Introduction
Acute myeloid leukemia (AML) is an aggressive
hematological malignancy with an incidence rate of 3.7 per 100,000
worldwide, and it is characterized by the clonal proliferation of
myeloid hematopoietic stem cells with the inhibition of normal
hematopoiesis (1). AML is a highly
heterogeneous disease in terms of clinical presentation,
cytogenetics/genetics and clinical outcome (1). Due to its considerable variability, it
is recommended that AML treatment should be more personalized and
precisely targeted based on the risk classifications of each
patient (2). At present, the
European LeukemiaNet risk classification is widely used in the
clinical management of AML; however, there is marked heterogeneity
among patients in clinical practice, particularly those in
intermediate groups in the classification system (2). Therefore, it is crucial to identify
novel potential prognostic and predictive biomarkers to improve our
understanding of leukemogenesis so that molecular-based
stratification can be applied to risk-adapted therapies and
ultimately improve the clinical outcome of AML.
Changes in lipid metabolism affect numerous cellular
processes that are relevant to cancer biology, including cell
proliferation, death, differentiation and motility (3). In the phosphatidylcholine biosynthesis
pathway, the conversion of lysophosphatidylcholine (LPC) to
phosphatidylcholine is catalyzed by cytosolic enzymes of the LPC
acyltransferase (LPCAT) family (4).
To date, LPCAT1, LPCAT2, LPCAT3 and LPCAT4 have been
identified and partially characterized as the four members of the
LPCAT family. A number of studies have demonstrated that the
overexpression of LPCAT1 is frequent in diverse human cancer
types, including prostate cancer (5,6), breast
cancer (7,8), gastric cancer (9), clear cell renal cell carcinoma
(10), lung cancer (11), hepatocellular carcinoma (12), oral squamous cell carcinoma (13) and colorectal cancer (14). Moreover, LPCAT1 overexpression
has been found to be associated with unfavorable pathological
characteristics and survival in several types of cancer (5–11).
However, the potential roles and clinical implications of LPCAT
family members in AML remain poorly investigated. Therefore, the
aim of the present study was to investigate the prognostic role of
the expression of LPCAT family members in AML, and to determine
whether this has the potential to be used as a new biomarker for
the diagnosis and prognosis of AML, and for the optimization of
clinical decision-making in the treatment of the disease.
Materials and methods
Patients
The first cohort included in the present study
comprised 173 patients with AML for whom LPCAT family
(LPCAT1/2/3/4) expression data were available from The
Cancer Genome Atlas (TCGA) database (TCGA-LAML, NEJM 2013)
(https://cancergenome.nih.gov/ and
http://www.cbioportal.org/) (15). The clinical and molecular
characteristics obtained for the cohort included age (median, 58
years; age range, 18–88 years), sex (81 male and 92 female), white
blood cell (WBC) counts, peripheral blood (PB) blasts, bone marrow
(BM) blasts, French-American-British (FAB) subtype, karyotype and
the frequencies of known common genetic mutations, as well as gene
expression levels. Due to the independent disease entity of
patients with FAB-M3, the non-M3 AML cohort was used in the
survival analysis. Following induction chemotherapy, 100 of the
patients received only chemotherapy as a consolidation treatment,
whereas 73 patients underwent hematopoietic stem cell
transplantation (HSCT) with/without chemotherapy as a consolidation
treatment. This cohort of patients with AML was used for the
identification of LPCAT family members whose expression was
associated with prognosis, and for the analysis of the clinical
implications of LPCAT1 expression.
A second cohort was also included, comprising 78
patients (median age, 62 years, age range 18–85 years) with
cytogenetically normal AML (CN-AML) from a Gene Expression Omnibus
(GEO) dataset (GSE12417) (16). The
online tool GenomicScape (http://genomicscape.com/microarray/survival.php) was
applied to validate the prognostic value of LPCAT1
expression among the patients with CN-AML in this cohort (17).
A third cohort, comprising 48 patients with AML (26
male and 22 female; median age, 60 years; age range, 18–82 years)
and 20 healthy volunteers (11 male and 9 female; median age, 56
years; age range, 18–71 years) from Jiangyin People's Hospital
(Jiangyin, China), was also enrolled in the present study. All the
patients with AML were treated at Jiangyin People's Hospital
between June 2015 and December 2018. The diagnosis of the patients
was based on the FAB and World Health Organization (WHO) criteria
(18,19). Patients with de novo AML
>18 years were included. Patients with antecedent hematological
diseases or therapy-associated AML were excluded. The study
protocol was approved by the Institutional Ethics Committee of
Jiangyin People's Hospital, and all the participants provided
written informed consent. This cohort of patients with AML was used
to validate the changes of LPCAT1 expression in patients
with AML.
Sample preparation, RNA isolation and
reverse transcription
PB samples were examined to identify the changes in
LPCAT1 expression that occur during the development of AML
since PB contains blasts, and the collection of BM samples from
patients with AML in the medical laboratory of Jiangyin People's
Hospital (Jiangyin, China) was challenging. PB samples were
collected from the 20 controls and the 48 patients with AML at
diagnosis, and from 15 of the patients with AML at complete
remission (CR). Nucleated cells were obtained from PB using red
blood cell lysis buffer (Beijing Solarbio Science & Technology
Co., Ltd.). Total RNA was extracted from the PB nucleated cells
using TRIzol® reagent (Invitrogen; Thermo Fisher
Scientific, Inc.). Reverse transcription was performed to
synthesize cDNA from the RNA using the PrimeScript™ RT reagent kit
(Takara Bio, Inc.) according to the manufacturer's
instructions.
Quantitative PCR (qPCR) analysis
qPCR analysis was conducted to detect LPCAT1
and GAPDH transcripts using TB Green Premix Ex Taq™ II
(Takara Bio, Inc.). The primers used were as follows: LPCAT1
forward, 5′-ACCTATTCCGAGCCATTGACC-3′ and reverse,
5′-CCTAATCCAGCTTCTTGCGAAC-3′; and GAPDH forward,
5′-AATCCCATCACCATCTTCCAG-3′ and reverse, 5′-GAGCCCCAGCCTTCTCCAT-3′.
GAPDH served as the reference gene. qPCR conditions were as
follows: 95°C for 30 sec, followed by 40 cycles of 95°C for 10 sec,
60°C for 1 min, 72°C for 1 min, and 80°C for 30 sec. The relative
LPCAT1 transcript level was calculated using on the
2−∆∆Cq method (20).
Statistical analysis
The Mann-Whitney U test or the Kruskal-Wallis test
followed by Dunn's post hoc test was used for the comparison of
continuous variables, and Pearson's χ2 or Fisher's exact
test were used for the comparison of categorical variables. The
effect of LPCAT1 expression on leukemia-free survival (LFS)
and overall survival (OS) was analyzed using the Kaplan-Meier
method with log-rank test, and Cox regression analysis. Two-tailed
P-values of <0.05 in all statistical analyses were considered to
indicate a statistically significant difference.
Results
Identification of prognosis-associated
LPCAT family member expression in AML
To investigate the prognostic value of LPCAT family
members in AML, expression data on all LPCAT family members
(LPCAT1/2/3/4) in AML were extracted from TCGA. The
prognostic value of LPCAT1/2/3/4 expression was investigated
following the division of the patients into two groups (lower and
higher) by the median level of LPCAT1/2/3/4 mRNA
(1161.1579/2249.6413/1218.6589/477.0187). The results of Cox
regression univariate analysis revealed that LPCAT1/2/3
expression was associated with OS in AML, and LPCAT3
expression was associated with LFS, whereas LPCAT1/2
expression showed a trend being associated with LFS (Table I). However, despite the well-known
prognostic factors (age, WBC and ELN risks) showing significant
associations, only LPCAT1 expression was identified as an
independent prognostic biomarker in AML by Cox regression
multivariate analysis, and exhibited a significant association with
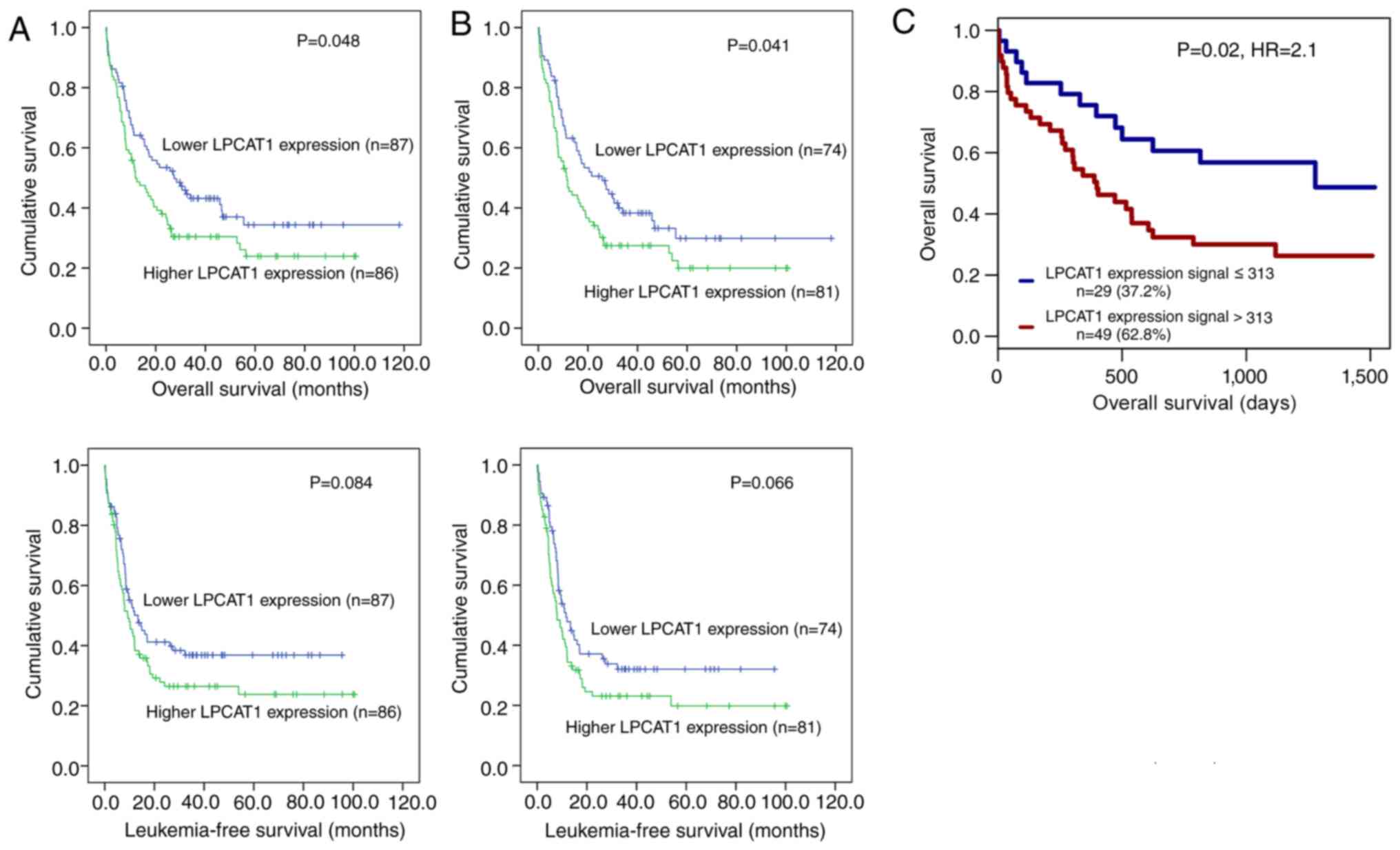
OS (Table I). Furthermore,
Kaplan-Meier analysis also demonstrated that patients with higher
expression levels of LPCAT1 exhibited significantly shorter
OS time compared with those with lower expression of LPCAT1
among total-AML and non-M3 AML cases, whereas a trend for LFS time
was observed which did not reach statistical significance (Fig. 1A and B).
 | Table I.Cox regression analysis of variables
for survival in patients with acute myeloid leukemia. |
Table I.
Cox regression analysis of variables
for survival in patients with acute myeloid leukemia.
| A, Overall
survival |
|---|
|
|---|
|
| Univariate
analysis | Multivariate
analysis |
|---|
|
|
|
|
|---|
| Variables | HR (95% CI) | P-value | HR (95% CI) | P-value |
|---|
| Age | 1.040
(1.027–1.054) | <0.001 | 1.042
(1.027–1.058) | <0.001 |
| WBC | 1.003
(0.999–1.006) | 0.119 | 1.007
(1.002–1.011) | 0.002 |
| ELN risks | 1.918
(1.519–2.423) | <0.001 | 1.935
(1.458–2.566) | <0.001 |
| LPCAT1
expression | 1.447
(1.000–2.095) | 0.050 | 1.467
(1.012–2.128) | 0.043 |
| LPCAT2
expression | 0.666
(0.460–0.964) | 0.031 | 0.924
(0.630–1.354) | 0.684 |
| LPCAT3
expression | 1.548
(1.069–2.240) | 0.021 | 1.704
(0.712–1.622) | 0.732 |
| LPCAT4
expression | 0.748
(0.516–1.084) | 0.125 | 1.060
(0.725–1.552) | 0.763 |
|
| B, Leukemia-free
survival |
|
|
| Univariate
analysis | Multivariate
analysis |
|
|
|
|
|
Variables | HR (95%
CI) | P-value | HR (95%
CI) | P-value |
|
| Age | 1.035
(1.022–1.048) | <0.001 | 1.037
(1.022–1.051) | <0.001 |
| WBC | 1.003
(1.000–1.006) | 0.091 | 1.007
(1.003–1.011) | 0.001 |
| ELN risks | 1.842
(1.466–2.315) | <0.001 | 1.831
(1.393–2.406) | <0.001 |
| LPCAT1
expression | 1.382
(0.955–1.999) | 0.086 | 1.422
(0.980–2.062) | 0.064 |
| LPCAT2
expression | 0.715
(0.495–1.034) | 0.075 | 0.979
(0.666–1.439) | 0.915 |
| LPCAT3
expression | 1.536
(1.062–2.223) | 0. 023 | 1.130
(0.753–1.695) | 0.556 |
| LPCAT4
expression | 0.738
(0.509–1.071) | 0.110 | 1.028
(0.704–1.501) | 0.887 |
Validation of the association of
LPCAT1 expression with prognosis in AML
To validate the prognostic value of LPCAT1
expression in AML, GEO data (GSE12417) on 78 patients with CN-AML
were analyzed using the online web tool GenomicScape. Kaplan-Meier
analysis revealed that the patients with higher expression levels
of LPCAT1 presented significantly shorter OS times compared
with those with lower expression levels of LPCAT1 (Fig. 1C).
Validation of LPCAT1 overexpression in
newly diagnosed cases of AML
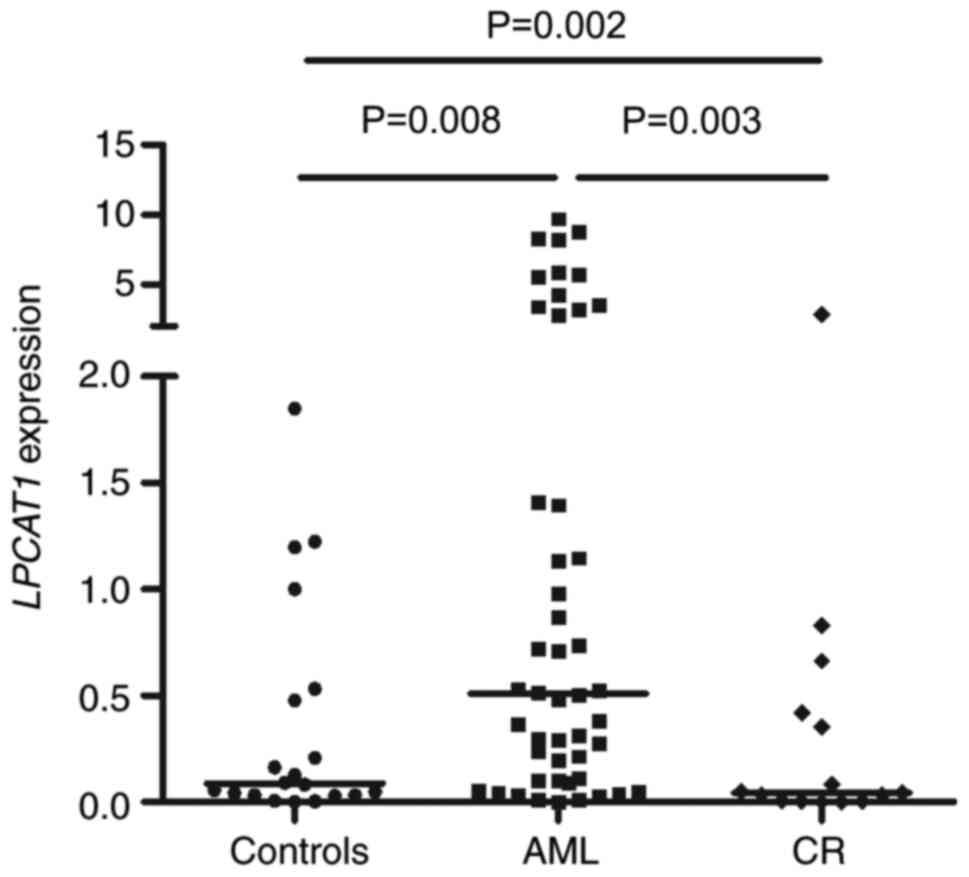
In order to further explore the expression of
LPCAT1 in AML, the mRNA levels of LPCAT1 in patients
newly diagnosed with AML were further examined. According to the
RT-qPCR results for the third cohort, LPCAT1 expression was
significantly increased in patients with newly diagnosed AML
compared with that in normal controls (Fig. 2). Furthermore, LPCAT1
expression levels in patients with AML at CR were significantly
lower compared with those in patients with newly diagnosed AML
(Fig. 2).
Clinical implications of LPCAT1
expression in AML
Due the significant prognostic value of
LPCAT1 expression in AML, the associations of LPCAT1
expression with the clinical and biological characteristics of
patients were further investigated, based on TCGA data. As shown in
Table II, no significant
differences were identified between patients with lower and higher
levels of LPCAT1 expression in terms of sex, age, WBC count
and BM blasts (P>0.05). However, patients with higher expression
of LPCAT1 exhibited lower numbers of PB blasts compared with
patients with lower expression of LPCAT1 (P=0.001).
Moreover, significant differences were detected between the two
groups regarding the distribution of FAB classification subtypes
and cytogenetic features (P<0.001 and P=0.033, respectively).
Patients with higher expression of LPCAT1 were frequently
classified as FAB-M4/M5 (P=0.002 and P<0.001, respectively) and
less frequently as FAB-M3 or t(15;17) (P=0.063 and P=0.028,
respectively). In addition, associations of LPCAT1
expression with common gene expression and mutations in AML were
also observed (Table II). Higher
LPCAT1 expression was associated with nucleophosmin 1
(NPM1) mutation, isocitrate dehydrogenase 1 (IDH1)
wild-type and CCAAT/enhancer-binding protein α (CEBPA)
wild-type (P=0.018, P=0.063 and P=0.080, respectively). Moreover,
LPCAT1 expression was further compared between patients with
and without NPM1, IDH1, CEBPA and TP53 gene
mutations, and the differences between the wild-type and mutant
groups were observed to be statistically significant for all four
genes (Fig. 3).
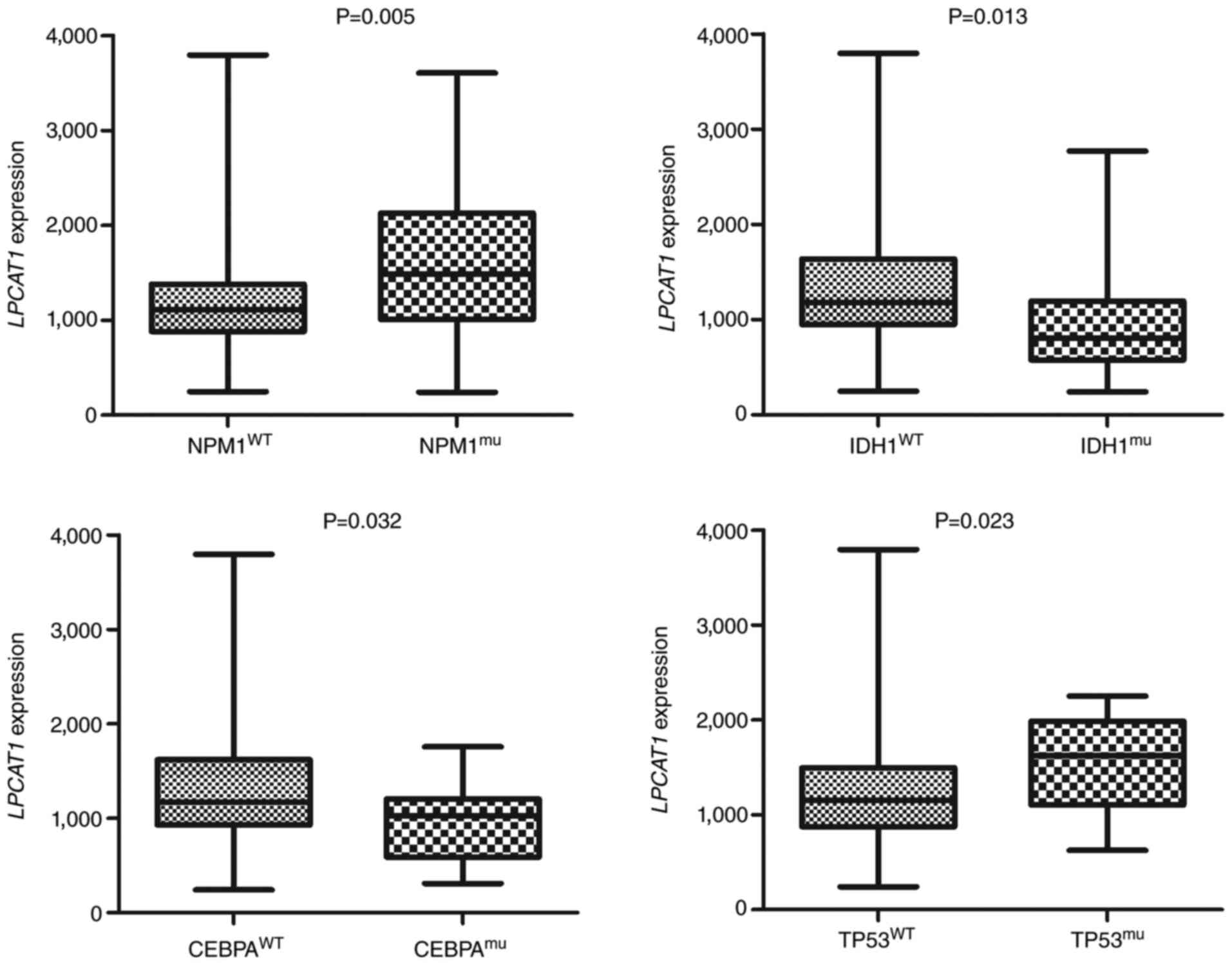 | Figure 3.Associations of LPCAT1
expression with gene mutations in AML. Data on patients with AML
are derived from TCGA database (TCGA-LAML, NEJM 2013) (15). LPCAT1 expression in AML
patients with and without NPM1, IDH1, CEBPA and TP53
mutations. LPCAT1, lysophosphatidylcholine acyltransferase
1; AML, acute myeloid leukemia; NPM1, nucleophosmin 1;
IDH1, isocitrate dehydrogenase 1; CEBPA,
CCAAT/enhancer-binding protein α; TCGA, The Cancer Genome Atlas;
WT, wild-type; mu, mutant. |
 | Table II.Association of LPCAT1
expression with clinicopathological characteristics in patients
with acute myeloid leukemia. |
Table II.
Association of LPCAT1
expression with clinicopathological characteristics in patients
with acute myeloid leukemia.
|
| LPCAT1
expression |
|
|---|
|
|
|
|
|---|
| Parameters | Low (n=87) | High (n=86) | P-value |
|---|
| Sex,
male/female | 42/45 | 39/47 | 0.761 |
| Age, median
(range), years | 57 (18–82) | 58.5 (22–88) | 0.311 |
| Median WBC count
(range), ×109/l | 18.7
(0.5–297.4) | 15.6
(0.4–137.2) | 0.808 |
| Median PB blasts
(range), % | 50 (0–98) | 18 (0–94) | 0.001 |
| Median BM blasts
(range), % | 72 (30–99) | 73 (30–100) | 0.449 |
| FAB classification,
n |
|
| <0.001 |
| M0 | 12 | 4 | 0.063 |
| M1 | 26 | 18 | 0.222 |
| M2 | 23 | 15 | 0.199 |
| M3 | 12 | 4 | 0.063 |
| M4 | 9 | 25 | 0.002 |
| M5 | 2 | 16 | <0.001 |
| M6 | 1 | 1 | 1.000 |
| M7 | 1 | 2 | 0.621 |
| No
data | 1 | 1 | 1.000 |
| Cytogenetics,
n |
|
| 0.033 |
|
Normal | 39 | 41 | 0.761 |
|
t(15;17) | 12 | 3 | 0.028 |
|
t(8;21) | 2 | 5 | 0.278 |
|
inv(16) | 5 | 5 | 1.000 |
| +8 | 6 | 2 | 0.278 |
|
del(5) | 0 | 1 | 0.497 |
|
−7/del(7) | 6 | 1 | 0.117 |
|
11q23 | 0 | 3 | 0.121 |
|
Others | 5 | 9 | 0.280 |
|
Complex | 10 | 15 | 0.288 |
| No
data | 2 | 1 | 1.000 |
| Gene mutation,
n |
|
|
|
|
FLT3 (+/+) | 20/67 | 29/57 | 0.131 |
|
NPM1 (+/+) | 17/70 | 31/55 | 0.018 |
|
DNMT3A (+/+) | 18/69 | 24/62 | 0.292 |
|
IDH2 (+/+) | 12/75 |
5/81 | 0.124 |
|
IDH1 (+/+) | 12/75 |
4/82 | 0.063 |
|
TET2 (+/+) | 10/77 |
5/81 | 0.280 |
|
RUNX1 (+/+) |
9/78 |
6/80 | 0.590 |
|
TP53 (+/+) |
4/83 | 10/76 | 0.103 |
|
NRAS (+/+) |
3/84 |
8/78 | 0.132 |
|
CEBPA (+/+) | 10/77 |
3/83 | 0.080 |
|
WT1 (+/+) |
7/80 |
3/83 | 0.329 |
|
PTPN11 (+/+) |
3/84 |
5/81 | 0.496 |
|
KIT (+/+) |
3/84 |
4/82 | 0.720 |
|
U2AF1 (+/+) |
4/83 |
3/83 | 1.000 |
|
KRAS (+/+) |
3/84 |
4/82 | 0.720 |
|
SMC1A (+/+) |
3/84 |
4/82 | 0.720 |
|
SMC3 (+/+) |
2/85 |
5/81 | 0.278 |
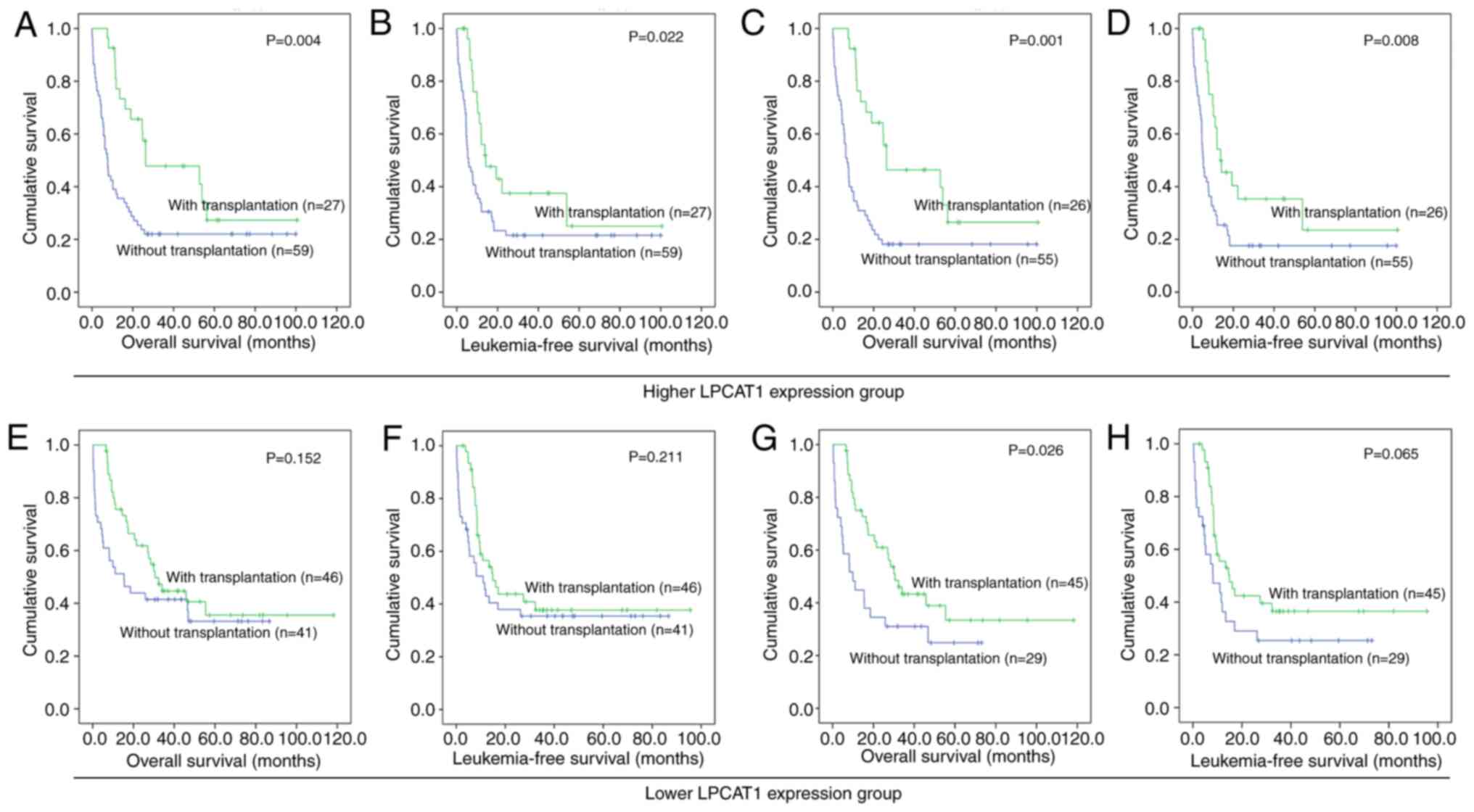
Patients with AML and higher LPCAT1
expression may benefit from HSCT
To investigate whether HSCT is able to overcome the
adverse outcomes associated with higher expression of
LPCAT1, the survival times of patients who had or had not
received HSCT after induction chemotherapy were compared in the
lower and higher LPCAT1 expression groups. In the higher
LPCAT1 expression group, the patients who had undergone HSCT
following induction therapy exhibited significantly longer OS and
LFS times compared with those who only received chemotherapy after
induction therapy in both total-AML and non-M3-AML cases (Fig. 4A-D). In the lower LPCAT1
expression group, no significant differences were observed in OS
and LFS between patients who had undergone HSCT and those who had
not among total-AML and only in LFS among non-M3-AML cases
(Fig. 4E-H). These results suggest
that patients with AML and higher LPCAT1 expression may
benefit from HSCT, and LPCAT1 expression may guide the
decision of whether to select HSCT or chemotherapy as an
appropriate treatment for patients with AML after induction
therapy.
Discussion
Studies have demonstrated the biological role of
LPCAT1 in diverse human cancer types. For example, Morita
et al (12) reported that the
overexpression of LPCAT1 promoted the proliferation,
migration and invasion of hepatocellular carcinoma cells. In
addition, in oral squamous cell carcinoma cell lines, the knockdown
of LPCAT1 resulted in decreased cellular proliferation,
invasiveness and migration, as well as decreased intercellular
platelet-activating factor (PAF) concentration and PAF receptor
expression (13). Furthermore, Du
et al (10) revealed that
LPCAT1-knockdown in clear cell renal cell carcinoma
inhibited cell proliferation, migration and invasion, and induced
cell cycle arrest at the G0/G1 phase.
Moreover, short hairpin RNA-mediated LPCAT1 silencing in
lung adenocarcinoma not only abrogated cell proliferation,
migration and invasion in vitro, but also arrested tumor
growth and brain metastases in vivo (11). Mechanically, LPCAT1
dysregulation has been shown to at least partially affect the
progression of lung adenocarcinoma through the PI3K/AKT signaling
pathway via the targeting of MYC transcription (11). However, studies investigating the
direct role of LPCAT1 in AML are lacking. Therefore, further
functional and clinical studies are required to investigate the
potential role of LPCAT1 during leukemogenesis in AML.
The present study investigated the clinical
implications of the expression of LPCAT family members in AML, and
demonstrated that LPCAT1 expression is significantly
associated with the survival of patients with AML. In addition, the
present study indicated that LPCAT1 expression may act as a
potential biomarker to guide the choice between HSCT and
chemotherapy for the further treatment of patients with AML after
induction therapy. These results emphasize the potential of
LPCAT1 expression as a valuable indicator for the clinical
management of AML. Although this is, to the best of our knowledge,
the first study to report the clinical significance of
LPCAT1 expression in AML, a number of studies have
demonstrated the prognostic role of LPCAT1 expression in
numerous solid tumors. For example, Zhou et al (5) reported that LPCAT1 expression
was associated with the progression of prostate cancer
independently of patient ethnicity and age, prostate-specific
antigen level and the positivity of surgical resection margins, and
suggested that it may be a novel biomarker for the diagnosis and
prognosis of prostate cancer, as well as for studying its
pathogenesis. Furthermore, Grupp et al (6) demonstrated that high LPCAT1
expression independently predicted a high risk of biochemical
recurrence in prostate cancer. In breast cancer, LPCAT1
expression has been shown to be significantly associated with tumor
grade and TNM stage, as well as increased proliferative activity,
negative estrogen receptor status, negative progesterone receptor
status, positive human epidermal growth factor receptor 2 status,
and deletions of phosphatase and tensin homolog and
cyclin-dependent kinase inhibitor 2A (7,8), with
multivariate analysis revealing that upregulated LPCAT1
expression is an independent predictor of early tumor recurrence in
breast cancer (8). Uehara et
al (9) reported that
LPCAT1 expression was positively associated with tumor
differentiation and negatively associated with the depth of tumor
invasion, lymph node metastasis and tumor stage in gastric cancer.
In addition, Du et al (10)
revealed that LPCAT1 expression was significantly associated
with higher tumor grade, higher TNM stage, larger tumor size and
shorter OS time in clear cell renal cell carcinoma. Moreover,
LPCAT1 expression was found to negatively impact prognosis
in lung adenocarcinoma (11). Thus,
it may be inferred that LPCAT1 expression plays a key role
in AML and in the treatment response following HSCT. However, the
associations between LPCAT1 expression and AML biology
require further investigation.
The NPM1 gene encodes a multifunctional
protein that shuttles between the nucleus and cytoplasm, and has
prominent nucleolar localization. NPM1 mutations are common
in AML and comprise a unique subtype in the 2016 WHO classification
of hematopoietic neoplasms (19).
NPM1 mutations represent the most common genetic lesion in
adult AML and cause the aberrant cytoplasmic delocalization of
NPM1 mutants. NPM1 mutants have been demonstrated to
maintain the leukemic state through homeobox gene overexpression
(21). The present study identified
a link between LPCAT1 and NPM1 mutations in patients
with AML. However, the exact association between LPCAT1
expression and NPM1 mutations remains poorly defined.
Further studies are required to determine the potential mechanism
by which the overexpression of LPCAT1 contributes to the
leukemogenesis caused by NPM1 mutations.
In conclusion, the findings of the present study
indicate that LPCAT1 expression may serve as an independent
prognostic biomarker to guide the treatment choice between HSCT and
chemotherapy in patients with AML.
Acknowledgements
Not applicable.
Funding
This study was supported by Scientific Research
Projects from the Wuxi Commission of Health and Family Planning
(grant no. MS201642).
Availability of data and materials
TCGA database (TCGA-LAML, NEJM 2013; https://cancergenome.nih.gov/ and http://www.cbioportal.org/) and GEO (GSE12417) data
are available online. The other datasets used and/or analyzed
during the current study are available from the corresponding
author on reasonable request.
Authors' contributions
JL conceived and designed the study. KW, ZW and YS
analyzed the data. WT, XX and YC performed the experiments; KW and
JL wrote the paper. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
All procedures performed in the study were approved
by the Ethics Committee of Jiangyin People's Hospital and complied
with the 1964 Declaration of Helsinki and its later amendments or
comparable ethical standards. Informed consent was obtained from
all patients included in this study.
Patient consent for publication
Not applicable.
References
|
1
|
Estey E and Döhner H: Acute myeloid
leukaemia. Lancet. 368:1894–1907. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Döhner H, Estey E, Grimwade D, Amadori S,
Appelbaum FR, Büchner T, Dombret H, Ebert BL, Fenaux P, Larson RA,
et al: Diagnosis and management of AML in adults: 2017 ELN
recommendations from an international expert panel. Blood.
129:424–447. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Santos CR and Schulze A: Lipid metabolism
in cancer. FEBS J. 279:2610–2623. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Law SH, Chan ML, Marathe GK, Parveen F,
Chen CH and Ke LY: An updated review of lysophosphatidylcholine
metabolism in human diseases. Int J Mol Sci. 20:11492019.
View Article : Google Scholar
|
|
5
|
Zhou X, Lawrence TJ, He Z, Pound CR, Mao J
and Bigler SA: The expression level of lysophosphatidylcholine
acyltransferase 1 (LPCAT1) correlates to the progression of
prostate cancer. Exp Mol Pathol. 92:105–110. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Grupp K, Sanader S, Sirma H, Simon R, Koop
C, Prien K, Hube-Magg C, Salomon G, Graefen M, Heinzer H, et al:
High lysophosphatidylcholine acyltransferase 1 expression
independently predicts high risk for biochemical recurrence in
prostate cancers. Mol Oncol. 7:1001–1011. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Lebok P, von Hassel A, Meiners J,
Hube-Magg C, Simon R, Höflmayer D, Hinsch A, Dum D, Fraune C, Göbel
C, et al: Up-regulation of lysophosphatidylcholine acyltransferase
1 (LPCAT1) is linked to poor prognosis in breast cancer. Aging
(Albany NY). 11:7796–7804. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Abdelzaher E and Mostafa MF:
Lysophosphatidylcholine acyltransferase 1 (LPCAT1) upregulation in
breast carcinoma contributes to tumor progression and predicts
early tumor recurrence. Tumour Biol. 36:5473–5483. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Uehara T, Kikuchi H, Miyazaki S, Iino I,
Setoguchi T, Hiramatsu Y, Ohta M, Kamiya K, Morita Y, Tanaka H, et
al: Overexpression of lysophosphatidylcholine acyltransferase 1 and
concomitant lipid alterations in gastric cancer. Ann Surg Oncol. 23
(Suppl 2):S206–S213. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Du Y, Wang Q, Zhang X, Wang X, Qin C,
Sheng Z, Yin H, Jiang C, Li J and Xu T: Lysophosphatidylcholine
acyltransferase 1 upregulation and concomitant phospholipid
alterations in clear cell renal cell carcinoma. J Exp Clin Cancer
Res. 36:662017. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Wei C and Dong X, Lu H, Tong F, Chen L,
Zhang R, Dong J, Hu Y, Wu G and Dong X: LPCAT1 promotes brain
metastasis of lung adenocarcinoma by up-regulating PI3K/AKT/MYC
pathway. J Exp Clin Cancer Res. 38:952019. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Morita Y, Sakaguchi T, Ikegami K,
Goto-Inoue N, Hayasaka T, Hang VT, Tanaka H, Harada T, Shibasaki Y,
Suzuki A, et al: Lysophosphatidylcholine acyltransferase 1 altered
phospholipid composition and regulated hepatoma progression. J
Hepatol. 59:292–299. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Shida-Sakazume T, Endo-Sakamoto Y, Unozawa
M, Fukumoto C, Shimada K, Kasamatsu A, Ogawara K, Yokoe H, Shiiba
M, Tanzawa H and Uzawa K: Lysophosphatidylcholine acyltransferase1
overexpression promotes oral squamous cell carcinoma progression
via enhanced biosynthesis of platelet-activating factor. PLoS One.
10:e01201432015. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Mansilla F, da Costa KA, Wang S, Kruhøffer
M, Lewin TM, Orntoft TF, Coleman RA and Birkenkamp-Demtröder K:
Lysophosphatidylcholine acyltransferase 1 (LPCAT1) overexpression
in human colorectal cancer. J Mol Med (Berl). 87:85–97. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Cancer Genome Atlas Research Network, ;
Ley TJ, Miller C, Ding L, Raphael BJ, Mungall AJ, Robertson A,
Hoadley K, Triche TJ Jr, Laird PW, et al: Genomic and epigenomic
landscapes of adult de novo acute myeloid leukemia. N Engl J Med.
368:2059–2074. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Metzeler KH, Hummel M, Bloomfield CD,
Spiekermann K, Braess J, Sauerland MC, Heinecke A, Radmacher M,
Marcucci G, Whitman SP, et al: An 86-probe-set gene-expression
signature predicts survival in cytogenetically normal acute myeloid
leukemia. Blood. 112:4193–4201. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Kassambara A, Rème T, Jourdan M, Fest T,
Hose D, Tarte K and Klein B: GenomicScape: An easy-to-use web tool
for gene expression data analysis. Application to investigate the
molecular events in the differentiation of B cells into plasma
cells. PLoS Comput Biol. 11:e10040772015. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Bennett JM, Catovsky D, Daniel MT,
Flandrin G, Galton DA, Gralnick HR and Sultan C: Proposed revised
criteria for the classification of acute myeloid leukaemia. A
report of the French-American-British Cooperative Group. Ann Intern
Med. 103:620–625. 1985. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Arber DA, Orazi A, Hasserjian R, Thiele J,
Borowitz MJ, Le Beau MM, Bloomfield CD, Cazzola M and Vardiman JW:
The 2016 revision to the World Health Organization classification
of myeloid neoplasms and acute leukemia. Blood. 127:2391–2405.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T))method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Falini B, Brunetti L, Sportoletti P and
Martelli MP: NPM1-mutated acute myeloid leukemia: From bench to
bedside. Blood. 136:1707–1721. 2020. View Article : Google Scholar : PubMed/NCBI
|