Introduction
Capmatinib is an anticancer medication used to treat
certain types of cancer, particularly non-small cell lung cancer
(NSCLC) involving a mesenchymal-epithelial transition (MET) exon 14
skipping mutation (1). This
mutation leads to overexpression of the MET receptor tyrosine
kinase, which is a protein that is involved in a number of
important cellular processes, including cell growth, survival and
migration, and also promotes the formation of epithelial cells from
mesenchymal cells (2). Capmatinib
targets NSCLC tumors by inhibiting overactivity of c-Met and
blocking tumor growth, and the results of a Phase Ib/II clinical
trial previously reported that capmatinib has a high objective
response rate in patients with MET exon 14 skipping NSCLC (3). Although capmatinib has demonstrated
efficacy in treating NSCLC, side effects of this treatment have
been reported. Common side effects include peripheral edema, nausea
and a decreased appetite (3). A
rare and potentially life-threatening side effect associated with
capmatinib treatment is the development of interstitial lung
disease (ILD). ILD is a broad term that describes a group of lung
disorders that cause inflammation and scarring of the lung tissue,
leading to breathing difficulties, coughing and fever (4). ILD can be caused by a variety of
factors, such as exposure to environmental toxins and certain
medications, including capmatinib (5). However, the incidence of
capmatinib-induced ILD is low, with the few case reports that have
been published all showing successful treatment with
corticosteroids (6–8). However, given the potentially serious
nature of this side effect, healthcare providers should be aware of
this risk and closely monitor patients receiving capmatinib for
signs or symptoms of ILD. Early recognition of the signs or
symptoms of ILD, discontinuation of capmatinib treatment and the
prompt initiation of corticosteroids have been reported to lead to
complete resolution of ILD (4).
Case report
A 50-year-old man with a history of hypertension and
a past history of smoking presented to Far Eastern Memorial
Hospital (New Taipei City, Taiwan) in March 2018 with the chief
complaint of coughing that had persisted for 2 months. The patient
smoked one pack of cigarettes/day for 2 years, before quitting
smoking 25 years prior to hospital admission. A chest X-ray showed
a right upper lobe mass of 3.3 cm and subsequent chest computed
tomography (CT) showed multiple nodules, with the largest measuring
3.3 cm in the right upper lobe. The patient was subsequently
diagnosed with adenocarcinoma after a CT-guided biopsy in April
2018. The patient underwent a right upper lobe video-assisted
thoracoscopic surgery lobectomy with radical lymph node dissection
and was diagnosed with pathological stage IB T2aN0M0 (9) adenocarcinoma according to the 8th
edition American Joint Committee on Cancer Tumor-Node-Metastasis
system, with no mutation of EGFR, anaplastic lymphoma kinase (ALK)
or ROS proto-oncogene 1, receptor tyrosine kinase (ROS-1). Due to
the healthcare insurance system in Taiwan, following surgical
resection of early stage lung cancer, genetic testing was limited
to individual testing of commonly observed genes. Adjuvant
chemotherapy with Ufur (tegafur, 100 mg; uracil, 224 mg) twice
daily was administered to the patient between September 2018 and
August 2019, without any evidence of recurrence of the disease.
Further CT scans performed in May and November 2020 demonstrated
stable disease with no recurrence observed.
However, in May 2021, the patient developed
progressive disease with right-sided pleural effusion and small
nodules in the left lower lobe. Analysis of the malignant pleural
effusion revealed persistent adenocarcinoma via cytology and cell
block: Samples were fixed in 10% formalin at 25°C for 24 h and
sliced into 4- to 5-µm thick sections. Hematoxylin and eosin
staining was applied at 25°C, with hematoxylin used for 1–2 min and
eosin for 30 sec. A light field microscope was used to visualize
the results. There were no mutations of EGFR, ALK or ROS-1,
although the patient was now programmed cell death-ligand 1
(PD-L1)-positive, with a tumor proportion score of ≥50%. The
patient received 500 mg pemetrexed and 75 mg cis-platinum
(per m2 body surface area, every 3 weeks, in an infusion
for 6 cycles) between June 2021 and October 2021, followed by
nivolumab between November 2021 and September 2022. The patient
then presented with left-sided weakness, slurred speech and an
imbalanced gait for 1 week in October 2022. A brain CT showed right
temporal, left frontal and left cerebellar metastasis, with a
midline shift towards the left side of ~13 mm. The patient
underwent a right temporal craniotomy for right temporal tumor
excision in October 2022, followed by stereotactic body radiation
therapy, with a total of 2,500 cGy administered in five fractions.
The pathology of the brain tumor demonstrated metastatic carcinoma
and the results of ACTDrug®+ next-generation
sequencing-based assay (performed by ACT Genomics, Co. Ltd.)
demonstrated the presence of the MET exon 14 skipping mutation. The
patient was then prescribed capmatinib (200 mg/three times daily)
in November 2022.
The patient was again admitted to hospital in
January 2023 due to progressive dyspnea, and treatment with
capmatinib was maintained up to January 2023. A chest X-ray showed
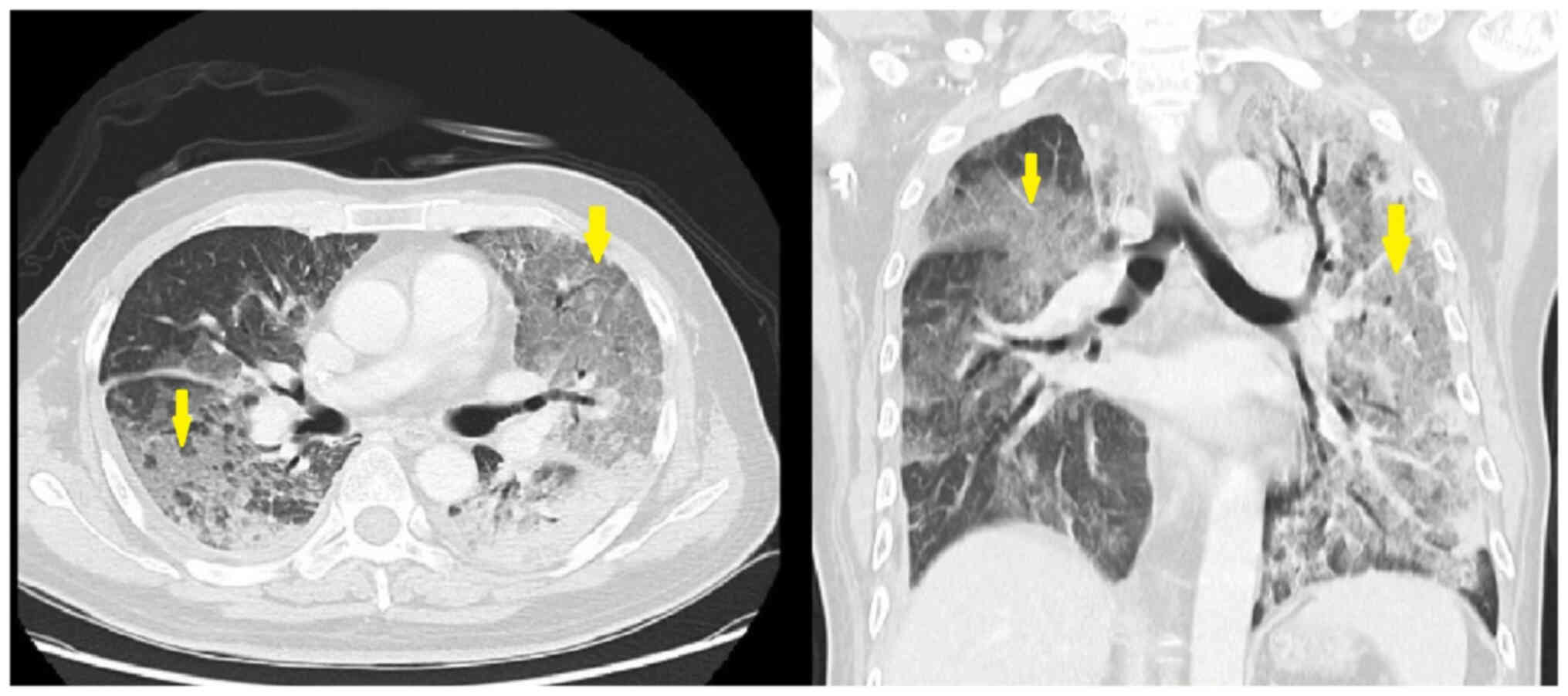
bilateral infiltrations. Chest CT scan images showed extensive
ground-glass opacity in both lungs and subpleural consolidation,
which led to a suspected diagnosis of drug-induced ILD and
pneumonia (Fig. 1). The patient was
tested for influenza A and B, coronavirus disease 2019, and
Legionella and Mycoplasma antibodies, which are
potential causes of ILD and were common tests conducted in Taiwan
in 2021; however, these tests were negative. Systemic steroids
consisting of 120 mg methylprednisolone per day and antibiotics
consisting of 750 mg levofloxacin per day were then prescribed and
the patient's oxygenation status improved. The follow-up chest
X-ray also showed improvement of the bilateral infiltrations.
Antibiotics were discontinued and systemic steroids were gradually
titrated until the patient was only receiving oral prednisolone.
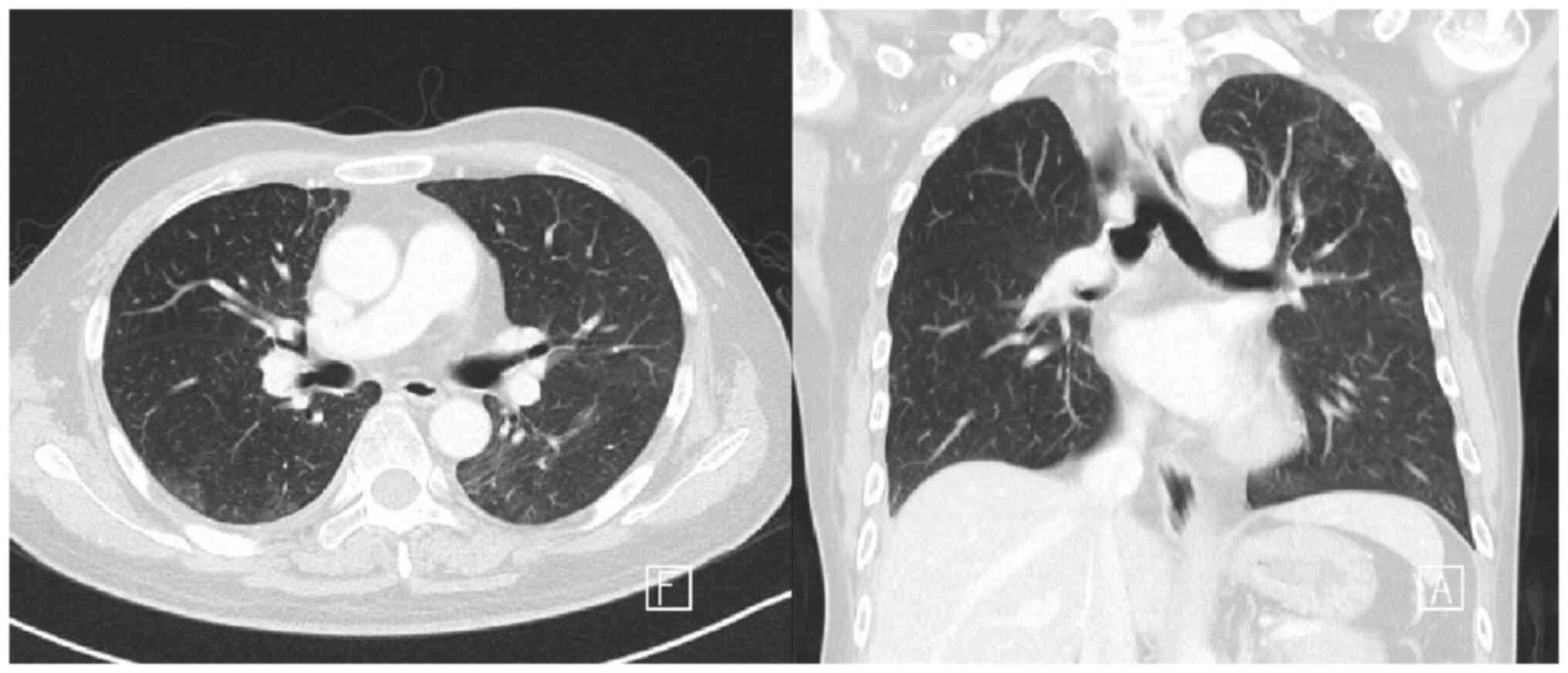
The follow-up chest CT images demonstrated marked regressive
changes in the bilateral ground-glass opacity (Fig. 2). The patient was discharged after
14 days of treatment. Treatment with oral tepotinib, another type
of MET inhibitor, was provided once daily [administered as two 225
mg tablets (450 mg)] for 21 days at 1 month post-discontinuation of
capmatinib treatment. The patient undergoes monthly follow-up chest
X-rays, with chest CT scans every 3 months. The last follow-up was
in June 2023, and currently, there are no signs of ILD.
Discussion
The development of ILD is a rare but serious side
effect associated with the use of capmatinib for NSCLC. Although
the incidence of ILD caused by capmatinib treatment is low (three
reported cases), it is important for healthcare providers to be
aware of the potential risks and to monitor patients closely for
signs and symptoms of ILD. There were three case reports that
emphasized the emergence of ILD due to capmatinib therapy. Among
these, two cases saw resolution after undergoing corticosteroid
treatment, while another two cases exhibited a successful shift to
tepotinib as an alternative targeted therapy. These findings
closely parallel the conclusions drawn in our article (6–8). Both
the prompt recognition of signs and symptoms of ILD and the
management of capmatinib-induced ILD is crucial to avoid potential
complications of this condition and to ensure the best possible
outcomes for patients (4,6–8). The
discontinuation of capmatinib treatment and prompt initiation of
corticosteroid treatment can lead to complete resolution of ILD in
certain cases, as demonstrated in the present case report.
The primary emphasis in ILD metabolomics research
has centered around the examination of lung tissue, bronchoalveolar
lavage fluid and exhaled breath condensate samples derived from
individuals suffering from idiopathic pulmonary fibrosis, the
prevailing subtype among ILD cases (10). By conducting a thorough analysis of
protein precipitation of serum samples, it has been reported that
lysophosphatidylcholine (LysoPC), a substance that acts as a
precursor for lysophosphatic acid, serves a pivotal role in
distinguishing between patients and healthy controls (11). This highlights the significance of
LysoPC as a potential biomarker for identifying individuals
affected by the condition, providing valuable insights into the
underlying mechanisms of the disease and offering a promising
avenue for further diagnostic and therapeutic developments in the
field of medical research (11).
Given the potential risk of ILD with capmatinib
treatment, it is important for healthcare providers to educate
patients on the signs and symptoms of this condition and to
encourage patients to promptly report any concerns. Further
research is needed to better understand the risk factors,
pathophysiology and optimal management of this rare but serious
side effect of capmatinib treatment.
In conclusion, the present case report demonstrates
the potential for capmatinib to cause ILD, a rare but serious side
effect resulting from the administration of capmatinib treatment.
Early recognition of ILD and discontinuation of the capmatinib
treatment, in addition to the prompt administration of
corticosteroids, can lead to complete resolution of ILD. Healthcare
providers should closely monitor patients taking capmatinib for any
signs or symptoms of ILD.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author upon reasonable
request.
Authors' contributions
CYC designed the study, revised the manuscript for
intellectual content and gave final approval for publication. BJL
obtained medical images, analyzed patient data and drafted the
manuscript. CYC and BJL confirm the authenticity of all the raw
data. Both authors read and approved the final version of the
manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
The patient provided written informed consent for
this case study to be published.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Wolf J, Seto T, Han JY, Reguart N, Garon
EB, Groen HJ, Tan DSW, Hida T, de Jonge M, Orlov SV, et al:
Capmatinib (INC280) in patients (pts) with METex14-mutated advances
NSCLC: An update from phase 2 GEOMETRY mono-1 study. Pneumologie.
74((S 01)): S1342020.
|
|
2
|
Zhang Y, Xia M, Jin K, Wang S, Wei H, Fan
C, Wu Y, Li X, Li X, Li G, et al: Function of the c-Met receptor
tyrosine kinase in carcinogenesis and associated therapeutic
opportunities. Mol Cancer. 17:452018. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Wu YL, Zhang L, Kim DW, Liu X, Lee DH,
Yang JC, Ahn MJ, Vansteenkiste JF, Su WC, Felip E, et al: Phase
Ib/II study of capmatinib (INC280) plus gefitinib after failure of
epidermal growth factor receptor (EGFR) inhibitor therapy in
patients with EGFR-mutated, MET factor-dysregulated non-small-cell
lung cancer. J Clin Oncol. 36:3101–3109. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Kubo K, Azuma A, Kanazawa M, Kameda H,
Kusumoto M, Genma A, Saijo Y, Sakai F, Sugiyama Y, Tatsumi K, et
al: Consensus statement for the diagnosis and treatment of
drug-induced lung injuries. Respir Investig. 51:260–277. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Antoniou KM, Margaritopoulos GA,
Tomassetti S, Bonella F, Costabel U and Poletti V: Interstitial
lung disease. Eur Respir Rev. 23:40–54. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Kanemura H, Takeda M, Shimizu S and
Nakagawa K: Interstitial lung disease associated with capmatinib
therapy in a patient with non-small cell lung cancer harboring a
skipping mutation of MET exon 14. Thorac Cancer. 12:549–552. 2021.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Hashiguchi MH, Sato T, Yamamoto H,
Watanabe R, Kagyo J, Domoto H and Shiomi T: Successful tepotinib
challenge after capmatinib-induced interstitial lung disease in a
patient with lung adenocarcinoma harboring MET exon 14 skipping
mutation: Case report. JTO Clin Res Rep. 3:1002712021.PubMed/NCBI
|
|
8
|
Tseng LW, Chang JWC and Wu CE: Safety of
tepotinib challenge after capmatinib-induced pneumonitis in a
patient with non-small cell lung cancer harboring MET exon 14
skipping mutation: A case report. Int J Mol Sci. 23:118092022.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Amin MB, Greene FL, Edge SB, Compton CC,
Gershenwald JE, Brookland RK, Meyer L, Gress DM, Byrd DR and
Winchester DP: The eighth edition AJCC cancer staging manual:
Continuing to build a bridge from a population-based to a more
‘personalized’ approach to cancer staging. CA Cancer J Clin.
67:93–99. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Kang YP, Lee SB, Lee JM, Kim HM, Hong JY,
Lee WJ, Choi CW, Shin HK, Kim DJ, Koh ES, et al: Metabolic
profiling regarding pathogenesis of idiopathic pulmonary fibrosis.
J Proteome Res. 15:1717–1724. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Rindlisbacher B, Schmid C, Geiser T, Bovet
C and Funke-Chambour M: Serum metabolic profiling identified a
distinct metabolic signature in patients with idiopathic pulmonary
fibrosis-a potential biomarker role for LysoPC. Respir Res.
19:72018. View Article : Google Scholar : PubMed/NCBI
|