Introduction
Esophageal cancer (EC) is a highly malignant tumor
and a major threat to health worldwide; it has a 5-year survival
rate of <10% and 300,000 people succumb to the disease, half of
whom are from China. In China, EC is characterized by its distinct
geographic distribution and differences in ethnic prevalence
(1). Ningxia, in Western China, has
one of the highest prevalence and mortality rates of esophageal
carcinoma in the world. Despite advances in clinical treatment, the
complexity of cancer has posed a formidable challenge to both
clinicians and researchers. Due to its relapse and metastasis
characteristics, prognostic factors are essential to improve the
classic risk classification in EC.
Chronic infection and inflammation can induce cancer
formation via proinflammatory factors by promoting angiogenesis and
metastasis contributing to cancer development and growth. Toll-like
receptors (TLRs) are pathogen recognizing receptors that mediate
innate immune responses including the secretion of cytokines as
well as the release of chemokines, thus limiting microbe spreading
and triggering inflammatory responses (2–6). The
TLR family consists of >10 members in humans. TLR9 is one of the
important members in this family. Ligand binding to TLR9 activates
several different signaling factors, such as nuclear factor-κB
(NF-κB) eventually characterized by increased production of
inflammatory mediators (7). Recent
studies found that high expression of TLR9 occurred not only in
immune cells, but also in various cancer cells including breast,
brain, ovarian, gastric, lung and prostate cancer cells (8). The role of TLR9 expressed by tumor
cells in the evasion of immune surveillance was demonstrated in
animal experiments showing that TLR9 stimulation may lead to tumor
progression and inflammation and cell survival increasing (9). Furthermore, treatment of
TLR9-expressing cancer cells with synthetic TLR9 ligands that are
reminiscent of bacterial DNA increases the invasion of breast and
prostate cancer cells in vitro (10). These findings may be useful in
elucidating potential prognostic markers. However, currently, very
little is known about the regulation of TLR9 expression and its
actual role in EC cells.
The purpose of the present study was to investigate
the expression of TLR9 in human EC cells and normal and malignant
esophageal squamous epithelium and to analyze its possible
association with EC invasion and prognosis. Therefore, we analyzed
the protein levels of TLR9 by immunohistochemical techniques,
western blotting, flow cytometric analysis. The mRNA levels of
tumor progression and migration-related factors such as matrix
metalloproteinase-2 (MMP-2), MMP-7 and cyclooxygenase-2 (COX-2)
were examined by reverse transcription-polymerase chain reaction
(RT-PCR). Furthermore, we performed MTT analysis and scratch assays
to examine the direct effects of cytosine phosphate guanosine
oligodinucleotide (CpG ODN), on tumor migration and the
proliferation of tumor cells to further characterize the possible
role of functional TLR9 expression in EC.
Materials and methods
Chemicals
The full phosphorothioated ODN 1816 (5′-TCCAT
GACGTTCCTGACGTT-3′) and primers were synthesized by SBS Genetech
(Beijing, China). The mouse monoclonal antibodies against
FITC-conjugated TLR9, TLR9, GAPDH, NF-κB and IgG2α isotype control
were purchased from Abcam (Beijing, China). Annexin V-FITC/PI kit
was obtained from Bender (Shenzhen, China). TRIzol, RPMI-1640 and
FBS were from Gibco (Shanghai, China). Chloroquine was purchased
from Sigma-Aldrich (Shanghai, China). Reverse transcription kit was
bought from TransGen Biotechnology (Beijing, China). BCA and ECL
kit were from Pierce (Shanghai, China).
Cell culture
TE10 cells were cultivated in RPMI-1640 medium
supplemented with 10% FBS, penicillin (100 U/ml) and streptomycin
(100 g/ml). Cells were maintained at 37°C in a humidified incubator
gassed with 95% O2 and 5% CO2.
RNA extraction and RT-PCR analysis
Total RNA was extracted from TE10 cells by TRIzol.
The purity and concentration of RNA was determined by
spectrophotometry at 260 and 280 nm. Complementary DNA (cDNA) was
synthesized using a reverse transcription kit. Quantitative PCR was
performed as follows: 94°C for 5 min, 35 cycles of denaturation at
94°C for 30 sec, annealing at 62°C for 30 sec, and extension at
72°C for 30 sec, and a single extension at 72°C for 5 min. Primers
used for the PCR were: TLR9: sense, 5′-GGACA CTCCCAGCTCTGAAG-3′ and
antisense, 5′-TTGGCTG TGGATGTTGTTGT-3′; MMP2: sense, 5′-CTTCCAAGT
CTGGAGCGATGT-3′ and antisense, 5′-TACCGTCAAAGG GGTATCCAT-3′; MMP7:
sense, 5′-CGGGGTACCATAATG TCCTGAATGATACC-3′ and antisense,
5′-CCCAAGCTTT GCCGTCCAGAGACAATTG-3′; COX-2: sense, 5′-GCCTGA
ATGTGCCATAAGACTGAC-3′ and antisense, 5′-AAA
CCCACAGTGCTTGACACAGA-3′; β-actin: sense, 5′-TGG CACCCAGCACAATGAA-3′
and antisense, 5′-CTAAGT CATAGTCCGCCTAGAAGCA-3′. PCR products were
applied to 1.5% agarose gel electrophoresis. The gel was scanned
and the electrophoresis image was input into Kodak gel image
analysis system.
Western blotting
Cells were washed with PBS three times and lysed
with RIPA buffer. The protein concentration was determined with BCA
kit according to the manufacturer’s instructions. Equal quantities
of protein were loaded and ran on SDS/polyacrylamide gels and then
transferred to a PVDF membrane. Membranes were blocked with 5%
dried milk and incubated with primary antibody of TLR9 in TBST
overnight at 4°C. After rinsing in milk-TBST, blots were incubated
in the horseradish peroxidase-conjugated secondary antibody. The
expression of TLR9 was detected by using the enhanced
chemiluminescence (ECL) detection system and X-ray films.
Flow cytometry
TE10 cells were detached with 0.05% trypsin/0.02%
EDTA and washed with cold PBS. For detection of TLR9 expression,
cells were fixed and permeabilized using the Cytofix/Cytoperm kit
according to the manufacturer’s instructions. Mouse anti-human TLR9
mAb or the appropriate isotypic IgG2a control mAb was performed at
0.5 mg/106 cells for 30 min on ice. After washing with
cold PBS, cells were stained with fluorescein (FITC)-conjugated
anti-mouse IgG. Cells were analyzed with a BD FACSCalibur flow
cytometer (BD Biosciences, San Jose, CA, USA) and gated using
forward vs. side scatter to exclude dead cells and debris.
Fluorescence of 104 cells per sample was acquired in
logarithmic mode for visual inspection of the distributions and in
linear mode for quantifying the expression of the relevant
molecules by calculating the mean fluorescence intensity with Cell
Quest Pro software.
Cell viability assay
Cells were seeded and grown on sterile 96-well
plates. The experimental cell concentration was 3×105/l.
Cells were pretreated with 10 μg/ml CpG ODN (TLR9 ligand) or CQ
(TLR9 inhibitor) for 1 h. Then, 10 μg/ml CpG ODN were added to the
cells and incubated for 12, 24 or 48 h. Cell growth was then
quantified using the MTT-based In Vitro Toxicology Assay
kit. A value was measured in a microplate reader at the wavelength
of 450 nm at 37°C incubated for 4 h.
Enzyme-linked immunosorbent assay
(ELISA)
TE10 cells were treated with 20 μg/ml CpG ODN for
12, 24 and 48 h. The supernatant was collected and the level of
NF-κB p65 in culture medium was quantified according to the
manufacturer’s directions. Absorbance was determined at 450 nm
using a microplate reader.
Scratch/(wound-healing) assay
TE10 cellular suspension at a concentration of
5×105/ml was inoculated into a 6-well culture plate at 2
ml per well, and cultured for 24 h. The medium was removed and
replaced by 20 μg/ml of CPG ODN 1816 culture medium or CQ with a
concentration of 100 or 200 μg/ml after the cells reached 80%
confluence. The supernatant was discarded and a wound (scratch) was
created. The wound was created in the confluent layer of cells
using a sterile scraping cutter and the ability of cells to heal
the wound was analyzed. The assays were documented using digital
photography.
Tissue samples and patients
The project was reviewed and approved by the Ethics
Committee of Ningxia Medical University. A total of 60 sections
resected by radical operation for esophageal carcinoma, which were
filed and randomly selected in the Department of Pathology, the
General Hospital of Ningxia Medical University from March 1992 to
September 2011. The other 30 sections from normal esophageal
tissues as control were from the same patients undergoing
esophageal surgery for the tumors but without cancer cell
infiltration. After fixation in 10% formalin and embedding in
paraffin, 5 μm serial sections were made for each specimen.
Immunohistochemical analysis
Tissue sections were de-waxed, soaked in alcohol,
and treated in antigen unmasking solution in the microwave for 10
min followed by incubation in 3% hydrogen peroxide for 10 min to
inactivate endogenous peroxidase activity. Sections were then
incubated at 4°C overnight with anti-TLR9 (1:100 dilution) primary
antibody. Immunostaining was performed by using the
Histostain™-Plus kit according to the manufacturer’s
instructions.
Statistical analysis
All experiments were replicated at least three times
on TE10 cells. All data are expressed as the means ± SD. Data were
analyzed by Student’s t-test and one-way ANOVA, and statistical
significance for comparison of means of different groups was
calculated using LSD-t analyses. P<0.05 was considered to
indicate a statistically significant difference.
Results
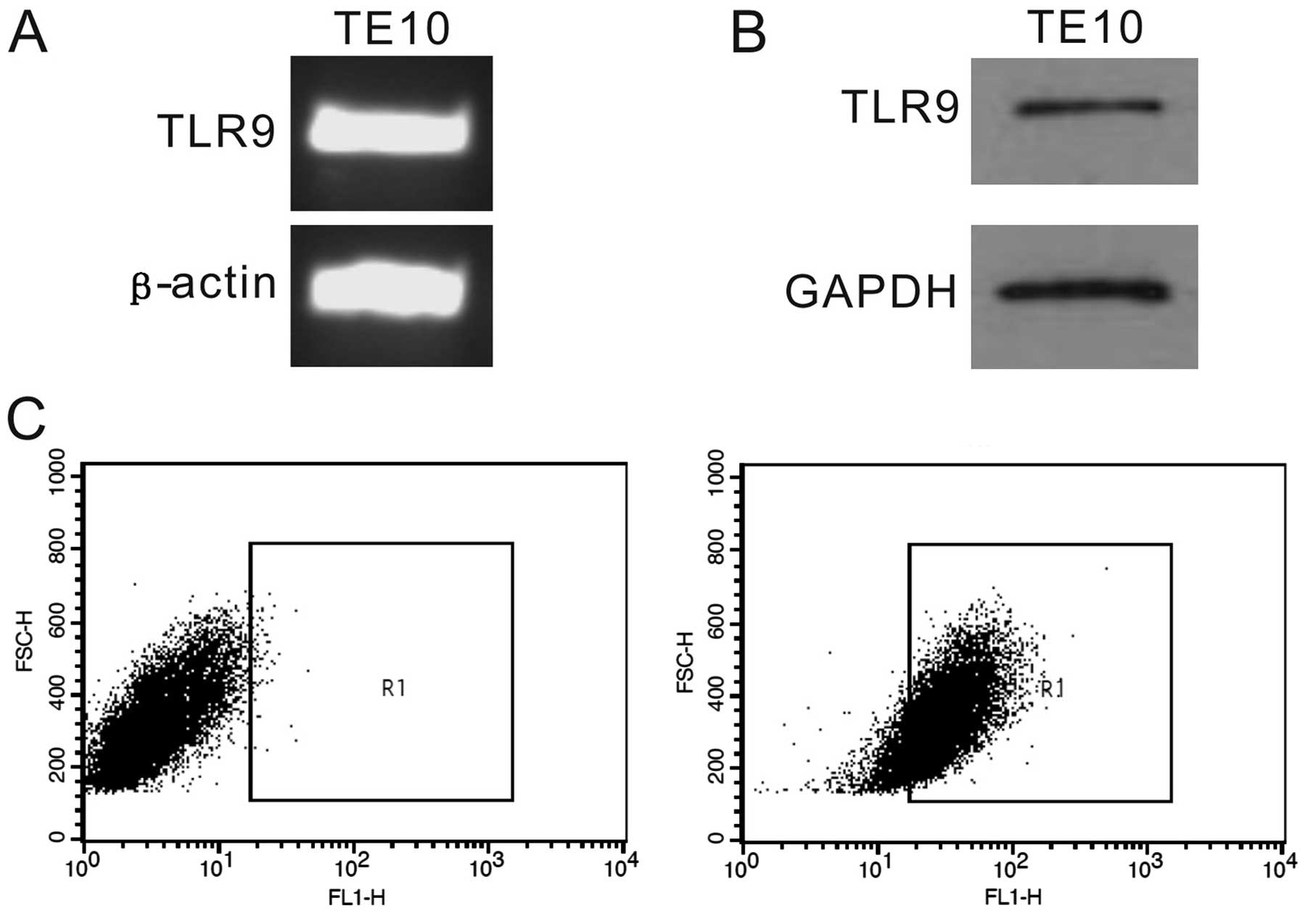
TLR9 expression in TE10 cells
The expression of TLR9 mRNA in EC cell line TE10 was
analyzed by RT-PCR (Fig. 1A). The
results revealed that TLR9 mRNA expressed in TE10 cells. To confirm
the RT-PCR findings, we further examined the protein level of TLR9
in TE10 cells by western blotting (Fig.
1B) and flow cytometric analysis (Fig. 1C). We found that TLR9 protein was
expressed in TE10 cells.
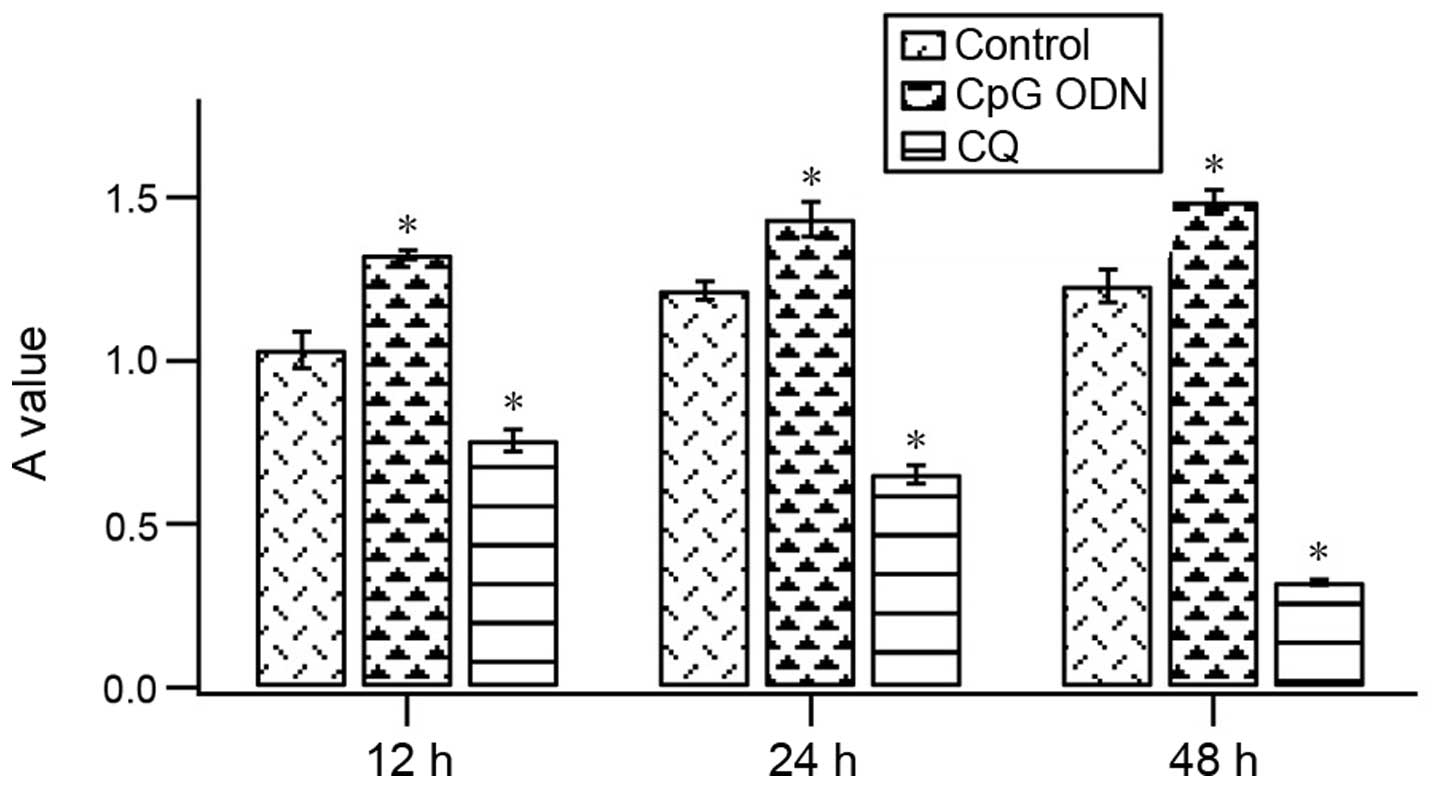
CpG ODN promotes TE10 cell growth
MTT assay was performed to investigate the effect of
CpG ODN and CQ on the proliferation of TE10 cells. When cells were
pretreated with 10 μg/ml CpG ODN or 10 μg/ml CQ, and then treated
with 10 μg/ml CpG ODN for 12, 24 or 48 h, the proliferation was
significantly promoted compared with the control groups (Fig. 2). However, when cells were
pretreated with TLR9 inhibitor CQ, the proliferation was not
enhanced by CpG ODN.
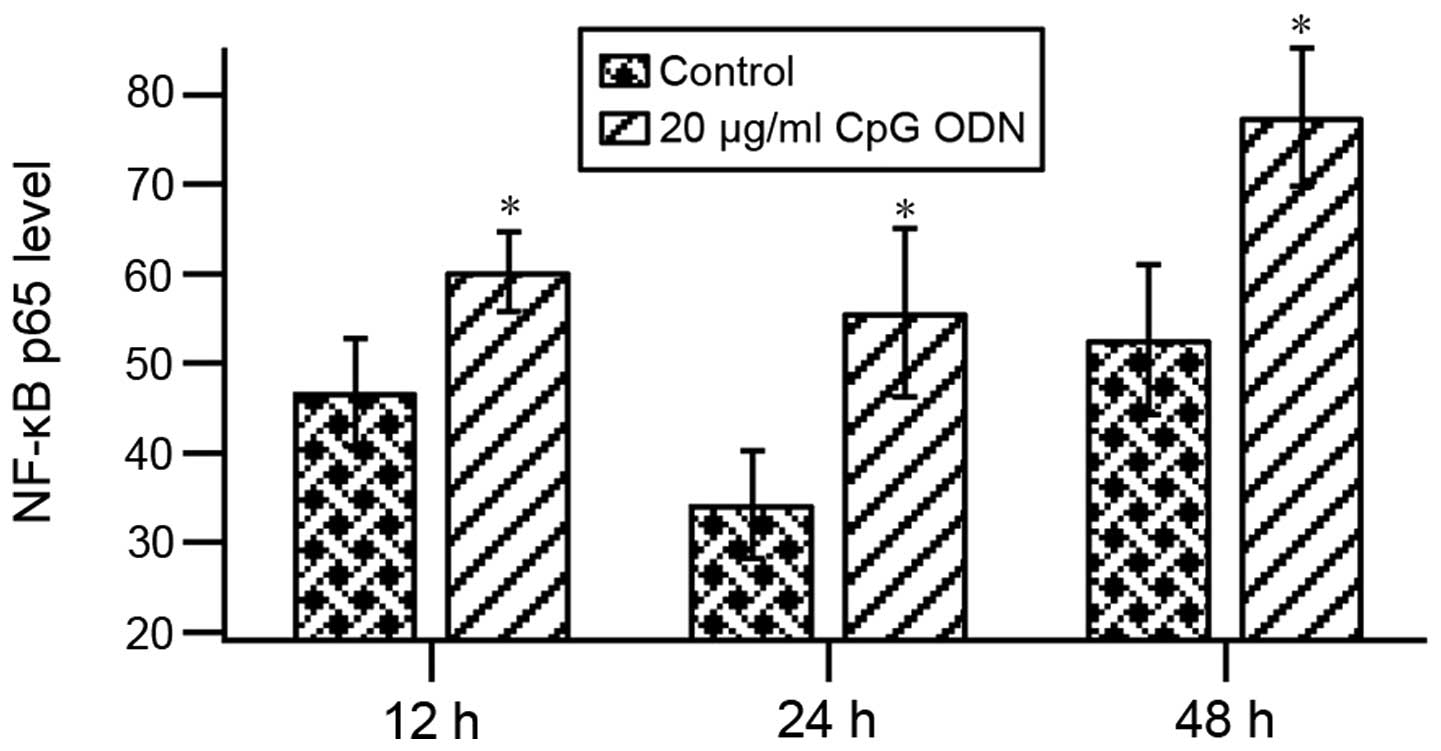
CpG ODN promotes NF-κB p65
expression
Upon the recognition of CpG ODN, TLR9 recruits
specific intracellular adaptor proteins such as NF-κB to initiate
signaling pathways. The ELISA assay was performed to evaluate the
activation of NF-κB. The results showed that NF-κB p65 expression
significantly increased at 12, 24 and 48 h of treatment of cells
with 20 μg/ml CpG ODN by comparison with untreated cells indicating
that CpG ODN activated NF-κB through the TLR9 signaling pathway
(Fig. 3).
CpG ODN promotes MMP-2, MMP-7 and COX-2
mRNA expression
NF-κB activation leads to upregulation of the
expression of many proinflammatory and apoptosis-related genes.
Therefore, we investigated the effects of TLR9 on the gene
expression of MMP-2, MMP-7 and COX-2 in TE10 cells treated with
different concentrations of TLR9 ligand CpG ODN and inhibitor CQ.
As shown in Fig. 4, the mRNA levels
of MMP-2, MMP-7 and COX-2 were markedly increased in TE10 cells
treated with CpG ODN, but were suppressed by CQ.
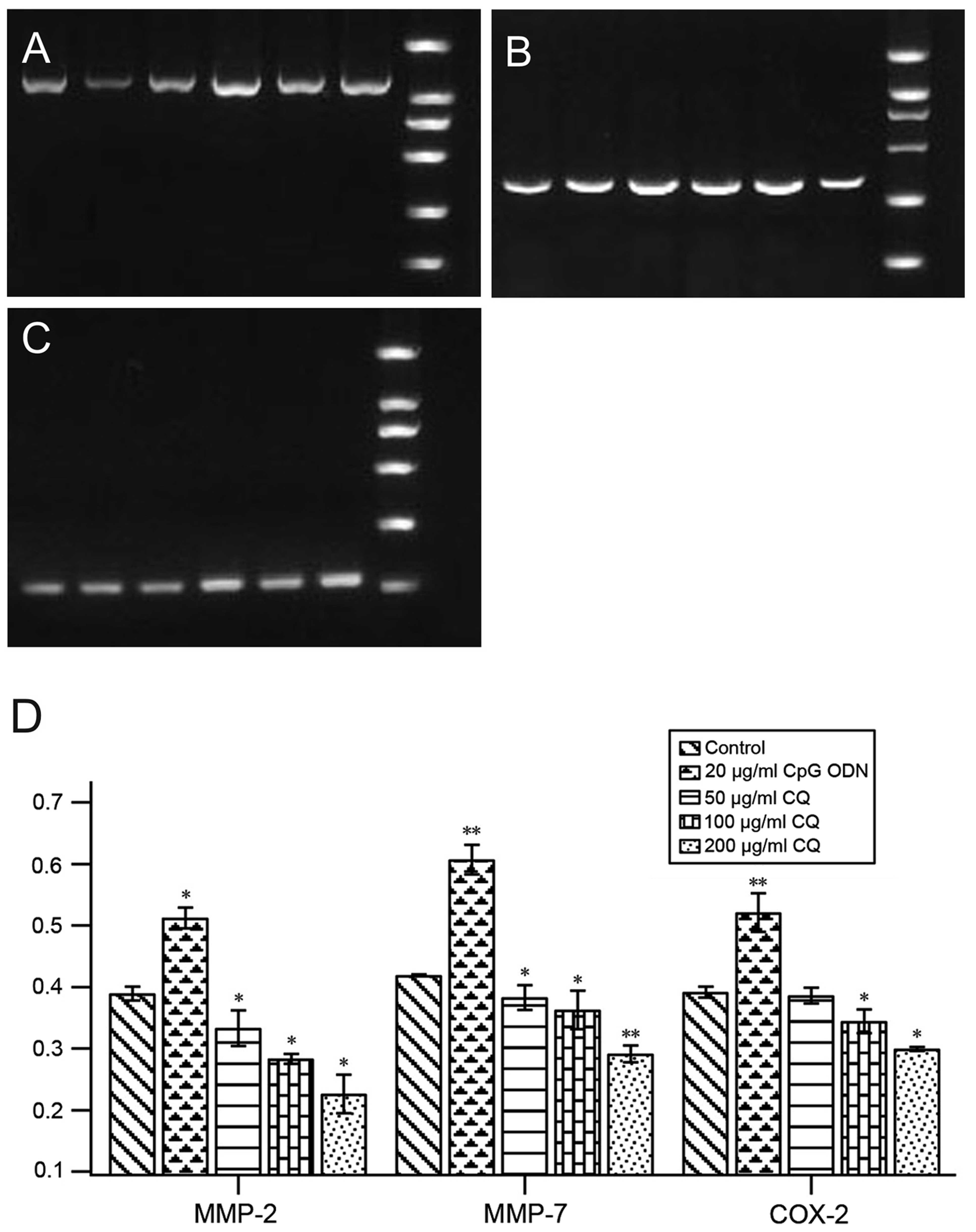 | Figure 4CpG ODN promotes mRNA levels of MMP-2,
MMP-7 and COX-2 as detected by RT-PCR. (A) MMP-2, (B) MMP-7, (C)
COX-2, (D) analyses of (A-C). From right: lane 1, marker; lane 2,
10 μg/ml CpG ODN; lane 3, 20 μg/ml CpG ODN; lane 4, 50 μg/ml CQ;
lane 5, 100 μg/ml CQ; lane 6, 200 μg/ml CQ. *P<0.05,
**P<0.01 compared with control. |
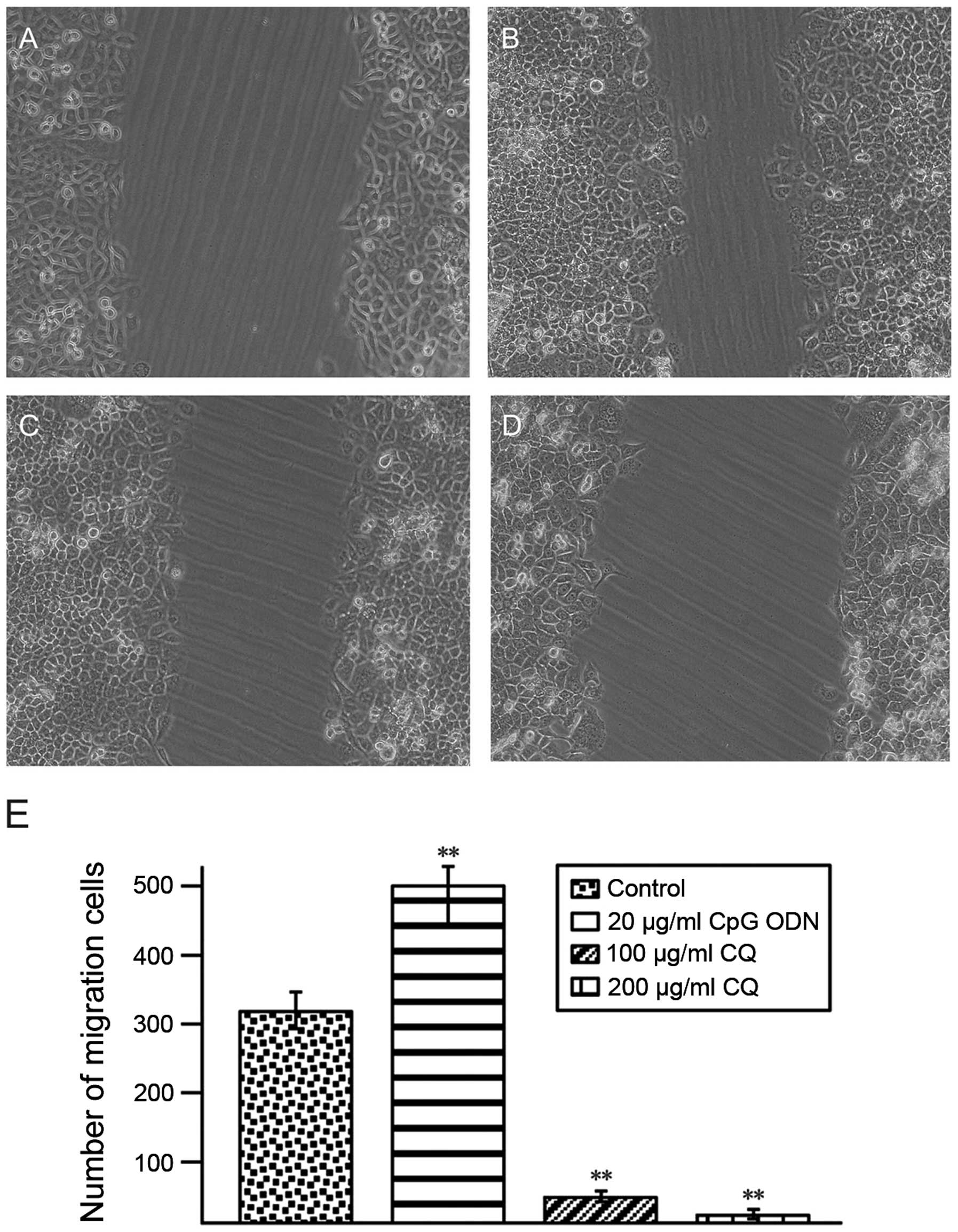
CpG ODN promotes TE10 cell migration
Cells scratch assay results showed that following
CpG ODN treatment, cell migration to the damage zone increased and
the migrated cell numbers after 48 h of treatment were markedly
increased (Fig. 5A). However, CQ
treatment inhibited TE10 cell migration (Fig. 5B and C).
TLR9 expression in human EC and its
association with EC clinicopathological characteristics
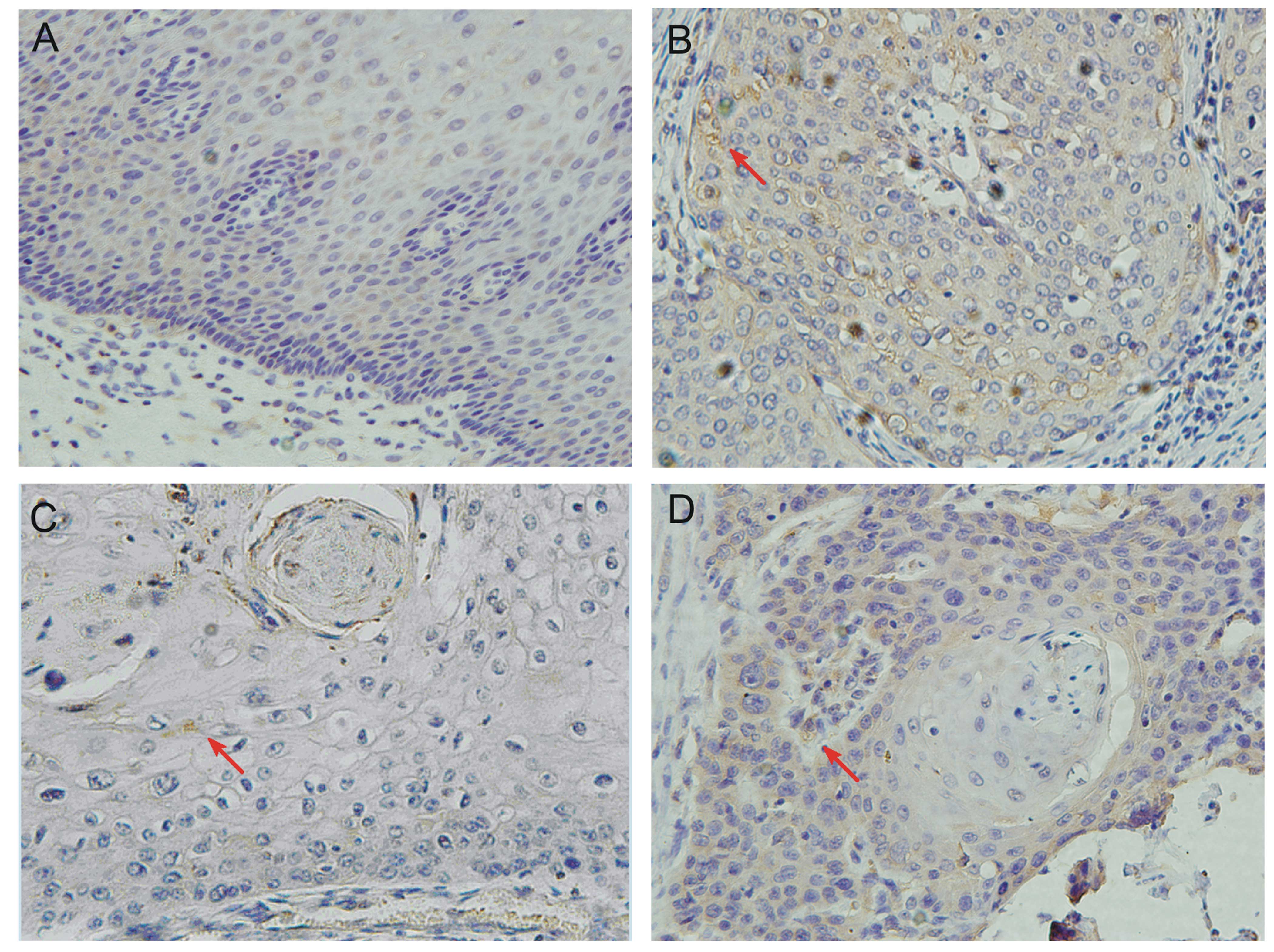
The expression of TLR9 in human EC tissues was
examined using immunohistochemical method. To determine the
prognostic value of TLR9 protein for EC patients, we assessed 60
esophageal carcinoma cases and 30 adjacent noncancerous tissues.
Tissue sections were dewaxed and immunostained with anti-TLR9
primary antibody. The results in Fig.
6 show that TLR9 expressed in both carcinoma tissues and
adjacent noncancerous tissues. However, among 60 esophageal
carcinoma tissues, TLR9 expression was found in 48 cases and the
positive expression rate was 80%. Among 30 adjacent noncancerous
tissues, TLR9 expression was found in 17 cases and the positive
expression rate was 56.7%. The positive rate in carcinoma tissues
was significantly higher than that in noncancerous tissues
(P<0.05). TLR9 protein located mainly in the cytoplasm and cell
surface (yellow and brown).
The clinicopathological analyses indicated that TLR9
expression in esophageal carcinoma was closely related to the
degree of tumor differentiation, tumor size, location, and Tumor
Node Metastasis (TNM) stage (P<0.05), and there was no
significant association with age, gender, lymph node metastasis of
patients (P>0.05) (Table I).
 | Table IStatistical analysis of TLR9
expression and clinicopathological factors in esophageal
carcinoma. |
Table I
Statistical analysis of TLR9
expression and clinicopathological factors in esophageal
carcinoma.
| Characteristics | Patients | TLR9 (+) n (%) | χ2 | P-value |
|---|
| Adjacent tissue
control | 30 | 17 (56.7%) | | |
| Esophageal
carcinoma | 60 | 48 (80%) | 5.428 | 0.02 |
| Age |
| ≥60 years | 38 | 29 (76.3%) | 1.103 | 0.294 |
| <60 years | 22 | 14 (63.6%) | | |
| Gender |
| Male | 37 | 25 (67.6%) | 0.799 | 0.371 |
| Female | 23 | 18 (78.3%) | | |
| Position |
| Upper
esophagus | 48 | 42 (87.5%) | 6.257 | 0.012 |
| Lower
esophagus | 12 | 6 (50.0%) | | |
| Tumor size |
| ≥5 cm | 27 | 14 (51.9%) | 4.848 | 0.028 |
| <5 cm | 33 | 26 (78.8%) | | |
| Tumor
metastases |
| Positive | 19 | 14 (73.7%) | 1.699 | 0.192 |
| Negative | 41 | 23 (56.1%) | | |
| Tumor stage |
| I/II | 36 | 21 (58.3%) | 4.159 | 0.041 |
| III/IV | 24 | 20 (83.3%) | | |
| Tumor
differentiation |
| Well and
moderately differentiated | 38 | 20 (52.6%) | 5.111 | 0.024 |
| Poorly
differentiated | 22 | 18 (81.8%) | | |
Discussion
The present study analyzed the significance of TLR9
expression in cultured esophageal tumor cells as well as esophageal
carcinoma tissues. We demonstrated that high basal level of TLR9 is
present in the EC cell line, TE10, consistent with its
overexpression and localization in esophageal carcinoma tissues,
indicating an association of TLR9 expression with invasion and
prognosis of EC.
TLR9 expression has been described in various cancer
cell lines and different human tumors (8–11). To
date, the association between TLR9 and clinicopathological
parameters of cancer patients has not been widely evaluated. Tanaka
et al demonstrated that cell surface stimulation of TLR9
promotes cell proliferation and survival in human hepatocellular
carcinoma (12). TLR9 expression
has been shown to be significantly higher in high grade gliomas
compared to low-grade gliomas (13). In breast cancer, it has been shown
that the mRNA and protein levels of TLR9 significantly increased in
recurrent breast carcinomas cells (14,15).
It has been reported that the gene of TLR9 is correlated with the
invasive and metastatic potential of human pancreatic carcinoma
(16). In lung cancers, TLR9 was
found to express in a selection of human lung cancer tissues and
various lung tumor cell lines (17). These findings suggest that high TLR9
expression and TLR9 signaling promote tumor growth, survival and
immune evasion (18). Thus, in this
study, we investigated the possible role of TLR9 in EC. Firstly, we
measured the TLR9 expression in EC TE10 cells by western blotting,
RT-PCR and flow cytometric techniques. The results from different
methods showed that TLR9 expressed in TE10 cells. The results were
consistent in three experiments. The MTT assay showed that CpG ODN
could promote EC cell proliferation and TLR9 inhibitor CQ could
suppress this effect of CpG ODN. In a scratch assay, TE10 cell
migration to heal a scratched area on the plate surface was
measured. The data showed that CpG ODN treatment markedly enhanced
cell migration, but CQ treatment inhibited cell migration. The data
suggest a role of TLR9 in EC cell proliferation and migration.
TLR9 recognizes the ODN with CpG motif. Accumulating
data indicated that TLR9 agonist CpG ODN can promote tumor
development and metastasis (8–11,19).
It has been proven that in TLR9 knockout mice, microbial DNA
fragments cannot result in cancer invasion (20). It was also shown that the
immunomodulating effect of natural and synthetic ODNs is mainly
transmitted by TLR9 (21). After
binding with CpG ODN, TLR9 signal pathway leads to the downstream
activation of NF-κB and MAPK signaling pathways (22,23),
which may upregulate the expression of proinflammatory and
apoptosis-related genes. Thus, in this study, we investigated the
effect of CpG ODN on NF-κB expression in EC TE10 cells. We found
that CpG ODN could markedly activate NF-κB p65 expression by
comparison with untreated cells. The results indicated that CpG ODN
activates the NF-κB signaling pathway by binding to TLR9 in EC
cells.
Next, we examined the mRNA levels of three
downstream genes of NF-κB pathway upon CpG ODN treatment. MMPs are
members of the neutral proteinase family. They were previously
thought to be anti-fibrotic due to their ability to degrade and
remodel of extracellular matrix. However, recent studies have shown
that MMPs are implicated in tumor progression and migration
(24–26). MMP-2 is a member of the
metalloproteinase family, which degrades various components of the
extracellular matrix (27). MMP-2
has been shown to be important in development and cell motility,
and has an important role in cancer metastasis (28,29).
MMP-7 is a highly active MMP family member, which can activate
other family members, such as MMP-2 and MMP-9, and play a central
role in the degradation of the extracellular matrix (30). It also inhibits apoptosis of cancer
cells, reduces cell adhesion and induces angiogenesis, making it
easier for the cancer cells to invade small blood vessels and
lymphatic tube and metastasize (31,32).
COX-2 has been extensively studied as an inducible expression
protein and has been detected in various tumor tissues such as
pancreatic cancer, colorectal carcinoma, non-small lung cancer
positively correlates with tumor invasion and lymphatic metastasis
(33,34). We then detected the effects of CpG
ODN and CQ on mRNA expression of MMP-2, MMP-7 and COX-2. The
results showed that CpG ODN increased MMP-2, MMP-7 and COX-2 mRNA
expression and CQ inhibited their expression as expected indicating
that CpG ODN may bind to TLR9, and then activates NF-κB, so to
upregulate MMP-2, MMP-7 and COX-2 gene expression. However, the
actual roles of these three factors in EC require further
study.
Lastly, the expression of TLR9 in human EC tissues
was examined and its association with EC clinicopathological
characteristics was analyzed. In the present study, TLR9 highly
expressed in carcinoma tissues but weakly expressed in adjacent
noncancerous esophageal tissues. Similarly, Droemann et al
found TLR9 highly expressed in lung cancer cells but weakly
expressed in adjacent noncancerous lung tissues (17). In esophageal carcinomas, extensive
TLR9 expression was associated with high tumor grade and TNM stage,
but not with age, gender, lymph node metastasis of patients.
Extensive TLR9 expression and association with poor differentiation
has also been noted in breast and prostate cancer, which is
consistent with our results (14,35).
To date, there are very few reports on TLR9 expression in EC.
Kauppila et al reported that high TLR9 expression was
associated with poor differentiation, a high proliferation rate and
increased TLR9 expression contributed to the growth and metastatic
properties of esophageal adenocarcinoma (36). A study by Heikki et al showed
that expression of TLR9 in the basal parts of normal esophageal
epithelium related to cell proliferation and differentiation, and
in dysplastic epithelium and in disseminated carcinomas indicated
that TLR9 may serve as a novel marker for esophageal squamous
dysplasia and carcinoma with metastatic potential (37).
In summary, we showed that TLR9 is highly expressed
in cultured EC cells and in esophageal carcinoma tissues. CpG ODN
could bind to TLR9 thus markedly activate NF-κB p65 expression and
three cancer metastasis-related genes. In esophageal carcinomas,
extensive TLR9 expression associated with high tumor grade and
tumoral aggressiveness. Therefore, TLR9 might contribute to
esophageal squamous cell carcinogenesis and may represent a
suitable therapeutic target in EC. However, the mechanisms of the
upregulation of TLR9 in esophageal malignancy require further
investigation.
Acknowledgements
We thank all the members of the Immunology
Laboratory for their help. This study was supported by Ningxia
Natural Science Foundation Program (NZ11100); Fund of Ningxia
Department of Education [(2010)297] and Ningxia Medical University
Doctor Open Issue (KF2010-39). This study was also supported by the
National Natural Science Foundation of China (grant nos. 31060140
and 31260243). The Project Sponsored by the Scientific Research
Foundation for the Returned Overseas Chinese Scholars, State
Education Ministry and the Program for New Century Excellent
Talents in University (NCET), State Education Ministry for Dr Yin
Wang.
References
|
1
|
He J, Gu D, Wu X, Reynolds K, Duan X, Yao
C, Wang J, Chen CS, Chen J, Wildman RP, Klag MJ and Whelton PK:
Major causes of death among men and women in China. N Engl J Med.
353:1124–1134. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Fukata M and Abreu MT: Pathogen
recognition receptors, cancer and inflammation in the gut. Curr
Opin Pharmacol. 9:680–687. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Takeda K and Akira S: Microbial
recognition by Toll-like receptors. J Dermatol Sci. 34:73–82. 2004.
View Article : Google Scholar
|
|
4
|
Underhill DM: Toll-like receptors:
networking for success. Eur J Immunol. 33:1767–1775. 2003.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Barton GM and Medzhitov R: Toll-like
receptor signaling pathways. Science. 300:1524–1525. 2003.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Takeda K, Kaisho T and Akira S: Toll-like
receptors. Annu Rev Immunol. 21:335–376. 2003. View Article : Google Scholar
|
|
7
|
Wagner H: The immunobiology of the TLR9
subfamily. Trends Immunol. 25:381–386. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Merrell MA, Ilvesaro JM, Lehtonen N, Sorsa
T, Gehrs B, Rosenthal E, Chen D, Shackley B, Harris KW and Selander
KS: Toll-like receptor 9 agonists promote cellular invasion by
increasing matrix metalloproteinase activity. Mol Cancer Res.
4:437–447. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Berger R, Fiegl H, Goebel G, Obexer P,
Ausserlechner M, Doppler W, Hauser-Kronberger C, Reitsamer R, Egle
D, Reimer D, Müller-Holzner E, Jones A and Widschwendter M:
Toll-like receptor 9 expression in breast and ovarian cancer is
associated with poorly differentiated tumors. Cancer Sci.
101:1059–1066. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Ilvesaro JM, Merrell MA, Swain TM,
Davidson J, Zayzafoon M, Harris KW and Selander KS: Toll like
receptor-9 agonists stimulate prostate cancer invasion in vitro.
Prostate. 67:774–781. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Ren T, Xu L, Jiao S, Wang Y, Cai Y, Liang
Y, Zhou Y, Zhou H and Wen Z: Tlr9 signaling promotes tumor
progression of human lung cancer cell in vivo. Pathol Oncol Res.
15:623–630. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Tanaka J, Sugimoto K, Shiraki K, Tameda M,
Kusagawa S, Nojiri K, Beppu T, Yoneda K, Yamamoto N, Uchida K,
Kojima T and Takei Y: Functional cell surface expression of
toll-like receptor 9 promotes cell proliferation and survival in
human hepatocellular carcinomas. Int J Oncol. 37:805–814.
2010.PubMed/NCBI
|
|
13
|
Wang C, Cao S, Yan Y, Ying Q, Jiang T, Xu
K and Wu A: TLR9 expression in glioma tissues correlated to glioma
progression and the prognosis of GBM patients. BMC Cancer.
10:415–426. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Jukkola-Vuorinen A, Rahko E, Vuopala KS,
Desmond R, Lehenkari PP, Harris KW and Selander KS: Toll-like
receptor-9 expression is inversely correlated with estrogen
receptor status in breast cancer. J Innate Immun. 1:59–68. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
González-Reyes S, Marín L, González L,
González LO, del Casar JM, Lamelas ML, González-Quintana JM and
Vizoso FJ: Study of TLR3, TLR4 and TLR9 in breast carcinomas and
their association with metastasis. BMC Cancer. 10:665–673.
2010.PubMed/NCBI
|
|
16
|
Wu HQ, Wang B, Zhu SK, Tian Y, Zhang JH
and Wu HS: Effects of CPG ODN on biological behavior of PANC-1 and
expression of TLR9 in pancreatic cancer. World J Gastroenterol.
17:996–1003. 2011.PubMed/NCBI
|
|
17
|
Droemann D, Albrecht D, Gerdes J, Ulmer
AJ, Branscheid D, Vollmer E, Dalhoff K, Zabel P and Goldmann T:
Human lung cancer cells express functionally active Toll-like
receptor 9. Respir Res. 6:1–10. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Zeromski J, Mozer-Lisewska I and Kaczmarek
M: Significance of Toll-like receptors expression in tumor growth
and spreading: a short review. Cancer Microenviron. 1:37–42. 2008.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Jurk M and Vollmer J: Therapeutic
applications of synthetic CpG oligodeoxynucleotides as TLR9
agonists for immune modulation. BioDrugs. 21:387–401. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Hemmi H, Takeuchi O, Kawai T, Kaisho T,
Sato S, Sanjo H, Matsumoto M, Hoshino K, Wagner H, Takeda K and
Akira S: A Toll-like receptor recognizes bacterial DNA. Nature.
408:740–745. 2000. View
Article : Google Scholar : PubMed/NCBI
|
|
21
|
Takeshita F, Gursel I, Ishii KJ, Suzuki K,
Gursel M and Klinman DM: Signal transduction pathways mediated by
the interaction of CpG DNA with Toll-like receptor 9. Semin
Immunol. 16:17–22. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Kuo CC, Kuo CW, Liang CM and Liang SM: A
transcriptomic and proteomic analysis of the effect of CpG-ODN on
human THP-1 monocytic leukemia cells. Proteomics. 5:894–906. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Kostjuk S, Loseva P, Chvartatskaya O,
Ershova E, Smirnova T, Malinovskaya E, Roginko O, Kuzmin V,
Izhevskaia V, Baranova A, Ginter E and Veiko N: Extracellular
GC-rich DNA activates TLR9- and NF-κB-dependent signaling pathways
in human adipose-derived mesenchymal stem cells (haMSCs). Expert
Opin Biol Ther. 12(Suppl 1): S99–S111. 2012.PubMed/NCBI
|
|
24
|
Zhao H, Dong Y, Tian X, Tan TK, Liu Z,
Zhao Y, Zhang Y, Harris DCh and Zheng G: Matrix metalloproteinases
contribute to kidney fibrosis in chronic kidney diseases. World J
Nephrol. 2:84–89. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Folgueras AR, Pendas AM, Sanchez LM and
Lopez-Otin C: Matrix metalloproteinases in cancer: from new
functions to improved inhibition strategies. Int J Dev Biol.
48:411–424. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Zeng ZS, Cohen AM and Guillem JG: Loss of
basement membrane type IV collagen is associated with increased
expression of metalloproteinases 2 and 9 (MMP-2 and MMP-9) during
human colorectal tumorigenesis. Carcinogenesis. 20:749–755. 1999.
View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Bartsch JE, Staren ED and Appert HE:
Matrix metalloproteinase expression in breast cancer. J Surg Res.
110:383–392. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Jezierska A and Motyl T: Matrix
metalloproteinase-2 involvement in breast cancer progression: a
mini-review. Med Sci Monit. 15:RA32–RA40. 2009.PubMed/NCBI
|
|
29
|
Sims JD, McCready J and Jay DG:
Extracellular heat shock protein (Hsp)70 and Hsp90 alpha assist in
matrix metalloproteinase-2 activation and breast cancer cell
migration and invasion. PLoS One. 6:e188482011. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Lee KH, Shin SJ, Kim KO, Kim MK, Hyun MS,
Kim TN, Jang BI, Kim SW, Song SK, Kim HS, Bae SH and Ryoo HM:
Relationship between E-cadherin, matrix metalloproteinase-7 gene
expression and clinicopathological features in gastric carcinoma.
Oncol Rep. 16:823–830. 2006.PubMed/NCBI
|
|
31
|
Okayama H, Kumamoto K, Saitou K, Hayase S,
Kofunato Y, Sato Y, Miyamoto K, Nakamura I, Ohki S, Sekikawa K and
Takenoshita S: CD44v6, MMP-7 and nuclear Cdx2 are significant
biomarkers for prediction of lymph node metastasis in primary
gastric cancer. Oncol Rep. 22:745–755. 2009.PubMed/NCBI
|
|
32
|
Yeh YC, Sheu BS, Cheng HC, Wang YL, Yang
HB and Wu JJ: Elevated serum matrix metalloproteinase-3 and -7 in
H. pylori-related gastric cancer can be biomarkers
correlating with a poor survival. Dig Dis Sci. 55:1649–1657.
2010.PubMed/NCBI
|
|
33
|
Sugie S, Tsukino H, Mukai S, Akioka T,
Shibata N, Nagano M and Kamoto T: Cyclooxygenase 2 genotypes
influence prostate cancer susceptibility in Japanese men. Tumour
Biol. Nov 8–2013.(Epub ahead of print).
|
|
34
|
Lu J, Li XF, Kong LX, Ma L, Liao SH and
Jiang CY: Expression and significance of cyclooxygenase-2 mRNA in
benign and malignant ascites. World J Gastroenterol. 19:6883–6887.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Vaisanen MR, Vaisanen T, Jukkola-Vuorinen
A, Vuopala KS, Desmond R, Selander KS and Vaarala MH: Expression of
Toll-like receptor-9 is increased in poorly differentiated prostate
tumors. Prostate. 70:817–824. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Kauppila JH, Takala H, Selander KS,
Lehenkari PP, Saarnio J and Karttunen TJ: Increased Toll-like
receptor 9 expression indicates adverse prognosis in esophageal
adenocarcinoma. Histopathology. 59:643–649. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Heikki T, Kauppila JH, Soini Y, Selander
KS, Vuopala KS, Lehenkari PP, Saarnio J and Karttunen TJ: Toll-like
receptor 9 is a novel biomarker for esophageal squamous cell
dysplasia and squamous cell carcinoma progression. J Innate Immun.
3:631–638. 2011. View Article : Google Scholar : PubMed/NCBI
|