Introduction
Meningiomas are typically benign intracranial
tumors, and rarely metastasize extracranially (1). Metastasis occurs in <1% of
meningiomas, and common metastatic sites include the lung, liver,
lymph node, bone and pleura (2).
Tumors with malignant histological features are associated with a
higher metastatic rate (3); however,
there are reports of metastasis from benign meningiomas (2,4). Rawat
et al (5) reported 77 cases of
meningioma with extracranial metastasis in 1995, and ~70 additional
cases of meningioma with extracranial metastasis were identified in
the literature (2–4,6–27). There are no definitive criteria for the
prediction of metastasis in meningiomas, and the discovery of
metastasis frequently occurs following recurrence of the primary
tumor (23–25). Therefore comprehensive examinations
for patients with a history of recurrent intracranial meningioma
are required for the detection of distant metastases, despite the
tumor being benign.
Case report
A 54-year-old female was admitted to the Second
Hospital of Hebei Medical University (Shijiazhuang, China) with
primary symptoms of a progressive headache for the preceding 3
months, and nausea accompanied by vomiting for 4 days. Physical
examination was normal, except for bilateral papilloedema. Chest
plain radiograph was normal. Magnetic resonance imaging (MRI)
revealed a contrast-enhancing tumor in the left base of the middle
cranial fossa.
A gross total resection of the tumor (~6×5×5 cm) was
performed via a left fronto-temporal craniotomy (Simpson Grade III)
(28). Post-surgical pathological
examination revealed a transitional meningioma with meningiothelial
and fibroblastic components, which was classified as World Health
Organization grade I (29).
Immunohistochemical examination was not performed to explore the
histological features. Postoperative computed tomography (CT)
indicated that the tumor had been completely removed.
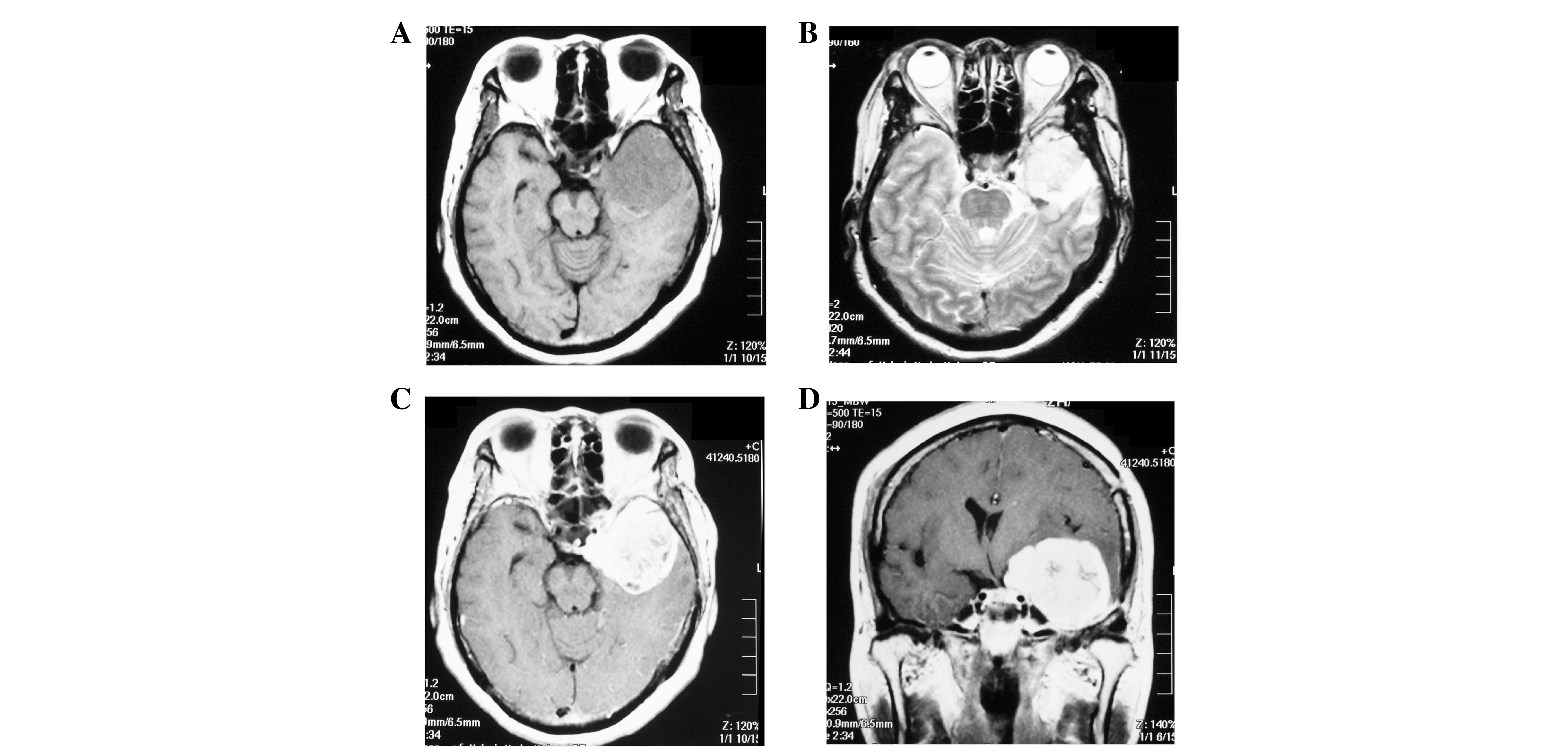
One year and 3 months later, the patient experienced
tinnitus in the left ear and dizziness for 1 month. Magnetic
resonance imaging (MRI) revealed a recurrent mass of 4×5×5 cm at
the original site and the tumor was once again completely resected
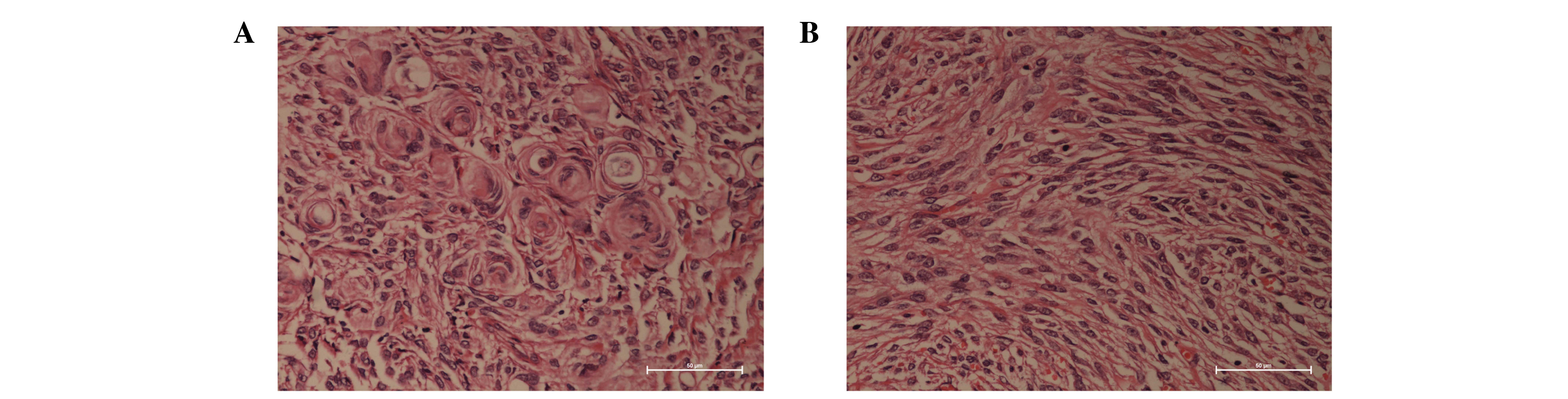
(Fig. 1). Pathological diagnosis was
transitional meningioma with similar characteristics to those of
the original tumor (Fig. 2).
Following surgery, significant signs of impairment to the
oculomotor nerve were observed. Radiotherapy was administered
(specific radiation dose unknown) 1 month following the second
surgery.
Eighteen months following the second surgery, the
patient presented with a history of dizziness for 2 months, and MRI
examination revealed another tumor recurrence at the original site.
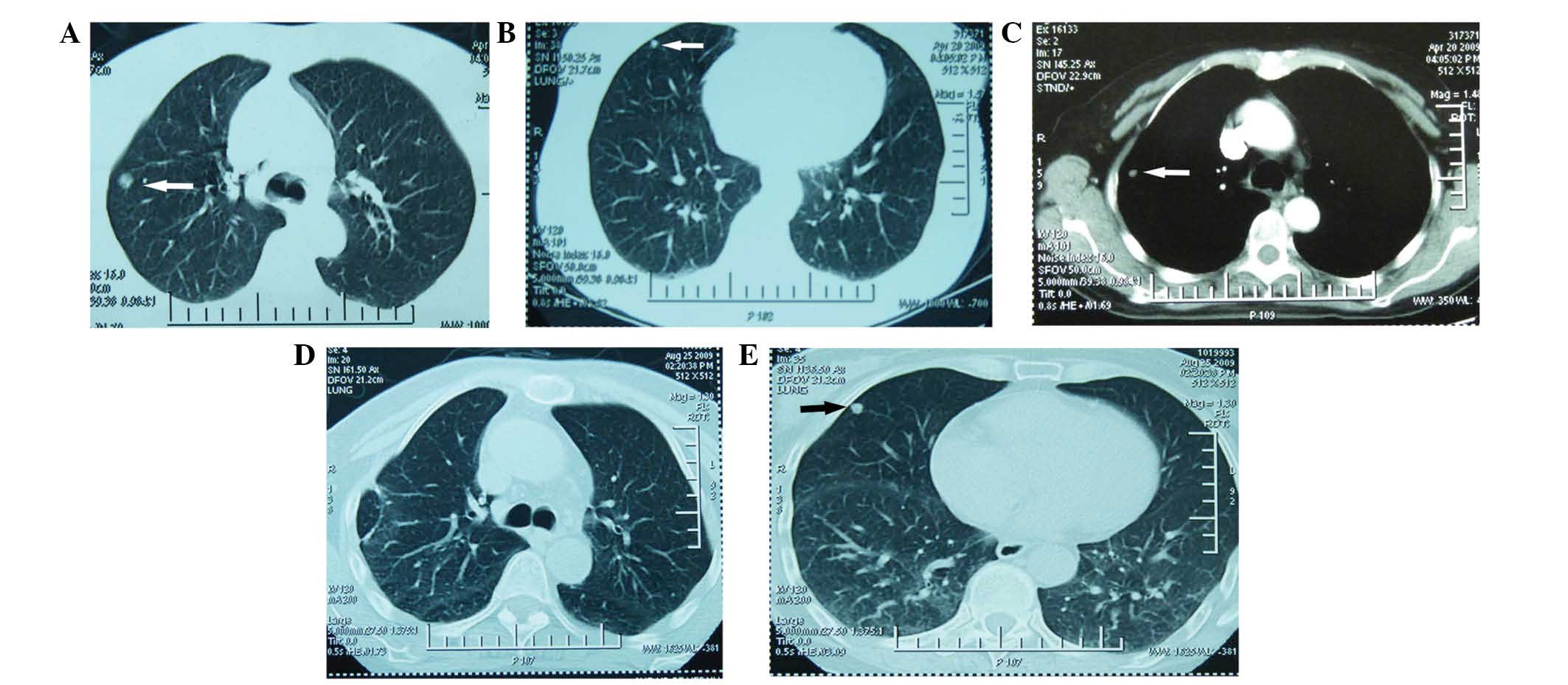
A pre-operative chest CT scan revealed multiple pulmonary nodules
in the superior lobe of the right lung (Fig. 3). Gamma Knife (dose of total, DT: 12
Gy/50%, 8 mmx1 1) was used to remove the intracranial tumor;
however, a postoperative MRI indicated that the tumor had not been
completely removed. In order to clarify the nature of the lesions
in the right lung, wedge resection of the superior lobe of the
right lung was performed 7 days later, to remove the nodules
located in the junction of the tip and posterior section under
direct vision of a thoracoscope. The pathological report indicated
transitional meningioma features, similar to those of the
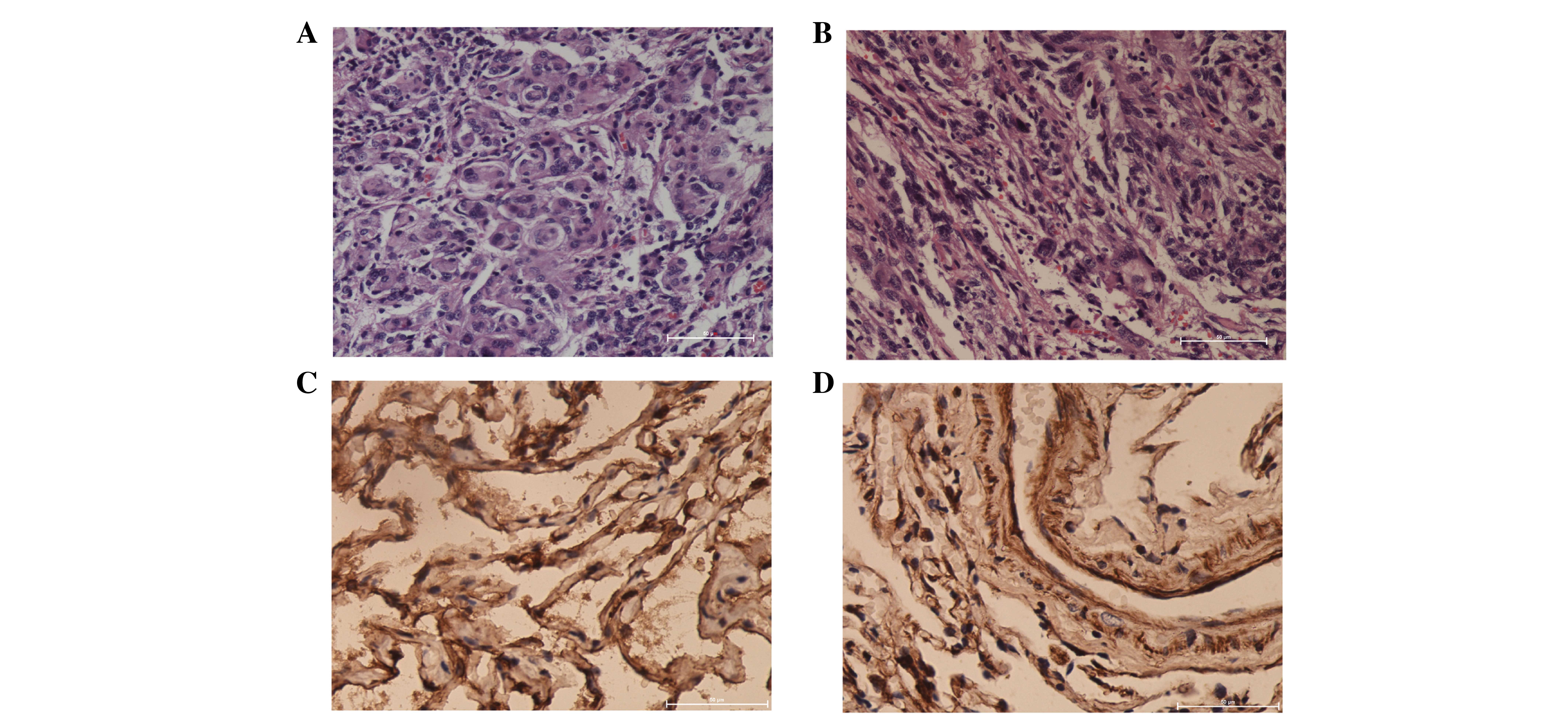
intracranial tumor. Histological examination revealed that the
tumor was positive for vimentin and epithelial membrane antigen
(Fig. 4). The nodules in the anterior
segment were placed under observation.
The patient recovered uneventfully, and was
discharged from hospital 10 days post surgery. The intracranial and
pulmonary residual tumors were kept under follow-up observation.
Compared with the previous image, it appeared that the tumor was
enlarged as indicated in the follow-up CT/MRI scans (Fig. 3E). In view of no notable clinical
symptoms at that time, the patient's family refused further
surgical treatment to remove the residual mass.
To date, the patient remains in a relatively stable
condition, except for Broca's aphasia. Regular clinical follow-ups
for the patient will continue.
Discussion
Meningiomas are slow growing tumors, which are
generally considered to be benign. Meningiomas account for 15–20%
of all intracranial tumors, and are twice as likely to occur in
females (1,30). Ectopic meningiomas are particularly
rare and the majority originate from embryonic nests of arachnoid
cells, which were trapped in ectopic locations during development.
Hoye et al (31) classified
these extracranial meningiomas into four groups, one of which is
extracranial metastases of meningiomas.
Meningiomas rarely metastasize; however, cases of
extracranial metastatic meningioma have previously been reported
(3,4,6–9). According to current statistics, the lung
is the most common site of metastasis (9). In addition, other sites, including the
liver, lymph node, bone and pleura, may also occasionally exhibit
metastases (2,10,32).
Pulmonary metastases rarely induce symptoms in the patient. They
typically present as single or multiple round, non-calcified
parenchymal nodules of varying size, and multiple deposits are
identified in 50% of cases (8). The
mean interval between diagnosis of the primary tumor and discovery
of the first metastases is ~6 years (8), although the longest interval documented
was 24 years (33). In addition,
metastases are frequently discovered following recurrence of the
primary lesion.
However, the mechanisms underlying metastasis remain
to be elucidated. Hematogenous metastasis may be the most likely
mechanism for extracranial spread. Figueroa et al (10) revealed that in 75% of patients
reported to have had metastasizing meningioma, metastases were
associated with previous surgery on the primary lesion or invasion
of the sinuses. A second route underlying the development of
metastasis may be via the cerebrospinal fluid pathway (12). It was hypothesized that surgical
interference may release the tumor from its cohesive state into the
bloodstream or cerebrospinal fluid. However, despite the relatively
large number of surgical resections performed, metastasis remains a
rare event (4).
The World Health Organization classification of
tumors of the nervous system details 15 histopathological variants
of meningioma (26). Extracranial
metastases from meningiomas are considered to be a significant
indicator of malignancy, and have been found to arise in 11–23% of
patients with anaplastic meningiomas (2,11,34,35). High
proliferative potential, as indicated by mitotic rate,
bromodeoxyuridine labeling index, proliferating cell nuclear
antigen labeling index or MIB-1 monoclonal antibody staining of
Ki-67 nuclear protein, has been suggested to enhance the risk of
metastases (36). However, the
clinical behavior of meningioma does not always correlate with
histological features. A higher rate of cellular proliferation is
not a requirement for the development of extracranial metastasis,
and individual meningiomas of any histological subtype are able to
metastasize (7,10,11,37).
In addition, a review of the literature suggested
that there may be multiple risk factors for metastasis, including
previous craniotomy venous sinus invasion, local recurrence,
papillary morphology and histological malignancy (13).
In the present case, the time between diagnosis of
the primary tumor and detection of right lung metastasis was ~2
years and 9 months, markedly shorter than the average time. Prior
to detection of the distant metastasis, multiple craniotomies,
radiotherapy and Gamma Knife treatments were performed in the
present case. The patient exhibited no clinical symptoms for a
significant time-period prior to the detection of multiple
pulmonary nodules in the superior lobe of the right lung. The
present case highlights the necessity for clinicians to perform
comprehensive examinations for patients with a history of recurrent
intracranial meningioma in order to detect distant metastases as
early as possible, even though the tumors are benign. Although
there was no clear evidence of spread through the hematogenous
route or cerebrospinal fluid in the present case, elucidation of
the mechanisms underlying hematogenous spread remains a
priority.
Acknowledgements
This study was funded by the Natioanal Natural
Science Foundation of China (grant no. 61271367).
References
|
1
|
Rachlin JR and Rosenblum ML: Etiology and
biology of meningiomas. Meningiomas. Al-Mefty O: Raven Press. (New
York). 27–35. 1991.
|
|
2
|
Pramesh CS, Saklani AP, Pantvaidya GH,
Heroor AA, Naresh KN, Sharma S and Deshpande RK: Benign
metastasizing meningioma. Jpn J Clin Oncol. 32:86–88. 2003.
View Article : Google Scholar
|
|
3
|
Kaminski JM, Movsas B, King E, Yang C,
Kronz JD, Alli PM, Williams J and Brem H: Metastatic meningioma to
the lung with multiple pleural metastases. Am J Clin Oncol.
24:579–582. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Fulkerson DH, Horner TG and Hattab EM:
Histologically benign intraventricular meningioma with concurrent
pulmonary metastasis: Case report and review of the literature.
Clin Neurol Neurosurg. 110:416–419. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Rawat B, Franchetto AA and Elavathil J:
Extracranial metastases of meningioma. Neuroradiology. 37:38–41.
1995. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Nabeya Y, Okazaki Y, Watanabe Y, Tohnosu
N, Yamazaki M, Matsuda M, Iizuka H, Akutsu N, Kono T, Sato H and
Kubosawa H: Metastatic malignant meningioma of the liver with
hypoglycemia: Report of a case. Surg Today. 28:953–958. 1998.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Kros JM, Cella F, Bakker SL, Paz Y, Geuze
D and Egeler RM: Papillary meningioma with pleural metastasis: Case
report and literature review. Acta Neurol Scand. 102:200–202. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kovoor JM, Jayakumar PN, Srikanth SG,
Indiria B and Devi MG: Solitary pulmonary metastasis from
intracranial meningiothelial meningioma. Australas Radiol.
46:65–68. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Erman T, Hanta I, Haciyakupoğlu S, et al:
Huge bilateral pulmonary and pleural metastasis from intracranial
meningioma: A case report and review of the literature. J
Neurooncol. 74:179–181. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Figueroa BE, Quint DJ, Mckeever PE and
Chandler WF: Extracranial metastatic meningioma. Br J Radiol.
72:513–516. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Drummond KJ, Bittar RG and Fearnside MR:
Metastatic atypical meningioma: Case report and review of the
literature. J Clin Neurosci. 7:69–72. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Chamberlain MC and Glantz MJ:
Cerebrospinal fluid-disseminated meningioma. Cancer. 103:1427–1430.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Adlakha A, Rao K, Adlakha H, et al:
Meningioma metastatic to the lung. Mayo Clin Proc. 74:1129–1133.
1999. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Tao CY, Wang JJ, Li H and You C: Malignant
intraventricular meningioma with craniospinal dissemination and
concurrent pulmonary metastasis. World J Surg Oncol. 12:2382014.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Scognamiglio G, D'Antonio A, Rossi G, et
al: CD90 expression in atypical meningiomas and meningioma
metastasis. Am J Clin Pathol. 141:841–849. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Rico-Cotelo M, Prieto-González Á,
Reyes-Santías RM, et al: Cervical lymphatic metastasis of an
intracranial meningioma. Rev Neurol. 56:225–228. 2013.(In Spanish).
PubMed/NCBI
|
|
17
|
Celenk F, Erkilic S, Durucu C, Baysal E
and Kanlikama M: Late metastasis of an intracranial meningioma to
the hard palate. J Craniofac Surg. 23:1912–1914. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Wang Z, Kong M, Li J, et al: Intraspinal
rhabdoid meningioma metastasis to the liver. J Clin Neurosci.
18:714–716. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Rampurwala M, Pazooki M and Schauer P:
Delayed hepatic metastasis from a benign fibroblastic meningioma
thirty-one years after surgical resection of the intracranial
tumor. J Clin Oncol. 29:e214–e215. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Moir JA, Haugk B and French JJ: Hepatic
metastasis via a ventriculo-peritoneal shunt from an intracranial
meningioma: Case report and review of the literature. Case Rep
Gastroenterol. 4:267–272. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Fulkerson DH, Horner TG and Hattab EM:
Histologically benign intraventricular meningioma with concurrent
pulmonary metastasis: Case report and review of the literature.
Clin Neurol Neurosurg. 110:416–419. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Akai T, Shiraga S, Iizuka H, et al:
Recurrent meningioma with metastasis to the skin incision - case
report. Neurol Med Chir (Tokyo). 44:600–602. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Williamson BE, Stanton CA and Levine EA:
Chest wall metastasis from recurrent meningioma. Am Surg.
67:966–968. 2001.PubMed/NCBI
|
|
24
|
Sironi M, Caneva A, Pasquinelli G, et al:
Aspiration biopsy cytology of pleuro-pulmonary metastasis from a
recurrent meningioma. Oncol Rep. 4:1165–1167. 1997.PubMed/NCBI
|
|
25
|
Tworek JA, Mikhail AA and Blaivas M:
Meningioma: Local recurrence and pulmonary metastasis diagnosed by
fine needle aspiration. Acta Cytol. 41:946–947. 1997.PubMed/NCBI
|
|
26
|
Simpson D: The recurrence of intracranial
meningiomas after surgical treatment. J Neurol Neurosurg
Psychiatry. 20:22–39. 1957. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Louis DN, Ohgaki H and Wiestler OD: The
2007 WHO classification of tumors of the central nervous system.
Acta Neuropathologica. 114:97–109. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Shin MS, Holman WL, Herrera GA and Ho KJ:
Extensive pulmonary metastasis of an intracranial meningioma with
repeated recurrence: Radiographic and pathologic features. South
Med J. 89:313–318. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Enam SA, Abdulrauf S, Mehta B, Malik GM
and Mahmood A: Metastasis in meningioma. Acta Neurochir (Wien).
138:1172–1178. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Demonte F and Al-Mefty O: Meningiomas.
Brain Tumors. Kaye AH and Laws ER Jr: Churchill Livingstone. (New
York). 675–704. 1995.
|
|
31
|
Hoye SJ, Hoar CS Jr and Murray JE:
Extracranial meningiomas presenting as tumor of the neck. Am J
Surg. 100:486–489. 1960. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Karasick JL and Mullan SF: A survey of
metastatic meningiomas. J Neurosurg. 40:206–212. 1974. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Stoller JK, Kavuru M, Mehta AC, Weinstein
CE, Estes ML and Gephardt GN: Intracranial meningioma metastatic to
the lung. Cleve Clin J Med. 54:521–527. 1987. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Evans JJ, Lee JH, Suh J and Golubic M:
Neurosurgery: Principles and Practice. Moore AJ and Newell DW:
Springer-Verlag. London: 205–234. 2005. View Article : Google Scholar
|
|
35
|
Kabus D, Sidhu GS, Wieczorek RL and Choi
HS: Metastatic meningioma. Hemangiopericytoma or angioblastic
meningioma? Am J Surg Pathol. 17:1144–1150. 1993. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Ohta M, Iwaki T, Kitamoto T, Takeshita I,
Tateishi J and Fukui M: MIB1 staining index and scoring of
histologic features in meningioma. Indicators for the prediction of
biologic potential and postoperative management. Cancer.
74:3176–3189. 1994. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Hishima T, Fukayama M, Funata N, Mochizuki
M, Hayashi Y, Koike M and Ikeda T: Intracranial meningioma
masquerading as a primary pleuropulmonary tumor. Pathol Int.
45:617–621. 1995. View Article : Google Scholar : PubMed/NCBI
|