Introduction
The defining feature of a mature cystic teratoma is
the presence of differentiated components of any combination of two
or three embryonal layers (endoderm, mesoderm and ectoderm)
(1).
Although mature teratomas are the most frequently
occurring ovarian germ cell tumors (16–20% of all ovarian
neoplasms), the incidence of fallopian tube teratomas is extremely
low (2), with only ~70 cases of
mature fallopian tube teratoma reported in the literature (2). Teratomas of the fallopian tube are
generally solitary tumors. However, in certain cases, they may be
accompanied by various ovarian neoplasms. In the literature, the
accompanying neoplasms have consisted of ovarian teratomas
(including a struma ovarii) in 6 cases, benign ovarian tumors other
than teratomas in 3 cases and ovarian cystadenocarcinomas in 2
cases (3–5). Fallopian tube teratomas are usually
asymptomatic, but they may occasionally lead to reduced parity,
leukorrhea, menstrual irregularity, postmenopausal bleeding or
abdominal pain (5). The present study
reports the case of patient with a mature cystic teratoma of the
left fallopian tube coexisting with mature cystic teratomas of the
bilateral ovaries.
Case report
A 31-year-old woman (gravida 0, para 0) was referred
to the Department of Gynecology, Gyeongsang National University
Hospital (Gyeongsangnam, Korea) after an adnexal mass was
identified during pelvic ultrasonography, which was performed at a
regular checkup in April 2012. Computed tomography scans revealed a
multi-lobulated, 4.5×3.5-cm cystic mass, with fat and calcification
in the left adnexa, which was suspected to be a cystic teratoma of
the left ovary. The results of a complete blood count, urinalysis,
serological tests, electrocardiogram and chest X-ray were within
the normal ranges. Serum cancer antigen (CA)-125 and CA19-9 levels
were 18 and 4 U/ml, respectively (normal ranges, <35 and <37
U/ml, respectively).
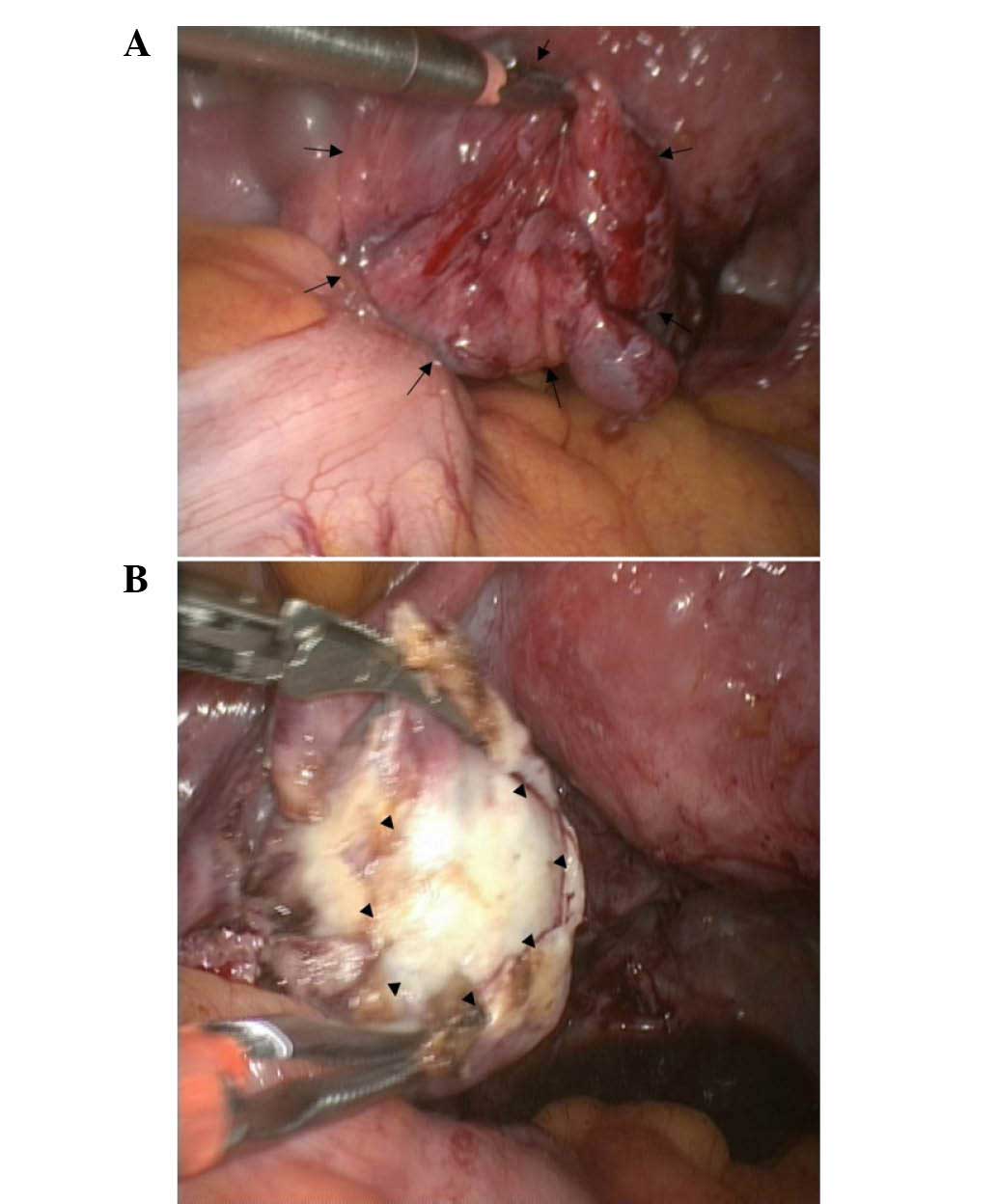
The patient underwent laparoscopic surgery with a
diagnosis of a cystic teratoma of the left ovary. At the time of
surgery, the left fallopian tube appeared to be distended by 4×3 cm
and contained cream-colored sebaceous material and hair (Fig. 1A). The ipsilateral ovary also
contained cream-colored sebaceous material and hair (Fig. 1B). The uterus, the right ovary and the
right fallopian tube were evaluated as normal. The patient
subsequently underwent a left salpingectomy and left ovarian
cystectomy.
The CT images were retrospectively evaluated with
focus on the left fallopian tube components after surgery. Computed
tomography scans showed a cystic mass with a fat attenuation
component in the left hemipelvis. The mass was connected with a
dilated folding tubular structure. The tubular structure was 5 mm
in diameter and demonstrated fat attenuation (−105 HU). These CT
findings were consistent with those of fallopian tube teratomas
(Fig. 2).
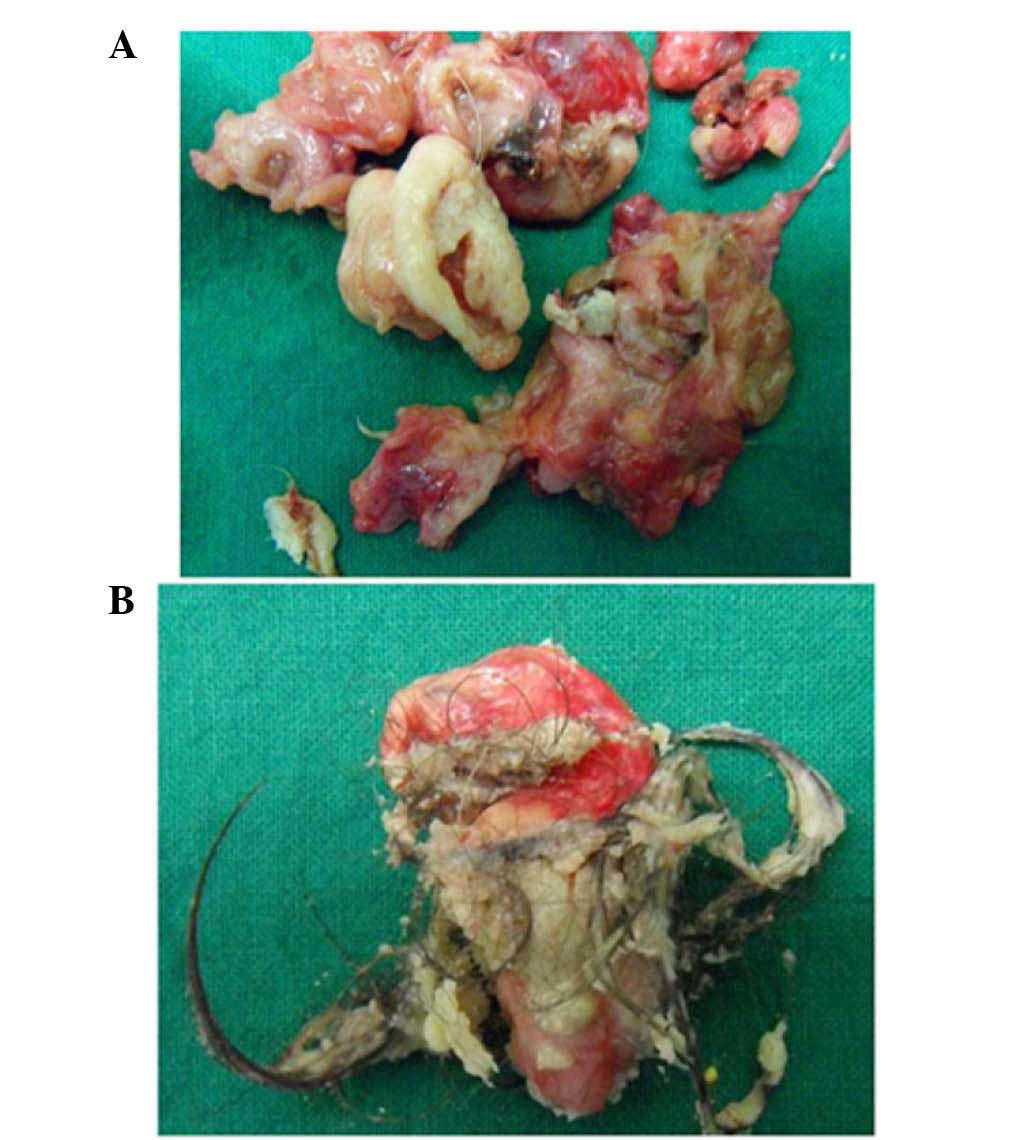
Grossly, a cystic mass, 3.5 cm in diameter, was
present within the ampulla of the fallopian tube, which was filled
with fatty tissue and yellowish greasy material and hairs (Fig. 3A). The left ovary exhibited fatty,
tan-pink, focally calcified cut surfaces, which were surrounded by
a 2.0×2.0×1.5-cm uniloculated cyst containing coarse black hair
(Fig. 3B). The samples were grossly
examined, dissected, embedded in paraffin blocks and cut into 3 µm
sections. The sections were then stained using standard hematoxylin
and eosin, and representative blocks were selected from each tumor
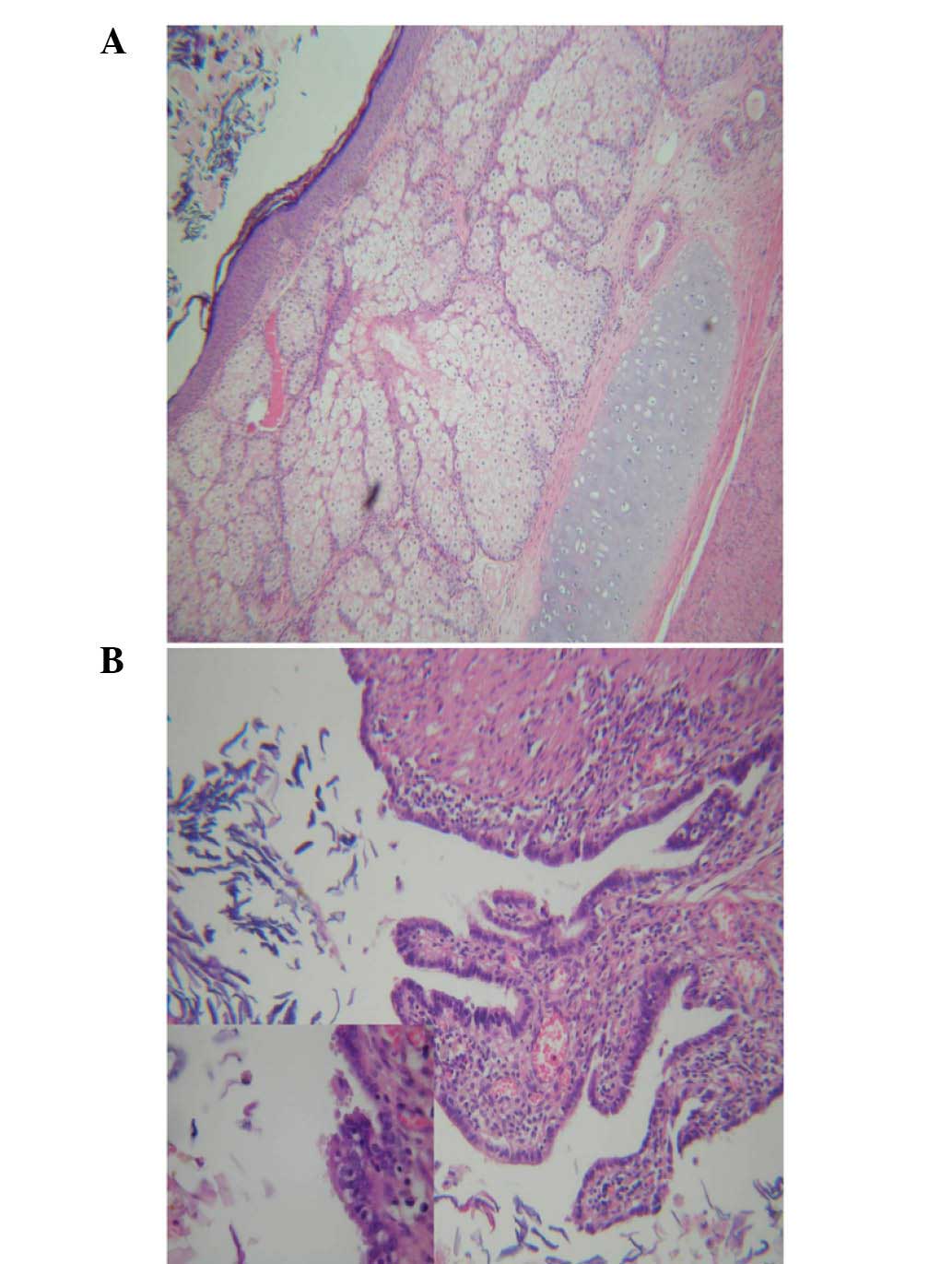
for microscopic analysis. Microscopic examination revealed squamous
epithelium with sebaceous glands, and hair follicles with mucous
glands and mature cartilage (Fig.
4).
Histopathological examination showed components from
each germ cell layer; therefore, the diagnosis of mature cystic
teratomas of the left fallopian tube and ovary was confirmed. The
patient was discharged from the hospital at 3 days post-surgery.
There were no abnormal findings when the patient revisited the
Department of Gynecology, Gyeongsang National University Hospital
at 10 days post-surgery. At 26 months post-surgery, the patient
became pregnant and underwent a cesarean section at 39+2 weeks due
to fetal distress. A cystic mass of the right ovary was
incidentally found during cesarean section. A right ovarian
cystectomy was performed and histopathology revealed it to be a
teratoma. The patient continued to receive annual follow-up after
the second surgical intervention and demonstrated no evidence of
disease at a routine 2-year follow-up examination. Written informed
consent was obtained from the patient for the publication of this
report and any accompanying images.
Discussion
Tumors of the fallopian tube are uncommon. Primary
malignant tumors of the fallopian tube account for 0.3–1.9% of
gynecological malignancies (6).
Benign tumors of the fallopian tube are even less common, the
majority being adenomatoid tumors (7). Teratomas of the fallopian tube are rare,
and to date, only ~70 cases have been reported in the global
literature (3). Due to their rarity,
the actual incidence and histogenesis of mature cystic teratoma of
the fallopian tube remains unknown (8).
This condition affects patients aged between 17–67
years, although the majority of patients are 30–49 years of age
(2). An analogous age-associated
trend is found for size (range, 0.2–31 cm in diameter) and weight
(≤2,400 g) (9). As a result, the
volume of the teratoma, and thus its speed of growth, appears to be
inversely proportional to patient age, with juveniles exhibiting
greater volumes than older patients. The gravidity of patients with
teratomas of the fallopian tube is variable. The majority of
studies have reported a high prevalence rate in multipara patients
compared with nullipara or primipara patients (2,3,8). The patient in the present case was
nullipara. The patient underwent a left ovarian cystectomy and left
salpingectomy. At 26 months post-surgery, the patient became
pregnant and underwent a cesarean section. A right ovarian teratoma
was found incidentally.
The literature suggests that teratomas are slightly
more prevalent in the right fallopian tube than in the left; in a
recent study, 34 cases occurred on the right side, 28 occurred on
the left side and 6 occurred bilaterally (3). Intraluminal teratomas are the most
common type and may also occur at intramural and serosal locations
(internal layer, 22 cases; serosal layer, 4 cases; muscular layer,
2 cases; and combined, 3 cases) (3,5).
Teratoma is able to develop in any region of the
fallopian tube, but the ampulla and isthmus are the most common
sites (9). The diagnosis and clinical
manifestation of teratomas are associated with their location.
Furthermore, teratomas of the fallopian tube have been associated
with subfertility, infertility, irregular menstruation,
menorrhagia, leukorrhea, ectopic pregnancy, adnexal masses and
lower abdominal pain (8–12). The patient in the present study
experienced no specific symptoms. Occasionally, tubal teratomas may
cause infertility, however, the patient in the present study
conceived spontaneously at 26 months post-surgery.
Teratomas of the fallopian tube are generally
solitary tumors (2,9–11).
However, certain cases have been accompanied by various
gynecological neoplasms, including struma ovarii (4), ovarian teratoma (5), uterine myoma (3,5), ectopic
pregnancy (8) and uterine anomaly
(13) Moreover, certain cases have
also been associated with gynecological malignancies, such as
ovarian adenocarcinoma (5),
endometrial carcinoma (14) and
cervical squamous carcinoma (5).
The methods used for the detection of this neoplasm
include ultrasonography, pelvic CT scan, nuclear magnetic resonance
imaging, hysterosalpingography and laparoscopy (10,13,15).
However, tubal teratomas are not usually preoperatively diagnosed
due to their ambiguous clinical manifestation. To date, no cases
involving preoperative diagnosis have been reported. All reported
cases have been identified incidentally during surgical procedures
and subsequently confirmed by histopathological analysis. The
prognosis for such patients is favorable.
In conclusion, the present case described a patient
with a mature cystic teratoma of the left fallopian tube, in
addition to bilateral ovarian teratomas. If a patient presents with
an adnexal mass, it is important for gynecological surgeons to
consider the occurrence of tubal teratomas when making a
differential diagnosis. Although the incidence of tubal teratomas
is low, it is necessary to be aware of this possibility. It is also
important to consider that tubal teratomas may be associated with
other gynecological conditions. Thus, the abdomen and pelvis should
be inspected in a meticulous manner and every effort should be made
to identify coexisting lesions.
References
|
1
|
Robert JK: Mature cystic teratoma.
Blaustein's Pathology of the Female Genital Tract. 4th.
Springer-Verlag: New York; pp. pp879–883. 1994
|
|
2
|
Khatib G, Guzel AB, Kucukgoz-Gulec U,
Vardar MA, Musaev A and Melekoglu R: Mature cystic teratoma of the
fallopian tube. J Obstet Gynaecol. 33:120–124. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Chao T, Chao J, Kuan LJ, Li YT, Kuo TC,
Chang YC and Nieh S: Mature solid teratoma of the fallopian tube
associated with uterine leiomyomas. J Chin Med Assoc. 71:425–427.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Hoda SA and Huvos AG: Struma salpingis
associated with struma ovarii. Am J Surg Pathol. 17:1187–1189.
1993. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Mazzarella P, Okagaki T and Richart RM:
Teratoma of the uterine tube. A case report and review of the
literature. Obstet Gynecol. 39:381–388. 1972.PubMed/NCBI
|
|
6
|
Raju KS, Barker GH and Wiltshaw E: Primary
carcinoma of the fallopian tube. Report of 22 cases. Br J Obstet
Gynaecol. 88:1124–1129. 1981. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Fox H and Buckley CH: The female genital
tract and ovaries. Oxford Textbook of Pathology. 2a:McGee JOD,
Isaacson PG and Wright NA: pp1613–1614. 1992.
|
|
8
|
Kutteh WH and Albert T: Mature cystic
teratoma of the fallopian tube associated with an ectopic
pregnancy. Obstet Gynecol. 78:984–986. 1991.PubMed/NCBI
|
|
9
|
Ingec M, Kadanali S and Erdogan F: Huge
teratoma of the fallopian tube: A case report. J Reprod Med.
52:247–249. 2007.PubMed/NCBI
|
|
10
|
Fujiwara S, Yamashita Y, Yoshida Y, Terai
Y, Okuda K and Ohmichi M: Mature cystic teratoma of the fallopian
tube. Fertil Steril. 94:2708–2709. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Johnson C and Hansen KA: Mature cystic
teratoma of the fallopian tube. Fertil Steril. 86:995–996. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Matts SJ: An unusual cause of right iliac
fossa pain for the gynaecologist: Benign fallopian tube teratoma. J
Obstet Gynaecol. 18:194–195. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Yoshioka T and Tanaka T: Mature solid
teratoma of the fallopian tube: Case report. Eur J Obstet Gynecol
Reprod Biol. 89:205–206. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Roncati L, Barbolini G, Ghirardini G and
Rivasi F: Mature solid teratoma of the fallopian tube mimicking
metastasis of endometrial adenocarcinoma: A case report. Int J Surg
Pathol. 18:561–563. 2010.PubMed/NCBI
|
|
15
|
Li S, Fang X, Chen J and Xia X: Mature
cystic teratoma of the fallopian tube associated with incomplete
uterine mediastinum: A case report and literature review. Oncol
Lett. 6:153–155. 2013.PubMed/NCBI
|