Introduction
Cervical cancer is the most common malignant tumor
of the female reproductive system in China. It is diagnosed mostly
at advanced stages when its prognosis is poor. The 5-year survival
rate is only 60%. The survival rate of patients with distant
metastasis is even lower. In recent years, with the progresses made
in surgical treatments, radiotherapy and chemotherapy, the 5-year
survival rate of patients has improved. However, the long-term
survival rate is still not satisfactory. Therefore, newer
approaches like gene therapy against tumor proliferation and
invasion have gained widespread interest (1). Hepsin is a recently discovered gene, the
hepsin protein is involved in the dissolution of the cell membrane
matrix and results in abnormal signal transduction between cells,
moreover, the high expression of hepsin is related to the
development and metastasis of malignant tumors (2). The high mobility group box 1 (HMGB1)
protein, belonging to high mobility group protein family, is a
non-histone chromosomal protein, expressed in the early stages of
embryonic development, and is almost absent from highly
differentiated tissues. HMGB1 has been confirmed to be present in
malignant, invasive and poor-prognosis tumors (3). In this study, the immunohistochemical SP
method was used to detect HMGB1 and hepsin protein expression in
cervical carcinoma and control tissues. We studied the relationship
of the levels of expression of these proteins in tumors with their
rates of invasion, and metastasis, as well as their prognoses. Our
results point to possible pathogenesis mechanisms, aids the search
for new tumor markers to more accurately predict prognosis, and
provide new ideas for genetic target treatments of cervical
cancer.
Patients and methods
Patient data
Seventy cervical cancer patients who initially
received surgical treatments and had completely preserved clinical
and pathological data, in the Department of Obstetrics and
Gynecology, Xuzhou Central Hospital from May 2008 to June 2010,
were selected to participate in the study. Inclusion criteria
included: i) A definite pathological diagnosis; ii) clinical data
were complete; iii) no radiotherapy or chemotherapy had been
performed before operation; and iv) there were no brain, liver,
kidney or other organ dysfunctions. The age of the patients ranged
from 22 to 74 years with an average of 42.6±13.2 years. There were
59 cases of squamous cell carcinoma and 11 cases of adenocarcinoma.
Classification according to the FIGO standards (4) placed 28 cases in the low degree (I and
II classification), and 42 in the high degree (III and IV
classification). Also, based on pathological differentiation, there
were 8 patients with high differentiation, 25 with moderate
differentiation, and 37 with poor differentiation, and 47 patients
had lymph node metastasis, and 23 did not have any. Tissues 2 cm
away from the tumor border were used for the paracancerous tissue
group, and 20 cases of normal cervical tissue, from accessory
resections were taken for the control group. Comparing the average
ages of the control and the cervical cancer groups, the difference
was not statistically significant (P>0.05), indicating that the
division in both groups could be used for other comparisons. All
subjects signed written informed consents and the Ethics Committee
of Xuzhou Central Hospital approved the study. The 70 cervical
cancer patients were followed-up; the last day of the follow-up was
July 1, 2015, and the average follow-up time was 52.1 months.
Immunohistochemistry
Paraffin-embedded tissues were collected and
immunohistochemistry used the SP method. Mouse polyclonal hepsin
antibody (dilution, 1:100; cat. no. sc-517056) and mouse monoclonal
HMGB1 antibody (dilution, 1:150; cat. no. sc-135809) (both from
Santa Cruz Biotechnology, Inc., Santa Cruz, CA, USA) were used. SP
immunohistochemical kits were purchased from Beijing Zhongshan
Golden Bridge Biotechnology Co. (Beijing, China). Experimental
steps were conducted according to the kit's specifications.
Phosphatase-buffered saline (PBS) was used instead of primary
antibody as a negative control, and the positive control was an
antibody known to be positive on the samples.
Result judgments
HMGB1 positive staining signal was brown and
disseminated in small particles, all of which were located in the
cytoplasm of the cells. The hepsin protein was distributed in the
nucleus and the cytoplasm and consisted of brownish yellow or brown
particles. For each slice, 10 consecutive views at ×400
magnification were examined, 200 cells were counted in each view,
and all the positive cells were counted, in order to calculate the
positivity rate. The percentage of positive cells were then
calculated, and each sample was assigned points: 0–5% was noted as
0 points, 6–25% was noted as 1 point, 26–50% was 2 points, and more
than 50% was noted as 3 points. Additionally, the staining
intensity was also ranked by points: Unpigmented cells were marked
0 points, pale yellow cells were given 1 point, brownish-yellow
cells were given 2 points, and brown cells were given 3 points.
Multiplying the points of both scores resulted in definite
comprehensive scores: A score of 0–1 meant tissue was the negative
for HMGB1 or hepsin staining, a score of 2–3 meant the tissue was
weakly positive (+), 4–6 meant tissue was moderately positive (++)
and a score of 9 meant the tissue was strongly positive (+++).
Statistical analysis
The SPSS software package (SPSS, Inc., Chicago, IL,
USA) was used for data analysis, measurement data were expressed by
mean ± SD. The t-test (Fisher's exact test) was used in comparison
between groups, χ2 test and exact tests were used to
compare the rate of two samples, and for correlations the Pearson's
test was adopted. The survival rate was calculated using the
Kaplan-Meier survival curve and was analyzed by the log-rank test.
A P<0.05 was considered to indicate a statistically significant
difference.
Results
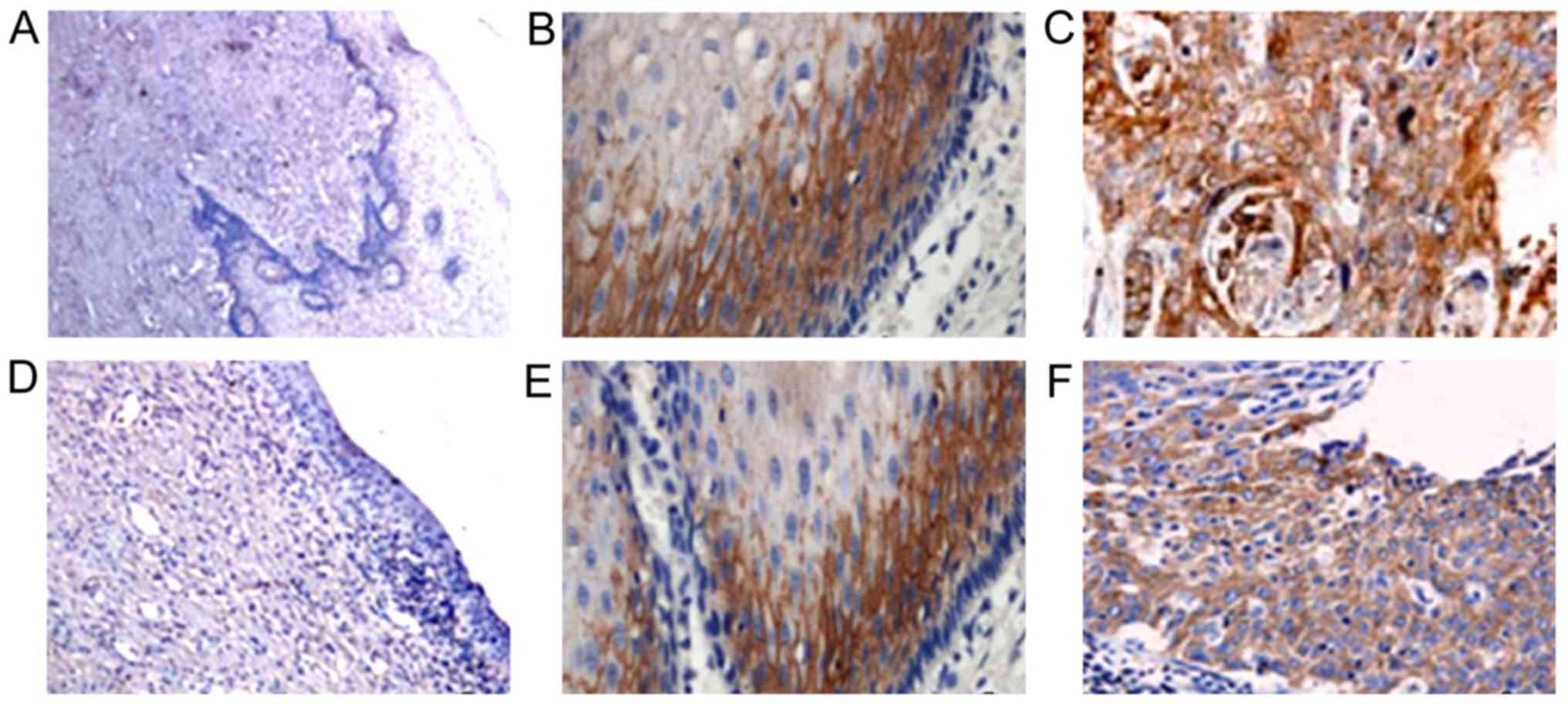
The expression of HMGB1 and hepsin in
cervical carcinoma, paracancerous and normal tissues
HMGB1 was mainly expressed in the cytoplasm of
cervical cancer cells, and was almost absent from normal tissues
(only 5% of them had some expression). The positive rate for
paracancerous tissues was 22.9% (16/70), and the differences
between these two groups had statistical significance (P<0.05).
The positive expression rate of HMGB1 in cervical cancer tissues
was 95.7% (67/70), and when compared to the rates in the normal and
paracancerous groups the differences were statistically significant
(P<0.05).
The hepsin protein was mainly expressed in the
cytoplasm of the cervical cancer cells, and there were only 2 cases
of hepsin expression in 20 cases of normal tissues (positive rate
of 10%). The positive expression rate in paracancerous tissues was
61% (43/70), and in the cervical carcinoma group was 90% (63/70),
the differences among the three groups were statistically
significant (P<0.05) (Table I and
Fig. 1).
 | Table I.Expression levels of HMGB1 and hepsin
in different tissues (n, %). |
Table I.
Expression levels of HMGB1 and hepsin
in different tissues (n, %).
|
|
| Positive rate |
|---|
|
|
|
|
|---|
| Tissues | Cases | HMGB1 | Hepsin |
|---|
| Normal | 20 | 5.0% (1/20) | 10% (2/20) |
| Paracancerous | 70 | 22.9% (16/70) | 61% (43/70) |
| Cervical cancer | 70 | 95.7% (67/70) | 90% (63/70) |
| F-value |
| 24.581 | 11.538 |
| P-value |
| 0.001 | 0.001 |
Relationship between expression of
HMGB1 and hepsin with the pathological and clinical signs of
cervical cancer
In 70 cases of cervical cancer, the expression of
HMGB1 was independent of age, histological type, the degree of
differentiation, and TNM stage (P-values >0.05). Only the depth
of tumor invasion, and presence of lymph node metastasis correlated
with the expression of HMGB1 (P<0.05).
The expression of hepsin was not related to the
tumor pathological type (P>0.05). But, it was related to the
degree of differentiation, the depth of invasion, the presence of
lymph node metastasis and the TNM stage (P-values <0.05)
(Table II).
 | Table II.Relationship of HMGB1 and hepsin with
clinicopathological factors of cervical cancer. |
Table II.
Relationship of HMGB1 and hepsin with
clinicopathological factors of cervical cancer.
|
|
| HMGB1 | Hepsin |
|---|
|
|
|
|
|
|---|
| Pathological
factors | Cases | + | P-value | + | P-value |
|---|
| Age (years) |
|
|
|
|
|
|
<55 | 48 | 47 (97.9) | 0.257 | 44 (91.7) | 0.126 |
| ≥55 | 22 | 20 (90.9) |
| 18 (81.8) |
| Pathological
types |
|
Localization | 34 | 31 (91.2) | 0.204 | 28 (82.4) | 0.067 |
|
Infiltrating | 36 | 36 (100) |
| 35 (97.2) |
| Degree of
differentiation |
|
|
|
|
|
| Poor | 37 | 36 (97.3) | 0.191 | 36 (97.3) | 0.044 |
| High and
middle | 33 | 30 (90.9) |
| 27 (81.8) |
| Depth of
invasion |
|
|
|
|
|
|
T1+T2 | 14 | 11 (78.6) | 0.043 | 8 (57.1) | 0.013 |
|
T3+T4 | 56 | 56 (100) |
| 55 (98.2) |
| Lymph node
metastasis |
|
|
|
|
|
|
Negative | 23 | 20 (87.0) | 0.048 | 18 (78.3) | 0.035 |
|
Positive | 47 | 47 (100) |
| 45 (95.7) |
| TNM stage |
|
|
|
|
|
| I+II | 28 | 25 (89.3) | 0.087 | 24 (85.7) | 0.021 |
| III+IV | 42 | 42 (100) |
| 39 (92.9) |
Correlation analysis of hepsin and
HMGB1
In 70 cases of cervical cancer tissues, the
expressions of hepsin and HMGB1 were simultaneously positive 67.1%
(47/70), and simultaneously negative 21.4% (15/70), here was a
positive correlation between them (r=15.27, P<0.05) (Table III).
 | Table III.Correlation analysis of hepsin and
HMGB1 in cervical cancer. |
Table III.
Correlation analysis of hepsin and
HMGB1 in cervical cancer.
|
| HMGB1 |
|
|
|---|
|
|
|
|
|
|---|
| Hepsin | + | − | R-value | P-value |
|---|
| + | 47 | 7 |
|
|
| − | 1 | 15 | 15.27 | 0.01 |
Comparison of prognosis of cervical
cancer patients with different expression intensity of hepsin and
HMGB1 protein
All subjects were followed-up for 5 years. On July
1, 2015, 66 patients completed their follow-up, while 3 patients
with hepsin positive expression and 1 with HMGB1 positive
expression failed to complete it. The rate of failure to complete
the 5-year follow-up was 5.7%, and the data of patients without a
complete follow-up were not used anymore. During the follow-up
period, in the 66 cases of cervical cancer patients, 34 (51.5%,
34/66) died, and 32 (48.5%, 32/66) were alive, the 5-year survival
rate was 39.3%, and the median survival time was 36.9 months. The
log-rank test showed that expression of hepsin and HMGB1 protein
(either strong or weak) were related to the patients' 5-year
survival rate and median survival time (P<0.05). Comparing the
risk of death (HR) in cervical cancer patients with the strongly
positive expression of hepsin and HMGB1 protein with weakly and
moderately positive expressions, the differences had statistical
significance (P<0.05) (Table
IV).
 | Table IV.Survival analysis of cervical cancer
patients with different expression intensity levels for hepsin and
HMGB1 protein. |
Table IV.
Survival analysis of cervical cancer
patients with different expression intensity levels for hepsin and
HMGB1 protein.
| Category | Cases | 5-year survival rate
(%) | Median survival time
(month) | HR value | 95% CI | P-value |
|---|
| HMGB1 protein
expression |
|
|
|
|
|
|
| + to
++ | 43 | 22 (51.2) | 54.1 | 11.637 | 4.351–38.213 | 0.002 |
|
+++ | 24 | 7
(29.2) | 24.8 |
|
|
|
| Hepsin protein
expression |
|
|
|
|
|
|
| + to
++ | 46 | 19 (41.3) | 41.6 | 10.142 | 4.285–33.275 | 0.006 |
|
+++ | 17 | 6
(35.3) | 27.3 |
|
|
|
Discussion
Cervical cancer is one of the most common malignant
tumors in females. The incidence rate increases year by year, with
a high degree of malignancy and a high mortality rate. The typical
features of malignant tumors are the invasiveness and high
metastasis rates. It is thought that cell regulatory factors and
other patient inherent factors play an important role in allowing
for invasion and metastasis of the tumors. A large number of
clinical trials have shown that patients with high expression of
invasive biological factors have a worse prognosis. Therefore, it
is very important to find new gene therapy targets for cervical
cancer (1,2). Study has shown that hepsin and HMGB1
proteins are involved in regulating the development of malignant
tumors (3). This study was conducted
to investigate the expression of hepsin and HMGB1 proteins in
cervical carcinoma tissues, and to explore the relationship between
their expression and the tumor proliferation, differentiation, and
metastasis. We aimed at providing a theoretical and experimental
basis for early diagnosis and prognosis, and new insights for more
targeted treatments.
The relationship between HMGB1 protein expression
and cervical cancer has been studied. HMGB1 is a cytokine
discovered 30 years ago, it is believed to be important for the
survival, proliferation, invasion and metastasis of malignant tumor
cells, but the research on it is still in the exploratory stages
(4). In recent years, many studies
have linked the expression of HMGB1 to invasion, distant metastasis
and poor prognosis in gastric, colorectal cancer and pancreatic
cancers (5–9). However, study of HMGB1 in cervical
cancer is scarce, and its pathogenic mechanisms are still not
clear. A group of researchers detected the expression of HMGB1 in 3
kinds of cervical cancer cell lines (C-4I, CaSki and ME-180)
(10), their results showed that
HMGB1 was barely expressed in normal cervical cells, but
overexpressed in a highly invasive cervical cancer cell line.
Others found that the expression of HMGB1 in cervical cancer was
higher than that in normal cervical tissues, and the positivity
rate in invasive cervical cancer was significantly higher than that
in the pre-invasive carcinoma tissues (11). Yet another study showed HMGB1 being
highly expressed in recurrent squamous cell carcinoma of the
cervix, compared to other tumor markers, the specificity of HMGB1
was higher, it was suggested that HMGB1 expression levels could be
used as a tumor marker to evaluate the prognosis of patients with
cervical squamous-cell carcinoma (12). In our study immunohistochemical
methods were used to detect the expression of HMGB1 protein in
cervical normal and cancer tissues, and results indicated that the
HMGB1 protein was not expressed in normal cervical tissues, but
highly expressed in cervical cancer tissues. Moreover, a higher
positive expression rate of HMGB1 was found in cervical cancer
patients with high tumor infiltrating degrees and lymph node
metastases. Cervical cancer patients with positive expression of
HMGB1 protein had a poor prognosis, which was consistent with
findings of others and further suggests a link between HMGB1
overexpression and the development of cervical cancer.
At present, there is no unified theory on the role
of HMGB1 in the development of cervical cancer. It was found that
HMGB1 stimulates the endothelial progenitor cell migration and
neovascularization using its receptor RAGE (13). Also, the expression of HMGB1 was
correlated with the expression of the RAGE protein in cervical
squamous cell carcinoma tissues, suggesting positive feedback
signal is important for cervical cancer. In addition, it was shown
that HMGB1 led to MAPKs phosphorylation by Ras and MAPK pathway,
thus activating the nuclear factor-κB (NF-κB), which in turn
activated gene transcription to promote cell proliferation and
differentiation, tumor formation and metastasis (14). Studies have shown that in the process
of invasion and metastasis of cervical cancer cells, HMGB1 may be
related to the activation of matrix metalloproteinases (MMPs) and
protein hydrolases such as MMP-2 and MMP-9, thus dissolving the
extracellular matrix and promoting cancer cell invasion and distant
metastases (15). Nevertheless,
further study is needed in order to clarify the specific mechanisms
and pathways involved.
The hepsin gene was first found in the cDNA of
hepatocellular carcinoma cells, and mainly locates on the human
chromosome 19 (q11-q13.2) (16). The
hepsin protein is a type II transmembrane serine protease. It is
involved in the dissolution of the extracellular matrix and the
abnormal signal transduction between cancerous cells. The
dissolution of extracellular matrix is a prerequisite for invasion
and metastasis of cancer cells, however, the mechanisms by which
hepsin acts are not clear. It was found that hepsin could dissolve
extracellular basement membrane and guide cancer cell invasion and
metastasis through the activation of a pathway for the plasminogen
activator (pro-uPA) of the precursor urokinase type (17). It has been proposed that hepsin may
activate the double chain hepatocyte growth factor, which leads to
the degradation of the cell basement membrane resulting in a weaker
intercellular adhesion force, that facilitates cellular movement,
invasion and metastasis (18). Others
believe that the hepsin gene may act on cancer cells through the
HGF/Met pathway, reducing the adhesion between cells, and thereby
promoting invasion and metastasis of malignant tumor cells
(19).
A large number of studies have confirmed that hepsin
protein is highly expressed in various tumor tissues (20–22).
Hepsin is highly overexpressed in prostate cancer tissues, and its
expression level correlates with the Gleason score, the prognosis
and recurrence rate of the tumor (23). The expression of hepsin in endometrial
carcinoma is significantly higher than that in the normal
endometrium and in benign hyperplasia, and the levels of expression
are related to pathological factors such as infiltration and
metastasis (24). Therefore, hepsin
is considered a group of key enzymes promoting tumor metastasis
(25,26). Then again, there are few studies on
the clinical levels of hepsin gene in cervical cancer, although it
may be a new marker of cervical cancer and a promising therapeutic
target. In this study the expression of hepsin in different
cervical tissues was examined. The results suggest that the
expression rate of hepsin protein changes gradually start at a low
level in normal cervical tissue, increasing in paracancerous tissue
and then getting high in cervical cancer tissue. Importantly, the
levels of hepsin were related to the differentiation degree,
invasion depth, lymph node metastasis presence and TNM stage of
cervical cancer, which suggests that hepsin is closely linked with
the development, metastasis and invasion of cervical cancer. We
conclude the levels of hepsin may be considered a risk factor for
tumor development and metastasis.
In conclusion, this study showed that the expression
levels of hepsin and HMGB1 were related to the depth of invasion,
the presence of lymph node metastasis of cervical cancer and the
prognosis for patients. This suggests that both proteins may play a
synergistic role in the genesis and development of cervical cancer.
We believe that the combined detection of hepsin and HMGB1
expression is helpful in the diagnosis and prognosis of cervical
cancer, and propose them as a pair of new markers for cervical
cancer. Moreover, blocking both signal transduction pathways may
become a successful strategy for inhibiting cervical cancer.
References
|
1
|
Li J, Kang LN and Qiao YL: Review of the
cervical cancerdisease burden in mainland China. Asian Pac J Cancer
Prev. 12:1149–11453. 2011.PubMed/NCBI
|
|
2
|
Tanimoto H, Yan Y, Clarke J, Korourian S,
Shigemasa K, Parmley TH, Parham GP and O'Brien TJ: Hepsin, a cell
surface serine protease identified in hepatoma cells, is
overexpressed in ovarian cancer. Cancer Res. 57:2884–2887.
1997.PubMed/NCBI
|
|
3
|
Ulloa L and Messmer D: High-mobility group
box 1 (HMGB1)protein: friend and foe. Cytokine Growth Factor Rev.
17:189–201. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Kong TW, Piao X, Chang SJ, Paek J, Lee Y,
Lee EJ and Ryu HS: A predictive model for parametrial invasion in
patients with FIGO Stage IB cervical cancer: individualized
approach for primary treatment. Int J Gynecol Cancer. 26:184–191.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Ohmori H, Luo Y and Kuniyasu H:
Non-histone nuclear factor HMGB1 as a therapeutic target in
colorectal cancer. Expert Opin Ther Targets. 15:183–193. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Chung HW, Lee SG, Kim H, Hong DJ, Chung
JB, Stroncek D and Lim JB: Serum high mobility group box-1 (HMGB1)
is closely associated with the clinical and pathologic features of
gastric cancer. J Transl Med. 7:382009. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Moriwaka Y, Luo Y, Ohmori H, Fujii K,
Tatsumoto N, Sasahira T and Kuniyasu H: HMGB1 attenuates
anti-metastatic defense of the lymph nodes in colorectal cancer.
Pathobiology. 77:17–23. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Cebrián MJ, Bauden M, Andersson R,
Holdenrieder S and Ansari D: Paradoxical role of HMGB1 in
pancreatic cancer: tumor suppressor or tumor promoter? Anticancer
Res. 36:4381–4389. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Liu Z, Du R, Long J, Guo K, Ge C, Bi S and
Xu Y: microRNA-218 promotes gemcitabine sensitivity in human
pancreatic cancer cells by regulating HMGB1 expression. Chin J
Cancer Res. 27:267–278. 2015.PubMed/NCBI
|
|
10
|
Bandiera A, Bonifacio D, Manfioletti G,
Mantovani F, Rustighi A, Zanconati F, Fusco A, Di Bonito L and
Giancotti V: Expression of HMGI(Y) proteins in squamous
intraepithelial and invasive lesions of the uterine cervix. Cancer
Res. 58:426–431. 1998.PubMed/NCBI
|
|
11
|
Fu X, Du XQ and Hao H: Study on the
expression and clinical significance of high mobility group protein
HMGB1 in cervical squamous cell carcinoma. Chinese Journal of
Cancer Control. 15:357–359. 2008.
|
|
12
|
Sheng X, Du X, Zhang X, Li D, Lu C, Li Q,
Ma Z, Song Q and Wang C: Clinical value of serum HMGB1 levels in
early detection of recurrent squamous cell carcinoma of uterine
cervix: comparison with serum SCCA CYFRA21-1, and CEA levels. Croat
Med J. 50:455–464. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Mitola S, Belleri M, Urbinati C, Coltrini
D, Sparatore B, Pedrazzi M, Melloni E and Presta M: Cutting edge:
extracellular high mobility group box-1 protein is a proangiogenic
cytokine. J Immunol. 176:12–15. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Weng H, Deng Y, Xie Y, Liu H and Gong F:
Expression and significance of HMGB1, TLR4 and NF-κB p65 in human
epidermal tumors. BMC Cancer. 13:3112013. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Wang JL, Wu DW, Cheng ZZ, Han WZ, Xu SW
and Sun NN: Expression of high mobility group box-B1 (HMGB-1) and
matrix metalloproteinase-9 (MMP-9) in non-small cell lung cancer
(NSCLC). Asian Pac J Cancer Prev. 15:4865–4869. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Yin M, Xu Y, Lou G, Hou Y, Meng F, Zhang
H, Li C and Zhou R: LAPTM4B overexpression is a novel predictor of
epithelial ovarian carcinoma metastasis. Int J Cancer. 129:629–635.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Lipari MT, Li W, Moran P, Kong-Beltran M,
Sai T, Lai J, Lin SJ, Kolumam G, Zavala-Solorio J, Izrael-Tomasevic
A, et al: Furin-cleaved proprotein convertase subtilisin/kexin type
9 (PCSK9) is active and modulates low density lipoprotein receptor
and serum cholesterol levels. J Biol Chem. 287:43482–43491. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Goulet B, Chan G, Chambers AF and Lewis
JD: An emerging role for the nuclear localization of maspin in the
suppression of tumor progression and metastasis. Biochem Cell Biol.
90:22–38. 2012.PubMed/NCBI
|
|
19
|
Secord A Alvarez, Darcy KM, Hutson A,
Huang Z, Lee PS, Jewell EL, Havrilesky LJ, Markman M, Muggia F and
Murphy SK: The regulation of MASPIN expression in epithelial
ovarian cancer: association with p53 status, and MASPIN promoter
methylation: a gynecologic oncology group study. Gynecol Oncol.
123:314–319. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Zhang C, Zhang M, Wu Q, Peng J, Ruan Y and
Gu J: Hepsin inhibits CDK11p58 IRES activity by suppressing unr
expression and eIF-2α phosphorylation in prostate cancer. Cell
Signal. 27:789–797. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Zhang M, Zhao J, Tang W, Wang Y, Peng P,
Li L, Song S, Wu H, Li C, Yang C, et al: High Hepsin expression
predicts poor prognosis in gastric cancer. Sci Rep. 6:369022016.
View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Pelkonen M, Luostari K, Tengström M,
Ahonen H, Berdel B, Kataja V, Soini Y, Kosma VM and Mannermaa A:
Low expression levels of hepsin and TMPRSS3 are associated with
poor breast cancer survival. BMC Cancer. 15:4312015. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Stephan C, Yousef GM, Scorilas A, Jung K,
Jung M, Kristiansen G, Hauptmann S, Kishi T, Nakamura T, Loening
SA, et al: Hepsin is highly overexpressed in and a new candidate
for a prognostic indicator in prostate cancer. J Urol. 171:187–191.
2004. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Matsuo T, Nakamura K, Takamoto N, Kodama
J, Hongo A, Abrzua F, Nasu Y, Kumon H and Hiramatsu Y: Expression
of the serine protease hepsin and clinical outcome of human
endometrial cancer. Anticancer Res. 28(1A): 159–164.
2008.PubMed/NCBI
|
|
25
|
Lucas JM, True L, Hawley S, Matsumura M,
Morrissey C, Vessella R and Nelson PS: The androgen-regulated type
II serine protease TMPRSS2 is differentially expressed and
mislocalized in prostate adenocarcinoma. J Pathol. 215:118–125.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Wilson S, Greer B, Hooper J, Zijlstra A,
Walker B, Quigley J and Hawthorne S: The membrane-anchored serine
protease, TMPRSS2, activates PAR-2 in prostate cancer cells.
Biochem J. 388:967–972. 2005. View Article : Google Scholar : PubMed/NCBI
|