Introduction
According to global cancer statistics for 2022, ~20
million new cancer cases were diagnosed worldwide, resulting in 9.7
million deaths. Projections suggest that the number of cancer cases
will rise to 35 million by 2050, reflecting population growth and
aging trends (1). These estimates
highlight the serious threat posed by malignant tumors to global
health, as well as their substantial social and economic impact.
Therefore, improving cancer treatment is not only a medical
priority but also a crucial public health objective. Cancer
immunotherapy has emerged as a transformative approach that
mobilizes the patient's own immune system to recognize and
eliminate malignant cells (2,3). Major
immunotherapeutic strategies, including immune checkpoint
inhibitors (ICIs), adoptive cell transfer and cancer vaccines, have
made substantial advancements in the treatment of various diseases
and have provided patients with advanced cancer with the
possibility of a long-term life (4,5).
However, the broader application of these therapies is limited by
issues such as primary or acquired resistance, limited response
rates and immune-related adverse events. There is a pressing need
to identify novel strategies that can enhance the efficacy and
expand the applicability of cancer immunotherapy (6,7).
Metformin, a first-line biguanide agent for type 2
diabetes mellitus, is widely recognized for its favorable safety
and tolerability profile. It improves glycemic control through
multiple mechanisms: Reducing intestinal glucose absorption,
decreasing hepatic glucose output (gluconeogenesis) and enhancing
insulin sensitivity in peripheral tissues (8–10).
Beyond its glucoregulatory actions, metformin has garnered
significant interest in oncology over the past decade. A growing
body of preclinical evidence suggests that metformin may possess
direct and indirect antitumor properties and could potentially
augment the efficacy of cancer immunotherapy (11–14).
It may exert an anti-tumor effect via activating the adenosine
monophosphate-activated protein kinase (AMPK)/mammalian target of
rapamycin (mTOR) pathway (12),
decreasing programmed death ligand 1 (PD-L1) expression (15), suppressing mitochondrial complex I
activity (16) and modulating the
tumor microenvironment (TME) (17,18).
Numerous clinical studies have shown its association with a lower
risk and better prognosis for cancer patients (19–21).
It has also been shown to work in concert with immunotherapy
(22,23), establishing a theoretical basis for
the concurrent use of metformin and immunotherapy (24–26).
Despite these promising preclinical and
pharmacological insights, the clinical efficacy of combining
metformin with immunotherapy remains controversial (27,28).
Therefore, a meta-analysis was performed in the present study to
synthesize the available evidence regarding the association between
metformin use and survival outcomes in cancer patients receiving
ICIs, with the aim of clarifying its potential role as an
adjunctive therapy in immunotherapy.
Materials and methods
Search strategy and study
selection
This meta-analysis was conducted in accordance with
the PRISMA guidelines (29). A
systematic literature search was performed using four electronic
databases: PubMed (https://pubmed.ncbi.nlm.nih.gov/), Embase (https://www.embase.com/), the Cochrane Library
(https://www.cochranelibrary.com/) and
Web of Science (https://www.webofscience.com/), covering publications
from January 2015 to December 2024. The search strategy utilized a
combination of medical subject headings and free-text terms. Key
words included ‘metformin’, ‘metoguanide’, ‘glucophage’, ‘metformin
hydrochloride’, ‘immunotherapy’, ‘immune checkpoint inhibitor’,
‘tumor’, ‘cancer’ and other associated terms.
The literature search and screening process employed
a dual-independent reviewer approach to minimize selection bias.
Any disagreements between the two reviewers (YQ and HL) at either
stage were first addressed through discussion to reach a consensus.
For persistent disagreements, a third reviewer (YF) was consulted
to arbitrate and make the final decision.
Inclusion and exclusion criteria
The eligibility of studies was determined based on
the pre-specified Population, Intervention, Comparator, Outcomes,
Study design framework (30).
Studies were included if they met the following criteria: i)
Enrolled adult patients (≥18 years) with histologically or
cytologically confirmed cancer; ii) examined the impact of
metformin use, in combination with immunotherapy [e.g.,
anti-programmed cell death 1 (PD-1)/PD-L1, anti-cytotoxic
T-lymphocyte associated protein-4 agents], on survival outcomes;
iii) reported at least one of the primary outcomes of interest,
such as overall survival (OS) or progression-free survival (PFS),
with provision of hazard ratios (HR) and corresponding 95%
confidence intervals (CI) (or sufficient data for their
calculation); iv) were published in English.
Exclusion criteria: i) Duplicate publications; ii)
systematic reviews, narrative reviews, editorials, commentaries and
preclinical studies; iii) case reports or conference abstracts
lacking full outcome data; iv) they lacked essential outcome data
of interest even after attempting to contact the corresponding
authors.
Quality evaluation
The methodological quality of the included
observational studies was appraised using the Newcastle-Ottawa
Scale (NOS) (31). The NOS tool
assesses studies across three domains: i) The selection of the
study groups, ii) the comparability of these groups, and iii) the
ascertainment of the outcome. A star system is used for rating,
with a maximum score of nine stars. Based on the total NOS score,
studies were classified as high quality (7–9 stars), moderate
quality (4–6 stars), or low quality (0–3 stars). In line with
standard methodological practice, only studies rated as moderate or
high quality were included in the subsequent meta-analysis to
enhance the robustness of the pooled findings.
Data extraction
A standardized, pre-piloted data extraction form was
used to collect relevant information from the included studies. The
extracted data encompassed the following domains: First author and
publication year; study design; country or region where the study
was conducted; patient population characteristics, including sample
size and cancer type; details of the interventions (ICI regimen and
metformin usage); and primary outcomes of interest, specifically OS
and PFS, with a focus on obtaining HRs and their 95% CI.
Statistical analysis
All statistical computations for the meta-analysis
were performed using STATA software (version 18.0; StataCorp.). The
pooled HR, along with its 95% CI, served as the primary summary
measure. In accordance with the Cochrane Handbook recommendations
(30), which state that
heterogeneity is always expected among studies from different
settings and that model selection should not be based solely on
statistical tests for heterogeneity, a random-effects model was
applied for all meta-analyses to provide a more conservative and
generalizable estimate of the overall effect. Potential publication
bias was assessed both graphically using a funnel plot and
statistically using Begg's test (32). A sensitivity analysis, performed by
sequentially excluding each study and recalculating the pooled
estimate, was conducted to evaluate the robustness of the findings.
P<0.05 was considered to indicate a statistically significant
difference.
Results
Basic characteristics of the included
studies
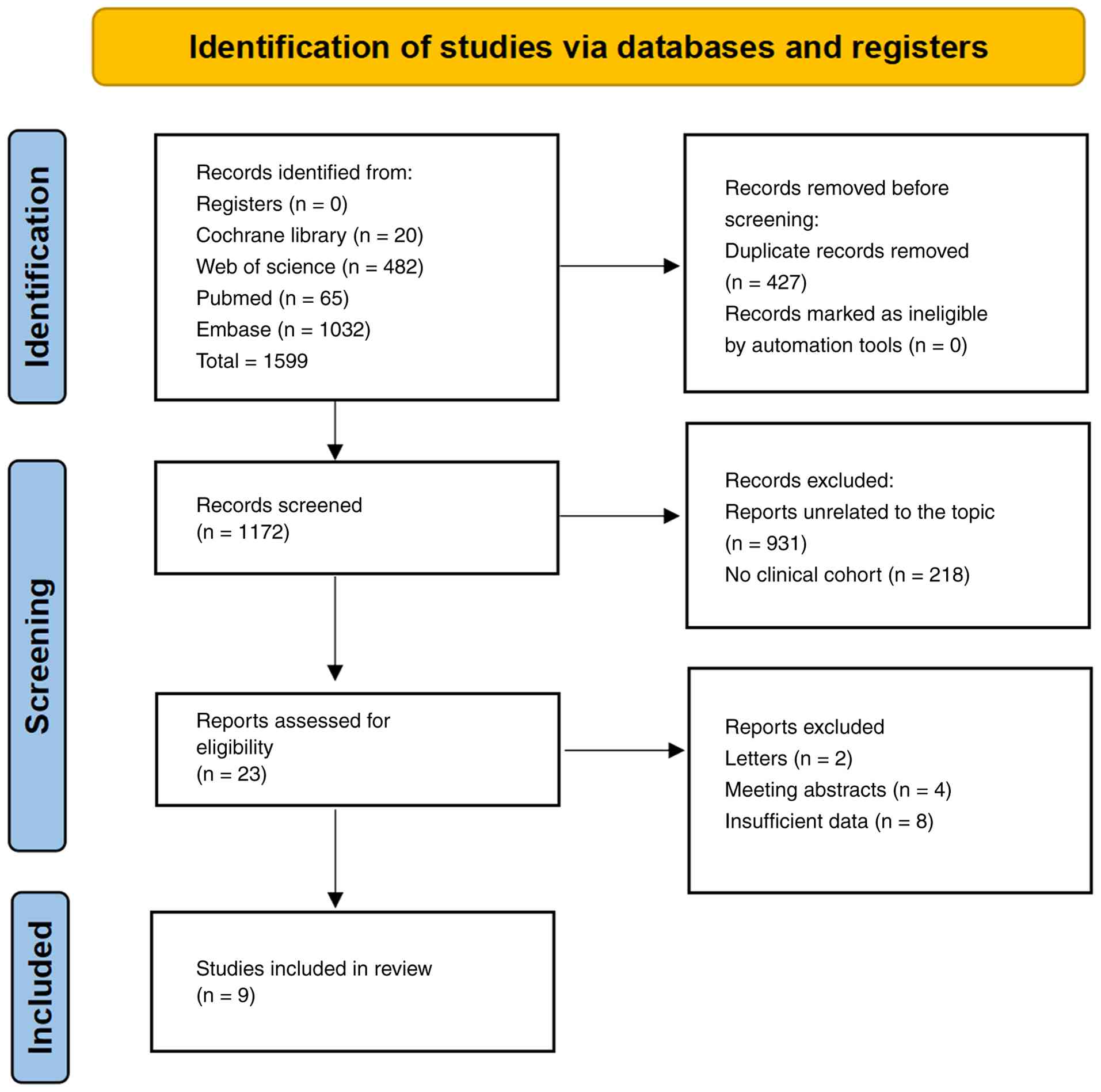
A total of 1,599 papers were obtained for this
investigation and 427 duplicate studies were removed. Based on a
review of the article content, 931 studies irrelevant to the
research topic and 218 studies lacking clinical cohorts were
excluded. Additionally, 14 other studies were excluded, comprising
2 letters, 4 conference papers and 8 studies with missing data. In
conclusion, this meta-analysis was comprised of 9 publications, all
of which were written in English (27,28,33–39).
The procedure for screening the available literature is shown in
Fig. 1.
In all, there were 5,014 individuals who
participated in the 9 studies, with 579 of them being metformin
users. The outcome indicators of 9 articles included OS and 8
reporting on related PFS, including melanoma, lung cancer, renal
cancer, lymphoma and digestive system cancer. A total of 3 articles
pertained to Asian nations and there were six articles pertaining
to countries that are not inside the Asian region, such as Europe
or the US. A variety of immunotherapies, such as ipilimumab,
nivolumab, pembrolizumab, atezolizumab, sintilimab and
camrelizumab, were used in the treatment of cancer patients. The
quality scores of all articles included in the study were not less
than 7 (Table I). The primary
features of the included studies are shown in Table II.
 | Table I.Newcastle-Ottawa scale scores for
quality assessment of included studies. |
Table I.
Newcastle-Ottawa scale scores for
quality assessment of included studies.
|
| Selection | Comparability | Outcome |
|
|---|
|
|
|
|
|
|
|---|
| Author/s, year | Representativeness
of the exposed cohort | Selection of the
non-exposed cohort | Ascertainment of
exposure | Outcome absent at
baseline | Control for age and
sex | Adjust for
potential confounders | Assessment of
outcome | Sufficiently long
follow-up duration | Adequacy of
follow-up of cohorts | Total | (Refs.) |
|---|
| Chiang et
al, 2023 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 9 | (27) |
| Afzal et al,
2018 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 7 | (28) |
| Afzal et al,
2019 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 7 | (33) |
| Wang et al,
2020 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 8 | (34) |
| Gaucher et
al, 2021 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 8 | (35) |
| Cortellini et
al, 2021 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 8 | (36) |
| Yang et al,
2023 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 8 | (37) |
| Fiala et al,
2023 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 9 | (38) |
| Wang et al,
2024 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 9 | (39) |
 | Table II.The main characteristics of studies
included in this meta-analysis. |
Table II.
The main characteristics of studies
included in this meta-analysis.
| Author/s, year | Country | Cancer type | Study design | ICIs | Total sample
size | Males, n (%) | Metformin vs. no
metformin | Outcome
measures | (Refs.) |
|---|
| Chiang et
al, 2023 | China | Lung,
gastrointestinal, hepatobiliary, gynecological | Cohort | NA | 878 | NA | 86/599 | OS, PFS | (27) |
| Afzal et al,
2018 | US | Melanoma | Cohort | Ipilimumab,
Nivolumab, Pembrolizumab | 55 | 34 (61.8) | 33/22 | OS, PFS, DCR | (28) |
| Afzal et al,
2019 | US | NSCLC | Cohort | Nivolumab,
Pembrolizumab, Atezolizumab | 50 | 28 (56.0) | 21/29 | OS, PFS, ORR | (33) |
| Wang et al,
2020 | Multiple
countries | Melanoma | Cohort | Nivolumab,
Pembrolizumab | 330 | 209 (63.0) | 34/296 | OS, PFS | (34) |
| Gaucher et
al, 2021 | France | Lung, melanoma,
renal and urothelial, head and neck, Hodgkin lymphoma | Cohort | Ipilimumab,
Nivolumab, Pembrolizumab | 372 | 244 (65.6) | 17/355 | OS | (35) |
| Cortellini et
al, 2021 | Multiple
countries | NSCLC | Cohort | Pembrolizumab | 1,545 | 1,028 (66.5) | 125/1420 | OS, PFS, ORR | (36) |
| Yang et al,
2023 | Korea | NSCLC | Cohort | Pembrolizumab,
Nivolumab, Atezolizumab | 466 | 347 (74.5) | 89/377 | OS, PFS | (37) |
| Fiala et al,
2023 | Multiple
countries | Metastatic
urothelial cancer | Cohort | Pembrolizumab | 802 | 491 (61.2) | 98/704 | OS, PFS | (38) |
| Wang et al,
2024 | China | Lung, esophageal,
gastroin-testinal, hepatobiliary and pancreatic | Cohort | Sintilimab,
Camrelizumab, Tirelizumab, Pembrolizumab | 516 | 393 (76.2) | 76/440 | OS, PFS | (39) |
PFS in patients receiving metformin
with immunotherapy
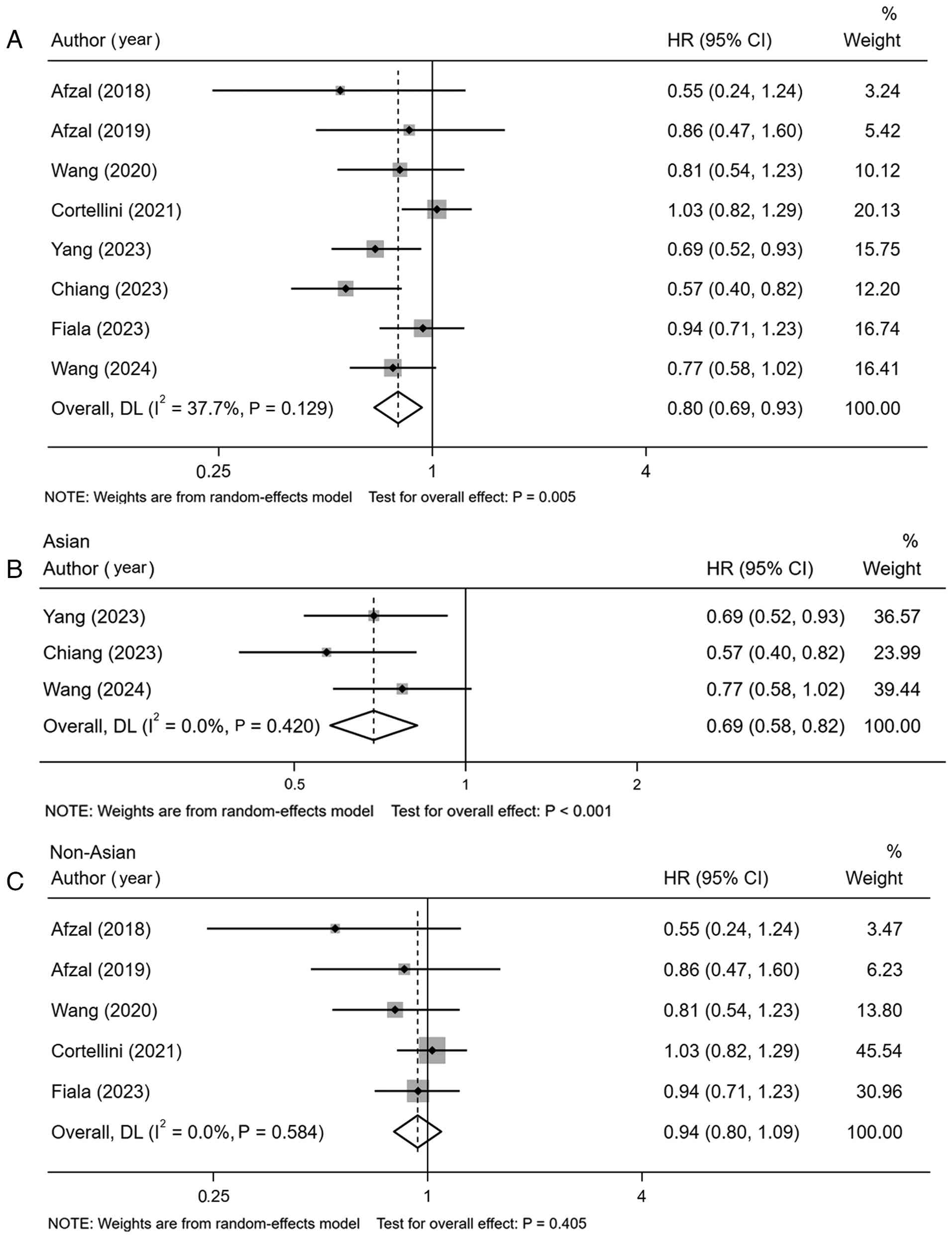
A meta-analysis of 8 studies evaluating PFS was
performed to assess the impact of metformin as an adjunct to ICIs
in cancer patients. The pooled results indicated that concurrent
administration of metformin was associated with a statistically
significant improvement in PFS (HR=0.80, 95% CI: 0.69–0.93,
P=0.005) (Fig. 2A). In a subgroup
analysis stratified by geographical region, a significant PFS
benefit was observed in Asian populations (HR=0.69, 95% CI:
0.58–0.82; P<0.001) (Fig. 2B),
whereas the effect was not statistically significant in non-Asian
populations (HR=0.94, 95% CI: 0.80–1.09; P=0.405) (Fig. 2C).
OS in patients receiving metformin
with immunotherapy
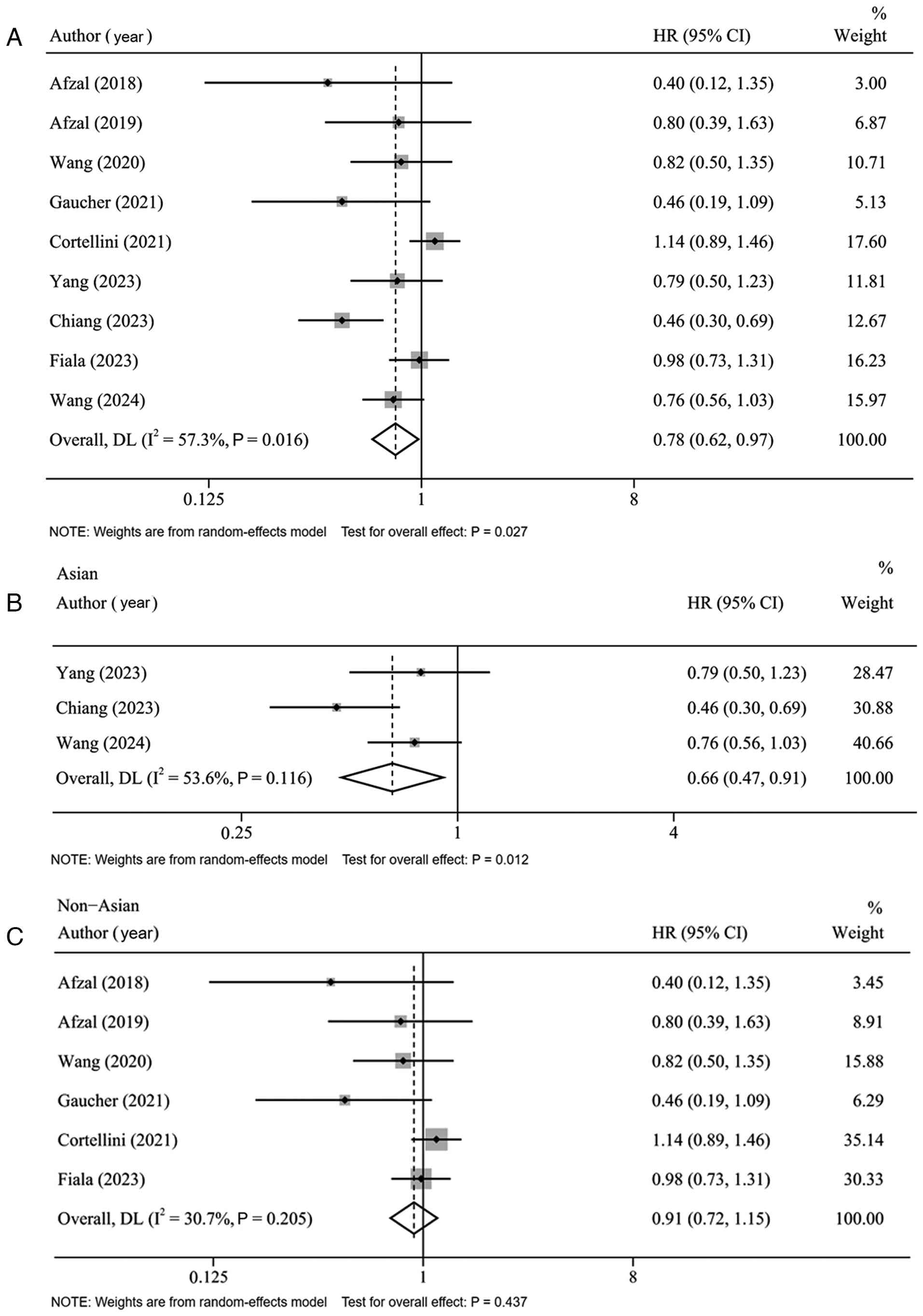
A total of 9 studies were included in the analysis
for the OS endpoint. The combined analysis revealed that the
addition of metformin to immunotherapy was associated with a
significant improvement in OS, yielding a pooled HR of 0.78 (95%
CI: 0.62–0.97; P=0.027) (Fig. 3A).
Subgroup analysis based on geographic region demonstrated a
pronounced OS benefit among Asian patients (HR=0.66, 95% CI:
0.47–0.91; P=0.012) (Fig. 3B),
while no significant improvement was observed in non-Asian cohorts
(HR=0.91, 95% CI: 0.72–1.15, P=0.437) (Fig. 3C).
The results of this meta-analysis suggest that the
concomitant use of metformin with immune checkpoint inhibitors is
associated with improvements in both PFS and OS in cancer patients.
However, the observed benefit exhibits regional variation, with a
more pronounced effect size observed within Asian populations
compared to non-Asian groups. This finding underscores the
potential influence of ethnic or regional factors on treatment
efficacy and highlights the need for further investigation into the
underlying mechanisms driving these differences.
Assessment of publication bias and
sensitivity analysis
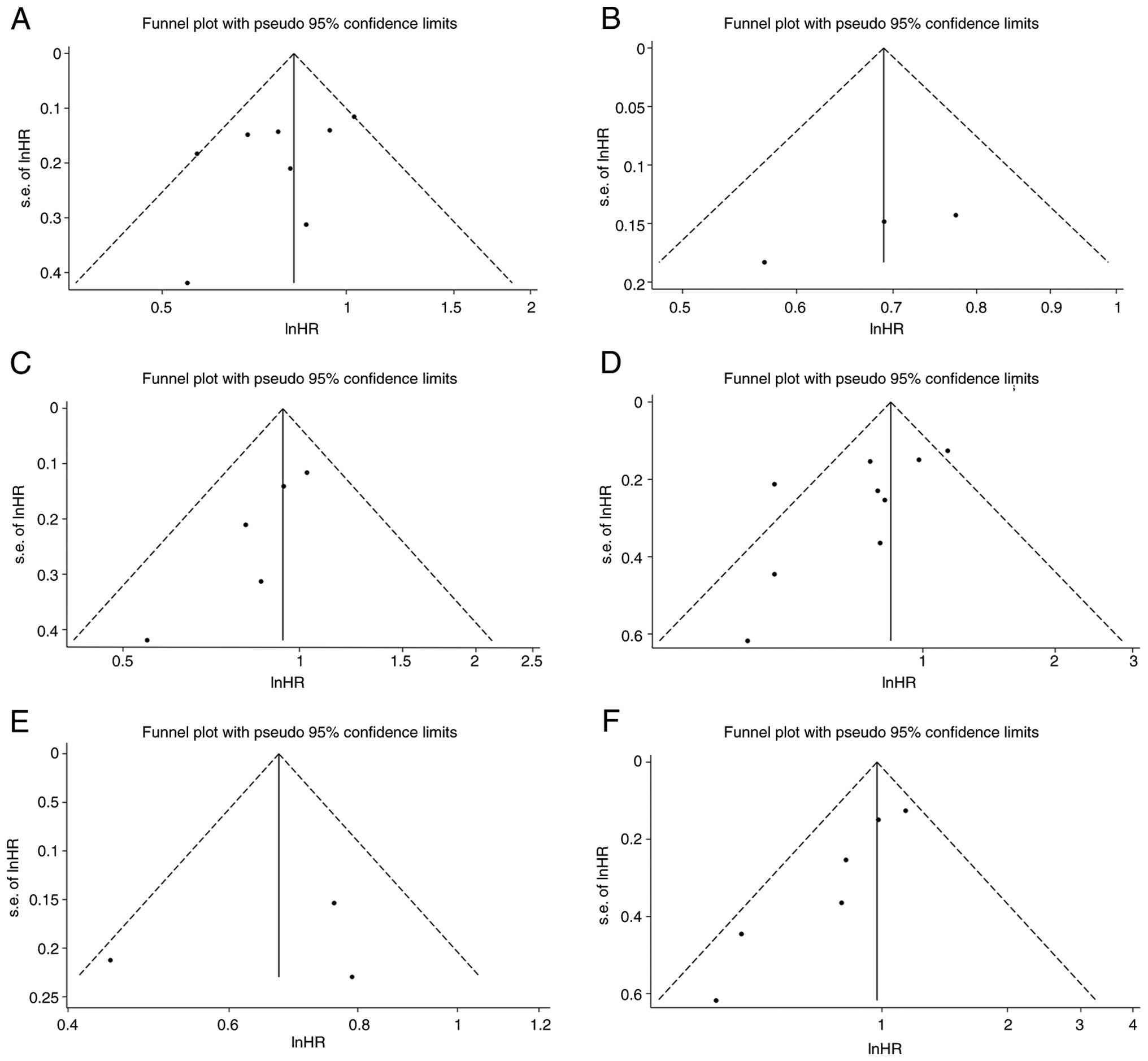
Potential publication bias was evaluated using a
funnel plot inspection and Begg's rank correlation test. The Begg's
test result was not statistically significant (P>0.05), and the
funnel plot showed approximate symmetry. These findings suggest
that publication bias is unlikely to have substantially influenced
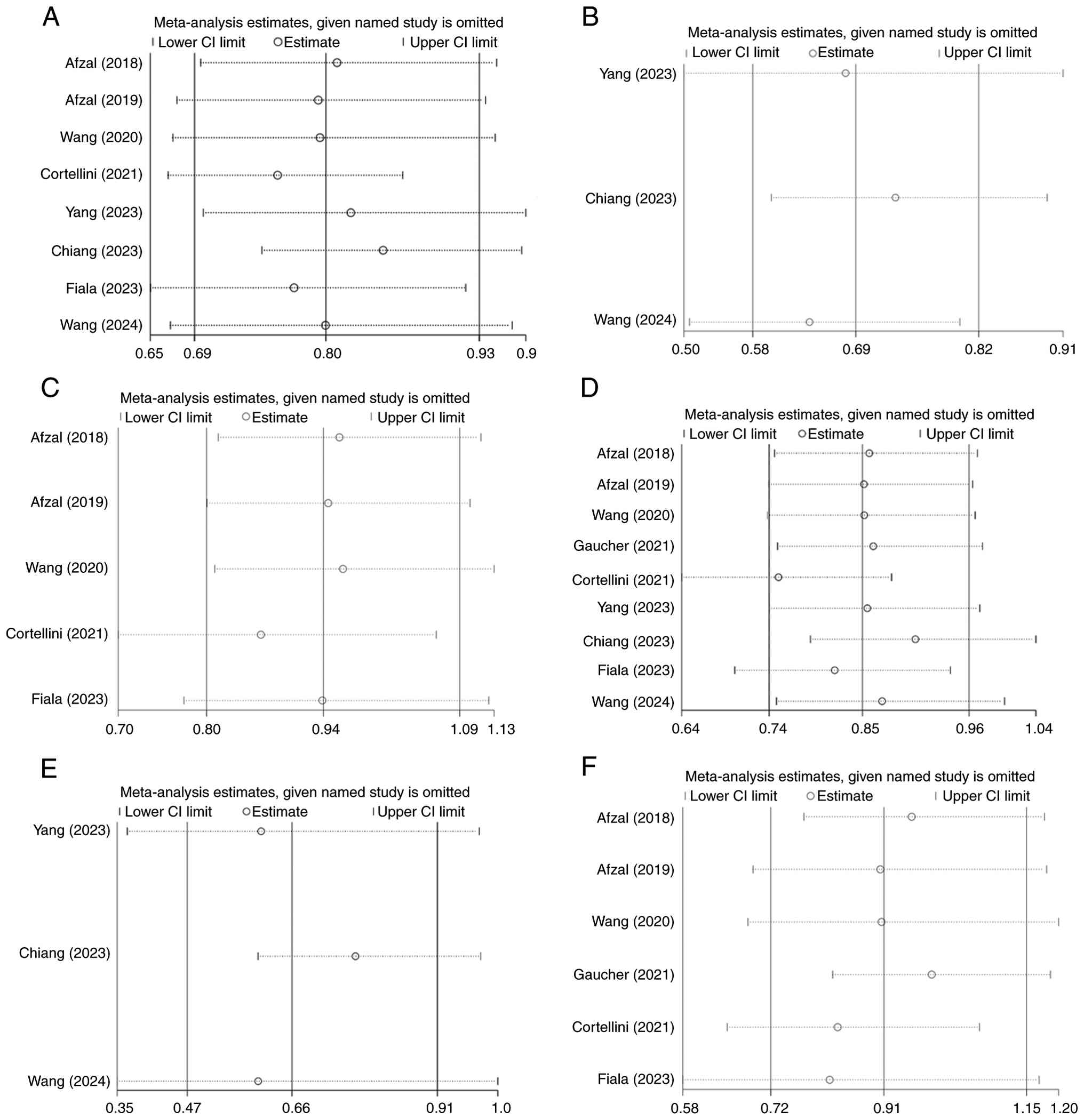
the overall results of this meta-analysis (Fig. 4). A sensitivity analysis was
performed to assess the robustness and stability of the pooled
results. This was conducted using the leave-one-out method, which
involves iteratively removing each individual study and
recalculating the summary effect size for the remaining studies.
The results demonstrated that no single study exerted a
disproportionate influence on the overall effect estimate. This
confirms that the meta-analytic findings are robust and not unduly
dependent on any particular study included in the analysis
(Fig. 5).
Discussion
The present meta-analysis, encompassing 9 studies
and 5,014 cancer patients, investigated the association between
concomitant metformin use and survival outcomes in patients
receiving ICIs. The pooled results demonstrate that metformin use
is significantly associated with improved PFS (HR=0.80, 95% CI:
0.69–0.93, P=0.005) and OS (HR=0.78, 95% CI: 0.62–0.97; P=0.027) in
this patient population. However, subgroup analyses revealed a
striking geographical disparity: The survival benefit was
statistically significant and pronounced in Asian populations (OS:
HR=0.66, 95% CI: 0.47–0.91, P=0.012; PFS: HR=0.69, 95% CI:
0.58–0.82, P<0.001) but was not observed in non-Asian cohorts.
These findings suggest a complex interaction between metformin and
immunotherapy, potentially modulated by regional factors.
Previous meta-analyses, including the study by Wen
et al (40), evaluated
metformin across various anticancer treatment modalities. In
contrast, the present analysis focused specifically on ICI-based
therapies, thereby offering a more immunotherapy-oriented
perspective. In addition, compared with the meta-analysis conducted
by Shen et al (41), which
reported no significant survival benefit and suggested a potential
unfavorable effect of metformin on overall survival, the present
study incorporated additional clinical studies published up to 2024
and applied stricter inclusion criteria by excluding conference
abstracts, letters, studies lacking complete survival data and
those with lower methodological quality, which may enhance data
completeness and analytical reliability. By contrast, the pooled
analysis performed in the present study demonstrated a
statistically significant improvement in both OS and PFS with
metformin use in combination with ICIs. The present subgroup
analysis further provides meta-analytic evidence suggesting a
potentially greater survival benefit among Asian patients. This
regional trend was not clearly delineated in prior studies and may
offer new insights into population-based stratification strategies
in precision immunotherapy. Furthermore, this observation raises
the possibility that differences in metabolic phenotype, genetic
background or treatment patterns may interact with
metformin-mediated immunomodulation.
The observed OS benefit aligns with the premise
derived from preclinical studies that metformin can potentiate
anti-tumor immunity (42–44). Metformin can inhibit the
proliferation and metabolism of tumor cells by activating the AMPK
signaling pathway and inhibiting mTOR signaling (45). It can also reduce the expression of
PD-L1 and block PD-1/PD-L1 signaling, thereby enhancing the
anti-tumor activity of T cells (46). Metformin may also enhance
immune-cell activity and regulate the TME. A theoretical foundation
for its combination with immunotherapy is provided by the
aforementioned findings. Turpin et al (16) published an article in 2024 examining
the utilization of patient-derived explant culture (PDEC) to
investigate the tumor immune microenvironment (TIME), employing
this model to assess the impact of anti-tumor agents, including the
combination of venetoclax and metformin, on immune-cell
functionality. The study's findings indicated that the PDEC model
demonstrated that metformin activated dendritic cells within the
TIME by inhibiting mitochondrial respiratory chain complex, thereby
augmenting the anti-tumor immune response of CD4+ T cells, and
underscored the significance of the PDEC model in investigating the
TIME and the mechanisms of drug action. Tan et al (47) assessed the anti-tumor efficacy of
combining PD-1 inhibitors with mTOR inhibitors rapamycin or
metformin in triple-negative breast cancer (TNBC). According to
their data, metformin and rapamycin may both significantly lower
PD-L1 expression and inhibit mTOR pathway activity in TNBC. The
combination of PD-1 inhibitors with these agents markedly decreased
tumor growth and metastasis, increased CD8+ T-cell infiltration and
tumor-cell apoptosis, and amplified the anti-tumor efficacy of PD-1
inhibitors. Wabitsch et al (26) revealed that non-alcoholic
steatohepatitis (NASH) reduces the efficacy of ICI therapy for
liver cancer by impairing the metabolism and migration capabilities
of CD8+ T cells. In NASH mice, metformin therapy may enhance CD8+
T-cell metabolic activity, regaining the effectiveness of ICI
treatment. These fundamental study results provide a strong
theoretical foundation for metformin's possible use in cancer
immunotherapy. Building on this mechanistic understanding, a recent
study on TNBC has demonstrated that low-dose metformin activates
the AMPK-acetyl-CoA carboxylase-fatty acid β-oxidation signaling
axis, thereby inducing Src kinase activation and enhancing
anti-tumor immunity, whereas high-dose metformin suppresses this
pathway and may even exert tumor-promoting effects (48). However, critical details regarding
metformin dosage, treatment duration, timing of metformin
initiation relative to ICI therapy (before, concurrent with or
after ICI), and steady-state blood concentration in patients were
unavailable in the included studies, limiting further exploration
of optimal therapeutic parameters. Future prospective studies
designing combination therapies should emphasize dose optimization
and clearly report the timing of metformin initiation relative to
ICI to maximize efficacy while minimizing toxicity.
Additionally, studies indicate that diabetes can
alter the immune landscape within the TME of solid tumors,
potentially fostering an immunosuppressive state (49). The immunomodulatory benefits of
metformin, particularly its potential to enhance antitumor
immunity, may be closely linked to the improvement of diabetic
metabolic conditions. This interplay warrants further investigation
through well-controlled animal studies employing both diabetic and
non-diabetic models to dissect the specific contributions of
metabolic normalization vs. direct drug effects. Beyond metabolic
factors, substantial evidence suggests that heterogeneity in the
TME may lead to differential efficacy. For instance, brain tumors
and uveal melanomas, characterized by minimal tumor-infiltrating
immune cells and a macrophage-dominated milieu, often exhibit
resistance to ICIs (50–52). In contrast, malignancies such as
lung adenocarcinoma, head and neck squamous cell carcinoma and
cutaneous melanoma, which typically display richer immune cell
infiltration, tend to respond more favorably to immunotherapy
(53–55). Future multi-center studies with
large-sample cohorts for individual cancer types are warranted to
explore the impact of metformin on immunotherapy outcomes across
different tumor sites.
The most intriguing finding of the present analysis
is the significant disparity in treatment effect between Asian and
non-Asian populations. The reasons for this heterogeneity are
likely multifactorial and may involve differences in tumor biology,
genetic predisposition, pharmacogenomics and clinical practice
patterns. The lack of a statistically significant benefit in
non-Asian cohorts underscores the potential influence of divergent
genetic backgrounds, lifestyles or clinical management approaches.
Future research should integrate multi-omics data, including
genomics and metabolomics, to elucidate the underlying mechanisms,
and conduct multicenter trials to validate and refine
population-specific therapeutic strategies. The study by Bouchi
et al (56) highlighted that
the pathophysiology of diabetes, levels of obesity and insulin
resistance among patients vary across Eastern and Western
populations, along with disparities in pharmacological choices and
treatment methodologies. Lin et al (57) utilized genome-wide association
analysis, cross-ancestry meta—analysis and Mendelian randomization
analysis to explore the genetic structure of metabolites in Han
Chinese and European populations and their correlation with
diseases. They revealed the genetic differences in metabolites
between these ethnic groups and their impact on complex diseases,
underscoring the importance of ethnic diversity in genetic
research. These recent advances in metabolic research also provide
unique insights into the present subgroup analysis results. The
metabolic genetics, pharmacological sensitivities, immunological
responses and other characteristics of individuals from different
locations may be very different from one another. The efficiency of
immunotherapy in combination with metformin metabolic processes may
be impacted by changes in dietary and lifestyle practices.
Subsequent research should account for additional personalized
variables and investigate its mechanism of action in more
depth.
The present meta-analysis has several limitations.
Selection bias may exist, since all of the included studies are
retrospective cohort studies. The lack of individual patient data
prevented more detailed analyses, such as examining the impact of
gene expression or metabolic state on the outcomes. In conclusion,
it may be suggested that metformin may enhance the anti-tumor
efficacy of immunotherapy by collaborating with it, offering a
theoretical foundation for future combination treatment strategies
that emphasize immune modulation.
In conclusion, this meta-analysis provides evidence
that metformin use is associated with enhanced survival outcomes in
cancer patients treated with immune checkpoint inhibitors, with a
particularly significant effect observed in Asian populations.
These results underscore the potential of metformin as an
inexpensive, widely available and generally well-tolerated agent to
augment cancer immunotherapy. However, the geographical
heterogeneity in treatment response cautions against its broad,
indiscriminate use and emphasizes the necessity for predictive
biomarkers. Future efforts should be directed toward prospective,
randomized controlled trials specifically designed to validate the
efficacy of metformin and ICI combination therapy. These trials
should prioritize biomarker-driven patient selection, potentially
focusing on individuals whose tumors exhibit specific metabolic
vulnerabilities or who belong to ethnic subgroups most likely to
benefit.
Acknowledgements
Not applicable.
Funding
This work was supported by the 2024 ‘Wild Goose Array Talents’
Discipline Leader Fund of Wuxi People's Hospital (grant no.
2024-YZ-XKDTR-HD-2024), 2025 ‘Wild Goose Array Talents’ Discipline
Leader Fund of Wuxi People's Hospital (grant no. YZ-XKDTR-HD-2025),
2020 ‘Taihu Lake Talent Program’ Leading Experts (2020–2024) (grant
no. 2020-THRC-LJ-HD) and Oncology-Wuxi Municipal Innovation Team
(14th Five-Year Plan) (grant no. CXTD-1).
Availability of data and materials
The data generated in the present study may be
requested from the corresponding author.
Authors' contributions
YQ, HL and YF contributed to study
conceptualization, data curation, formal analysis, investigation,
methodology, writing of the original draft, and review and editing
of the manuscript. SL and DH were involved in study
conceptualization, supervision, validation, and review and editing
of the manuscript. SL and DH confirm the authenticity of all the
raw data. All authors have read and approved the final version of
the manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Bray F, Laversanne M, Sung H, Ferlay J,
Siegel RL, Soerjomataram I and Jemal A: Global cancer statistics
2022: GLOBOCAN estimates of incidence and mortality worldwide for
36 cancers in 185 countries. CA Cancer J Clin. 74:229–263.
2024.PubMed/NCBI
|
|
2
|
Mellman I, Coukos G and Dranoff G: Cancer
immunotherapy comes of age. Nature. 480:480–489. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Wang DR, Wu XL and Sun YL: Therapeutic
targets and biomarkers of tumor immunotherapy: Response versus
non-response. Signal Transduct Target Ther. 7:3312022. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Yang L, Ning Q and Tang SS: Recent
advances and next breakthrough in immunotherapy for cancer
treatment. J Immunol Res. 2022:80522122022.PubMed/NCBI
|
|
5
|
Kong X, Zhang J, Chen S, Wang X, Xi Q,
Shen H and Zhang R: Immune checkpoint inhibitors: Breakthroughs in
cancer treatment. Cancer Biol Med. 21:451–472. 2024.PubMed/NCBI
|
|
6
|
Weiss SA and Sznol M: Resistance
mechanisms to checkpoint inhibitors. Curr Opin Immunol. 69:47–55.
2021. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Dobosz P, Stępień M, Golke A and
Dzieciątkowski T: Challenges of the immunotherapy: Perspectives and
limitations of the immune checkpoint inhibitor treatment. Int J Mol
Sci. 23:28472022. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Hunter RW, Hughey CC, Lantier L, Sundelin
EI, Peggie M, Zeqiraj E, Sicheri F, Jessen N, Wasserman DH and
Sakamoto K: Metformin reduces liver glucose production by
inhibition of fructose-1-6-bisphosphatase. Nat Med. 24:1395–1406.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Horakova O, Kroupova P, Bardova K,
Buresova J, Janovska P, Kopecky J and Rossmeisl M: Metformin
acutely lowers blood glucose levels by inhibition of intestinal
glucose transport. Sci Rep. 9:61562019. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhou ZY, Ren LW, Zhan P, Yang HY, Chai DD
and Yu ZW: Metformin exerts glucose-lowering action in high-fat fed
mice via attenuating endotoxemia and enhancing insulin signaling.
Acta Pharmacol Sin. 37:1063–1075. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Hua Y, Zheng Y, Yao Y, Jia R, Ge S and
Zhuang A: Metformin and cancer hallmarks: Shedding new lights on
therapeutic repurposing. J Transl Med. 21:4032023. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Foretz M, Guigas B and Viollet B:
Metformin: Update on mechanisms of action and repurposing
potential. Nat Rev Endocrinol. 19:460–476. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
O'Connor L, Bailey-Whyte M, Bhattacharya
M, Butera G, Hardell KNL, Seidenberg AB, Castle PE and
Loomans-Kropp HA: Association of metformin use and cancer
incidence: A systematic review and meta-analysis. J Natl Cancer
Inst. 116:518–529. 2024. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Mu W, Jiang Y, Liang G, Feng Y and Qu F:
Metformin: A promising antidiabetic medication for cancer
treatment. Curr Drug Targets. 24:41–54. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Lu Y, Xin D, Guan L, Xu M, Yang Y, Chen Y,
Yang Y, Wang-Gillam A, Wang L, Zong S and Wang F: Metformin
downregulates PD-L1 expression in esophageal squamous cell
catrcinoma by inhibiting IL-6 signaling pathway. Front Oncol.
11:7625232021. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Turpin R, Liu R, Munne PM, Peura A,
Rannikko JH, Philips G, Boeckx B, Salmelin N, Hurskainen E,
Suleymanova I, et al: Respiratory complex I regulates dendritic
cell maturation in explant model of human tumor immune
microenvironment. J Immunother Cancer. 12:e0080532024. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Nishida M, Yamashita N, Ogawa T, Koseki K,
Warabi E, Ohue T, Komatsu M, Matsushita H, Kakimi K, Kawakami E, et
al: Mitochondrial reactive oxygen species trigger
metformin-dependent antitumor immunity via activation of
Nrf2/mTORC1/p62 axis in tumor-infiltrating CD8T lymphocytes. J
Immunother Cancer. 9:e0029542021. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Hanahan D, Michielin O and Pittet MJ:
Convergent inducers and effectors of T cell paralysis in the tumour
microenvironment. Nat Rev Cancer. 25:41–58. 2025. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Yao K, Zheng H and Li T: Association
between metformin use and the risk, prognosis of gynecologic
cancer. Front Oncol. 12:9423802022. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Brancher S, Støer NC, Weiderpass E,
Damhuis RAM, Johannesen TB, Botteri E and Strand TE: Metformin use
and lung cancer survival: A population-based study in Norway. Br J
Cancer. 124:1018–1025. 2021. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Almeida-Nunes DL, Silvestre R,
Dinis-Oliveira RJ and Ricardo S: Enhancing immunotherapy in ovarian
cancer: The emerging role of metformin and statins. Int J Mol Sci.
25:3232023. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Zhu L, Yang K, Ren Z, Yin D and Zhou Y:
Metformin as anticancer agent and adjuvant in cancer combination
therapy: Current progress and future prospect. Transl Oncol.
44:1019452024. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Munoz LE, Huang L, Bommireddy R, Sharma R,
Monterroza L, Guin RN, Samaranayake SG, Pack CD, Ramachandiran S,
Reddy SJC, et al: Metformin reduces PD-L1 on tumor cells and
enhances the anti-tumor immune response generated by vaccine
immunotherapy. J Immunother Cancer. 9:e0026142021. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Cha JH, Yang WH, Xia W, Wei Y, Chan LC,
Lim SO, Li CW, Kim T, Chang SS, Lee HH, et al: Metformin promotes
antitumor immunity via endoplasmic-reticulum-associated degradation
of PD-L1. Mol Cell. 71:606–620.e7. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Eikawa S, Nishida M, Mizukami S, Yamazaki
C, Nakayama E and Udono H: Immune-mediated antitumor effect by type
2 diabetes drug, metformin. Proc Natl Acad Sci USA. 112:1809–1814.
2015. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Wabitsch S, McCallen JD, Kamenyeva O, Ruf
B, McVey JC, Kabat J, Walz JS, Rotman Y, Bauer KC, Craig AJ, et al:
Metformin treatment rescues CD8+ T-cell response to immune
checkpoint inhibitor therapy in mice with NAFLD. J Hepatol.
77:748–760. 2022. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Chiang CH, Chen YJ, Chiang CH, Chen CY,
Chang YC, Wang SS, See XY, Horng CS, Peng CY, Hsia YP, et al:
Effect of metformin on outcomes of patients treated with immune
checkpoint inhibitors: A retrospective cohort study. Cancer Immunol
Immunother. 72:1951–1956. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Afzal MZ, Mercado RR and Shirai K:
Efficacy of metformin in combination with immune checkpoint
inhibitors (anti-PD-1/anti-CTLA-4) in metastatic malignant
melanoma. J Immunother Cancer. 6:642018. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Page MJ, Bossuyt PM, Boutron I, Boutron I,
Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan
SE, et al: The PRISMA 2020 statement: An updated guideline for
reporting systematic reviews. Int J Surg. 88:1059062021. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Higgins JPT, Thomas J, Chandler J,
Cumpston M, Li T, Page MJ and Welch VA: Cochrane Handbook for
Systematic Reviews of Interventions. 2nd edition. John Wiley &
Sons; Chichester: 2019, View Article : Google Scholar
|
|
31
|
Wells GA, Shea B, O'Connell D, Peterson J,
Welch V, Losos M and Tugwell P: The newcastle-ottawa scale (NOS)
for assessing the quality of nonrandomised studies in
meta-analyses. Ottawa Hospital Research Institute; 2014
|
|
32
|
Begg CB and Mazumdar M: Operating
characteristics of a rank correlation test for publication bias.
Biometrics. 50:1088–1101. 1994. View
Article : Google Scholar : PubMed/NCBI
|
|
33
|
Afzal MZ, Dragnev K, Sarwar T and Shirai
K: Clinical outcomes in non-small-cell lung cancer patients
receiving concurrent metformin and immune checkpoint inhibitors.
Lung Cancer Manag. 8:LMT112019. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Wang DY, McQuade JL, Rai RR, Park JJ, Zhao
S, Ye F, Beckermann KE, Rubinstein SM, Johnpulle R, Long GV, et al:
The impact of nonsteroidal anti-inflammatory drugs, beta blockers,
and metformin on the efficacy of anti-PD-1 therapy in advanced
melanoma. Oncologist. 25:e602–e605. 2020. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Gaucher L, Adda L, Séjourné A, Joachim C,
Guillaume C, Poulet C, Liabeuf S, Gras-Champel V, Masmoudi K,
Houessinon A, et al: Associations between dysbiosis-inducing drugs,
overall survival and tumor response in patients treated with immune
checkpoint inhibitors. Ther Adv Med Oncol.
13:175883592110005912021. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Cortellini A, Di Maio M, Nigro O, Leonetti
A, Cortinovis DL, Aerts JG, Guaitoli G, Barbieri F, Giusti R,
Ferrara MG, et al: Differential influence of antibiotic therapy and
other medications on oncological outcomes of patients with
non-small cell lung cancer treated with first-line pembrolizumab
versus cytotoxic chemotherapy. J Immunother Cancer. 9:e0024212021.
View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Yang J, Kim SH, Jung EH, Kim SA, Suh KJ,
Lee JY, Kim JW, Kim JW, Lee JO, Kim YJ, et al: The effect of
metformin or dipeptidyl peptidase 4 inhibitors on clinical outcomes
in metastatic non-small cell lung cancer treated with immune
checkpoint inhibitors. Thorac Cancer. 14:52–60. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Fiala O, Buti S, Takeshita H, Okada Y,
Massari F, Palacios GA, Dionese M, Scagliarini S, Büttner T,
Fornarini G, et al: Use of concomitant proton pump inhibitors,
statins or metformin in patients treated with pembrolizumab for
metastatic urothelial carcinoma: Data from the ARON-2 retrospective
study. Cancer Immunol Immunother. 72:3665–3682. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Wang J, Lin J and Guo H, Wu W, Yang J, Mao
J, Fan W, Qiao H, Wang Y, Yan X and Guo H: Prognostic impact of
metformin in solid cancer patients receiving immune checkpoint
inhibitors: Novel evidences from a multicenter retrospective study.
Front Pharmacol. 15:14194982024. View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Wen J, Yi Z, Chen Y, Huang J, Mao X, Zhang
L, Zeng Y, Cheng Q, Ye W, Liu Z, et al: Efficacy of metformin
therapy in patients with cancer: A meta-analysis of 22 randomised
controlled trials. BMC Med. 20:4022022. View Article : Google Scholar : PubMed/NCBI
|
|
41
|
Shen J, Ye X, Hou H and Wang Y: Clinical
evidence for the prognostic impact of metformin in cancer patients
treated with immune checkpoint inhibitors. Int Immunopharmacol.
134:1122432024. View Article : Google Scholar : PubMed/NCBI
|
|
42
|
Xue J, Li L, Li N, Li F, Qin X, Li T and
Liu M: Metformin suppresses cancer cell growth in endometrial
carcinoma by inhibiting PD-L1. Eur J Pharmacol. 859:1725412019.
View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Wang Z, Lu C, Zhang K, Lin C, Wu F, Tang
X, Wu D, Dou Y, Han R, Wang Y, et al: Metformin combining PD-1
inhibitor enhanced anti-tumor efficacy in STK11 mutant lung cancer
through AXIN-1-dependent inhibition of STING ubiquitination. Front
Mol Biosci. 9:7802002022. View Article : Google Scholar : PubMed/NCBI
|
|
44
|
Jiang H, Suo H, Gao L, Liu Y, Chen B, Lu
S, Jin F and Cao Y: Metformin plays an antitumor role by
downregulating inhibitory cells and immune checkpoint molecules
while activating protective immune responses in breast cancer. Int
Immunopharmacol. 118:1100382023. View Article : Google Scholar : PubMed/NCBI
|
|
45
|
Kim K, Yang WH, Jung YS and Cha JH: A new
aspect of an old friend: The beneficial effect of metformin on
anti-tumor immunity. BMB Rep. 53:512–520. 2020. View Article : Google Scholar : PubMed/NCBI
|
|
46
|
Panaampon J, Zhou Y and Saengboonmee C:
Metformin as a booster of cancer immunotherapy. Int
Immunopharmacol. 121:1105282023. View Article : Google Scholar : PubMed/NCBI
|
|
47
|
Tan X, Li Y, Hou Z, Zhang M, Li L and Wei
J: Combination therapy with PD-1 inhibition plus rapamycin and
metformin enhances anti-tumor efficacy in triple negative breast
cancer. Exp Cell Res. 429:1136472023. View Article : Google Scholar : PubMed/NCBI
|
|
48
|
Park JH, Jung KH, Jia D, Yang S, Attri KS,
Ahn S, Murthy D, Samanta T, Dutta D, Ghidey M, et al: Biguanides
antithetically regulate tumor properties by the dose-dependent
mitochondrial reprogramming-driven c-Src pathway. Cell Rep Med.
6:1019412025. View Article : Google Scholar : PubMed/NCBI
|
|
49
|
Garstka MA, Kedzierski L and Maj T:
Diabetes can impact cellular immunity in solid tumors. Trends
Immunol. 46:295–309. 2025. View Article : Google Scholar : PubMed/NCBI
|
|
50
|
Salmon H, Remark R, Gnjatic S and Merad M:
Host tissue determinants of tumour immunity. Nat Rev Cancer.
19:215–227. 2019.PubMed/NCBI
|
|
51
|
Giraldo NA, Becht E, Vano Y, Petitprez F,
Lacroix L, Validire P, Sanchez-Salas R, Ingels A, Oudard S, Moatti
A, et al: Tumor-infiltrating and peripheral blood T-cell
immunophenotypes predict early relapse in localized clear cell
renal cell carcinoma. Clin Cancer Res. 23:4416–4428. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
52
|
Ganss R: Tumour vessel remodelling: New
opportunities in cancer treatment. Vasc Biol. 2:R35–R43. 2020.
View Article : Google Scholar : PubMed/NCBI
|
|
53
|
Reck M, Rodríguez-Abreu D, Robinson AG,
Hui R, Csőszi T, Fülöp A, Gottfried M, Peled N, Tafreshi A, Cuffe
S, et al: Pembrolizumab versus chemotherapy for PD-L1-positive
non-small-cell lung cancer. N Engl J Med. 375:1823–1833. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
54
|
Burtness B, Harrington KJ, Greil R,
Soulières D, Tahara M, de Castro G Jr, Psyrri A, Basté N, Neupane
P, Bratland Å, et al: Pembrolizumab alone or with chemotherapy
versus cetuximab with chemotherapy for recurrent or metastatic
squamous cell carcinoma of the head and neck (KEYNOTE-048): A
randomised, open-label, phase 3 study. Lancet. 394:1915–1928. 2019.
View Article : Google Scholar : PubMed/NCBI
|
|
55
|
Larkin J, Chiarion-Sileni V, Cowey CL,
Gonzalez R, Grob JJ, Cowey CL, Lao CD, Schadendorf D, Dummer R,
Smylie M, et al: Combined nivolumab and ipilimumab or monotherapy
in untreated melanoma. N Engl J Med. 373:23–34. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
56
|
Bouchi R, Kondo T, Ohta Y, Goto A, Tanaka
D, Satoh H, Yabe D, Nishimura R, Harada N, Kamiya H, et al: A
consensus statement from the Japan Diabetes Society: A proposed
algorithm for pharmacotherapy in people with type 2 diabetes. J
Diabetes Investig. 14:151–164. 2023. View Article : Google Scholar : PubMed/NCBI
|
|
57
|
Lin C, Xia M, Dai Y, Huang Q, Sun Z, Zhang
G, Luo R, Peng Q, Li J, Wang X, et al: Cross-ancestry analyses of
Chinese and European populations reveal insights into the genetic
architecture and disease implication of metabolites. Cell Genom.
5:1008102025. View Article : Google Scholar : PubMed/NCBI
|