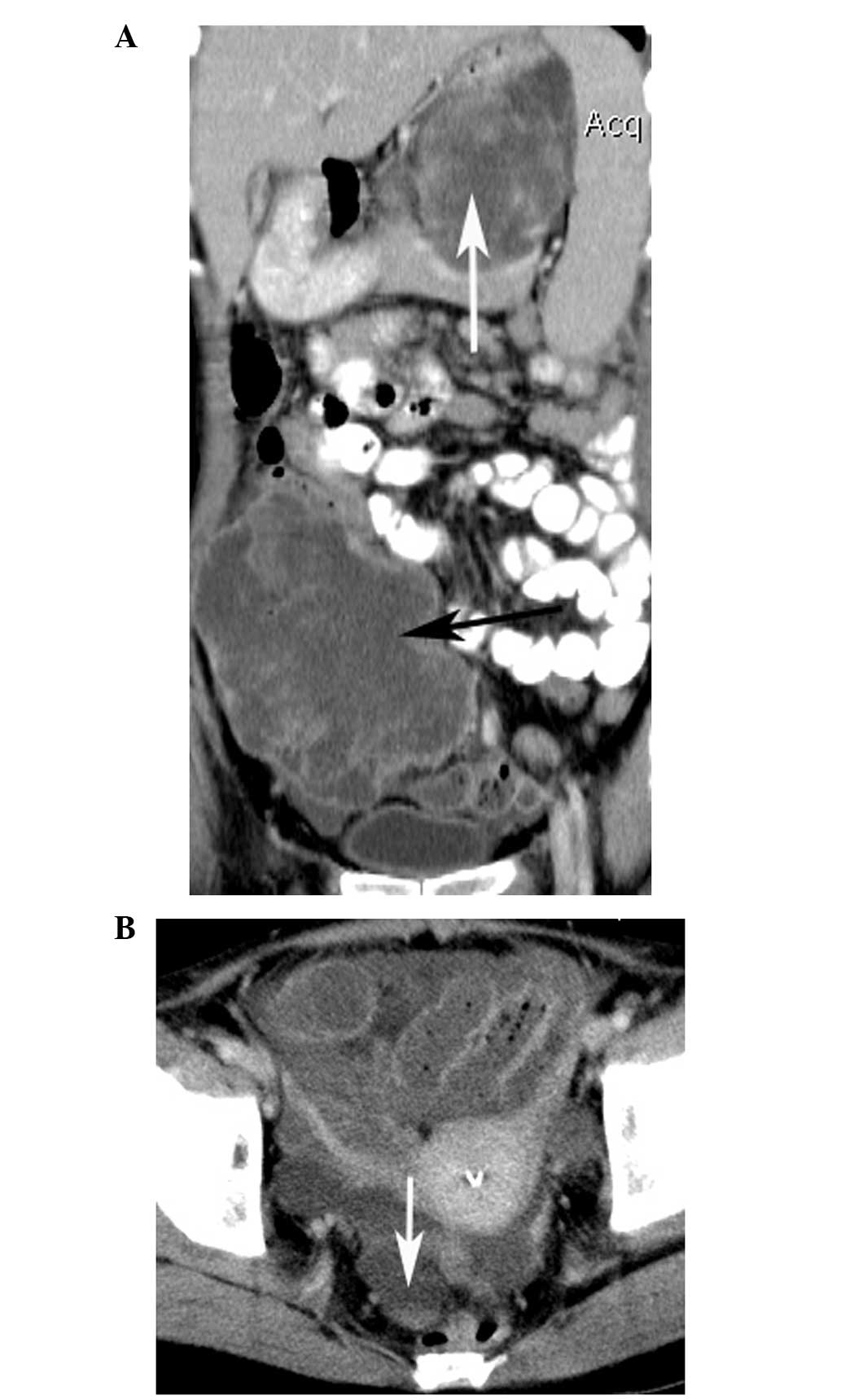 |
Figure 5
|
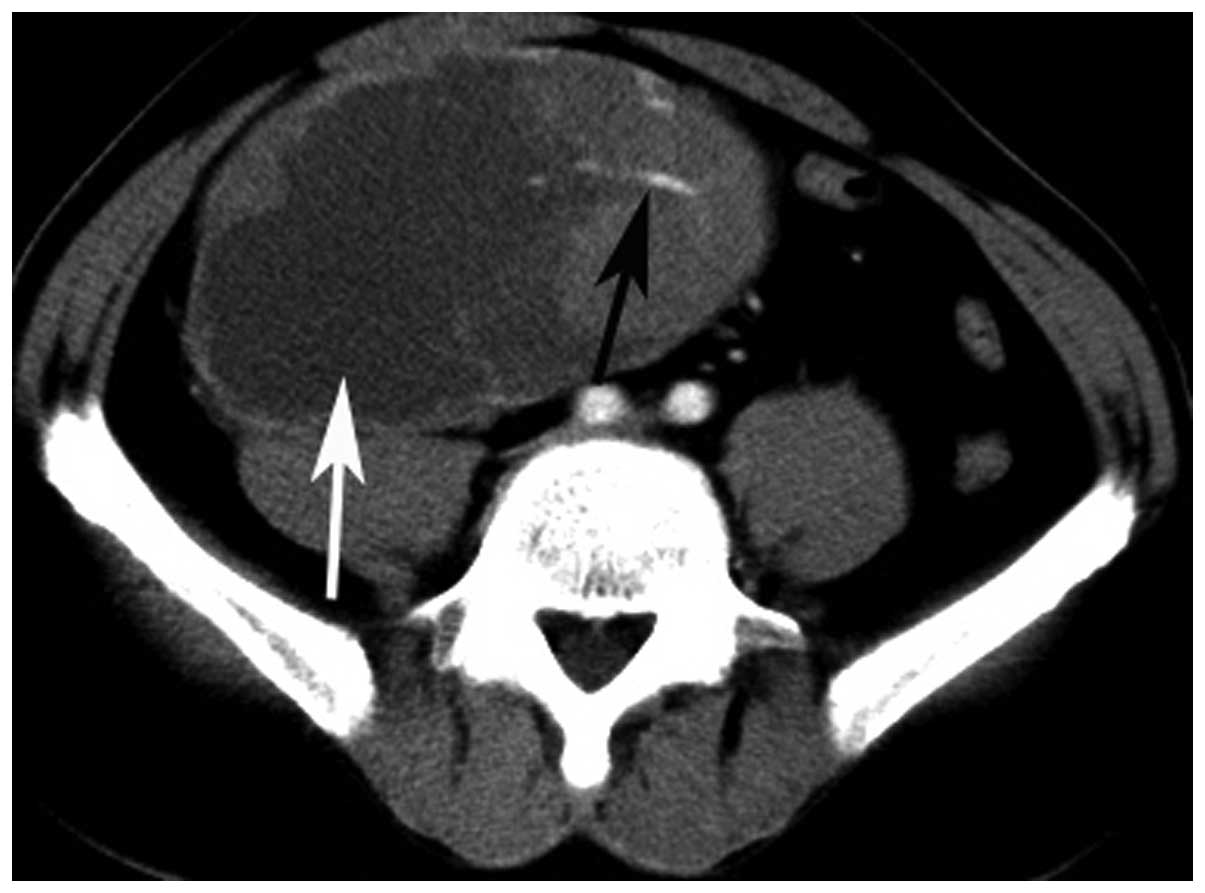 |
Figure 6
|
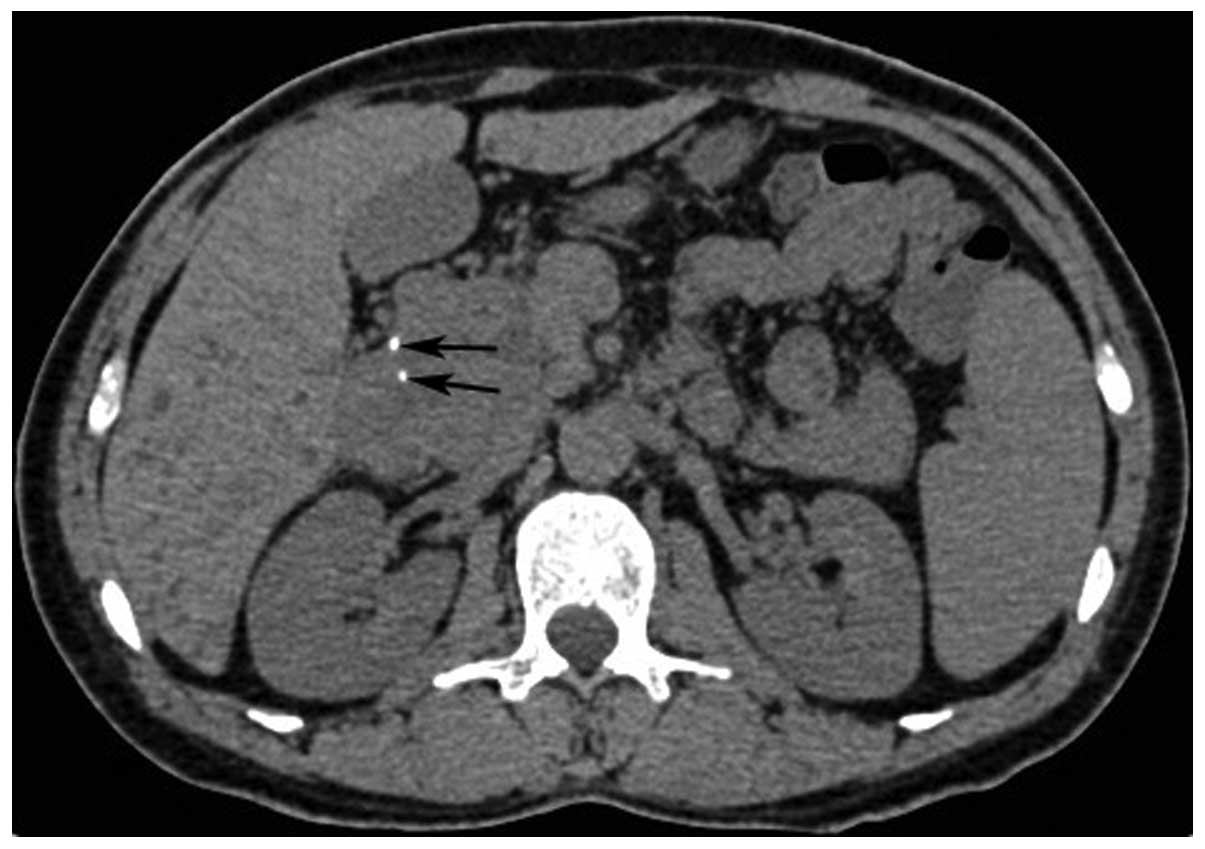 |
Figure 7
|
View References
|
1
|
Joensuu H: Risk stratification of patients
diagnosed with gastrointestinal stromal tumor. Hum Pathol.
39:1411–1419. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Yamamoto H, Kojima A, Nagata S, Tomita Y,
Takahashi S and Oda Y: KIT-negative gastrointestinal stromal tumor
of the abdominal soft tissue: a clinicopathologic and genetic study
of 10 cases. Am J Surg Pathol. 35:1287–1295. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Kim HC, Lee JM, Kim SH, et al: Primary
gastrointestinal stromal tumors in the omentum and mesentery: CT
findings and pathologic correlations. AJR Am J Roentgenol.
182:1463–1467. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Barros A, Linhares E, Valadão M, Gonçalves
R, Vilhena B, Gil C and Ramos C: Extragastrointestinal stromal
tumors (EGIST): a series of case reports. Hepatogastroenterology.
58:865–868. 2011.PubMed/NCBI
|
|
5
|
Fagkrezos D, Touloumis Z, Giannila M,
Penlidis C, Papaparaskeva K and Triantopoulou C:
Extra-gastrointestinal stromal tumor of the omentum: a rare case
report and review of the literature. Rare Tumors. 4:e442012.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Goukassian ID, Kussman SR, Toribio Y and
Rosen JE: Secondary recurrent multiple EGIST of the mesentery: A
case report and review of the literature. Int J Surg Case Rep.
3:463–466. 2012. View Article : Google Scholar
|
|
7
|
Ulusan S, Koc Z and Kayaselcuk F:
Gastrointestinal stromal tumours: CT findings. Br J Radiol.
81:618–623. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kim HC, Lee JM, Choi SH, et al: Imaging of
gastrointestinal stromal tumors. J Comput Assist Tomogr.
28:596–604. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Sandrasegaran K, Rajesh A, Rushing DA,
Rydberg J, Akisik FM and Henley JD: Gastrointestinal stromal
tumors: CT and MRI findings. Eur Radiol. 15:1407–1414. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Tateishi U, Hasegawa T, Satake M and
Moriyama N: Gastrointestinal stromal tumor. Correlation of computed
tomography findings with tumor grade and mortality. J Comput Assist
Tomogr. 27:792–798. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Zhang W, Peng Z and Xu L:
Extragastrointestinal stromal tumor arising in the rectovaginal
septum: report of an unusual case with literature review. Gynecol
Oncol. 113:399–401. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Alkhatib L, Albtoush O, Bataineh N,
Gharaibeh K, Matalka I and Tokuda Y: Extragastrointestinal stromal
tumor (EGIST) in the abdominal wall: Case report and literature
review. Int J Surg Case Rep. 2:253–255. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Agaimy A and Wünsch PH: Gastrointestinal
stromal tumours: a regular origin in the muscularis propria, but an
extremely diverse gross presentation. A review of 200 cases to
critically re-evaluate the concept of so-called
extra-gastrointestinal stromal tumours. Langenbecks Arch Surg.
391:322–329. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Goh BK, Chow PK, Kesavan SM, Yap WM, Chung
YF and Wong WK: A single-institution experience with eight
CD117-positive primary extragastrointestinal stromal tumors:
critical appraisal and a comparison with their gastrointestinal
counterparts. J Gastrointest Surg. 13:1094–1098. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Reith JD, Goldblum JR, Lyles RH and Weiss
SW: Extragastrointestinal (soft tissue) stromal tumors: an analysis
of 48 cases with emphasis on histologic predictors of outcome. Mod
Pathol. 13:577–585. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Kim KH, Nelson SD, Kim DH, et al:
Diagnostic relevance of overexpressions of PKC-θ and DOG-1 and
KIT/PDGFRA gene mutations in extragastrointestinal stromal tumors:
a Korean six-centers study of 28 cases. Anticancer Res. 32:923–937.
2012.PubMed/NCBI
|
|
17
|
Patnayak R, Jena A, Parthasarathy S, et
al: Primary extragastrointestinal stromal tumors: a
clinicopathological and immunohistochemical study - a tertiary care
center experience. Indian J Cancer. 50:41–45. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Yamamoto H, Oda Y, Kawaguchi K, et al:
c-kit and PDGFRA mutations in extragastrointestinal stromal tumor
(gastrointestinal stromal tumor of the soft tissue). Am J Surg
Pathol. 28:479–488. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Ogawa H, Gotoh K, Yamada T, et al: A case
of KIT-negative extra-gastrointestinal stromal tumor of the lesser
omentum. Case Rep Gastroenterol. 6:375–380. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Fletcher CD, Berman JJ, Corless C, et al:
Diagnosis of gastrointestinal stromal tumors: A consensus approach.
Hum Pathol. 33:459–465. 2002. View Article : Google Scholar : PubMed/NCBI
|





















