Introduction
Bladder cancer (BCa) is one of the most common type
of cancer of the urinary system (1).
In USA, ~81,190 new cases of BCa were diagnosed in 2018, accounting
for 4.7% of all new cancer cases, and ~17,240 BCa-associated
mortality cases were reported, accounting for 2.8% of all mortality
cases (2). According to the tumor
invasion depth, BCa can be divided into non-muscle invasive bladder
cancer (NMIBC) and muscle invasive bladder cancer (MIBC) (3). Furthermore, ~70% of BCa cases are
NIMBCs, which are characterized by a high-recurrence rate (30-80%)
(4,5). Surgery is the main treatment for
patients with BCa. Transurethral resection of bladder tumors
remains the most commonly used treatment for NMIBC (6), whereas radical cystectomy (RC) combined
with pelvic lymph node dissection (LND) is currently the main
procedure to treat MIBC (7,8).
Based on a statistical analysis of clinical data, it
was reported that increasing the extent of pelvic lymph node
clearance might improve the survival rate of patients with BCa
following RC (9,10). Furthermore, a previous study
demonstrated that extended LND improves the survival rate of
patients with BCa (11). However,
the optimal range of surgical resection and the number of LNDs
remain unclear (12–14). The present study aimed therefore to
evaluate the appropriate number of LNDs to be performed in patients
with BCa.
Following a review of the literature, the majority
of studies investigating the impact of LNDs on the survival rate
and perioperative results of patients with BCa treated with RC were
based on data from medical centers in developed countries (15–17). A
multicenter prospective study on this issue has been previously
conducted in Germany (18). To the
best of our knowledge, there are only a few comparative studies of
data obtained from two medical centers of different countries. The
present study compared data on the degree of LND performed in
patients with BCa who underwent RC treatment in our medical center
with data from USA patients with BCa who underwent RC, which were
collected from the Surveillance, Epidemiology and End Results
(SEER) database.
Materials and methods
Data source and patients
Data from 17,859 patients with BCa who underwent RC
and pelvic lymphadenectomy between January 2004 and December 2015
were collected from the SEER using the National Cancer Institute's
SEER*Stat software version 8.3.5 (19). Bladder malignancies with the ICD-O-3
surgical method site code C670-C679 (seer.cancer.gov/manuals/2018/appendixc.html) were
selected. BCa surgical treatment information was obtained from the
RX summary variable (codes 50, 60–64, 70–74 and 80 were defined as
RC). The SEER database provides information about patients with
cancer, including demographic information, primary tumor location,
cancer staging, treatment and survival time, from 18 registries,
which covers ~28% of the American population (19).
The exclusion criteria were as follows: i) Patients
with unknown number of lymph nodes; ii) patients with unknown
survival time; iii) patients with unknown Tumor-Node-Metastasis
(TNM) stage (20); and iv) patients
aged under 18 years. A total of 17,730 patients with BCa were
qualified and included in the present study.
A total of 158 patients with BCa diagnosed at the
Shanghai Tenth People's Hospital between January 2016 and December
2018 were included in this study. Patients were followed up until
December 2018. The study was approved by the Ethics Committee of
Shanghai Tenth People's Hospital of Tongji University, and written
informed consent was obtained from the patients or their next of
kin if the patient did not have the ability to sign due to lack of
consciousness or physical difficulties.
Study variables
Patient-level clinical information was extracted
from the SEER and the Shanghai Tenth People's Hospital databases
and included age at diagnosis, sex, ethnicity, marital status,
tumor grade, histological type, SEER stage, TNM stage and number of
lymph nodes removed. According to the status of lymph node
metastasis, patients were divided into two groups: N0 and
N-positive (N+). (N+) included the three stages N1, N2 and N3. The
clinicopathological characteristics included age at diagnosis
(<68, 68–78 and >78 years), sex (female and male), ethnicity
(white, black and others) and marital status (married and
unmarried). Tumor variables included SEER stages (localized,
regional and distant), histological type (transitional cell
carcinoma and other), T stage (Ta + Tis, T1, T2, T3 and T4) and M
stage (M0 and M1; cancer.gov/publications/dictionaries/cancer-terms/def/overall-survival).
Tumor grades I, II, III and IV represented well-differentiated,
moderately differentiated, poorly differentiated and
undifferentiated tumors, respectively.
Statistical analysis
χ2 test was used to analyze the
clinicopathological characteristics associated with N-stage.
Kaplan-Meier curves and log-rank test were used to assess the
overall survival (OS) time of patients with BCa. Univariate and
multivariate Cox regression analyses were used to determine the
clinicopathological characteristics associated with OS.
Multivariable Cox regression was used to analyze the patients'
median survival time (MST) following stratification by N-stage in
the SEER and Shanghai Tenth People's Hospital Urology databases.
The stratification boundary for optimal number of LNDs was
determined using X-tile software version 3.6.1 (21). SPSS (version 20.0; IBM Corp.) was
used for all the statistical analyses. P<0.05 was considered to
indicate a statistically significant difference.
Results
Demographic and clinical
characteristics of patients with BCa
A total of 17,730 and 158 patients with BCa were
identified from the SEER database and Shanghai Tenth People's
Hospital databases, respectively. For American N0 and N+ patients,
the median number of dissected nodes was 11.0 [IQR (interquartile
range)=3.0–21.0] and 14.0 (IQR=8.0–23.0), respectively. The median
number of LNDs for Chinese N0 and N+ patients was 5.0 (IQR=2.0–7.0)
and 5.0 (IQR=1.5–10.5), respectively. Table I presents the association between the
clinicopathological characteristics and N-stage of patients with
BCa from the two aforementioned databases following χ2
test analysis. The age at diagnosis was stratified using X-tile
software. The age of patients from the SEER and Shanghai Tenth
People's Hospital database was divided into three groups as
follows: <68, 68–78 and >78 years (Fig. S1). The majority of patients with BCa
were men (75.0% American patients and 86.1% Chinese patients). The
results from χ2 test demonstrated a significant
association between N-stage and numerous variables, including age
at diagnosis (P<0.001), sex (P<0.001), ethnicity (P=0.020),
marital status (P=0.002), SEER stage (P<0.001), tumor grade
(P<0.001), histological type (P=0.009), T-stage (P<0.001) and
M-stage (P<0.001), in patients from the SEER database. In
Chinese patients, N-stage was associated with T-stage (P<0.001)
and M-stage (P<0.001; Table
I).
 | Table I.Clinicopathological characteristics
of patients with bladder cancer stratified by N-stage in the SEER
and Shanghai Tenth People's Hospital Urology databases. |
Table I.
Clinicopathological characteristics
of patients with bladder cancer stratified by N-stage in the SEER
and Shanghai Tenth People's Hospital Urology databases.
| A, SEER
database |
|---|
|
|---|
|
|
| N0 | N+ |
|
|---|
|
|
|
|
|
|
|---|
| Characteristic | All patients, n
(%) | Number (%) | Number (%) | P-value |
|---|
| Total | 17,730 | 13,421 (75.7) | 4,309 (24.3) |
|
| Age at diagnosis,
years |
|
|
| <0.001 |
|
<68 | 8,279 (46.7) | 6,083 (73.5) | 2,196 (26.5) |
|
|
68-78 | 6,567 (37.0) | 5,119 (78.0) | 1,448 (22.0) |
|
|
>78 | 2,884 (16.3) | 2,219 (76.9) | 665 (23.1) |
|
| Sex |
|
|
| <0.001 |
|
Female | 4,431 (25.0) | 3,257 (73.5) | 1,174 (26.5) |
|
|
Male | 13,299 (75.0) | 10,164 (76.4) | 3,135 (23.6) |
|
| Ethnicity |
|
|
| 0.020 |
|
White | 15,722 (88.7) | 11,932 (75.9) | 3,790 (24.1) |
|
|
Black | 308 (6.3) | 802 (72.3) | 308 (27.7) |
|
|
Other | 211 (5.1) | 687 (76.5) | 211 (23.5) |
|
| Marital status |
|
|
| 0.002 |
|
Yes | 11,192 (63.1) | 8,558 (76.5) | 2,634 (23.5) |
|
| No | 6,538 (36.9) | 4,863 (74.4) | 1,675 (25.6) |
|
| SEER stage |
|
|
| <0.001 |
|
Localized | 2,432 (13.7) | 2,432 (100.0) | 0 (0.0) |
|
|
Regional | 14,045 (79.2) | 10,436 (74.3) | 3,609 (25.7) |
|
|
Distant | 1,253 (7.1) | 553 (44.1) | 700 (3.9) |
|
| Grade |
|
|
| <0.001 |
| I | 183 (1.0) | 167 (91.3) | 16 (8.7) |
|
| II | 889 (5.0) | 758 (85.3) | 131 (14.7) |
|
|
III | 5,090 (28.7) | 3,751 (73.7) | 1,339 (26.3) |
|
| IV | 10,545 (59.5) | 7,896 (74.9) | 2,649 (25.1) |
|
|
Unknown | 1,023 (5.8) | 849 (83.0) | 174 (17.0) |
|
| Histological
type |
|
|
| 0.009 |
|
Transitional cell
carcinoma | 16,014 (90.3) | 12,166 (76.0) | 3,848 (24.0) |
|
|
Others | 1,716 (9.7) | 1,255 (73.1) | 461 (26.9) |
|
|
T-stagea |
|
|
| <0.001 |
| Ta +
Tis | 495 (2.8) | 494 (99.8) | 1 (0.2) |
|
| T1 | 2,067 (11.7) | 1,974 (95.5) | 93 (4.5) |
|
| T2 | 6,617 (37.3) | 5,799 (87.6) | 818 (12.4) |
|
| T3 | 5,452 (30.8) | 3,481 (63.8) | 1,971 (36.2) |
|
| T4 | 3,099 (17.5) | 1,673 (54.0) | 1,426 (46.0) |
|
|
M-stagea |
|
|
| <0.001 |
| M0 | 16,874 (95.2) | 13,106 (77.7) | 3,768 (22.3) |
|
| M1 | 856 (4.8) | 315 (36.8) | 541 (63.2) |
|
| Removed lymph
nodes |
|
|
| 0.810 |
|
Mean | 15.1 | 14.3 | 17.6 |
|
|
Median | 11.0 | 11.0 | 14.0 |
|
|
IQR | 4.0–21.0 | 3.0–21.0 | 8.0–23.0 |
|
|
| B, Shanghai
Tenth People's Hospital Urology database |
|
|
|
| N0 | N+ |
|
|
|
|
|
|
|
|
Characteristic | All patients, n
(%) | Number
(%) | Number
(%) | P-value |
|
| Total | 158 | 125 (79.1) | 33 (20.9) |
|
| Age at diagnosis,
years |
|
|
| 0.969 |
|
<68 | 91 (57.6) | 72 (79.1) | 19 (20.9) |
|
|
68-78 | 46 (29.1) | 36 (78.3) | 10 (21.7) |
|
|
>78 | 21 (13.3) | 17 (81.0) | 4
(19.0) |
|
| Sex |
|
|
| 0.819 |
|
Female | 22 (13.9) | 17 (77.3) | 5 (22.7) |
|
|
Male | 136 (86.1) | 108 (79.4) | 28 (20.6) |
|
|
T-stagea |
|
|
| <0.001 |
| Ta +
Tis | 6 (4.8) | 6 (100.0) | 0 (0.0) |
|
| T1 | 61 (38.6) | 56 (91.8) | 5 (8.2) |
|
| T2 | 29 (18.4) | 27 (93.1) | 2 (6.9) |
|
| T3 | 31 (19.6) | 22 (71.0) | 9 (29.0) |
|
| T4 | 31 (19.6) | 14 (45.2) | 17 (54.8) |
|
|
M-stagea |
|
|
| <0.001 |
| M0 | 150 (94.9) | 123 (82.0) | 27 (18.0) |
|
| M1 | 8 (5.1) | 2 (25.0) | 6 (75.0) |
|
| Removed lymph
nodes |
|
|
| <0.001 |
|
Mean | 5.2 | 4.9 | 6.3 |
|
|
Median | 5.0 | 5.0 | 5.0 |
|
|
IQR | 2.0–7.3 | 2.0–7.0 | 1.5–10.5 |
|
Effects of N-stage on the OS of
patients who underwent RC
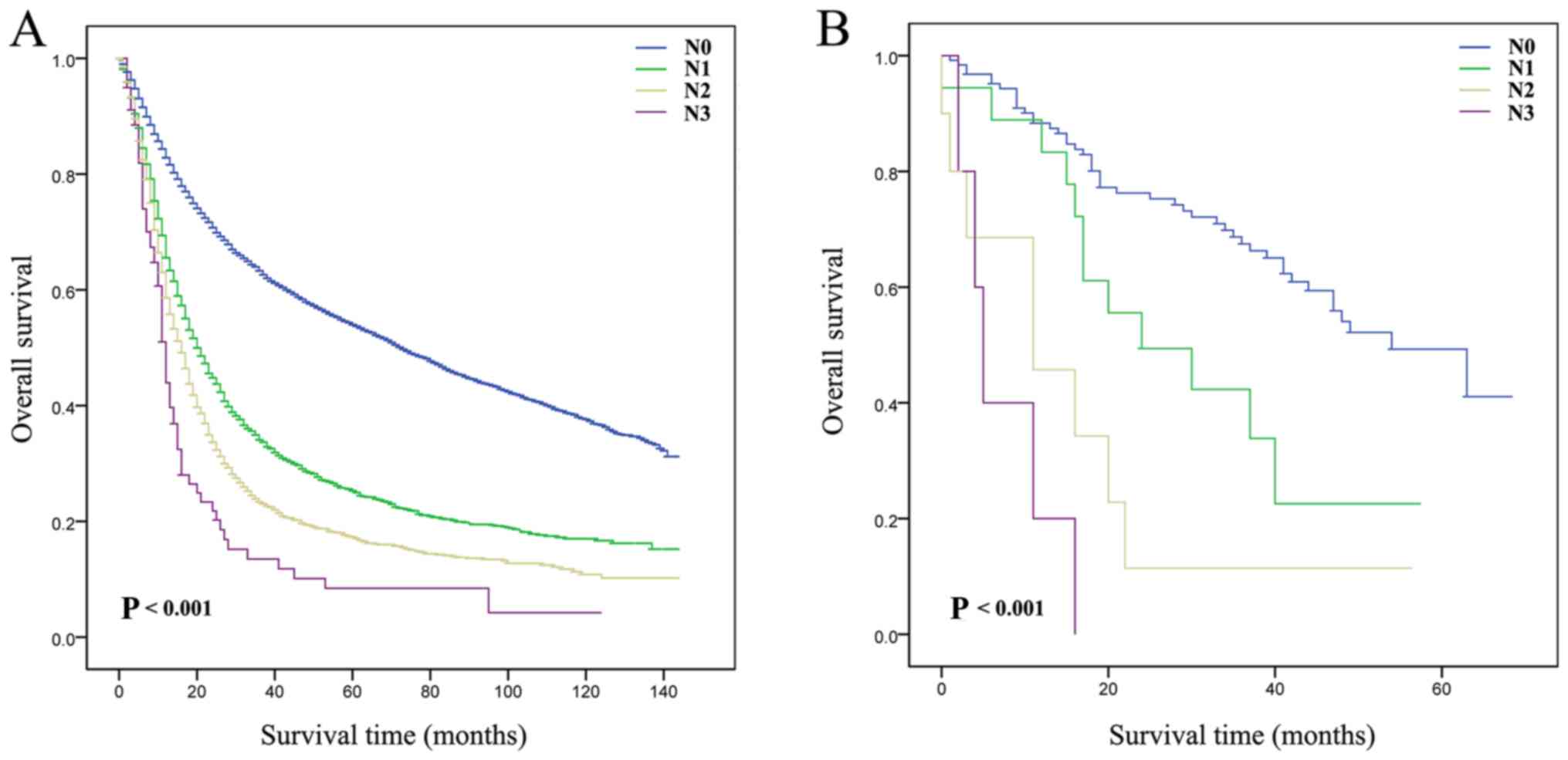
The effect of N-stage on the OS of patients who
underwent RC from the two aforementioned databases was analyzed by
Kaplan-Meier curves. The results demonstrated that the survival
time of American patients from the SEER database was significantly
different depending on the N-stage (P<0.001; Fig. 1A). In addition, a significant
difference in the survival time of Chinese patients between the
N-stage subgroups was demonstrated (P<0.001; Fig. 1B). These findings suggested that
N-stage was significantly associated with OS, and that the survival
time of patients decreased as N-stage increased.
Identification of risk factors for
patients with BCa who underwent RC
Univariate and multivariate Cox regression were used
to analyze the clinicopathological characteristics associated with
the OS of patients with BCa who underwent RC. The results from
univariate Cox regression analysis demonstrated that age at
diagnosis (P<0.001), sex (P<0.001), ethnicity (P<0.001),
marital status (P<0.001), SEER stage (P<0.001), histological
type (P<0.001), tumor grade (P<0.001), T-stage (P<0.001;
TI: P=0.824), N-stage (P<0.001), M-stage (P<0.001) and number
of removed lymph nodes (P<0.001) were significantly associated
with the OS of American patients from the SEER database (Table II). The results from univariate Cox
regression analysis demonstrated that age at diagnosis (P<0.001;
68–78: P=0.041), N-stage (P<0.001), M-stage (P=0.003) and number
of removed lymph nodes (≥8 nodes: P=0.009) were significantly
associated with the OS of Chinese patients from the Shanghai Tenth
People's Hospital Urology database (Table III). The results from multivariate
Cox regression analysis demonstrated that only sex, T-stage and
M-stage were not associated with the OS in both American and
Chinese patients.
 | Table II.Univariate and multivariate Cox
regression analyses predicting the overall survival of patients
with bladder cancer from the SEER database. |
Table II.
Univariate and multivariate Cox
regression analyses predicting the overall survival of patients
with bladder cancer from the SEER database.
|
| Univariate Cox
regression | Multivariate Cox
regression |
|---|
|
|
|
|
|---|
| Characteristic | Hazard ratio (95%
CI) | P-value | Hazard ratio (95%
CI) | P-value |
|---|
| Age at diagnosis,
years |
|
|
|
|
|
<68 | Reference |
| Reference |
|
|
68-78 | 1.37
(1.31–1.43) | <0.001 | 1.39
(1.33–1.46) | <0.001 |
|
>78 | 2.09
(1.98–2.21) | <0.001 | 1.98
(1.87–2.09) | <0.001 |
| Sex |
|
|
|
|
|
Female | Reference |
| Reference |
|
|
Male | 0.88
(0.84–0.92) | <0.001 | – | 0.198 |
| Ethnicity |
|
|
|
|
|
White | Reference |
| Reference |
|
|
Black | 1.33
(1.23–1.44) | <0.001 | 1.24
(1.15–1.35) | <0.001 |
|
Other | 0.83
(0.750.92) | <0.001 | 0.81
(0.73–0.90) | <0.001 |
| Marital status |
|
|
|
|
|
Yes | Reference |
| Reference |
|
| No | 1.26
(1.21–1.31) | <0.001 | 1.19
(1.14–1.25) | <0.001 |
| SEER stage |
|
|
|
|
|
Localized | Reference |
| Reference |
|
|
Regional | 2.11
(1.96–2.28) | <0.001 | 1.47
(1.14–1.90) | 0.003 |
|
Distant | 6.34
(5.77–6.98) | <0.001 | 2.72
(2.09–3.54) | <0.001 |
| Grade |
|
|
|
|
| I | Reference |
| Reference |
|
| II | 1.48
(1.16–1.89) | 0.002 | 1.26
(0.99–1.67) | 0.065 |
|
III | 1.66
(1.32–2.09) | <0.001 | 1.38
(1.10–1.74) | 0.006 |
| IV | 1.48
(1.18–1.86) | 0.001 | 1.28
(1.01–1.61) | 0.038 |
|
Unknown | 1.28
(1.01–1.64) | 0.046 | 1.24
(0.97–1.59) | 0.084 |
| Histological
type |
|
|
|
|
|
Transitional cell
carcinoma | Reference |
| Reference |
|
|
Others | 1.37
(1.28–1.46) | <0.001 | 1.22
(1.14–1.31) | <0.001 |
|
T-stagea |
|
|
|
|
| Ta +
Tis | Reference |
| Reference |
|
| T1 | 1.02
(0.86–1.21) | 0.824 | 1.04
(0.87–1.25) | 0.646 |
| T2 | 1.30
(1.11–1.53) | 0.001 | 0.90
(0.66–1.22) | 0.488 |
| T3 | 2.84
(2.43–3.34) | <0.001 | 1.65
(1.22–2.24) | 0.001 |
| T4 | 4.25
(3.62–4.99) | <0.001 | 2.11
(1.56–2.85) | <0.001 |
|
N-stagea |
|
|
|
|
| N0 | Reference |
| Reference |
|
| N+ | 2.41
(2.30–2.51) | <0.001 | 1.85
(1.76–1.94) | <0.001 |
|
M-stagea |
|
|
|
|
| M0 | Reference |
| Reference |
|
| M1 | 3.12
(2.88–3.38) | <0.001 | – | 0.113 |
| Removed lymph
nodes, no. |
|
|
|
|
| ≤5 | Reference |
| Reference |
|
|
6-12 | 0.85
(0.80–0.90) | <0.001 | 0.72
(0.68–0.76) | <0.001 |
|
≥13 | 0.71
(0.68–0.75) | <0.001 | 0.62
(0.59–0.65) | <0.001 |
 | Table III.Univariate and multivariate Cox
regression analyses predicting the overall survival of patients
with bladder cancer from the Shanghai Tenth People's Hospital
Urology database. |
Table III.
Univariate and multivariate Cox
regression analyses predicting the overall survival of patients
with bladder cancer from the Shanghai Tenth People's Hospital
Urology database.
|
| Univariate Cox
regression | Multivariate Cox
regression |
|---|
|
|
|
|
|---|
| Characteristic | Hazard ratio (95%
CI) | P-value | Hazard ratio (95%
CI) | P-value |
|---|
| Age at diagnosis,
years |
|
|
|
|
|
<68 | Reference |
| Reference |
|
|
68-78 | 1.74
(1.02–2.96) | 0.041 | 1.25
(0.71–2.19) | 0.435 |
|
>78 | 3.04
(1.66–5.56) | <0.001 | 3.60
(1.84–7.05) | <0.001 |
| Sex |
|
|
|
|
|
Female | Reference |
| Reference |
|
|
Male | 0.85
(0.46–1.58) | 0.600 | – | 0.236 |
|
T-stagea |
|
|
|
|
| Ta +
Tis | Reference |
| Reference |
|
| T1 | 1.56
(0.21–11.73) | 0.669 | 1.05
(0.14–8.07) | 0.966 |
| T2 | 2.83
(0.37–21.93) | 0.320 | 1.77
(0.22–14.12) | 0.592 |
| T3 | 4.11
(0.55–30.91) | 0.170 | 2.96
(0.39–22.56) | 0.296 |
| T4 | 7.53
(1.02–55.56) | 0.048 | 4.74
(0.60–37.22) | 0.139 |
|
N-stagea |
|
|
|
|
| N0 | Reference |
| Reference |
|
| N+ | 3.39
(2.06–5.57) | <0.001 | 2.40
(1.33–4.35) | 0.004 |
|
M-stagea |
|
|
|
|
| M0 | Reference |
| Reference |
|
| M1 | 3.33
(1.52–7.28) | 0.003 | – | 0.591 |
| Removed lymph
nodes, no. |
|
|
|
|
| ≤1 | Reference |
| Reference |
|
|
2-7 | 0.73
(0.44–1.22) | 0.236 | 0.66
(0.39–1.13) | 0.131 |
| ≥8 | 0.36
(0.17–0.77) | 0.009 | 0.27
(0.12–0.62) | 0.002 |
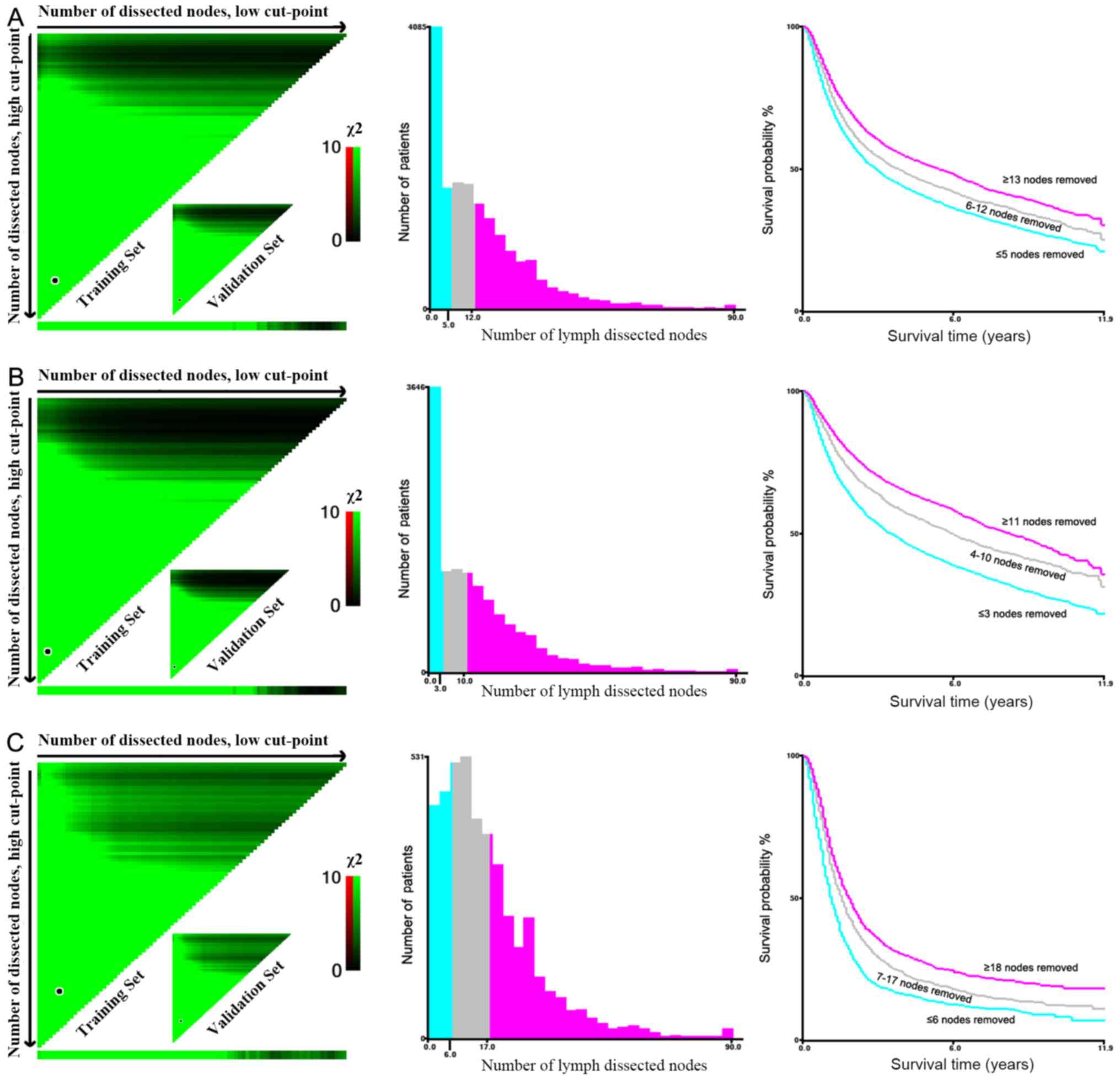
The number of LNDs was stratified using X-tile
software (21). The number of LNDs
in American patients from the SEER database was divided as follows:
≤5, 6–12 and ≥13 nodes (Fig. 2A).
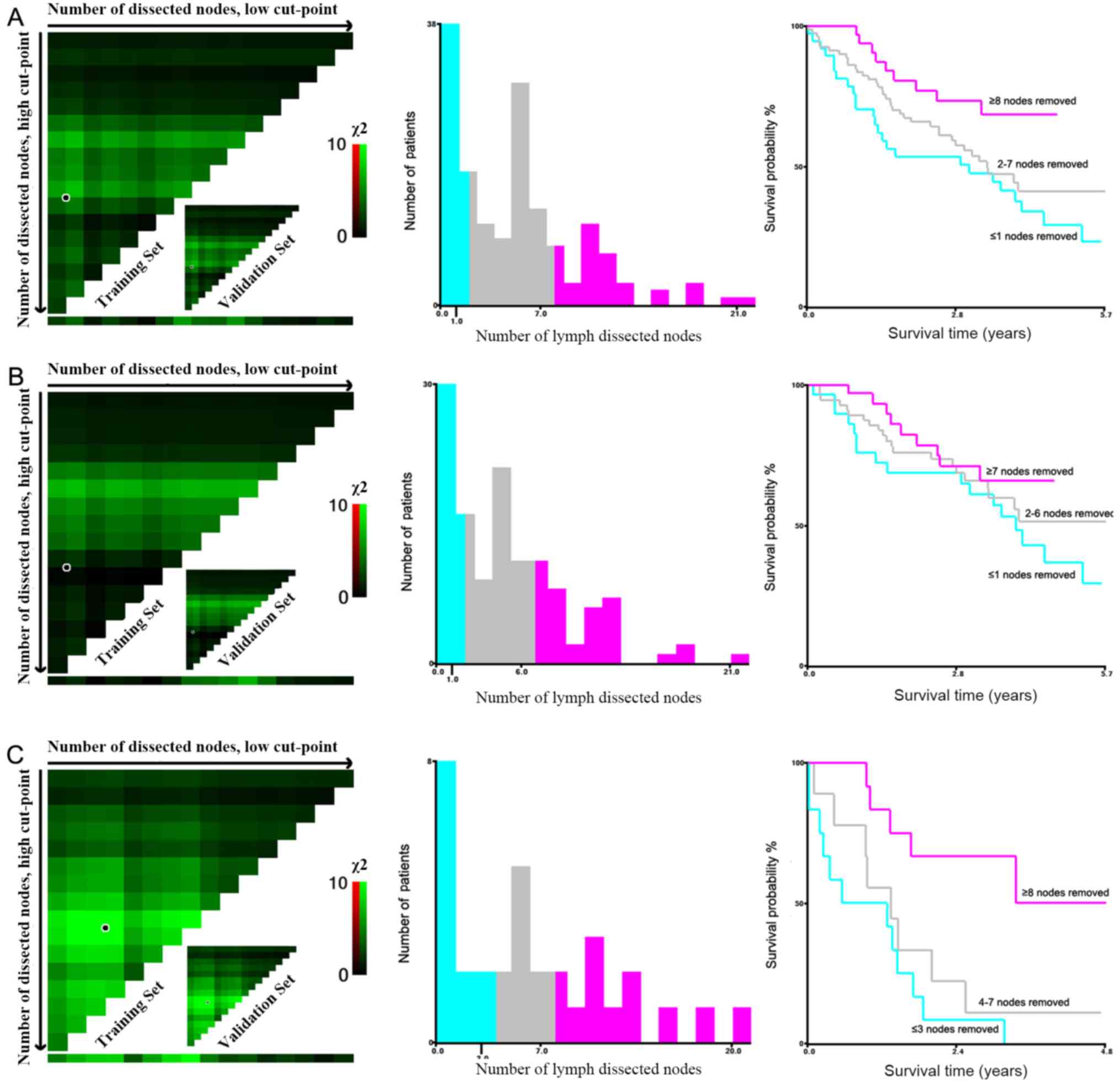
The number of LNDs in Chinese patients from the Shanghai Tenth
People's Hospital database was divided as follows: ≤1, 2–7 and ≥8
nodes (Fig. 3A). The number of LNDs
was also stratified according to patients with BCa patients with
different N stages. American patients with BCa with N0-stage was
classified as: ≤3, 4–10 and ≥11 nodes (Fig. 2B); the N+-stage patients as: ≤6, 7–17
and ≥18 nodes (Fig. 2C).
Simultaneously, the same stratified analysis was performed on data
from Chinese patients with BCa. Results were as follows: ≤1, 2–6
and ≥7 nodes for N0-stage (Fig. 3B);
≤3, 4–7 and ≥8 nodes for N+-stage (Fig.
3C).
The results from multivariate Cox regression
analysis demonstrated that the number of LNDs [6–12 vs. ≤5 nodes,
hazard ratio (HR) =0.72, 95% confidence interval (CI)=0.68–0.76;
P<0.001; ≥13 vs. ≤5 nodes, HR=0.62, 95% CI=0.59–0.65,
P<0.001] was significantly associated with the OS of American
patients from the SEER database (Table
II). The results from multivariate Cox regression analysis
demonstrated that the number of LNDs (≥8 vs. ≤1 nodes, HR=0.27, 95%
CI=0.12–0.62, P=0.002) was significantly associated with the OS of
Chinese patients from the Shanghai Tenth People's Hospital Urology
database (Table III). These
findings suggested that higher number of LNDs was a protective
factor for patients with BCa who underwent RC.
Effect of LND on the MST of patients
with BCa according to N-stage
Patients from the two aforementioned databases were
divided into two subgroups according to N-stage, namely N0 and N+.
The difference between the number of LNDs and the prognosis of
patients with BCa who underwent RC according to the N-stage
subgroup was evaluated (Table IV).
The number of LNDs in N0 and N+ patients was stratified using
X-tile software. The results demonstrated that LND [N0:4–10 vs. ≤3
nodes, HR=0.72, 95% CI=0.68–0.77, P<0.001; ≥11 vs. ≤3 nodes,
HR=0.58, 95% CI=0.54–0.61, P<0.001; N+:7–17 vs. ≤6 nodes,
HR=0.75, 95% CI=0.68–0.82, P<0.001; ≥18≤6 nodes, HR=0.62, 95%
CI=0.56–0.68, P<0.001] remained an independent prognostic factor
for the MST of American patients with BCa at different N-stages
(Table IV). Among N0 Chinese
patients, those in the ≥7 nodes group had increased MST compared
with that of patients in the ≤1 node group (43.0 vs. 30.5 months;
P=0.226; failed to calculate HR and 95% CI because there was no
difference in statistical analysis; Table IV). In addition, N+ Chinese patients
in the ≥8 nodes group had a longer MST compared with that of
patients in the ≤3 nodes group (23.5 vs. 10.5 months; HR=0.19, 95%
CI=0.07–0.56; P=0.003; Table IV).
Furthermore, regarding N0 American patients, those in the ≥11 nodes
group had a longer MST compared with that of patients in the ≤3
nodes group (MST, 34.0 vs. 27.0 months; HR=0.58, 95% CI=0.54–0.61;
P<0.001; Table IV). Among the
American N+ patients, those in the ≥18 nodes group had a longer MST
compared with that of patients in the ≤6 nodes group (MST, 17.0 vs.
12.0 months; HR=0.62, 95% CI=0.56–0.68; P<0.001; Table IV). For Chinese patients, only ≥8
nodes was significant for MST in N+-stage patients (HR=0.19, 95%
CI=0.07–0.56, P=0.003; Table IV).
In addition, the number of LNDs in each N-stage was generally
higher in American patients (Table
IV).
 | Table IV.Multivariate Cox regression analyses
for patients stratified by N-stage in the SEER and Shanghai Tenth
People's Hospital Urology databases. |
Table IV.
Multivariate Cox regression analyses
for patients stratified by N-stage in the SEER and Shanghai Tenth
People's Hospital Urology databases.
| A, SEER
database |
|---|
|
|---|
| Characteristic | MST, months | Hazard ratio (95%
CI) | P-value |
|---|
| N0a |
|
|
|
| Removed lymph
nodes, no. |
|
|
|
| ≤3 | 27.0 | Reference |
|
|
4-10 | 33.0 | 0.72
(0.68–0.77) | <0.001 |
|
≥11 | 34.0 | 0.58
(0.54–0.61) | <0.001 |
|
N+a |
|
|
|
| Removed lymph
nodes, no. |
|
|
|
| ≤6 | 12.0 | Reference |
|
|
7-17 | 15.0 | 0.75
(0.68–0.82) | <0.001 |
|
≥18 | 17.0 | 0.62
(0.56–0.68) | <0.001 |
|
| B, Shanghai
Tenth People's Hospital Urology database |
|
|
Characteristic | MST,
months | Hazard ratio
(95% CI) | P-value |
|
| N0a |
|
|
|
| Removed lymph
nodes, no. |
|
|
|
| ≤1 | 30.5 | Reference |
|
|
2-6 | 34.0 | – | 0.919 |
| ≥7 | 43.0 | – | 0.226 |
| N+a |
|
|
|
| Removed lymph
nodes, no. |
|
|
|
| ≤3 | 10.5 | Reference |
|
|
4-7 | 16.0 | 0.59
(0.24–1.48) | 0.262 |
| ≥8 | 23.5 | 0.19
(0.07–0.56) | 0.003 |
Discussion
The present study analyzed data from American and
Chinese patients with BCa, and demonstrated that LND was an
independent prognostic factor for OS. Furthermore, increased number
of LNDs was associated with increased survival time. These results
were similar to those from previous studies, which reported that
extended LND can increase the survival time of patients with BCa
who underwent RC, and reduce the recurrence rate (22,23).
Numerous studies reported these results in American patients
(24,25), although no comparison has been made
to date with Chinese patients.
At present, it is usual to divide the LND during RC
in patients with BCa into four grades according to the size of the
clearing scope as follows: Limited LND, standard LND, extended LND
and super-extended LND (15).
Previous studies reported that expanding the extent and number of
LNDs has a crucial impact on the prognostic significance, not only
for lymph node-positive patients but also for the postoperative
prognosis of lymph node-negative patients (26,27). In
addition, it was reported that LND might be an independent
prognostic factor for the prognosis of patients with BCa, since
extended LND can reduce micrometastasis (28). Dhar et al (29) demonstrated that patients with
extended LND have a higher lymph node positivity rate (extended
lymph node dissection (26%) vs. limited lymph node dissection
(13%). Abol-Enein et al (30)
demonstrated that the 5 year disease-free survival rate of patients
undergoing extended LND in a non-randomized prospective cohort
study was 66.6% (extended lymphadenectomy) vs. 54.7% (standard
lymphadenectomy). In addition, extended LND can also reduce the
probability of pelvic organ metastasis (27,31).
Although numerous studies reported this result, some controversies
exist. Gschwend et al (18)
demonstrated in a prospective randomized trial that extended LND
failed to present a significant advantage over limited LND
regarding the recurrence-free survival, cancer-specific survival
and OS of patients with BCa. Whether LND may be considered as an
independent prognostic factor for BCa remains unclear.
The present study analyzed data from 17,730 American
patients with BCa from the SEER database. For comparative analysis,
the clinical information of 158 Chinese patients with BCa was
collected from the center database of the Shanghai Tenth People's
Hospital. One experienced senior surgeon performed operation on all
Chinese patients in order to ensure reliable and convincing data,
and to avoid unreliable data deviations from different surgeons.
The result from this study demonstrated that N-stage may be
considered as a risk factor for the OS of both American and Chinese
patients. In addition, the OS of N+ patients was significantly
lower compared with that of N0 patients in the two populations. In
addition, the survival time was significantly prolonged as the
number of LNDs increased for different N-stage patients form the
two different populations.
In the present study, the results from multivariate
Cox regression analysis demonstrated that the number of LND was
correlated with patient's OS time and directly proportional to the
postoperative survival benefit. The increased number of LNDs
reduced the likelihood of potential lymph node metastases. This
increased the possibility of prolonged survival time after surgery.
In addition, the median number of LNDs in American patients was
significantly higher compared with that in Chinese patients (11.0
vs. 5.0 nodes). These findings suggested that the removal of a
larger quantity of lymph nodes increased the patients' survival.
These results were consistent with those from previous reports
(32,33). Furthermore, it has been reported that
extended LND can reduce the risk of recurrence and tumor burden
(34). Extended LND can provide
survival benefit in patients and facilitate the collection of other
prognostic information, including tumor burden, lymph node density
and lymph node extracapsular infiltration (9,10,17). The
present study also demonstrated that the number of LNDs in Chinese
patients was generally low compared with that in American patients.
It could therefore be recommended that surgeons expand the range of
LND in order to increase the number of LNDs during radical
resection in patients with BCa. This may increase the patients' OS
time and reduce the disease recurrence rate.
Stratified analysis demonstrated that, different LND
groups could achieve better survival benefits compared to ≤3 groups
(N0-stage) and ≤6 groups (N+stage) for American patients with
different N-stage (P<0.001). For Chinese patients, only the ≥8
nodes group had a longer MST compared with the ≤6 groups in N+stage
(P=0.003). The minimum number of LNDs according to data from the
Shanghai Tenth People's Hospital database was only 1 node. The
median LND for American patients was more than twice the median LND
for Chinese patients. In addition, the median LND in Chinese
patients was ≤6 nodes, which the number in SEER database analysis
presented a worse prognosis and a shorter OS time in American
patients. These observations may be due to the lack of universal
robot surgery in Shanghai Tenth People's Hospital and inaccurate
postoperative pathological lymph node count. The lack of awareness
by our institution (Department of Urology, Shanghai Tenth People's
Hospital) about the prognostic value of LND may explain these
results.
This study presented some limitations. Firstly, the
SEER database is a retrospective dataset with limitations inherent
to retrospective research, for example retrospective analysis is
prone to selection and recall bias (35). Moreover, the data from the SEER
database were collected by different cancer centers and, depending
on the statistician, there may be selection bias. Secondly, data
from Chinese patients were only collected from Shanghai Tenth
People's Hospital and may therefore not be representative of all
Chinese patients with BCa. Thirdly, information of only 158 Chinese
patients was collected, which is a small sample size. Further
multicenter prospective clinical trials are therefore required.
In conclusion, the present study demonstrated that
the number of LNDs was an independent prognostic factor for the
survival of patients with BCa. In addition, an increased number of
LNDs had a protective effect on the OS of patients with BCa.
Furthermore, the number of LNDs in Chinese patients was lower
compared with that in American patients. The number of LNDs should
therefore be increased when treating patients with BCa in
China.
Supplementary Material
Supporting Data
Acknowledgements
Not applicable.
Funding
This work was supported by the National Natural
Science Foundation of China (grant no. 81870517).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
KW, HS, WM and BP were involved in the study
conception and design. LY, WL and JX obtaining and performing
relevant statistical analysis from two databases . KW, GW and DF
were involved in data analysis and interpretation. KW and BP wrote
the manuscript.
Ethics approval and consent to
participate
The study protocol was approved by The Biomedical
Ethics Committee of the Tenth People's Hospital in Shanghai.
Written informed consent was obtained from the patients or their
next of kin if the patient did not have the ability to sign due to
lack of consciousness or physical difficulties. All authors read
and approved the final manuscript.
Patient consent for publication
Written informed consent was obtained from each
patient prior to publication.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Zhang ZF, Zhang HR, Zhang QY, Lai SY, Feng
YZ, Zhou Y, Zheng SR, Shi R and Zhou JY: High expression of TMEM40
is associated with the malignant behavior and tumorigenesis in
bladder cancer. J Transl Med. 16:92018. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Siegel RL, Miller KD and Jemal A: Cancer
statistics, 2018. CA Cancer J Clin. 68:7–30. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Czerniak B, Dinney C and McConkey D:
Origins of bladder cancer. Ann Rev Pathol. 11:149–174. 2016.
View Article : Google Scholar
|
|
4
|
Burger M, Catto JW, Dalbagni G, Grossman
HB, Herr H, Karakiewicz P, Kassouf W, Kiemeney LA, La Vecchia C,
Shariat S and Lotan Y: Epidemiology and risk factors of urothelial
bladder cancer. Eur Urol. 63:234–241. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Mao W, Huang X, Wang L, Zhang Z, Liu M, Li
Y, Luo M, Yao X, Fan J and Geng J: Circular RNA hsa_circ_0068871
regulates FGFR3 expression and activates STAT3 by targeting
miR-181a-5p to promote bladder cancer progression. J Exp Clin
Cancer Res. 38:1692019. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Babjuk M, Oosterlinck W, Sylvester R,
Kaasinen E, Böhle A and Palou-Redorta J; European Association of
Urology (EAU), : EAU guidelines on non-muscle-invasive urothelial
carcinoma of the bladder. Eur Urol. 54:303–314. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Gupta NP, Goel R, Hemal AK, Dogra PN, Seth
A, Aron M, Kumar R and Ansari MS: Radical cystectomy in
septuagenarian patients with bladder cancer. Int Urol Nephrol.
36:353–358. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Alfred Witjes J, Lebret T, Comperat EM,
Cowan NC, De Santis M, Bruins HM, Hernández V, Espinós EL, Dunn J,
Rouanne M, et al: Updated 2016 EAU guidelines on muscle-invasive
and metastatic bladder cancer. Eur Urol. 71:462–475. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Konety BR, Joslyn SA and O'Donnell MA:
Extent of pelvic lymphadenectomy and its impact on outcome in
patients diagnosed with bladder cancer: Analysis of data from the
surveillance, epidemiology and end results program data base. J
Urol. 169:946–950. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Siemens DR, Mackillop WJ, Peng Y, Wei X,
Berman D and Booth CM: Lymph node counts are valid indicators of
the quality of surgical care in bladder cancer: A population-based
study. Urol Oncol. 33:e415–e423. 2015. View Article : Google Scholar
|
|
11
|
May M, Herrmann E, Bolenz C, Tiemann A,
Brookman-May S, Fritsche HM, Burger M, Buchner A, Gratzke C,
Wülfing C, et al: Lymph node density affects cancer-specific
survival in patients with lymph node-positive urothelial bladder
cancer following radical cystectomy. Eur Urol. 59:712–718. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Herr H, Lee C, Chang S and Lerner S;
Bladder Cancer Collaborative G, : Standardization of radical
cystectomy and pelvic lymph node dissection for bladder cancer: A
collaborative group report. J Urol. 171:1823–1828. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Hedgepeth RC, Zhang Y, Skolarus TA and
Hollenbeck BK: Variation in use of lymph node dissection during
radical cystectomy for bladder cancer. Urology. 77:7720112011.
View Article : Google Scholar
|
|
14
|
Simone G, Papalia R, Ferriero M,
Guaglianone S, Castelli E, Collura D, Muto G and Gallucci M:
Stage-specific impact of extended versus standard pelvic lymph node
dissection in radical cystectomy. Int J Urol. 20:390–397. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Bruins HM, Veskimae E, Hernandez V,
Imamura M, Neuberger MM, Dahm P, Stewart F, Lam TB, N'Dow J, van
der Heijden AG, et al: The impact of the extent of lymphadenectomy
on oncologic outcomes in patients undergoing radical cystectomy for
bladder cancer: A systematic review. Eur Urol. 66:1065–1077. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Cole AP, Dalela D, Hanske J, Mullane SA,
Choueiri TK, Meyer CP, Nguyen PL, Menon M, Kibel AS, Preston MA, et
al: Temporal trends in receipt of adequate lymphadenectomy in
bladder cancer 1988 to 2010. Urol Oncol. 33:e509–e517. 2015.
View Article : Google Scholar
|
|
17
|
Maruf M, Sidana A, Purnell S, Jain AL,
Brancato SJ and Agarwal PK: Lymph node dissection during radical
cystectomy following prior radiation therapy: Results from the SEER
database. Int Urol Nephrol. 50:257–262. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Gschwend JE, Heck MM, Lehmann J, Rübben H,
Albers P, Wolff JM, Frohneberg D, de Geeter P, Heidenreich A,
Kälble T, et al: Extended versus limited lymph node dissection in
bladder cancer patients undergoing radical cystectomy: Survival
results from a prospective, randomized trial. Eur Urol. 75:604–611.
2019. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Mao W, Ma B, Huang X, Gu S, Luo M, Fan J
and Geng J: Which treatment is best for patients with AJCC stage IV
bladder cancer? Int Urol Nephrol. 51:1145–1156. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Compton CC, Byrd DR, Garciaaguilar J,
Kurtzman SH and Olawaiye A: AJCC Cancer Staging Atlas. Springer.
(Berlin). 2012. View Article : Google Scholar
|
|
21
|
Camp RL, Dolled-Filhart M and Rimm DL:
X-tile: A new bio-informatics tool for biomarker assessment and
outcome-based cut-point optimization. Clin Cancer Res.
10:7252–7259. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Leissner J, Hohenfellner R, Thuroff JW and
Wolf HK: Lymphadenectomy in patients with transitional cell
carcinoma of the urinary bladder; significance for staging and
prognosis. BJU Int. 85:817–823. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
von Landenberg N, Speed JM, Cole AP,
Seisen T, Lipsitz SR, Gild P, Menon M, Kibel AS, Roghmann F, Noldus
J, et al: Impact of adequate pelvic lymph node dissection on
overall survival after radical cystectomy: A stratified analysis by
clinical stage and receipt of neoadjuvant chemotherap. Urol Oncol.
36:e13–e78. 2018. View Article : Google Scholar
|
|
24
|
Stabile A, Muttin F, Zamboni S, Moschini
M, Gandaglia G, Fossati N, Dell'Oglio P, Capitanio U, Cucchiara V,
Mazzone E, et al: Therapeutic approaches for lymph node involvement
in prostate, bladder and kidney cancer. Expert Rev Anticancer Ther.
19:739–755. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Lee EK, Herr HW, Dickstein RJ, Kassouf W,
Munsell MF, Grossman HB, Dinney CP and Kamat AM: Lymph node density
for patient counselling about prognosis and for designing clinical
trials of adjuvant therapies after radical cystectomy. BJU Int.
110:E590–E595. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Sharma M, Goto T, Yang Z and Miyamoto H:
The impact of perivesical lymph node metastasis on clinical
outcomes of bladder cancer patients undergoing radical cystectomy.
BMC Urol. 19:772019. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Perera M, McGrath S, Sengupta S, Crozier
J, Bolton D and Lawrentschuk N: Pelvic lymph node dissection during
radical cystectomy for muscle-invasive bladder cancer. Nat Rev
Urol. 15:686–692. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Herr HW, Bochner BH, Dalbagni G, Donat SM,
Reuter VE and Bajorin DF: Impact of the number of lymph nodes
retrieved on outcome in patients with muscle invasive bladder
cancer. J Urol. 167:1295–1298. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Dhar NB, Klein EA, Reuther AM, Thalmann
GN, Madersbacher S and Studer UE: Outcome after radical cystectomy
with limited or extended pelvic lymph node dissection. J Urol.
179:873–878. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Abol-Enein H, Tilki D, Mosbah A, El-Baz M,
Shokeir A, Nabeeh A and Ghoneim MA: Does the extent of
lymphadenectomy in radical cystectomy for bladder cancer influence
disease-free survival? A prospective single-center study. Eur Urol.
60:572–577. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Poulsen AL, Horn T and Steven K: Radical
cystectomy: Extending the limits of pelvic lymph node dissection
improves survival for patients with bladder cancer confined to the
bladder wall. J Urol. 160:2015–2019. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Koppie TM, Vickers AJ, Vora K, Dalbagni G
and Bochner BH: Standardization of pelvic lymphadenectomy performed
at radical cystectomy: Can we establish a minimum number of lymph
nodes that should be removed? Cancer. 107:2368–2374. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Herr HW: Extent of surgery and pathology
evaluation has an impact on bladder cancer outcomes after radical
cystectomy. Urology. 61:105–108. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Masson-Lecomte A, Vordos D, Hoznek A, Yiou
R, Allory Y, Abbou CC, de la Taille A and Salomon L: External
validation of extranodal extension and lymph node density as
predictors of survival in node-positive bladder cancer after
radical cystectomy. Ann Surg Oncol. 20:1389–1394. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Crump K: The potential effects of recall
bias and selection bias on the epidemiological evidence for the
carcinogenicity of glyphosate. Risk Anal. 30:134402019.
|