Introduction
Mixed epithelial and stromal tumor (MEST) is a
biphasic renal tumor predominant in women, possessing epithelial
(tubular glandular architecture) and stromal (similar to the
ovarian stroma, expressing estrogen and progesterone receptors and
CD10) elements, with only 10 diagnosed cases among 4,532 renal
tumors between 1987 and 2005 as reported by the Cleveland Clinic
(1). MEST is classified as a mixed
mesenchymal and epithelial tumor in the current World Health
Organization classification (2).
Tumorigenesis is likely hormonally determined. These tumors are
mostly benign, but malignant transformation of the stromal element
has also been reported (1).
Computed tomography (CT) shows several variants,
including solid enhancing components or cystic tumors, such as
Bosniak III or IV. This suggests that differential diagnosis from
cystic renal cell carcinoma (RCC) and/or plain RCC may be
challenging. Renal MEST is usually resected based on a preoperative
diagnosis of RCC, which may lead to surgical overtreatment.
Bilateral and multiple cases are rarely reported
(1). We herein present a case with
bilateral and multiple MESTs, in which overtreatment was
avoided.
Case report
A 43-year-old Japanese woman consulted a primary
care physician for gross hematuria. The patient's medical and
family history was unremarkable. Urinalysis revealed mild occult
blood reaction 1+ and red blood cells (RBCs) 30–49/high-power
field. The serum creatinine level and estimated glomerular
filtration rate were 0.64 mg/dl and 79.9 ml/min/1.73 m2,
respectively. On MAG3 renal scintigraphy, the split renal function
was 41 and 59% in the right and left kidneys, respectively. On
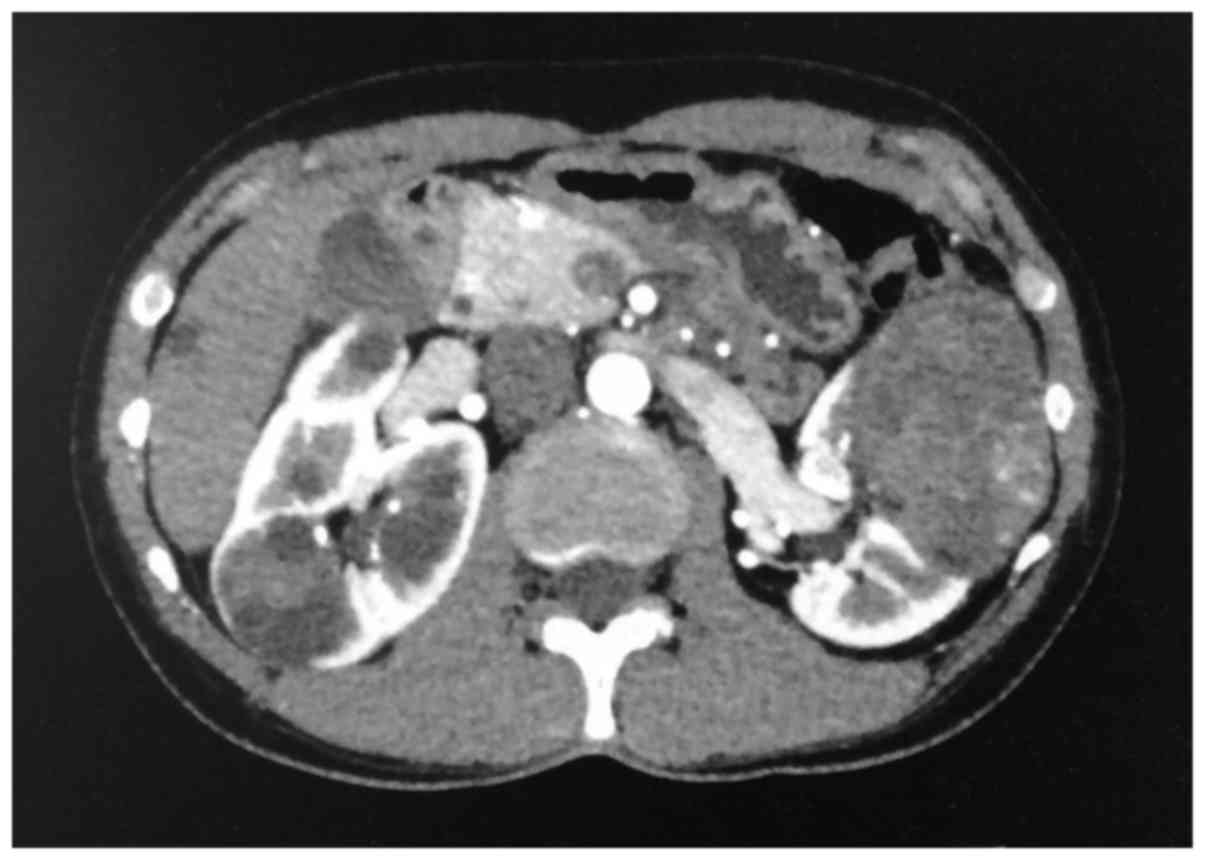
abdominal CT, 2 tumors (73 and 28 mm in diameter) were identified
in the left kidney, and 5 tumors (15–50 mm in diameter) were
identified in the right kidney. The tumors were heterogeneous on
CT, appearing as enhanced masses including cysts with irregular
septa, suggesting Bosniak IV cystic RCC; solid masses were
observed, which were enhanced in the corticomedullary phase and
washed out in the delayed phase (Fig.
1). Genetic testing excluded Von Hippel-Lindau disease. Therapy
was planned based on the preoperative diagnosis of RCC. Preserving
the right kidney appeared to be difficult due to the presence of 5
large tumors. Therefore, left partial nephrectomy followed by right
radical nephrectomy was planned. Following left nephrectomy, the
resected tumors were pathologically diagnosed as MESTs, without
malignant characteristics. Accordingly, the right kidney tumors
were also suspected to be MESTs and a CT-guided biopsy confirmed
this diagnosis; thus, the right kidney was spared. The patient is
currently periodically followed-up with CT every 4–6 months.
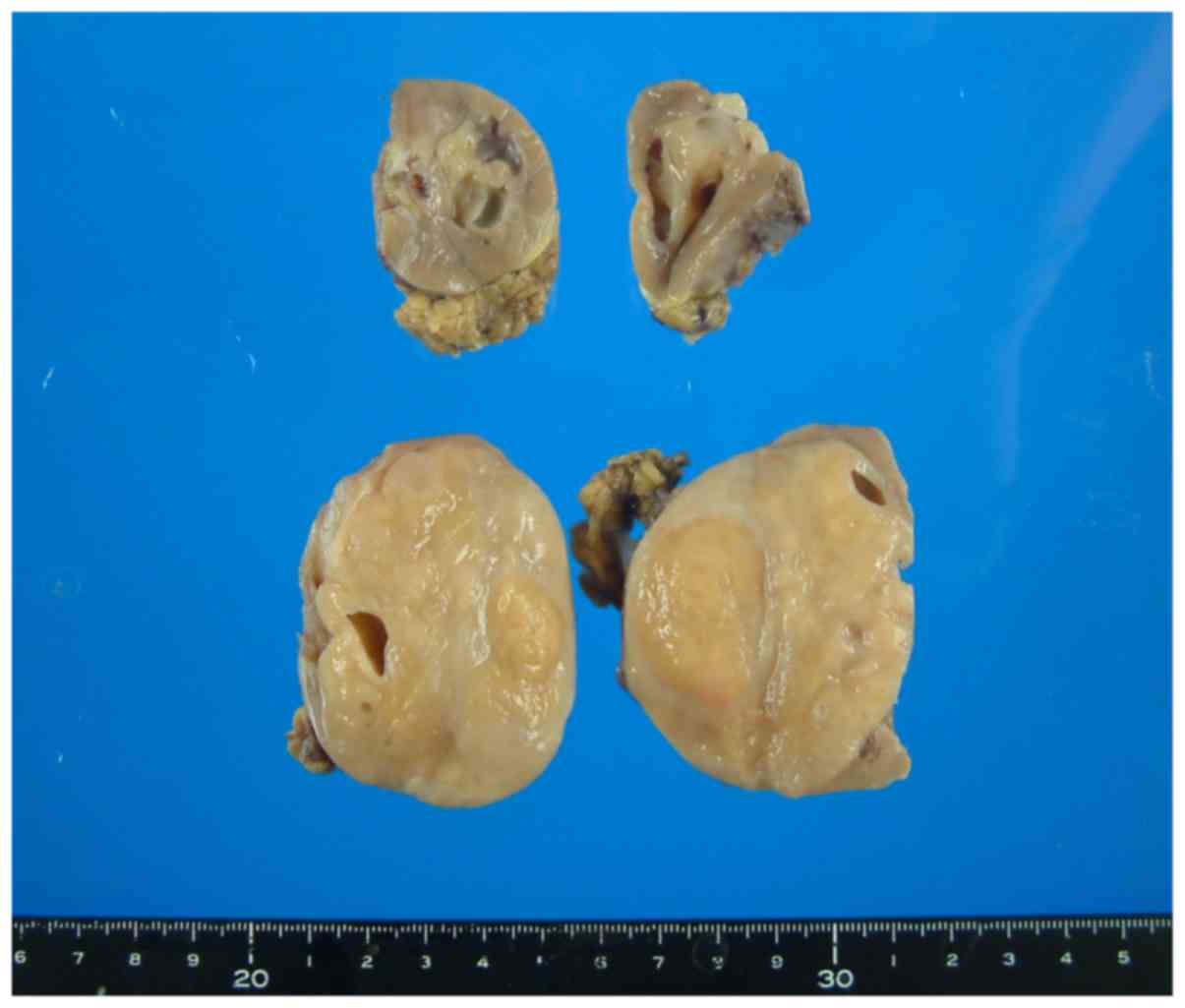
Grossly, the partially resected left kidney
contained two well-demarcated, brownish tumors. The cut surface of
the tumors was mostly solid and firm, with occasional cystic spaces
(Fig. 2).
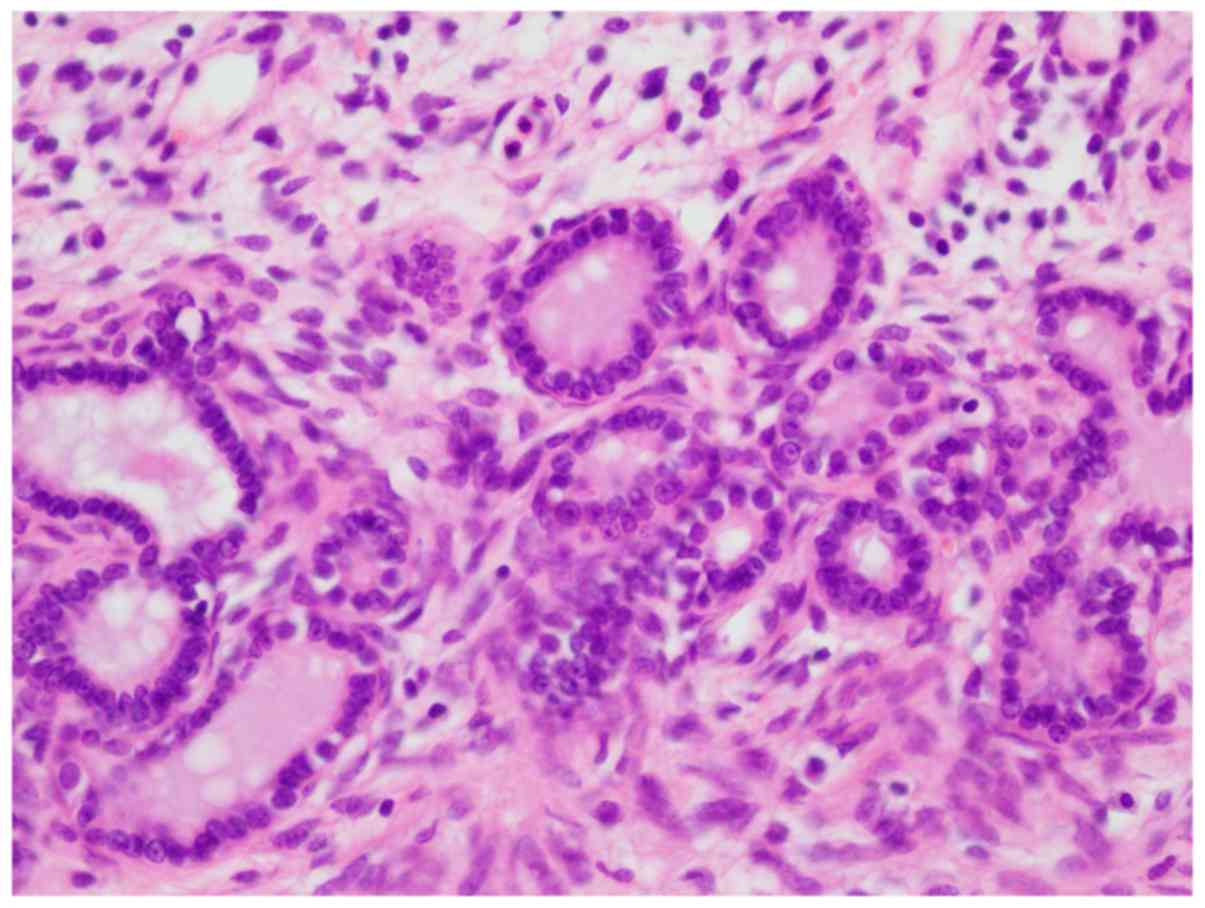
Histologically, the tumors were well demarcated from
the surrounding renal parenchyma, without a pseudocapsule. The
tumors predominantly comprised a stromal element, with bland
spindle cells. The stroma exhibited various-sized tubuloglandular
and cystic formations lined by columnar epithelia, without atypia.
The stromal cells were spindle-shaped, with scanty cytoplasm and
without nuclear atypia. Immunohistochemically, the stroma cells
were positive for estrogen receptor (ER), progesterone receptor
(PR), α-smooth muscle actin (SMA) and vimentin (Fig. 3). The pathological and
immunohistochemical findings were compatible with the diagnosis of
MEST. There were only few structurally abnormal cells and the
mitotic count was low, suggesting benign MEST.
The needle biopsy specimen from the contralateral
kidney also confirmed the diagnosis of MEST; thus, the right kidney
was spared.
Discussion
MEST is a biphasic tumor comprising epithelial and
stromal components, and is classified as a mixed mesenchymal and
epithelial tumor in the current World Health Organization
classification (2). Of the 4,532
renal tumors, 10 (0.2%) were diagnosed as MEST between 1987 and
2005 at the Cleveland Clinic (1).
The mean patient age was 46 years, with a male:female ratio of 1:6
(3,4). In men, MEST tends to occur following
endocrine treatment for prostate cancer. Bilateral cases are rare,
with the first bilateral MEST reported in 2008 by Sangoi et
al (5).
The present case is rare, and presented with gross
hematuria. Lane et al reported that 67% of the patients
presented with hematuria, flank pain and a palpable mass (1). Recent studies reported the most common
characteristics of MEST to be a flank mass (31.8%) and gross
hematuria (27.3%) (4). A total of
25% of MESTs are incidentally discovered, and they comprise
0.20–0.28% of all renal tumors (6).
The tumors are generally sized >5 cm (mean, 12.3 cm) (4). The patient presented herein also had
large tumors (2 tumors with diameters of 73 and 28 mm in the left
kidney; and 5 tumors sized 10–51 mm in the right kidney), resulting
in gross hematuria.
Radiologically, MEST includes various proportions of
solid and cystic components. Lane et al reported that 7/10
(70%) MESTs had solid enhancing components, including 3 Bosniak IV
lesions and 4 solid enhancing lesions (1). Additionally, the radiological
characteristics of MEST include thin, hair-like septae, curvilinear
calcifications an and irregular surface (1). These characteristics were consistent
with those observed in the present case. The left kidney tumors
exhibited solid components that were enhanced in the early phase
and washed out in the delayed phase, which caused difficulty in
distinguishing them from clear-cell RCCs. However, the right kidney
tumors displayed mixed characteristics, including solid masses and
cystic lesions with enhancing solid components, suggesting Bosniak
IV RCC. Thus, the preoperative diagnosis of MEST based solely on
radiological characteristics is likely problematic.
Grossly, the proportion of cystic to solid component
varies. In cases with a dominant cystic architecture, cystic
nephroma may be the suspected diagnosis. The microscopic
characteristics of MEST are epithelial cells arranged in a
tubulocystic pattern in a background of stroma with bland spindle
cells (4,7). Immunohistochemically, MEST stains
positive for epithelial components with antibodies to cytokeratin
(CK), particularly CK7. Stromal components express vimentin, SMA,
caldesmon and desmin, whereas expression of CD10, calretinin,
inhibin, ER and PR may also be resent (4). ER and PR were positive in 4 and 2 of 4
cases, respectively (1). The tumors
in the present case were positive for ER, PR, α-SMA and
vimentin.
MESTs are generally benign, but rare cases of
malignant transformation have been reported (8,9). Some
cases also exhibit an aggressive course, with tumor recurrence or
disease-related death (8,9). Lane et al (1) reported that 1 of 10 (10%) MESTs had a
malignant sarcomatous component. In the present case, the 2 left
kidney tumors were completely removed by partial nephrectomy and
the 5 right kidney tumors remained untreated. These 5 tumors
included 4 cystic tumors with small enhancing solid components and
1 solid tumor. The solid tumor was pathologically diagnosed as
benign MEST following CT-guided needle biopsy. In the majority of
previous reports, MEST was surgically removed, as RCC was suspected
and preoperative radiological diagnosis of MEST is difficult.
Therefore, active surveillance of unresected MESTs has not been
previously reported. However, there is a possibility that the
remaining tumors are malignant, although the solid parts in these
cystic lesions are scarce, so the possibility of a rapidly growing
malignant tumor is low. Although right kidney tumor removal was not
performed, the patient undergoes periodical CT check-ups every 4–6
months to monitor the malignant potential in the remaining
tumors.
Glossary
Abbreviations
Abbreviations:
|
MEST
|
mixed epithelial and stromal tumor
|
|
CT
|
computed tomography
|
|
RCC
|
renal cell carcinoma
|
References
|
1
|
Lane BR, Campbell SC, Remer EM, Fergany
AF, Williams SB, Novick AC, Weight CJ, Magi-Galluzzi C and Zhou M:
Adult cystic nephroma and mixed epithelial and stromal tumor of the
kidney: Clinical, radiographic, and pathologic characteristics.
Urology. 71:1142–1148. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Eble JN, Sauter G, Epstein JI and
Sesterhenn IA: World Health Organization Classification of
TumorsPathology and Genetics of Tumours of the Urinary System and
Male Genital Organs. IARC Press; Lyon: 2004
|
|
3
|
Montironi R, Mazzucchelli R, Lopez-Beltran
A, Martignoni G, Cheng L, Montorsi F and Scarpelli M: Cystic
nephroma and mixed epithelial and stromal tumour of the kidney:
Opposite ends of the spectrum of the same entity? Eur Urol.
54:1237–1246. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Moslemi MK: Mixed epithelial and stromal
tumor of the kidney or adult mesoblastic nephroma: An update. Urol
J. 7:141–147. 2010.PubMed/NCBI
|
|
5
|
Sangoi AR and Higgins JP: Bilateral mixed
epithelial stromal tumor in an end-stage renal disease patient: The
first case report. Hum Pathol. 39:142–146. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Terao H, Makiyama K, Yanagisawa M, Miyake
M, Sano F, Kita K, Murakami T, Nakaigawa N, Ogawa T, Uemura H, et
al: Mixed epithelial and stromal tumor of kidney: A case report.
Hinyokika Kiyo. 55:495–498. 2009.(In Japanese). PubMed/NCBI
|
|
7
|
Truong LD, Williams R, Ngo T, Cawood C,
Chevez-Barrios P, Awalt HL, Brown RW, Younes M and Ro JY: Adult
mesoblastic nephroma: Expansion of the morphologic spectrum and
review of literature. Am J Surg Pathol. 22:827–839. 1998.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Suzuki T, Hiragata S, Hosaka K, Oyama T,
Kuroda N, Hes O and Michal M: Malignant mixed epithelial and
stromal tumor of the kidney: Report of the first male case. Int J
Urol. 20:448–450. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Adsay NV, Eble J, Srigley JR, Jones EC and
Grignon DJ: Mixed epithelial and stromal tumor of the kidney. Am J
Surg Pathol. 24:958–970. 2000. View Article : Google Scholar : PubMed/NCBI
|