Introduction
Bronchial asthma is a common clinical disease. An
epidemiological study found that the rates of morbidity, mortality
and prevalence of bronchial asthma are increasing worldwide. In
China, the incidence of bronchial asthma has doubled over the past
decade. The World Health Organization defines bronchial asthma as a
chronic airway inflammation that is caused by various inflammatory
cells, including eosinophils (EOS), mast cells and T lymphocytes
(1–3).
Chronic airway inflammation is characterized by the
infiltration of EOS, an increase in serum immunoglobulin (Ig)E and
excessive secretion of airway mucus (4–6),
which result in airway structural changes and may even develop into
refractory asthma or severe asthma (7). Hyssopus officinalis L., an
Uygur medicine, is a perennial herb of Labiatae. The herb has been
shown to relieve coughing and asthma; however, the underlying
mechanisms are yet to be elucidated. Previous studies have shown
that Hyssopus officinalis L. plays an anti-inflammatory role
by regulating the secretion of interleukin (IL)-4, IL-17 and
interferon-γ (IFN-γ), as well as regulating the imbalance between
Th1/Th2 cytokines (8–10). However, the role of Hyssopus
officinalis L. in the regulation of immune function has not yet
been investigated. Therefore, the aim of the present study was to
investigate the effect of Hyssopus officinalis L. on
immunity in a mouse model of chronic asthma. In addition, the study
investigated whether Hyssopus officinalis L. was able to
increase immune reactions and thus, may be used to improve and
perfect the mechanisms underlying the treatment of asthma.
Materials and methods
Extract preparation
Crude herbs (200 g) were extracted using 6,000 ml
water. The solvents in the extracts were removed via rotary
evaporation under reduced pressure (EYELA-digital water bath
SB-100; Eyela, Tokyo, Japan). The aqueous extract was then
freeze-dried and stored at 4°C. The aqueous extract was diluted
with saline water prior to use. In a previous study, the toxicology
and dosage were assessed (11).
Animals and model establishment
A total of 32 female BALB/c mice were purchased from
the Animal Experiment Center at Xinjiang Medical University
(Ürümqi, China). The mice were housed in microisolator cages and
received food and water. The laboratory temperature was maintained
at 24±1°C, and the relative humidity was maintained between 40 and
80%. All the experimental protocols were approved by the regional
Animal Ethics Committee of Xinjiang Medical University.
The BALB/c mice (age, 6–8 weeks) were randomly
divided into four groups, which included the normal, chronic
asthma, dexamethasone and Hyssopus officinalis L. groups.
The chronic asthma, dexamethasone and Hyssopus officinalis
L. groups were administered an intraperitoneal injection of 0.2 ml
sensitizing agent, which contained 100 μg ovalbumin (OVA;
Sigma-Aldrich, St. Louis, MO, USA) and 1 mg aluminum hydroxide gel,
on days 1 and 15. In addition, initiating on day 22, the mice were
administered 1% OVA for 30 min three times a week for eight weeks.
The normal group were treated with phosphate-buffered saline (PBS)
instead of OVA (12). Drugs were
chronically administered to the animals 1 h prior to the challenges
[0.005 mg/10 g body weight dexamethasone (TianYaoYaoYe Co., Ltd.
Hubei, China); 0.04 g/10 g body weight Hyssopus officinalis
L. (Pharmacy of Uyghur Hospital, Xinjiang, China)], once per day
for eight weeks. Animals were euthanized following the last
challenge and samples were collected.
Bronchoalveolar lavage fluid (BALF) and
serum harvesting
The chest was opened and the bronchus principalis
dexter was ligated in the bifurcation. BALF was collected using 0.4
ml PBS, three times in total according to a previously described
method (13,14,15).
The number of neutrophils was determined using the CytoSpin™
centrifuge (Thermo Fisher Scientific, Waltham, MA, USA).
The levels of serum IgE and IgG were analyzed using
an ELISA, measuring the change of absorbance at 450 nm (Bei Lai Yin
Biological Technology Co., Ltd., Wuhan, China).
Periodic acid-Schiff (PAS) staining and
analysis
Lung tissue samples were stained with PAS (Jiancheng
Bioengineering Institute of Nanjing, Nanjing, China) and analyzed
using an optical microscope (Olympus CX22, Olympus Tokyo, Japan). A
minimum of ten airways were observed in each section. The PAS
positively-stained cells were counted and scored using previously
described methods (16,17,18).
The scoring method used was as follows: 0, <5%; l, 5–25%; 2,
25–50%; 3, 50–5%; and 4, >75% PAS positively-stained cells.
Statistical analysis
SPSS 17.0 statistical software (SPSS, Inc., Chicago,
IL, USA) was used for statistical analysis. Data are presented as
the mean ± standard error of the mean. Comparisons between the
groups were performed using analysis of variance followed by the
Dunnett’s test, where P<0.05 was considered to indicate a
statistically significant difference.
Results
Behavioral alterations
Following the challenge with OVA, the mice presented
with a number of symptoms, including anxiety, nose scratching,
coughing, inspiratory dyspnea, shortness of breath, retardation,
piloerection and cyanosis. The activity decreased following
continuous challenges. However, the symptoms were relieved in the
dexamethasone and Hyssopus officinalis L. groups.
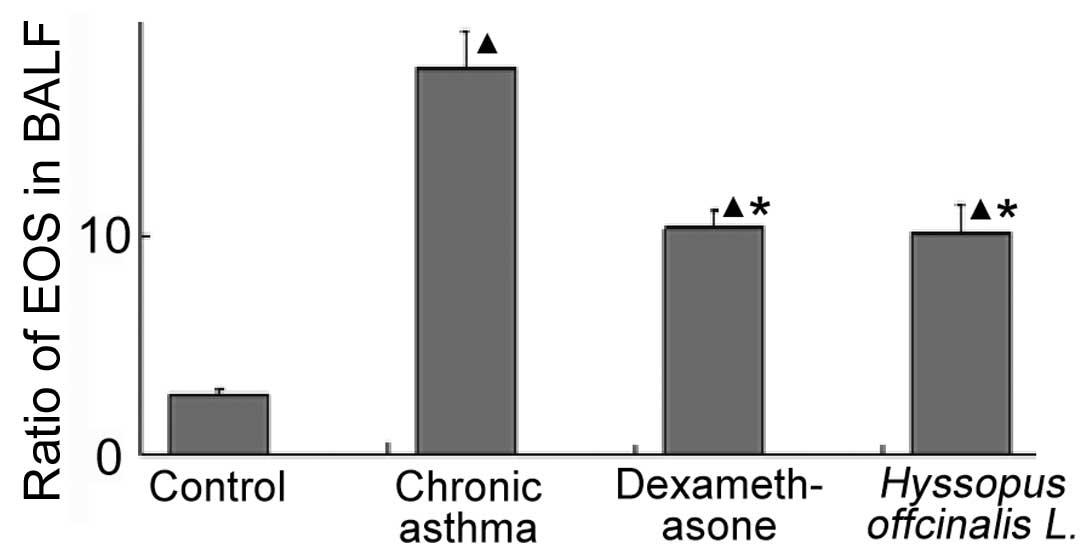
Ratio of EOS in the BALF
Fig. 1 shows that
the percentage of EOS in the chronic asthma group was higher
compared with the other groups. Furthermore, the ratio of EOS in
the dexamethasone group was similar to the ratio observed in the
Hyssopus officinalis L. group (10.27±0.85 and 10.08±1.29,
respectively).
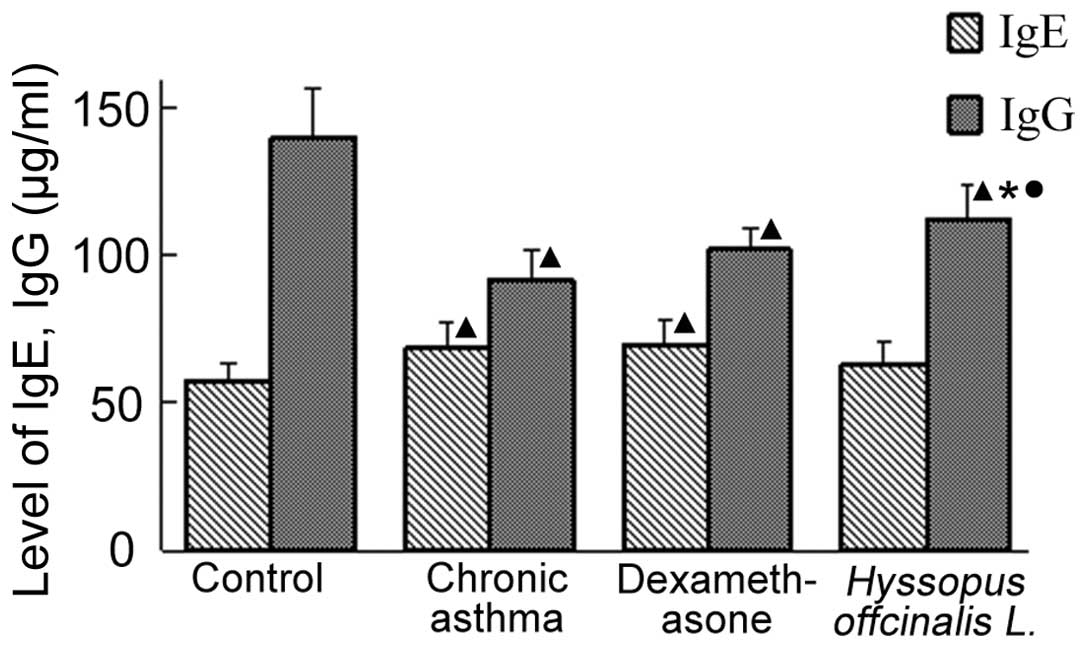
Level of IgE and IgG in the serum
As shown in Fig. 2,
the level of IgE in the Hyssopus officinalis L. group were
similar to the levels observed in the normal group. In addition,
the level of IgG in the chronic asthma and dexamethasone groups
were lower compared with the normal group; however, the
concentration of IgG in the Hyssopus officinalis L. group
was higher compared with the chronic asthma and dexamethasone
groups.
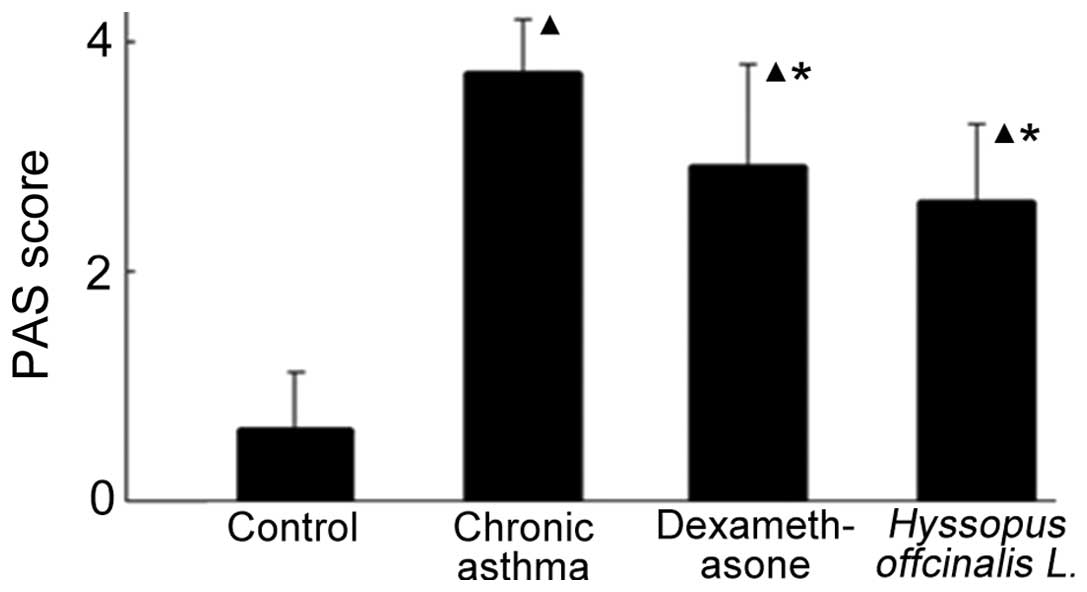
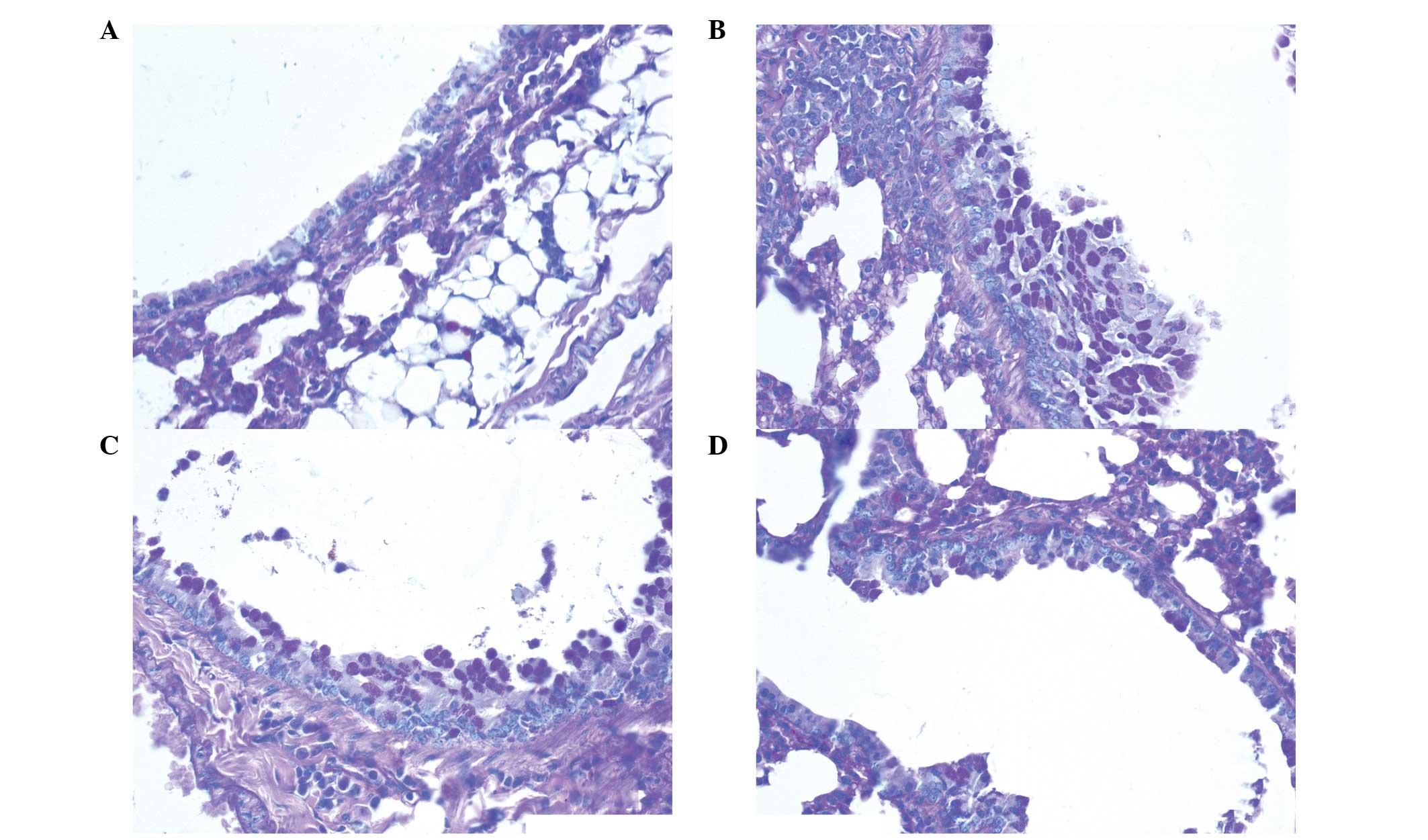
Secretion of mucus in the airway
The secretion of airway mucus in the chronic asthma
group was aggravated (Figs. 3 and
4). In addition, the secretion of
mucus increased in the dexamethasone and Hyssopus
officinalis L. groups; however, the levels were highest in the
chronic asthma group.
Discussion
Asthma is a type I allergic disease, and IgE has an
important role in the development of asthma (19). Previous studies have demonstrated
that there are various levels of inflammatory responses in patients
who suffer from asthma, and allergic airway inflammation with
increasing EOS is the main pathological feature of asthma (20,21).
Numerous studies have identified a correlation between the
infiltrate level of EOS and the severity of airway inflammation
(22–24). The variety of cell types present in
BALF may reflect the degree of inflammation in the peripheral
airways, which is also the main factor causing bronchial
hyperresponsiveness in asthma (25). Therefore, airway inflammation is
the basic condition of reversible airway inhibition, as well as
non-special hyperresponsiveness of the bronchus. In the present
study, the percentage of EOS in the BALF and the levels of IgE in
the chronic asthma group were higher compared with the normal group
(P<0.05). PAS staining revealed that mucus secretion was
elevated in the chronic asthma group. Furthermore, the level of IgG
was observed to decrease in the chronic asthma group. These results
indicated that the immune reaction in individuals suffering chronic
asthma is restrained.
Hormonal nebulizer inhalation has become a common
clinical treatment for non-special airway inflammation; however,
this suppresses the immune system. Due to the geography and climate
of the Autonomous region of Xinjiang, the incidence of asthma is
increasing. There are a number of effective strategies and
medicines for treating asthma in Uygur medicine. Hyssopus
officinalis L. is an Uygur medicine used for the treatment of a
number of conditions, including asthma, coughing, fever and
rheumatism (26). In a number of
previous studies, Hyssopus officinalis L. has been
demonstrated to affect the expression of a number of cytokines
(8–10). In the present study, mice treated
with Hyssopus officinalis L. and dexamethasone were shown to
have decreased levels of EOS in the BALF when compared with mice in
the chronic asthma group (10.08±1.29, 10.27±0.85 and 17.56±1.71,
respectively; P<0.05). In addition, the level of IgE and the
secretion of airway mucus were reduced. Mice treated with
Hyssopus officinalis L. were also shown to have higher
levels of IgG when compared with the dexamethasone and asthma
groups (111.71±11.79, 101.69±7.02 and 91.27±10.69, respectively;
P<0.05). These observations indicate that Hyssopus
officinalis L. may exhibit an anti-inflammatory effect by
inhibiting the infiltration of EOS and reducing the level of IgE in
the lung tissue; thus, regulating immunity.
In conclusion, the results of the present study
demonstrate the effect of Hyssopus officinalis L. on chronic
asthma, and may provide a novel therapeutic strategy for the
treatment of chronic asthma. However, further investigation is
required to determine the specific mechanism.
Acknowledgements
The study was supported by grants for innovation
from Xinjiang Medical University (no. XJC2012-20), the Autonomous
Region of Xinjiang Leading Academic Discipline Project of Pathogeny
Biology (no. XYDXK 50780328) and the National Science Foundation of
the Autonomous Region of Xinjiang (no. 200821129).
References
|
1
|
Lemanske RF Jr and Busse WW: Asthma:
clinical expression and molecular mechanisms. J Allergy Clin
Immunol. 125(Suppl 2): S95–S102. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Herrick CA and Bottomly K: To respond or
not to respond: T cells in allergic asthma. Nat Rev Immunol.
3:405–412. 2003. View
Article : Google Scholar : PubMed/NCBI
|
|
3
|
Wei M, Chu X, Guan M, et al:
Protocatechuicacid suppresses ovalbumin-induced airway inflammation
in a mouse allergic asthma model. Int Immunopharmacol. 4:780–788.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Wang W, Huang KW, Wu BM, Wang YJ and Wang
C: Correlation of eosinophil counts in induced sputum and
fractional concentration of exhaled nitric oxide and lung functions
in patients with mild to moderate asthma. Chin Med J (Engl).
125:3157–3160. 2012.PubMed/NCBI
|
|
5
|
Hannah JG and Sutton BJ: IgE in allergy
and asthma today. Nat Rev Immunol. 8:205–217. 2008. View Article : Google Scholar
|
|
6
|
Rogers DF: Airway mucus hypersecretion in
asthma: an undervalued pathology? Curr Opin Pharmacol. 4:241–250.
2004. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Zhao KZ, Lu JR, Zhang YF, et al: Changes
of the levels of interleukin-13 and total immunoglobulin E in
children with asthma. Jilin Da Xue Xue Bao Yi Xue Ban. 29:212–213.
2003.(In Chinese).
|
|
8
|
Wang YN, Ma J, Ma XM, et al: Effects of
Uygur herb Hyssopus officinalis L. on cytokines in allergic
asthma mice. Shanghai Zhong Yiyao Daxue Xuebao. 22:58–60. 2008.
|
|
9
|
Hou M, Zhu M, Ma XM, et al: Effects of
Uygur medicine Hyssopus officinalis L. on serum IL-17 level
and balance of Th1/Th2 of asthma rats. Zhongguo Xian Dai Yi Xue Za
Zhi. 20:365–368. 2010.(In Chinese).
|
|
10
|
Hou M, Ma XM, Ding JB, et al: Effect of
Uygur medicine Hyssopus officinalis L. on serum eotaxin-2,
eotaxin-3 and sP-selectin level of asthma rats. Science &
Technology Review. 28:90–93. 2009.
|
|
11
|
Ma XP, Ma XM, Ding JB, et al: Extraction
process of polysaccharide from Hyssopus officinalis. Chin
JMAP. 28:437–439. 2011.
|
|
12
|
Du Q, Zhang Q, Shen L, et al: Effects of
astragaloside IV on airway remodeling in a murine model of chronic
asthma. Zhongguo Yao Li Xue Tong Bao. 27:1430–1434. 2011.(In
Chinese).
|
|
13
|
Kim MS, Cho KA, Cho YJ and Woo SY: Effects
of interleukin-9 blockade on chronic airway inflammation in murine
asthma models. Allergy Asthma Immunol Res. 5:197–206. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Chong L, Zhang W, Nie Y, Yu G, Liu L, et
al: Protective effect of curcumin on acute airway inflammation of
allergic asthma in mice through Notch1–GATA3 signaling pathway.
Inflammation. Apr 6–2014.(Epub ahead of print).
|
|
15
|
Blonder JP, Mutka SC, Sun X, Qiu J, et al:
Pharmacologic inhibition of S-nitrosoglutathione reductase protects
against experimental asthma in BALB/c mice through attenuation of
both bronchoconstriction and inflammation. BMC Pulm Med. 14:32014.
View Article : Google Scholar
|
|
16
|
Asano T, Kume H, Taki F, et al:
Thalidomide attenuates airway hyperresponsiveness and eosinophilic
inflammation in a murine model of allergic asthma. Biol Pharm Bull.
33:1028–1032. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Lu S, Li C, Ming M and Luo Z: Inhalation
of inactivated Mycobacterium phlei down-regulates expression of
nuclear factor-kappa B and intercellular adhesion molecule in
asthmatic mice. Chinese J Pathophysiol. 30:333–338. 2014.
|
|
18
|
Zhang W, Zhu T, Wang D, et al:
Rosuvastatin attenuates airway inflammation of chronic asthma in
mice. Med J West China. 26:150–153. 2014.
|
|
19
|
Chu Y: Progress in the association of high
affinity IgE receptor with asthma. Int J Pediatrics. 38:280–282.
2011.
|
|
20
|
Stone KD, Prussin C and Metcalfe DD: IgE,
mast cells, basophils, and eosinophils. J Allergy Clin Immunol.
125(Suppl 2): S73–S80. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Locksley RM: Asthma and allergic
inflammation. Cell. 140:777–783. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Hargreave FE and Nair P: Point: Is
measuring sputum eosinophils useful in the management of severe
asthma? Yes Chest. 139:1270–1273. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Regina MCPinto, Alberto C, Luciene A, et
al: Clinical characteristics and possible phenotypes of an adult
severe asthma population. Respir Med. 106:47–56. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Jatakanon A, Lim S, Kharitonov SA, Chung
KF and Barnes PJ: Correlation between exhaled nitric oxide, sputum
eosinophils, and methacholine responsiveness in patients with mild
asthma. Thorax. 53:91–95. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Ichiki H, Hoshino T, Kinoshita T, et al:
Thioredoxin suppresses airway hyperresponsiveness and airway
inflammation in asthma. Biochem Biophys Res Commun. 334:1141–1148.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Liu YM and Wushati Y: Hyssopus
offcinalis L.. J Uygur Med. Xinjiang Science & Technology
& Hygiene Publishing House; Ürümqi, China: pp. 423–429.
1999
|