Introduction
With the incidence of ischemic encephalopathy
gradually increased, people have payed increased attention to the
prevention and treatment of cerebral ischemia-reperfusion injury
(1,2). Cerebral infarction is a common cause of
ischemic encephalopathy, thrombolytic therapy after cerebral
infarction in time can save the lives of patients, but also may
cause ischemia-reperfusion injury. Therefore, if the mechanism of
ischemia-reperfusion injury is clear, it is of great significance
for timely target treatment for ischemia-reperfusion injury. In
recent years, there were more studies on ischemia-reperfusion
injury, but there is still not a unified opinion on the prevention
and treatment of ischemia-reperfusion injury. Studies showed that
the expression of telomerase was increased in the brain tissues of
patients with ischemia-reperfusion injury (2,3), while
some researchers found that telomerase was overexpressed after the
injury of brain tissue, considering the protective effect of
telomerase on ischemia-reperfusion injury in order to reduce the
tissue damage (4). Human umbilical
cord blood mesenchymal stem cells (hUCB-MSCs) can secrete a variety
of cytokines and neurotrophic factors and promote nerve
regeneration, but the conventional route of administration can not
fully play the role of hUCB-MSCs. So some scholars proposed nasal
administration of hUCB-MSCs to improve neurological function in
rats with ischemia-reperfusion injury (5). At present, the study of hUCB-MSCs on
nerve injury in rats with ischemia-reperfusion injury is scarce. So
the aim of our study was to investigate the effects of hUCB-MSCs on
rats with ischemia-reperfusion injury, in order to explore the
mechanism of the prevention and treatment of ischemia-reperfusion
injury.
Materials and methods
Animals
Experiments were performed using 100 healthy adult
Wistar rats weighing 180–220 g, provided by College Animal Center,
Harbin Medical University. Rats were kept in the animal house under
constant temperature (18–25°C) and humidity (60 to 70%) on natural
light with C060 sterilized commercial feed and free water intake,
with 12 h before fasting. The study was approved by the Ethics
Committee of Harbin Medical University.
Modeling method
All rats were randomly divided into control group
and observation group and treated with 10% chloral hydrate (3.5
ml/kg) at RT. After anesthesia, the middle cerebral artery
ischemia-reperfusion model was established by the suture method,
and the specific modeling method was according to the method given
by Chopp and Li (6). Then the rats
in the observation group were treated with hUCB-MSCs (10 ml/kg) by
nasal administration for 14 days, with the saline in the control
group. The neurological deficit score and foot fault test were
evaluated at 1, 7 and 14 days after treatment, and the rats were
sacrificed at 14 days to detect the expression of telomerase
reverse transcriptase (TERT) in brain tissue.
The source of hUCB-MSCs: 30 ml human umbilical cord
blood was taken under sterile conditions with heparin
anticoagulant, then transferred into a 15 ml centrifuge tube and
centrifuged at 2,800 × g for 20 min. The upper plasma was removed,
collecting the white blood cells in interface layer, and stored at
4°C. The expression of TERT was detected by western blot analysis.
The above operations are carried out by the researchers in our
laboratory according to the instructions, and the reagents and kits
were purchased from LanPai Biotechnology Co., Ltd. (Shanghai,
China).
Observation and evaluation of
indicators
The criteria for mNSS (7)
The four aspects as sensory, motor, reflex and
muscle tensionin of rats were scored with the total score of 18.
The higher the score, the more serious the nerve damage.
Foot fault test
The foot fault test was used to evaluate the
disorder of rat forelimb, placing the rats on the Hanging mesh grid
(2.5×2.5 cm), then recording the total number of bilateral forelimb
movement and the number of left forelimb foot errors. The percent
of the number of left forelimb foot errors to the total number of
bilateral forelimb movement as the statistical results.
Statistical analysis
The statistical analysis was performed with SPSS
21.0 (IBM Corp., Armonk, NY, USA) and the obtained data are in
normal distribution. Measurement data were expressed as mean ± SD
and the t-test was performed. Counting data were calculated by
Chi-square test. A P-value <0.05 was considered as a significant
difference.
Results
Comparison of neurological deficit
score between the two groups
There was no significant difference in the scores of
mNSS between the two groups before the model establishment
(P>0.05), but after the model established there was significant
difference in two groups respectively (P<0.05). At 1 day after
the operation, the mNSS score of two groups was peaked, which was
decreased in the groups with the progress of treatment. The degree
of decline in the observation group was significantly greater than
that in the control group (P<0.05; Table I).
 | Table I.Neurological deficit score in two
groups (mean ± SD). |
Table I.
Neurological deficit score in two
groups (mean ± SD).
|
|
| mNSS score |
|---|
|
|
|
|
|---|
| Groups | n | Preoperative | Postoperative day
1 | Postoperative day
7 | Postoperative day
14 |
|---|
| Control group | 50 | 0.56±0.12 |
11.51±0.56a |
8.52±0.84a |
6.85±1.25a |
| Observation
group | 50 | 0.58±0.14 |
10.54±0.58a |
4.59±0.68a,b |
3.25±0.52a,b |
| Group |
|
| F=12.32, P=0.002 |
|
| Time |
|
| F=8.12, P=0.026 |
|
| Time group |
|
| F=9.15, P=0.012 |
|
Comparison of foot fault number
between the groups
There was no significant difference in the foot
fault number between the two groups before ischemia-reperfusion
model establishment (P>0.05), but after the model established
the foot fault frequency was significantly increased in each group.
At 1 day after operation, the number of foot errors peaked, but it
was decreased in the groups with the progress of treatment. The
number of foot errors was decreased significantly in the
observation group compared to that in the control group (P<0.05;
Table II).
 | Table II.The number of foot errors in the two
groups (mean ± SD). |
Table II.
The number of foot errors in the two
groups (mean ± SD).
|
|
| Wrong steps |
|---|
|
|
|
|
|---|
| Group | n | Preoperative | Postoperative day
1 | Postoperative day
7 | Postoperative day
14 |
|---|
| Control group | 50 | 0.44±0.15 |
29.5±3.82a |
23.65±3.43a |
16.98±2.68a |
| Observation
group | 50 | 0.42±0.12 |
28.32±3.46a |
20.32±3.24a,b |
6.52±1.87a,b |
| Group |
|
| F=10.45, P=0.002 |
|
| Time |
|
| F=7.43, P=0.034 |
|
| Time group |
|
| F=8.65, P=0.027 |
|
The gray value of TERT content in
brain tissue in the two groups
The gray value of TERT content in the observation
group was 0.983±0.056 LOD, which was significantly higher than that
in the control group with the gray value of 0.458±0.052 LOD
(P<0.05; Table III).
 | Table III.The gray value of TERT content in
brain tissue of the two groups (mean ± SD). |
Table III.
The gray value of TERT content in
brain tissue of the two groups (mean ± SD).
| Group | n | TERT (WB, LOD) |
|---|
| Control group | 50 | 0.458±0.052 |
| Observation
group | 50 | 0.983±0.056 |
| T value |
| 8.62 |
| P-value |
| <0.05 |
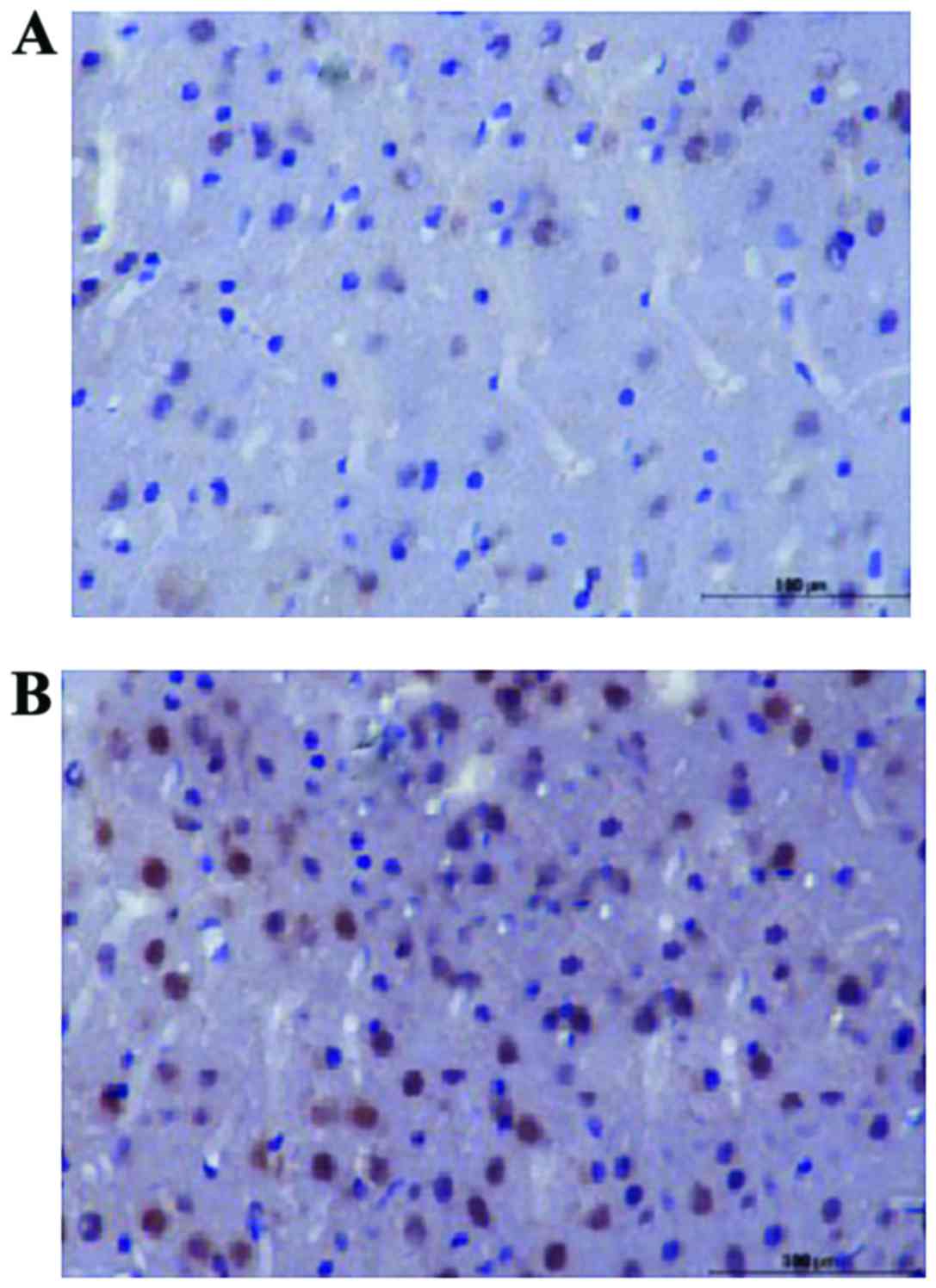
Comparison of groups of rats with
brain tissue immunohistochemical reaction
The H&E staining showed the nucleus or cytoplasm
in the brain tissue of rats was brown or yellow brown in the
observation group, which showed positive reaction (Fig. 1A). The cytoplasm and the nucleus were
stained yellow in the control group, suggested the neurons were
shrunken (Fig. 1B).
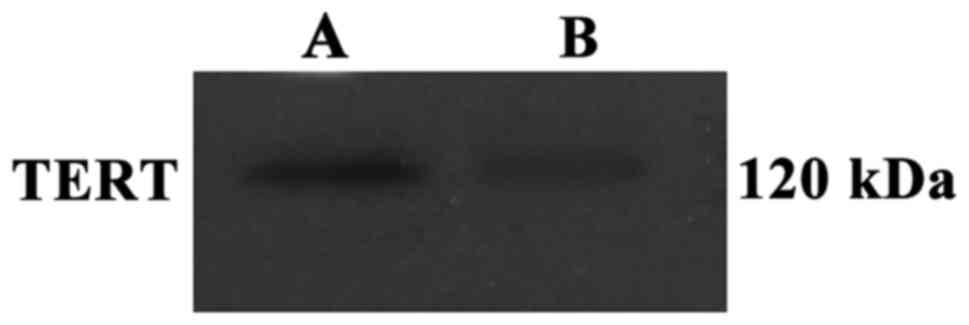
TERT protein expression in two
groups
As Fig. 2 shows, the
expression of TERT protein in brain tissue of rats in observation
group was significantly decreased compared to that in the control
group.
Discussion
Ischemia and hypoxia is an important factor for
tissue necrosis. For the brain tissue, short-term ischemia and
hypoxia can cause irreversible tissue damage (8). In recent years, with the deep study of
ischemic diseases, increased number of studies found that ischemia
is not the only factor for the tissue damage (9). Free radical release caused by
ischemia-reperfusion plays an important role in the tissue injury
induced by ischemia and hypoxia, which is known as
ischemia-reperfusion injury. Telomerase refers to an enzyme that is
responsible for telomere elongation in cells and is a basic
nucleoprotein reverse transcriptase that binds telomere DNA to the
eukaryotic chromosome ends. The primary role of telomerase is to
maintain telomere integrity and prevents its loss in cell division
(10). The activity of telomerase is
inhibited in normal cells, but it can be significantly activated in
tumor cells. TERT, as a catalytic subunit of telomerase, not only
activates telomerase activity, but also protects mitochondria and
has an anti-apoptotic effect. Studies showed that TERT can
effectively improve neuronal apoptosis and neurological function in
patients with ischemia-reperfusion injury (11). Stem cell therapy is a more popular
treatment in recent years, which have a good therapeutic effect for
some diseases. Some scholars have found that hUCB-MSCs contains a
variety of cytokines and nerve growth factors, which can
effectively improve neuronal damage, but these growth factors can
not pass through the blood-brain barrier (12). Nasal administration not only allows
drugs to enter the brain tissue, but also reduces the loss of stem
cells.
In this study, there were no significant differences
in the scores of mNSS between the two groups before the model
establishment (P>0.05), but there was significant differences in
two groups after the operation (P<0.05). At 1 day after the
operation, the mNSS score of two groups peaked, which was decreased
in the groups with the progress of treatment. The degree of decline
in the observation group was significantly greater than that in the
control group (P<0.05). Similarly, there were no significant
differences in the number of preoperative footsteps between the two
groups before the model establishment (P>0.05), but there was
significant differences in two groups after the operation
(P<0.05). At 1 day after the operation, the number of
preoperative footsteps was peaked, which was reduced in the groups
with the progress of treatment. The degree of reduction in the
observation group was significantly greater than that in the
control group (P<0.05). The results in our study showed that
hUCB-MSCs could effectively reduce the neurological injury of rats
with ischemia-reperfusion injury, which was consistent with the
decrease of neuronal apoptosis in brain tissue. Zhao et al
also found that after administration of hUCB-MSCs, neuronal
dysfunction in rats with ischemia-reperfusion injury was improved,
which was possibly related to the effects of TERT on promoting
astrocyte proliferation and activation, increasing hypoxia ischemic
rat brain astrocytes proliferation and promoting neuronal survival
(13). With the gray value of the
TERT protein as 0.458±0.052 LOD in the control group, which was
significantly lower than that in the observation group with
0.983±0.056 LOD, which suggested that hUCB-MSCs could effectively
promote the expression of TERT in brain tissue of rats with
ischemia-reperfusion. Chen et al also found that hUCB-MSCs
significantly increased the expression of TERT protein in rat brain
by nasal administration, possibly related to the effect of
hUCB-MSCs on promoting the expression of TERT in brain tissue
induced by cytokines and neurotrophic factors (14).
In conclusion, hUCB-MSCs can effectively improve the
neurological function of cerebral ischemia-reperfusion injury in
rats and improve the expression of TERT in brain tissue, which may
help to reduce cerebral ischemia-reperfusion injury.
Acknowledgements
The study was supported by the Post-Doctoral Initial
Fund of Heilongjiang Province (LBH-Q15091) and the Distinguished
Young Scholars Fund of the Fourth Clinical Medical College of
Haerbin Medical University (HYDSYJQ201506).
References
|
1
|
Lahiani A, Zahavi E, Netzer N, Ofir R,
Pinzur L, Raveh S, Arien-Zakay H, Yavin E and Lazarovici P: Human
placental eXpanded (PLX) mesenchymal-like adherent stromal cells
confer neuroprotection to nerve growth factor (NGF)-differentiated
PC12 cells exposed to ischemia by secretion of IL-6 and VEGF.
Biochim Biophys Acta. 1853:422–430. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Yu H, Chen P, Yang Z, Luo W, Pi M, Wu Y
and Wang L: Electro-acupuncture at conception and governor vessels
and transplantation of umbilical cord blood-derived mesenchymal
stem cells for treating cerebral ischemia/reperfusion injury.
Neural Regen Res. 9:84–91. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Guerrero-Beltrán CE, Tapia E,
Sánchez-González DJ, Martínez-Martínez CM, Cristobal-García M and
Pedraza-Chaverri J: Tert-Butylhydroquinone pretreatment protects
kidney from ischemia-reperfusion injury. J Nephrol. 25:84–89. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Khan I, Ali A, Akhter MA, Naeem N, Chotani
MA, Iqbal H, Kabir N, Atiq M and Salim A: Epac-Rap1-activated
mesenchymal stem cells improve cardiac function in rat model of
myocardial infarction. Cardiovasc Ther. 35:352017. View Article : Google Scholar
|
|
5
|
Karantalis V and Hare JM: Use of
mesenchymal stem cells for therapy of cardiac disease. Circ Res.
116:1413–1430. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Chopp M and Li Y: Treatment of neural
injury with marrow stromal cells. Lancet Neurol. 1:92–100. 2002.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Chen J, Sanberg PR, Li Y, Wang L, Lu M,
Willing AE, Sanchez-Ramos J and Chopp M: Intravenous administration
of human umbilical cord blood reduces behavioral deficits after
stroke in rats. Stroke. 32:2682–2688. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Luo CJ, Zhang FJ, Zhang L, Geng YQ, Li QG,
Hong Q, Fu B, Zhu F, Cui SY, Feng Z, et al: Mesenchymal stem cells
ameliorate sepsis-associated acute kidney injury in mice. Shock.
41:123–129. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Sun T, Gao GZ, Li RF, Li X, Li DW, Wu SS,
Yeo AE and Jin B: Bone marrow-derived mesenchymal stem cell
transplantation ameliorates oxidative stress and restores
intestinal mucosal permeability in chemically induced colitis in
mice. Am J Transl Res. 7:891–901. 2015.PubMed/NCBI
|
|
10
|
Chung DJ, Choi CB, Lee SH, Kang EH, Lee
JH, Hwang SH, Han H, Lee JH, Choe BY, Lee SY and Kim HY:
Intraarterially delivered human umbilical cord blood-derived
mesenchymal stem cells in canine cerebral ischemia. J Neurosci Res.
87:3554–3567. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Li J, Qu Y, Chen D, Zhang L, Zhao F, Luo
L, Pan L, Hua J and Mu D: The neuroprotective role and mechanisms
of TERT in neurons with oxygen-glucose deprivation. Neuroscience.
252:346–358. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Leong KH, Zhou LL, Lin QM, Wang P, Yao L
and Huang ZT: Therapeutic effects of various methods of MSC
transplantation on cerebral resuscitation following cardiac arrest
in rats. Mol Med Rep. 13:3043–3051. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Zhao F, Qu Y, Xiong T, Duan Z, Ye Q and Mu
D: The neuroprotective role of TERT via an antiapoptotic mechanism
in neonatal rats after hypoxia-ischemia brain injury. Neurosci
Lett. 515:39–43. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Chen M, Xiang Z and Cai J: The
anti-apoptotic and neuro-protective effects of human umbilical cord
blood mesenchymal stem cells (hUCB-MSCs) on acute optic nerve
injury is transient. Brain Res. 1532:63–75. 2013. View Article : Google Scholar : PubMed/NCBI
|