Introduction
Childhood acute leukemia (AL) is the most common
malignant tumor that invades the blood system of children. It is
also the malignant tumor of children with the highest incidence
rate, which seriously threatens the life and health of children
(1–3). At present, the pathogenesis of
childhood AL remains unclear. It is generally believed that its
occurrence is closely related to genetic and environmental factors,
but there are still no measures to prevent and control the
occurrence of this disease (4).
Therefore, it is necessary for people to further understand and
explore the pathogenesis of childhood AL, which is of great
significance for its prevention and treatment in the future.
As a novel deoxycytidine analog and nucleoside
reductase inhibitor, gemcitabine (GEM) is a metabolic anticancer
drug with a molecular weight of 263.20 and a molecular formula of
C9H11F2N3O4
(5). Clinically, it is mainly
applied as a second-line drug for advanced pancreatic cancer
adopted when fluorouracil treatment fails, which can markedly
improve patients' quality of life. Besides, this drug exhibits a
highly curative effect on metastatic non-small cell lung cancer.
Studies have denoted that GEM can act on the DNA synthesis stage in
tumor cells to inhibit DNA synthesis and make DNA strand breaks. In
addition, a study has pointed out that GEM can also impede the
self-repair function of DNA (6). It
is worth noting that the side effects of the drug become more
serious as the infusion time prolongs. Especially for elderly
patients with poor renal function, appropriate dose reduction or
intermittent administration should be adopted in clinical treatment
(7). A large number of studies have
confirmed that GEM performs well in treating non-small cell lung
cancer and pancreatic cancer, but there are few reports on whether
GEM can be used to treat childhood AL.
Micro ribonucleic acids (miRNAs) are a kind of
non-coding single-stranded RNAs with a length of ~20–24
nucleotides, which participate in the biological processes of
regulating individual development, growth, and proliferation,
differentiation and apoptosis of cells (8–10). Some
studies have pointed out that over 90% of genes are regulated by
miRNAs. Thus, it is essential to investigate the regulatory effect
of miRNAs in physiological and pathological processes of the body.
Some studies have discovered that the level of miR-125a-3p declines
in the case of acute myeloid leukemia, but there are few reports on
whether GEM can affect the proliferation and apoptosis of childhood
AL cells by regulating the level of miR-125a-3p.
In this study, the level of miR-125a-3p in the
peripheral blood of healthy children and AL children was compared.
The results revealed that the level of miR-125a-3p in the
peripheral blood of AL children was overtly reduced. Then,
childhood AL cells were primarily cultured and purified. After
incubation, the effect of GEM on proliferation and apoptosis of
childhood AL cells was observed and its mechanism of action is
reported.
Materials and methods
Reagents
GEM was from Jianze Co., 1640 medium and fetal
bovine serum were from HyClone, culture plates and bottles were
from Corning, the 5-ethynyl-2′-deoxyuridine (EdU) and terminal
deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) kits
were from Nanjing KeyGen Biotech Co., Ltd., miR-125a-3p mimic and
miRNA extraction kit were from Shanghai Gene Pharma Co., Ltd., MTT
was from Amresco, LLC, SYBR Primer Ex Taq fluorescent quantitative
polymerase chain reaction (PCR) kit was from Takara, miR-125a-3p
and U6 primers were from Applied Biosystems; Thermo Fisher
Scientific, Inc., and c-myc, reduced glyceraldehyde-phosphate
dehydrogenase (GAPDH) primary anti-antibody and hypothalamic
regulatory peptides (HRP) labeled secondary antibody were from
Beijing Bioss Biotechnology Co., Ltd.
Instruments
The fluorescent inverted microscope was from
Olympus. The CO2 incubator was from Thermo Fisher
Scientific, Inc. The fluorescence quantitative PCR instrument was
from Applied Biosystems; Thermo Fisher Scientific, Inc. The
ultrapure water meter was from Millipore, France. The high-speed
low-temperature centrifuge was from Beckman Coulter, Inc.
Clinical data
Nineteen untreated children (10 males and 9 females)
with AL diagnosed by bone marrow cell morphology analysis, flow
cytometry immunotyping and fusion gene in Yidu Central Hospital of
Weifang (Weifang, China) from August 2015 to September 2018 were
selected. Nine children with normal bone marrow and without
hematological diseases were randomly selected as control. This
study was conducted with the informed consent of family members of
the children. The study was approved by the Ethics Committee of
Yidu Central Hospital of Weifang.
Methods
Detection of miR-125a-3p level in
peripheral blood of healthy children and children with AL by
quantitative reverse transcription-PCR (qRT-PCR)
The peripheral blood of children in each group was
collected and added with TRIzol reagent. Total RNA in each group of
blood was extracted and reverse transcribed into complementary
deoxyribonucleic acid (cDNA), and the target gene fragment was
amplified adopting the first strand cDNA as a template. The sample
was put into a fluorescence quantitative PCR instrument.
Information on the primers is provided in Table I with U6 gene as the internal
reference.
 | Table I.Sequence information of miR-125a-3p
and U6 primers. |
Table I.
Sequence information of miR-125a-3p
and U6 primers.
| Gene name | Primer sequences |
|---|
| miR-125a-3p |
ACGTGTGTAGCTTATCAGACTG |
|
|
AATGGTTGTTCTCCACACTCTC |
| U6 |
GCGCGTCGTGAAGCGTTC |
|
| GTGCAGGGTCCGAGGT |
Culture and transfection of childhood
AL cells
Under aseptic conditions, the bone marrow samples
collected were added with separation liquid, centrifuged at 200 × g
for 15 min at 4°C, and then the intermediate cell layer was inhaled
and transferred into a new EP tube, washed with phosphate-buffered
saline (PBS) solution and centrifuged again at 200 × g for 5 min at
4°C. The supernatant was discarded, and the suspended sediment was
inoculated in a culture bottle with 1640 complete culture medium,
placed in a CO2 incubator to start the culture, and
subcultured after 3–5 days. The cells were randomly divided into
three groups: GEM group (10 µg/ml, 24 h), GEM + miR-125a-3p mimic
group (when the cell fusion degree was over 80%, miR-125a-3p mimic
was transfected into childhood AL cells using Lipofectamine 2000
transfection technology, with GEM final concentration reaching 10
µg/ml), and control group (childhood AL cells without any
treatment).
Detection of GEM's effect on
proliferation of childhood AL cells through EdU staining
Cells in each group were fixed with 4%
paraformaldehyde for 15 min, and permeabilized with 0.3% Triton
X-100 solution for 15 min. EdU staining solution was added to each
well and protected from light for 30 min. After washing with PBS
solution, the anti-fluorescence quencher was added, and staining
was observed under a fluorescence microscope.
Detection of the GEM effect on
apoptosis of childhood AL cells by TUNEL staining
Cells in each group were collected, fixed and
permeabilized as indicated above. Each well of cells was added with
50 µl of TUNEL detection solution, then incubated at 37°C in the
dark for 60 min, washed three times with PBS solution for 5 min,
added with anti-fluorescence quencher, and finally placed under a
microscope to observe the TUNEL staining.
Detection of c-myc protein level in
childhood AL cells via western blotting
Each group of cells were lysed utilizing RIPA
lysate, centrifuged at 500 × g for 5 min at 4°C and collected. The
protein concentration of cells in each group was detected by
Bradford method to ensure the same amount of protein samples
loaded. Then SDS-PAGE was performed, and the cells were transferred
to a PVDF membrane. Then, the membrane was sealed with 5% defatted
milk powder solution for 1 h, and incubated with c-myc primary
anti-antibody (1:1,000) and internal reference GAPDH primary
anti-antibody (1:1,000) overnight at 4°C and then the HRP labeled
secondary antibody for 1 h. Finally, DAB color development solution
was applied, and the band optical density value was analyzed.
Statistical analysis
SPSS 17.0 software was employed for analysis. The
data were expressed by mean standard ± deviation, and the mean of
two samples was tested by t-test. P<0.05 indicates that the
difference is statistically significant.
Results
Decreased level of miR-125a-3p in
peripheral blood of AL children
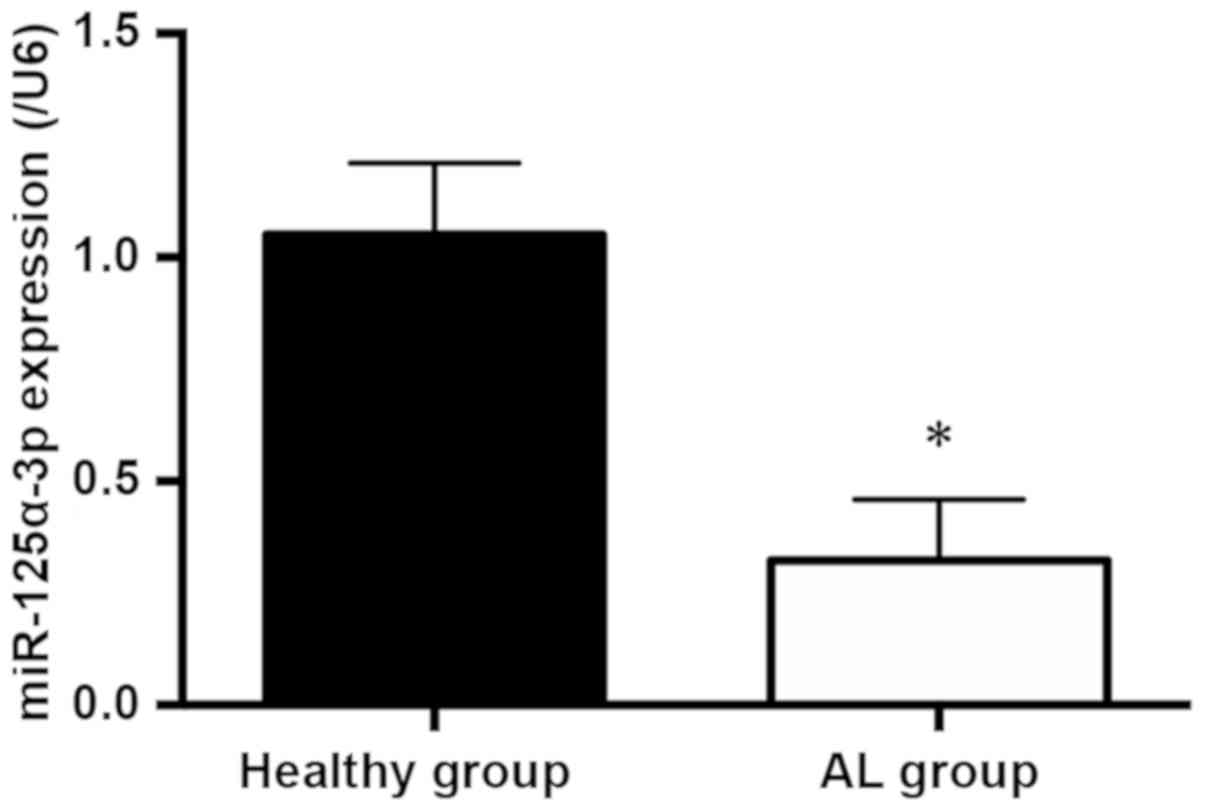
The qRT-PCR results are exhibited in Fig. 1. Compared with that in the healthy
children group, the miR-125a-3p level in the peripheral blood cells
of AL children was remarkably reduced (P<0.05).
Culture of childhood AL cells
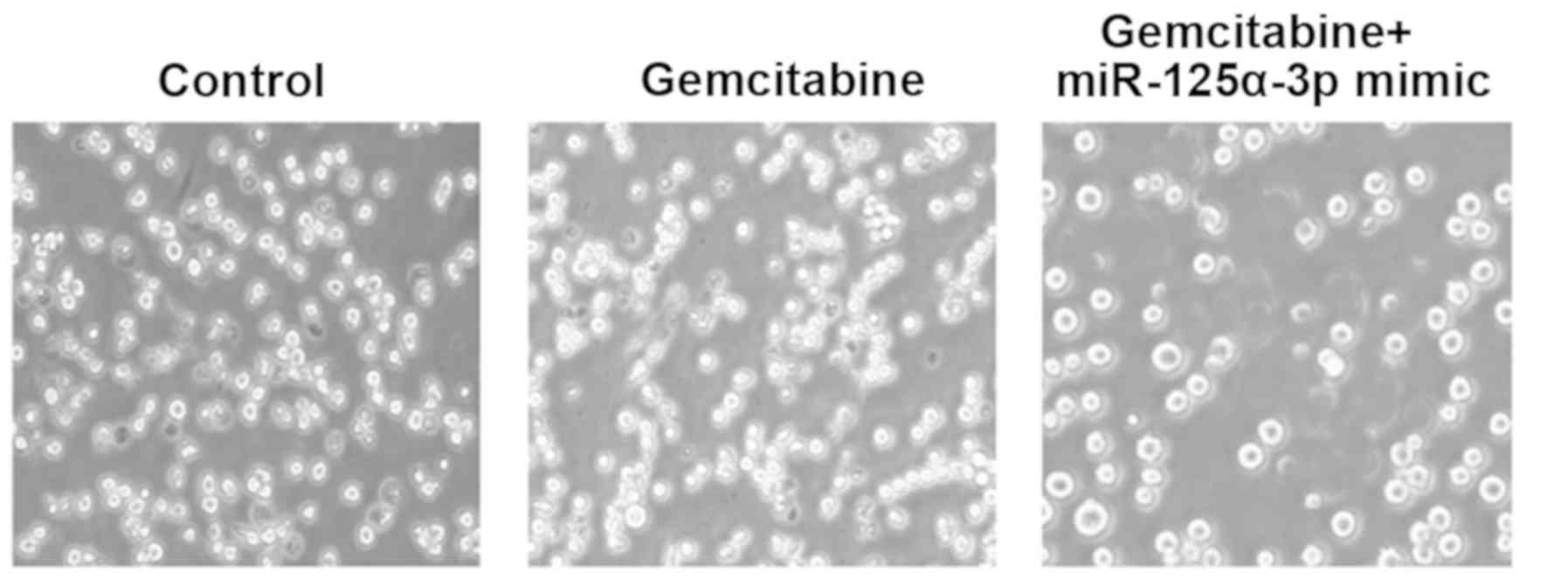
Morphology of cells was observed under a microscope
(Fig. 2). Childhood AL cells were
seen as small round bright spots, clusters of cells were observed,
and there were a great number of cells. Compared with the childhood
AL group, cells grew in suspension in the culture plate, with weak
opacity and the occurrence of dead cell fragments in the GEM group.
In the GEM + miR-125a-3p mimic group, compared with the former two
groups, the number of cells was distinctly reduced, the cell state
was relatively poor, and more dead cells floated in the culture
well.
GEM inhibits the proliferation of
childhood AL cells
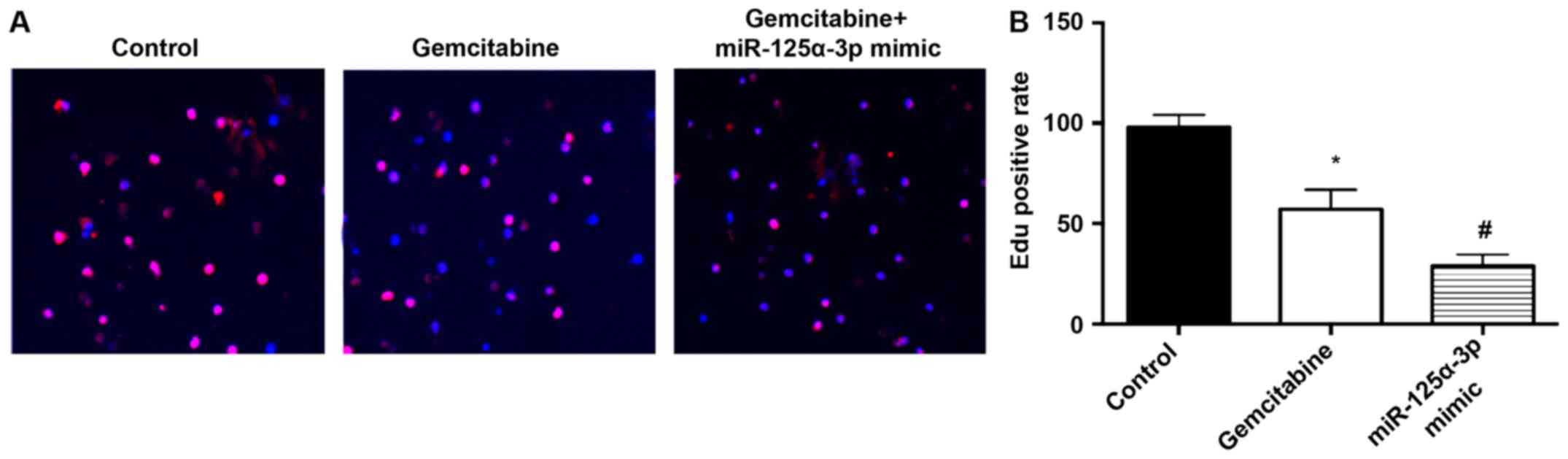
Fig. 3A presents EdU
staining results. Compared with that in the control group, the
proliferation rate of cells in the GEM group was alleviated
(P<0.05). Compared with that in the GEM group, the proliferation
rate of cells in the GEM + miR-125a-3p mimic group was enhanced
(P<0.05) (Fig. 3B).
GEM promotes apoptosis of childhood AL
cells
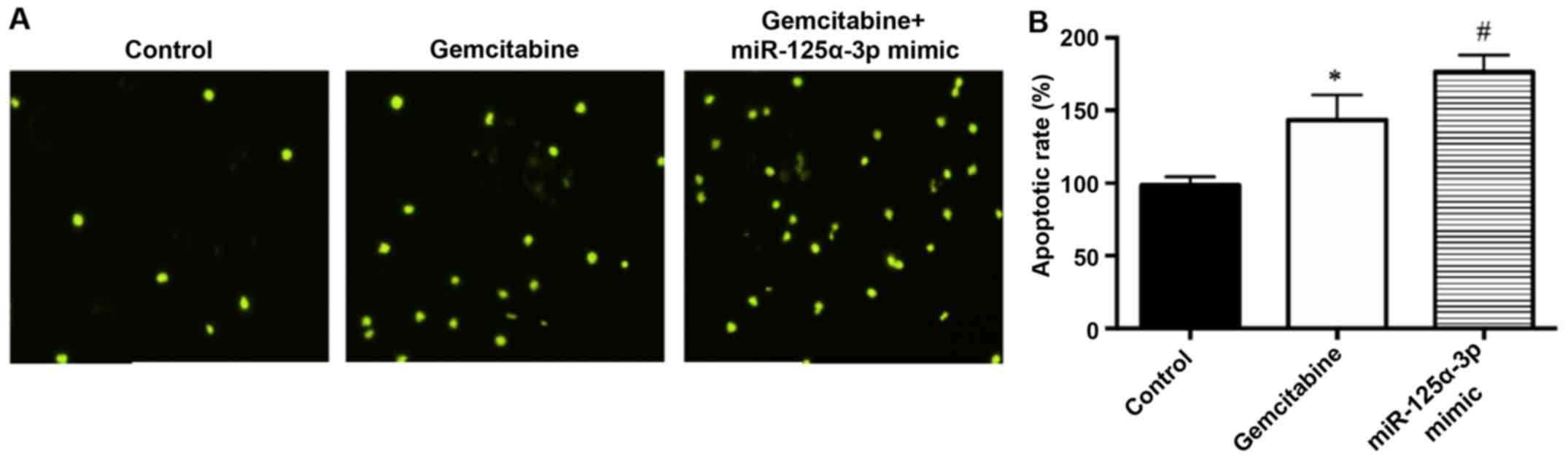
TUNEL staining results are presented in Fig. 4A. Compared with that in the control
group, the apoptosis rate of cells in the GEM group was decreased
(P<0.05). Compared with that in the GEM group, the apoptosis
rate of cells in the GEM + miR-125a-3p mimic group increased
(P<0.05) (Fig. 4B).
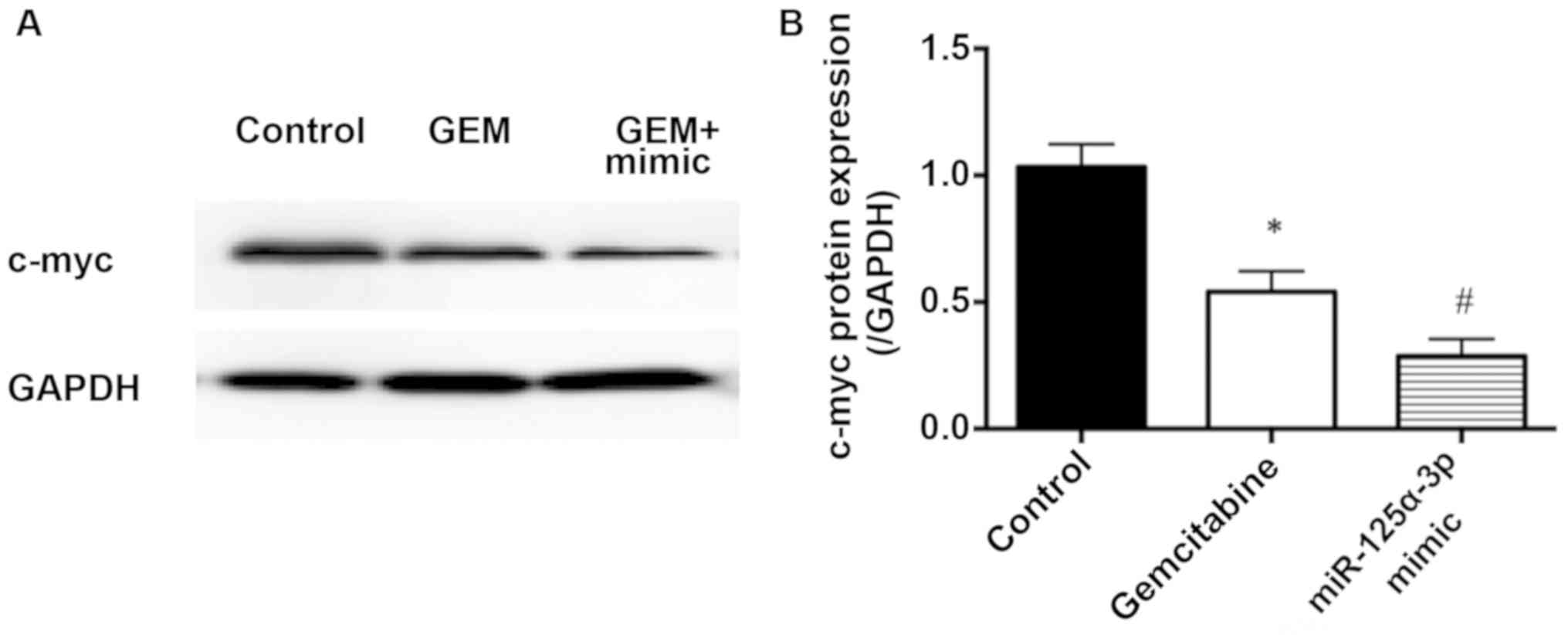
GEM impedes the protein level of c-myc
in childhood AL cells
Western blotting bands are revealed in Fig. 5A. Compared with that in the control
group, the protein level of c-myc in the GEM group was
downregulated (P<0.05). Compared with that in the GEM group, the
protein level of c-myc in the GEM + miR-125a-3p mimic group was
distinctly reduced (P<0.05), as shown in Fig. 5B.
Discussion
Childhood AL generally refers to childhood acute
lymphoblastic leukemia. Due to abnormal clonal proliferation of
precursor B, T or mature B lymphocytes, extensive infiltration of
organs and tissues throughout the body destroys normal structures
and functions of organs, eventually leading to organ failure and
even death (11,12). With the advancement of molecular
biology technology, certain progress has been made in the treatment
of childhood AL. According to statistics, the 5-year disease-free
survival rate of patients with childhood AL can reach >80%, and
some of them can even be cured (13,14).
However, there are still patients who can not be effectively
relieved even if they are treated. As a result, it is particularly
vital to find new anti-leukemia drugs with low toxicity (15,16).
In recent years, research on non-coding RNAs has
received increased attention, and the biological function of miRNAs
in the body is worth exploring. The generation process of miRNAs in
organisms is as follows. The precursor miRNAs are sheared and
processed by some nucleases to generate mature miRNAs. They then
bind to the target gene mRNA through base complementary pairing to
enhance its degradation or hinder its translation into protein
(17). Increasingly more studies
have proved that miRNAs play a key role in childhood AL. A study
discovered the abnormal expression of miRNAs in blood samples of
children with AL, and further indicated that miR-125b and miR-203
are potential molecular markers for diagnosing childhood AL
(18). In addition, the study by
Swellam et al (19) denoted
that the levels of miR-143 and miR-182 in bone marrow samples of
children with AL are decreased, and the prognosis of patients is
poor. It reveals that abnormally expressed miRNAs play a key role
in the development and progression of childhood AL.
In this study, the level of miR-125a-3p in the
peripheral blood of healthy children and AL children was analyzed.
qRT-PCR results showed that the level of miR-125a-3p in the
peripheral blood of AL children was reduced as remarkably as ~50%,
as shown in Fig. 1. Then the bone
marrow of AL children was collected, and leukemic cells were
extracted and separated. GEM was chosen to incubate the cells, and
then miR-125a-3p mimic was transfected into leukocytes by means of
Lipofectamine 2000 transfection technology to explore regulatory
effect of GEM on proliferation and apoptosis of childhood AL cells.
Subsequently, EdU staining was adopted to investigate the effect of
GEM on proliferation of childhood AL cells. The results corroborate
that GEM can notably inhibit cell proliferation compared to the
control group. TUNEL staining was applied to determine the
regulatory effect of GEM on apoptosis of childhood AL cells. The
results indicate that GEM can markedly impede apoptosis of cells,
and the combined use of GEM and miR-125a-3p mimic has a greater
effect on inhibiting apoptosis of cells. miR-125a-3p can bind to
its downstream target gene c-myc, which is an important member of
oncogenic genes and participates in the regulation of the
occurrence and development of various tumors (20). In order to explore the mechanism of
GEM, western blotting was chosen to uncover how GEM regulates
c-myc, the downstream target of miR-125a-3p. Results are shown in
Fig. 5, the protein expression level
of c-myc in childhood AL cells was reduced markedly after GEM
treatment.
In conclusion, GEM can effectively inhibit
proliferation and promotes apoptosis of childhood AL cells. Its
mechanism of action may be related to the upregulation of
miR-125a-3p to inhibit the expression of c-myc. The results of this
study provide an experimental basis for miR-125a-3p to be applied
in the treatment of childhood AL.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
WX wrote the manuscript. WX and YY collected and
analyzed general data of patients. SY performed PCR. GL and WX
helped with EdU staining and TUNEL staining. All authors read and
approved the final manuscript.
Ethics approval and consent to
participate
The study was approved by the Ethics Committee of
Yidu Central Hospital of Weifang (Weifang, China) and informed
consents were signed by the patients' guardians.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Intusoma U, Nakorn CN and
Chotsampancharoen T: Intracranial hemorrhage in childhood acute
leukemia: Incidence, characteristics, and contributing factors.
Pediatr Neurol. 99:23–30. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Park SH, Lee MJ, Park CJ, Jang S, Seo EJ,
Im HJ and Seo JJ: Bone marrow recovery of hematopoietic stem cells
and microenvironment after chemotherapy in childhood acute
lymphoblastic leukemia: Consecutive observations according to
chemotherapy schedule. Pediatr Hematol Oncol. 36:222–235. 2019.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Rahmani M, Fardi M, Farshdousti Hagh M,
Hosseinpour Feizi AA, Talebi M and Solali S: An investigation of
methylation pattern changes in the IKZF1 promoter in patients with
childhood B-cell acute lymphoblastic leukemia. Blood Res.
54:144–148. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Boulet-Craig A, Robaey P, Barlaam F,
Laniel J, Oswald V, Jerbi K, Sultan S, Affret-Bertout L, Drouin S,
Krajinovic M, et al: Visual short-term memory activation patterns
in adult survivors of childhood acute lymphoblastic leukemia.
Cancer. 125:3639–3648. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Hara H, Kawamoto T, Fukase N, Kawakami Y,
Takemori T, Fujiwara S, Kitayama K, Nishida K, Kuroda R and Akisue
T: Gemcitabine and docetaxel combination chemotherapy for advanced
bone and soft tissue sarcomas: Protocol for an open-label,
non-randomised, Phase 2 study. BMC Cancer. 19:7252019. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Cornacchia MA, Coromilas AJ, Gallitano SM,
Frank RC and Halasz CL: Subacute cutaneous lupus erythematosus
induced by gemcitabine in 2 patients with pancreatic cancer. JAAD
Case Rep. 5:596–601. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Macchini M, Chiaravalli M, Zanon S,
Peretti U, Mazza E, Gianni L and Reni M: Chemotherapy in elderly
patients with pancreatic cancer: Efficacy, feasibility and future
perspectives. Cancer Treat Rev. 72:1–6. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Mohr AM and Mott JL: Overview of microRNA
biology. Semin Liver Dis. 35:3–11. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Simonson B and Das S: MicroRNA
therapeutics: The next magic bullet? Mini Rev Med Chem. 15:467–474.
2015. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Pepin G and Gantier MP: microRNA Decay:
Refining microRNA regulatory activity. MicroRNA. 5:167–174. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Kanderova V, Kuzilkova D, Stuchly J,
Vaskova M, Brdicka T, Fiser K, Hrusak O, Lund-Johansen F and Kalina
T: High-resolution antibody array analysis of childhood acute
leukemia cells. Mol Cell Proteomics. 15:1246–1261. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Madhusoodhan PP, Carroll WL and Bhatla T:
Progress and prospects in pediatric leukemia. Curr Probl Pediatr
Adolesc Health Care. 46:229–241. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Wiemels J: Perspectives on the causes of
childhood leukemia. Chem Biol Interact. 196:59–67. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Pui CH, Carroll WL, Meshinchi S and Arceci
RJ: Biology, risk stratification, and therapy of pediatric acute
leukemias: An update. J Clin Oncol. 29:551–565. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Zimmermannova O, Zaliova M, Moorman AV,
Al-Shehhi H, Fronkova E, Zemanova Z, Kalina T, Vora A, Stary J,
Trka J, et al: Acute lymphoblastic leukemia with aleukemic
prodrome: Preleukemic dynamics and possible mechanisms of
immunosurveillance. Haematologica. 102:e225–e228. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Pålsson A, Malmström M and Follin C:
Childhood leukaemia survivors' experiences of long-term follow-ups
in an endocrine clinic - A focus-group study. Eur J Oncol Nurs.
26:19–26. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Umerez M, Garcia-Obregon S,
Martin-Guerrero I, Astigarraga I, Gutierrez-Camino A and
Garcia-Orad A: Role of miRNAs in treatment response and toxicity of
childhood acute lymphoblastic leukemia. Pharmacogenomics.
19:361–373. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Piatopoulou D, Avgeris M, Drakaki I,
Marmarinos A, Xagorari M, Baka M, Pourtsidis A, Kossiva L,
Gourgiotis D and Scorilas A: Clinical utility of miR-143/miR-182
levels in prognosis and risk stratification specificity of
BFM-treated childhood acute lymphoblastic leukemia. Ann Hematol.
97:1169–1182. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Swellam M, Hashim M, Mahmoud MS, Ramadan A
and Hassan NM: Aberrant expression of some circulating miRNAs in
childhood acute lymphoblastic leukemia. Biochem Genet. 56:283–294.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Jackstadt R and Hermeking H: MicroRNAs as
regulators and mediators of c-MYC function. Biochim Biophys Acta.
1849:544–553. 2015. View Article : Google Scholar : PubMed/NCBI
|