Introduction
Ovarian cancer is one of the three major types of
malignant tumor and is common in the female reproductive system.
Approximately 70% of patients are diagnosed once the tumor has
metastasized to the abdominal cavity outside of the reproductive
organs, which represents International Federation of Gynecology and
Obstetrics (FIGO) stage (2) III or IV
disease, for which the respective 5-year overall survival (OS)
rates are only ~31 and 13% (3,4). The
mortality rate of malignant ovarian tumors is the highest among the
gynecological malignant tumors, and has become a serious threat to
the lives and health of women with primary tumors. Surgery is
prioritized in order to cure ovarian cancer, and is supplemented by
being combined with post-surgical chemotherapy. Tumor cells are
successfully removed in ~45% of patients, and this is dependent on
the tumor size and location, and the individual experience of the
surgeons (5). The main cause of
recurrent ovarian cancer remains unclear. Various types of
consolidation therapy have been studied in a series of clinical
trials, but none have been demonstrated to improve survival time in
ovarian cancer (5–7).
Several studies (8,9) have
introduced positron emission tomography/computed tomography
(PET/CT)-guided intensity-modulated radiotherapy (IMRT) for the
treatment of ovarian cancer. Du et al (8) demonstrated that use of fludeoxyglucose
(18F-FDG)-PET/CT for ovarian cancer recurrence of
retroperitoneal lymph nodes to design the IMRT plan can improve the
accuracy of the gross tumor volume (GTV) sketch and improve the
clinical therapeutic effect. Huang et al (9) reported the case of a 68-year-old female
with ovarian cancer and a large abdominal metastasis (FIGO stage
III), who did not undergo surgery, but received PET/CT imaging
orientation-guided IMRT. The patient did not experience any
significant acute or chronic radiation response. Subsequently,
following 4 cycles of chemotherapy, all lesions disappeared, the
cancer antigen (CA)-125, CA19-9 and carcinoembryonic antigen levels
dropped to normal levels, and the patient experienced 3 years
without recurrence. The present study retrospectively studied 42
patients with stage III or IV ovarian tumors using PET/CT-guided
IMRT, and observed the curative effect and acute or chronic
radiation reaction. Due to metastasis, only partial tumor resection
was possible by surgery and chemotherapy, but certain patients
experienced recurrence; furthermore, a number of patients refused
surgery and chemotherapy.
Patients and methods
Patient characteristics
Between January 2012 and December 2015, 42 patients
with FIGO stage III or IV ovarian cancer from the 323rd Hospital of
the People's Liberation Army (Xi'an, China) underwent IMRT. There
were 21 cases of recurrence following surgery (FIGO III or IV), and
11 patients were unable to tolerate or rejected surgery, and were
therefore only treated with 5–10 cycles of chemotherapy of 105 mg
cisplatin administered as a peritoneal perfusion, followed by 180
mg Taxol and 100 mg cisplatin (Table
I). A total of 10 patients, who were either older (>70
years) or in poor general health were unable to undergo surgery and
only received IMRT. All patients were pathologically diagnosed with
ovarian cancer; 21 cases were diagnosed via postoperative
pathology, and the remainder were differentially diagnosed using a
detecting human epididymis protein 4 (HE4) and CA-125 in the serum,
and auxiliary puncture lesion or abdominal cavity effusion gland
cancer. Prior to radiotherapy the patients were systematically
assessed through lab testing (blood and urine) and clinical imaging
results to rule out any possible inflammation and bleeding.
18F-FDG-PET/CT examination was performed prior to
radiotherapy positioning, and the staging and lesion size
measurement. Patients were examined by 18F-FDG-PET/CT
after 1 and 3 months of radiotherapy, and CA-125 and HE4 tumor
markers were analyzed. The patients were treated with up to 6
cycles of chemotherapy depending on the curative effect and their
systemic tolerance.
 | Table I.Patient, tumor and treatment
characteristics. |
Table I.
Patient, tumor and treatment
characteristics.
| Characteristics | Value |
|---|
| Median age (range),
years | 65 (45–86) |
| Histology, n (%) |
|
|
Epithelial tissue | 34 (81.0) |
|
Mesenchyme | 5 (11.9) |
|
Other | 3 (7.1) |
| KPS score, n (%) |
|
| ≥70 | 25 (59.5) |
|
<70 | 17 (40.5) |
| Peritoneal cavity
effusion, n (%) |
|
| Yes | 15 (35.7) |
| No | 27 (64.3) |
| Radiation dose
(median, range) | 50 (30–60) |
| ≥50 Gy, n
(%) | 24 (57.1) |
| <50
Gy, n (%) | 18 (42.9) |
| Stage, n (%) |
|
| III | 26 (61.9) |
| IV | 16 (38.1) |
| Pro-surgery, n
(%) |
|
| No | 17 (40.5) |
| 1 | 14 (33.3) |
| ≥2 | 11 (26.2) |
| Pro-chemotherapy, n
(%) |
|
| Yes | 26 (61.9) |
| No | 16 (38.1) |
| Group, n (%) |
|
| Surgery +
chemotherapy + radiotherapy | 25 (59.5) |
|
Chemotherapy +
radiotherapy | 12 (28.6) |
|
Radiotherapy | 5 (11.9) |
Radiotherapy
All patients underwent 18F-FDG-PET-/CT
simulation positioning, using PET/CT imaging with a standardized
uptake value (SUV) of 3.0. The GTV, with an external expansion of 5
mm for the clinical target volume (CTV) boundary, the planning
target volume (PTV) surrounding the CTV, which did not require
amplification and the organs at risk, including the affected lymph
nodes and areas of the liver, kidney, small intestine and bladder,
were contoured for treatment planning purposes. Patients were
treated with a median prescription dose of 5,040 cGy (range,
4,500-5,500 cGy) with a median dose/fraction of 200 cGy (range,
180–220 cGy), once daily, 5 times a week, for a total of 12–15
times over a period of 10–14 days, with a treatment break two
times. The localization of the treatment was altered as the
treatment progressed through repetitive PET/CT imaging. The plans
were created to limit the volume receiving 40 Gy (V40) of the
kidney, liver and small bowel to <30%, the V40 of the rectum to
<60%, the V45 of the bladder to <50%, the V20 of the lung to
<20% and the V25 of the heart to <25%.
Toxicity evaluation
Patients were monitored for acute and late toxicity
using Common Terminology Criteria for Adverse Events (CTCAE) V4.03
(7,8)
with data obtained by a radiation oncologist from electronic
hospital records. Patients were evaluated for disease status and
for the appearance of acute and late toxicity according to their
medical history, physical examination, and the aforementioned
laboratory and radiological tests (8). Acute toxicities were defined as events
occurring 28 days after radiotherapy completion, while late
toxicities were defined as events occurring ≥28 days after
radiotherapy completion. On average, patients were followed up by a
radiation oncologist for 3 year following the completion of
radiation therapy.
Statistical analysis
All patients were followed up for a total of 3
years, once every 6 months after radiotherapy. To evaluate the
degree of improvement in the clinical symptoms of the patients, the
KPS score, CA-125 levels, local control (LC) rate, disease
progression, OS rate and 18F-FDG PET/CT findings were
analyzed. Based on their re-examination, it was possible to
determine the curative effect of radiotherapy. Statistical
comparisons utilized univariate and the multivariate Cox
proportional hazards model to evaluate the impact of clinical
factors. The Kaplan-Meier method was used to derive actuarial
estimates of LC rate, progression-free survival (PFS) rate and OS
rate, which were measured from the time between treatment and
mortality. The survival data were analyzed using the log-rank test.
Statistical tests were performed using SPSS 19 software (IBM
Corporation, Armonk, NY, USA).
Results
Improvements in LCP, FS and OS
rate
In the first follow-up year, no evident increase of
the local lesions was observed in 38 patients with stable local
lesions. Following 1 year follow-up, the follow-up intervals were
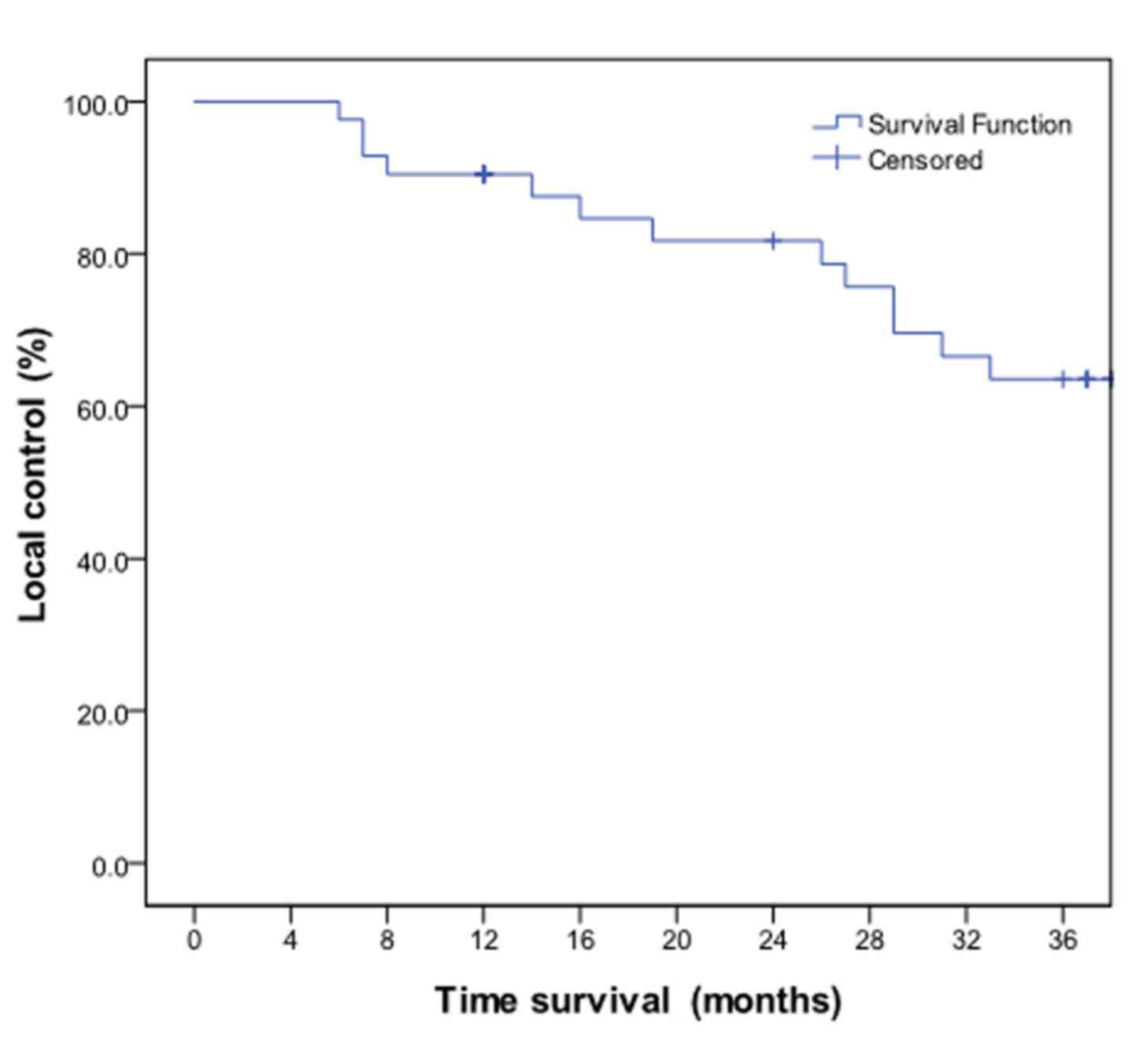
1.5, 2, 2.5 and 3 years. The 1-year LC rate was 90.5%, the 2-year
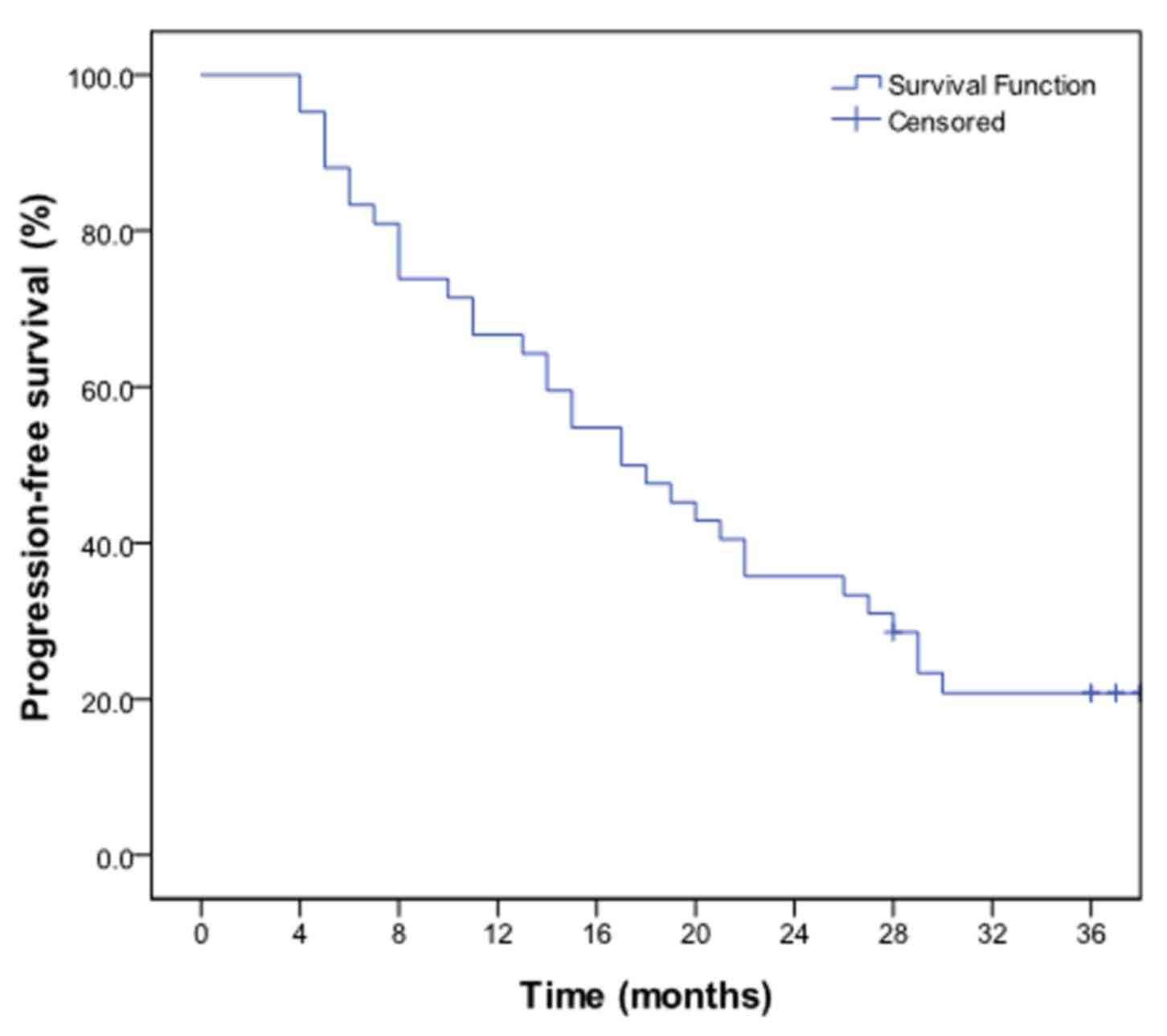
LC rate was 83.3% and the 3-year LC rate was 62.0% (Fig 1). The 1-, 2- and 3-year PFS rates were
66.7, 33.3 and 21.4%, respectively, and the median PFS time was
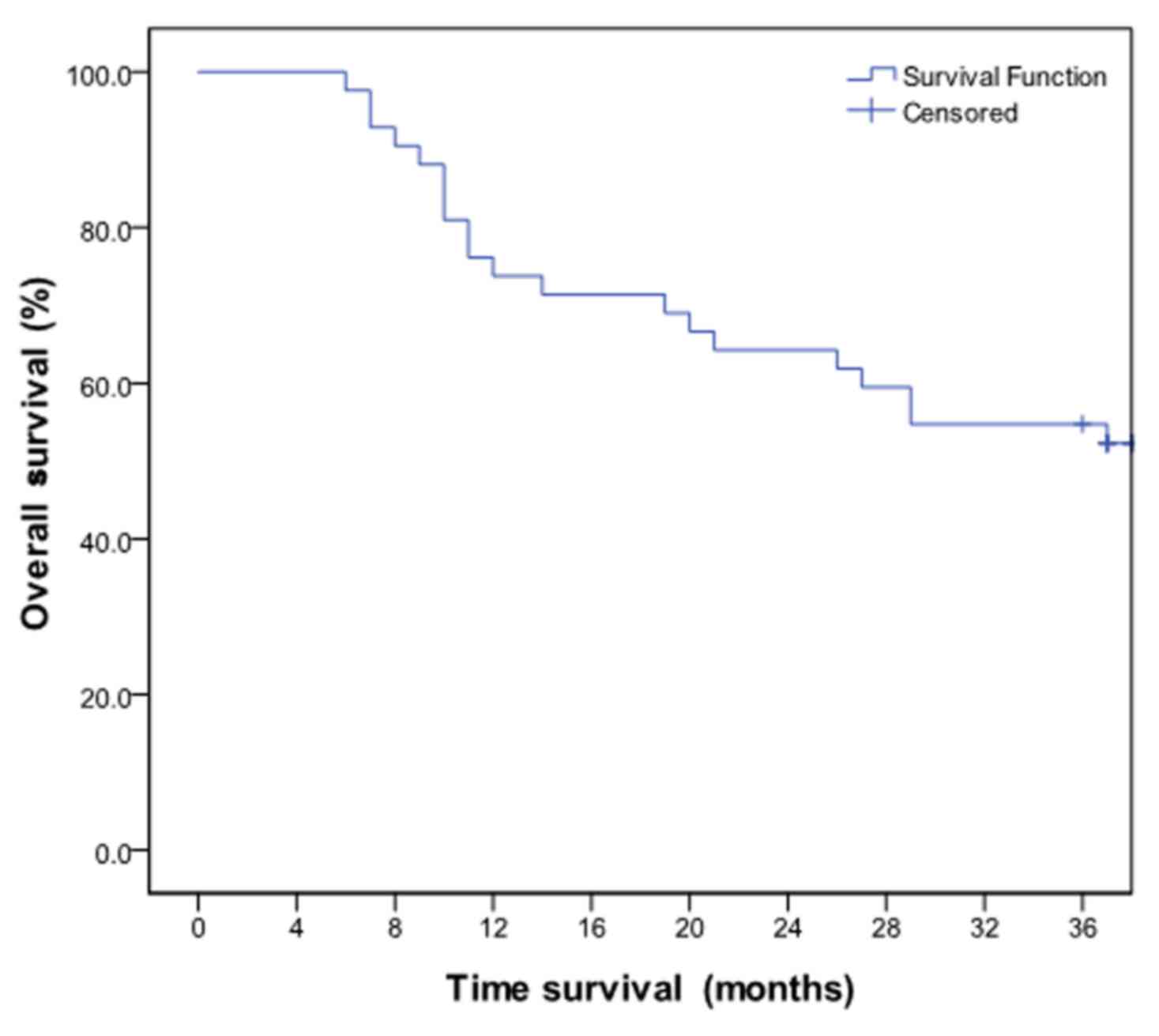
20.3 months (Fig. 2). The 1-, 2- and
3-year OS rates were 73.8, 64.3 and 52.4%, respectively (Fig. 3).
Lower incidence of acute and late
toxicities
All the patients were observed for acute
gastrointestinal or hematological reactions during radiation
therapy, and the results revealed that 90.5% of the
gastrointestinal reactions were less than level 2 (7,8) and that
only 9.5% of gastrointestinal reactions were around level 3
(Table II). Although the lesions in
the patients were indicated to be large and the distribution range
to be wide, there were no symptoms of intestinal obstruction or
intestinal bleeding. The gastrointestinal reaction was reversed by
symptomatic treatment or at 3 days after the termination of
radiotherapy. The acute toxicity of the blood was deemed to be
acceptable; the hematological reaction in 92.9% of the patients was
less than level 2, while that of 7.1% of the patients was around
level 3 (Table III).
 | Table II.Acute toxicities. |
Table II.
Acute toxicities.
|
| Grade |
|---|
|
|
|
|---|
| Acute
toxicities | ≤2 | 3 |
|---|
| Gastrointestinal, n
(%) | 38 (90.5) | 4 (9.5) |
| Hematological, n
(%) | 39 (92.9) | 3 (7.1) |
 | Table III.Late toxicities. |
Table III.
Late toxicities.
|
| Grade |
|---|
| Late
toxicities | ≤2 | 3 |
|---|
| Gastrointestinal, n
(%) | 18 (42.9) | 0 (0.0) |
| Hematological, n
(%) | 24 (57.1) | 1 (2.4) |
The incidence of side effects of late toxicity was
only 42.9%, which was less than the percentage of level 2
gastrointestinal reactions. The patients were able to tolerate the
side effects and symptomatic treatment was used to alleviate them.
No level 3 gastrointestinal side effects were reported. A total of
1/42 (2.4%) patients with hematological side effects was no more
than level 3 (Table IV).
 | Table IV.Multivariate analysis using Cox's
proportional hazard model. |
Table IV.
Multivariate analysis using Cox's
proportional hazard model.
|
|
|
|
| 95% CI |
|---|
|
|
|
|
|
|
|---|
| Variable | SE | P-value | HR | Min | Max |
|---|
| KPS | 0.531 | 0.003 | 0.203 | 0.072 | 0.575 |
| Age | 0.480 | 0.728 | 1.182 | 0.461 | 3.030 |
| TNM | 0.526 | 0.426 | 1.520 | 0.542 | 4.263 |
| Peritoneal
metastasis | 0.559 | 0.545 | 1.403 | 0.469 | 4.201 |
| Surgery | 0.307 | 0.132 | 1.589 | 0.870 | 2.903 |
| Chemotherapy | 0.622 | 0.712 | 1.258 | 0.372 | 4.261 |
| Dose | 0.665 | 0.693 | 1.300 | 0.353 | 4.788 |
Multivariate analysis showing KPS
score as an independent prognostic factor
Multivariate analysis was performed on KPS score,
the total radiation dose administered to patients,
Tumor-Node-Metastasis classification (10), peritoneal metastasis, and whether or
not patients underwent chemotherapy or surgical treatment. The
results suggested that KPS score was the only index associated with
prognosis (P<0.003). Patient age, tumor stage, radiotherapy
dose, the presence of peritoneal cavity effusion and whether or not
the patients underwent surgery or chemotherapy exhibited no clear
association with prognosis.
Use of radiotherapy results as an
equally effective treatment option
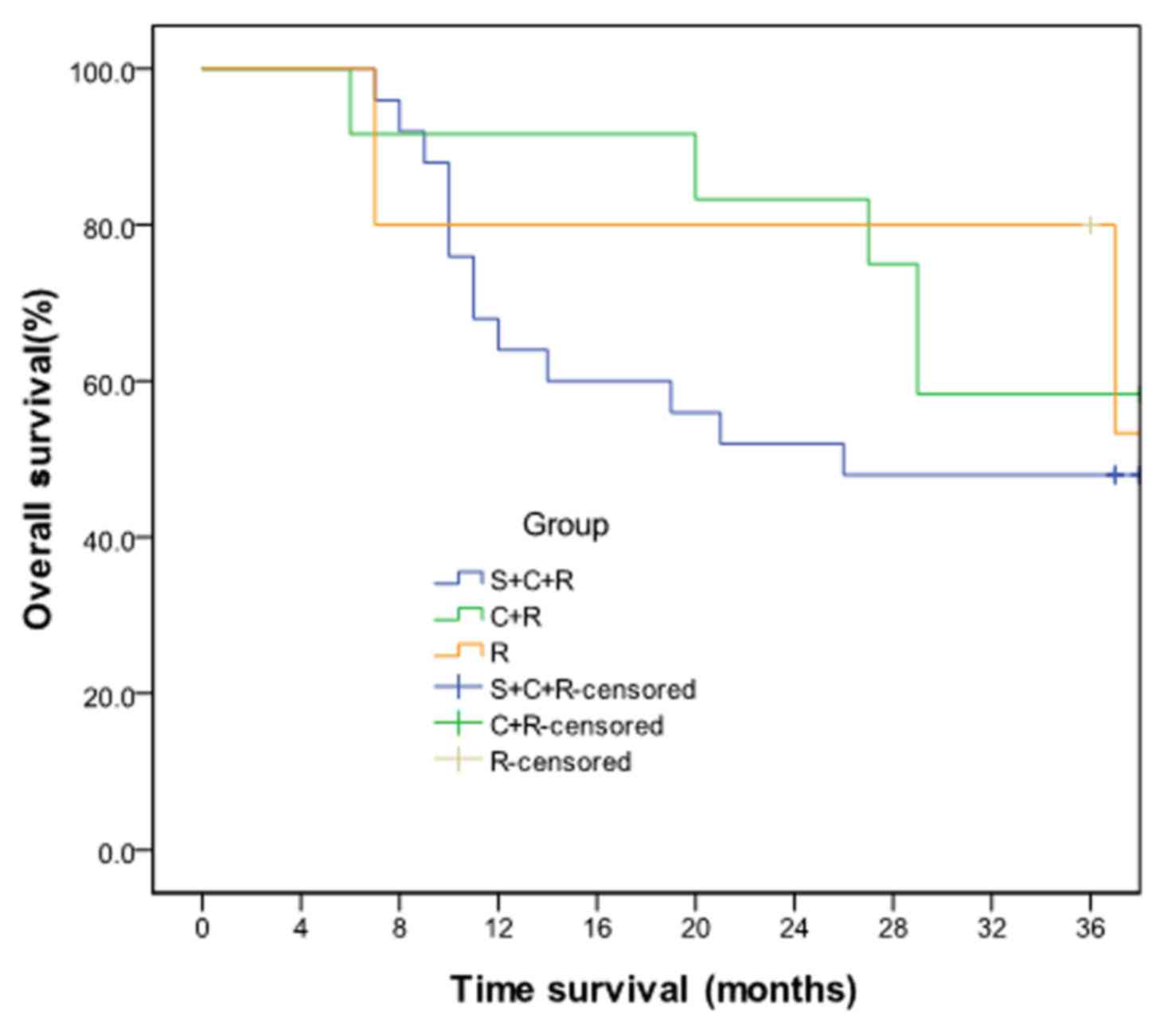
Treatment was administered to patients who received
three different treatment types: Surgery plus chemotherapy and
radiotherapy (S+C+R; n=12), chemotherapy plus radiation therapy
(C+R; n=12) and radiation therapy (R; n=18). The difference in OS
time was not statistically significant (P=0.637), but the survival
curves of the three groups were not identical (Fig. 4). However, radiotherapy resulted in a
similar OS time to that achieved following surgery or chemotherapy.
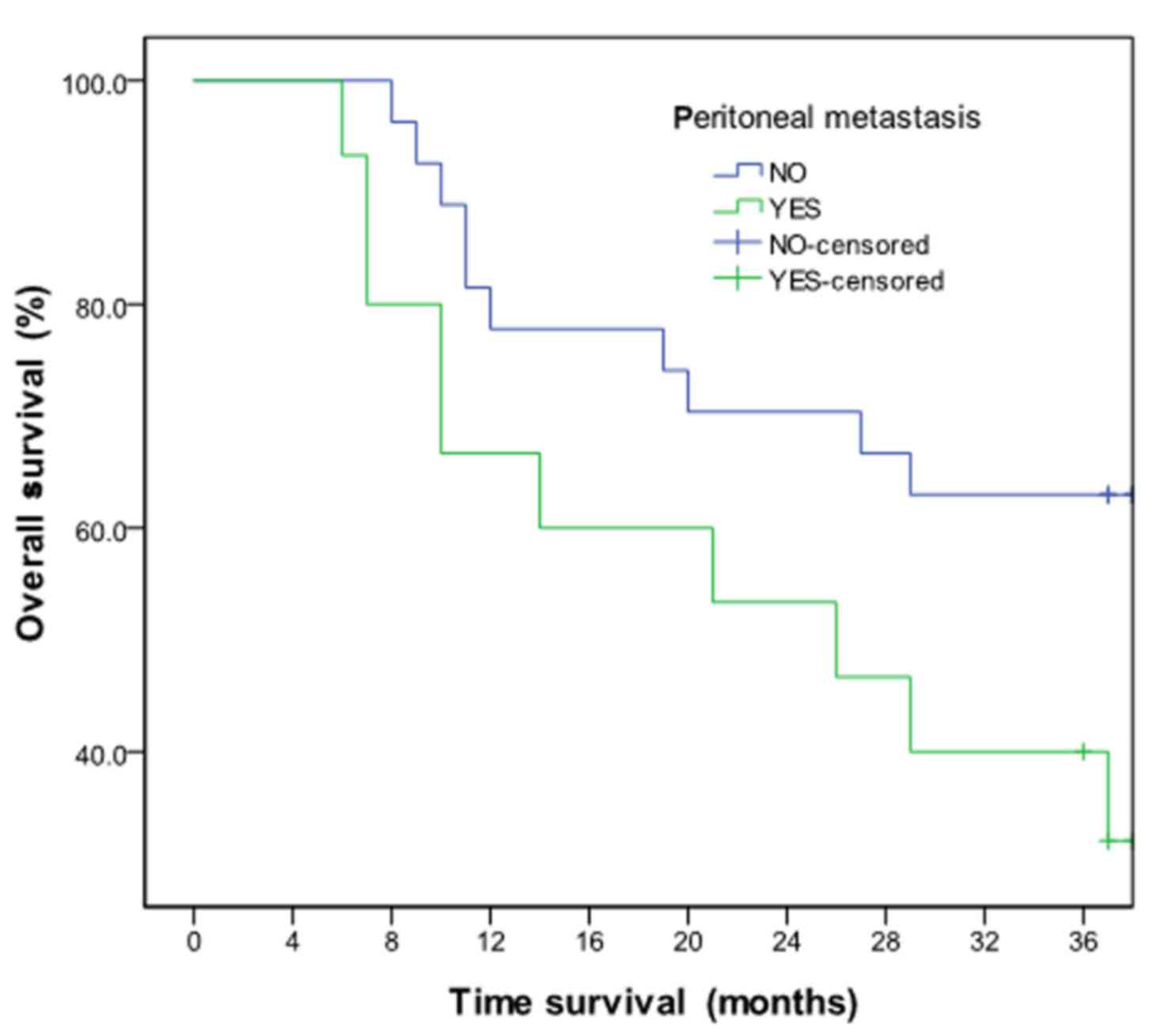
The OS times of patients in the peritoneal metastasis group were
not statistically significantly different from those of patients
without peritoneal metastasis (P=0.059; Fig. 5).
Radiotherapeutic effect in 3 typical
patients
Case 1
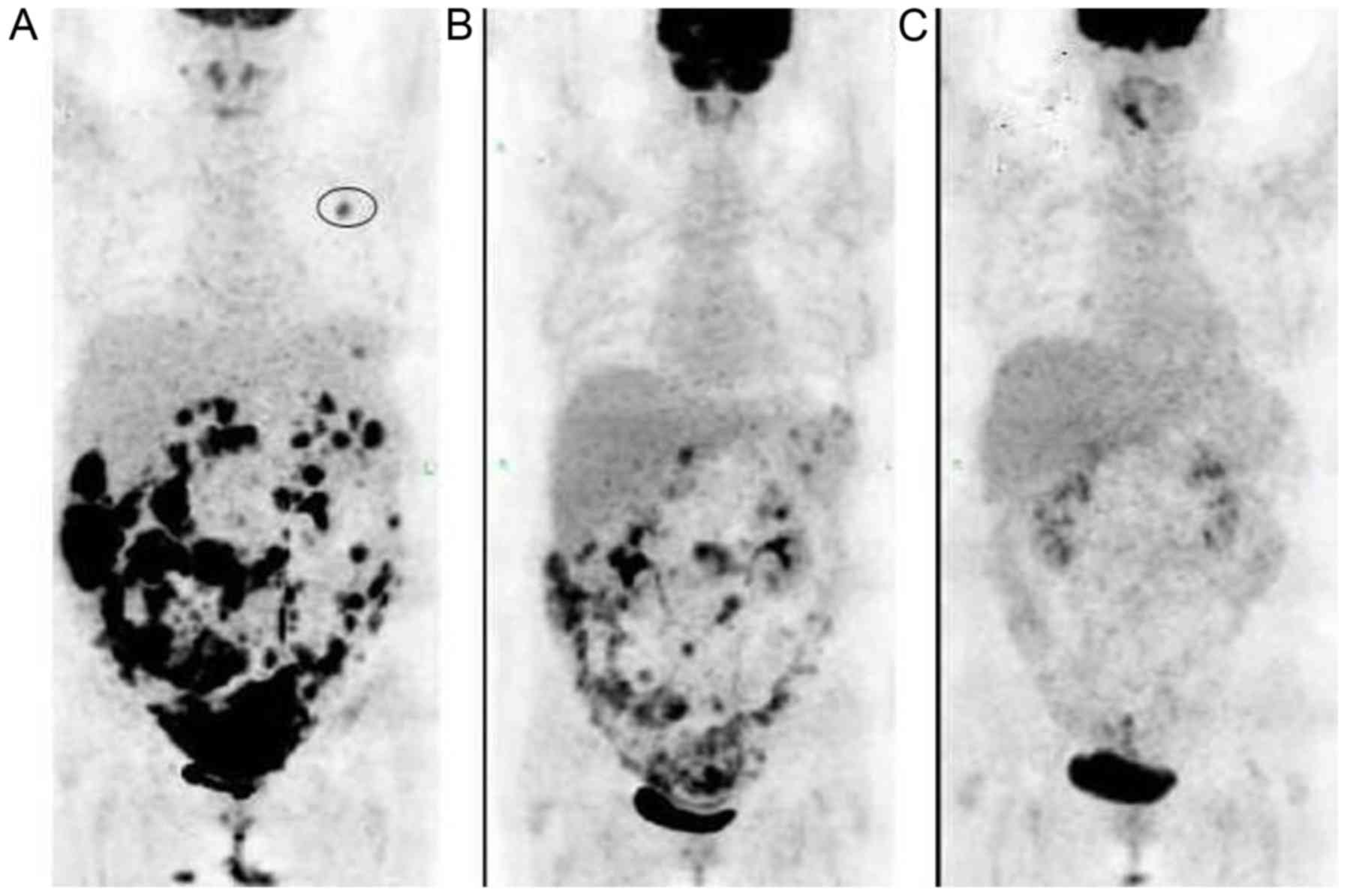
In September 2012, a 59-year-old female presented
with visible and diffusely distributed abdominopelvic lesions, a
large area of peritoneal planting with abdominal cavity effusion in
large quantities, and coronary heart disease, as shown in Fig. 6A, which lead to a refusal of surgery
and chemotherapy. The patient underwent IMRT consisting of a single
200-cGy fraction once daily, 5 times per week, for 14 cycles in
total (the pulmonary lesions were not treated). Following the
second treatment, the abdominopelvic lesions became significantly
smaller and exhibited reduced metabolism, while the heart was not
targeted possibly due to the abscopal effect (Fig. 6B), while the pulmonary lesions were no
longer present. Radiotherapy was continued 11 times, with a total
dose of 50 Gy. From the third PET-CT review (Fig. 6C), the results revealed that the
metabolism of the lesions, particularly the pulmonary lesions, had
disappeared. This may have been caused by distant effects of the
radiation.
Case 2
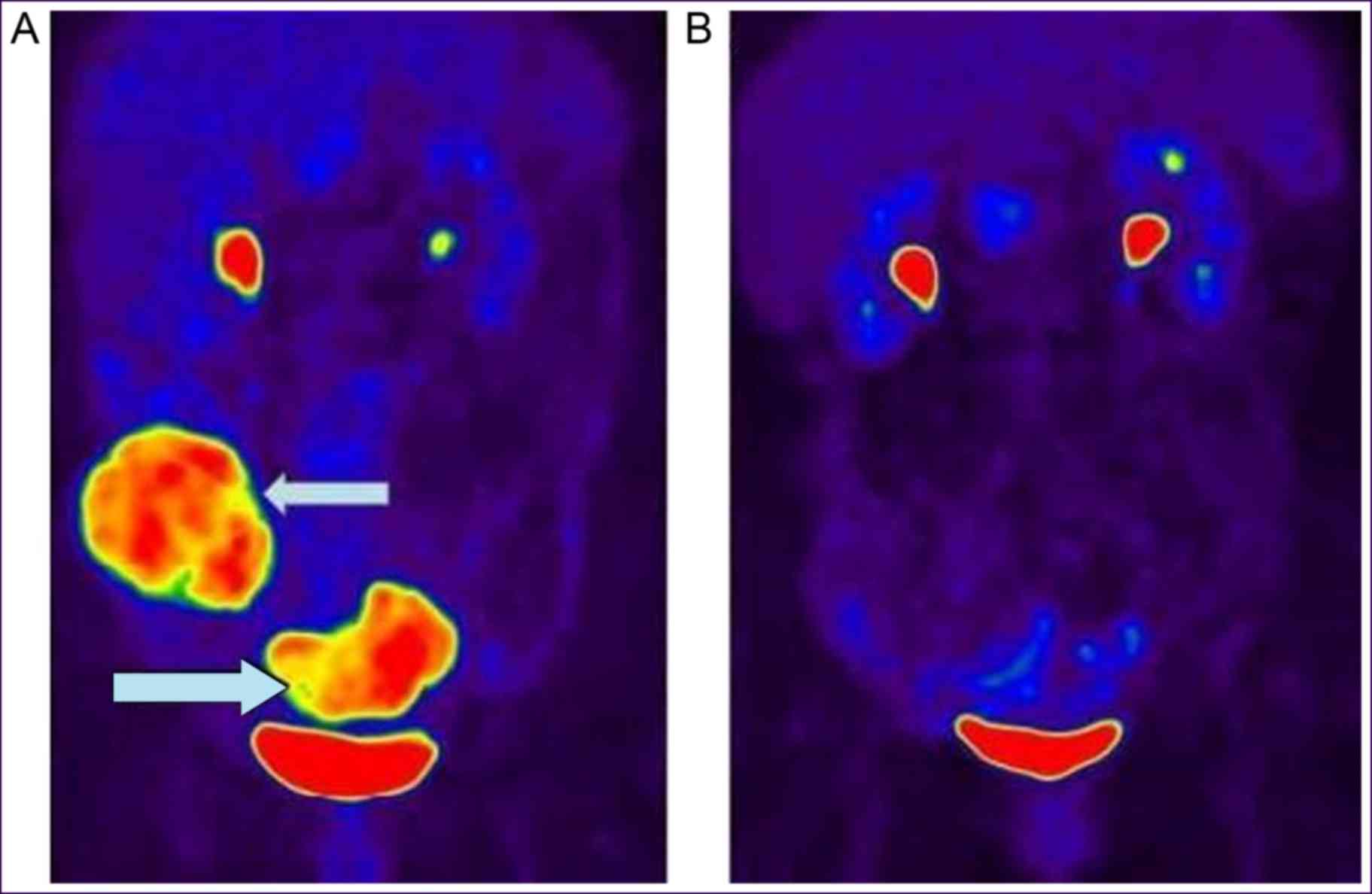
In August, 2012, the second case was that of an
84-year-old female presenting with abdominal pain, diarrhea and
emaciation, and pathologically diagnosed primary ovarian cancer,
metastases and obstruction in the ascending colon, caused by an
incomplete ileus and diagnosed by colonoscopy (Fig. 7A). Due to the age, poor health and
poor heart function of the patient, surgery and chemotherapy were
not possible. Therefore, the patient underwent local IMRT with a
single dose of 200 cGy, 5 times per week, up to a total of 4,800
cGy. Following radiotherapy, the PET/CT scan revealed that all the
lesions had disappeared, and that the complete remission of
symptoms had been achieved (Fig. 7B).
However, the patient succumbed to gastric cancer three years
later.
Case 3
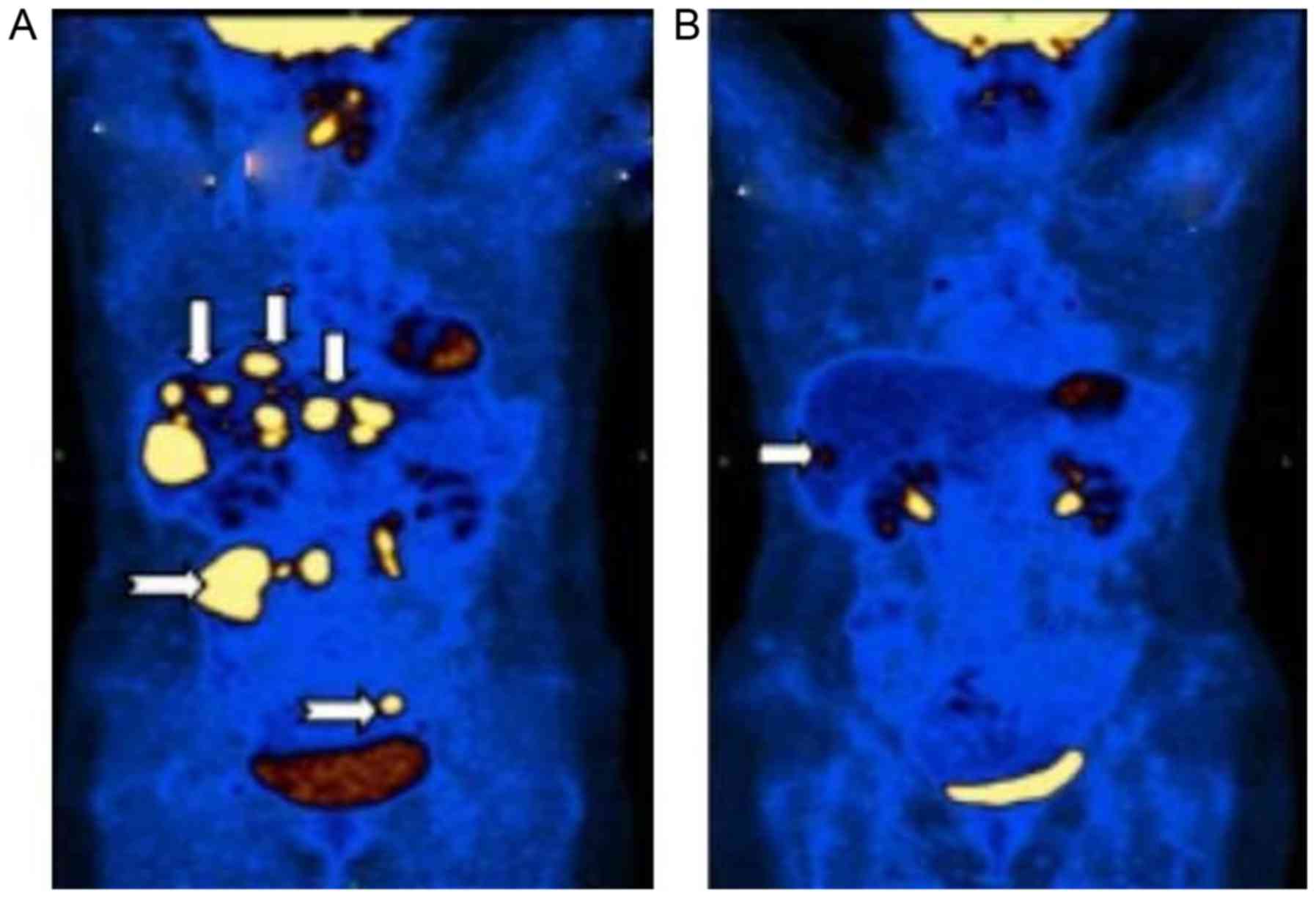
In August, 2013, the third case was that of a
58-year-old female with ovarian cancer, who at 22 months
post-surgery underwent four cycles of chemotherapy following
multiple abdominal and multiple intrahepatic metastases (Fig. 8A). The patient was treated with local
IMRT at a single dose of 200 cGy/day, 5 times per week, for a total
of 13 cycles (total, 4,600 cGy). Following IMRT, the PET/CT scan
revealed that the multiple abdominal tumors had mostly disappeared,
with one residual lesion due to the low radiation dose (Fig. 8B).
Discussion
The 18F-FDG-PET/CT technique demonstrates
high diagnostic value for the identification of primary ovarian
cancer in patients who present with a pelvic mass of unknown
origin. PET/CT has been identified as a useful method for detecting
recurrence in individuals with increased serum levels of CA-125 and
no findings on CT, or in those with normal levels of CA-125 and
recurrence detected by CT that was performed due to clinical
symptoms. PET/CT, detecting recurrence in patients, demonstrated
the value of qualitative diagnosis, improving the diagnosis of
ovarian cancer. In the present study, PET/CT-guided IMRT in
patients with recurrent ovarian cancer improved the delineation of
GTV and reduced the likelihood of treatment that is not targeted
correctly to the tumor location, and therefore improved the
clinical outcome. Certain studies have suggested that standard CT
for radiation treatment planning (RTP), which is acquired during
free breathing but lacks measures for compensating for the
breathing motion, results in deformation and misplacement of tumor
locations. In certain cases, fluoroscopy or slow CT can provide a
general impression of the breathing motion, but these approaches
are not considered to be sufficient for RTP procedures. As free
breathing occurs during PET, the resultant images are blurred
according to the breathing motion and thus provide a good
impression of the tumor shape and location (11,12). In
the most common RTP scenario, where 3DCT and 3D PET scans are
acquired, a respiratory expanded GTV approach is recommended.
Furthermore, PET-CT can aid in distinguishing between the active
and necrotic portions in mixed cystic and solid lesions. However,
the target area with PET-CT is larger compared with CT as indicated
in the present study. The aforementioned finding correspond with
the findings reported by Mundt et al (13). In the present study of patients with
stage III or IV disease, the majority of the patients had numerous,
widely distributed lesions, a large volume flow rate and an
irregular shape, thus the outline of the GTV was difficult to
determine. A PET/CT SUV value of 3.0 was set for the GTV border,
with a 5 mm surrounding boundary for the CTV, while the PTV
boundary was no more than that for the CTV. The PTV target area
should be in close proximity to tumor edge, in order to reduce the
ray radiation to normal tissue area. Following 12–15 treatments
with radiotherapy, the patients rested for 10–14 days, prior to
PET/CT localization and redesign, and a repeat of the treatment,
due to the following reasons: i) a number of the older patients
underwent surgery or chemotherapy multiple times, due to poor
physical condition, more lesions and a wide metastasis
distribution. A number of patients with primary peritoneal tumors
indicated more metastases with large ascites and a larger
radiotherapy volume, causing normal tissue to receive a relatively
large quantity of radiation. In addition, the prolonged treatment
interval could reduce the acute toxicity of the gastrointestinal
system and the blood caused by the radiotherapy; ii) after resting,
the majority of patients exhibited significantly smaller lesions,
abdominal lesions and ascites volume, and the location changed and
iii) in a small number of patients, following PET/CT positioning,
novel lesions appeared, and repeating treatment could improve the
effects of the original treatment
In cases of peritoneal metastasis with a large
amount of ascites, an abdominal cavity drainage tube was used for
various durations according to the tolerance of the patient. To
ensure the location of the metastasis accurately, we treated
patients with peritoneal effusion prior to radiotherapy, following
a 1–2 cm incision to release the peritoneal effusion. The use of
the drainage tube process was smooth and all patients successfully
completed radiotherapy.
The choice of radiation dose and the sensitivity of
the ovarian tumors to radiotherapy are associated with FIGO stage
III and IV ovarian cancer, a large tumor volume and a wide
distribution. According to the results of LC, OS and PFS analysis,
as well as multivariate analysis with adverse effects of treatment
and tolerance to treatment, the effect of treatment in patients in
the present study resulted in little improvement compared with the
effect of surgery and/or chemotherapy.
De Meerleer et al (14) studied patients with FIGO stage III and
IV postoperative residual or recurrent ovarian cancer using whole
abdominopelvic radiotherapy (WAPRT) in the palliative treatment of
chemotherapy-resistant ovarian cancer with bulky peritoneal
disease. All patients exhibited disease, including gastrointestinal
obstruction or an incomplete ileus. A dose of 33 Gy was prescribed,
to be delivered in 22 fractions of 1.5 Gy to the abdomen and
pelvis. Delivery of whole abdomen pelvic RT using IMAT offers
palliation therapy in cases of peritoneal metastatic ovarian
cancer. WAPRT can resolve intestinal obstructions for at least 3
months, suggesting that a total of 33 Gy WAPRT is effective and
safe. Rochet et al (15–17)
reported a similar study regarding lesion-involved field
irradiation. Brown et al (18)
studied involved field radiation therapy for locoregionally
recurrent ovarian cancer, for which the total dose of the local
lesion was ≥45 Gy and the median dose was 59.2 Gy (range, 45–68.2
Gy). Definitive IFRT can yield excellent LC, protracted
disease-free intervals and even complete remission in carefully
selected patients. RT should be considered as a tool in the
curative management of locoregionally recurrent ovarian cancer. In
a study undertaken by Chundury et al (19), the total median radiation dose was
5,040 cGy (range, 4,500-7,000 cGy). The results revealed an
association between using IMRT for recurrent chemorefractory
ovarian cancer and good LC and limited radiation-associated
toxicity. Future studies should be performed to determine the
subpopulation that will most benefit from IMRT, and to assess
whether other techniques, such as stereotactic body radiotherapy,
may be suitable.
The present study reported that the 1-, 2- and
3-year LC rates were 90.5, 83.3 and 69.0%, respectively. Chundury
et al (19) reported similar
results, but 18.2% of the patients exhibited relatively mild
disease (FIGO stage I or II), with a small lesion range. According
to the results of slow side radiation reactions, which revealed no
more than level 3 gastrointestinal reactions and a small number of
patients with level 3 blood toxicity, we hypothesized that a mean
total radiation dose of 5,000 cGy to patients with FIGO stage III
and IV ovarian cancer is feasible and effective.
The present study demonstrated that disease
progression in patients was first identified in the appearance of
new lesions in areas that had not been treated with radiotherapy,
including the liver capsule, peritoneum and pelvic cavity.
Therefore, systemic chemotherapy drugs or abdominal cavity
perfusion chemotherapy is required for the majority of patients
presenting with abdominal cavity effusion while undergoing
radiotherapy. According to the study by Dembo et al
(20) in 1979, the 5-year OS rate in
patients with stage I–III ovarian cancer treated by radiotherapy
was 58%, and the 5-year OS rate of the patients treated with
chlorambucil plus pelvic RT was 41%. In 2010, the 3-year OS rate of
neoadjuvant chemotherapy or primary surgery in stage IIIC or IV
ovarian cancer was recorded to be ~48% (21). In the present study, the 3-year OS
rate of patients treated with radiotherapy was 52.4% (22/42
patients), which was similar to the results found by Brown et
al and Chundury et al (18,19);
however, the present study enrolled patients with late-stage
disease as follows: 15/42 patients (35.7%) with peritoneal
metastasis and peritoneal effusion, 12/42 patients (28.6%) who
refused surgery and opted for chemotherapy plus radiotherapy, and
5/42 patients (11.9%) who were unable to tolerate surgery or
chemotherapy and opted for radiotherapy. In general, the causes of
the positive curative effect, resulting from radiotherapy, were
associated with the PET/CT localization design scheme. Although the
survival analysis of three groups (S+C+R, C+R and R) revealed no
statistically significant differences, the results suggested that
patients who did not undergo surgery exhibited a good survival
trend. The good survival trend may be associated with chemotherapy
or surgery, or the patient's health condition. According to the
survival analysis of patients with or without peritoneal metastasis
and effusion, although no statistically significant differences
were observed, survival was improved in patients without peritoneal
metastasis or effusion. Of the various factors assessed in the
patient survival analysis, it was revealed that KPS was the only
factor associated with survival. For the PET/CT-guided IMRT in the
treatment of patients with advanced ovarian cancer, the general
condition of the patient is important.
The current study presented the case of a
59-year-old female with diffusely distributed abdominal pelvic
visible lesions who was treated with 18F-FDG
PET/CT-guided IMRT, and in whom the metabolism of the lesions
dissipated and the peritoneal effusion completely subsided
(Fig. 6). The health condition of the
patient was poor and due to abdominal metastasis, the patient was
unable to undergo surgery. In addition, she did not wish to receive
chemotherapy, due to the severe adverse effects. Although this was
a specific case, the present study did reveal that patients unable
to undergo surgery and chemotherapy should be enrolled in future
studies. The fact that the pulmonary lesions also disappeared
without treatment may be associated with the abscopal effect. For
the two other selected cases from the present study, namely an
elderly patient unable to tolerate surgery (Fig. 7) and a 58-year-old female with ovarian
cancer, who at 22 months post-surgery underwent four cycles of
chemotherapy following abdominal multiple metastasis and multiple
intrahepatic metastasis (Fig. 8),
PET/CT-guided IMRT obtained a good curative effect and
significantly prolonged the survival time. Therefore, this approach
should be trialed as a treatment option and future studies should
incorporate a larger number of cases.
For patients with advanced ovarian cancer,
18F-FDG-PET/CT-guided IMRT is a safe and effective
treatment method, particularly for patients unable to undergo
surgery and chemotherapy. Furthermore, the KPS score was the only
factor significantly associated with the OS time. To verify this
result, the number of cases should be increased to perform
randomized controlled prospective studies in future.
Acknowledgements
Not applicable.
Funding
Not applicable.
Availability of data and materials
All data generated or analyzed during this study are
included in this published article.
Authors' contributions
YD contributed to the study design, data collection
and writing of the manuscript. XL contributed to data collection
and data analysis. XLL and YM contributed to data analysis and
interpretation of data, TY and WL performed the follow-up of
patients and were responsible for chemotherapy scheduling. SH
contributed to the study design, data analysis, interpretation of
data, writing of the manuscript and revision of the manuscript. All
authors read and approved the final manuscript.
Ethics statement and consent to
participate
The present study was approved by the 323 Hospital
of People's Liberation Army Ethics Board (approval no.,
LZ323-003-89; XI'an, China). Consent to participate was obtained
from all patients.
Patient consent for publication
The patients provided written informed consent for
publication.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Rudolf F, Joaquim LC, Vieira C,
Bjerregaard-Andersen M, Andersen A, Erlandsen M, Sodemann M,
Andersen PL and Wejse C: The Bandim tuberculosis score: Reliability
and comparison with the Karnofsky performance score. Scand J Infect
Dis. 45:256–264. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Kosary CL: FIGO stage, histology,
histologic grade, age and race as prognostic factors in determining
survival for cancers of the female gynecological system: An
analysis of 1973-87 SEER cases of cancers of the endometrium,
cervix, ovary, vulva, and vagina. Semin Surg Oncol. 10:31–46. 1994.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Poveda A: Advanced ovarian cancer: Update,
remarks and conclusions on optimal therapy. Int J Gynecol Cancer.
10:57–60. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Stuart G, Avall-Lundqvist E, du Bois A,
Bookman M, Bowtell D, Brady M, Casado A, Cervantes A, Eisenhauer E,
Friedlaender M, et al: 3rd international ovarian cancer consensus
conference: Outstanding issues for future consideration. Ann Oncol.
8 Suppl 16:viii36–viii38. 2005.
|
|
5
|
Ozols RF: Treatment goals in ovarian
cancer. Int J Gynecol Cancer. 1 Suppl 15:S3–S11. 2005. View Article : Google Scholar
|
|
6
|
Heintz AP, Odicino F, Maisonneuve P, Quinn
MA, Benedet JL, Creasman WT, Ngan HY, Pecorelli S and Beller U:
Carcinoma of the ovary. FIGO 6th annual report on the results of
treatment in gynecological cancer. Int J Gynaecol Obstet. 1 Suppl
95:S161–S192. 2006. View Article : Google Scholar
|
|
7
|
Ozols RF: Update on gynecologic oncology
group (GOG) trials in ovarian cancer. Cancer Invest. 2 Suppl
22:S11–S20. 2004. View Article : Google Scholar
|
|
8
|
Du XL, Jiang T, Sheng XG, Li QS, Wang C
and Yu H: PET/CT scanning guided intensity-modulated radiotherapy
in treatment of recurrent ovarian cancer. Eur J Radiol.
81:3551–3556. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Huang S, Dang Y, Li F, Wei W, Ma Y, Qiao S
and Wang Q: Biological intensity-modulated radiotherapy plus
neoadjuvant chemotherapy for multiple peritoneal metastases of
ovarian cancer: A case report. Oncol Lett. 9:1239–1243. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Deng J, Zhang R, Pan Y, Wang B, Wu L, Jiao
X, Bao T, Hao X and Liang H: Comparison of the staging of regional
lymph nodes using the sixth and seventh editions of the
tumor-node-metastasis (TNM) classification system for the
evaluation of overall survival in gastric cancer patients: Findings
of a case-control analysis involving a single institution in China.
Surgery. 156:64–74. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Lindner H, Willich H and Atzinger A:
Primary adjuvant whole abdominal irradiation in ovarian carcinoma.
Int J Radiat Oncol Biol Phys. 19:1203–1206. 1990. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Sorbe B and Swedish-Norgewian Ovarian
Cancer Study Group: Consolidation treatment of advanced (FIGO stage
III) ovarian carcinoma in complete surgical remission after
induction chemotherapy: A randomized, controlled, clinical trial
comparing whole abdominal radiotherapy, chemotherapy, and no
further treatment. Int J Gynecol Cancer. 13:278–286. 2003.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Mundt AJ, Lujan AE, Rotmensch J, Waggoner
SE, Yamada SD, Fleming G and Roeske JC: Intensity-modulated whole
pelvic radiotherapy in women with gynecologic malignancies. Int J
Radiat Oncol Biol Phys. 52:1330–1337. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
De Meerleer G, Vandecasteele K, Ost P,
Delrue L, Denys H, Makar A, Speleers B, Van Belle S, Van den
Broecke R, Fonteyne V and De Neve W: Whole abdominopelvic
radiotherapy using intensity-modulated arc therapy in the
palliative treatment of chemotherapy-resistant ovarian cancer with
bulky peritoneal disease: A single-institution experience. Int J
Radiat Oncol Biol Phys. 79:775–781. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Rochet N, Jensen AD, Sterzing F, Munter
MW, Eichbaum MH, Schneeweiss A, Sohn C, Debus J and Harms W:
Adjuvant whole abdominal intensity modulated radiotherapy (IMRT)
for high risk stage FIGO III patients with ovarian cancer
(OVAR-IMRT-01)- Pilot trial of a phase I/II study: Study protocol.
BMC Cancer. 7:2272007. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Rochet N, Kieser M, Sterzing F, Krause S,
Lindel K, Harms W, Eichbaum MH, Schneeweiss A, Sohn C and Debus J:
Phase II study evaluating consolidation whole abdominal
intensity-modulated radiotherapy (IMRT) in patients with advanced
ovarian cancer stage FIGO III-The OVAR-IMRT-02 Study. BMC Cancer.
11:412011. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Rochet N, Lindel K, Katayama S, Schubert
K, Herfarth K, Schneeweiss A, Sohn C, Harms W and Debus J:
Intensity-modulated whole abdomen irradiation following adjuvant
carboplatin/taxane chemotherapy for FIGO stage III ovarian cancer:
Four-year outcomes. Strahlenther Onkol. 191:582–589. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Brown AP, Jhingran A, Klopp AH, Schmeler
KM, Ramirez PT and Eifel PJ: Involved-field radiation therapy for
locoregionally recurrent ovarian cancer. Gynecol Oncol.
130:300–305. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Chundury A, Apicelli A, DeWees T, Powell
M, Mutch D, Thaker P, Robinson C, Grigsby PW and Schwarz JK:
Intensity modulated radiation therapy for recurrent ovarian cancer
refractory to chemotherapy. Gynecol Oncol. 141:134–139. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Dembo AJ, Bush RS, Beal FA, Bean HA,
Pringle JF and Sturgeon JF: The princess margaret hospital study of
ovarian cancer: Stage I, II and asymptomatic III presentations.
Cancer Treat Rep. 63:249–254. 1979.PubMed/NCBI
|
|
21
|
Vergote I, Tropé CG, Amant F, Kristensen
GB, Ehlen T, Johnson N, Verheijen RH, van der Burg ME, Lacave AJ,
Panici PB, et al: Neoadjuvant chemotherapy or primary surgery in
stage IIIC or IV ovarian cancer. N Engl J Med. 363:943–953. 2010.
View Article : Google Scholar : PubMed/NCBI
|