Introduction
Verrucous hyperplasia (VH) is a potentially
malignant disorder presenting as a white or pink exophytic mucosal
lesion with a typical verrucous or papillary surface. VH is
considered a variant of oral verrucous carcinoma (VC), which mimics
its presentation both clinically and histopathologically. The first
ever verrucous papillary lesion reported was by Fridell and
Rosenthal in 1941(1). In 1948,
Ackermann observed 31 similar cases and formulated the term
‘verrucous carcinoma’ for such a condition (2). The term ‘verrucous hyperplasia’ was
also coined by Ackermann and McGavran (3). However, a complete clinical and
histological analysis of such oral mucosal lesions was performed by
Shear and Pindborg (4) to
differentiate it from VC and verrucous leukoplakia (VL).
Initially, the most common site reported for the
occurrence of VH was the gingiva and alveolar mucosa (4). However, a previous study revealed
buccal mucosa (41%) to be more frequently involved (5). Other sites with predilection for the
occurrence of VH are the tongue, palate, labial mucosa, sino-nasal
mucosa, larynx and perianal region (5). VH generally occurs in individuals in
the 4 to 6th decade of life.
There is a striking association between habits of
tobacco chewing, areca nut chewing and smoking with the occurrence
of VH and its malignant transformation into VC or oral squamous
cell carcinoma. The rate of malignant transformation of VH reported
is 5.1% in ~54.6 months (6). The
transformation rate of VL is 4-15% in 5-8 years (7).
VH can be differentiated from VC only by
histopathological analysis. In VC, the hyperplastic epithelium
invades the connective tissue, whereas in VH, the hyperplastic
epithelium remains superficial to the normal epithelium. It is
crucial for clinicians to be highly knowledgeable in order to
correctly diagnose the condition and to be able to effectively
perform the biopsy. The sample should include the normal tissue
along with a margin of the lesion in adequate depth.
Immunohistochemical markers, such as p53, E-cadherin, Ki-67 and
MMP-1 can also be used as an effective aid in differentiating VH
from VC (8).
Various treatment modalities that have been utilized
in the treatment of VH are surgical excision, radiotherapy,
chemotherapy or a combination of these. Photodynamic therapy has
also been recently used as a resort for the treatment of VH
(5,6,8). The
present study describes a case of VH that was successfully managed
surgically in the clinic followed by reconstruction using the
buccal fat pad (BFP), which is hardly used in such cases.
Case report
A 37-year-old male patient reported to a dental
clinic in Nagpur December, 2015 with the chief complaint of a
painless growth over the left cheek for a period of 3 months. The
patient was referred to Sharad Pawar Dental College, Wardha, India
for further treatment. He complained of a burning sensation in
relation to the lesion. The patient also provided a history of
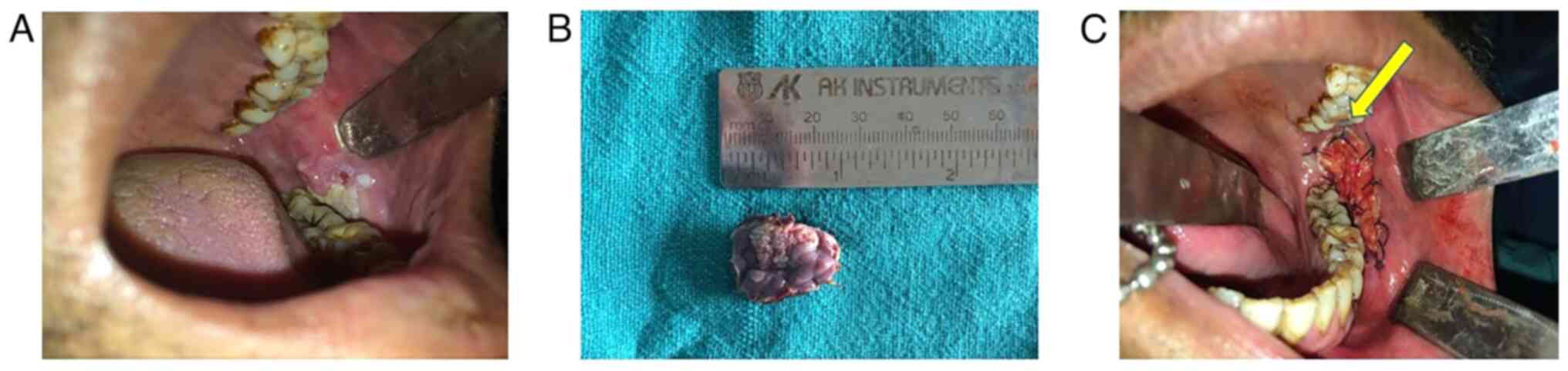
tobacco chewing and smoking over the past 10 years. An intraoral
examination revealed a whitish pink exophytic growth with defined
margins, measuring 2.5x1.5 cm over the left buccal mucosa (Fig. 1A). The lesion was firm,
non-purulent, non-tender and without any ulcerations. A provisional
diagnosis of leukoplakia was made. Written informed consent was
obtained from the patient for inclusion in the study and
investigations were carried out following the rules of the
Declaration of Helsinki of 1975.
The lesion was managed by a wide local excision
under local anaesthesia and the sample was sent for
histopathological analysis to the Oral Pathology Department of
Sharad Pawar Dental College, Wardha (Fig. 1B). Tissues were stained using
Harris' haematoxylin solution at a temperature of 60-70˚C for 6 h
and then rinsed under tap water. Subsequently, 10% acetic acid and
85% ethanol were used to differentiate the tissue twice for 2 and
10 h followed by rinsing with tap water again. The tissues were
saturated in lithium carbonate solution for 12 h and then rinsed.
Final staining was carried out with eosin Y ethanol solution for 48
h. Tissues were dehydrated using 95% ethanol twice for 0.5 h
followed by soaking in xylene for 1 h at 60-70˚C and then paraffin
for 12 h. Slices (12-µm-thick) were sectioned from the stained
samples, dewaxed, mounted and imaged using a Nikon NIS-Elements
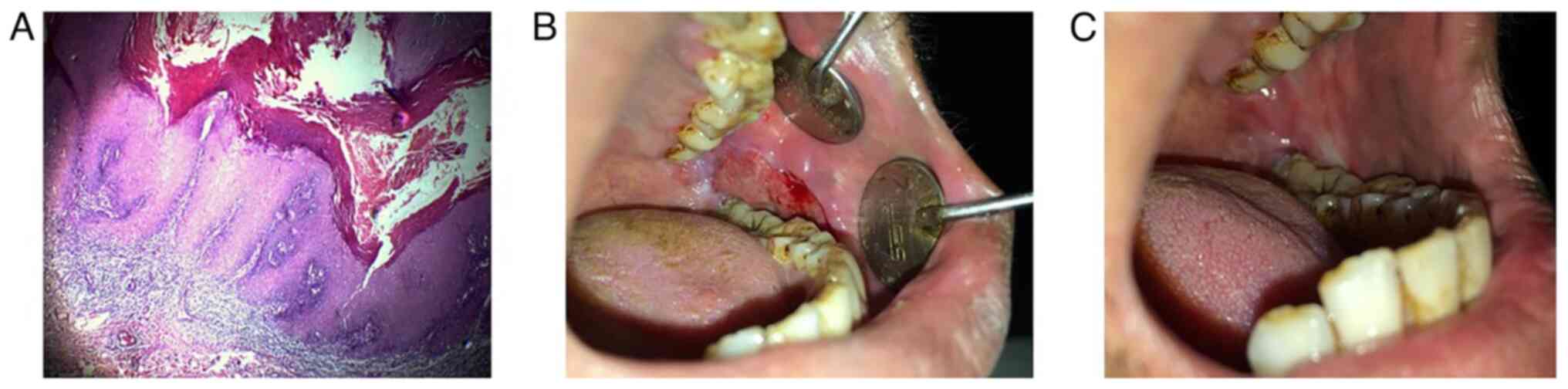
microscope at x4 magnification. A histological examination depicted
a parakeratinized epithelium with long, broad pushing rete pegs and
a parakeratin layer exhibiting a typical chevron pattern with
scanty connective tissue. The epithelium exhibited basal cell
hyperplasia, a loss of stratification, acanthosis, individual cell
keratinization, cellular and nuclear pleomorphism at places and
minimal abnormal mitotic figures (Fig.
2A). Depending on the histopathological features, the final
diagnosis of oral VH was made. Reconstruction of the defect was
performed using the BFP (Fig. 1C).
The BFP was used due to its higher vascularity, its proximity to
the donor site and to provide less scar contracture.
The patient was recalled for regular follow-up.
After 2 weeks, the surgical site was in a healthy condition with
uneventful healing (Fig. 2B). At
the end of 3 months, the BFP exhibited complete mucolisation
(Fig. 2C). The patient remains on
follow-up and there are currently no signs of recurrence even after
2.5 years.
Discussion
VH basically represents a premalignant alteration in
the normal oral mucous membrane. Histologically, six different
stages have been suggested, which include normal mucosa,
hyperkeratosis, VH, VC, papillary squamous cell carcinoma and less
differentiated squamous cell carcinoma (9). Hence, VH is considered a precursor of
VC, which is clinically indistinguishable from the latter. A
histopathological analysis is therefore considered a gold standard
for diagnosing a case of VH.
Shear and Pindborg (4) classified VH into a blunt and sharp
variety. The blunt variety comprises of broader, flatter and less
keratinized verrucous processes, whereas sharp processes are long,
narrow and heavily keratinized, leading to a white appearance. VH
was reclassified by Wang et al (5) into a plaque and mass type. The
features of the mass type variety are associated more with the
histopathological criteria. Hence, it was suggested that the plaque
type variety be known by the term VL and the mass type as VH. VL is
a non-homogeneous leukoplakia with an excessive rate of malignant
transformation. The mass type of VH has a thinner keratin surface
with a higher malignant potential, rendering early treatment
indispensable.
A high-risk association between habits, such as
areca nut and tobacco chewing and smoking, and the occurrence of VH
has been reported. Shear and Pindborg (4) reported that the gingiva and alveolar
mucosa were the most common sites for the occurrence of VH;
however, the buccal mucosa has now been established as the most
prevalent site (5). In the case
presented herein, the lesion was located on the buccal mucosa,
which is consistent with the literature. This frequent involvement
may also be associated with the habit of the placement of betel nut
or tobacco in the buccal vestibule (5). The study conducted by Shiu and Chen
(10) reported that the rate of
malignant transformation was 7.2 years in patients with habits of
areca nut or tobacco chewing and 22.4 years for individuals without
any associated risk factor or habit.
The key to the successful treatment of VH lies in
the accurate diagnosis made by the clinician and the pathologist;
this is achieved by possessing awareness and knowledge of the
clinical and histological presentation of the lesion. VH can be
treated with similar modalities as VC due to the overlapping
clinical features. Different procedures that have been used in the
treatment of VH are surgical excision, chemotherapy, radiotherapy,
cryotherapy or a combination of these. Surgical excision is the
most conventional and reliable treatment. A wide surgical excision
with adequate soft tissue margin and depth is paramount to
preventing recurrence of the lesion (8,9,11,12).
Some studies have demonstrated the use of cryogun (Brymill Corp.)
cryotherapy and topical 5-aminolevulinic acid-mediated photodynamic
therapy as an effective treatment modality for VH and leukoplakic
lesions (11,12).
The BFP, which has been used as a pedicled or free
graft since the 1970s, has hardly been used for reconstruction
following the excision of VH (13). In the cased described in the
present study, the defect using BFP was successfully reconstructed
with no recurrence in a long follow-up period of 2.5 years. The BFP
consists of a central body with four processes (buccal, pterygoid,
superficial and deep temporal). The major volume is constituted by
body and buccal extension, which is released conveniently by an
intraoral buccal incision at the tuberosity area. However, in the
case presented herein, the BFP was available within the defect. It
epithelializes within a few weeks, eliminating the requirement of
any skin grafts (14). The
function of the BFP is lubrication during the contracture of
muscles, and a loss of this fat can induce some scar contracture
and the adhesion of muscles; thus, the patient was advised to
perform active mouth opening exercises. Hence, no marked
contracture or adhesion occurred in the present case. The mouth
opening of the patient was not negatively affected. BFP was
preferred over skin grafts, artificial dermal templates or other
treatment modalities due to its high vascularity, the proximity of
the donor site to the wound site, its economic suitability, less
scar contracture than skin grafts and a lower probability of
infection or morbidity (14).
In conclusion, VH is a potentially malignant lesion
whose distinction from VC can only be made histologically. There is
a high risk of the malignant transformation of VH. Hence. the
treatment of VH should be conducted at the earliest possible time
point to prevent grievous consequences. The excision of the lesion
should also include normal adjacent tissue to prevent recurrence.
The present study described a case of VH which was successfully
diagnosed and treated by surgical excision with no signs of
recurrence.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
AJ was involved in the conception and design of the
study, as well as in the acquisition, analysis and interpretation
of the patient's data. ST was involved in the analysis,
interpretation of patient's data for the study and in the drafting
of the study. AR was involved in the conception of the study and in
the acquisition of patient data. AY was involved in the conception
and design of the study. ST and AJ confirm the authenticity of all
the raw data. All authors have read and approved the final
manuscript.
Ethics approval and consent to
participate
Written informed consent was obtained from the
patient for inclusion in the study and investigations were carried
out following the rules of the Declaration of Helsinki of 1975.
Patient consent for publication
The patient provided written informed consent for
the publication images related to his case.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Florin EH, Kolbusz RV and Goldberg LH:
Verrucous carcinoma of the oral cavity. Int J Dermatol. 33:618–622.
1994.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Ackerman LV: Verrucous carcinoma of the
oral cavity. Surgery. 23:670–678. 1948.PubMed/NCBI
|
|
3
|
Ackerman LV and McGavran MH: Proliferating
benign and malignant epithelial lesions of the oral cavity. J Oral
Surg (Chic). 16:400–413. 1958.PubMed/NCBI
|
|
4
|
Shear M and Pindborg JJ: Verrucous
hyperplasia of the oral mucosa. Cancer. 46:1855–1862.
1980.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Wang YP, Chen HM, Kuo RC, Yu CH, Sun A,
Liu BY, Kuo YS and Chiang CP: Oral verrucous hyperplasia:
Histologic classification, prognosis, and clinical implications. J
Oral Pathol Med. 38:651–656. 2009.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Grover S, Jha M, Sharma B, Kapoor S,
Mittal K, Parakkat NK, Shivappa AB and Kaur R: Verrucous
hyperplasia: Case report and differential diagnosis. Sultan Qaboos
Univ Med J. 17:e98–e102. 2017.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Neville BW, Damm DD, Allen CM and Bouquot
JE (eds): Epithelial pathology. In: Oral and Maxillofacial
Pathology. 3rd edition. W.B. Sauders Company, Philadelphia, PH,
pp388-397, 2009.
|
|
8
|
Klieb HB and Raphael SJ: Comparative study
of the expression of p53, Ki67, E-cadherin and MMP-1 in verrucous
hyperplasia and verrucous carcinoma of the oral cavity. Head Neck
Pathol. 1:118–122. 2007.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Hansen LS, Olson JA and Silverman S Jr:
Proliferative verrucous leukoplakia. A long-term study of thirty
patients. Oral Surg Oral Med Oral Pathol. 60:285–298.
1985.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Shiu MN and Chen THH: Impact of betel
quid, tobacco and alcohol on three-stage disease natural history of
oral leukoplakia and cancer: Implication for prevention of oral
cancer. Eur J Cancer Prev. 13:39–45. 2004.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Hwang MJ, Yang YJ, Lee YP and Chiang CP:
Cryotherapy is effective for treatment of oral verrucous
hyperplasia-case report. J Dent Sci. 16:1025–1026. 2021.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Lin HP, Chen HM, Cheng SJ, Yu CH and
Chiang CP: Cryogun cryotherapy for oral leukoplakia. Head Neck.
34:1306–1311. 2012.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Neder A: Use of buccal fat pad for grafts.
Oral Surg Oral Med Oral Pathol. 55:349–350. 1983.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Chakrabarti J, Tekriwal R, Ganguli A,
Ghosh S and Mishra PK: Pedicled buccal fat pad flap for intraoral
malignant defects: A series of 29 cases. Indian J Plast Surg.
42:36–42. 2009.PubMed/NCBI View Article : Google Scholar
|