Introduction
Gestational trophoblastic diseases (GTDs) are a
group of disorders caused by the abnormal growth of trophoblast
cells derived from placenta-forming tissues during pregnancy
(1,2).
GTDs can usually be diagnosed by ultrasound scans and blood tests
during pregnancy (3). Malignant GTDs
are diagnosed by an elevated level of β-human chorionic
gonadotropin (hCG) (1,4). According to data from a study by the
French Trophoblastic Disease Reference Center, ~30% of patients
were initially diagnosed as having ectopic pregnancies, and 7 out
of 18 patients initially received a misdiagnosis (5).
GTD is a term that includes benign and malignant
tumors in this tissue. Hydatidiform moles are included in the
benign GTD group upon clinicopathological classification. There are
four types of malignant GTD; invasive moles, choriocarcinoma,
placental site trophoblastic tumors and epithelioid trophoblastic
tumors (6,7). Hydatidiform moles can occasionally
progress to invasive moles or choriocarcinoma and spread rapidly.
Choriocarcinoma, a malignant GTD, is a highly invasive tumor that
is more likely to spread to other organs, including the lungs,
liver and brain, through hematogenous routes (8,9). A
previous study reported that the incidence of choriocarcinoma in
pregnant women was approximately three to nine times higher in Asia
than in Europe and North America (10,11).
Compared with the hydatidiform mole, which accounts for 80% of all
GTD cases, choriocarcinoma is relatively rare, and placental site
trophoblastic tumors and epithelioid trophoblastic tumors are even
less well known, and have been the subject of fewer studies
(10,12).
According to the International Federation of
Gynecology and Obstetrics (FIGO), the majority of cases of
choriocarcinoma are chemotherapy-sensitive, with a survival rate of
nearly 100% in low-risk groups and >80% in high-risk groups
(13–15). There are four stages in FIGO staging
system: stage 1 (only in the uterus), stage 2 (expansion into
genital structures), stage 3 (extension of disease into lungs) and
stage 4 (extension to the metastatic sites of the whole body)
(15). Despite the fact that
chemotherapy results in a significant cure rate, when cancer cells
widely metastasize, the cure rate remains poor (16). Therefore, the development of effective
therapies is the focus of present studies. In the present review,
the characteristics of each type of GTD are presented, as well as
the current strategies for GTD treatment, focusing on novel
promising stem cell therapies.
Types of GTD
Hydatidiform mole
A hydatidiform mole is a disease caused by the
atypical growth of normal trophoblastic cells, and is the most
common benign lesion of the GTDs. The moles are classified into two
types, complete hydatidiform moles and partial hydatidiform moles,
according to morphological, histopathological and cytogenetic
analysis (11). The treatment of the
majority of patients afflicted with the two types of hydatidiform
mole is focused on removal by dilation and curettage (17,18). There
are two main risk factors for developing the moles: i) Maternal
age; women ≤16 years or >40 years of age are 5 to 10 times more
likely to develop hydatidiform moles than women aged 16–40 years;
and ii) a previous history of a hydatidiform mole, which increases
the incidence of another developing by ~1.8% (19).
Invasive moles
An invasive mole is a neoplasia that grows in the
uterine wall; it can spread to other areas of the body, including
the vagina, vulva and lungs, and usually occurs following
conception in women of reproductive age (20,21). The
most common signs of an invasive mole are prolonged vaginal
bleeding and uterine enlargement. Invasive moles are clinically
diagnosed by changes in hCG levels and are generally curable by
extirpative procedures or hysterectomy (22).
Choriocarcinoma
Choriocarcinoma is a trophoblastic cancer that is
liable to spread to multiple organs through hematogenous pathways.
The most common symptom is vaginal bleeding, which also occurs in
women with hydatidiform moles or during abnormal pregnancy
(23). Choriocarcinoma is a rare
cancer; however, the incidence of choriocarcinoma in Asian women is
~3 to 9 times higher than that in women in Europe and North America
(9,24). Due to the high potential of vascular
invasion, there are high risks of early metastasis to other organs,
including the lungs, vagina, brain and liver (13,25). The
majority of choriocarcinomas are treated with single-agent or
combination chemotherapy depending on the severity, and the
chemotherapy has been shown to exhibit a significant therapeutic
effect (26). However, drug
resistance and systemic metastasis decrease the cure rate of
chemotherapy (26).
Placental site trophoblastic
tumors
A placental site trophoblastic tumor is a monophasic
neoplasm GTD originating from extravillous trophoblasts (27,28); it is
a benign lesion that develops from the placental implantation site
and accounts for 0.25–5% of GTD cases globally (29). However, 10–15% of cases of this
disease were reported to be clinically malignant tumors (30). Placental site trophoblastic tumors are
a unique manifestation compared with other types of GTD, and this
is due to several features: i) relatively low hCG serum levels; ii)
late-onset metastasis; iii) slower growth; and iv) less sensitivity
to chemotherapy (29). As the
placental site trophoblastic tumor is generally resistant to
chemotherapy, hysterectomy has been reported as an appropriate
treatment (31).
Epithelioid trophoblastic tumors
An epithelioid trophoblastic tumor is a rare form of
GTD. In 1998, it was identified as a distinct entity (32). It has been reported that this tumor
commonly develops in fertile women with a history of gestational
events, including molar pregnancy and spontaneous abortion, and
that latency is between 2 months and 25 years (33). The incidence rate for the tumor is
<2% among all GTDs (34). An
epithelioid trophoblastic tumor is clinically similar to a
placental site trophoblastic tumor as, it is resistant to
chemotherapy and is slow growing (35). For patients with non-metastatic
epithelioid trophoblastic tumors, a hysterectomy is recommended to
maximize the therapeutic opportunity (34).
Current therapeutic methods and research for
GTD
Malignant GTDs in the gestational trophoblastic
neoplasm (GTN) classification include invasive moles,
choriocarcinoma, placental site trophoblastic tumors and
epithelioid trophoblastic tumors (26). Treatment of invasive moles and
choriocarcinoma is principally associated with chemotherapy
(36). The FIGO anatomical staging
system is used to appraise the prognosis of patients and predict
appropriate therapeutic strategies (15). Lung metastasis occurs in ~70% of
patients with GTN, and brain metastasis occurs in 8–15% (37). The brain metastasis of a GTN is
characterized by central necrosis and hemorrhage. Therefore, these
patients are likely to present with neurological deterioration and
intracerebral hemorrhage (ICH) (38).
The probability of a cure rests on several prognostic factors,
including age, pregnancy status, β-hCG concentration, extent of
metastasis and tumor size (10).
Current treatments for GTD
One of the most effective remedies for hydatidiform
moles is the termination of pregnancy (39–41). The
termination of pregnancy diminishes the symptoms and prevents
subsequent complications (42).
Another possible treatment is chemotherapy. Methotrexate and
dactinomycin are major chemotherapeutic drugs used in GTD (43). Hydatidiform moles have been
successfully treated with methotrexate (44). In addition, the main treatment for
invasive moles and choriocarcinoma is chemotherapy (36). The appropriate treatment for patients
in the low-risk disease group is single-agent chemotherapy
(36). The majority of patients with
choriocarcinoma (~95%) caused by molar pregnancy belong to this
group, and treatment with methotrexate and dactinomycin alleviated
the entire choriocarcinoma in 50–90% of patients (10,45). Of
the total molar pregnancies, 80–85% of cases are benign without
local relapse or metastasis to other organs. A total of 15–20% are
invasive, and <5% are malignant with metastatic lesions
(45). In the case of the high-risk
disease group, combination chemotherapy is required instead of
single-agent chemotherapy (46). A
previous study showed that patients with recurrent malignant
trophoblastic diseases also had a favorable prognosis with
multiple-agent therapy, and 5-year survival rates were
significantly increased (47).
Chemotherapy is regarded as the primary treatment
for patients with GTN. However, patients with chemo-resistant or
recurrent tumors require surgical therapy. Prior to performing
resection, medical imaging tests are attempted in order to confirm
the presence of lesions in the primary site or other organs. The
majority of these tests are combined with chemotherapy to minimize
metastatic potential by tissue manipulation during the treatment
period. Furthermore, this combination therapy has the advantage of
reducing the length of the hospitalization period and the number of
chemotherapy cycles (37).
Treatment of GTD with direct enzyme
prodrug therapy (DEPT)
DEPT is defined as a therapy that converts pro-drugs
to drugs at the desired location using artificially introduced
enzymes (48,49). DEPT has the advantage of reducing the
systemic toxicity of drugs by gaining active drugs only at a
specific location (50). Due to this
feature, a number of studies have been conducted to demonstrate the
therapeutic effect of DEPT on choriocarcinoma.
Among the various types of DEPT, antibody-DEPT
(ADEPT) exhibited antitumor effects in choriocarcinoma animal
xenograft models (51). In ADEPT,
antibodies designed against cancer antigens are connected to
enzymes, and antibody-connected enzymes can selectively bind to
cancer cells. Effective ADEPT should be able to produce long-term
cytotoxicity in tumors linked with antibodies without serious
toxicity to normal tissues (52). In
a previous study using ADEPT, bacterial enzyme carboxypeptidase G2
exhibited a significant reduction of tumor growth resistance to
conventional chemotherapy in a human choriocarcinoma xenograft
model (51).
Gene-DEPT (GDEPT) is a method of selectively
delivering genes that convert cytotoxic-prodrugs to drugs in tumor
sites (53). The genes are
selectively expressed in cancer cells by tumor-specific promoters
or viral transfection. Weyel et al (54) confirmed that tumor growth in the
choriocarcinoma xenograft model was inhibited by GDEPT using
β-glucuronidase, which converts HMR 1826 to doxorubicin. GDEPT can
be used to selectively target human malignancies, including GTNs,
while reducing the adverse effects of biological drugs.
Gene therapy using genetically engineered
neural stem cells (NSCs)
NSCs as a gene delivery tool for
cancer treatment
NSCs are progenitor cells of the central nervous
system (CNS) and are defined as self-renewing, multipotent cells
that differentiate into neurons, astrocytes and oligodendrocytes
(55). It has been assumed that it
would be feasible to develop alternative therapies for neurological
diseases using the multipotential characteristics of NSCs (56). According to data from a studies
published since 2000, NSCs were detected near the metastatic tumor
when the stem cells were transplanted into a site remote from the
brain neoplasia in animal models and found to be effective in
delivering diverse therapeutic genes such as suicide genes and
immunomodulatory genes to tumor foci (57–59). NSCs
have several unique features: i) prolonged cell proliferation; ii)
integration into the brain of the host without changing normal
functions; and iii) migration toward neoplasms (60,61).
Therefore, it is possible to target cancer cells by producing NSCs
with chemotherapeutic properties (57,61).
Tumor-tropism of NSCs is indicated by
chemoattractant factors produced in glioblastoma multiform or
normal tissue injured by tumor growth (62). To investigate this ability of the
NSCs, the majority of studies were initially performed using
intracranial glioma animal models, and their migration ability to
various cancer types, including breast cancer, melanoma brain
metastases, pancreatic cancer, neuroblastoma and lung cancer, was
further confirmed (63,64). In a 2008 study, a correlation was
identified between hypoxia and NSC migration ability (62). In glioma xenograft models, NSCs were
distributed in hypoxic regions of intracranial tumors, and the
expression of chemoattractant factors, including stromal
cell-derived factor-1, vascular endothelial growth factor (VEGF)
and urokinase-type plasminogen activator, were relatively decreased
in hypoxia-inducible factor-1α-knockdown cells (62). In addition, a variety of factors,
including stem cell factor/c-kit system, VEGF/VEGF receptor, high
mobility group box 1/receptor for advanced glycation end products,
hepatocyte growth factor/c-met signaling, Annexin II and monocyte
chemoattractant protein 1, were identified, which were associated
with tumor-tropism of NSCs toward tumors (65). Based on the inherent migration ability
of NSCs, stem cell therapy expressing anticancer genes has emerged
as a promising therapy for metastatic cancer, including GTNs.
GDEPT and immunomodulatory gene
therapy using NSCs
GDEPT using NSCs, a method that uses genetically
engineered NSCs to express a gene encoding an enzyme that converts
a non-cytotoxic or low cytotoxic prodrug to a cytotoxic metabolite,
is a major approach for cancer therapy (66). These genetically engineered NSCs
confer the following advantages on an effective cancer treatment:
i) cancer-specific migration; ii) minimization of the risk of
adverse drug events; and iii) increased treatment efficiency
(61). Since NSCs have the capability
for cancer selective migration, genetically engineered NSCs can
deliver the anticancer genes at the tumor sites. Furthermore, Joo
et al (67) reported that
tumors were suppressed in the left and right hemispheres of the
brain when genetically engineered NSCs were injected into the left
hemisphere in brain metastasis animal models. This suggests that
NSCs can migrate to the tumor-forming sites anywhere in the body
and inhibit tumor growth. Cancer treatment using foreign enzymes
expressed at the tumor site is an essential feature of GDEPT and
can minimize the side effects when compared with conventional
chemotherapy (57). The anticancer
genes of GDEPT for humans typically use those originated from other
species in order to minimize the pro-drug activity of endogenous
enzymes (68). One example of stem
cells expressing such genes is HB1.F3.CD cells, which are
genetically engineered NSCs expressing the Escherichia coli
(E. coli) cytosine deaminase (CD) gene. HB1.F3.CD cells were
genetically engineered from fetal telencephalon-derived HB1.F3
cells (69). The CD gene originating
in E. coli converts non-cytotoxic agent 5-fluorocytosine
(5-FC) to cytotoxic agent 5-fluorouracil (5-FU) (70). E. coli CD is an enzyme from the
pyrimidine salvage pathway that deaminates the anti-fungal drug to
5-FU (71). Compared with direct 5-FU
chemotherapy, the CD/5-FC approach may be clinically beneficial due
to the unique property of 5-FC, in that it can cross the blood
brain barrier (72,73). Numerous studies demonstrated that
HB1.F3.CD cells expressing the CD gene significantly inhibited the
proliferation of cancer cells and suppressed tumor growth in the
presence of 5-FC (63,69,74–76).
Treatment of sickness by enhancing or diminishing
the immune response is termed immunotherapy. The use of cytokine
genes to increase the antitumor response is particularly effective
in cancer treatment. A previous study by Panelli and Marincola
identified that 9% of renal cell carcinoma and 7% of melanoma
patients were cured when treated with high concentrations of
interleukin (IL)-2 in a total of 283 patients (77). Thus, NSCs engineered to express
immunomodulatory genes, including interferon (IFN)-β, IL-4, IL-12
and IL-23, can effectively treat cancer by expressing them at the
tumor site (57). For example, in
mouse xenograft models with human colorectal cancer, tumors of mice
injected with NSCs expressing CD alone (HB1.F3.CD) exhibited a 56%
reduction of tumor volume compared with the control, while those of
mice injected with NSCs expressing CD and IFN-β (HB1.F3.CD.IFN-β)
exhibited a reduction of ~76% (75).
Furthermore, treatment with these stem cells in choriocarcinoma
metastasis or xenograft models inhibited tumor growth and decreased
metastasis (78). Kim et al
(78) reported that the volume of the
choriocarcinoma tumor was smaller by approximately half compared
with that of the control groups when using therapeutic genes in a
choriocarcinoma xenograft model, and that the lung metastatic area
of the HB1.F3.CD.IFN-β group was reduced by ~45% compared with that
of the HB1.F3 group in a metastasis model.
However, stem cell-based gene therapy has two major
challenges to overcome. The first challenge is the safety of the
therapy. When human stem cells remain stable in the body, the cells
can cause genetic and epigenetic alterations (79). Furthermore, undifferentiated embryonic
stem cells are likely to form teratocarcinoma (79). The second challenge is the immune
response. The vector that introduces the gene has the potential to
induce an immune response, and non-autologous stem cells will
result in immunological rejection (79). These issues are obstacles preventing
phase III clinical trials of stem cell-based gene therapy from
being conducted, and further studies should be performed in order
to address them.
Overall, NSC therapy is a promising strategy as it
is suitable as a tool for delivering anticancer genes to the
metastatic sites of the body and it has been proven to have
significant therapeutic effects. However, additional research is
essential for the development of a stable and effective therapeutic
method.
Conclusions
In the present review, conventional therapeutic
tools and novel research fields for treating GTD were investigated
and these are summarized in Table I.
Chemotherapy, a major treatment for GTNs, has already achieved a
significant cure rate. Depending on the extent of metastasis
determined by FIGO stage, chemotherapy with a single or multiple
agents is used; however, there is a possibility of systemic
toxicity and recurrence. Furthermore, chemotherapy has limited
effects on recurrent tumors due to their chemical resistance. It is
imperative to overcome these problems in order to effectively treat
the tumors at the metastatic site.
 | Table I.Current and potential therapeutic
methods for gestational trophoblastic disease. |
Table I.
Current and potential therapeutic
methods for gestational trophoblastic disease.
| Treatments | Cancer type | (Refs.) |
|---|
| Conventional
therapy |
|
|
|
Surgical therapy |
|
|
|
Resection | GTN | (37,38) |
|
Chemotherapy |
|
|
|
Methotrexate
and/or dactinomycin | GTN | (43) |
|
Methotrexate and
EMA/COa | Hydatidiform
mole | (44) |
| DEPT |
|
|
|
ADEPT |
|
|
|
Carboxypeptidase
G2 |
Choriocarcinoma | (51,52) |
|
GDEPT |
|
|
|
β-glucuronidase |
Choriocarcinoma | (54) |
| NSC
therapy |
|
|
|
Carboxyl
esterase | Lung cancer | (64) |
|
CD and/or
IFN-β | Breast cancer and
choriocarcinoma | (63,78) |
|
CD and HSV-1
thymidine kinase | Ovarian
carcinoma | (70) |
|
Interleukin
12 | Glioma | (80) |
|
Interleukin
23 | Glioma | (81) |
Previous studies have demonstrated that NSCs have
the ability to migrate to the metastatic regions of the whole body,
as demonstrated by studies in which NSC injected in the left
hemisphere suppressed tumors in the right hemisphere. The intrinsic
properties of these cells are expected to be clinically useful for
the targeted delivery of therapeutic agents to tumors that have
spread throughout the body. However, the number of NSCs that can
reach tumor nodules located at a considerable distance from the
injected site will likely be limited. Therefore, studies of
NSC-based therapy should maintain or improve the intrinsic tumor
tropisms of NSCs.
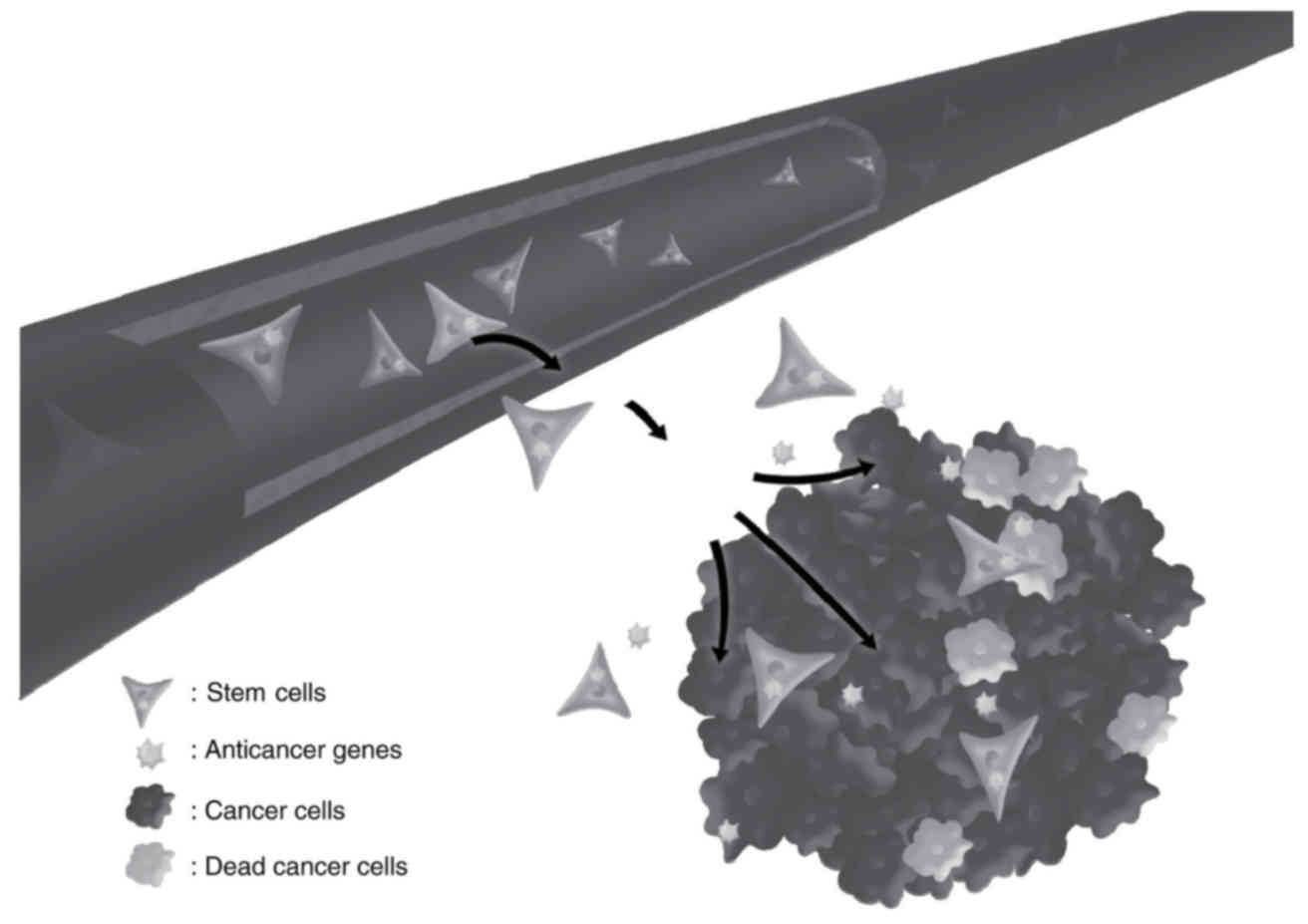
As a result of the cancer-specific migration effect,
NSCs are better suited as a therapeutic delivery tool for
metastatic tumors than other cell types. The CD/5-FC approach with
NSCs has a tremendous advantage in the field of drug delivery for
cancer treatment. Furthermore, NSCs expressing several therapeutic
genes, e.g. CD-expressing NSCs in combination with IFN-β, exhibited
synergism of tumor suppression. Thus, genetically engineered stem
cells expressing anticancer genes migrate to the metastatic sites
and selectively target cancer cells (Fig.
1). Although chemotherapy for GTNs has considerable cure rates,
combination with novel therapies is required to ensure definitive
treatment of patients with metastasis and recurrence.
Acknowledgements
Not applicable.
Funding
This study was supported by the Basic Science
Research Program through the National Research Foundation of Korea
funded by the Ministry of Education, Science and Technology (grant
no. 2016R1D1A1A09919809), and by the Global Research and
Development Center Program through the National Research Foundation
of Korea funded by the Ministry of Science and ICT (grant no.
2017K1A4A3014959).
Availability of data and materials
Not applicable.
Authors' contributions
GSK and KCC were involved in the study conception
and design. GSK collected and assembled data; prepared the figure
and table. GSK and KAH wrote the manuscript, and KCC reviewed
literature. GSK and KAH ensured that questions related to the
accuracy or integrity of the work are appropriately investigated
and resolved. GSK, KAH and KCC agreed to be accountable for all
aspects of the work, and KCC provided final approval of the
manuscript to be published.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Sun P, Wu Q, Ruan G, Zheng X, Song Y, Zhun
J, Wu L and Gotlieb WH: Expression patterns of maspin and mutant
p53 are associated with the development of gestational
trophoblastic neoplasia. Oncol Lett. 12:3135–3142. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Savage P, Williams J, Wong SL, Short D,
Casalboni S, Catalano K and Seckl M: The demographics of molar
pregnancies in England and Wales from 2000–2009. J Reprod Med.
55:341–345. 2010.PubMed/NCBI
|
|
3
|
Begum SA, Bhuiyan ZR, Akther R, Afroz R,
Chowdhury A and Keya KA: A review on gestational trophoblastic
disease. Bangladesh Med J. 44:2015.
|
|
4
|
Gestational Trophoblastic Disease
Treatment (PDQ®). Health Professional Version. In: PDQ
Cancer Information Summaries [Internet]. National Cancer Institute
(US). (Bethesda, MD). 2002.
|
|
5
|
Horowitz NS, Goldstein DP and Berkowitz
RS: Placental site trophoblastic tumors and epithelioid
trophoblastic tumors: Biology, natural history, and treatment
modalities. Gynecol Oncol. 144:208–214. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Lee YJ, Park JY, Kim DY, Suh DS, Kim JH,
Kim YM, Kim YT and Nam JH: Comparing and evaluating the efficacy of
methotrexate and actinomycin D as first-line single chemotherapy
agents in low risk gestational trophoblastic disease. J Gynecol
Oncol. 28:e82017. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
May T, Goldstein DP and Berkowitz RS:
Current chemotherapeutic management of patients with gestational
trophoblastic neoplasia. Chemother Res Pract.
2011:8062562011.PubMed/NCBI
|
|
8
|
Guo J, Zhong C, Liu Q, Xu J, Zheng Y, Xu
S, Gao Y, Guo Y, Wang Y, Luo Q, et al: Intracranial choriocarcinoma
occurrence in males: Two cases and a review of the literature.
Oncol Lett. 6:1329–1332. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Tian Q, Xue Y, Zheng W, Sun R, Ji W, Wang
X and An R: Overexpression of hypoxia-inducible factor 1α induces
migration and invasion through Notch signaling. Int J Oncol.
47:728–738. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Seckl MJ, Sebire NJ and Berkowitz RS:
Gestational trophoblastic disease. Lancet. 376:717–729. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Lurain JR: Gestational trophoblastic
disease I: Epidemiology, pathology, clinical presentation and
diagnosis of gestational trophoblastic disease, and management of
hydatidiform mole. Am J Obstet Gynecol. 203:531–539. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Lima LL, Parente RC and Maestá I: Amim
Junior J, de Rezende Filho JF, Montenegro CA and Braga A: Clinical
and radiological correlations in patients with gestational
trophoblastic disease. Radiol Bras. 49:241–250. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Soper JT: Gestational trophoblastic
disease. Obstet Gynecol. 108:176–187. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Ghaemmaghami F, Behtash N, Soleimani K and
Hanjani P: Management of patients with metastatic gestational
trophoblastic tumor. Gynecol Oncol. 94:187–190. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
FIGO Committee on Gynecologic Oncology:
Current FIGO staging for cancer of the vagina, fallopian tube,
ovary, and gestational trophoblastic neoplasia. Int J Gynaecol
Obstet. 105:3–4. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Chen Y, Qian H, Wang H, Zhang X, Fu M,
Liang X, Ma Y, Zhan Q, Lin C and Xiang Y: Ad-PUMA sensitizes
drug-resistant choriocarcinoma cells to chemotherapeutic agents.
Gynecol Oncol. 107:505–512. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Suksai M, Suwanrath C, Kor-Anantakul O,
Geater A, Hanprasertpong T, Atjimakul T and Pichatechaiyoot A:
Complete hydatidiform mole with co-existing fetus: Predictors of
live birth. Eur J Obstet Gynecol Reprod Biol. 212:1–8. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Schwentner L, Schmitt W, Bartusek G,
Kreienberg R and Herr D: Cervical hydatidiform mole pregnancy after
missed abortion presenting with severe vaginal bleeding: Case
report and review of the literature. Eur J Obstet Gynecol Reprod
Biol. 156:9–11. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Tse KY and Ngan HY: Gestational
trophoblastic disease. Best Pract Res Clin Obstet Gynaecol.
26:357–370. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
McDonald TW and Ruffolo EH: Modern
management of gestational trophoblastic disease. Obstet Gynecol
Surv. 38:67–83. 1983. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Ozalp SS, Telli E, Oge T, Tulunay G, Boran
N, Turan T, Yenen M, Kurdoglu Z, Ozler A, Yuce K, et al:
Multicenter analysis of gestational trophoblastic neoplasia in
Turkey. Asian Pac J Cancer Prev. 15:3625–3628. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Akyol A, Şimşek M and Üçer Ö: Giant
invasive mole presenting as a cause of abdominopelvic mass in a
perimenopausal woman: An unusual presentation of a rare pathology.
Obstet Gynecol Sci. 59:548–553. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Garner EI, Goldstein DP, Feltmate CM and
Berkowitz RS: Gestational trophoblastic disease. Clin Obstet
Gynecol. 50:112–122. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Ibi T, Hirai K, Bessho R, Kawamoto M,
Koizumi K and Shimizu K: Choriocarcinoma of the lung: Report of a
case. Gen Thorac Cardiovasc Surg. 60:377–380. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Berkowitz RS and Goldstein DP: Current
management of gestational trophoblastic diseases. Gynecol Oncol.
112:654–662. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Monchek R and Wiedaseck S: Gestational
trophoblastic disease: An overview. J Midwifery Womens Health.
57:255–259. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Shih IM and Kurman RJ: The pathology of
intermediate trophoblastic tumors and tumor-like lesions. Int J
Gynecol Pathol. 20:31–47. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Scully RE and Young RH: Trophoblastic
pseudotumor: A reappraisal. Am J Surg Pathol. 5:75–76. 1981.
View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Behnamfar F, Rouholamin S and Esteki M:
Presentation of Placental Site Trophoblastic Tumor with Amenorrhea.
Adv Biomed Res. 6:292017. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Eckstein RP, Paradinas FJ and Bagshawe KD:
Placental site trophoblastic tumour (trophoblastic pseudotumour): A
study of four cases requiring hysterectomy including one fatal
case. Histopathology. 6:211–226. 1982. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Newlands ES, Mulholland PJ, Holden L,
Seckl MJ and Rustin GJ: Etoposide and cisplatin/etoposide,
methotrexate, and actinomycin D (EMA) chemotherapy for patients
with high-risk gestational trophoblastic tumors refractory to
EMA/cyclophosphamide and vincristine chemotherapy and patients
presenting with metastatic placental site trophoblastic tumors. J
Clin Oncol. 18:854–859. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Park JW and Bae JW: Epithelioid
Trophoblastic Tumor in a Postmenopausal Woman: A Case Report. J
Menopausal Med. 22:50–53. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Rodríguez-Trujillo A, Martínez-Serrano MJ,
Saco A and Torné A: Two cases of epithelioid trophoblastic tumors
in postmenopausal women. Menopause. 24:1304–1308. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Davis MR, Howitt BE, Quade BJ, Crum CP,
Horowitz NS, Goldstein DP and Berkowitz RS: Epithelioid
trophoblastic tumor: A single institution case series at the New
England Trophoblastic Disease Center. Gynecol Oncol. 137:456–461.
2015. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Kim JH, Lee SK, Hwang SH, Kim JS, Yoon G,
Lee YY, Kim TJ, Choi CH, Kim BG, Bae DS, et al: Extrauterine
epithelioid trophoblastic tumor in hysterectomized woman. Obstet
Gynecol Sci. 60:124–128. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Abrão RA, de Andrade JM, Tiezzi DG, Marana
HR, Candido dos Reis FJ and Clagnan WS: Treatment for low-risk
gestational trophoblastic disease: Comparison of single-agent
methotrexate, dactinomycin and combination regimens. Gynecol Oncol.
108:149–153. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Lima LLA, Padron L, Câmara R, Sun SY,
Rezende J and Braga A: The role of surgery in the management of
women with gestational trophoblastic disease. Rev Col Bras Cir.
44:94–101. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Eoh KJ, Chung YS, Yim GW, Nam EJ, Kim S,
Kim SW and Kim YT: Role of surgical therapy in the management of
gestational trophoblastic neoplasia. Obstet Gynecol Sci.
58:277–283. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Berkowitz RS and Goldstein DP: Clinical
practice. Molar pregnancy. N Engl J Med. 360:1639–1645. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Hurteau JA: Gestational trophoblastic
disease: Management of hydatidiform mole. Clin Obstet Gynecol.
46:557–569. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
41
|
Gerulath AH, Ehlen TG, Bessette P,
Jolicoeur L and Savoie R;: Society of Obstetricians and
Gynaecologists of CanadaGynaecologic Oncologists of Canada; Society
of Canadian Colposcopists: Gestational trophoblastic disease. J
Obstet Gynaecol Can. 24:434–446. 2002.(In English; French).
PubMed/NCBI
|
|
42
|
Sebire NJ and Seckl MJ: Gestational
trophoblastic disease: Current management of hydatidiform mole.
BMJ. 337:a11932008. View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Kang WD, Choi HS and Kim SM: Weekly
methotrexate (50mg/m(2)) without dose escalation as a primary
regimen for low-risk gestational trophoblastic neoplasia. Gynecol
Oncol. 117:477–480. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
44
|
De Vos M, Leunen M, Fontaine C and De
Sutter P: Successful Primary Treatment of a Hydatidiform Mole with
Methotrexate and EMA/CO. Case Rep Med. 2009:4541612009. View Article : Google Scholar : PubMed/NCBI
|
|
45
|
Shanbhogue AK, Lalwani N and Menias CO:
Gestational trophoblastic disease. Radiol Clin North Am.
51:1023–1034. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
46
|
Wenzel L, Berkowitz RS, Newlands E,
Hancock B, Goldstein DP, Seckl MJ, Habbal R, Bernstein M, Kluhsman
B, Kulchak-Rahm A, et al: Quality of life after gestational
trophoblastic disease. J Reprod Med. 47:387–394. 2002.PubMed/NCBI
|
|
47
|
Lurain JR: Gestational trophoblastic
disease II: Classification and management of gestational
trophoblastic neoplasia. Am J Obstet Gynecol. 204:11–18. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
48
|
Karjoo Z, Chen X and Hatefi A: Progress
and problems with the use of suicide genes for targeted cancer
therapy. Adv Drug Deliv Rev. 99(Pt A): 113–128. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
49
|
Zawilska JB, Wojcieszak J and Olejniczak
AB: Prodrugs: a challenge for the drug development. Pharmacol Rep.
65:1–14. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
50
|
Schellmann N, Deckert PM, Bachran D, Fuchs
H and Bachran C: Targeted enzyme prodrug therapies. Mini Rev Med
Chem. 10:887–904. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
51
|
Springer CJ, Bagshawe KD, Sharma SK,
Searle F, Boden JA, Antoniw P, Burke PJ, Rogers GT, Sherwood RF and
Melton RG: Ablation of human choriocarcinoma xenografts in nude
mice by antibody-directed enzyme prodrug therapy (ADEPT) with three
novel compounds. Eur J Cancer. 27:1361–1366. 1991. View Article : Google Scholar : PubMed/NCBI
|
|
52
|
Bagshawe KD, Springer CJ, Searle F,
Antoniw P, Sharma SK, Melton RG and Sherwood RF: A cytotoxic agent
can be generated selectively at cancer sites. Br J Cancer.
58:700–703. 1988. View Article : Google Scholar : PubMed/NCBI
|
|
53
|
Zhang J, Kale V and Chen M: Gene-directed
enzyme prodrug therapy. AAPS J. 17:102–110. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
54
|
Weyel D, Sedlacek HH, Müller R and
Brüsselbach S: Secreted human beta-glucuronidase: A novel tool for
gene-directed enzyme prodrug therapy. Gene Ther. 7:224–231. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
55
|
Alenzi FQ, Lotfy M, Tamimi WG and Wyse RK:
Review: Stem cells and gene therapy. Lab Hematol. 16:53–73. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
56
|
Müller FJ, Snyder EY and Loring JF: Gene
therapy: Can neural stem cells deliver? Nat Rev Neurosci. 7:75–84.
2006. View Article : Google Scholar : PubMed/NCBI
|
|
57
|
Benedetti S, Pirola B, Pollo B, Magrassi
L, Bruzzone MG, Rigamonti D, Galli R, Selleri S, Di Meco F, De
Fraja C, et al: Gene therapy of experimental brain tumors using
neural progenitor cells. Nat Med. 6:447–450. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
58
|
Aboody KS, Brown A, Rainov NG, Bower KA,
Liu S, Yang W, Small JE, Herrlinger U, Ourednik V, Black PM, et al:
Neural stem cells display extensive tropism for pathology in adult
brain: Evidence from intracranial gliomas. Proc Natl Acad Sci USA.
97:12846–12851. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
59
|
Ahmed AU, Alexiades NG and Lesniak MS: The
use of neural stem cells in cancer gene therapy: Predicting the
path to the clinic. Curr Opin Mol Ther. 12:546–552. 2010.PubMed/NCBI
|
|
60
|
Consiglio A, Gritti A, Dolcetta D,
Follenzi A, Bordignon C, Gage FH, Vescovi AL and Naldini L: Robust
in vivo gene transfer into adult mammalian neural stem cells by
lentiviral vectors. Proc Natl Acad Sci USA. 101:14835–14840. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
61
|
Heo JR, Kim NH, Cho J and Choi KC: Current
treatments for advanced melanoma and introduction of a promising
novel gene therapy for melanoma (Review). Oncol Rep. 36:1779–1786.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
62
|
Zhao D, Najbauer J, Garcia E, Metz MZ,
Gutova M, Glackin CA, Kim SU and Aboody KS: Neural stem cell
tropism to glioma: Critical role of tumor hypoxia. Mol Cancer Res.
6:1819–1829. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
63
|
Yi BR, Hwang KA, Aboody KS, Jeung EB, Kim
SU and Choi KC: Selective antitumor effect of neural stem cells
expressing cytosine deaminase and interferon-beta against ductal
breast cancer cells in cellular and xenograft models. Stem Cell Res
(Amst). 12:36–48. 2014. View Article : Google Scholar
|
|
64
|
Yi BR, Kim SU and Choi KC: Co-treatment
with therapeutic neural stem cells expressing carboxyl esterase and
CPT-11 inhibit growth of primary and metastatic lung cancers in
mice. Oncotarget. 5:12835–12848. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
65
|
Magge SN, Malik SZ, Royo NC, Chen HI, Yu
L, Snyder EY, O'Rourke DM and Watson DJ: Role of monocyte
chemoattractant protein-1 (MCP-1/CCL2) in migration of neural
progenitor cells toward glial tumors. J Neurosci Res. 87:1547–1555.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
66
|
Bonini C, Bondanza A, Perna SK, Kaneko S,
Traversari C, Ciceri F and Bordignon C: The suicide gene therapy
challenge: how to improve a successful gene therapy approach. Mol
Ther. 15:1248–1252. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
67
|
Joo KM, Park IH, Shin JY, Jin J, Kang BG,
Kim MH, Lee SJ, Jo MY, Kim SU and Nam DH: Human neural stem cells
can target and deliver therapeutic genes to breast cancer brain
metastases. Mol Ther. 17:570–575. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
68
|
Green LK, Storey MA, Williams EM,
Patterson AV, Smaill JB, Copp JN and Ackerley DF: The Flavin
Reductase MsuE Is a Novel Nitroreductase that Can Efficiently
Activate Two Promising Next-Generation Prodrugs for Gene-Directed
Enzyme Prodrug Therapy. Cancers (Basel). 5:985–997. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
69
|
Park GT, Kim SU and Choi KC:
Anti-proliferative Effect of Engineered Neural Stem Cells
Expressing Cytosine Deaminase and Interferon-beta against Lymph
Node-Derived Metastatic Colorectal Adenocarcinoma in Cellular and
Xenograft Mouse Models. Cancer Res Treat. 49:79–91. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
70
|
Xie Y, Gilbert JD, Kim JH and Freytag SO:
Efficacy of adenovirus-mediated CD/5-FC and HSV-1 thymidine
kinase/ganciclovir suicide gene therapies concomitant with p53 gene
therapy. Clin Cancer Res. 5:4224–4232. 1999.PubMed/NCBI
|
|
71
|
Mahan SD, Ireton GC, Knoeber C, Stoddard
BL and Black ME: Random mutagenesis and selection of Escherichia
coli cytosine deaminase for cancer gene therapy. Protein Eng
Des Sel. 17:625–633. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
72
|
Vermes A, Guchelaar HJ and Dankert J:
Flucytosine: A review of its pharmacology, clinical indications,
pharmacokinetics, toxicity and drug interactions. J Antimicrob
Chemother. 46:171–179. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
73
|
Ardiani A, Johnson AJ, Ruan H,
Sanchez-Bonilla M, Serve K and Black ME: Enzymes to die for:
Exploiting nucleotide metabolizing enzymes for cancer gene therapy.
Curr Gene Ther. 12:77–91. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
74
|
Kim DJ, Yi BR, Lee HR, Kim SU and Choi KC:
Pancreatic tumor mass in a xenograft mouse model is decreased by
treatment with therapeutic stem cells following introduction of
therapeutic genes. Oncol Rep. 30:1129–1136. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
75
|
Yi BR, Park MA, Lee HR, Kang NH, Choi KJ,
Kim SU and Choi KC: Suppression of the growth of human colorectal
cancer cells by therapeutic stem cells expressing cytosine
deaminase and interferon-β via their tumor-tropic effect in
cellular and xenograft mouse models. Mol Oncol. 7:543–554. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
76
|
Yi BR, Kim SU and Choi KC: Additional
effects of engineered stem cells expressing a therapeutic gene and
interferon-β in a xenograft mouse model of endometrial cancer. Int
J Oncol. 47:171–178. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
77
|
Panelli MC and Marincola FM: Immunotherapy
update: from interleukin-2 to antigen-specific therapy. ASCO
educational book. Perry MC: American Society of Clinical Oncology.
467–473. 1998.
|
|
78
|
Kim GS, Heo JR, Kim SU and Choi KC:
Cancer-Specific Inhibitory Effects of Genetically Engineered Stem
Cells Expressing Cytosine Deaminase and Interferon-β Against
Choriocarcinoma in Xenografted Metastatic Mouse Models. Transl
Oncol. 11:74–85. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
79
|
Zwaka TP: Use of Genetically Modified Stem
Cells in Experimental Gene Therapies. National Institutes of Health
(US). (Bethesda, MD). 2006.
|
|
80
|
Ehtesham M, Kabos P, Kabosova A, Neuman T,
Black KL and Yu JS: The use of interleukin 12-secreting neural stem
cells for the treatment of intracranial glioma. Cancer Res.
62:5657–5663. 2002.PubMed/NCBI
|
|
81
|
Yuan X, Hu J, Belladonna ML, Black KL and
Yu JS: Interleukin-23-expressing bone marrow-derived neural
stem-like cells exhibit antitumor activity against intracranial
glioma. CancerRes. 66:2630–2638. 2006.
|