Introduction
Medulloblastoma (MB) is the most prevalent pediatric
central nervous system malignancy (1). The MB classification process has
evolved from relying solely on histopathological features to the
integration of molecular characteristics (2). The current international consensus
recognizes four MB subgroups: Wingless (WNT), Sonic hedgehog (SHH),
group 3 and group 4; which are based on distinctive-omic and
clinical features (2,3). Somatic CTNNB1 mutations and
chromosome 6 loss are common in the WNT subgroup (4), while the amplification of GLI1
or GLI2 and the deletion of Patched 1 (PTCH1) are
frequently observed in the SHH subgroup (5). Aberrant MYC amplification can
be detected in ~17% of patients with group 3 MB and is considered a
defining feature of this subgroup (1). In addition, isochromosome 17q has
been found in almost two-thirds of group 4 MB cases, and has been
associated with cell division protein kinase (CDK)6 and
MYCN amplification (6).
Despite considerable advances being made in the
understanding of the molecular characteristics of MB, the current
treatments for this disease are limited to maximal safe surgical
resection, chemotherapy and cranio-spinal irradiation (1). Molecularly targeted therapy for MB
remains in its infancy (7).
Furthermore, although the overall survival rates have improved in
recent years, a number of survivors suffer from chronic sequelae,
such as neurological and neuropsychological disabilities, resulting
in a poor quality of life for these children (8). In addition to the effect of the tumor
itself, another main cause of these sequelae is the treatments with
a high toxicity rate, particularly for patients in the very
high-risk group who inevitably receive high-intensity therapeutic
regimens (1). Instead of
indiscriminately acting on all rapidly dividing cells (not only
cancer cells, but also certain normal cells), targeted cancer
therapies focusing on interfering with specific molecules involved
in oncogenesis hold the promise of being less toxic than
traditional chemoradiotherapy (9).
Therefore, developing more targeted therapeutic strategies for MB
may prove to be instrumental in curtailing the adverse effects of
conventional therapies.
In the present study, datasets comprising MB and
normal brain samples from the Gene Expression Omnibus database
(GEO) were analyzed and a set of hub genes with a significantly
upregulated expression in MB was identified. In addition, two MB
cell lines, Daoy and D341 belonging to SHH and group 3,
respectively (10), were used to
investigate the potential of one identified hub gene [PDZ-binding
kinase (PBK)], as a therapeutic target for the treatment of
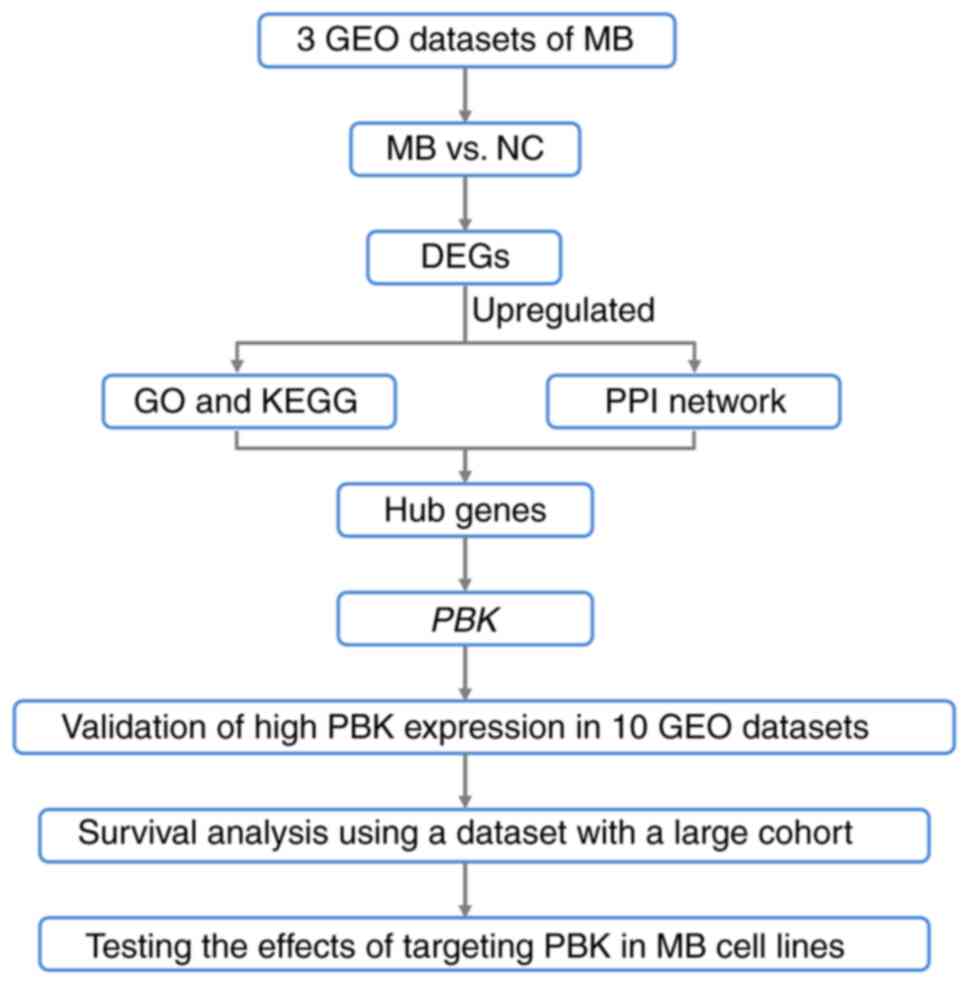
MB (please see the flow chart in Fig.
1).
Materials and methods
Identification of differentially
expressed genes (DEGs)
RNA-seq and microarray data were retrieved from the
GEO database (http://www.ncbi.nlm.nih.gov/geo/). Microarray data
comprised GSE35493 (based on Affymetrix Human Genome U133 Plus 2.0
Array, GPL570) (11) and GSE39182
(based on Agilent-014850 Whole Human Genome Microarray 4×44K
G4112F, GPL6480) (12). GSE35493
included 21 MB and 9 normal brain samples. GSE39182 included 20 MB
and 5 normal samples. In addition, RNA-seq data GSE148389 (based on
NextSeq 550, GPL21697) contained 14 normal and 26 tumor tissues
(13). All probes were annotated
by annotation files. Data processing was performed using R 3.6.0
software (https://www.r-project.org/). DEGs
between MB and normal samples in the GSE35493 and GSE39182
microarray datasets were screened using the Limma package (14), and GSE148389 RNA-seq data were
analyzed using the edgeR package (15). An adjusted P<0.05 and |log2 fold
change (FC)|≥1 were set as thresholds to identify the DEGs. Venn
diagrams (http://bioinformatics.psb.ugent.be/webtools/Venn/)
were utilized to detect and present the common DEGs among the three
datasets.
GO and KEGG pathway analyses of
upregulated DEGs
Gene Ontology (GO) and Kyoto Encyclopedia of Genes
and Genomes (KEGG) pathway enrichment analyses were performed using
the Database for Annotation, Visualization and Integrated Discovery
(DAVID, http://davidd.ncifcrf.gov/), which is
a database which can be used for processing functional annotation
with gene lists (16). The DEG
results were entered to obtain the enrichment of the biological
process, molecular function and cellular component terms of GO
analysis and KEGG pathway terms. A P<0.05 was considered to
indicate a statistically significant difference.
Protein-protein interaction (PPI)
network construction and identification of hub genes
To assess the functional associations among the
upregulated DEGs, the Search Tool for the Retrieval of Interacting
Genes (STRING, http://string-db.org/) database was
used to construct the PPI network of DEGs (17). Interactions with a combined score
>0.4 were considered significant. The PPI network was then
visualized using Cytoscape (version 3.8.0; http://cytoscape.org/) (18). Subsequently, hub genes among the
upregulated DEGs were identified using the Cytoscape plugin
cytoHubba. The top 10 hub genes were calculated according to the
maximal clique centrality (MCC) algorithm in cytoHubba (19).
Expression analysis of the hub gene,
PBK, and survival analysis
At the beginning of the present study, a number of
datasets comprising MB and normal brain samples were downloaded
following a search of the GEO database. GSE35493, GSE39182 and
GSE148389 were selected to identify DEGs between MB and normal
samples as these three datasets had relatively larger sample sizes
and were based on different platforms, which was considered
beneficial for obtaining more DEGs. The remaining datasets were
then used as validation sets to verify the high expression level of
PBK in MB, including GSE74195 (20), GSE50161 (21), GSE42656 (22), GSE19360 (23), GSE109401 (24), GSE86574 (25) and GSE62600 (26). PBK expression in the four MB
subgroups was also examined in datasets GSE85217 (27), GSE37418 (28) and GSE21140 (29). To date, only a few MB datasets
contain survival information, of which GSE85217 is the one with the
largest cohort, and the sample size of other datasets is too small
to conduct the survival analysis for four subgroups. Therefore, the
prognostic values of PBK were tested in GSE85217 with the
clinical data of a large cohort of patients with MB (27). Survival curves were drawn using
Graphpad Prism 9 (GraphPad Software, Inc.). Survival analysis was
completed using the Kaplan-Meier method and overall survival was
analyzed using the log-rank test.
MB cell lines and cell culture
The Daoy (HTB-186) and D341 (HTB-187) MB cell lines
were obtained from the American Type Culture Collection (ATCC).
Daoy cells were cultured in Dulbecco's modified Eagle's medium
(DMEM; cat. no. C11995, Gibco; Thermo Fisher Scientific, Inc.)
supplemented with 10% fetal bovine serum (FBS; cat. no. 10270-106,
Gibco; Thermo Fisher Scientific, Inc.), 1% penicillin/streptomycin
(P/S; cat. no. 15140-122, Gibco; Thermo Fisher Scientific, Inc.)
and 1% non-essential amino acid (NEAA; cat. no. 11140-035, Gibco;
Thermo Fisher Scientific, Inc.). D341 cells were cultured in DMEM
(cat. no. C11995; Gibco; Thermo Fisher Scientific, Inc.)
supplemented with 20% FBS, 1% P/S and 1% NEAA. Both cell lines were
maintained under a 95% O2 and 5% CO2
humidified atmosphere in an incubator at 37°C. The PBK inhibitor,
HI-TOPK-032, was purchased from MedChemExpress (cat. no.
HY-101550).
Western blot analysis
MB cells were plated at a density of
8.5×105 cells in 100-mm cell culture dishes and
harvested following treatment with HI-TOPK-032 for 48 h. Daoy cells
were treated at 0 (vehicle, DMSO), 1, 2 or 4 µM and D341 cells were
treated at 0, 1 or 2 µM. Cells were lysed using RIPA lysis buffer
(cat. no. P0013B; Beyotime Institute of Biotechnology), and the
protein concentrations were determined using the BCA kit (cat. no.
P0012; Beyotime Institute of Biotechnology). Proteins were then
separated using SDS-PAGE (10% gel for PBK, ERK1/2, Akt and
β-tubulin; 12% gel for cleaved caspase-3 and GAPDH) and transferred
to PVDF membranes (Merck Millipore). The membranes were blocked in
5% bovine serum albumin (cat. no. CCS30014.01, MRC, EN MOASAI
Biological Technology Co., Ltd.) for 1 h at room temperature, and
incubated overnight at 4°C with the following primary antibodies:
Anti-PBK (1:1,000; cat. no. 4942S, Cell Signaling Technology,
Inc.), anti-phosphorylated (p-)p44/42 MAPK (ERK1/2) (Thr202/Tyr204,
1:1,000; cat. no. AF1015, Affinity Biosciences), anti-p44/42 MAPK
(ERK1/2) (1:1,000, cat. no. BF8004, Affinity Biosciences),
anti-p-Akt (Ser473, 1:1,000, cat. no. T56569, Abmart Pharmaceutical
Technology Co., Ltd.), anti-Akt (1:1,000, cat. no. T55561, Abmart
Pharmaceutical Technology Co., Ltd.), anti-cleaved caspase-3
(1:500, cat. no. ab32042, Abcam), anti-β-tubulin (1:5,000, cat. no.
AP0064, Bioworld Technology, Inc.) and anti-GAPDH (1:2,000, cat.
no. TA-08, OriGene Technologies, Inc.). Subsequently, the membranes
were incubated with secondary antibodies (peroxidase-conjugated
goat anti-rabbit IgG, 1:5,000; cat. no. ZB-2301, or
peroxidase-conjugated goat anti-mouse IgG, 1:5,000, cat. no.
ZB-2305; both from OriGene Technologies, Inc.) for 1 h at room
temperature. After washing, the membranes were visualized using an
enhanced chemiluminescence reagent (Merck Millipore) and a Tanon
5200 Chemiluminescent Imaging System. Gel densities were measured
using ImageJ software (Version 1.53m, National Institutes of
Health).
Reverse transcription-quantitative PCR
(RT-qPCR)
Total RNA was extracted using TRIzol®
reagent (cat. no. 15596026, Thermo Fisher Scientific, Inc.) and the
RNA concentrations were assayed using a NanoDrop 2000
spectrophotometer (Thermo Fisher Scientific, Inc.). cDNA was
synthesized using reverse transcription kits (FastKing gDNA
Dispelling RT SuperMix; cat. no. KR118, Tiangen Biotech, Co., Ltd.)
according to the manufacturer's thermocycler guidelines (the
reaction setup comprised of 4 µl of 5X FastKing-RT SuperMix and 1
µg of total RNA, and the final volume was made up to 20 µl with
RNase-Free ddH2O; temperature protocol: 15 min at 42°C
for gDNA removing and reverse transcription followed by 3 min at
95°C for enzyme inactivation). The sequences of the PCR primer
pairs were as follows: PBK forward, CCAAACATTGTTGGTTATCGTGC
and reverse, GGCTGGCTTTATATCGTTCTTCT; and actin beta (ACTB)
forward, CATGTACGTTGCTATCCAGGC and reverse, CTCCTTAATGTCACGCACGAT.
qPCR was then performed according to the manufacturer's
instructions [one cycle of initial denaturation at 95°C for 3 min,
40 cycles of PCR (5 sec at 95°C for denaturation and 15 sec at 60°C
for annealing/extension), and ended with a melting/dissociation
curve stage (15 sec at 95°C, 1 min at 60°C and 1 sec at 95°C)] at a
final volume of 20 µl/well using SYBR-Green Talent qPCR Premix (10
µl; cat. no. FP209, Tiangen Biotech, Co., Ltd.), forward and
reverse primers (0.6 µl, Sangon Biotech, Co., Ltd.), cDNA (1 µl/50
ng), ROX Reference Dye (0.4 µl, Tiangen Biotech, Co., Ltd.) and
RNase-Free ddH2O (7.4 µl, Tiangen Biotech, Co., Ltd.).
The reaction was performed on the Applied Biosystems QuantStudio 3
Real-Time PCR System (Applied Biosystems; Thermo Fisher Scientific,
Inc.). In each run, the expression levels of PBK were
normalized to those of ACTB as a housekeeping gene [i.e.,
the expression level of ACTB was set as 1; the ΔCq value was
calculated as follows: ΔCq=Cq(PBK)-Cq(ACTB); the
difference in the expression level between PBK and
ACTB was 2ΔCq-fold and the expression level of
PBK was then normalized as 1/2ΔCq].
Cytotoxicity and cell proliferation
assay
The Cell Counting Kit-8 (CCK-8; cat. no. GK10001,
Glpbio Technology Inc.) assay was used to detect the viability of
the control and HI-TOPK-032-treated cells. The Daoy and D341 cells
were seeded in 96-well plates at a density of 2,000 and 10,000
cells per well in 100 µl of culture medium, respectively. For the
cytotoxicity assays, the cells were treated with HI-TOPK-032 at 0
(vehicle, DMSO), 0.5, 1, 1.5, 2, 2.5 and 3 µM. Following treatment
for 24 h (Daoy cells) or 72 h (D341 cells), 10 µl of CCK-8 solution
was added to each well followed by incubation for 3 h. The
absorbance values were measured using an ELX808 microplate reader
(BioTek Instruments, Inc.) at a wavelength of 450 nm. Cell
viability was calculated using the absorbance value of the treated
groups divided by the absorbance value of the control groups and
multiplied by 100%. Sigmoidal dose-response curves were fitted
using non-linear regression in Graphpad Prism 9 (GraphPad Software,
Inc.) to determine the IC50 values. For the cell
proliferation assay, the absorbance values were measured following
treatment with HI-TOPK-032 at 0, 1 or 2 µM for 0, 24, 48, or 72
h.
5-Ethynyl-2′-deoxyuridine (EdU)
assays
The cells were plated in 96-well plates at a density
of 5,000 (Daoy cells) and 10,000 (D341 cells) cells per well and
treated with HI-TOPK-032 at 0, 1 or 2 µM. Following incubation at
37°C for 24 h, EdU assay was performed using a Click EdU cell
proliferation kit with Alexa Fluor 594 (cat. no. C0078, Beyotime
Institute of Biotechnology) according to the manufacturer's
protocol. Images were obtained using an ECLIPSE Ti2-E inverted
microscope (Nikon Corporation) and the percentage of EdU-positive
cells was quantified using ImageJ software (Version 1.53m; National
Institutes of Health).
Apoptosis assay
The MB cells were seeded at a density of
1×105 cells in 60-mm cell culture dishes and treated
with HI-TOPK-032 at 0, 2 (D341 cells) or 4 µM (Daoy cells) for 24
h. The cells were then collected and washed twice with PBS followed
by staining with Annexin V-APC/7-AAD (Apoptosis Detection kit; cat.
no. KGA1017, Nanjing KeyGen Biotech Co., Ltd.) and Hoechst 33342
(cat. no. C1027, Beyotime Institute of Biotechnology) at room
temperature for 10 min protected from light. After staining, the
cells were transferred to a 24-well plate and fluorescence
microscopy images were obtained using an ECLIPSE Ti2-E inverted
microscope (Nikon Corporation). Positive cells were quantified
using ImageJ software (Version 1.53m; National Institutes of
Health).
Statistical analysis
Statistical analyses were performed using GraphPad
Prism 9 (GraphPad Software Inc.). All experiments were repeated
three times. Quantitative results are presented as the mean ±
standard deviation (SD). Statistically significant differences were
assessed using an unpaired Student's t-test, one-way or two-way
ANOVA with Tukey's HSD post hoc test. A value of P<0.05 was
considered to indicate a statistically significant difference.
Results
Identification of upregulated hub
genes in MB
The present study first screened for genes
differentially expressed between MB and normal brain samples to
identify potential therapeutic targets in MB. Following RNA-seq and
microarray data analyses, differential mRNA expression between MB
and normal samples in three datasets was found (Fig. 2A). In GSE148389, 6,906 DEGs were
identified (3,216 upregulated and 3,690 downregulated genes). In
GSE35493, 5,568 DEGs were determined (2,793 upregulated and 2,775
downregulated genes). In GSE39182, 2,405 DEGs were detected (818
upregulated and 1,587 downregulated genes). Venn diagrams presented
the overlapping DEGs in the three datasets. A total of 282
upregulated and 436 downregulated genes were identified as common
between the three datasets (Fig.
2B).
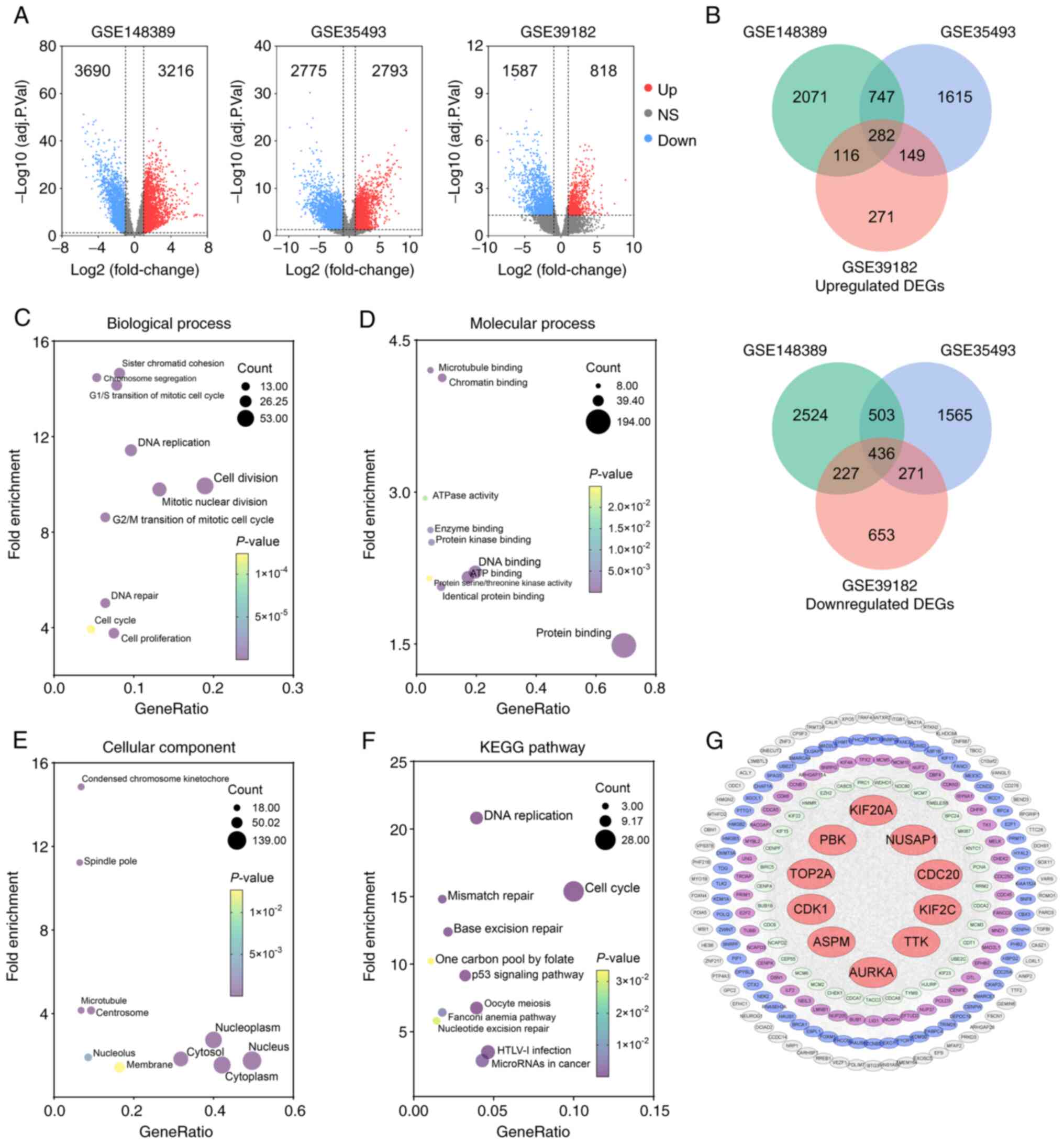 | Figure 2.Identification of upregulated hub
genes in MB following enrichment analysis and protein-protein
interaction network construction. (A) Volcano plots illustrating
upregulated DEGs (red dots) and downregulated DEGs (blue dots)
identified in the three datasets with the criteria of adjusted
P<0.05 and |log2FC| ≥1 (11–13).
(B) Venn diagram of overlapping upregulated or downregulated DEGs
among three datasets. (C-E) GO analysis of upregulated DEGs
presents the top 10 significant terms of GO analysis in (C)
biological process, (D) molecular function, and (E) celluar
component. (F) Significant KEGG pathway enrichment terms. (G) The
PPI network was constructed with upregulated genes. Red circular
nodes represent the top 10 hub genes. MB, medulloblastoma; DEGs,
differentially upregulated genes; GO, Gene Ontology; KEGG, Kyoto
Encyclopedia of Genes and Genomes; PPI, protein-protein
interaction; PBK, PDZ binding kinase; CDC20, cell division cycle
20; KIF2C, kinesin family member 2C; NUSAP1, nucleolar and spindle
associated protein 1; TTK, TTK protein kinase; KIF20A, kinesin
family member 20A; TOP2A, DNA topoisomerase II alpha; CDK1, cyclin
dedendent kinase 1; ASPM, assembly factor for spindle microtubules;
AURKA, Aurora kinase A. |
Subsequently, the upregulated DEGs were submitted to
DAVID to examine their functions and potential roles in the
molecular tumorigenesis of MB. Following the enrichment analysis,
the top 10 significant terms of GO analysis in three categories
(biological process, molecular function and cellular component) and
the significant KEGG enrichment terms were screened. In biological
process, the upregulated genes were associated predominately with
cell division, mitotic nuclear division, DNA replication and the
G2/M transition of mitosis (Fig.
2C). In molecular function, the upregulated genes were involved
primarily in protein binding, DNA binding and ATP binding (Fig. 2D). In addition, the cytosol,
cytoplasm, nucleus and nucleoplasm were significantly associated
with upregulated genes in the cellular component (Fig. 2E). The KEGG pathway analysis
revealed that upregulated genes were enriched, particularly in DNA
replication and the cell cycle (Fig.
2F).
To further investigate the functional associations
among the upregulated DEGs, the STRING online database was utilized
to analyze the PPI network of these genes. After removing isolated
and partially connected nodes, a grid network was constructed using
Cytoscape software (Fig. 2G). The
Cytoscape plugin cytoHubba was then exploited to determine the hub
genes in the PPI network. Finally, the top 10 hub genes [cell
division cycle 20 (CDC20), kinesin family member 2C
(KIF2C), nucleolar and spindle associated protein 1
(NUSAP1), PBK, TTK protein kinase (TTK), kinesin
family member 20A (KIF20A), DNA topoisomerase II alpha
(TOP2A), CDK1, assembly factor for spindle
microtubules (ASPM) and Aurora kinase A (AURKA)] were
determined using the MCC algorithm in cytoHubba (Fig. 2G).
Validation of the high expression and
prognostic significance of the hub gene, PBK, in MB
According to the GO and KEGG pathway analysis, the
upregulated genes were predominantly enriched in the cell cycle,
DNA replication and cell division. Among the top 10 hub genes,
PBK encodes PDZ-binding kinase, also known as
T-lymphokine-activated killer (T-LAK) cell-originated protein
kinase (TOPK), which is a serine/threonine protein kinase belonging
to the mitogen-activated protein kinase kinase (MAPKK) family and
plays a vital role in mitotic progression (30,31).
Furthermore, researchers have previously reported that PBK is
highly expressed in cerebellar granule cell precursors of early
postnatal mice and functions as a crucial regulator of progenitor
proliferation and self-renewal (32). Thus, given that MBs are embryonal
tumors originating from stem cells or progenitor cells in the
cerebellum or posterior fossa (33), the present study focused on the
possible role of PBK in MB. The significant upregulation of PBK was
first verified in MB by interrogating and analyzing additional
independent gene expression datasets, including data from patients
with MB (GSE74195, GSE50161 and GSE42656) and a spontaneous mouse
model of MB (GSE19360) (Fig.
3A-D).
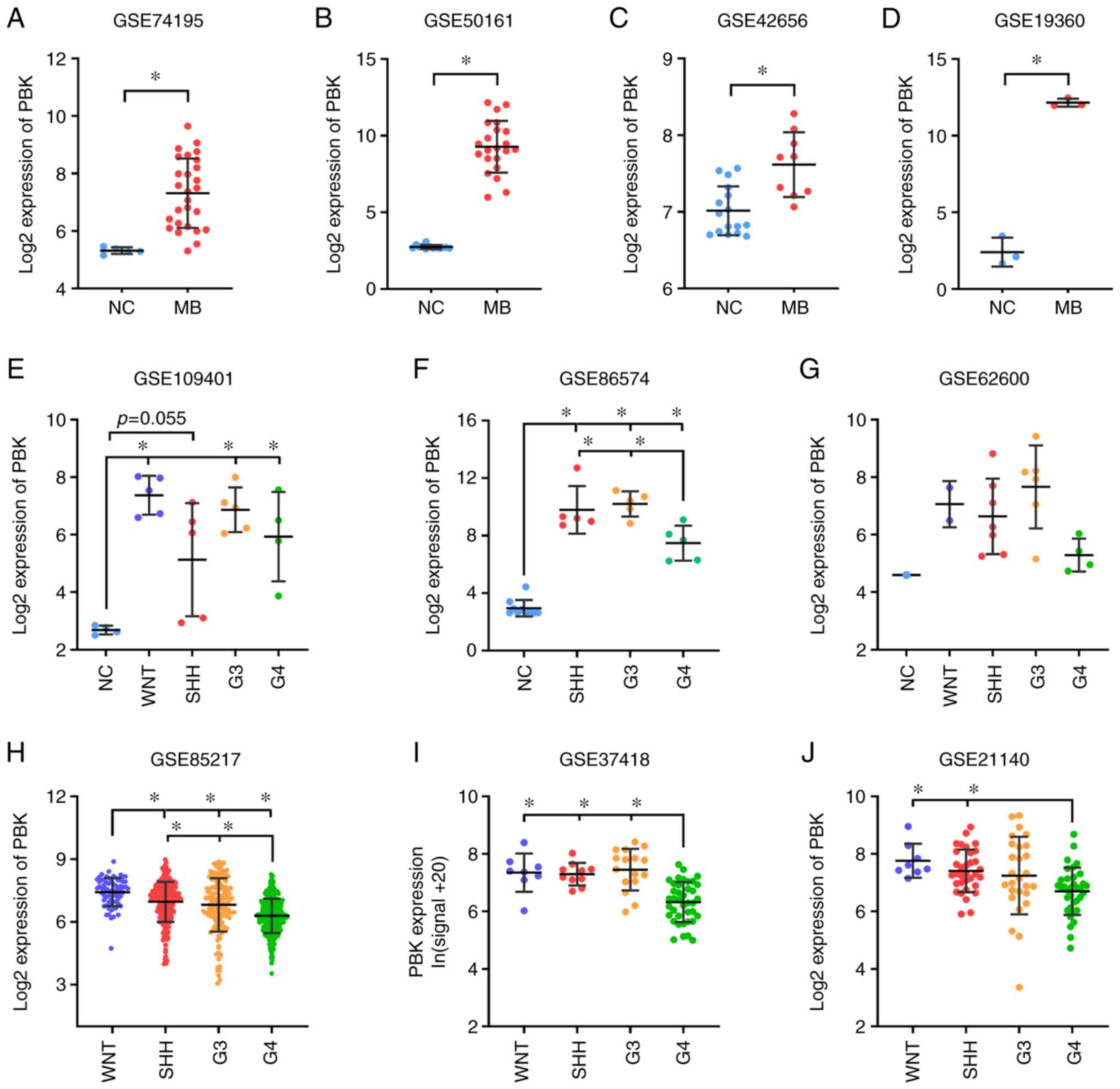 | Figure 3.Validation of the aberrant expression
of the hub gene, PBK, in MB. (A-D) Significant upregulation of PBK
in MB relative to normal brain control examined in expression
datasets GSE74195 (27 MB vs. 5 NC) (20), GSE50161 (22 MB vs. 13 NC) (21), GSE42656 (16 MB vs. 9 NC) (22) and GSE19360 (3 MB vs. 3 NC)
(23). (E-G) PBK was highly
expressed in all MB subgroups compared with normal brain tissue.
Sample size: GSE109401 (4 NC, 5 WNT, 5 SHH, 5 G3, 4 G4) (24), GSE86574 (10 NC, 5 SHH, 5 G3, 5 G4)
(25) and GSE62600 (1 NC, 2 WNT, 7
SHH, 6 G3, 4 G4) (26). (H-J) PBK
expression varied among MB subgroups, with group 4 MBs appearing to
have the lowest expression level. Sample size: GSE85217 (70 WNT,
223 SHH, 144 G3, 326 G4) (27),
GSE37418 (8 WNT, 10 SHH, 16 G3, 39 G4) (28) and GSE21140 (8 WNT, 33 SHH, 27 G3,
35 G4) (29). Quantitative results
are presented as the mean ± SD. Statistical significance was
determined using (A-D) an unpaired Student's t test or (E-J)
one-way ANOVA with Tukey's HSD post hoc test. *P<0.05. MB,
medulloblastoma; PBK, PDZ binding kinase; NC, normal control; WNT,
Wingless; SHH, Sonic hedgehog; G3, group 3; G4, group 4. |
Since MB is currently divided into four subgroups,
the expression level of PBK was also examined in the different
subgroups. Of note, PBK was highly expressed in all MB subgroups
compared with normal brain samples (Fig. 3E-G), suggesting that PBK may be
involved in the tumorigenesis of all subgroups. This is consistent
with the function of PBK as a mitotic serine/threonine kinase and
the rapid proliferating rate of MB cells. In addition, PBK
expression varied among the MB subgroups, with group 4 MBs
appearing to have the lowest expression level compared to the other
subgroups (Fig. 3H-J).
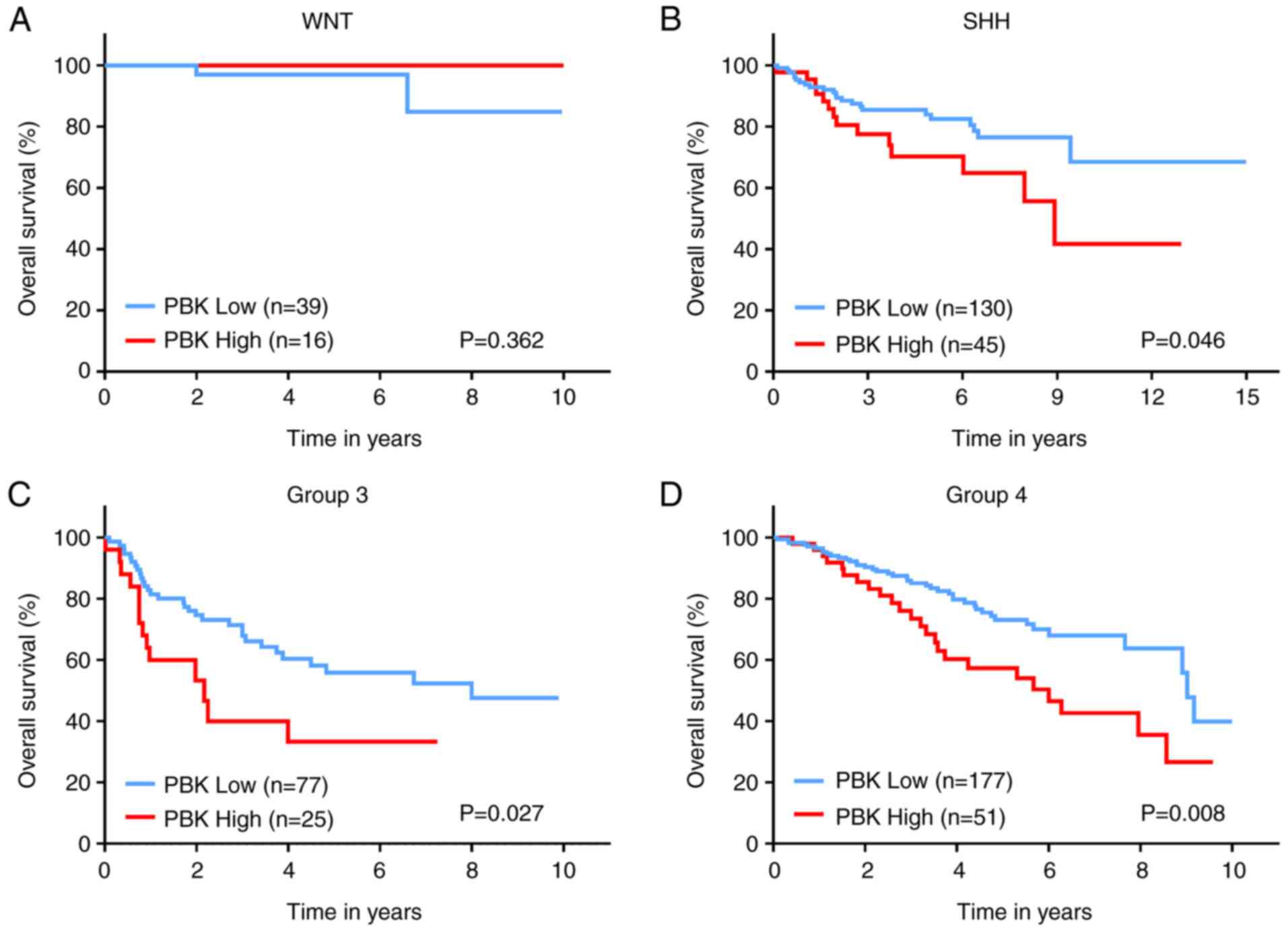
Subsequently, the prognostic significance of PBK in MB was assessed
by analyzing the survival information of patients with MB from a
large cohort. The overall survival curves revealed that a high PBK
expression was significantly associated with poorer clinical
outcomes in SHH, group 3 and group 4 MBs, apart from WNT MB
(Fig. 4). Taken together, these
results indicate that PBK is a crucial upregulated hub gene
in MB and is likely to serve as a prognostic marker.
Targeting PBK inhibits the
proliferation of MB cells and reduces the phosphorylation of
downstream signaling molecules
To further examine the potential of PBK as a
therapeutic target for MB, two commonly used MB cell lines, Daoy
and D341 belonging to the SHH and group 3 respectively, were
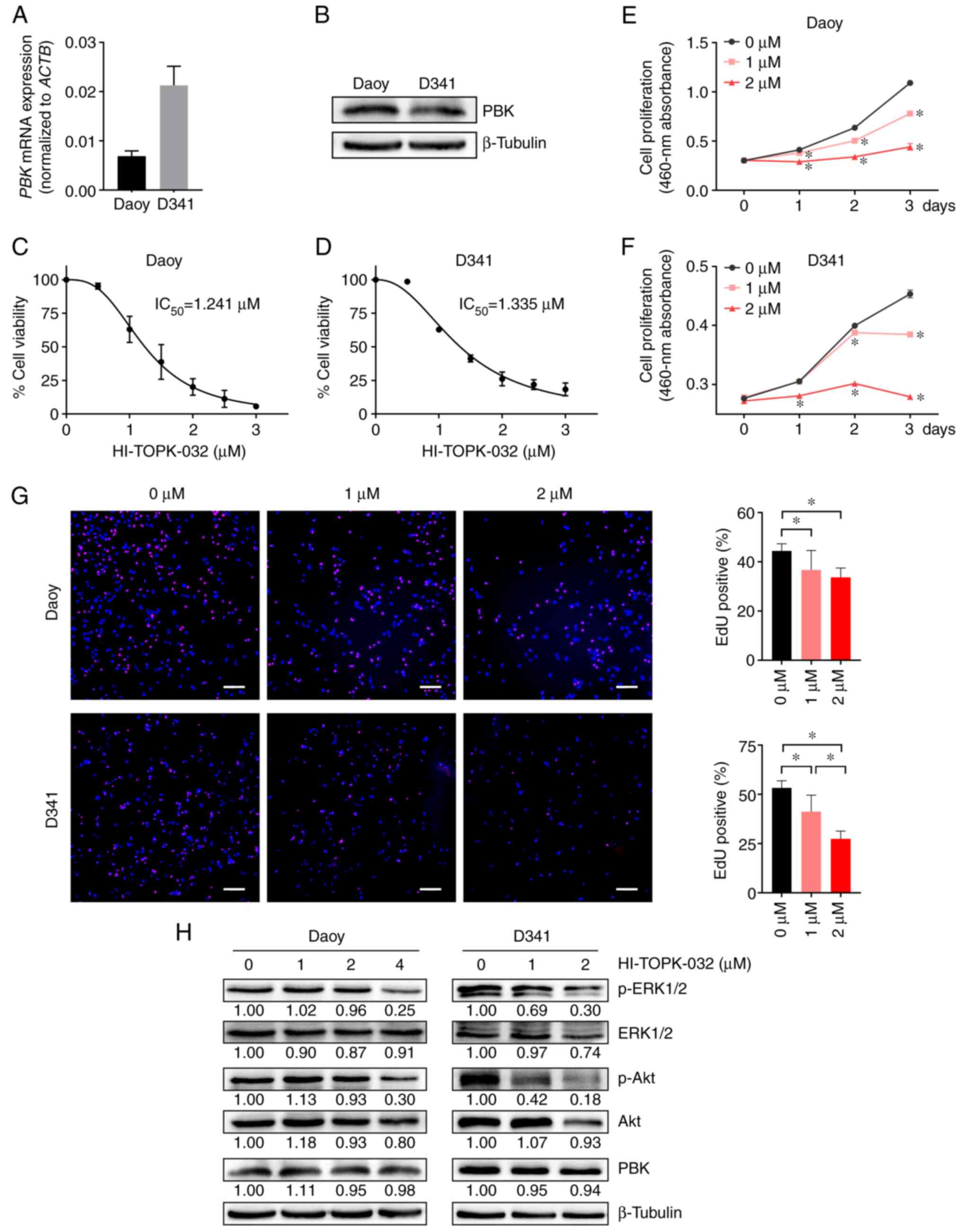
employed to perform experiments in vitro. First, PBK
expression was detected in Daoy and D341 cells using RT-qPCR and
western blot analysis. The results revealed that both cell lines
had a robust expression of PBK (Fig.
5A and B). While the D341 cells exhibited a higher PBK mRNA
expression, the Daoy cells appeared to have a higher protein
expression, suggesting that the translation efficiency of PBK may
differ between the two cell lines. However, this inconsistency may
also be caused by the different reference genes (housekeeping
genes) used in the two assays. The MB cells were then treated with
a widely-used PBK inhibitor (HI-TOPK-032) to observe its effects on
cell viability and proliferation. In the CCK-8 assay, the viability
of the Daoy and D341 cells was effectively inhibited by HI-TOPK-032
in a concentration dependent manner with an IC50 value
of 1.241 and 1.335 µM, respectively (Fig. 5C and D). Moreover, HI-TOPK-032 also
markedly decreased MB cell growth in a manner dependent on the
degree of PBK suppression, as shown in Fig. 5E and F. Consistently, the two MB
cell lines treated with HI-TOPK-032 at a concentration of 1 or 2 µM
exhibited a lower proliferation rate than the control group in the
EdU assay (Fig. 5G). These data
demonstrated that targeting PBK with its specific inhibitor
significantly impaired the proliferation of MB cells in
vitro.
The present study then examined the phosphorylation
status of two critical downstream targets of PBK to elucidate the
mechanisms underlying the effects of HI-TOPK-032 on MB cell
proliferation. Western blot analysis revealed that treatment with
the PBK inhibitor, HI-TOPK-032, resulted in a slight or moderate
reduction in the total levels of downstream signaling molecules,
including ERK1/2 and Akt (Fig.
5H). However, a considerable decrement in the phosphorylated
form of downstream proteins was observed in the HI-TOPK-032-treated
MB cells (Fig. 5H). These two
signaling molecules have been reported as essential downstream
effectors of PBK in regulating cell proliferation (34,35).
Additionally, the level of PBK in the MB cells remained stable
following HI-TOPK-032 treatment (Fig.
5H), in accordance with previous studies (36,37).
Taken together, these results suggest that HI-TOPK-032 may inhibit
the proliferation of MB cells by suppressing the phosphorylation of
downstream target proteins of PBK by blocking its kinase
activity.
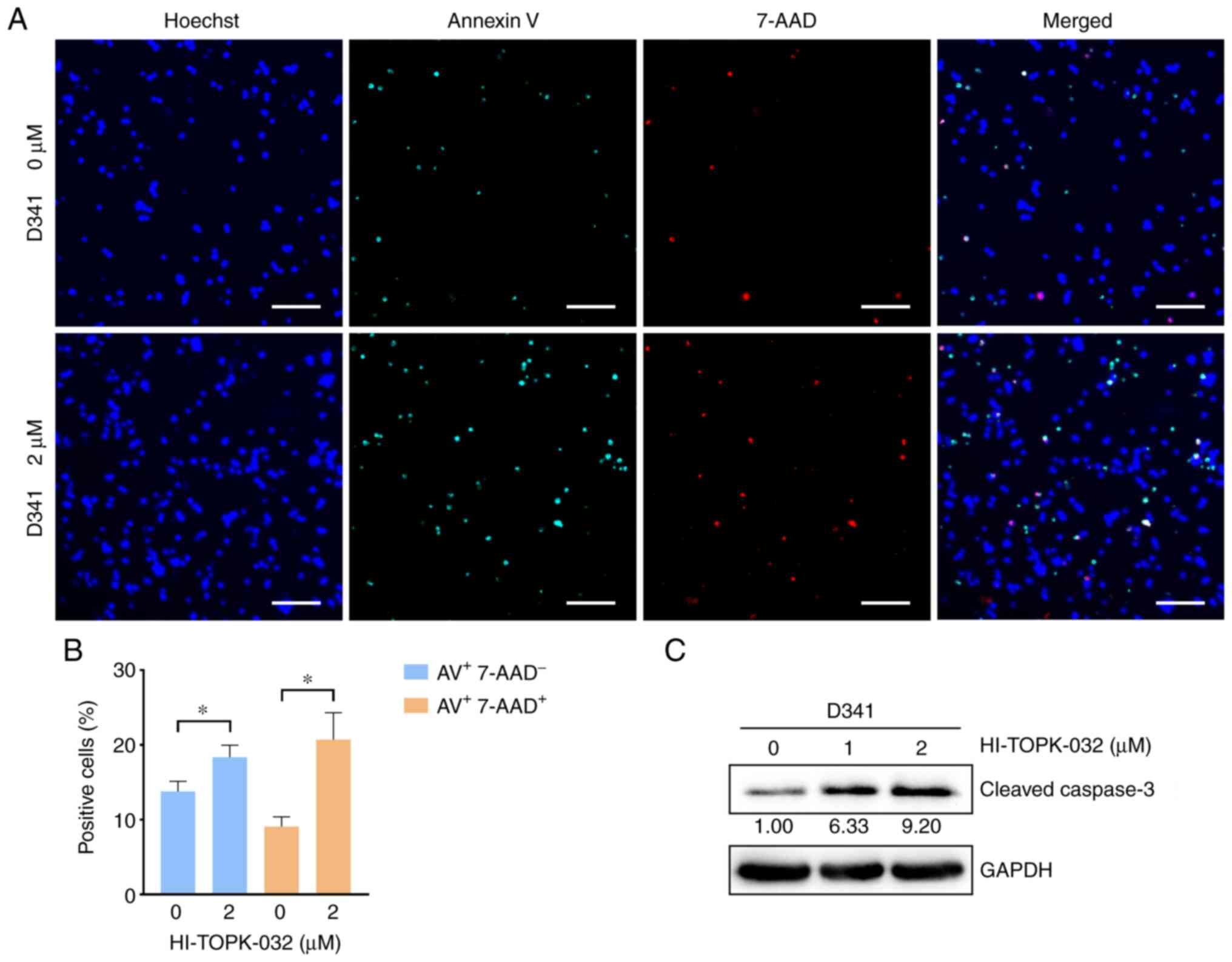
PBK inhibitor HI-TOPK-032 promotes the
apoptosis of MB cells with the activation of caspase-3
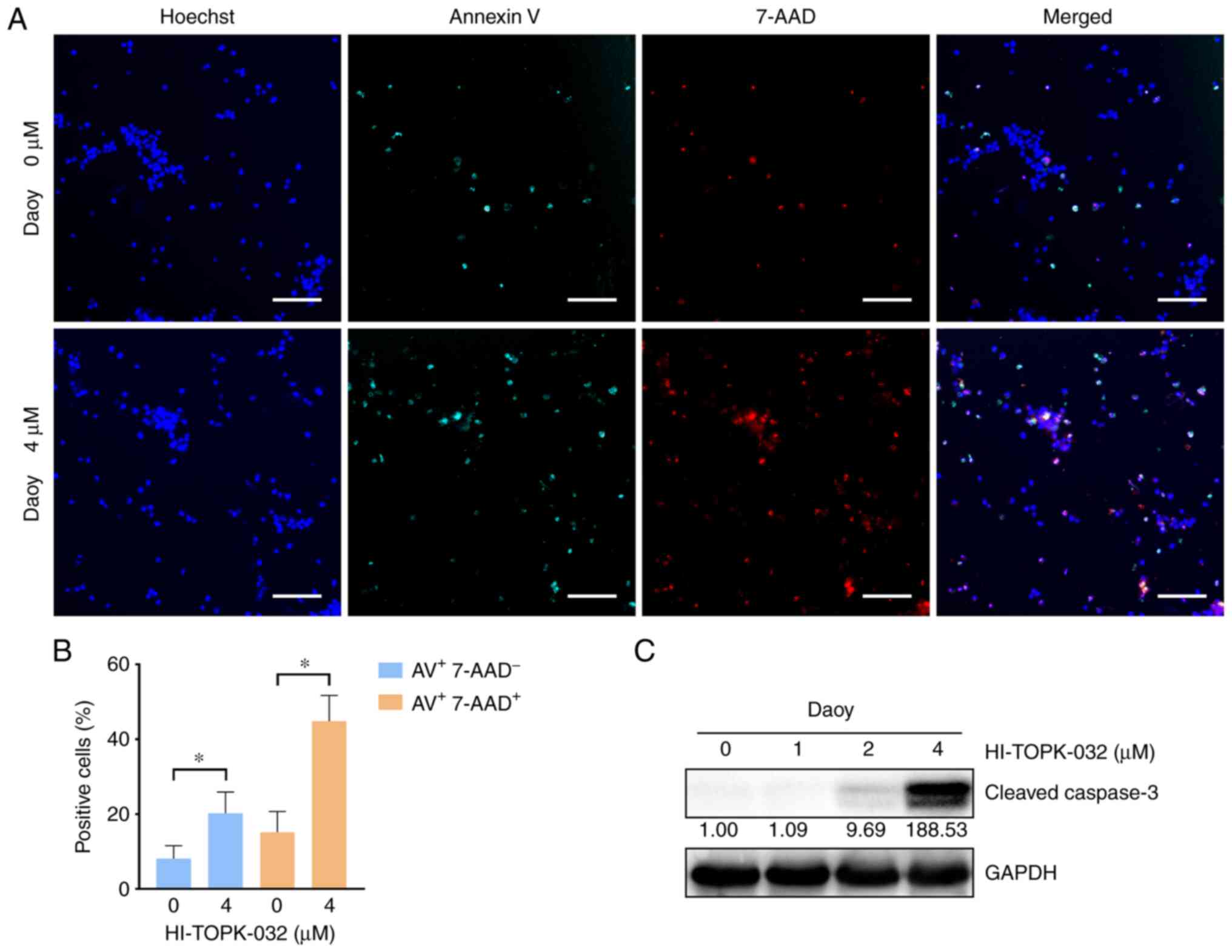
To examine the effects of PBK inhibitor specifically
on cell survival, cell apoptosis was measured by monitoring the
externalization of phosphatidylserine (PS) in MB cells treated with
HI-TOPK-032. Since HI-TOPK-032 would remain in the cell pellets
following centrifugation and its color would interfere with the
accuracy of flow cytometry detection, Annexin V/7-AAD-positive
cells were observed and quantified under a fluorescence microscope.
Annexin V single-positive cells represent early apoptotic cells,
while Annexin V and 7-AAD double-positive cells indicate late-stage
apoptotic cells and necrotic cells. The percentage of Annexin V
single-positive cells was markedly higher in the
HI-TOPK-032-treated group as compared with the control group, and
the proportion of double-positive cells also exhibited similar
results (Figs. 6A and B, and
7A and B). Subsequently, the
activation of caspase-3 was examined using western blot analysis to
further examine the apoptosis of MB cells. In line with PS
externalization, the level of cleaved caspase-3 in the Daoy and
D341 cells was substantially increased following treatment with
HI-TOPK-032 (Figs. 6C and 7C). Thus, targeting PBK also induces the
caspase-dependent apoptosis of MB cells.
Discussion
As the most frequent malignant brain tumor in
pediatrics, MB not only poses a grave threat to the lives of
children, but also leads to disabling consequences and a poor
quality of life for survivors. As the standard therapeutic regimens
for MB (surgical intervention followed by cranio-spinal irradiation
and adjuvant chemotherapy) often lead to a high morbidity rate,
numerous patients suffer from short- and long-term sequelae
following treatment (1). Targeted
therapies provide further options for managing this refractory
disease and possibilities to reduce the treatment-related toxicity
(7). The present study first
identified the DEGs between MB and normal brain samples, and then
screened 10 hub genes from the significantly upregulated genes in
MB. These hub genes have been reported in multiple cancers (e.g.,
breast, prostate cancer and glioma) by their oncogenic functions
(38–47); however, but to the best of our
knowledge, PBK has not been previously studied as a
therapeutic target for MB. Therefore, PBK was selected as
the target gene for further exploration in the present study.
PBK, a mitotic serine/threonine protein kinase
belonging to the MAPKK family, has been found to be expressed
exclusively in proliferating and multipotent cells, particularly in
germinal and fetal cells, as well as cancer cells (35). Additionally, Dougherty et al
(32) reported PBK expression in
rapidly proliferating central nervous system cells of mice, such as
adult subependymal neuronal progenitors and granular cell
precursors of the postnatal cerebellum, and its suppression in
neurons, mature glia and quiescent cells. MB is a type of embryonal
tumor, which is now considered to arise from stem cells or
progenitor cells in the cerebellum or posterior fossa (33). Hence, the significant upregulation
in PBK expression in MB suggests that this protein may play a
critical role in the pathogenesis of MB. The present study then
verified the highly expressed level of PBK in MB by examining
several independent gene expression datasets. Notably, the
expression level of PBK was markedly higher in all MB subgroups
than normal brain tissue, and a high PBK expression was associated
with a poor clinical outcome in SHH, group 3 and group 4 MBs.
Currently, investigations on targeted therapies for
MB are mainly based on distinctive aberrant signaling pathways in a
specific subgroup, such as the hedgehog pathway in the SHH
subgroup, or more general alterations of certain pathways in MB,
such as the PI3K pathway (6,7).
Since WNT MBs have a favorable prognosis, major efforts have been
made to search for novel therapeutic approaches for non-WNT MBs.
Interfering with the PTCH1/SMO/SUFU/GLI axis in the hedgehog
pathway with small molecules is considered a promising therapy for
SHH MBs. The SMO inhibitor, vismodegib, for instance, is being/has
been tested in some clinical trials (NCT01878617) (48). However, resistance has been found
in patients with SMO or SUFU mutations, or
GLI2 amplifications (7,49).
For group 3 and group 4 MBs, fewer targeted treatment options are
available due to the insufficient knowledge of their specific tumor
drivers (6,7). Accordingly, other novel treatment
targets remain to be explored. Of note, PBK is upregulated in all
MB subgroups, which also has significant prognostic implications.
Therefore, the present study further examined the effects of
targeting PBK with its inhibitor, HI-TOPK-032, on MB cell lines
[Daoy cells (SHH) and D341 cells (group 3)]. HI-TOPK-032 is the
most widely used PBK inhibitor that can occupy the ATP-binding site
of PBK and block its kinase activity (37). The pharmacological inhibition of
PBK led to a marked decrease in cell proliferation and a notable
increase in apoptosis, with the diminished phosphorylation of
downstream effectors of PBK, including ERK1/2 and Akt. These
results underscore the potential of PBK as a therapeutic target in
MB treatment.
Previous studies have also reported the
overexpression of PBK in multiple cancer types, such as glioma,
leukemia, colorectal, ovarian, skin and lung cancer (31,50).
Targeting PBK with HI-TOPK-032 or other novel inhibitors, such as
OTS514, OTS964 and ADA-07 in these cancer types has shown promising
anticancer efficacy as well (31,35).
Notably, a prerequisite for a suitable candidate target for cancer
treatment is that its targeting can eliminate cancer cells, while
sparing normal tissue. PBK is rarely detectable in neurons and
mature glia, but highly expressed in MB cells, rendering it an
attractive target for MB treatment. Considering that PBK is also
expressed in active stem/progenitor cells in the brain, whether
treating MB by PBK inhibition would affect these cells warrants
further investigation. Of note, Joel et al (38) found that normal neural stem cells
had a better tolerance for HI-TOPK-032 in vitro than glioma
initiating cells, suggesting the possibility of identifying an
effective dose of PBK inhibitor to destroy cancer cells, with
minimal damage to normal stem cells.
It is worth noting that varied responses of MB cells
to the PBK inhibitor HI-TOPK-032 were observed in the different
assays in the present study. While the IC50 value of
HI-TOPK-032 was similar in the Daoy and D341 cells in the CCK-8
assay, the D341 cells appeared to be more sensitive to HI-TOPK-032
than the Daoy cells in the apoptosis assay. The possible reason is
that the cell density of Daoy and D341 cells was the same in the
apoptosis experiments, and the number of D341 (10,000 cells/well)
used in the CCK-8 assay was higher than that of Daoy cells (2,000
cells/well). Although the concentration (or total amount) of
HI-TOPK-032 was the same for both cell lines, the absolute quantity
of HI-TOPK-032 per cell was different (less for the D341 cells) in
the CCK-8 assay. Therefore, it is hypothesized that the cell
density may also influence the response of MB cells to HI-TOPK-032.
As regards the limitations of the present study, the specific
function of PBK in MB cells was not examined by knocking down this
protein. Loss-of-function assays are thus required in the future to
determine the role of PBK in regulating MB cell proliferation and
apoptosis. In addition, it is necessary to evaluate the effects of
PBK knockdown in MB cells on tumor growth in vivo by using
animal models, particularly orthotopic xenograft models. The
preclinical testing of PBK inhibitors in animal models of MB,
including patient-derived orthotopic xenograft models, is also an
essential step in confirming the efficacy of PBK-targeted
therapy.
In conclusion, the present study identified
PBK as a hub gene with an upregulated expression in MB. The
aberrant expression of PBK was validated in all MB subgroups and
higher expression levels of PBK also indicated poorer clinical
outcomes in non-WNT MBs. Moreover, targeting PBK with its inhibitor
impaired the proliferation and induced the apoptosis of two MB cell
lines in vitro. Thus, PBK may prove to be a potential
prognostic biomarker and therapeutic target in the management of
MB.
Acknowledgements
The authors would like to thank Mr. Enio Barci
(Ludwig Maximilian University of Munich) for his comments on the
English writing of the manuscript.
Funding
The present study was supported by the 70th China Postdoctoral
Science Foundation (grant no. 2021M701618).
Availability of data and materials
The data used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
ML, HW, YD and WZ conceived the study and wrote the
manuscript. HW and ML performed the bioinformatics analyses. YD and
ML conducted the experiments and analyzed the data. HY, ZZ, QH, YB,
PW, MZ and JG made substantial contributions to the design of the
study. All authors discussed the results and revised the
manuscript. YD, HW, ML and WZ confirm the authenticity of all the
raw data. All authors have read and approved the final
manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Northcott PA, Robinson GW, Kratz CP,
Mabbott DJ, Pomeroy SL, Clifford SC, Rutkowski S, Ellison DW,
Malkin D, Taylor MD, et al: Medulloblastoma. Nat Rev Dis Primers.
5:112019. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Hovestadt V, Ayrault O, Swartling FJ,
Robinson GW, Pfister SM and Northcott PA: Medulloblastomics
revisited: Biological and clinical insights from thousands of
patients. Nat Rev Cancer. 20:42–56. 2020. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Louis DN, Perry A, Wesseling P, Brat DJ,
Cree IA, Figarella-Branger D, Hawkins C, Ng HK, Pfister SM,
Reifenberger G, et al: The 2021 WHO classification of tumors of the
central nervous system: A summary. Neuro Oncol. 23:1231–1251. 2021.
View Article : Google Scholar
|
|
4
|
Northcott PA, Buchhalter I, Morrissy AS,
Hovestadt V, Weischenfeldt J, Ehrenberger T, Gröbner S, Segura-Wang
M, Zichner T, Rudneva VA, et al: The whole-genome landscape of
medulloblastoma subtypes. Nature. 547:311–317. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Juraschka K and Taylor MD: Medulloblastoma
in the age of molecular subgroups: A review. J Neurosurg Pediatr.
24:353–363. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
DeSouza RM, Jones BR, Lowis SP and Kurian
KM: Pediatric medulloblastoma-update on molecular classification
driving targeted therapies. Front Oncol. 4:1762014. View Article : Google Scholar
|
|
7
|
Maier H, Dalianis T and Kostopoulou ON:
New approaches in targeted therapy for medulloblastoma in children.
Anticancer Res. 41:1715–1726. 2021. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Van Ommeren R, Garzia L, Holgado BL,
Ramaswamy V and Taylor MD: The molecular biology of medulloblastoma
metastasis. Brain Pathol. 30:691–702. 2020. View Article : Google Scholar
|
|
9
|
Baudino TA: Targeted cancer therapy: The
next generation of cancer treatment. Curr Drug Discov Technol.
12:3–20. 2015. View Article : Google Scholar
|
|
10
|
Ivanov DP, Coyle B, Walker DA and
Grabowska AM: In vitro models of medulloblastoma: Choosing the
right tool for the job. J Biotechnol. 236:10–25. 2016. View Article : Google Scholar
|
|
11
|
Birks DK, Donson AM, Patel PR, Sufit A,
Algar EM, Dunham C, Kleinschmidt-DeMasters BK, Handler MH, Vibhakar
R and Foreman NK: Pediatric rhabdoid tumors of kidney and brain
show many differences in gene expression but share dysregulation of
cell cycle and epigenetic effector genes. Pediatr Blood Cancer.
60:1095–1102. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Valdora F, Banelli B, Stigliani S, Pfister
SM, Moretti S, Kool M, Remke M, Bai AH, Brigati C, Hielscher T, et
al: Epigenetic silencing of DKK3 in medulloblastoma. Int J Mol Sci.
14:7492–7505. 2013. View Article : Google Scholar
|
|
13
|
Kanchan RK, Perumal N, Atri P, Chirravuri
Venkata R, Thapa I, Klinkebiel DL, Donson AM, Perry D, Punsoni M,
Talmon GA, et al: MiR-1253 exerts tumor-suppressive effects in
medulloblastoma via inhibition of CDK6 and CD276 (B7-H3). Brain
Pathol. 30:732–745. 2020. View Article : Google Scholar
|
|
14
|
Ritchie ME, Phipson B, Wu D, Hu Y, Law CW,
Shi W and Smyth GK: limma powers differential expression analyses
for RNA-sequencing and microarray studies. Nucleic Acids Res.
43:e472015. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Robinson MD, McCarthy DJ and Smyth GK:
edgeR: A bioconductor package for differential expression analysis
of digital gene expression data. Bioinformatics. 26:139–140. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Huang da W, Sherman BT and Lempicki RA:
Systematic and integrative analysis of large gene lists using DAVID
bioinformatics resources. Nat Protoc. 4:44–57. 2009. View Article : Google Scholar
|
|
17
|
Szklarczyk D, Gable AL, Lyon D, Junge A,
Wyder S, Huerta-Cepas J, Simonovic M, Doncheva NT, Morris JH, Bork
P, et al: STRING v11: Protein-protein association networks with
increased coverage, supporting functional discovery in genome-wide
experimental datasets. Nucleic Acids Res. 47:D607–D613. 2019.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Shannon P, Markiel A, Ozier O, Baliga NS,
Wang JT, Ramage D, Amin N, Schwikowski B and Ideker T: Cytoscape: A
software environment for integrated models of biomolecular
interaction networks. Genome Res. 13:2498–2504. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Chin CH, Chen SH, Wu HH, Ho CW, Ko MT and
Lin CY: cytoHubba: Identifying hub objects and sub-networks from
complex interactome. BMC Syst Biol. 8 (Suppl 4):S112014. View Article : Google Scholar
|
|
20
|
de Bont JM, Kros JM, Passier MM,
Reddingius RE, Sillevis Smitt PA, Luider TM, den Boer ML and
Pieters R: Differential expression and prognostic significance of
SOX genes in pediatric medulloblastoma and ependymoma identified by
microarray analysis. Neuro Oncol. 10:648–660. 2008. View Article : Google Scholar
|
|
21
|
Griesinger AM, Birks DK, Donson AM, Amani
V, Hoffman LM, Waziri A, Wang M, Handler MH and Foreman NK:
Characterization of distinct immunophenotypes across pediatric
brain tumor types. J Immunol. 191:4880–4888. 2013. View Article : Google Scholar
|
|
22
|
Henriquez NV, Forshew T, Tatevossian R,
Ellis M, Richard-Loendt A, Rogers H, Jacques TS, Reitboeck PG,
Pearce K, Sheer D, et al: Comparative expression analysis reveals
lineage relationships between human and murine gliomas and a
dominance of glial signatures during tumor propagation in vitro.
Cancer Res. 73:5834–5844. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Ishida Y, Takabatake T, Kakinuma S, Doi K,
Yamauchi K, Kaminishi M, Kito S, Ohta Y, Amasaki Y, Moritake H, et
al: Genomic and gene expression signatures of radiation in
medulloblastomas after low-dose irradiation in Ptch1 heterozygous
mice. Carcinogenesis. 31:1694–1701. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Rivero-Hinojosa S, Lau LS, Stampar M,
Staal J, Zhang H, Gordish-Dressman H, Northcott PA, Pfister SM,
Taylor MD, Brown KJ and Rood BR: Proteomic analysis of
medulloblastoma reveals functional biology with translational
potential. Acta Neuropathol Commun. 6:482018. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Amani V, Donson AM, Lummus SC, Prince EW,
Griesinger AM, Witt DA, Hankinson TC, Handler MH, Dorris K,
Vibhakar R, et al: Characterization of 2 novel ependymoma cell
lines with chromosome 1q gain derived from posterior fossa tumors
of childhood. J Neuropathol Exp Neurol. 76:595–604. 2017.
View Article : Google Scholar
|
|
26
|
Hooper CM, Hawes SM, Kees UR, Gottardo NG
and Dallas PB: Gene expression analyses of the spatio-temporal
relationships of human medulloblastoma subgroups during early human
neurogenesis. PLoS One. 9:e1129092014. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Cavalli FMG, Remke M, Rampasek L, Peacock
J, Shih DJH, Luu B, Garzia L, Torchia J, Nor C, Morrissy AS, et al:
Intertumoral heterogeneity within medulloblastoma subgroups. Cancer
Cell. 31:737–754.e6. 2017. View Article : Google Scholar
|
|
28
|
Robinson G, Parker M, Kranenburg TA, Lu C,
Chen X, Ding L, Phoenix TN, Hedlund E, Wei L, Zhu X, et al: Novel
mutations target distinct subgroups of medulloblastoma. Nature.
488:43–48. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Northcott PA, Korshunov A, Witt H,
Hielscher T, Eberhart CG, Mack S, Bouffet E, Clifford SC, Hawkins
CE, French P, et al: Medulloblastoma comprises four distinct
molecular variants. J Clin Oncol. 29:1408–1414. 2011. View Article : Google Scholar
|
|
30
|
Gaudet S, Branton D and Lue RA:
Characterization of PDZ-binding kinase, a mitotic kinase. Proc Natl
Acad Sci USA. 97:5167–5172. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Huang H, Lee MH, Liu K, Dong Z, Ryoo Z and
Kim MO: PBK/TOPK: An effective drug target with diverse therapeutic
potential. Cancers (Basel). 13:22322021. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Dougherty JD, Garcia AD, Nakano I,
Livingstone M, Norris B, Polakiewicz R, Wexler EM, Sofroniew MV,
Kornblum HI and Geschwind DH: PBK/TOPK, a proliferating neural
progenitor-specific mitogen-activated protein kinase kinase. J
Neurosci. 25:10773–10785. 2005. View Article : Google Scholar
|
|
33
|
Hovestadt V, Smith KS, Bihannic L, Filbin
MG, Shaw ML, Baumgartner A, DeWitt JC, Groves A, Mayr L, Weisman
HR, et al: Resolving medulloblastoma cellular architecture by
single-cell genomics. Nature. 572:74–79. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Ayllón V and O'Connor R: PBK/TOPK promotes
tumour cell proliferation through p38 MAPK activity and regulation
of the DNA damage response. Oncogene. 26:3451–3461. 2007.
View Article : Google Scholar
|
|
35
|
Herbert KJ, Ashton TM, Prevo R, Pirovano G
and Higgins GS: T-LAK cell-originated protein kinase (TOPK): An
emerging target for cancer-specific therapeutics. Cell Death Dis.
9:10892018. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Kar A, Zhang Y, Yacob BW, Saeed J,
Tompkins KD, Bagby SM, Pitts TM, Somerset H, Leong S, Wierman ME
and Kiseljak-Vassiliades K: Targeting PDZ-binding kinase is
anti-tumorigenic in novel preclinical models of ACC. Endocr Relat
Cancer. 26:765–778. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Kim DJ, Li Y, Reddy K, Lee MH, Kim MO, Cho
YY, Lee SY, Kim JE, Bode AM and Dong Z: Novel TOPK inhibitor
HI-TOPK-032 effectively suppresses colon cancer growth. Cancer Res.
72:3060–3068. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Joel M, Mughal AA, Grieg Z, Murrell W,
Palmero S, Mikkelsen B, Fjerdingstad HB, Sandberg CJ, Behnan J,
Glover JC, et al: Targeting PBK/TOPK decreases growth and survival
of glioma initiating cells in vitro and attenuates tumor growth in
vivo. Mol Cancer. 14:1212015. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Liu T, Zhang H, Yi S, Gu L and Zhou M:
Mutual regulation of MDM4 and TOP2A in cancer cell proliferation.
Mol Oncol. 13:1047–1058. 2019. View Article : Google Scholar
|
|
40
|
Qiu R, Wu J, Gudenas B, Northcott PA,
Wechsler-Reya RJ and Lu Q: Depletion of kinesin motor KIF20A to
target cell fate control suppresses medulloblastoma tumour growth.
Commun Biol. 4:5522021. View Article : Google Scholar
|
|
41
|
Chandler BC, Moubadder L, Ritter CL, Liu
M, Cameron M, Wilder-Romans K, Zhang A, Pesch AM, Michmerhuizen AR,
Hirsh N, et al: TTK inhibition radiosensitizes basal-like breast
cancer through impaired homologous recombination. J Clin Invest.
130:958–973. 2020. View Article : Google Scholar
|
|
42
|
Zhao Y, He J, Li Y, Lv S and Cui H: NUSAP1
potentiates chemoresistance in glioblastoma through its SAP domain
to stabilize ATR. Signal Transduct Target Ther. 5:442020.
View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Jalalirad M, Haddad TC, Salisbury JL,
Radisky D, Zhang M, Schroeder M, Tuma A, Leof E, Carter JM, Degnim
AC, et al: Aurora-A kinase oncogenic signaling mediates
TGF-β-induced triple-negative breast cancer plasticity and
chemoresistance. Oncogene. 40:2509–2523. 2021. View Article : Google Scholar : PubMed/NCBI
|
|
44
|
Pai VC, Hsu CC, Chan TS, Liao WY, Chuu CP,
Chen WY, Li CR, Lin CY, Huang SP, Chen LT and Tsai KK: ASPM
promotes prostate cancer stemness and progression by augmenting
Wnt-Dvl-3-β-catenin signaling. Oncogene. 38:1340–1353. 2019.
View Article : Google Scholar : PubMed/NCBI
|
|
45
|
Yasukawa M, Ando Y, Yamashita T, Matsuda
Y, Shoji S, Morioka MS, Kawaji H, Shiozawa K, Machitani M, Abe T,
et al: CDK1 dependent phosphorylation of hTERT contributes to
cancer progression. Nat Commun. 11:15572020. View Article : Google Scholar : PubMed/NCBI
|
|
46
|
Cheng S, Castillo V and Sliva D: CDC20
associated with cancer metastasis and novel mushroom-derived CDC20
inhibitors with antimetastatic activity. Int J Oncol. 54:2250–2256.
2019.
|
|
47
|
Gao Z, Jia H, Yu F, Guo H and Li B: KIF2C
promotes the proliferation of hepatocellular carcinoma cells in
vitro and in vivo. Exp Ther Med. 22:10942021. View Article : Google Scholar : PubMed/NCBI
|
|
48
|
Robinson GW, Orr BA, Wu G, Gururangan S,
Lin T, Qaddoumi I, Packer RJ, Goldman S, Prados MD, Desjardins A,
et al: Vismodegib exerts targeted efficacy against recurrent sonic
hedgehog-subgroup medulloblastoma: Results from phase II pediatric
brain tumor consortium studies PBTC-025B and PBTC-032. J Clin
Oncol. 33:2646–2654. 2015. View Article : Google Scholar
|
|
49
|
Kool M, Jones DT, Jäger N, Northcott PA,
Pugh TJ, Hovestadt V, Piro RM, Esparza LA, Markant SL, Remke M, et
al: Genome sequencing of SHH medulloblastoma predicts
genotype-related response to smoothened inhibition. Cancer Cell.
25:393–405. 2014. View Article : Google Scholar
|
|
50
|
Wen H, Chen Z, Li M, Huang Q, Deng Y,
Zheng J, Xiong M, Wang P and Zhang W: An integrative pan-cancer
analysis of PBK in human tumors. Front Mol Biosci. 8:7559112021.
View Article : Google Scholar
|