Introduction
Pericardial cysts and primary/secondary lymph node
tumors are common in the middle mediastinum. By contrast,
neurogenic tumors rarely occur in this location, but are the most
common type of tumor in the posterior mediastinum. Neurogenic
tumors are typically encapsulated and can be classified into nerve
sheath, ganglion cell and paraganglionic cell neoplasms (1). Neurilemmomas are an example of one rare
type of mediastinal tumor originating from the vagus nerve
(2).
Mediastinal tumors have a higher incidence rate in
women compared with men. Furthermore, the tumors are malignant in
~50% of children and <10% of adults (3). Although mediastinal tumors typically
arise from the spinal nerve root, they may arise from any
intrathoracic nerve (1).
By performing a radiological examination,
mediastinal tumors can be observed as sharply-demarcated lesions
with rare calcifications (4). A
combination of multiple medical imaging techniques, including
computed tomography (CT), magnetic resonance imaging (MRI) and
percutaneous puncture biopsy, facilitates the characterization of
mediastinal tumors. Occasionally, video-assisted thoracic surgery
(VATS) exhibits advantages over thoracotomy for the
characterization of complex mediastinal tumors. VATS allows an
improved intraoperative view, which results in little tissue damage
and quicker patient recovery.
The present study reports the case of a large
schwannoma in the middle mediastinum, which was successfully
resected by VATS.
Case report
In January 2014, a 61-year-old woman was admitted to
The First Hospital of Jilin University (Changchun, China) with a
history of chest tightness and coughing for 1 year and facial edema
for 10 days. The patient described experiencing the symptoms of
chest tightness and coughing after exercise, which were relieved
following rest. The patient visited the hospital for treatment due
to the development of dyspnea and facial edema.
At presentation, the patient had a cough with no
symptoms of fever, sweating, ptosis, general fatigue or swallowing
impairment. The patient's diet and urine were normal, and little
change in body weight had occurred. Analysis of the patient's
medical history demonstrated no high blood pressure, coronary
atherosclerotic heart disease, glycuresis, hepatitis, bacillary
phthisis, food or drug allergies, and no drinking or smoking habit.
Physical examination determined that the patient was in a poor
general condition, with facial swelling, distention of the jugular
vein and thoracic symmetry. The patient's right tactile fremitus
was stronger than the left, with dullness on percussion and weak
breathing sounds from the right lung.
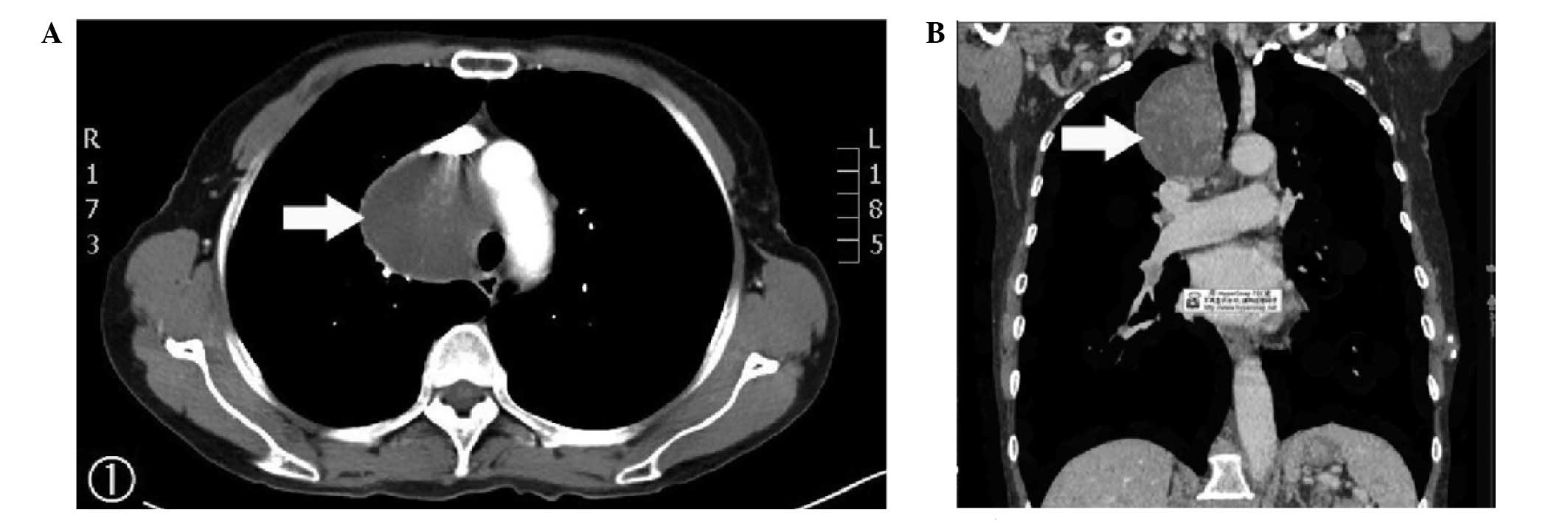
Pre-operative chest radiography, enhanced CT and
three-dimensional CT identified a well-circumscribed mass. The
large cyst measured 6.5×6.1×5.0 cm, located anterior to the trachea
and posterior to the superior vena cava. Enhanced CT was uneven and
the superior vena cava appeared flattened due to the pressure on
the right vagus nerve (Fig. 1). The
laboratory analyses and electrocardiogram results were normal.
Determination of cardiac function identified fractional shortening
of 34% (normal range, 25–45%) and an ejection fraction of 63%
(normal range, 50–65%). Furthermore, an abdominal ultrasound
revealed that the structures of the liver, gallbladder, pancreas
and kidneys were normal. In consideration of the aforementioned
observations, a mediastinal tumor was diagnosed.
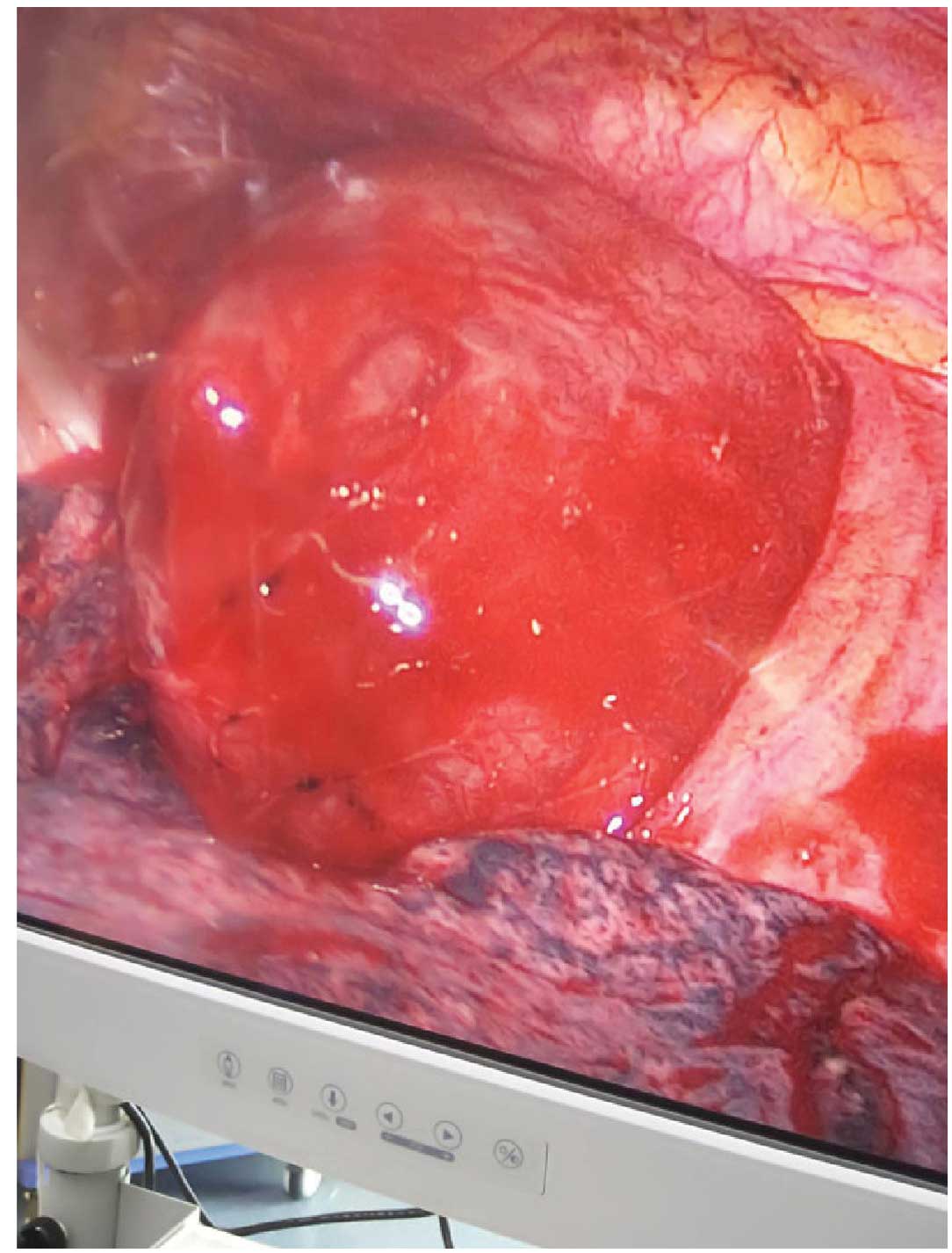
Prior to mediastinal tumor resection, the patient
underwent VATS under general anesthesia. VATS identified a single
solid tumor in the right mediastinum; it was strong but pliable in
texture, with a spherical shape and a surrounding capsule
integrated with dark red adjacent tissue. The tumor measured
~6.5×6.1×5.0 cm in size (Fig. 2).
Using video assistance, one small incision was made ~3 cm between
the right posterior axillary line and the fourth intercostal
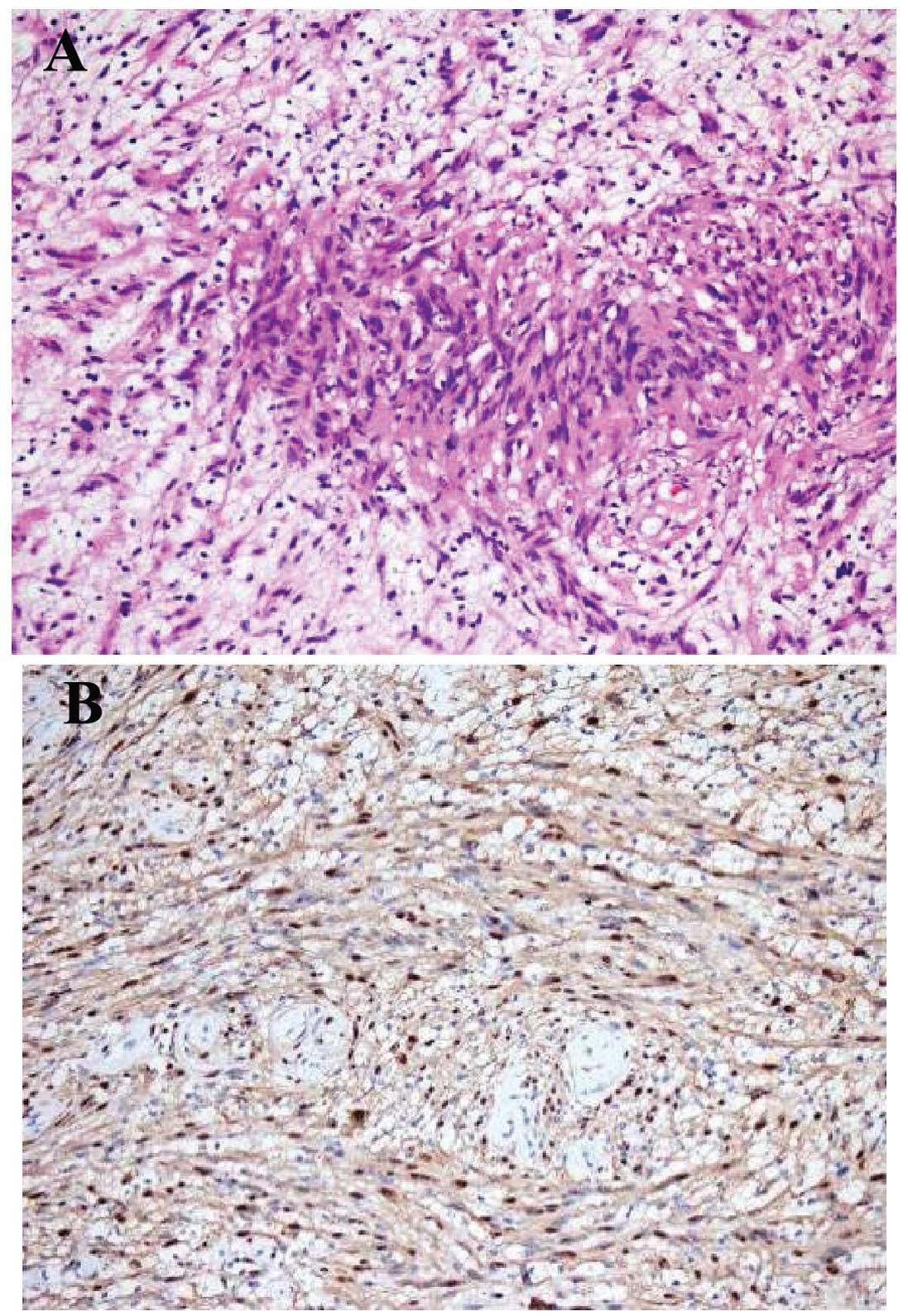
anterior axillary line, and the tumor was removed. Subsequent
pathological examination determined the distribution of spindle
cells in fascicles in loose stroma (hematoxylin and eosin staining;
magnification, ×200) and strong staining of S-100 protein,
clarifying the diagnosis of a schwannoma (Fig. 3). Following the surgery, the symptoms
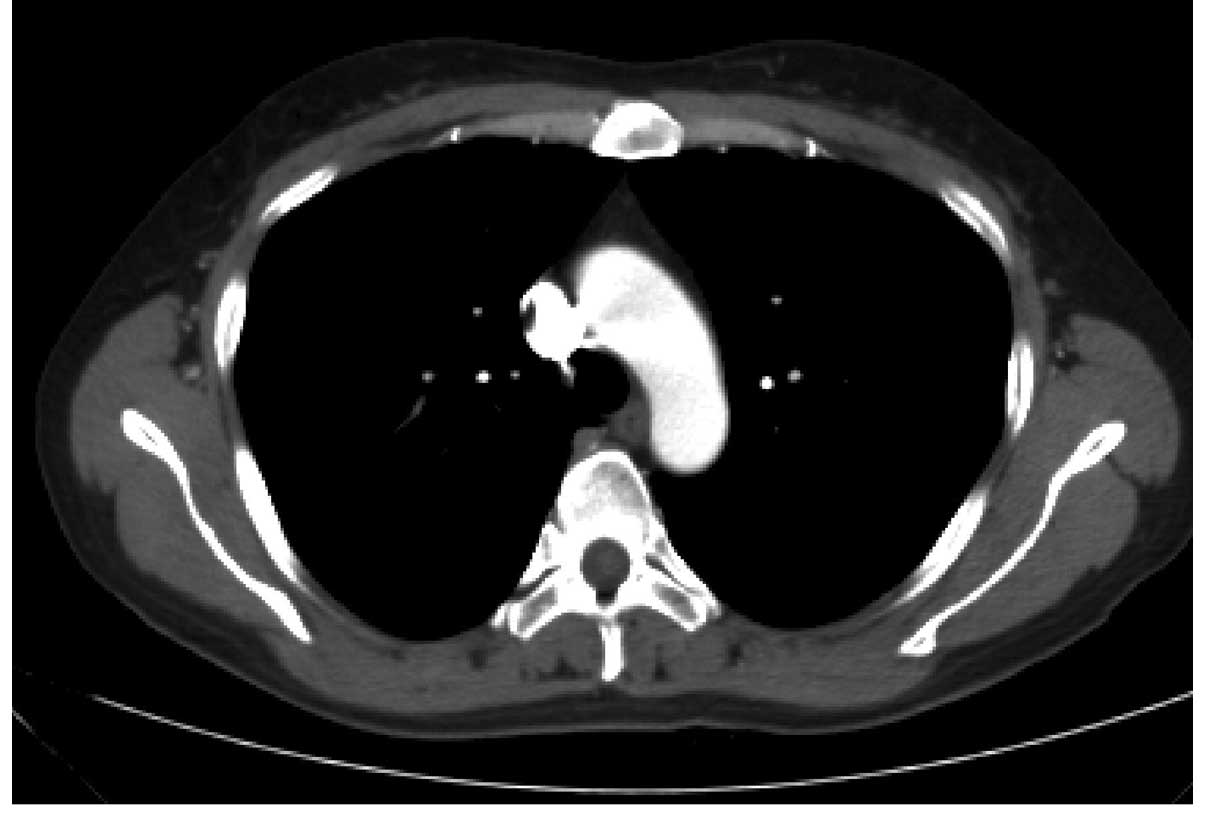
of chest pain, cough and facial edema disappeared. Furthermore,
post-operative chest CT identified no marked abnormalities of the
mediastinum (Fig. 4). During the
6-month follow-up period, no clinical manifestations or tumor
recurrence were observed. At the time of writing, the patient
remained alive.
Written informed consent was obtained from the
patient's guardian for the publication of the present case report
and any accompanying images.
Discussion
Mediastinal masses are typically divided into
anterior, middle and posterior tumors. Common primary tumors of the
anterior mediastinum include thymoma, thymic cysts of germ cell
tumors, and lymphoma and thyroid tumors (5). Embryonic cysts, pericardial cysts and
primary/secondary lymph node tumors are more common in the middle
mediastinum, whereas cystic lymphangioma is rare. By contrast,
neurogenic tumors are more common in the posterior mediastinum.
Only 5–15% of neurogenic tumors are cancerous and patients often
exhibit no evident symptoms. However, a small number of patients do
present with symptoms, including difficulty breathing, chest pain,
coughing, obstructive pneumonia and numbness of the limbs, due to
the pressure of the tumor on the trachea (2). Neurogenic tumors include neurinoma,
neurofibroma, neural sarcoma, paraganglioma, neuroblastoma,
sympathetic neuroma, paraganglioma and pheochromocytoma (6). Furthermore, benign schwannomas of the
vagus nerve are a rare type of middle mediastinal neurogenic tumor
of nerve sheath origin (1).
In the present study, enhanced chest CT was
performed to detect a mass in the mediastinum, anterior to the
trachea and posterior to the vena cava. The mass measured
6.5×6.1×5.0 cm in size with a clear boundary. Enhanced CT was
uneven, the superior vena cava was flattened due to pressure on the
vagus nerve and cysts could be distinguished. As neurogenic tumors
of the mediastinum predominantly originate from the spinal nerve
and paravertebral sympathetic trunk, they are commonly located on
each side of the thoracic paraspinal trench. However, neurogenic
tumors of the mediastinum rarely originate from the intrapulmonary,
phrenic or vagus nerves (1,3). Furthermore, patients with schwannoma
generally exhibit neurological symptoms; however, the patient in
the current case did not exhibit such symptoms, therefore, a
definite diagnosis could not be established.
In the present case, the tumor was located in the
middle mediastinal compartment, anterior to the trachea and
posterior to the superior vena cava. Therefore, VATS was employed
as opposed to a thoracotomy for the resection of the mediastinal
neurogenic tumor. Subsequent histological and immunohistochemical
analysis of the resected tumor facilitated the diagnosis of a
schwannoma. Neurogenic tumors typically arise in the posterior
mediastinum and are rare in the middle mediastinum, therefore, it
is difficult to determine a diagnosis on the basis of clinical
manifestation and iconography alone (7). Histopathological examination can aid in
determining a definite diagnosis.
In the present case, the tumor was successfully
removed using VATS. A thoracotomy can be performed as an
alternative resection strategy, however, the location of the tumor
in the middle mediastinum, particularly in the superior vena cava,
requires a good field of vision for the safe isolation of the tumor
without damage to vital mediastinal structures. In addition, the
clinician should be aware of abnormal blood vessels and ensure a
complete resection of the tumor. Thus, when iconography cannot not
provide a sufficient evaluation of the mediastinal mass, the
possibility of neurogenic tumor should be considered, despite the
tumor not occurring in the posterior mediastinum.
In conclusion, schwannoma in the middle mediastinum
is rare, however, in certain instances, the tumor may grow to a
large size. A combination of multiple medical imaging techniques,
such as CT, MRI and percutaneous puncture biopsy, facilitate the
diagnosis. Successful resection of middle mediastinal tumors by
thoracoscopy is rare. Selection of an appropriate surgical approach
is conducive to the successful rehabilitation of patients and a
reduction in complications.
References
|
1
|
Strollo DC, Rosado-de-Christenson ML and
Jett JR: Primary mediastinal tumors: Part II. Tumors of the middle
and posterior mediastinum. Chest. 112:1344–1357. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Mordant P, Le Pimpec-Barthes F and Riquet
M: Neurogenic tumors of the mediastinum in adults. Rev Pneumol
Clin. 66:81–94. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Kaneko M, Matsumoto I, Oda M and Watanabe
G: Multiple schwannoma of the intrathoracic vagal nerve; report of
a case. Kyobu Geka. 61:820–823. 2008.PubMed/NCBI
|
|
4
|
Tomiyama N, Honda O, Tsubamoto M, Inoue A,
Sumikawa H, Kuriyama K, Kusumoto M, Johkoh T and Nakamura H:
Anterior mediastinal tumors: Diagnostic accuracy of CT and MRI. Eur
J Radiol. 69:280–288. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Priola AM, Priola SM, Cardinale L, Cataldi
A and Fava C: The anterior mediastinum: Diseases. Radiol Med
(Torino). 111:312–342. 2006. View Article : Google Scholar
|
|
6
|
Hussein HA and Goda HA: Paravertebral
neurogenic tumors with intraspinal extension: Preoperative
evaluation and surgical approach. J Egypt Natl Canc Inst. 21:12–22.
2009.PubMed/NCBI
|
|
7
|
Cho JH, Kim J, Kim K, Choi YS, Kim HK and
Shim YM: A comparative analysis of video-assisted mediastinoscopy
and conventional mediastinoscopy. Ann Thorac Surg. 92:1007–1011.
2011. View Article : Google Scholar : PubMed/NCBI
|